BII Gastric Bypass Jacques Himpens European School of

BII Gastric Bypass Jacques Himpens European School of Laparoscopy

• Dr HIMPENS is A CONSULTANT WITH ETHICON ENDO-SURGERY performs workshops for GORE
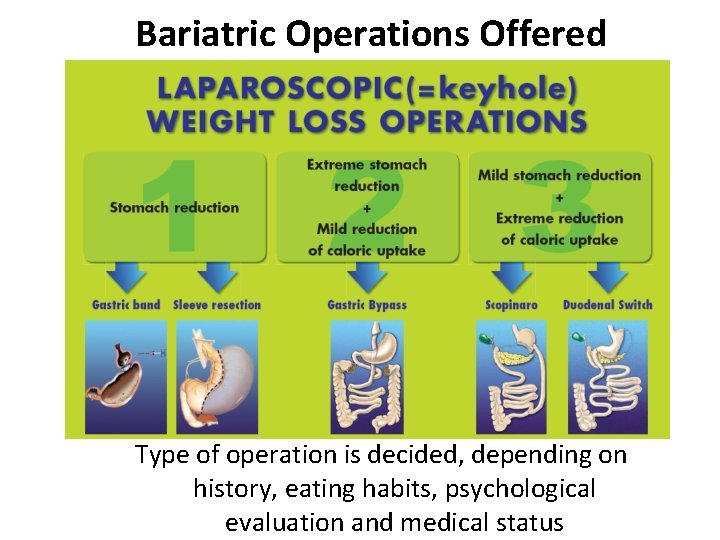
Bariatric Operations Offered Type of operation is decided, depending on history, eating habits, psychological evaluation and medical status

Choice of Procedure depends on associated conditions: Gastro-esophageal reflux: NO RESTRICTION! Diabetes

DIABETES Patients randomized to surgical therapy vs medical therapy more likely to get remission of type 2 diabetes through greater weight loss. Dixon et al. JAMA 2008 23; 299 (3) Malabsorptive procedures (biliopancreatic diversion and gastric bypass) more effective than restrictive procedures (gastroplasty and gastric banding). Levy P et al Obes Surg 2007 17 (9). METANALYSIS

Roux-en-Y gastric bypass is the only option in about 50% of the bariatric patients, either because of reflux, or because of diabetes, or both

Morbidly Obese Patient (reimbursement) BMI > 40 kg/m² BMI>35 kg/m² Metabolic Syndrome: - Hypertension - Cholesterol (HD and VLDL) - Abdominal perimeter - Sleep apnea - Insulin resistance

INSULIN RESISTANCE Obese patient needs more insulin than non obese in order to maintain eu-glycemic state

INSULIN RESISTANCE Regulated by INCRETINS probably produced in duodenum and proximal jejunum After bypass incretins secretion increased Early after bypass insulin resistance DISAPPEARS

INSULIN RESISTANCE early after bypass less insulin is needed for eu-glycemic state than before bypass If pancreas still has sufficient insulin producing capacity DM II disappears If pancreas no longer has sufficient insulin DM II will still exist but insulin needs

INSULIN RESISTANCE After bypass, and because of previous insulin resistance which is now abolished: When sugar is taken in, relatively too much insulin is produced tendency twrds hypoglycemia
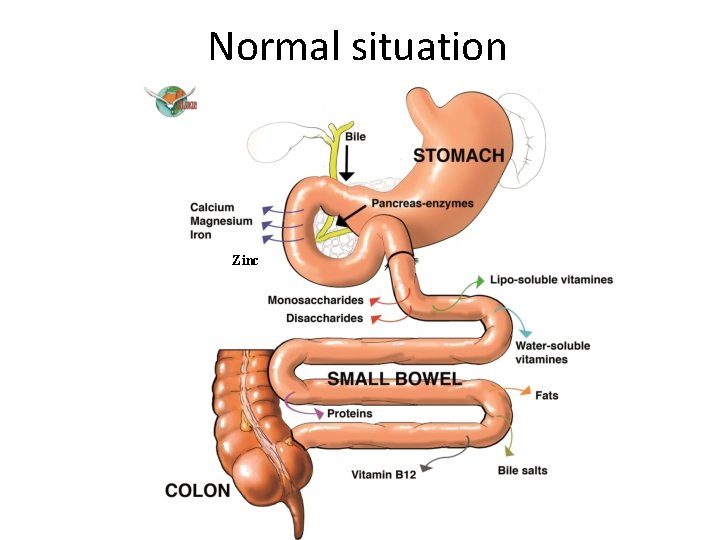
Normal situation Zinc
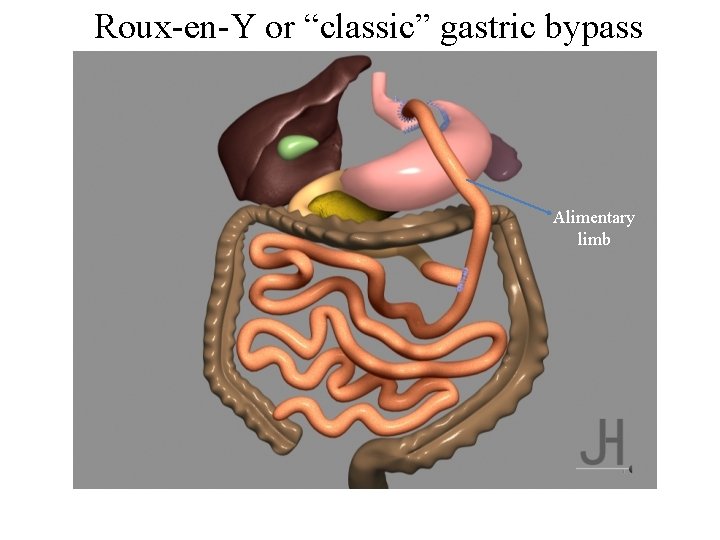
Roux-en-Y or “classic” gastric bypass Alimentary limb

BYPASS AND ABSORPTION of SUGARS Polysaccharides transit in stomach pouch Polysaccharides then move to alimentary loop, where digestive juices are absent Pace of transit into alimentary loop depends on size and compliance gastro enterostomy, and on length of alimentary loop

SUGARS ABSORPTION AND BYPASS Carbs are preferentially absorbed at level of alimentary loop via the brush border of the sma intestine: NO BUFFER FROM OTHER FOOD STUFFS Carbs are degraded to 6 C molecules (glucosidase); the more complex the sugars, the more 6 C molecules Portal system overwhelmed by sugars (tsunami) DUMPING SYNDROME TYPE 1 osmotic shock

DUMPING SYNDROME Not present in all bypass patients, actually only in minority of patients (Closset) Disappears after 1 -2 yrs Non-dumpers will eat sugars (Roslin)
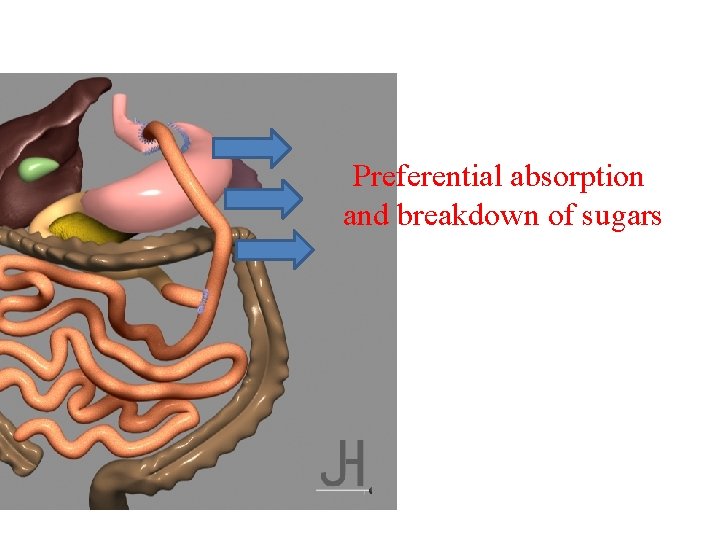
Preferential absorption and breakdown of sugars
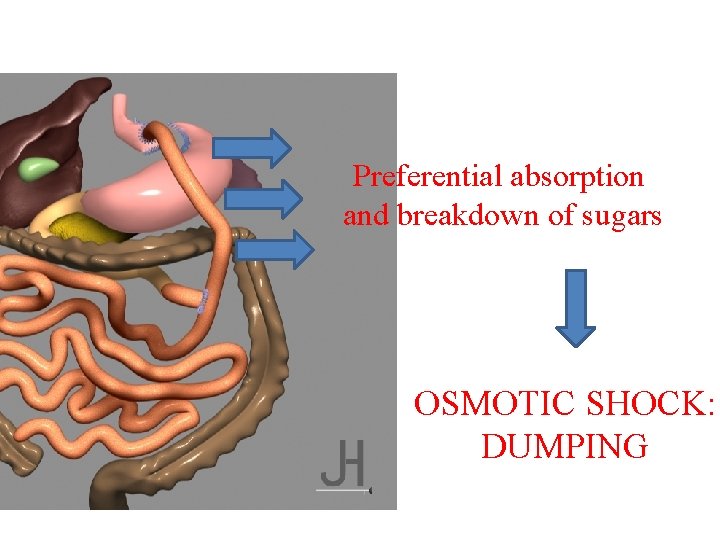
Preferential absorption and breakdown of sugars OSMOTIC SHOCK: DUMPING
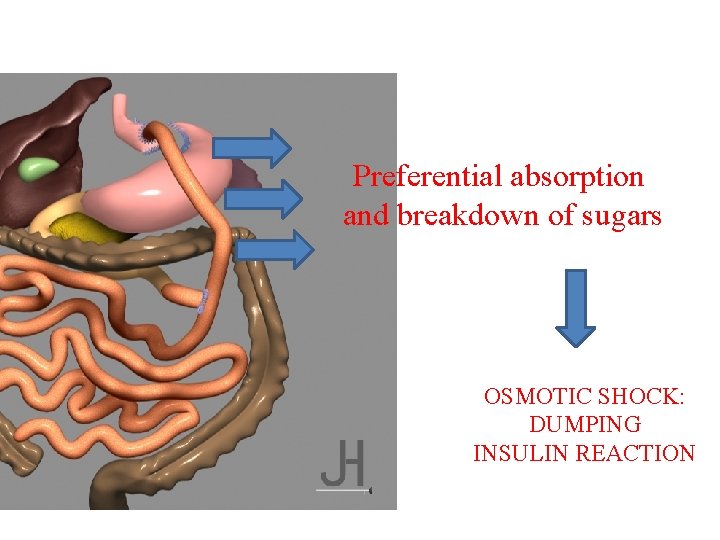
Preferential absorption and breakdown of sugars OSMOTIC SHOCK: DUMPING INSULIN REACTION
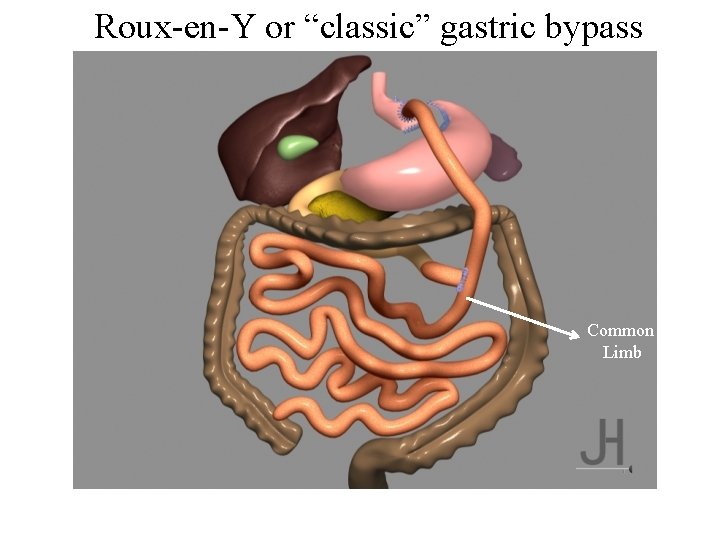
Roux-en-Y or “classic” gastric bypass h Common Limb
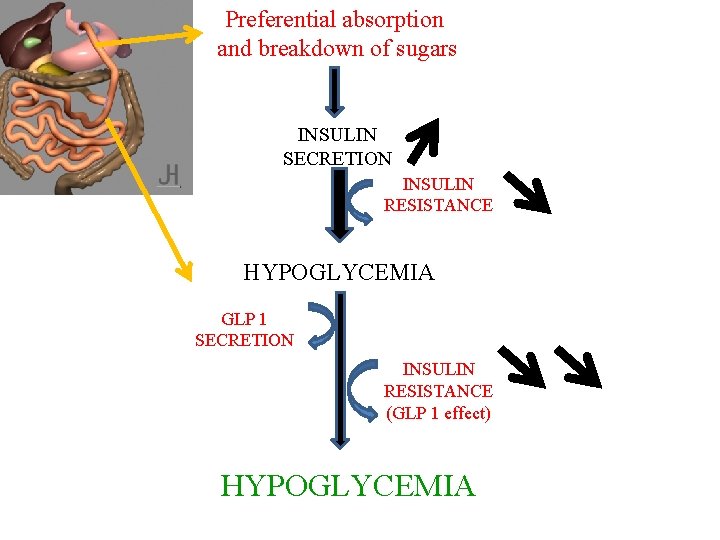
Preferential absorption and breakdown of sugars INSULIN SECRETION INSULIN RESISTANCE HYPOGLYCEMIA GLP 1 SECRETION INSULIN RESISTANCE (GLP 1 effect) HYPOGLYCEMIA

POSTPRANDIAL HYPOGLYCEMIA

POSTPRANDIAL“paradoxical” HYPOGLYCEMIA - Tiredness, exhaustion Syncopes Convulsions Cardiac arrhytmia’s

LONG TERM CONSEQUENCE: With time carbs transit much faster in alimentary limb insulin production β cell proliferation nesidioblastoma insulin stock exhausted DM II increased sensitivity to insulin, resulting in hypoglycemic symptoms

HOW TO AVOID THIS CONDITION ?

TREATMENT IS PREVENTIVE NO CARBS AFTER BYPASS “SWEET EATERS” ARE POOR CANDIDATES FOR BYPASS CONSIDER OTHER PROCEDURE Medication (acarbose, octreotide. . . )
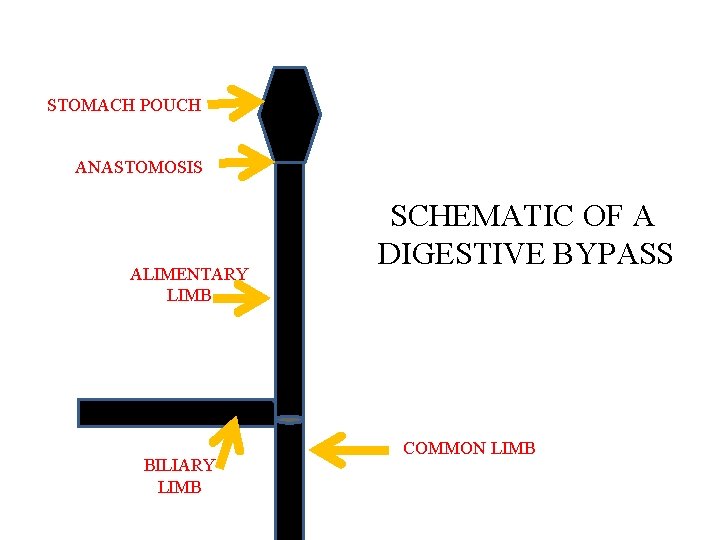
STOMACH POUCH ANASTOMOSIS ALIMENTARY LIMB BILIARY LIMB SCHEMATIC OF A DIGESTIVE BYPASS COMMON LIMB
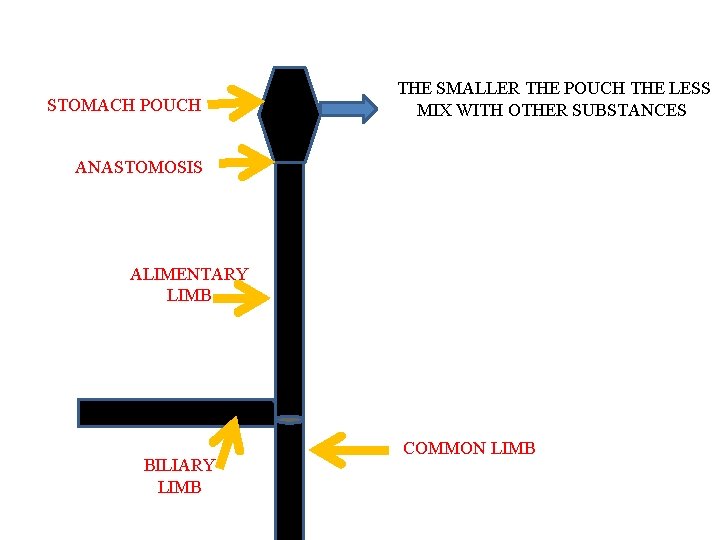
STOMACH POUCH THE SMALLER THE POUCH THE LESS MIX WITH OTHER SUBSTANCES ANASTOMOSIS ALIMENTARY LIMB BILIARY LIMB COMMON LIMB
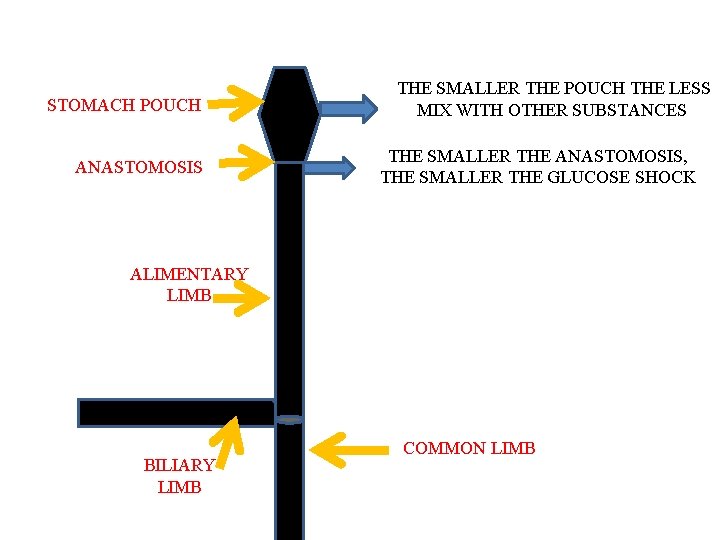
STOMACH POUCH ANASTOMOSIS THE SMALLER THE POUCH THE LESS MIX WITH OTHER SUBSTANCES THE SMALLER THE ANASTOMOSIS, THE SMALLER THE GLUCOSE SHOCK ALIMENTARY LIMB BILIARY LIMB COMMON LIMB
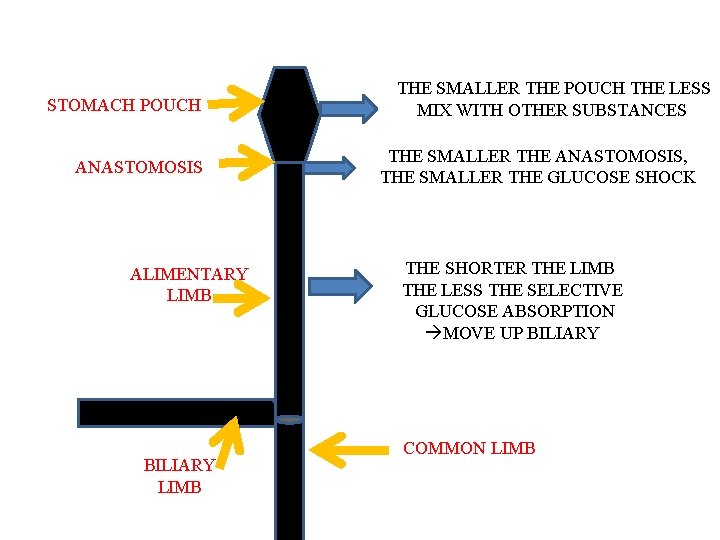
STOMACH POUCH ANASTOMOSIS ALIMENTARY LIMB BILIARY LIMB THE SMALLER THE POUCH THE LESS MIX WITH OTHER SUBSTANCES THE SMALLER THE ANASTOMOSIS, THE SMALLER THE GLUCOSE SHOCK THE SHORTER THE LIMB THE LESS THE SELECTIVE GLUCOSE ABSORPTION MOVE UP BILIARY COMMON LIMB

HOW TO REDUCE GLYCEMIC SHOCK STOMACH POUCH ANASTOMOSIS ALIMENTARY LIMB BILIARY LIMB INCREASE POUCH SIZE (but need of malabsorption!) (Scopinaro, DS)
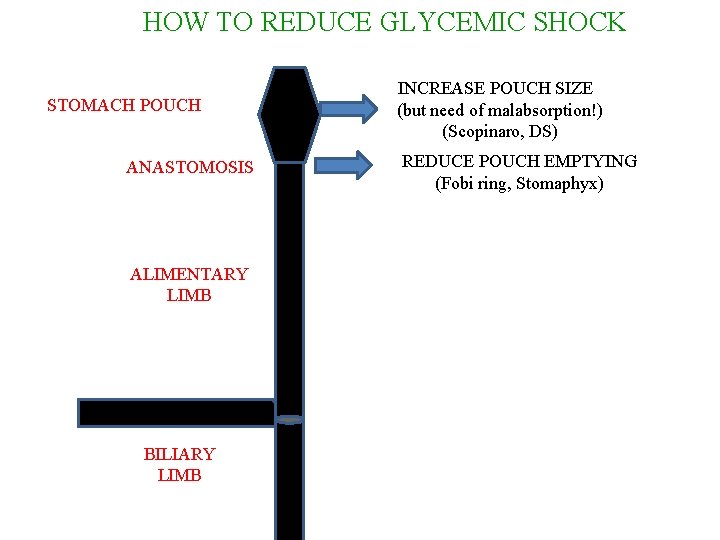
HOW TO REDUCE GLYCEMIC SHOCK STOMACH POUCH ANASTOMOSIS ALIMENTARY LIMB BILIARY LIMB INCREASE POUCH SIZE (but need of malabsorption!) (Scopinaro, DS) REDUCE POUCH EMPTYING (Fobi ring, Stomaphyx)

HOW TO REDUCE GLYCEMIC SHOCK STOMACH POUCH ANASTOMOSIS ALIMENTARY LIMB BILIARY LIMB INCREASE POUCH SIZE (but need of malabsorption!) (Scopinaro, DS) REDUCE POUCH EMPTYING (Fobi ring, Stomaphyx) REDUCE LENGTH ALIMENTARY LIMB

A “NEW” BYPASS ? ?
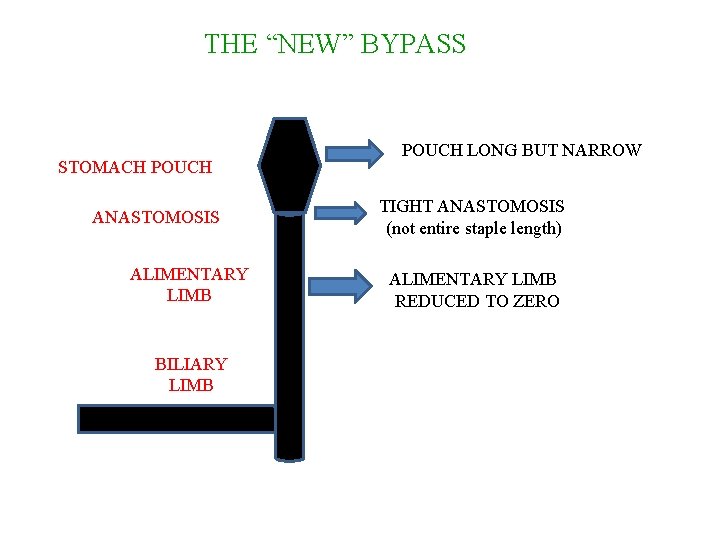
THE “NEW” BYPASS STOMACH POUCH ANASTOMOSIS ALIMENTARY LIMB BILIARY LIMB POUCH LONG BUT NARROW TIGHT ANASTOMOSIS (not entire staple length) ALIMENTARY LIMB REDUCED TO ZERO
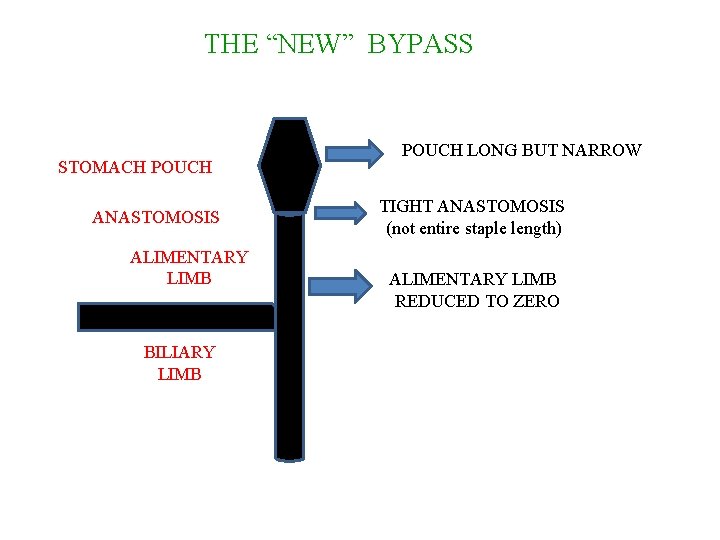
THE “NEW” BYPASS STOMACH POUCH ANASTOMOSIS ALIMENTARY LIMB BILIARY LIMB POUCH LONG BUT NARROW TIGHT ANASTOMOSIS (not entire staple length) ALIMENTARY LIMB REDUCED TO ZERO
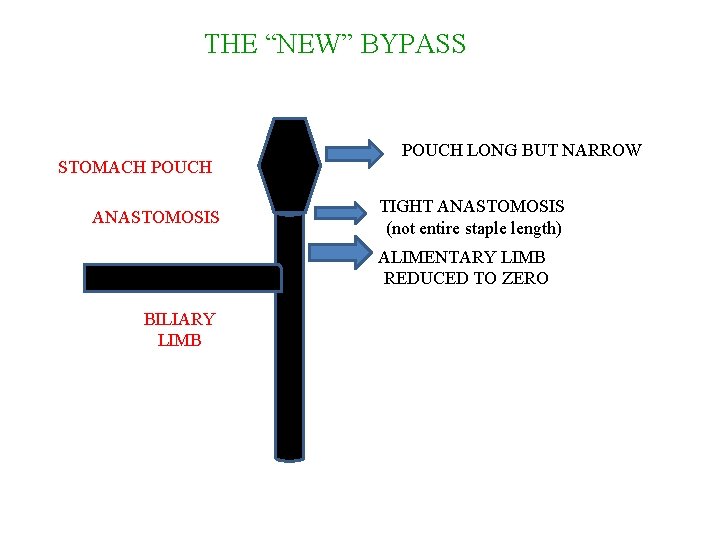
THE “NEW” BYPASS STOMACH POUCH ANASTOMOSIS POUCH LONG BUT NARROW TIGHT ANASTOMOSIS (not entire staple length) ALIMENTARY LIMB REDUCED TO ZERO BILIARY LIMB
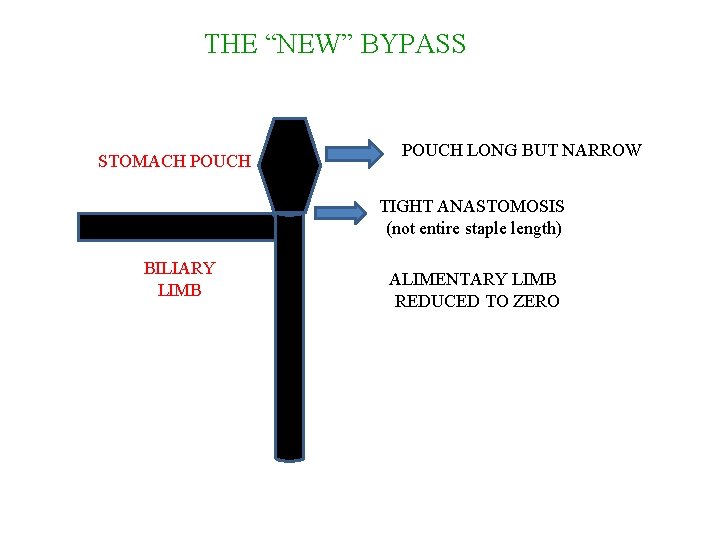
THE “NEW” BYPASS STOMACH POUCH LONG BUT NARROW TIGHT ANASTOMOSIS (not entire staple length) BILIARY LIMB ALIMENTARY LIMB REDUCED TO ZERO

“NEW” OPERATION THE MINI GASTRIC BYPASS
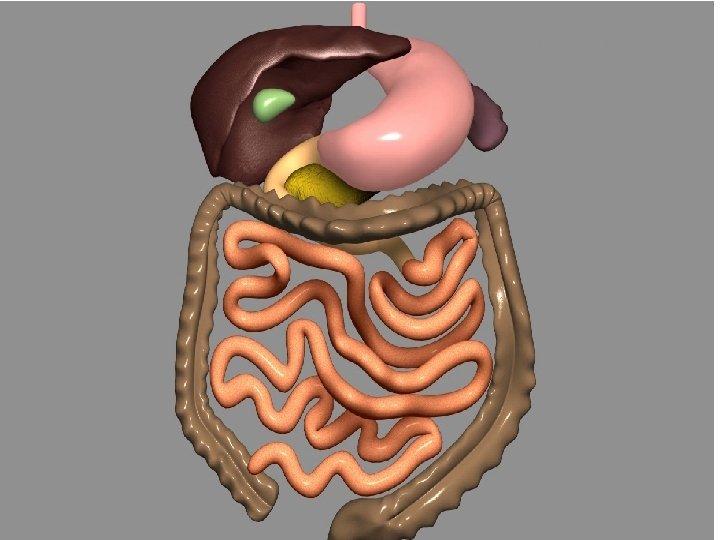
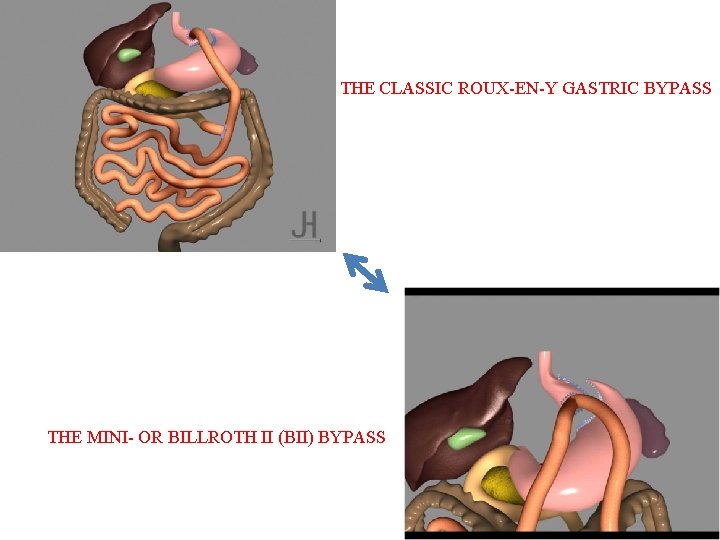
THE CLASSIC ROUX-EN-Y GASTRIC BYPASS THE MINI- OR BILLROTH II (BII) BYPASS

MINI BYPASS INTRODUCED BY RUTLEDGE USA DEMONIZED! (CANCER, ULCERS) CHEVALLIER PARIS

MINI BYPASS: PRO’S

MINI BYPASS: PRO’S EASIER TECHNIQUE LESS € 24 HRS

MINI BYPASS: PRO’S EASIER TECHNIQUE LESS € 24 HRS SIMILAR RESULTS? PROBABLY BETTER
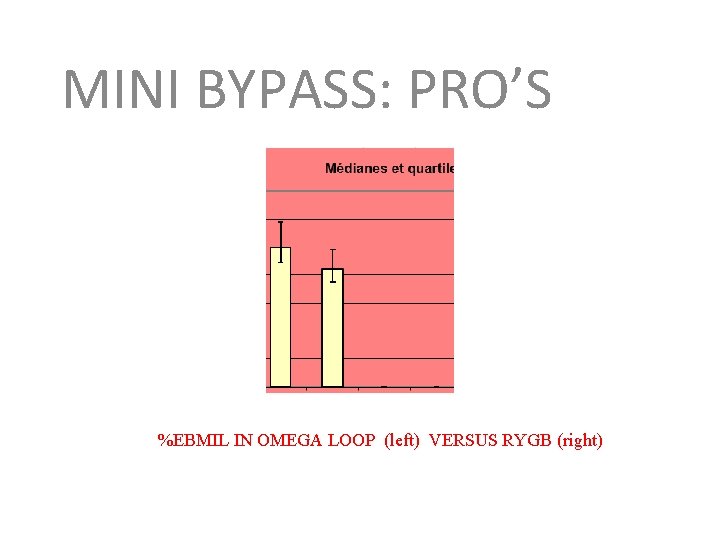
MINI BYPASS: PRO’S %EBMIL IN OMEGA LOOP (left) VERSUS RYGB (right)

MINI BYPASS: PRO’S EASIER TECHNIQUE LESS € 24 HRS SIMILAR RESULTS FULLY RECONVERTIBLE

MINI BYPASS: PRO’S EASIER TECHNIQUE LESS € 24 HRS SIMILAR RESULTS FULLY RECONVERTIBLE INSULIN SHOCK LESS
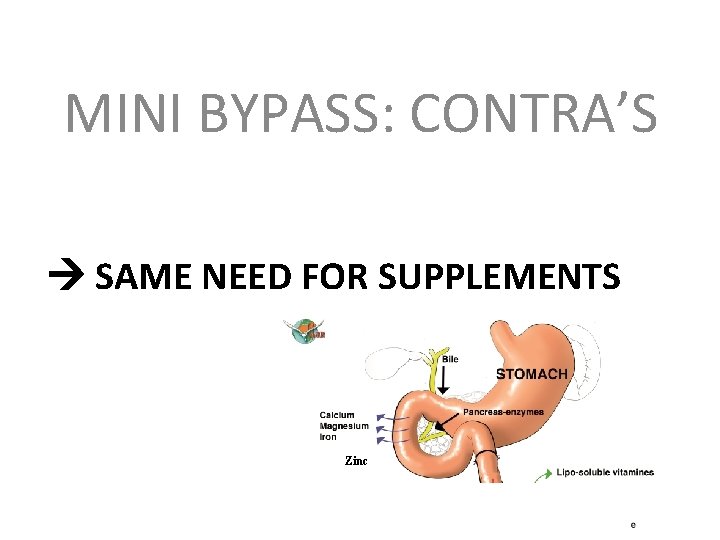
MINI BYPASS: CONTRA’S SAME NEED FOR SUPPLEMENTS Zinc

MINI BYPASS: CONTRA’S SAME NEED FOR SUPPLEMENTS IN LEAKS NO STENTS

Self Expandable Metal Stents (SEMS) Z stent Wallstent Ultraflex Endoscopic view of the Ultraflex

MINI BYPASS: CONTRA’S SAME NEED FOR SUPPLEMENTS IN LEAKS NO STENTS AFFERENT/EFFERENT LOOP SYNDROME

MINI BYPASS: CONTRA’S SAME NEED FOR SUPPLEMENTS IN LEAKS NO STENTS AFFERENT/EFFERENT LOOP SYNDROME AFFERENT LOOP
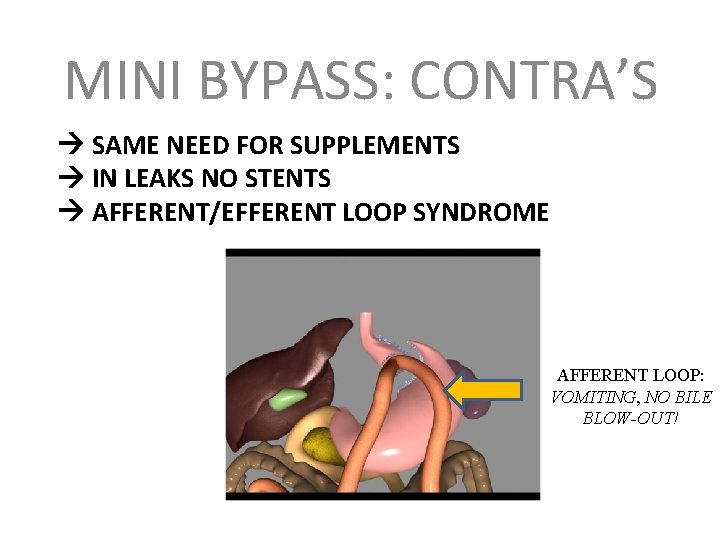
MINI BYPASS: CONTRA’S SAME NEED FOR SUPPLEMENTS IN LEAKS NO STENTS AFFERENT/EFFERENT LOOP SYNDROME AFFERENT LOOP: VOMITING, NO BILE BLOW-OUT!
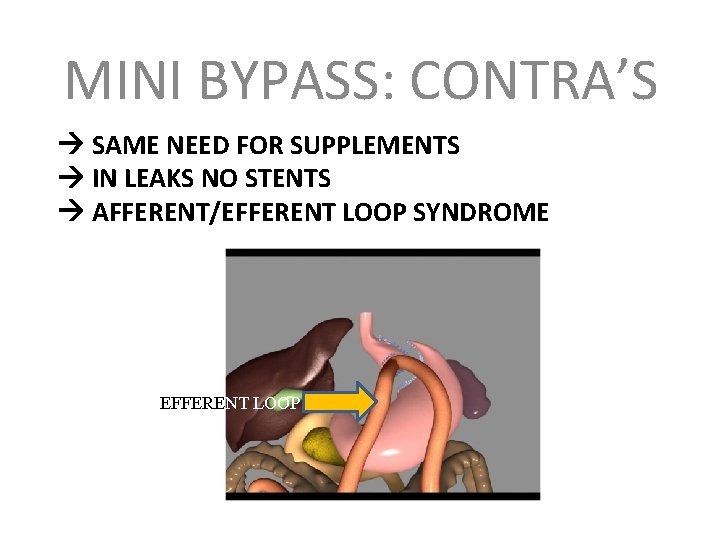
MINI BYPASS: CONTRA’S SAME NEED FOR SUPPLEMENTS IN LEAKS NO STENTS AFFERENT/EFFERENT LOOP SYNDROME EFFERENT LOOP
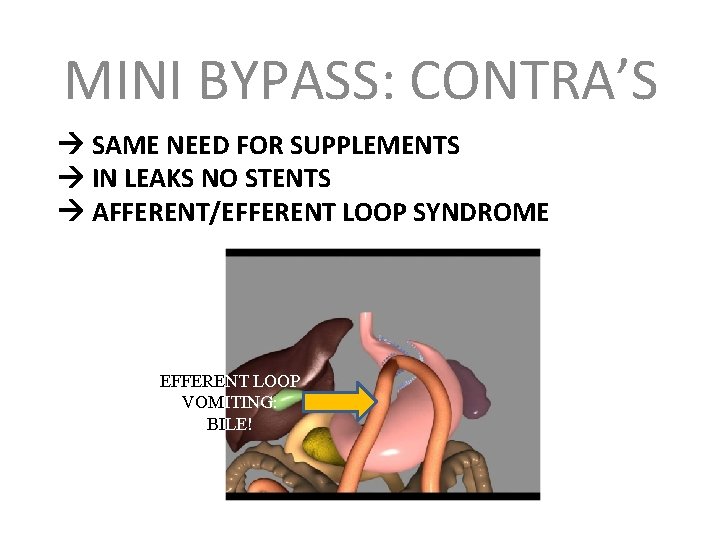
MINI BYPASS: CONTRA’S SAME NEED FOR SUPPLEMENTS IN LEAKS NO STENTS AFFERENT/EFFERENT LOOP SYNDROME EFFERENT LOOP VOMITING: BILE!

MINI BYPASS: CONTRA’S SAME NEED FOR SUPPLEMENTS IN LEAKS NO STENTS AFFERENT/EFFERENT LOOP SYN. LONG TERM? (ULCERS, CANCER)
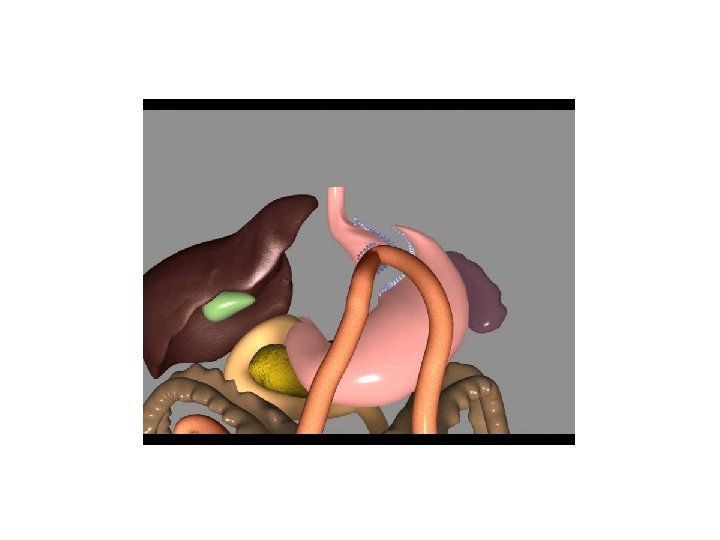


PATIENT CHARACTERISTICS PERIOD : 23/10/2007 31/03/2011 Total 492 patients 372 (75. 6%) available for review 331 WOMEN, 41 MEN Age at surgery: 34 yrs (18 -67) Preop BMI 40. 6 kg/m² (30 -57)

PATIENT CHARACTERISTICS PERIOD : 31/10/2007 31/03/2011 372 primary cases Ancillary procedures: Chole n=21 (5. 6%) “Nissen” n=14 Hiatoplasty n=52 “Nissen” + Hiatoplasty n=72 138 anti-reflux (37. 1%)
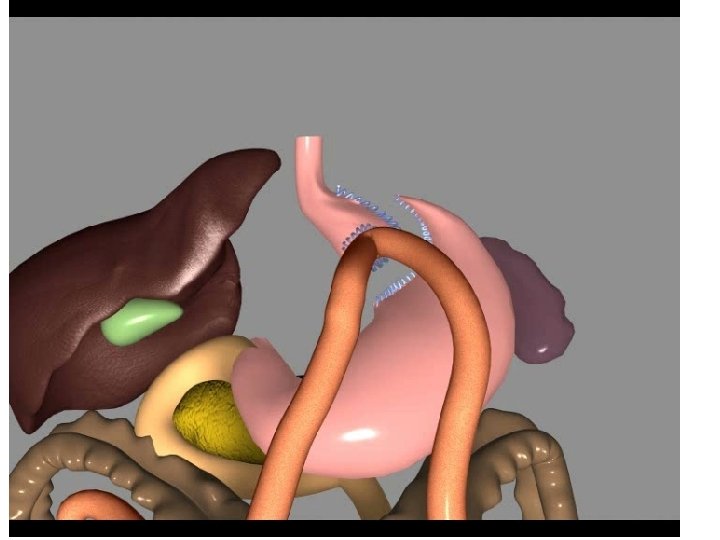
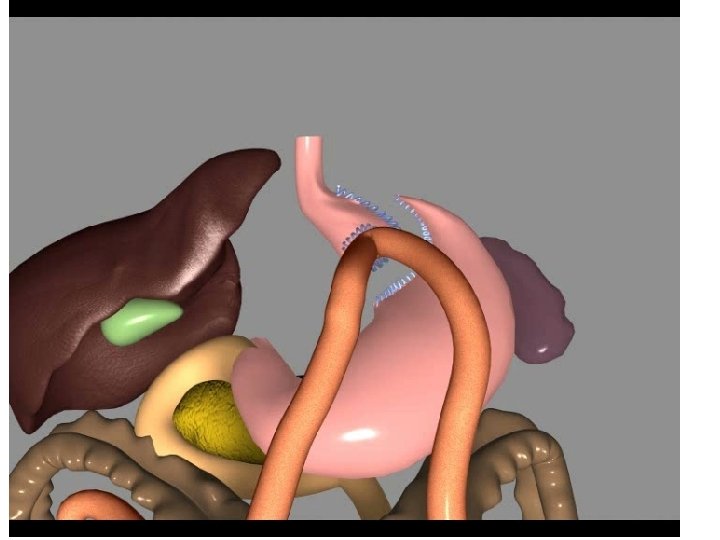

PATIENT CHARACTERISTICS PERIOD : 23/10/2007 31/03/2011 372 primary cases LOS 4. 3 days (2 -62) (median 2. 6)

RESULTS: COMPLICATIONS Total 372 pts LEAK 5 (1. 3%) BLEEDING 8 (2. 1%) INCISION. H. 2 (0. 5%)

PATIENT CHARACTERISTICS Late complications: Internal hernia: n= 6 (1. 6%) Cholecystitis: n=20 (/354) = 5. 6% Recurrent anastomotic ulcer (smokers) n=5 (1. 3%)

RESULTS: COMPLICATIONS PERIOD : 23/10/2007 31/03/2011 Total 372 pts LEAK : n=5 1 male heavy smoker 3 learning curve 1 bezoar blow-out

RESULTS: WEIGHT LOSS PERIOD : 23/10/2007 31/03/2011 Total 372 pts BMI: 26. 6+4. 3(20. 2 -32. 8) kg/m² EWL of 69. 9+8. 5(62 -82)% Follow-up median 32 [24 -42]

RESULTS: COMPLICATIONS PERIOD : 23/10/2007 31/03/2011 Total 234 pts “normal” Acid reflux n=7 5. 6% Bile reflux n=6 138 pts anti-reflux Bile reflux n=3 2. 2% Treatment: 9 ( conversion into RYGB )
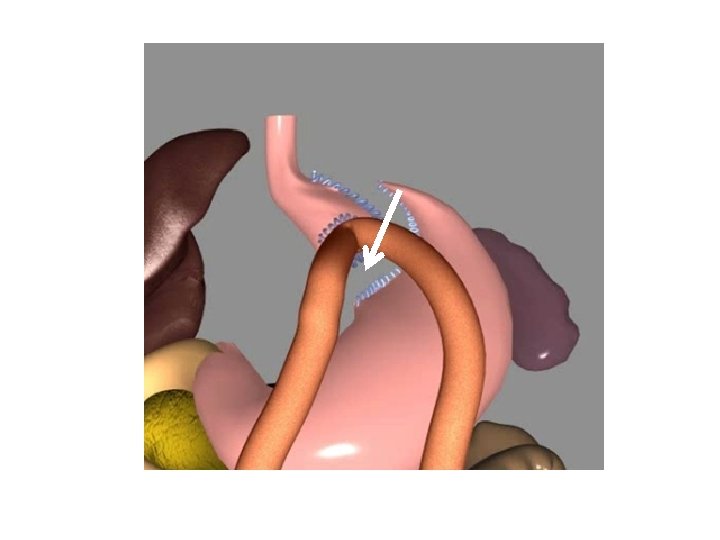
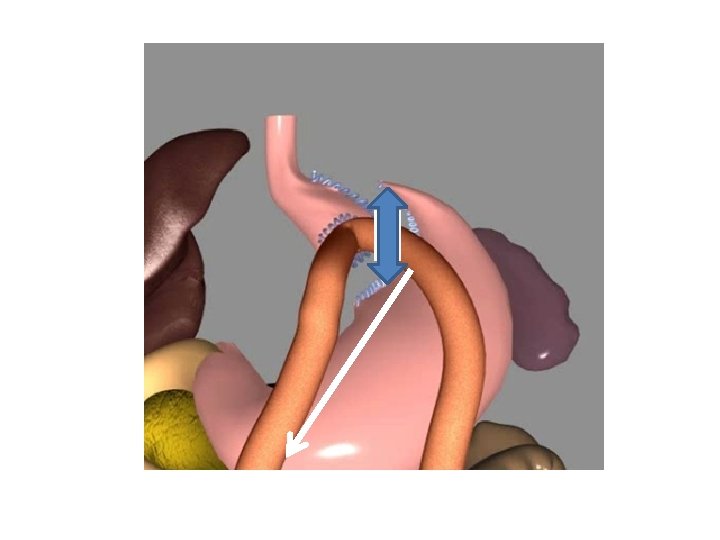
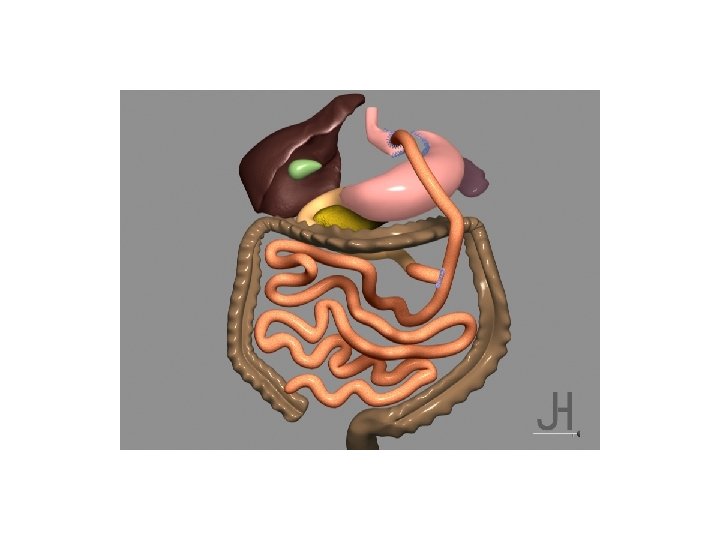

CONCLUSIONS 1/ REFLUX IS AN ISSUE AFTER MGB 2/ CONDITION IS TREATABLE (CONVERSION. . . ) 3/ RYGB CAN BE CONVERTED TO MGB AS WELL
- Slides: 73