Beyond LDL Cholesterol NMR Lipid Fractionation and Treating

Beyond LDL Cholesterol: NMR Lipid Fractionation and Treating Residual Risk Thomas G. Allison, Ph. D, MPH Mayo Clinic Rochester, MN

DISCLOSURE Relevant Financial Relationship(s) None Off Label Usage None

Learning Objectives As a result of attending this presentation, participants will be able to: 1. Address “residual risk” in the secondary prevention of CHD 2. Appropriately order NMR spectroscopy lipid results for intensive lipid management 3. Interpret NMR results to identify higher and lower risk patients with the same LDL

PROVE IT - TIMI 22: Study Design 4, 162 patients with an Acute Coronary Syndrome < 10 days Double-blind ASA + Standard Medical Therapy “Standard Therapy” Pravastatin 40 mg “Intensive Therapy” Atorvastatin 80 mg 2 x 2 Factorial: Gatifloxacin vs. placebo Duration: Mean 2 year follow-up (>925 events) Primary Endpoint: Death, MI, Documented UA requiring hospitalization, revascularization (> 30 days after randomization), or Stroke
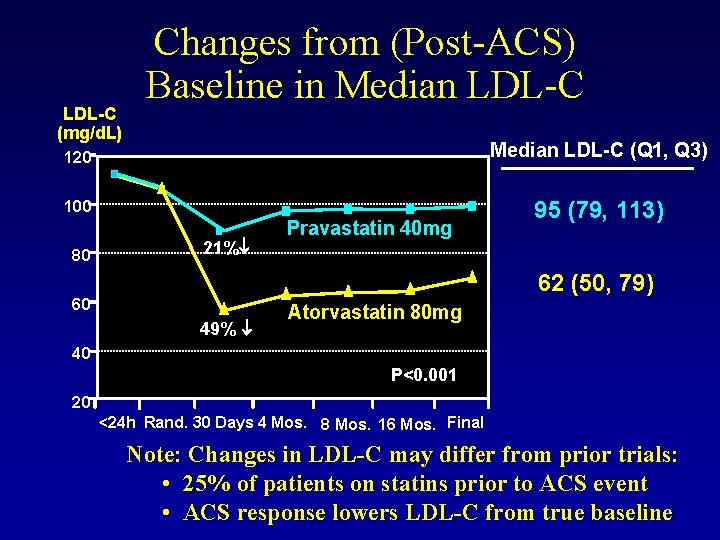
LDL-C (mg/d. L) Changes from (Post-ACS) Baseline in Median LDL-C 120 Median LDL-C (Q 1, Q 3) 100 95 (79, 113) 80 21% Pravastatin 40 mg 62 (50, 79) 60 49% Atorvastatin 80 mg 40 P<0. 001 20 <24 h Rand. 30 Days 4 Mos. 8 Mos. 16 Mos. Final Note: Changes in LDL-C may differ from prior trials: • 25% of patients on statins prior to ACS event • ACS response lowers LDL-C from true baseline
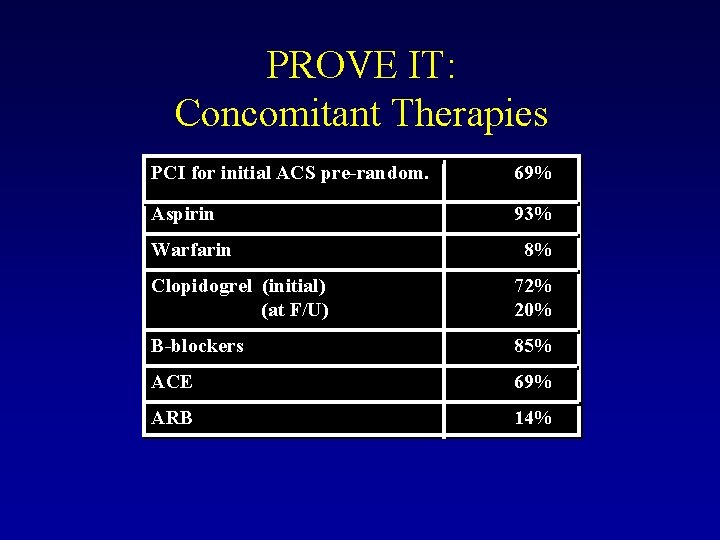
PROVE IT: Concomitant Therapies PCI for initial ACS pre-random. 69% Aspirin 93% Warfarin 8% Clopidogrel (initial) (at F/U) 72% 20% B-blockers 85% ACE 69% ARB 14%
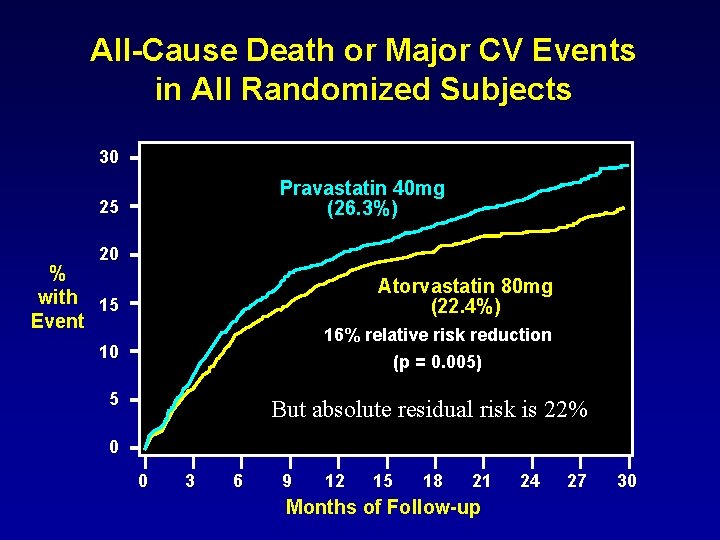
All-Cause Death or Major CV Events in All Randomized Subjects 30 Pravastatin 40 mg (26. 3%) 25 20 % with 15 Event Atorvastatin 80 mg (22. 4%) 16% relative risk reduction (p = 0. 005) 10 5 But absolute residual risk is 22% 0 0 3 6 9 12 15 18 21 Months of Follow-up 24 27 30

Sources of Residual Risk • Not providing appropriate medical therapy? • Inadequate control of non-lipid risk factors? • Not addressing emerging risk factors? – CRP, Lp(a) • Inadequate control of lipids using LDL target only? – Non-HDL – Apo B – Small, dense LDL
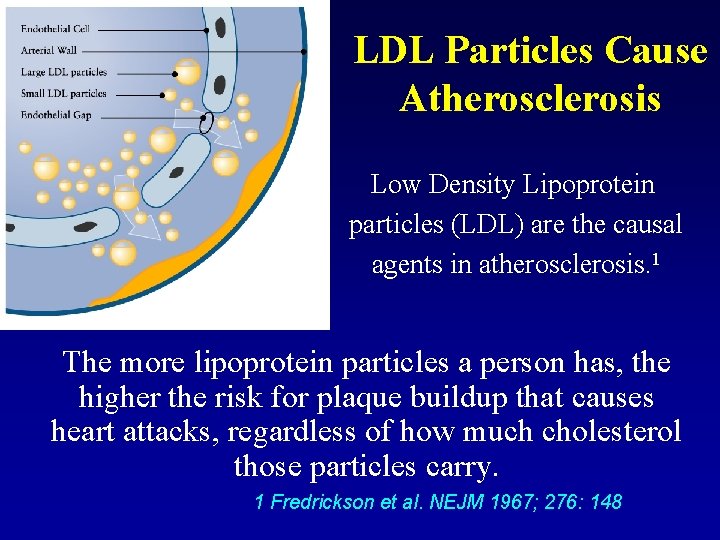
LDL Particles Cause Atherosclerosis Low Density Lipoprotein particles (LDL) are the causal agents in atherosclerosis. 1 The more lipoprotein particles a person has, the higher the risk for plaque buildup that causes heart attacks, regardless of how much cholesterol those particles carry. 1 Fredrickson et al. NEJM 1967; 276: 148

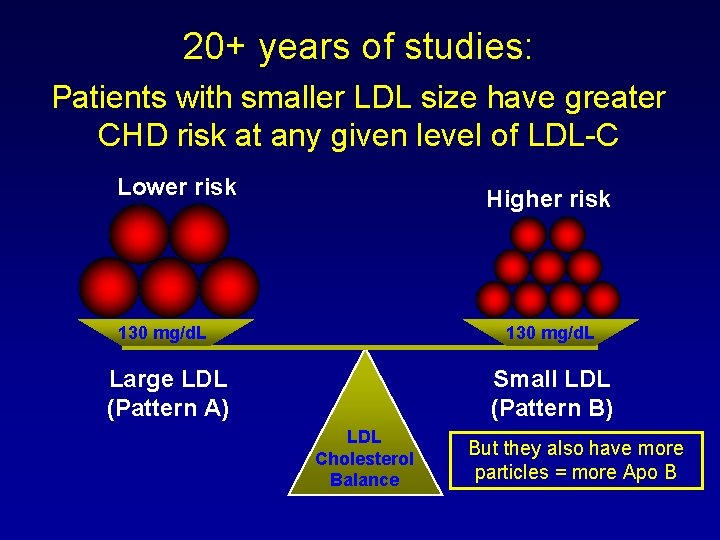
20+ years of studies: Patients with smaller LDL size have greater CHD risk at any given level of LDL-C Lower risk Higher risk 130 mg/d. L Large LDL (Pattern A) Small LDL (Pattern B) LDL Cholesterol Balance But they also have more particles = more Apo B


LDL Particle Number Has Been Repeatedly Shown to be Superior to LDL Cholesterol * Significant and independent in multivariate models adjusted for lipids Study CHD Status CHD Endpoint NMR Particle Number Associations* Cardiovascular Health Study Primary Prevention Arterioscler Thromb Vasc Biol. 2002 Incident MI or Angina Increased Total LDL-P Increased Small LDL-P Women’s Health Study Circulation 2002 Primary Prevention Incident MI, CHD Death, Stroke Increased Total LDL-P Increased Small LDL-P Healthy Women’s Study Am J Cardiol 2002 Primary Prevention EBCT Coronary Calcium Score Increased Total LDL-P Increased Small LDL-P Increased Large VLDL-P

LDL Particle Number Has Been Repeatedly Shown to be Superior to LDL Cholesterol * Significant and independent in multivariate models adjusted for lipids Study CHD Status CHD Endpoint NMR Particle Number Associations* Veterans Affairs HDL Secondary Intervention Trial (VA-HIT) Prevention Circulation 2006 Nonfatal MI or CHD Death Increased Total LDL-P Decreased Total HDL-P Pravastatin Limitation of Secondary Atherosclerosis in Coronary Prevention Arteries (PLAC-I) Am J Cardiol 2002 Angiographic Minimal Lumen Diameter Increased Total LDL-P Increased Small LDL-P Decreased Large HDL-P Framingham Offspring Study Am Heart Assoc 2004 Incident MI, Stroke, Claudication, Angina Increase in Total LDL-P Increase in Small LDL-P Secondary Prevention
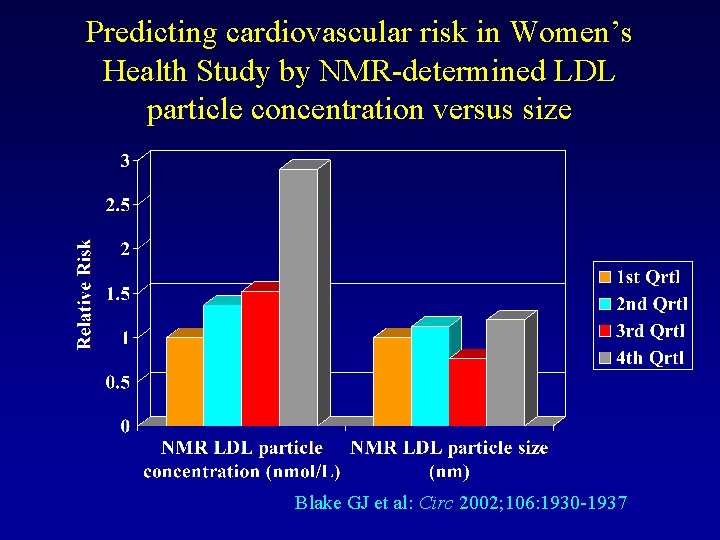
Predicting cardiovascular risk in Women’s Health Study by NMR-determined LDL particle concentration versus size Blake GJ et al: Circ 2002; 106: 1930 -1937

Small, Dense LDL • Modified apo-B has lower affinity for hepatic LDL-receptor – Longer residence time in circulation • • More easily oxidized Easier entry into arterial intima More readily retained in intima Atherogenicity twice as great as large LDL particle
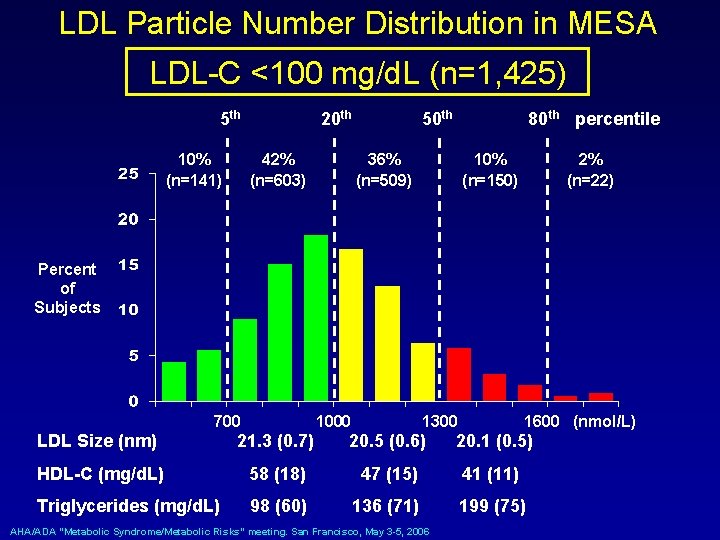
LDL Particle Number Distribution in MESA LDL-C <100 mg/d. L (n=1, 425) 5 th 10% (n=141) 20 th 42% (n=603) 50 th 80 th percentile 36% (n=509) 10% (n=150) 2% (n=22) Percent of Subjects 700 1000 1300 1600 (nmol/L) LDL Size (nm) 21. 3 (0. 7) 20. 5 (0. 6) 20. 1 (0. 5) HDL-C (mg/d. L) 58 (18) 47 (15) 41 (11) Triglycerides (mg/d. L) 98 (60) 136 (71) 199 (75) AHA/ADA “Metabolic Syndrome/Metabolic Risks” meeting. San Francisco, May 3 -5, 2006
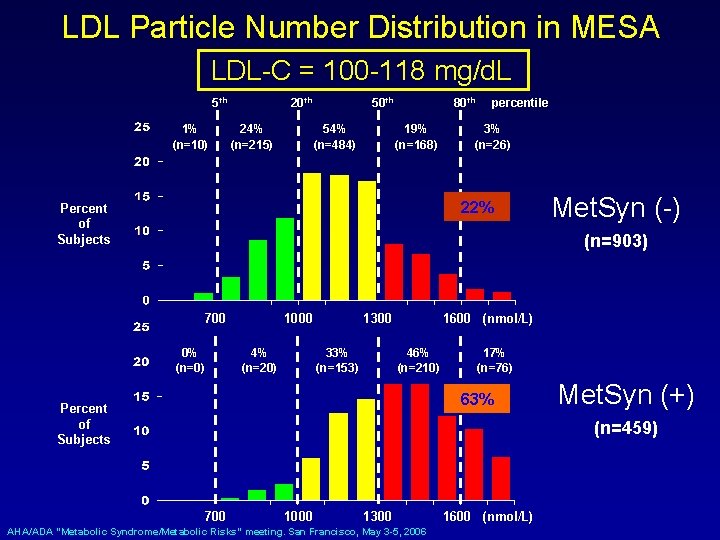
LDL Particle Number Distribution in MESA LDL-C = 100 -118 mg/d. L 5 th 1% (n=10) 20 th 24% (n=215) 50 th 54% (n=484) 80 th 19% (n=168) percentile 3% (n=26) 22% Percent of Subjects Met. Syn (-) (n=903) 700 0% (n=0) 1000 4% (n=20) 1300 33% (n=153) 1600 (nmol/L) 46% (n=210) 17% (n=76) 63% Percent of Subjects Met. Syn (+) (n=459) 700 1000 1300 AHA/ADA “Metabolic Syndrome/Metabolic Risks” meeting. San Francisco, May 3 -5, 2006 1600 (nmol/L)
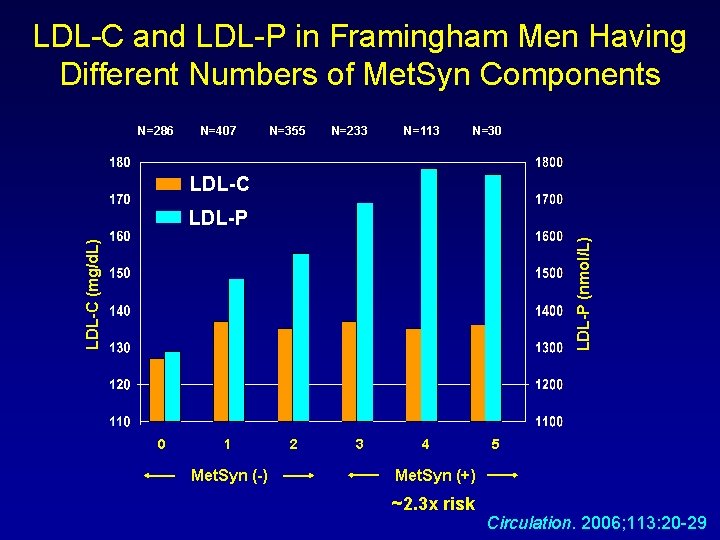
LDL-C and LDL-P in Framingham Men Having Different Numbers of Met. Syn Components N=286 N=407 N=355 N=233 N=113 N=30 LDL-C (mg/d. L) LDL-P (nmol/L) LDL-P 0 1 Met. Syn (-) 2 3 4 5 Met. Syn (+) ~2. 3 x risk Circulation. 2006; 113: 20 -29
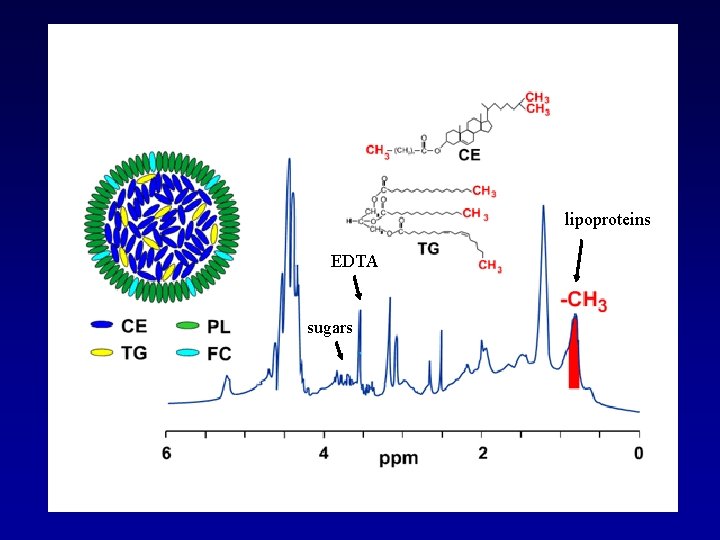
lipoproteins EDTA sugars



Case Study • 62 year old woman presenting with chest pain • S/p prior ischemic stroke • Family history of premature CHD – Mother MI age 52 • Treated hypertension – Hydrochlorothiazide 12. 5 mg – Current BP = 145/73 • No smoking or diabetes • Weight = 78. 6 kg; BMI = 27. 8 kg/m 2



Treated Hyperlipidemia • • Total cholesterol = 158 mg/d. L HDL cholesterol = 50 mg/d. L LDL cholesterol = 83 mg/d. L Triglycerides = 127 mg/d. L Current Rx = Atorvastatin 10 mg/day Lp(a) < 7 mg/d. L • FBG = 89 g/d. L CRP = 0. 9 mg/d. L Homocysteine = 7 µmol/L

Next Step 1. 2. 3. 4. Do nothing else for lipids? Increase Atorvastatin? Add Ezetimibe? Add niacin?

NMR Results • • Total LDL particles = 1300 nmol/L Small LDL particles = 1140 nmol/L Total HDL particles = 39 µmol/L Large HDL particles = 6. 6 µmol/L • Additional Rx – Niacin 500 mg b. i. d. – Amlodipine 2. 5 mg/day

Follow-Up 5 Months • • • Total cholesterol = 158 150 mg/d. L HDL cholesterol = 50 66 mg/d. L LDL cholesterol = 83 64 mg/d. L Triglycerides = 127 102 mg/d. L Total LDL particles = 1300 752 nmol/L Small LDL particles = 1140 425 nmol/L Total HDL particles = 39 43 µmol/L Large HDL particles = 6. 6 11. 1 µmol/L Weight 78. 6 77. 6 kg

Conclusions • Despite intervention and aggressive medical therapy, patients continue to have CHD events • This “residual risk” may still be present in some patients despite LDL cholesterol levels at target • NMR spectroscopy represents one potential strategy for identifying residual risk and guiding therapy

Total cholesterol • Questions • Comments LDL particle concentration LDL cholesterol

Case Study #2 • 63 year old man completing cardiac rehab • S/p recent CABG (LIMA LAD) – Prior PCI LAD and Cx • Treated hypertension – Atenolol 50 mg daily; current BP = 118/61 mm. Hg • Treated hyperlipidemia – Simvastatin 40 mg • Remote past smoking • Weight = 91. 8 kg; BMI = 31. 8 kg/m 2

Treated Hyperlipidemia • • Total cholesterol = 152 mg/d. L HDL cholesterol = 48 mg/d. L LDL cholesterol = 73 mg/d. L Triglycerides = 154 mg/d. L Current Rx = Simvastatin 40 mg/day Lp(a) < 7 mg/d. L FBG = 103 mg/d. L

Next Step 1. 2. 3. 4. Do nothing else for lipids? Increase Simvastatin? Add Ezetimibe? Add niacin?

NMR Results • • Total LDL particles = 1200 nmol/L Small LDL particles = 1008 nmol/L Total HDL particles = 35 µmol/L Large HDL particles = 6. 5 µmol/L • Additional Rx – Ezetimibe 10 mg/day

Follow-Up 10 Weeks • • • Total cholesterol = 152 138 mg/d. L HDL cholesterol = 48 45 mg/d. L LDL cholesterol = 73 65 mg/d. L Triglycerides = 154 140 mg/d. L Total LDL particles = 1200 1093 nmol/L Small LDL particles = 1008 943 nmol/L Total HDL particles = 36 35 µmol/L Large HDL particles = 6. 6 6. 5 µmol/L Weight 91. 8 90. 5 kg

Conclusion • Probably the wrong drug was added – A few more large LDL were cleared – Small, dense LDL minimally changed – No improvement in HDL • Now add niacin 500 mg b. i. d.
Spectrum 1 Spectrum 2

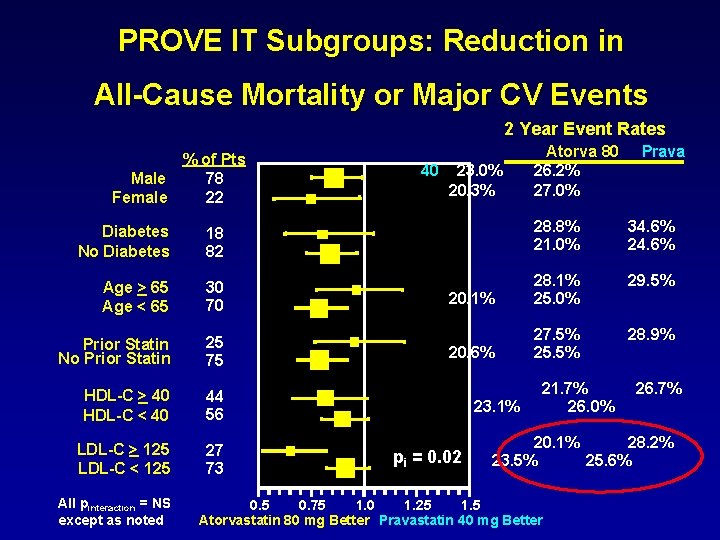
PROVE IT Subgroups: Reduction in All-Cause Mortality or Major CV Events 2 Year Event Rates % of Pts 78 Male Female 22 40 23. 0% 20. 3% Atorva 80 26. 2% 27. 0% Prava Diabetes No Diabetes 18 82 28. 8% 21. 0% 34. 6% 24. 6% Age > 65 Age < 65 30 70 29. 5% 20. 1% 28. 1% 25. 0% Prior Statin No Prior Statin 25 75 28. 9% 20. 6% 27. 5% 25. 5% HDL-C > 40 HDL-C < 40 44 56 LDL-C > 125 LDL-C < 125 27 73 All pinteraction = NS except as noted 23. 1% pi = 0. 02 21. 7% 26. 0% 26. 7% 20. 1% 28. 2% 23. 5% 25. 6% 0. 5 0. 75 1. 0 1. 25 1. 5 Atorvastatin 80 mg Better Pravastatin 40 mg Better
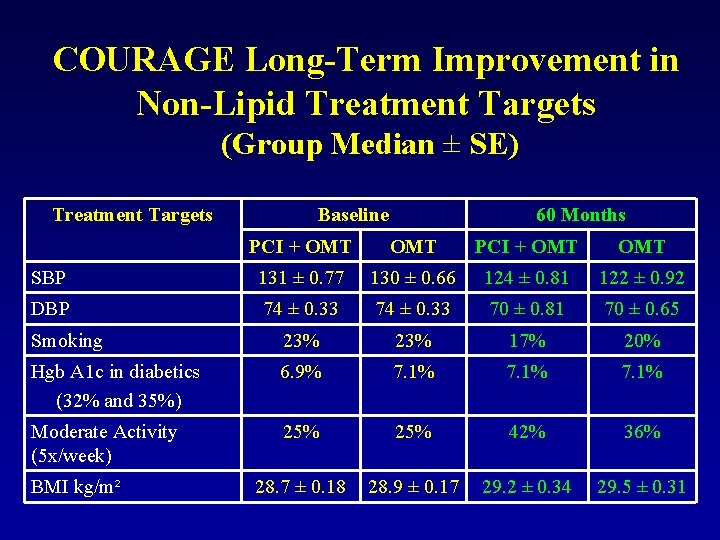
COURAGE Long-Term Improvement in Non-Lipid Treatment Targets (Group Median ± SE) Treatment Targets Baseline 60 Months PCI + OMT OMT SBP 131 ± 0. 77 130 ± 0. 66 124 ± 0. 81 122 ± 0. 92 DBP 74 ± 0. 33 70 ± 0. 81 70 ± 0. 65 Smoking 23% 17% 20% Hgb A 1 c in diabetics (32% and 35%) 6. 9% 7. 1% Moderate Activity (5 x/week) 25% 42% 36% 28. 7 ± 0. 18 28. 9 ± 0. 17 29. 2 ± 0. 34 29. 5 ± 0. 31 BMI kg/m²
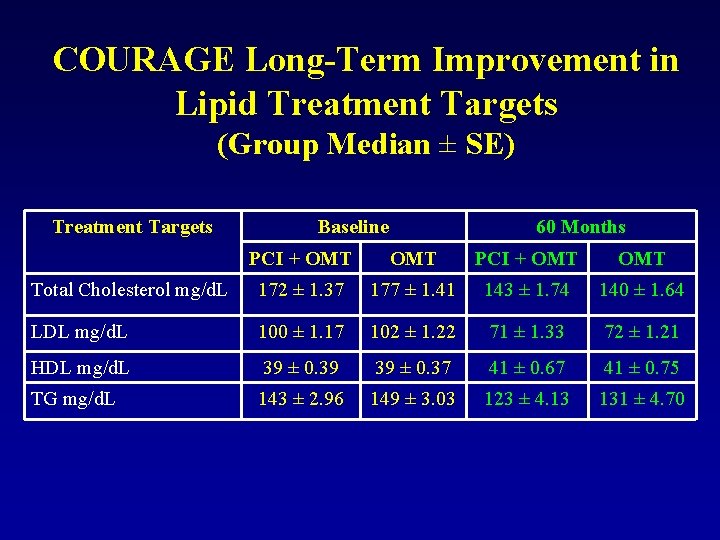
COURAGE Long-Term Improvement in Lipid Treatment Targets (Group Median ± SE) Treatment Targets Baseline 60 Months PCI + OMT OMT Total Cholesterol mg/d. L 172 ± 1. 37 177 ± 1. 41 143 ± 1. 74 140 ± 1. 64 LDL mg/d. L 100 ± 1. 17 102 ± 1. 22 71 ± 1. 33 72 ± 1. 21 HDL mg/d. L 39 ± 0. 39 39 ± 0. 37 41 ± 0. 67 41 ± 0. 75 TG mg/d. L 143 ± 2. 96 149 ± 3. 03 123 ± 4. 13 131 ± 4. 70
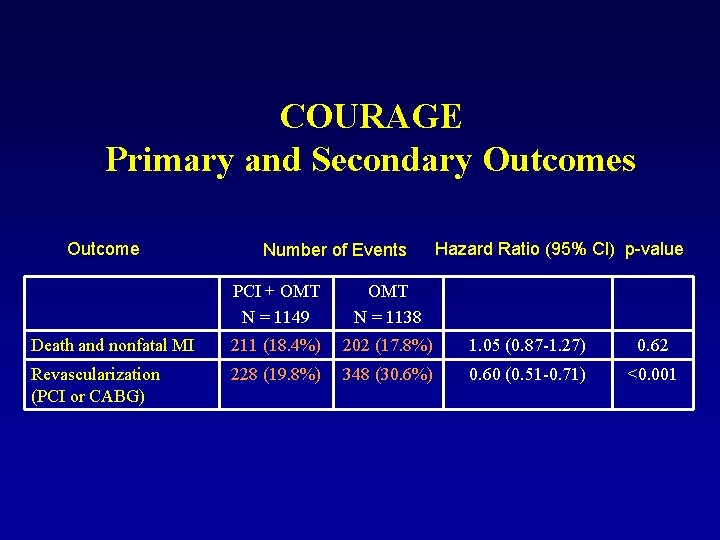
COURAGE Primary and Secondary Outcomes Outcome Number of Events Hazard Ratio (95% Cl) p-value PCI + OMT N = 1149 OMT N = 1138 Death and nonfatal MI 211 (18. 4%) 202 (17. 8%) 1. 05 (0. 87 -1. 27) 0. 62 Revascularization (PCI or CABG) 228 (19. 8%) 348 (30. 6%) 0. 60 (0. 51 -0. 71) <0. 001


- Slides: 45