BIO 534 Part 3 b Reproductive Physiology Female

BIO 534 Part 3 b – Reproductive Physiology • Female Reproductive Physiology, part 1: Endocrine regulation of the ovarian cycle, uterine cycle, secondary sex characteristics

Fundamental Themes • Again, HPA control involving Gn. RH, FSH, LH • Relatively more (periodic) regulation of gamete release, perhaps related to costs of reproduction and problems that could occur with concurrent but asynchronous pregnancies • Cyclic control of gamete development, release • Cyclic regulation of uterine structure/function
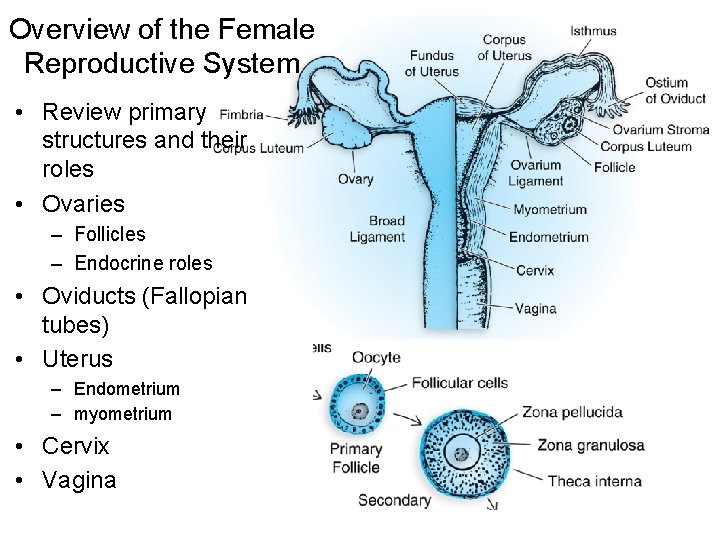
Overview of the Female Reproductive System • Review primary structures and their roles • Ovaries – Follicles – Endocrine roles • Oviducts (Fallopian tubes) • Uterus – Endometrium – myometrium • Cervix • Vagina

The Menstrual (Sexual) Cycle has 3 Components: • Ovarian cycle – Hormone production that affects cyclic uterine development/change – Ovum/Follicle development • Uterine Cycle – – Changes in endometrium vascularization, secretion Early: preparation for potential implantation Mid-cycle: maintenance Late: regression • Vaginal Cycle: changes in histological characteristics of vaginal epithelium during the sexual cycle – max growth during periovulatory period

Follicular Development During the Ovarian Cycle 6 -12/mo, via gonadotropin stimulation Thecal cells and granulosa cells serve important endocrine roles For an average 28 day cycle, this happens ______
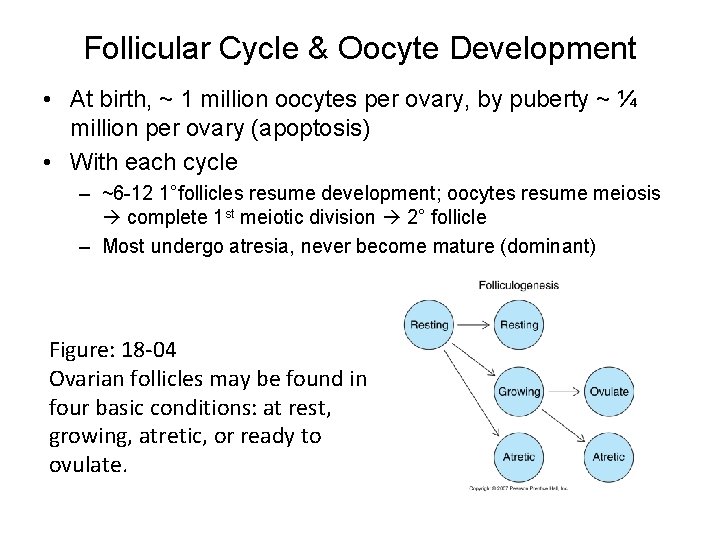
Follicular Cycle & Oocyte Development • At birth, ~ 1 million oocytes per ovary, by puberty ~ ¼ million per ovary (apoptosis) • With each cycle – ~6 -12 1°follicles resume development; oocytes resume meiosis complete 1 st meiotic division 2° follicle – Most undergo atresia, never become mature (dominant) Figure: 18 -04 Ovarian follicles may be found in four basic conditions: at rest, growing, atretic, or ready to ovulate.
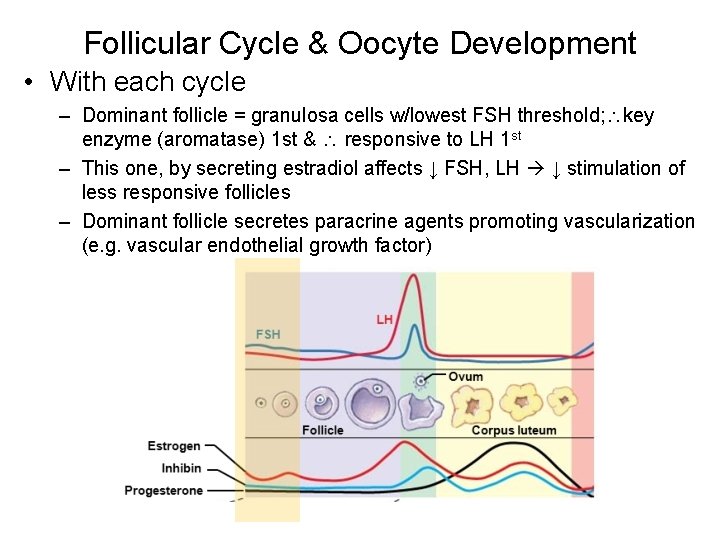
Follicular Cycle & Oocyte Development • With each cycle – Dominant follicle = granulosa cells w/lowest FSH threshold; key enzyme (aromatase) 1 st & responsive to LH 1 st – This one, by secreting estradiol affects ↓ FSH, LH ↓ stimulation of less responsive follicles – Dominant follicle secretes paracrine agents promoting vascularization (e. g. vascular endothelial growth factor)

So Far: Endocrine Inputs Simulate Gamete Development • So far, not much different than male system (other than more finite # of gametes overall and /month) • Next questions: How is cyclic release of gametes affected? • Note: The endocrine events that regulate follicular development also regulate the release of hormones that prepare the uterus for potential implantation • Thus, although somewhat separated, realize interaction
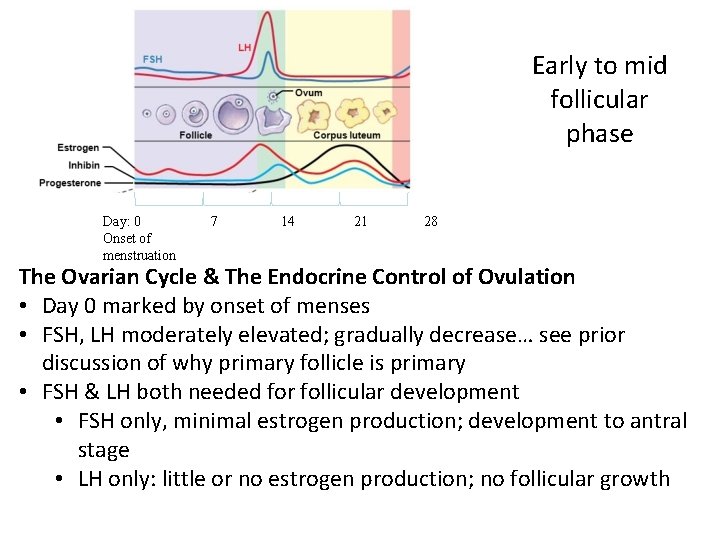
Early to mid follicular phase Day: 0 Onset of menstruation 7 14 21 28 The Ovarian Cycle & The Endocrine Control of Ovulation • Day 0 marked by onset of menses • FSH, LH moderately elevated; gradually decrease… see prior discussion of why primary follicle is primary • FSH & LH both needed for follicular development • FSH only, minimal estrogen production; development to antral stage • LH only: little or no estrogen production; no follicular growth

How do FSH/LH affect follicular hormone secretion? • FSH, LH and Estrogens needed for follicular development (& explain 1° follicle) • LH stimulates thecal cells to produce C 19 androgens from cholesterol � granulosa cells via CYP 17 gene/17 hydroxylase enzyme • FSH stimulates granulosa cells to convert the C 19 androgens to estrogens via activation of aromatase (next slide)
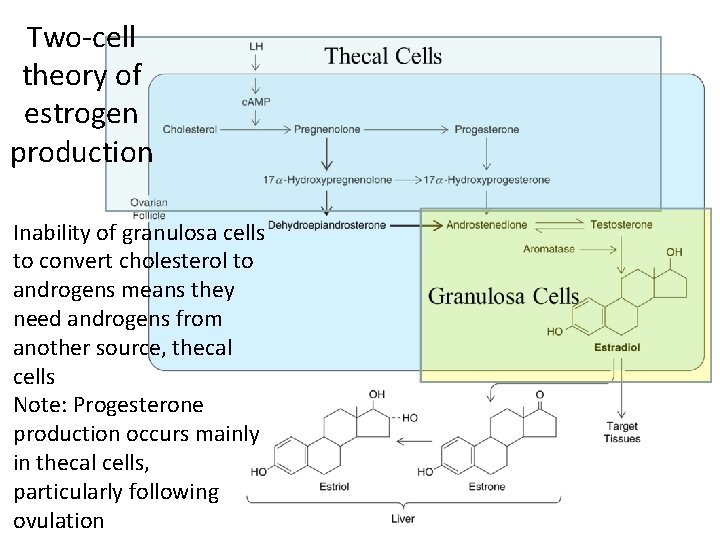
Two-cell theory of estrogen production Inability of granulosa cells to convert cholesterol to androgens means they need androgens from another source, thecal cells Note: Progesterone production occurs mainly in thecal cells, particularly following ovulation
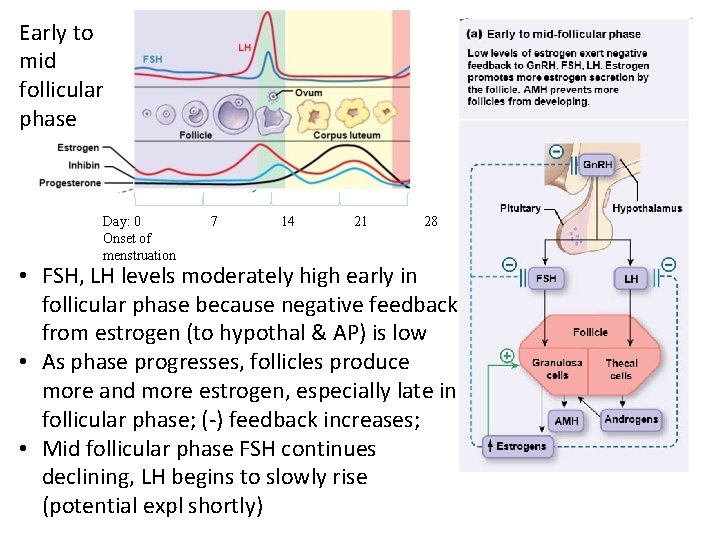
Early to mid follicular phase Day: 0 Onset of menstruation 7 14 21 28 • FSH, LH levels moderately high early in follicular phase because negative feedback from estrogen (to hypothal & AP) is low • As phase progresses, follicles produce more and more estrogen, especially late in follicular phase; (-) feedback increases; • Mid follicular phase FSH continues declining, LH begins to slowly rise (potential expl shortly)
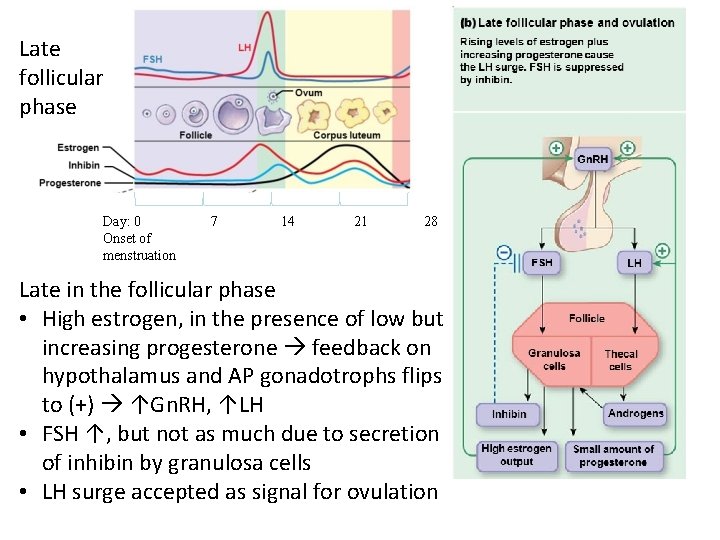
Late follicular phase Day: 0 Onset of menstruation 7 14 21 28 Late in the follicular phase • High estrogen, in the presence of low but increasing progesterone feedback on hypothalamus and AP gonadotrophs flips to (+) ↑Gn. RH, ↑LH • FSH ↑, but not as much due to secretion of inhibin by granulosa cells • LH surge accepted as signal for ovulation
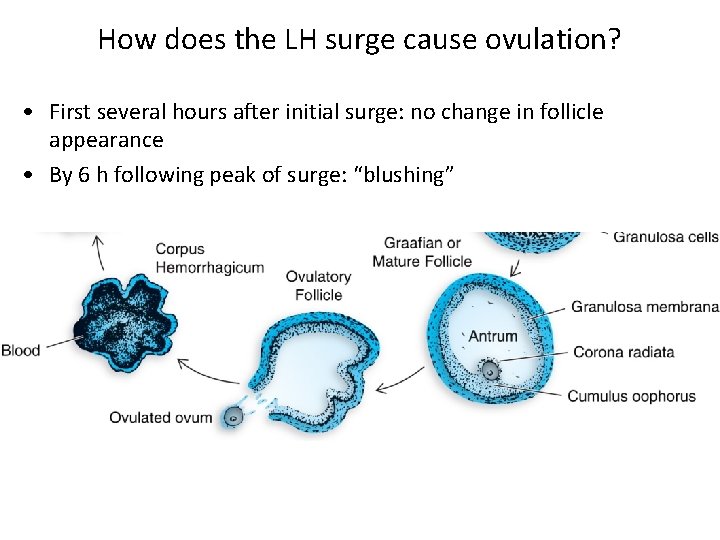
How does the LH surge cause ovulation? • First several hours after initial surge: no change in follicle appearance • By 6 h following peak of surge: “blushing”
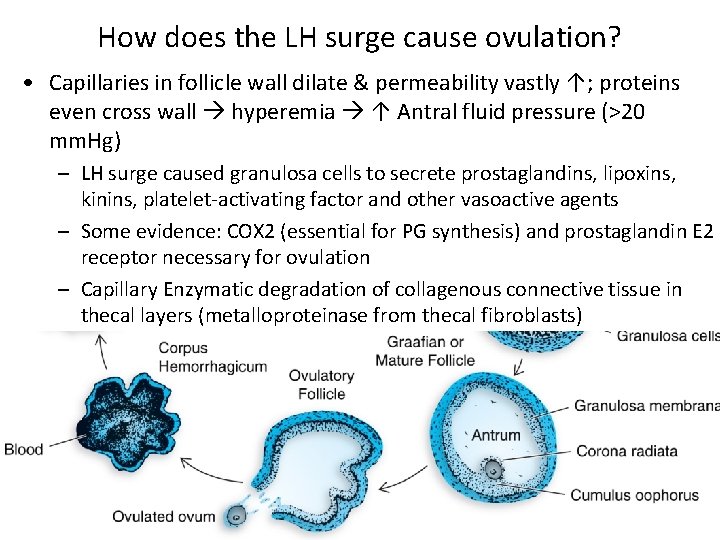
How does the LH surge cause ovulation? • Capillaries in follicle wall dilate & permeability vastly ↑; proteins even cross wall hyperemia ↑ Antral fluid pressure (>20 mm. Hg) – LH surge caused granulosa cells to secrete prostaglandins, lipoxins, kinins, platelet-activating factor and other vasoactive agents – Some evidence: COX 2 (essential for PG synthesis) and prostaglandin E 2 receptor necessary for ovulation – Capillary Enzymatic degradation of collagenous connective tissue in thecal layers (metalloproteinase from thecal fibroblasts)
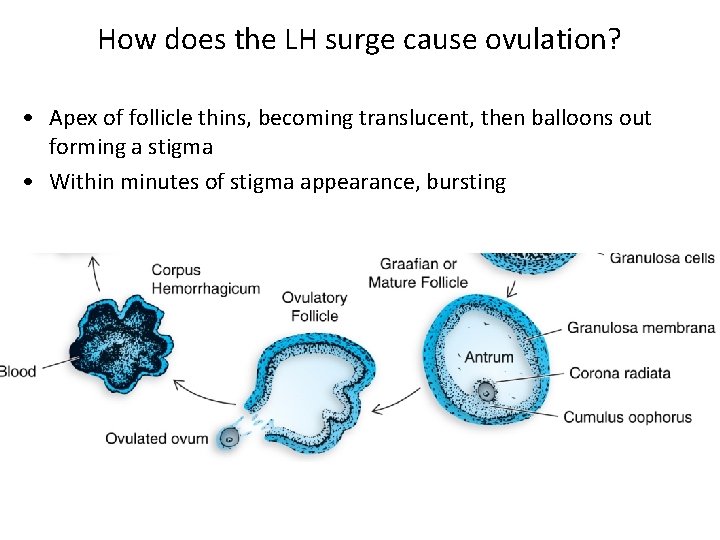
How does the LH surge cause ovulation? • Apex of follicle thins, becoming translucent, then balloons out forming a stigma • Within minutes of stigma appearance, bursting
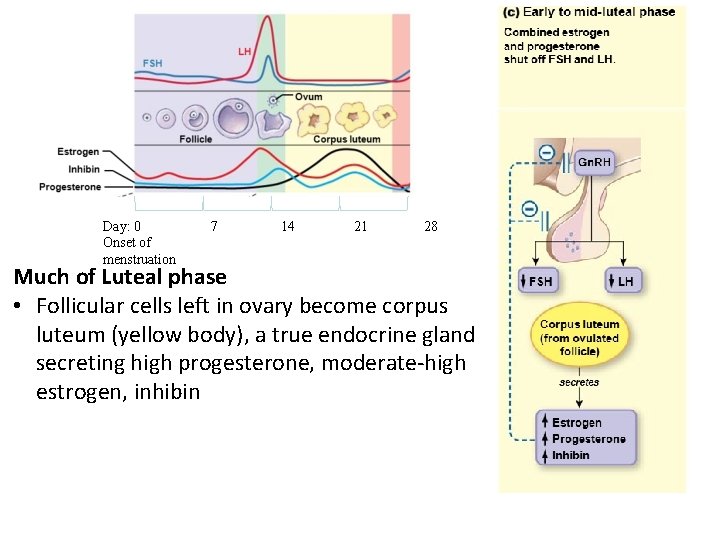
Day: 0 Onset of menstruation 7 14 21 28 Much of Luteal phase • Follicular cells left in ovary become corpus luteum (yellow body), a true endocrine gland secreting high progesterone, moderate-high estrogen, inhibin
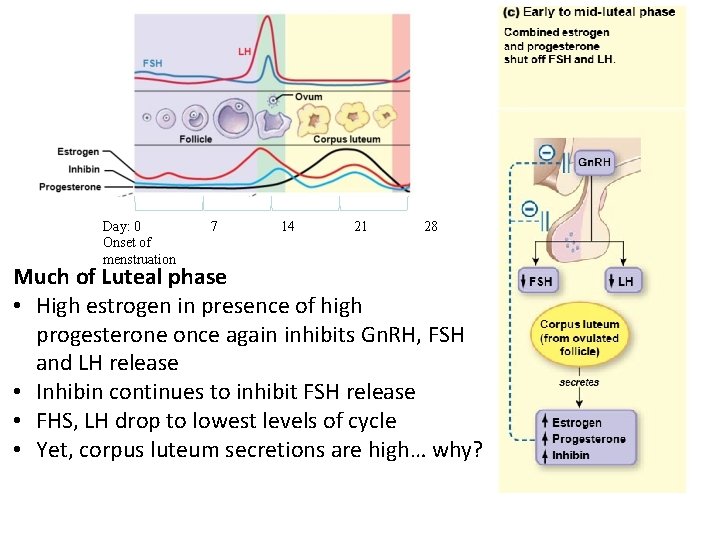
Day: 0 Onset of menstruation 7 14 21 28 Much of Luteal phase • High estrogen in presence of high progesterone once again inhibits Gn. RH, FSH and LH release • Inhibin continues to inhibit FSH release • FHS, LH drop to lowest levels of cycle • Yet, corpus luteum secretions are high… why?
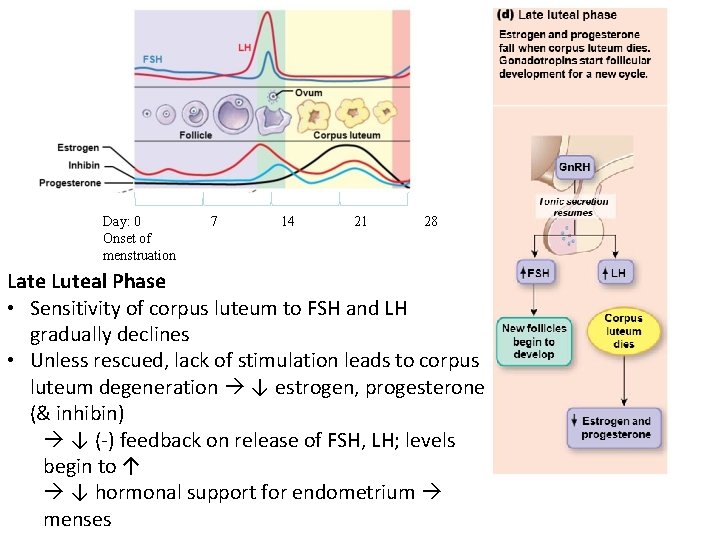
Day: 0 Onset of menstruation 7 14 21 28 Late Luteal Phase • Sensitivity of corpus luteum to FSH and LH gradually declines • Unless rescued, lack of stimulation leads to corpus luteum degeneration ↓ estrogen, progesterone (& inhibin) ↓ (-) feedback on release of FSH, LH; levels begin to ↑ ↓ hormonal support for endometrium menses

Actions of Estrogens • Estrogen does a lot of things – Feedback regulation of HPA – Autocrine feedback to granulosa – Endometrial proliferation, breast tissue, myometrium, cardiovascular, etc.

Estrogen Receptors • Two ER α and β: classic steroid hormone receptors – Estrogen binds, release of receptor from HSP, dimerization – Translocation (? ) to nucleus, recruitment of transcription complex factors/enzymes, binding to Estrogen response element – Initiation of transcription – Also seem to interact directly with other proteins (nonclassical) enhancing or repressing their actions

Progesterone Receptors • Two receptors PRA and PRB • PRA – most important in uterine and ovarian function • PRB – more important for progesterone responses in breast and other tissue

A Homework Question, in Two Slides • Low levels of estrogen and progesterone (-) feedback of gonadotropins (males and females) – Inhibition of Gn. RH secretion – Gn. RH is released in pulses due to activity of a pulse generator in the hypothalamus (neural) – Rhythmicity of Gn. RH neurons and those involved in modulating rhythm affected by various hormones, stress, dietary/metabolic cues • How: – Low levels of estrogen inhibit the hypothalamic Gn. RH pulse generator & suppress Gn. RH responsiveness in AP gonadotrophs – Progesterone inhibits Gn. RH secretion via actions in CNS in turn affecting pulse generator & directly inhibits release of LH from AP

A Homework Question, in Two Slides • Elevated estrogen causes positive feedback effect leading to an LH surge ovulation • At cellular level mechanism different than those mediating (-) feedback w/ lower estrogen – Estrogen at high enough levels acts at the AP to prime gonadotrophs to respond to Gn. RH – High enough estrogen at the hypothalamus may directly trigger a Gn. RH surge • But how is high estrogen causing the (immediately) preceding effects, when at low levels it inhibits release? That is, why are the cellular-level actions of high estrogen different from those of low estrogen? • Note: The answer is not in your book.

Next: Endocrine Regulation of Uterine Events of Menstrual (Sexual) Cycle
- Slides: 25