Better Care Fund Task Force Better Care Support

Better Care Fund Task Force Better Care Support Team Better Care Fund: reflecting on 2015/16, planning for 2016/17. Self-assessment tool The Better Care Fund

Introduction to this tool Contents It is around six months since this year’s local Better Care Fund programmes commenced. The Better Care Support Team would like to help local areas build on the experience and insight you have gained since that point, in order that this can inform programme plans for next financial year that continue to drive the national integrated agenda. In support of this, we have developed this toolkit. Before detailing the features of the toolkit on the next page, we’d like to provide a quick summary of the intentions behind it below. This toolkit should: ü Help you to internally benchmark your local area against those areas leading progress, showing opportunities for your local area to stretch and challenge itself further ü Support you in evaluating whether the schemes you have in place this year are the right ones to continue for next year, or whether they might need some adaptation ü Be suited to local shaping and adapting as appropriate by local areas, in order that you get best use out of its features ü Provide you with a general framework or ‘prompts’ through which to support discussion within local areas about the progress to date of BCF schemes, and the next steps for them ü Help you refresh plans on an annual basis This toolkit is not: Compulsory. We have designed this as a means of support for you to take, reshape, or leave as feels appropriate for your local area A form of performance monitoring or national reporting: we will not be asking for any results back from local areas The only means you should be using to assess the continued suitability of your current BCF schemes into 2016/17 – we would expect you have other formal means of evaluating this A source of definite answers: it is intended rather to help with the framing and prompting of some of the questions we would expect local areas are asking about their progress with integration, and their current Better Care Fund schemes 2

Self-assessment and evaluative framework An introduction to the two features of this toolkit There are two parts of this toolkit: one with a focus on local progress to integration, and one with a focus on your specific BCF schemes. Both should be helpful – however you may like to prioritise one over the other, or adapt them as necessary to suit your local area. Part One: Helping you benchmark your progress • against those leading • the way in implementing integrated care • Two: Supporting your discussions about thein • Part Exercise two: Reviewing 2015/16 schemes performance to date of your BCF schemes, preparation for 2016/17 planningand their long term future • This part is based on the Six Domains of Integrated Care implementation. (See slide 5) • • For each of the domains, we have created accompanying pages detailing relevant ‘good practice’: this is the behaviours, progress indicators, and characteristics that we’ve generally observed in local areas leading progress in these domains. We have used BCST insight work, subject experts and partners from other programmes and organisations, existing BCF “How-to Guides”*, and leadership insight and materials to populate these. • • • This part is intended to support local areas to focus attention on the schemes that they might need to re-evaluate before planning their 2016/17 integrated care programmes. It sets out a proposed scoring mechanism for local areas to rank their schemes from the most successful to the least. It should draw on local areas’ perception of the schemes’ successes to date. This is followed by a guided process to frame the sort of questions that should be asked of those schemes that come out with the lowest scores. We have then provided a short few questions to serve as prompts for your local area to consider when reviewing your progress against these areas. *http: //www. local. gov. uk/health-wellbeing-and-adult-socialcare/-/journal_content/56/10180/4096799/ARTICLE 3

How can you use this tool? Some options for making the most of this content… This tool has been designed to allow for as flexible use as possible. Below we have provided some different options for how you might pick up the content and frameworks in this document and make use of them in your local area - though you should also put some thought into how you can most effectively adapt these activities for your area. 1. A dedicated, facilitated workshop involving representatives across wider integration partners Most ve Intensi Wall-mount A 3 printouts of the ‘key characteristics of leading areas’ (part one), and the scoring sheets against each scheme (part two). Participants move around the room, review, score/self-assess, then come together to discuss. Options for reducing intensiveness: • For part one: identify specific key themes to focus on, and/or participants review ‘key characteristics’ content in advance of the session • For part two: Programme team agrees scoring criteria in advance of the session; participants score schemes in advance of the session and discuss reasoning at the session 2. Most value An extended board development session with senior sponsors/leads Carry out these activities in some form, or review this content, as part of an extended BCF/integrated programme board with time dedicated (i. e. 1 hour plus) to using the frameworks for reflecting on the past six months of BCF, and for beginning to form ideas for planning schemes for next year’s pooled fund. 3. A tool for discussion between project/programme leads in a set meeting to reflect on progress Less ve intensi Bring together programme manager and BCF scheme leads to reflect on progress to date. Options for increasing value: • For part one: Ensure there is a good balance of stakeholders from wider partners in the room, and a recommendation produced for senior sponsor review • For part two: Ensure scoring criteria is agreed by senior sponsors, and review lowest performing schemes at a more formal programme board/development session. A note of caution: The purpose of this tool is to reflect on progress to date and use this information to inform future planning. In order to be valuable there does need to be a clear link between this reflection activity, and the discussions between leaders involved in planning next year’s programmes and schemes. Less value 4
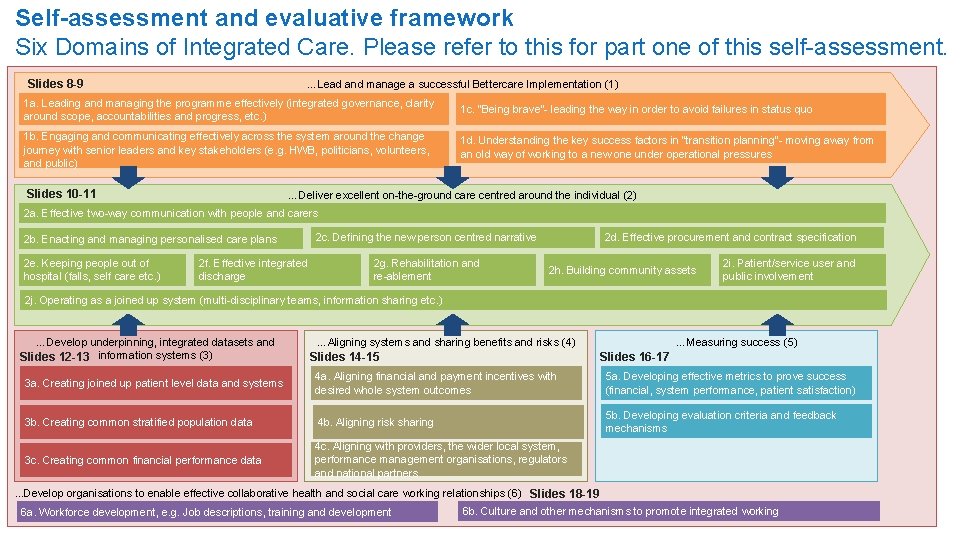
Self-assessment and evaluative framework How to use this tool (continued): The 6 ‘domains’ Six Domains of Integrated Care. Please refer to this for part one of this self-assessment. Slides 8 -9 …Lead and manage a successful Bettercare Implementation (1) 1 a. Leading and managing the programme effectively (integrated governance, clarity around scope, accountabilities and progress, etc. ) 1 b. Engaging and communicating effectively across the system around the change journey with senior leaders and key stakeholders (e. g. HWB, politicians, volunteers, and public) Slides 10 -11 1 c. “Being brave”- leading the way in order to avoid failures in status quo 1 d. Understanding the key success factors in “transition planning”- moving away from an old way of working to a new one under operational pressures …Deliver excellent on-the-ground care centred around the individual (2) 2 a. Effective two-way communication with people and carers 2 c. Defining the new person centred narrative 2 b. Enacting and managing personalised care plans 2 e. Keeping people out of hospital (falls, self care etc. ) 2 f. Effective integrated discharge 2 g. Rehabilitation and re-ablement 2 d. Effective procurement and contract specification 2 h. Building community assets 2 i. Patient/service user and public involvement 2 j. Operating as a joined up system (multi-disciplinary teams, information sharing etc. ) …Develop underpinning, integrated datasets and Slides 12 -13 information systems (3) …Aligning systems and sharing benefits and risks (4) …Measuring success (5) Slides 16 -17 Slides 14 -15 3 a. Creating joined up patient level data and systems 4 a. Aligning financial and payment incentives with desired whole system outcomes 5 a. Developing effective metrics to prove success (financial, system performance, patient satisfaction) 3 b. Creating common stratified population data 4 b. Aligning risk sharing 5 b. Developing evaluation criteria and feedback mechanisms 3 c. Creating common financial performance data 4 c. Aligning with providers, the wider local system, performance management organisations, regulators and national partners . . . Develop organisations to enable effective collaborative health and social care working relationships (6) Slides 18 -19 6 a. Workforce development, e. g. Job descriptions, training and development 6 b. Culture and other mechanisms to promote integrated working 5

Progress leader indicators – contents to section: Part one: Evaluating whole system progress to integrated care Checking the local pace of progress against that of the areas leading the way 6
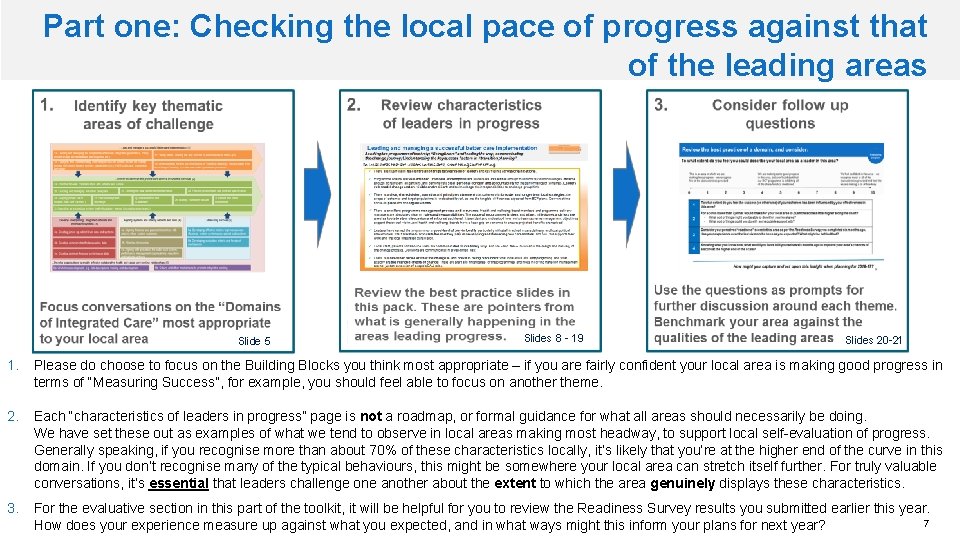
Part one: Checking the local pace of progress against that of the leading areas Slide 5 Slides 8 - 19 Slides 20 -21 1. Please do choose to focus on the Building Blocks you think most appropriate – if you are fairly confident your local area is making good progress in terms of “Measuring Success”, for example, you should feel able to focus on another theme. 2. Each “characteristics of leaders in progress” page is not a roadmap, or formal guidance for what all areas should necessarily be doing. We have set these out as examples of what we tend to observe in local areas making most headway, to support local self-evaluation of progress. Generally speaking, if you recognise more than about 70% of these characteristics locally, it’s likely that you’re at the higher end of the curve in this domain. If you don’t recognise many of the typical behaviours, this might be somewhere your local area can stretch itself further. For truly valuable conversations, it’s essential that leaders challenge one another about the extent to which the area genuinely displays these characteristics. 3. For the evaluative section in this part of the toolkit, it will be helpful for you to review the Readiness Survey results you submitted earlier this year. 7 How does your experience measure up against what you expected, and in what ways might this inform your plans for next year?

Domain 1. Leading and managing a successful Better Care Implementation If you would like some more information on this theme, please see our How-To Guide: http: //www. local. gov. uk/documents/10180/5572443/How+to+lead+and+manage+Better+Care+implementati on/90 f 695 ae-a 5 f 5 -4596 -bcec-345483 ec 8304 8

Leading and managing a successful better care implementation Leading the programme effectively; “Being brave” and leading the way; communicating the change journey; Understanding the key success factors in “transition planning” In local areas that are leaders in this area, some things we’re ü There are trustful and resilient relationships between senior leaders and key figures across organisations. seeing: ü Programme boards are well attended, involved, and empowered: leaders are influential enough to unblock system challenges, diverse enough to represent all partners, and demonstrate clear personal concern and accountability for the performance of schemes. Leaders role model change and are visible and resilient, and acknowledge their responsibilities to challenge groupthink. ü There is a clear, shared vision, narrative and principles statement that coheres with broader and longer term local strategies: the scope of schemes and target populations is understood by all, as are the tangible differences expected from BCF plans. Conversations focus on place and not organisations. ü There is excellent programme management process and assurance. Health and wellbeing board members and programme delivery managers are absolutely clear on roles and responsibilities. The scope of programmes is clear, and plans, milestones and risks are used as tools to steer discussion and action at each level. It is evident and understood how workstream/scheme management objectives support the overall vision, and health and wellbeing boards have a keen grip on schemes to ensure projected benefits are realised. ü Leaders have earned the programmes a good-level of buy-in locally, particularly with staff involved in care delivery, and local political stakeholders. Staff are able to articulate the role they play in developing and delivering new care models, and how this supports their work and the local integrated care vision. ü Local staff, patients and service users are communicated to in a timely way, and are – and feel – involved in the design and delivery of the change process. Decisions are communicated in a well-timed way. ü There is a described sense of what the change is, and how it is being resourced: what local areas are stopping doing, and what exactly are the intended effects of change. There are start and finish dates for the programmes, and roles involving transition management are not just an extension of people’s normal roles. 9

Domain 2. Delivering excellent on-the-ground care around the person 10

Delivering excellent on the ground care around the person In local areas that are leaders in this area, some things we’re seeing: Planning and co-ordinating care around the person… ü People are genuinely involved in designing their health and care – their plans are holistic, not just clinical, and reflect their goals, not just their needs. ü Plans are “asset based” – i. e. they articulate the knowledge and skills, and existing sources of support people bring to managing their own condition. There is genuine evidence of co-production and co-design between people and between professionals, demonstrating how people using the services are shaping them at governance and delivery levels. ü Local areas are able to evidence a measurable shift in culture – broadly things are beginning to focus around multidisciplinary primary and community care, GPs are involved with other professionals, and there is a much broader support for a selfmanagement ethic through a range of targeted interventions. ü Patient/person activation measures are being used: these measures enable practitioners to understand how engaged people are, and how willing and able they are to manage their own condition …Ensuring that this is supported by the wider infrastructure ü Contracts and service specifications should specify and meet ‘person centred care’, through an outcomes focus and through explicit involvement of patients’ wishes. There is evidence of personal budgets to support personal care. ü The role of the voluntary sector and social enterprise play is recognised and involved in creating truly integrated services. ü Procurement processes don’t exclude CICs/social enterprises from providing services through overly bureaucratic processes ü Community assets are planned and co-ordinated. JSNAs are accompanied by a joint assets vision to meet the needs assessment. ü The person centred narrative is pushing beyond merely ‘defining’ the cohort, through to work to link integrated datasets. 11
Domain 3. Develop underpinning, integrated datasets and information systems 12

Develop underpinning, integrated datasets and information systems Joining up patient level data; Creating common stratified financial performance data; creating common stratified population data In local areas that are leaders in this area , some things we’re seeing: ü Local areas have worked together to establish the vision, and plan: They have worked across organisations to define the project and specific objectives. They are aware of how sharing information will enable achievement of those objectives. There is strong leadership and sponsorship from commissioners, providers, patient groups and elsewhere. There are initial sessions with IG experts who will support the work and are involved early and focused on delivery. ü The work is underpinned and supported by trustful, resilient relationships between people and organisations. There is a governance structure in place across providers and other interested parties, setting out clear and immediate objectives. The formal decision making group has all major representatives across the system, and there is an IG and information sharing workstream with IG representatives from all participating organisations. An information sharing strategy has been agreed. ü Stakeholder engagement of data sharing has been considered and is thorough: there is secured clinical buy in and arrangements to engage with groups representing the interests of citizens. As a result there is a clear communications strategy which has been drafted and tested with patient groups and professionals. The legal basis for sharing has been identified, there is clarity regarding the specifications of data to be shared and data sharing agreements are signed with all major providers including GP practices. ü There is agreement on the technical solutions required through an implementation roadmap. This includes clarity about the roles including responsibilities of HSCIC, DSCROs and CSUs. Clarity on how requirements stemming from the privacy impact assessment have been met. ü Satisfactory information governance toolkits have been met and risks identified in privacy impact assessments have been addressed. Communications strategy has been implemented. Staff have been informed and trained and there is access to information governance support for the team. 13

Domain 4. Aligning systems and sharing risks and benefits If you would like some more information on this theme, please see our How-To Guide http: //www. local. gov. uk/documents/10180/5572443/150303+How+to+bring+budgets+tog ether+v 6 -WEB. pdf/f 343948 b-9 e 2 a-49 e 1 -9334 -70 ad 705 bb 8 a 0 14

Aligning systems and sharing risks and benefits Aligning financial and payment incentives with desired whole system goals; aligning risk sharing; aligning with providers, the wider local system, performance management, regulators and other national bodies In local areas that are leaders in this area, some things we’re seeing: ü There is strong trust and resilient relationships across the system ü Areas have linked datasets, and have analysed and jointly understood the risk profiles of their local population. There is a real understanding of how people are using their local services, and the impact that new service models including vanguards, devolution and personalised commissioning will have. ü There is strong understanding of how much they are spending on priority population groups across the local system, and how they are expecting to change this through their integration schemes ü Local finance working groups are in place for aligning strategy. This encompasses commissioners and local providers from across the spectrum. ü Finance working groups have a robust, detailed financial risk log and mitigation plan, and are regularly monitoring and tracking this. There is understanding of the whole system effect of risks being realised. ü Areas are checking their plans with peers to provide added insight and challenge ü Outcomes are informed by patients and service users. Payment incentives support the delivery of person-centred care and align with patient/service user preferred outcomes ü Local areas are looking to develop more innovative means of payment structures involving capitation, and gain and loss sharing across partners. ü There is familiarity with the legislation and funding streams surrounding the pooled budget. ü Plans have credibility through strong local assurance, owned by senior leaders and other relevant local scrutiny boards. Local areas have made efforts to engage with and understand the constraints and flexibilities of national planning, regulatory and assurance frameworks. 15

Domain 5. Measuring Success If you would like some more information on this theme, please see our How-To Guide http: //www. local. gov. uk/documents/10180/5572443/How+to+understand+measure+i mpact/dbedc 114 -bd 19 -40 f 5 -a 040 -db 3177736 b 23 16

Measuring success Developing effective metrics to prove success (financial, system performance, patient satisfaction); Developing evaluation criteria and feedback mechanisms In local areas that are leaders in this area, some things we’re seeing: ü Evaluation and monitoring systems are designed as an early part of the process, designed to run throughout the lifespan of the schemes and provide timely feedback for schemes ü Local areas have found means to incorporate patient/service user feedback and at the centre of commissioning ü Evaluation looks at the process measures as well as patient/care outcome measures ü There is a good understanding of exactly how areas expect their schemes to improve care and what outcomes they are expecting to see ü Evaluation method and criteria is signed up to by all partners, and buy-in is ensured ahead of recommissioning and evaluation discussions ü Scope is co-produced for each piece of evaluation work, so expectations are clear at the start ü Stakeholders are clear on what information they should and are able to provide to help deliver a good evaluation ü Milestones are mapped into the programme plan, as is what information will need to be fed into the conversations around these milestones ü There are established protocols and plans for the evaluation, consent forms and procedures, as well as the design of the evaluation team ü There is a strong understanding and confidence of the quality of data in use – and the process for cleaning and quality assuring this ü Thought has been given to how staff will respond to evaluation, and evaluation is viewed as a constructive, learning exercise ü Local areas understand the likelihood of changes to schemes in advance and are planning adaptable evaluation methods ü There is clarity across partners about what is to be evaluated and what they are looking to learn ü Evaluation is independent of the delivery of the project ü Opportunities to pair with academic networks and regional, or peer, local areas for peer evaluation are being taken/considered 17
Domain 6. Developing organisations to enable effective health and social care working relationships If you would like some more information on this theme, please see our How-To Guide http: //134. 213. 15. 24/documents/10180/5572443/How+to+work+together+across+health %2 C%20 care+and+beyond/d 828032 e-d 1 d 2 -4325 -a 017 -4 b 564 c 65 d 4 eb 18

Developing organisations to enable effective health and social care working relationships Developing the workforce to support new models of care; culture and other mechanisms to promote integrated working In local areas that are leaders in this area, some things we’re seeing: Early stages – jointly mapping the current workforce, and designing the new conditions for a sustainable integrated workforce. ü Strong relationships exist between different organisations ü System leaders can articulate a shared vision for the health and social care workforce of the local area. A shared workforce strategy is agreed, informed by a common understanding of the current state, and the particular challenges of individual organisations Looking forward – mapping the future workforce needs ü ü The future workforce strategy is underpinned by new models of care, in particular planned new models of care around the patient. The specific actions to transition to new models are mapped and there is a common understanding of the plan ü Senior system leaders are fostering new relationships with employers and education to equip a workforce for the future with the right skills ü Steps are being taken to join the local system with regional networks, to jointly approach workforce challenges by means of harmonising contracts, including by defining limits for pay and other working incentives ü Training that will need to take place is understood and jointly planned, to ensure it reads across different organisations to reduce duplication and make best use of it Implementing new models of workforce, enabling the conditions for future workforce ü ü Throughout the system there is a consistent focus on the person, and those delivering care understand how new models support them to deliver better, person centred care Frontline staff understand the part that their evolving training, working conditions and model of care delivery plays in achieving the local vision ü Necessary steps are taken to role model and support integrated working, such as colocation and joint training days ü Those involved in new models fully understand the responsibilities of their new roles: e. g. GPs as co-ordinators of care plan MDT meetings, etc. and are proactively delivering on these ü Programme leads are making use of best practice, tools and contract templates where available, and there are mechanisms in place for capturing and building on what works locally. ü Local areas are reaching out to other areas with ‘peer’ or regional profiles to understand means of supporting integrated care ü Where possible, local H&SC employers are making use of contract and T&Cs templates that support workers to transition to integrated care roles 19

Part one continued: Reflecting on the factors behind local progress in integrated care Having reviewed the characteristics of leaders in an area of integrated care, you should use the questions overleaf as prompts for further discussion within your local area leadership team. Guidance notes: • It will be clear that these questions do not come with any definite answers, however you might use them as a stimulus for discussion, and a means of reflecting collectively on your experience of integrating care to date. • It will be helpful to have sight of the Readiness Survey your local area completed in March. In this you assessed how ‘ready’ you felt as an area to make progress in each of the integrated care domains. 20
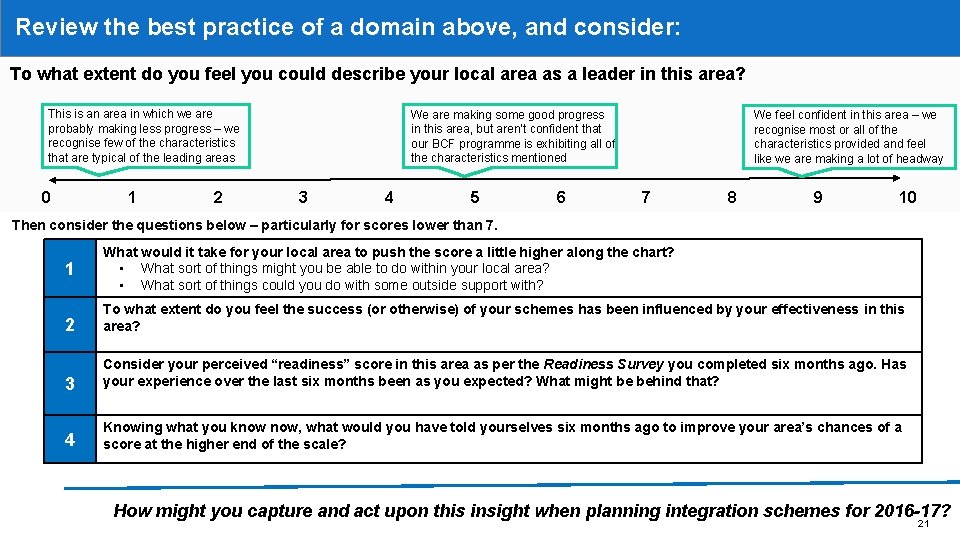
Review the best practice of a domain above, and consider: Self-assessment questions to consider against each set of principles To what extent do you feel you could describe your local area as a leader in this area? This is an area in which we are probably making less progress – we recognise few of the characteristics that are typical of the leading areas 0 1 2 We are making some good progress in this area, but aren’t confident that our BCF programme is exhibiting all of the characteristics mentioned 3 4 5 6 We feel confident in this area – we recognise most or all of the characteristics provided and feel like we are making a lot of headway 7 8 9 10 Then consider the questions below – particularly for scores lower than 7. 1 What would it take for your local area to push the score a little higher along the chart? • What sort of things might you be able to do within your local area? • What sort of things could you do with some outside support with? 2 To what extent do you feel the success (or otherwise) of your schemes has been influenced by your effectiveness in this area? 3 Consider your perceived “readiness” score in this area as per the Readiness Survey you completed six months ago. Has your experience over the last six months been as you expected? What might be behind that? 4 Knowing what you know now, what would you have told yourselves six months ago to improve your area’s chances of a score at the higher end of the scale? How might you capture and act upon this insight when planning integration schemes for 2016 -17? 21

Progress leader indicators – contents to section: Part two: Evaluating the current BCF schemes and interventions in your local area A framework to begin evaluating how 2015/16 schemes should fit into 2016/17 plans 22

Part Two: A framework to begin evaluating how 2015/16 schemes should fit into 2016/17 plans This exercise is intended to prompt discussions about the future of the 2015/16 BCF schemes. It does not provide any answers, but should enable local areas to begin evaluating how local BCF schemes have been working to date, and which ones are likely to need re-evaluating when planning for 2016/17. Guidance notes: • There is a Section A and a Section B to this exercise. See the following slides for a walk-through of the process • In Section A you will be asked to score your schemes against a number of statements. You should score the schemes as a group where possible; it’s actually the discussion and reasoning behind the scoring that should encourage you to reflect as a group on the success or otherwise of your schemes. • This is intended to be used as a template for local areas to recreate either in an Excel file, Powerpoint, or as is helpful. Please do adapt it to suit local needs, and to the context in which you might use it (a workshop, smaller group meeting, or board development session). • The exercise should be carried out by those who will be involved in the planning of 2016/17 schemes, with the right level of seniority to influence the process. 23
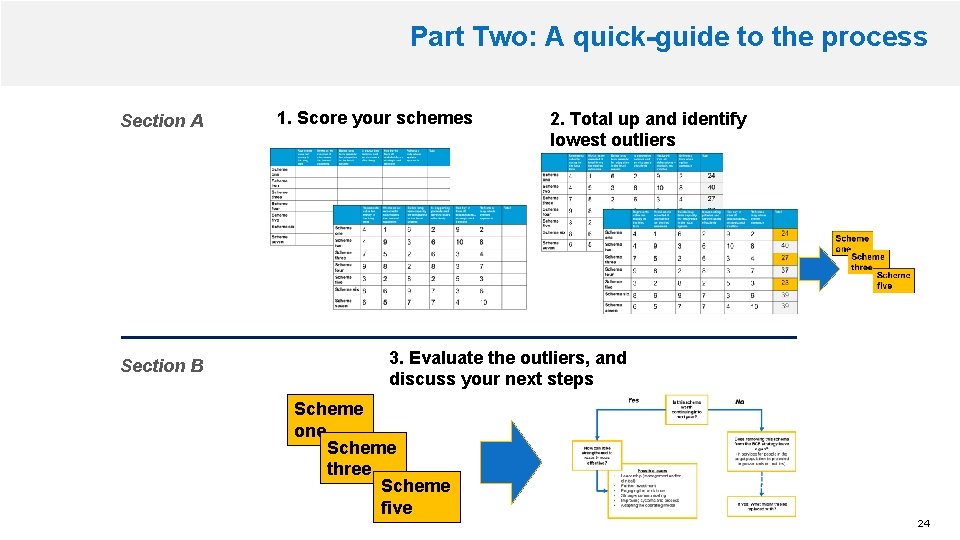
Part Two: A quick-guide to the process Section A Section B 1. Score your schemes 2. Total up and identify lowest outliers 3. Evaluate the outliers, and discuss your next steps Scheme one Scheme three Scheme five 24
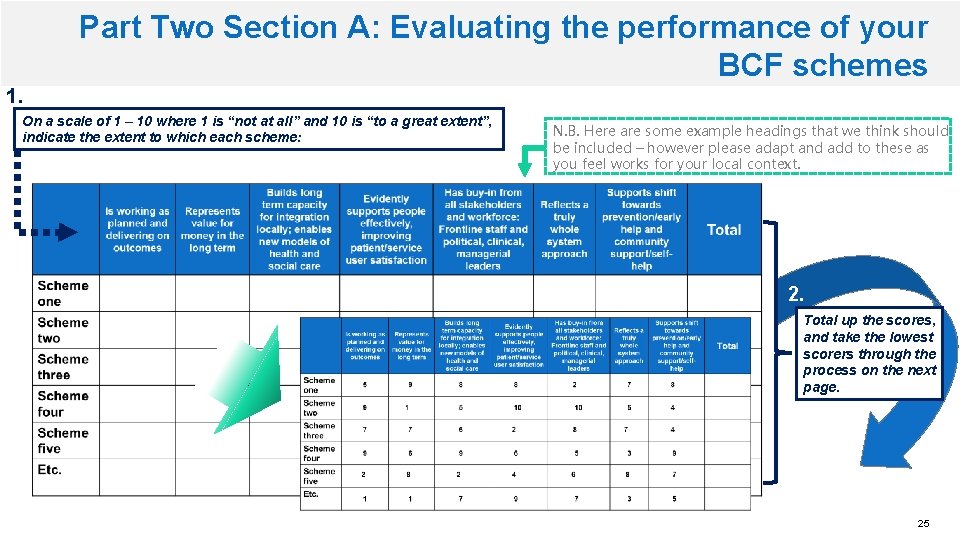
Part Two Section A: Evaluating the performance of your BCF schemes 1. On a scale of 1 – 10 where 1 is “not at all” and 10 is “to a great extent”, indicate the extent to which each scheme: N. B. Here are some example headings that we think should be included – however please adapt and add to these as you feel works for your local context. 2. Total up the scores, and take the lowest scorers through the process on the next page. 25
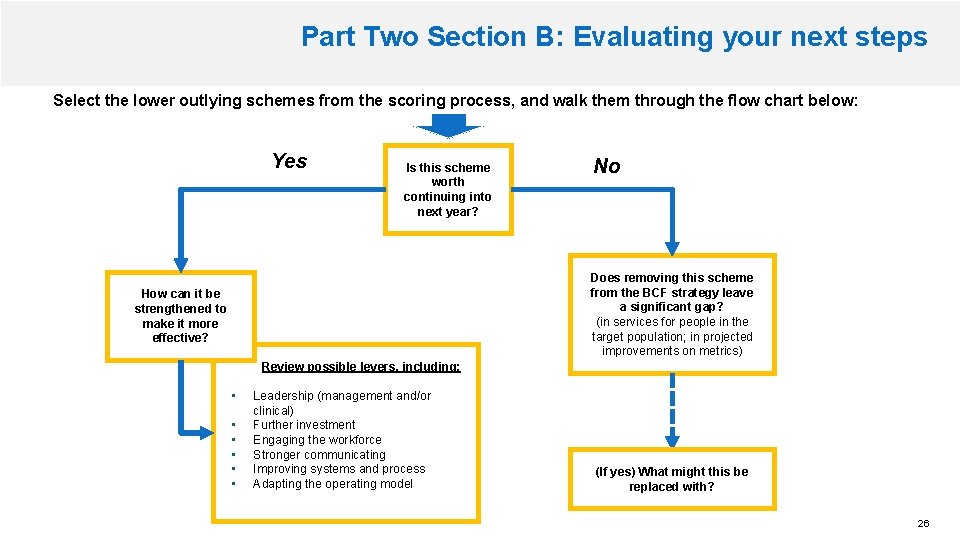
Part Two Section B: Evaluating your next steps Select the lower outlying schemes from the scoring process, and walk them through the flow chart below: Yes Is this scheme worth continuing into next year? No Does removing this scheme from the BCF strategy leave a significant gap? (in services for people in the target population; in projected improvements on metrics) How can it be strengthened to make it more effective? Review possible levers, including: • • • Leadership (management and/or clinical) Further investment Engaging the workforce Stronger communicating Improving systems and process Adapting the operating model (If yes) What might this be replaced with? 26
- Slides: 26