Best Practices Caring for Recently Arrived Arab and

“Best Practices Caring for Recently Arrived Arab and Muslim Women” Fatin Sahhar, MD Shahla Namak, MD Ammar Charestan, MD Fadya El Rayess, MD, MPH
Arabs & Muslims—What’s the Difference? • ~92% of Arabs are Muslims. – A minority of Arabs are Christian or Jewish. • ~20% of the world’s Muslims are Arab. – Most Iraqis are Arab Muslims – Iranians are not Arab. They are Aryan (not Semitic) and speak Farsi (not Arabic). 2

Muslims: Demographics • Which country do you think has the most Muslims?

Indonesia!
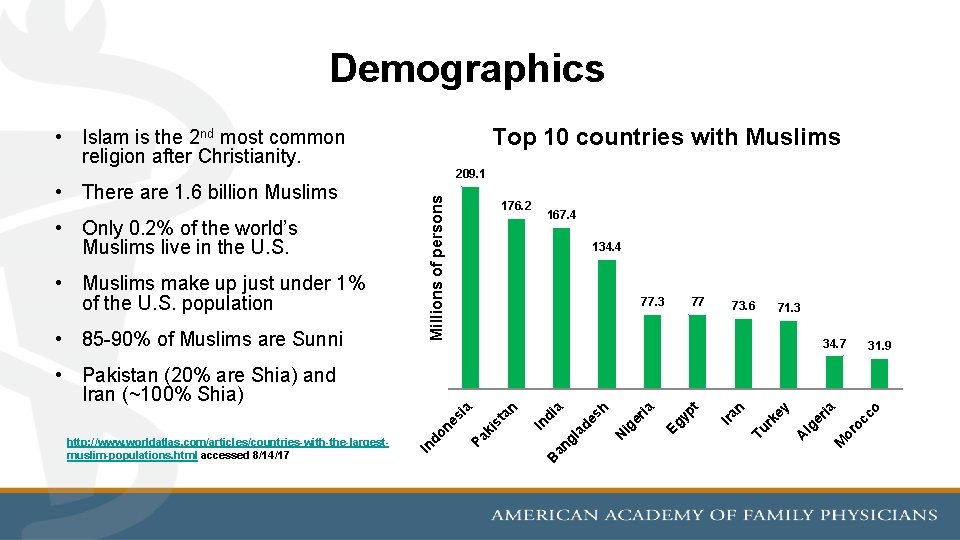
Demographics Top 10 countries with Muslims • Islam is the 2 nd most common religion after Christianity. • Only 0. 2% of the world’s Muslims live in the U. S. • Muslims make up just under 1% of the U. S. population • 85 -90% of Muslims are Sunni Millions of persons • There are 1. 6 billion Muslims 209. 1 176. 2 167. 4 134. 4 77. 3 77 73. 6 71. 3 34. 7 31. 9 oc co or M A lg er ia y rk e Tu n Ira t yp Eg ia ig er ad gl an N es h a di In B st an ki Pa In http: //www. worldatlas. com/articles/countries-with-the-largestmuslim-populations. html accessed 8/14/17 do ne s ia • Pakistan (20% are Shia) and Iran (~100% Shia)
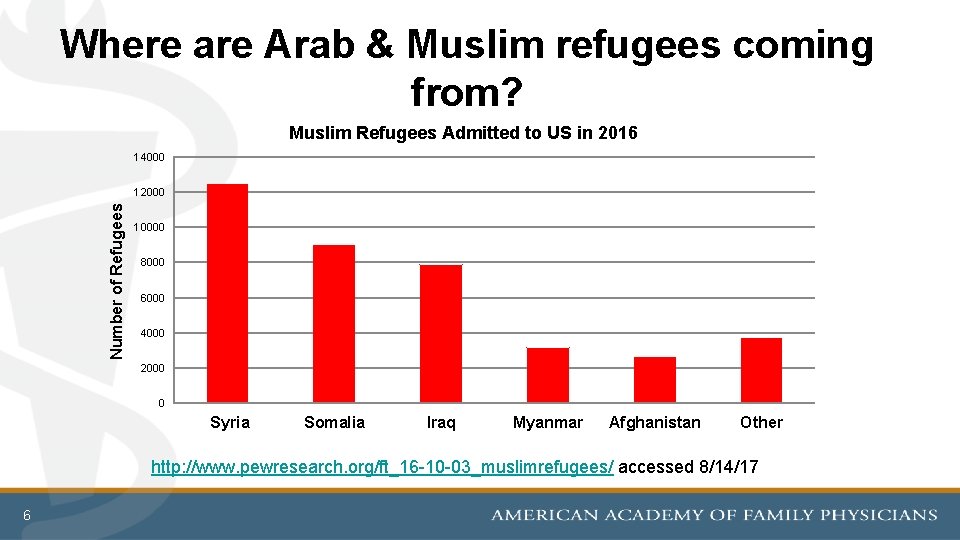
Where are Arab & Muslim refugees coming from? Muslim Refugees Admitted to US in 2016 14000 Number of Refugees 12000 10000 8000 6000 4000 2000 0 Syria Somalia Iraq Myanmar Afghanistan Other http: //www. pewresearch. org/ft_16 -10 -03_muslimrefugees/ accessed 8/14/17 6

Communication skills Arab and Muslim Women (A&MW) • • • 7 Gender preferences Things to avoid Modesty/Dress/ Hijab Building rapport Other communication tips: Ramadan, Informed consent, Sexuality

Gender Preference in Healthcare • A&MW prefer women medical providers and interpreters • They are not allowed to be alone with a male Provider. • Islam, allows for cross gender provider-patient situations under life-threatening conditions or when alternatives are unavailable. 8

What if only a Male Provider is Available ? • Refer to the client as “my sister” • Maintain minimal eye contact and a physical distance - (fear of invoking sexual impropriety) • Integrate the family during the medical encounter • If no relative, have a female staff chaperone w/exam • Minimize patient’s body exposure • Reassure that the relationship is protected by professional standards. 9

Other Things to Avoid with Members of the Opposite Sex • Hand shaking - women wearing the hijab - strict Muslim men. • Patting a patient's arm or giving a comforting hug - unless the provider is of the same gender. • Entering the room without knocking and giving time to women with hijab to cover appropriately. (inpt or outpt. ) 10

Muslim Women’s Dress Supposed to be Not supposed to be • • • Transparent Modest to maintain: - moral social order - protect a person's honor Cover the hair, arms, and legs in the presence of any teen or adult male who isn’t a direct lineage • It is a cultural interpretation, and it varies widely 11 • Shape-revealing • More conservative if western style

Building Rapport with Arab Women • • • 12 Ask about their family Encourage sharing their refugee stories/experiences Emphasize confidentiality, esp. w/sensitive issues Empower sharing views and expectation from the relationship Demonstrate genuine respect and acceptance of their beliefs Allow them to share safely how their religiosity helps them make sense of their experience

Informed Consent • “patient autonomy” and “next of kin” have little practical meaning for these patients” • In time of crisis or major decisions families will consult all members of the extended family, especially the men. • Less involvement would be considered neglect or abandonment of the health of a sick family member 13

Informed Consent and Patient Confidentiality 14 Challenges Suggested solutions • A woman may expect and prefer that a consultation is made with her husband possibly away from the bedside. • This might be in conflict w/ IC requirements: - full and truthful disclosures - autonomous decision-making Obtain her permission to discuss the case with her husband outside of her presence. Document the permission and discussion in the patient's medical record.

The Month of Ramadan • Muslims refrain from - food - drink - sexual activity - from dawn to dusk • Some Muslims still want to fast even though their illness exempts them. 15 • • Exemptions: Pregnant & Breast feeding Menstruating women, Children Elderly Those travelling Patients who must take medication throughout the day • Those who are ill

Human Sexuality • For most, a female will be “talked to” on her wedding day about the basics of sex. • Asking women about STI could be taken as offensive would imply a deviation from monogamy. 16 • GYN exams – Permitted: * married women * previously married women – Not permitted: * unmarried women unless serious medical condition

Breast Feeding • Preferred • Done privately by Arabic women in general and Muslim women. 17

Family Planning in Islam • There are references to family planning in – the Qu’ran, – the Hadith (a collections of words, actions or habits of the prophet Muhammed) and – the Fatwa (rulings on Islamic Shariah Law by religious scholars) 18 • Basic Framework – Muslims have a responsibility to inhabit and develop the earth – Marriage’s purpose includes procreation and enjoying company of spouse – The sanctity of life and welfare of mother both important

Birth Spacing • Birth spacing is permissible: – “And we have enjoined on man (to be dutiful and good) to his parent. His mother bore him in weakness and hardship, and his weaning is in two years. ” (Qur’an 31: 14) • Muslim religious scholars have agreed that the mother requires an additional year to recover. • They recommend 36 months for birth spacing. • Limiting then number of births at a population level is not El Hamri N. Approaches to FP in Muslim Community. J Fam Planning & Reproductive Health Care 2010: 36(1): 27 -31 19

Al Azl – Coitus Interruptus “We [the Companions of the • This is the basis of acceptance Prophet] used to practice coitus of reversible contraception interruptus during the lifetime of – OCPs the Messenger of Allah. The – Condoms Messenger of Allah came to know – Injections it and he didn’t forbid us from – IUDs/ Implants practicing it. ” (Hadith: Muslim • They are permissible with the 1440) consent of the wife El Hamri N. Approaches to FP in Muslim Community. J Fam Planning & Reproductive Health Care 2010: 36(1): 27 -31 20

Abortion Permissible • When mother’s life is in danger • In cases of – rape – severe fetal anomalies – unwanted pregnancies when family situation or social context could harm mother or child’s well being Debate about timing of ensoulment • 40 days post conception • 120 days post conception Shahawy S, Deshpande NA, Nour NM. Cross-Cultural Obstetric and Gynecologic Care of Muslim Patients. Obstet Gynecol 2015; 126: 969– 73 21

Best Practices for Family Planning Discussions • Focus on promoting the health of the family • Discuss importance of birth spacing, folic acid and early prenatal care • Discuss reversible contraceptives and inquire about views related to sterilization as appropriate • Consider reaching out to/ involving local religious leaders 22

“Cancer screening” • In 2010, only 45. 6% of Arab Americans underwent colorectal screening as compared to 70. 9% of the general population. • In 2014, only 52% of Am Muslim women had screening mammogram as compared to the national figure of 67%. 23 • Muslim immigrants show higher rates of cervical cancer mortality despite their lower incidence. – Screening rates are particularly low for first generation immigrants. – Arab American women who had lived in the U. S. for 10 years or longer are more likely to receive a Pap test. – Women who speak English very well are more likely to receive a Pap test

General Barriers to Cancer Screening Personal Factors: • Fear of pain/discomfort • Lack of awareness of the procedure • Don’t think it’s necessary • Misperception of the risk • Inadequate knowledge • Educational level • Lack of time • Fear of cancer diagnosis (Mammogram) • Embarrassment (PAP) • Threat to virginity (PAP) 24

General Barriers to Cancer Screening, cont. Cultural Factors: • Provider gender • Acculturation • Language barrier • Dealing with physical and/or emotional trauma- focus on immediate survival • Resettling in an unfamiliar culture • Having few medical services in their home countries prior to coming to US • Inattentiveness to personal health (secondary to war-torn lives or common views of illness as symptomatic)- “If does not hurt me, I do not have to go to a doctor today. ” 25

General Barriers to Cancer Screening, cont. Religious Factors: Systemic Factors: • Fatalism- “I’m going to leave it up to God, and • • • if I get sick, it’s God’s will. ” • Modesty • Negative religious coping (e. g. , viewing health problems as a punishment from God) 26 Lack of health insurance Lack of access to PCP Financial reasons Length of stay in US Difficulty with transportation

Possible Interventions: for Health Providers • • Undergo training for providing culturally sensitive health programs at your clinic or community Availability of female health professionals Availability of trained medical interpreter services Availability of mental health and behavioral health therapy – Deeper understanding of women’s refugee mental health could provide additional insight to their motivation for obtaining screening. • Respect for physician (as an authority figure) – – Utilize the positive attitude towards physicians to gear medical recommendations, adherence/compliance, and health promotion. Appointment reminders & recommendations from physicians were deemed especially effective • Alternative modes of screening, i. e. “HPV self-sampling”: – Consideration for modesty, privacy (can perform/mail without family’s knowledge) – Premarital sexual activity (cultural taboo) – Cost-effective, saves time 27

Possible Interventions: for Patients • Community Outreach programs to assist refugee women in providing culturally- and lingually-appropriate services: interpretation, health education, health promotion. • Patient Navigator programs to optimize patient-physician interactions in refugee communities: health education, explore barriers, tailor interventions, help to schedule appointment, make reminder calls, arrange transportation, resolve insurance issues, accompany patients to their appointments. • Promoting Knowledge about cancer screening. Health care professionals should learn about each patient’s exposure to medical services in her home country as well as the length of time she has spent in the US. • Transportation Services: shuttles or taxi vouchers provided by the health center; ready access to public transportation 28

Possible Interventions, cont. Sample Study • “Culturally Tailored Navigator Program” in Colorectal Cancer Screening • Goal – • Methods: – – – • Patients received an introductory letter with educational material followed by phone or in-person contact by a languageconcordant navigator. ” Navigators (community health workers) trained to identify and address patient reported barriers to CRC screening. Individually tailored interventions included: » patient education » procedure scheduling » translation and explanation of bowel preparation » help with transportation and insurance coverage Rates of colorectal cancer screening were assessed for intervention and usual care control patients. Results: – 29 A culturally-tailored, language concordant navigator program designed to identify and overcome barriers to colorectal cancer screening can significantly improve colonoscopy rates for low income, ethnically and linguistically diverse patients. Over a 9 -month study period, the incidence of CRC screening was more than double in intervention patients vs. usual care controls 27% and 11. 9% respectively

Possible Interventions, cont. • Faith-Based Messages: incorporating religiously tailored messages in cancer screening intervention has the potential to enhance cancer screening in this community. – Messages delivered by Imams and Islamic scholars who, as faith leaders, play an important role in providing health promotion message to their community – Emphasize the value of preventive cancer screening by addressing the concerns of modesty and predestination. • Positive religious coping: religious support mechanisms such as prayers, and congregational support, for understanding and managing life stressors. 30

Lastly… Healthcare professionals and public health officials should not make any absolute characterization about a patient or patient population based on her religious beliefs. Personal and psychological barriers to care can be overcome with tailored education and community-based programming. 31

Culturally sensitive practice with Arab clients in mental health setting. 1. Family and Gender constructions: - The family is important , male is dominant, female is perceived as physically and mentally weak. - it is common for women: not to have careers outside home. endure years of marital problems to avoid the stigma of divorce or the prospect of losing their children. 2. Individual development in Arab Societies: -The Father is the Head of the family and considered a powerful and Charismatic figure. - In Arab school system, the curriculum is based largely on rote learning and remembering facts, rather than on developing individual interpretations and analysis. 3. Process of acculturation: -Ethnic Arab immigrants to western countries are known to experience divided loyalties between the ways of the new country and those of the old and dilemma of whether to reject or embrace assimilation, secularism and western education. -Some factors may be associated with Arab peoples’ greater acculturation to and life satisfaction in some western countries. These factors include longer residence in a host country, younger age at immigration, not recently visiting one’s Arab country homeland being of a Christian religious background.

Culturally sensitive practice with Arab clients in mental health setting. • Cultural Facts: -Psychiatry and psychology therapies are considered as stigma. -Ethnic Arab clients often view affective disorders as having somatic origins. -It is difficult for an Arab client to divulge a personal problems and feeling to someone outside of the family or community. -Arab culture condemns suicide, and clients may not divulge suicidal feelings easily. For example if you ask directly most of depressed patient if they having thoughts of killing themselves, they reply that they are good people and would never entertain suicide thoughts. But if potentially suicidal patient are asked if they wish that God would let them die, they usually will reply in the affirmative.

Guidelines for mental Health Practice with Ethnic Arab Clients • • Client communication styles are formal, impersonal and restrained, These difficulties should not be constructed as client resistance. Practitioners should expect the Arab client to remain passive during the assessment interview and the helping process in general. Arab clients and their families place a great deal of responsibility on mental health practitioners to provide solutions to problems with little or no input from client. The helping should be direct and clear, with concrete targets. build a relationship (a trust) than to solve a problem. role of religion. incorporating traditional healing (rituals, incense burning, or visiting saints’ tombs. ) with the modern helping process. Arab families are expected to be involved and are consulted in times of crisis. If the cultural gap is too great, involving a cultural consultant who can mediate between the family and practitioners-might be advisable. The chosen consultant may be affiliated with the mental health agency, or a member of the community, but in all instances her or she would have to be deemed suitable by the family. • thank you!
- Slides: 34