Beyond Developmental Screening Ensuring FollowUp Services for Children

Beyond Developmental Screening: Ensuring Follow-Up Services for Children Identified At-Risk March 23 rd, 2017
We Want To Hear From You! Type questions into the Questions Pane at any time during this presentation
Patient-Centered Primary Care Institute Online Modules Webinars Website Learning Collaboratives Trainings TA Network

PCPCH Model of Care Oregon’s PCPCH Model is defined by six core attributes, each with specific standards and measures • Access to Care “Health care team, be there when we need you” • Accountability “Take responsibility for making sure we receive the best possible health care” • Comprehensive Whole Person Care “Provide or help us get the health care, information and services we need” • Continuity “Be our partner over time in caring for us” • Coordination and Integration “Help us navigate the health care system to get the care we need in a safe and timely way” • Person and Family Centered Care “Recognize that we are the most important part of the care team - and that we are ultimately responsible for our overall health and wellness” Learn more: http: //primarycarehome. oregon. gov

Presenters Colleen Reuland, MS Director, Oregon Pediatric Improvement Partnership (OPIP) Instructor, Department of Pediatrics Oregon Health & Science University. Suzanne Dinsmore, MD Pediatrician Childhood Health Associates of Salem

Learning Objectives • Provide an overview of community-level asset mapping conducted to identify follow-up resources and supports for children identified “at-risk” on developmental screening tools. • Describe applied methods and processes patient-centered primary care homes can use to better follow-up for children identified at-risk that identifies services that are the best match for the child and family. • Describe applied care coordination methods used to enhance the number of children identified at-risk for delays to receive services Note: About the Varied Audience for this Webinar and a Sweet Spot We Are Trying to Reach Given We have: – – – Primary Care Providers Early Learning Hubs Public Health EI CCOs Other early learning systems

Agenda • Background & context o Recommendations related to developmental screening in primary care o Momentum related to developmental screening on Oregon • Opportunity to focus on follow-up to developmental screening: Spotlight of an effort in three counties o Data gathered and primary opportunities identified o Community-level asset mapping conducted to identify follow-up resources and supports for children/families. o Pilot tools and strategies developed and being implemented by health care and early learning • Sharing from the front-line – A front-line provider’s perspective from this project and lessons learned for other PCPCH practices

Developmental Screening Recommendations for Primary Care Providers Bright Futures Recommendations for Primary Care Providers in the First Three Years of Life: o Standardized developmental surveillance at every visit across the five domains of a child’s development • Use of standardized developmental screening tool for children for whom concerns are identified o Implementation of standardized developmental screening tools three times in the first three years of life – 9 month visit – 18 month visit – 30 month visit (if practice not doing the 30 month visit, 24 month visit)

Momentum Around Developmental Screening In Oregon • Coordinated Care Organization Incentive Metric – Developmental Screening in First Three Years of Life • Patient Centered Primary Care Homes (PCPCH) Standards – Includes developmental screening – In 2017 Standards is a component of the must pass standards • Early Learning Hub Metrics – Includes CCO Developmental Screening Incentive Metric

Opportunity to NOW Focus on Follow-Up to Developmental Screening that is the Best Match for the Child & Family • Goals of screening – Identify children at-risk for developmental, social/or behavioral delays – For those children identified, provide 1) developmental promotion, 2) refer to services that can further evaluate and address delays • Many of these services live outside of traditional health care Children Identified “At-Risk” on Developmental Screening Tools This report is focused on children identified “at-risk” that should receive follow-up services. These are children that are identified “at-risk” for developmental, behavioral or social delays on standardized developmental screening tools. In the communities of focus for this work, a majority of providers are using the Ages and Stages Questionnaire (ASQ)3. Therefore the children of focus are those identified “at-risk” for delays based on the ASQ domain level findings.

From Developmental Screening To Services in OREGON: Opportunity to Connect the Fantastic Individual Silos Coordinated Care Organizations (Including Primary Care) 11 Early Learning Early Intervention

From Developmental Screening To Services in Oregon: Opportunity to Connect the Fantastic Individual Silos Early Learning Coordinated Care Organizations Goals Related to: 1) Well-Child Care 2) Developmental Screening 3) Coordination of Services Early Intervention Goals related to providing services to young children to achieve educational attainment goals School Readiness 12 Goals Related to: 1) Ensuring children are kindergarten ready 2) Family Resource Management- Family have info and support needed 3) Coordination of services

OPIP Projects Focus on Community- and Population Based Projects Focused on Enhancing Follow-Up Key Components of the Projects – Stakeholder Engagement & Community Asset Mapping 1. Engaging stakeholders in the community 2. Examining data related to where children identified at-risk “fall out” of the pathway to receiving services 3. Based on this stakeholder engagement and data, development of current and potential pathways from screening to services Ø Includes WHICH services Ø WHO to refer Ø HOW to refer – Develop and pilot new methods to improve follow-up, communication and coordination. Three Priority Areas of Focus: • Primary Care Practices – Enhanced Medical Decision Tree • Early Intervention – Methods to enhance coordination and communication • Priority early learning services identified by community: Home visiting, parenting supports, mental health – Methods to refer to these services, enhanced coordination 13

Stakeholder Engagement in Marion, Polk, and Yamhill Counties to Inform Community Asset Mapping CCOs (WVCH, YCCO) • Medical Director • Metrics Staff • Practice Support Staff • Mental Health Director • Staff that oversee services for children • Liaison to Early Learning Hubs • OHA Innovator Agent 14 Primary Care EI & Education • Practices that see large number of children and are doing developmental screening • EI/ECSE Program Coordinator • Practice staff engaged included: ü Physician ü Care Coordinator ü Referral Coordinator ü Practice Manager • School District Representative • EI Referral Intake Coordinator Early Learning Hub (Yamhill Early Learning Hub, Marion and Polk Early Learning Hub) • Director or Executive Director • Community Engagement Staff • Staff involved in efforts around developmental screening Home Visiting and Head Start/Early Head Start • Centralized home visiting referral programs • Public Health/ Ca. Coon/ Babies. First • Healthy Families • Other community services that provide home visiting • Early Head Start and Head Start Child Care and Parenting Supports • Childcare Resource and Referral Center • Childcare Centers conducting screening • Oregon Parenting Education Collaborative entities

Stakeholder Engagement: Current Systems and Processes Related to Follow-Up to Developmental Screening 1. Individual interviews and engagement: – Those screening, what is your follow-up; Those who could provide follow-up, what do you provide and how to people refer to you – Recruited three parent advisors whose children went through systems 2. Periodic group-level stakeholder meetings to provide updates and obtain community-level input and guidance • Early Learning Hubs (Yamhill Early Learning Hub & Marion and Polk Early Learning Hub) were critical partners – Leveraged shared table and relationships they have created within Early Learning System • Engaged new stakeholders with the Early Learning Hub groups – Leveraged Early Learning Hub parent advisory groups get feedback from parents 15
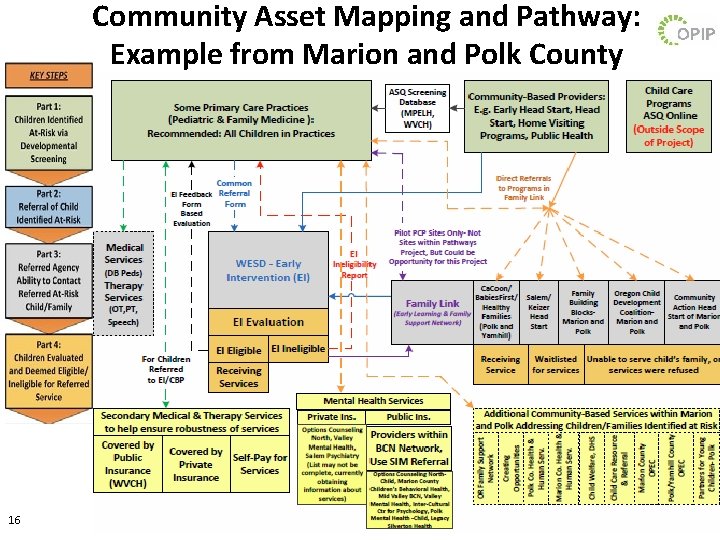
Community Asset Mapping and Pathway: Example from Marion and Polk County 16

Template for Community Asset Mapping Your Community Barebones Template Located Here: http: //oregonpip. org/projects/OPIP%20 General%20 Referral%20 and%20 Triage%20 Map. pdf • Step 1: Identify the specific programs that provide the specific services noted in the map. • Step 2: Identify the specific connection and feedback loops between the different entities. o Using the arrows within the Legend, create connections among the providers you have listed above and clarify if there are existing referral forms, methods, and communication feedback loops, and for whom – How are children referred to the other boxes? Does this happen in a standardized way? Which children get referred? – Is there communication back to the referring entity? Is this communication only for children that access the service? 17

Examination and Use of Data About Developmental Screening and Follow-Up for Children 0 -3 to Understand Current Processes and Needs • CCO level data about developmental screening – Total number of children screened as defined by 96110 claims – Screening rates by practices to which children 0 -3 are assigned – Examining data for disparities by race ethnicity • Pilot Practice-level data – Of developmental screens conducted, how many identify a child atrisk for delays – Of developmental screens where child identified at-risk for delays, follow-up steps • Early Intervention data – Referrals – Evaluation Results – Examining data for disparities by race ethnicity 18
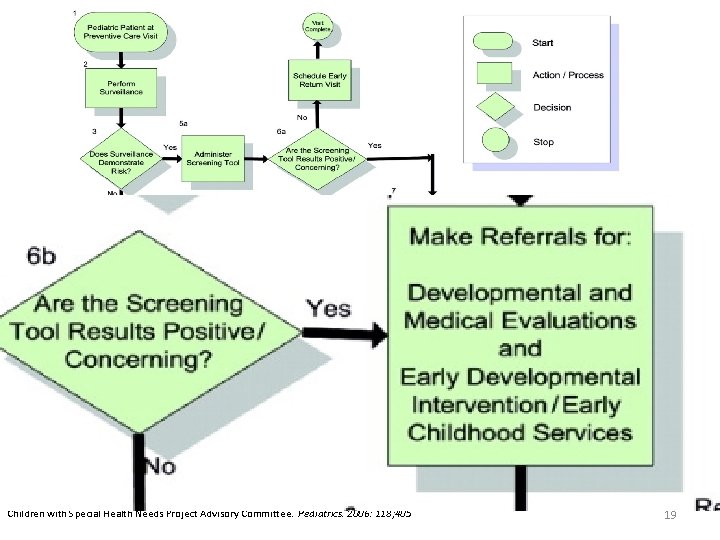
Identifying Infants and Young Children with Developmental Disorders in the Medical Home: An Algorithm for Developmental Surveillance and Screening. Council on Children with Disabilities, Section on Developmental Behavioral Pediatrics, Bright Futures Steering Committee and Medical Home Initiatives for Children with Special Health Needs Project Advisory Committee. Pediatrics. 2006: 118; 405 19
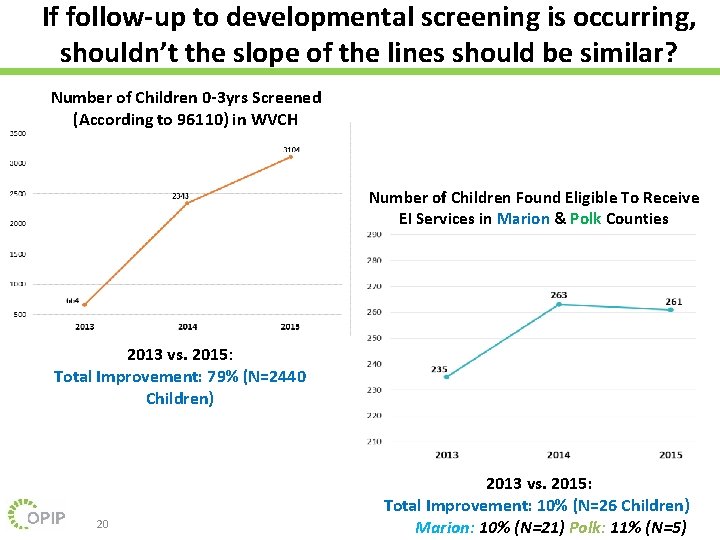
If follow-up to developmental screening is occurring, shouldn’t the slope of the lines should be similar? Number of Children 0 -3 yrs Screened (According to 96110) in WVCH Number of Children Found Eligible To Receive EI Services in Marion & Polk Counties 2013 vs. 2015: Total Improvement: 79% (N=2440 Children) 20 2013 vs. 2015: Total Improvement: 10% (N=26 Children) Marion: 10% (N=21) Polk: 11% (N=5)

For Those Children Identified “At-Risk” and Referred to Early Intervention Services, Improvement Opportunities Exist • Within pilot primary care practices, a majority of children identified “at-risk” had no documented follow-up – 60 -70% of those identified at risk were not referred to Early Intervention (Bright Futures Pathway) • Of children identified as “at-risk” that were referred to Early Intervention(915): – 562 (61%) were able to be evaluated. • Reasons for the 39% of referrals not being evaluated: Parental delay (18. 6%), an inability to contact the family (16. 8%), and the family declining the evaluation (2. 4%). – Of the children able to be evaluated (562), 347 (62%) were found to be eligible for services, meaning 38% were ineligible for services. 21

Qualitative Findings Related to Follow-Up to Developmental Screening for Young Children • Follow-up to screening in primary care – Confusion and lack of awareness within primary care about difference between recommendations for when to refer to EI vs EI Eligibility • Perception that many children referred will not be eligible impacts if and when they refer – Parent push back on referrals, cultural variations – Need for referral criteria that take into account child and family factors, particularly for those children for whom the delay may be because of lack of exposure to the developmental tasks asked about in the ASQ – Lack of awareness of resources within Early Learning and/or WHEN to refer to them • Need for parent supports – Developmental promotion that could in occur in the home – Education about referrals when provided – Parent support in navigation 22
23

Three Priorities Areas Identified for WHERE to Focus Improvement Pilots 1. For primary care practices conducting developmental screening, enhance follow-up for children identified – Part 1: Develop a follow-up medical decision tree that is based on ASQ and child and family factors and goes beyond developmental evaluation and EI – Part 2: Develop Parent supports in navigating referral process 2. For Early Intervention, enhance referral pathways, coordination and communication with the entity that referred the child; follow-up steps for EI ineligible 3. Within early learning, pilots of referrals from primary care to home visiting programs, parenting classes, and other supports 24

Part 1: Primary Care Providers Need a Follow-Up Medical Decision Tree To Identify Best Match for the Child/Family and is Anchored to Services in the Community Based on data and community engagement, six priority referrals are included in the medical decision tree: 1. Medical and Therapy Services (developmental evaluation and therapy services) 2. Early Intervention (EI) 3. Ca. Coon/Babies First 4. Centralized Home Visiting Referral (Includes Early Head Start and Head Start) 5. Parenting Classes 6. Mental Health 25
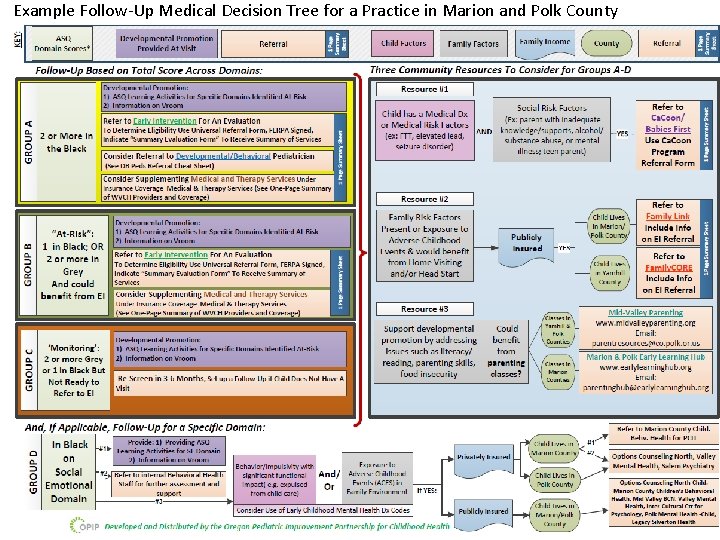
Example Follow-Up Medical Decision Tree for a Practice in Marion and Polk County 26
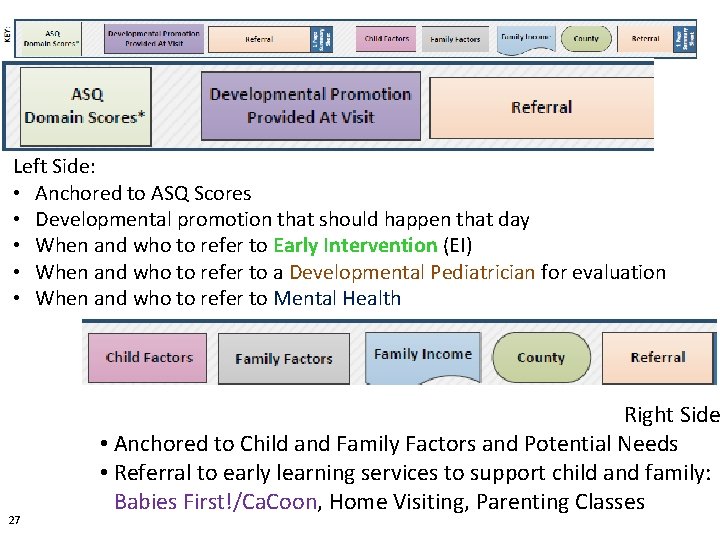
Left Side: • Anchored to ASQ Scores • Developmental promotion that should happen that day • When and who to refer to Early Intervention (EI) • When and who to refer to a Developmental Pediatrician for evaluation • When and who to refer to Mental Health 27 Right Side • Anchored to Child and Family Factors and Potential Needs • Referral to early learning services to support child and family: Babies First!/Ca. Coon, Home Visiting, Parenting Classes

Developmental Promotion: Options to Provide to All Children Identified at Risk Vroom! ASQ Learning Activities for the specific domains

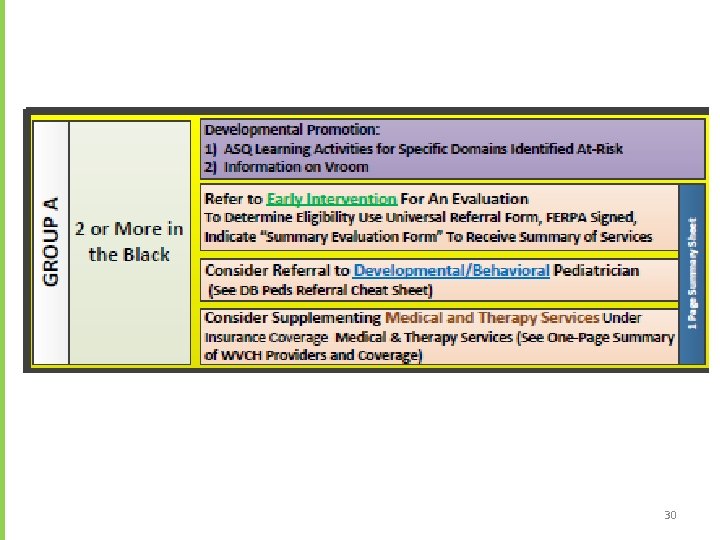
Referral Pathways by TOTAL Score Across Five Domains

30

Key to Referral to Early Intervention

Pilot of EI Communication When Unable to Evaluate: Goal is to Reduce the 2 in 5 Children Referred by Not Evaluated Feedback to Referring Provider • When they sent the “closure” letter • If they referred to Family. Link Completed Example: 32

Referral to Developmental Behavioral Pediatrician The ASQ domains which put the child “at-risk” matter in terms of whether you should refer to Developmental Behavioral Pediatrician – After consultation with experts in the field, the children most likely to be delayed in getting a medical evaluation and/or will not receive robust enough services from EI to address their needs: 1. Intellectual disability 2. Autism – Flags for these under-identified children are • Delays in communication (always one of the factors) And • Delays in problem solving or social emotional –

Consider Referral to Developmental Behavioral Pediatrician • Kid “In the BLACK” in the Communication domain AND either the Personal-Social domain or Problem Solving Domain • Or if the child is in the Black on 2 or more other domains and has any of the following presenting concerns: ü Kids with overall DD (or intellectual disability) or ASD who do not have identified cause, (may be seen initially by genetics instead) ü Kids who are not progressing in services as expected or recent increase in symptoms ü Kids who have challenging behaviors with inadequate response to behavioral interventions or medication. ü Kids with secondary medical issues that are not responding to usual treatments (including feeding and nutrition) ü Kids with rare/unusual genetic/chromosomal disorders (after initial visit with medical genetics) ü Kids with other chronic conditions that require inter-disciplinary team management (eg, child with CP, TBI etc) ü Kids who may be experiencing traumatic events

Follow-Up Based on EI Evaluation If Eligible for Early Intervention – Review Pilot Form of EI Services Receiving (Newly developed as part of this pilot) – Consider Supplementing for Services Under Insurance Coverage (CCO Summaries Newly Developed as part of the pilot)

Pilot EI Communication Form to Inform Possible Secondary Referral Being Developed (Likely in Place by March ‘ 17) 36

WVCH Summary of Services Related to Follow-Up 37

38
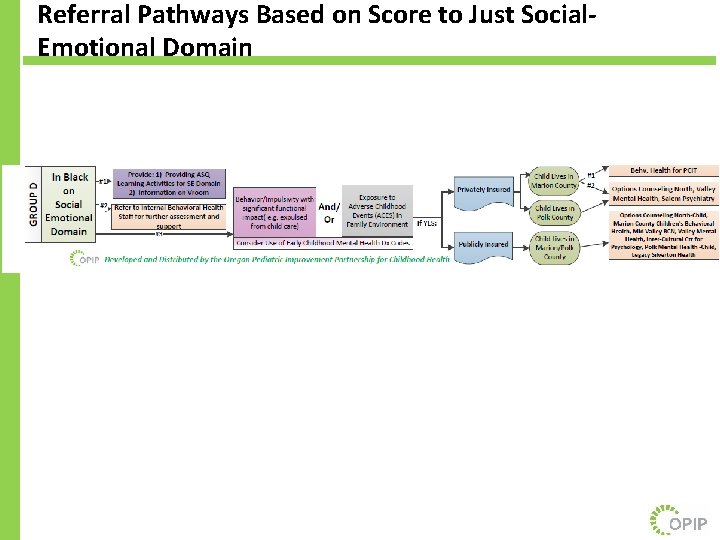
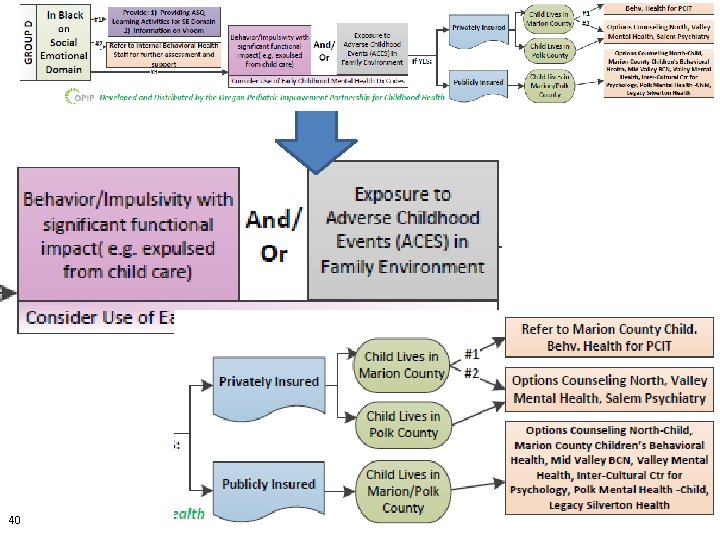
Referral Pathways Based on Score to Just Social. Emotional Domain
40
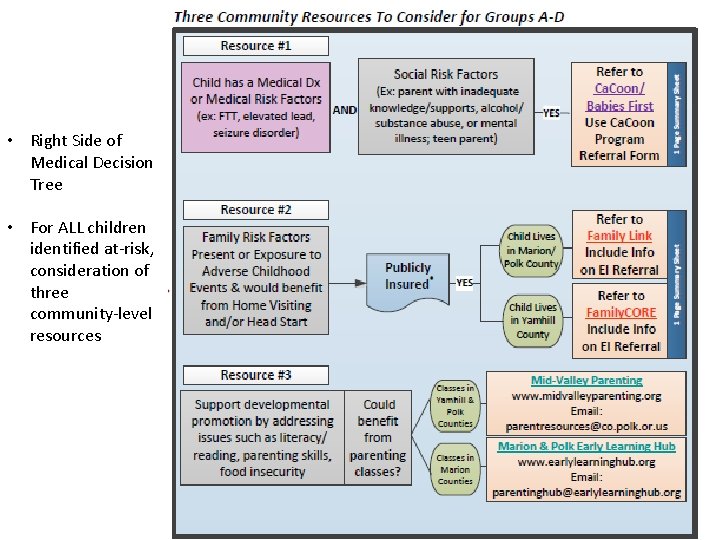
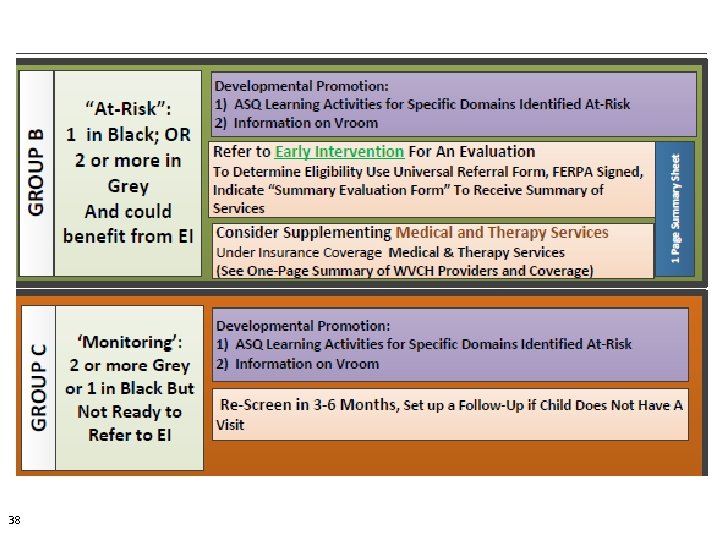
• Right Side of Medical Decision Tree • For ALL children identified at-risk, consideration of three community-level resources 41

Child and Family Factors Listed on the Back of the Decision Tree: Tied to Eligibility and Priority Criterion Within This Community • • • • 42 o o Lack of Prenatal Care o Support with Breastfeeding o Support with Infant Care o Drug Exposed Infant/Pregnancy Support with Attachment/Bonding o o Has Disability o Born Premature o Home Environment Concerns o Development Concerns o Social/Emotional Concerns o Behavior Concerns o Feeding Concerns o Health Concerns o Weight Concerns o Feels Depressed or Overwhelmed Isolation/Lack of Support with Parenting Has Disability Teen/Young Parent First Time Parent Tobacco Use Domestic Violence (present or history of) Alcohol/Drug Use Lack of Food/ Clothing/Housing Incarceration/Probation Low Income Migrant/Seasonal Worker Unemployed Homeless Receives TANF/SSI/SNAP

Follow-Up Medical Decision Tree to Determine “Best Match” for Services for the Child/Family • Disclaimer: o This is Version 1. 0 o Goal is to learn from this pilot experience and understand what works and doesn’t work (Funding ends June ‘ 17) o We are also tracking data to assess for capacity AND refinements to the process Ø We can only provide information about need for services if we have concrete data on children identified that SHOULD be referred o Email me if you are interested in receiving a version knowing: Ø We are learning from this pilot Ø They need to be customized for each community Ø We are exploring funding to support this customization, training and implementation support 43

Part 2: Care Coordination Supports to the Family Informed by parent advisors, developed tools and processes to better support families 1. Information Sheet (Developed through this project), Providers ended up using this to ensure shared decision making on referrals 2. Phone Follow-up (Developed through this project) 44

Pilot Education Sheet for Parents To Explain Referrals

Phone Follow-Up: Developed it because 39% of referred children not able to be evaluated • 2 in 5 children referred to EI don’t get evaluated • Some studies show that families make a decision on a referral in the first 48 hours • Researchers in Illinois found that phone follow-up (not necessarily contact) within two days of the referral significant increased follow through • Phone calls can also identify barriers to obtaining the evaluation

Pilot: Phone Follow-Up Script for Referred Children 47

Hearing from the Front Line: Experience of a Primary Care Practice in These Improvement Efforts Suzanne Dinsmore, MD Child Health Associates of Salem (CHAo. S)

Childhood Health Associates of Salem • • • 10 MD, 4 PA, 2 NP, 1 LCSW and 2 Psy. D’s 2 RN Care Coordinators and 2 Referral Coordinator 16, 000 kids All. Scripts Health. Matics 60% Medicaid, 35% commercial, 6% uninsured

Focus of Our Improvement Efforts Within Childhood Health Associates of Salem 1. Examination of our practice-level data and the need for improvement, provision of our data to inform the community-level conversations 2. Implementing OPIP’s Pilot Medical Decision Referral Algorithm • Incorporates ASQ, child and family risk factors • Goes beyond just developmental evaluation and EI, includes community based resources • Pilot with Family. Link (Centralized home visiting referral) 3. Refined Process for EI Referrals • Follow-up phone script and process • Process for using communication back from EI ü Child not able to be evaluated ü Child not eligible ü Child eligible, but on what 4. Parent Support – Using the Education Sheet • Value of it to facilitate shared decision making with families • Value of it from information management

An Applied Example from One of Our Primary Care Pilot Sites Of the children who received a developmental screen, 28% identified at-risk for delays for which developmental promotion should occur Number of children who were identified at-risk and SHOULD HAVE BEEN TO NUMBER REFERRED TO EI: REFERRED TO EI N=401 based on their developmental screen : 81% NOT REFERRED N= 76 N= 401 N= 1431 Number of ALL Children in Clinic (Publicly and Privately Insured) WHO RECEIVED A DEVELOPMENTAL SCREEN IN ONE YEAR: N=1431 Data Source: Data provided by Childhood Health Associates of Salem, Aug. & Jan 2017 51

Parent Education Sheet: • Useful Tool to Use in Shared Decision Making with the Family • Helps guide primary care provider on the resources available • Provides contact information and online resources for parents to learn more
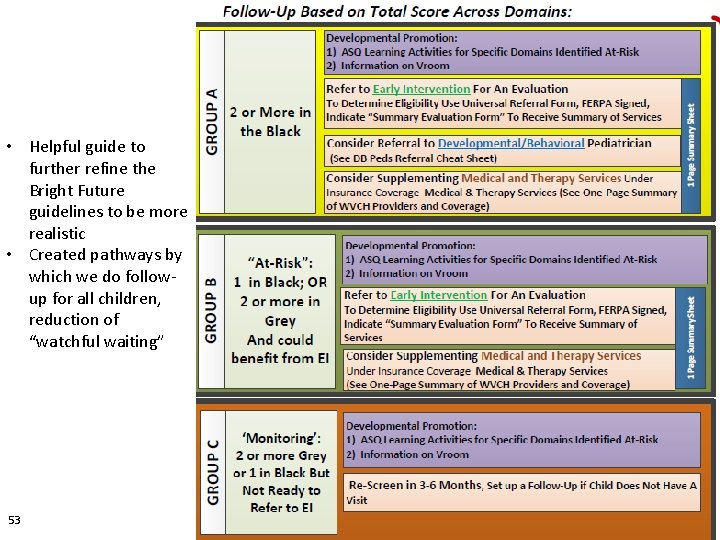
• Helpful guide to further refine the Bright Future guidelines to be more realistic • Created pathways by which we do followup for all children, reduction of “watchful waiting” 53
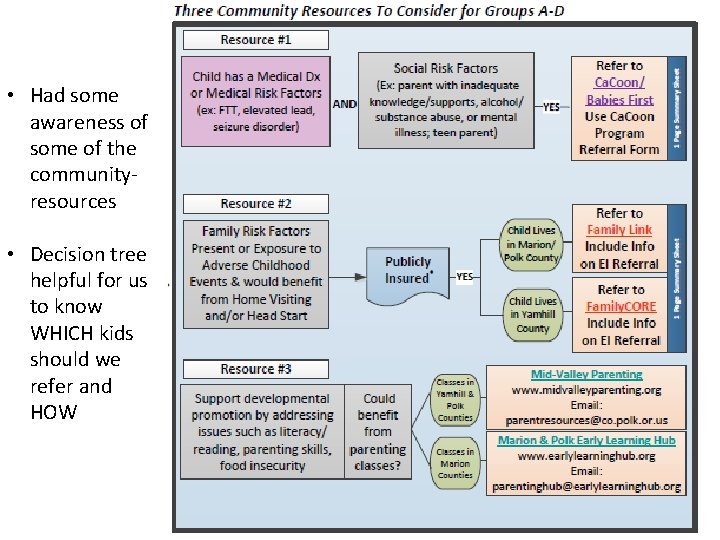
• Had some awareness of some of the communityresources • Decision tree helpful for us to know WHICH kids should we refer and HOW 54

Efforts are Engaging Primary Care in the Early Learning Efforts in Our Community 1) Enhanced awareness of the Early Learning System & Early Learning Hub • Obtained specific information about resources we had not known about, specific pathways for referral and follow-up – Parenting Education Collaborative – VROOM – ASQ Learning Activities – Centralized Home Visiting – Family Link Pilot – PCIT for Privately Insured Kids • Participated on community-level meetings focused on this population – Engagement of the CCO is different than engagement with the PCP given competing demands 2) For Early Learning Hubs: Leverage primary care given we see young children 11 times in the first three years of life for well-child care alone • Unique opportunity to partner with parents and connect • Unique opportunity to gather data to inform discussions about capacity Ø Based on the numbers through this project, already clear that there is not capacity within the systems for all the children we identify Ø Disparity in services available for working poor

What Questions Do You Have? Type questions into the Questions Pane at any time during this presentation

Spotlights Presented Today Are from Past OPIP Projects: Thank you to the Funders of This Work http: //oregon-pip. org/focus/Follow. Up. DS. html 1. Oregon Health Authority contracted with OPIP to provide consulting and technical assistance to Yamhill Early Learning Hub and Yamhill CCO on a community pilot focused on ensuring children identified at-risk for developmental, behavioral, and social delays receive follow-up services. (January-December ‘ 16) • Supported by Funding Opportunity Number CMS-1 G 1 -12 -001 from the U. S Department of Health and Human Services, Centers for Medicare & Medicaid Services 2. Willamette Education Service District contracted with OPIP to lead efforts in Marion, Polk and Yamhill County (May ‘ 16 -June ‘ 17) • In 2015 the Oregon Legislature directed Oregon Department of Education (ODE) to identify pathways from developmental screening to appropriate early learning services 57

Resources & Thanks! • http: //oregon-pip. org/focus/Follow. Up. DS. html • Documents Loaded to the Webinar – Progress Report – Early Childhood Mental Health Codes – Blank Template for Community Asset Mapping – Phone Follow-Up Script • Questions or follow-up – Colleen Reuland – reulandc@ohsu. edu • Thanks! • Please complete post-webinar survey
- Slides: 58