Best Practice for Breast Radiotherapy 2015 Clinical Oncology

Best Practice for Breast Radiotherapy: 2015 Clinical Oncology Audit Conference Royal College Radiologists Suzy Cleator: Consultant Clinical Oncologist, Imperial College Healthcare NHS Trust

Focus on Breast Adjuvant Radiotherapy (invasive disease) • Best practice defined by: • Acceptable Local control – other factors: • • • Patient population (screening vs symptomatic) Selection for breast conserving radiotherapy Quality of radiology Quality of pathology Quality of systemic therapy Quality/ appropriate selection of • Surgery (nipple/ skin preservation/ margins) • Radiotherapy • Minimizing toxicity: • • • Cardiac Musculoskeletal Cosmetic Second malignancy Brachial plexopathy • Avoiding unnecessary radiotherapy/ technology: • Avoid unnecessary radiotherapy – elderly, postmastectomy • Avoid inappropriate hyperfractionation/IMRT/boosts

Measuring Local Control • Most centres cannot quote their local control rate • ‘Contemporary’ UK local control rates captured by the UK START Trial

START Trial; local control • 17 centres for START-A and 23 for START-B • Patients were recruited after complete excision of primary invasive breast cancer (p. T 1– 3 a, p. N 0– 1, M 0) • Boost (10 Gy in 5 f) – no effect on local control/ cosmetic result (61% patients overall)

Local Recurrence Rates have Fallen

How to achieve good local control (from radiotherapy) • Do what was done in the START trial! • CT-planned 3 D conformal • Use whole breast radiotherapy post breast conservation • Apply boosts as indicated • Don’t miss the tumour bed – clips, appropriate use of shielding • ? Appropriate use of bolus post-mastectomy • Good set up – individual and departmental • Start within a time window

Whole breast vs Partial Breast • Rationale: • • > 90% of recurrences are adjacent to primary site Late toxicity relates to treated volume Reduction in poor cosmesis, chest wall discomfort, second malignancy Smaller volumes allow for acceleration and hypofractionation • But: • • It is not going to be more effective than WBRT It needs to be at least equivalent It should be better than surgery alone Not all partial breast irradiation is the same
Partial Breast Radiotherapy – techniques • Intra-operative • TARGIT: • • • Intraoperative single treatment 50 k. V (“soft”) x-rays (photons) Dedicated machine (Intrabeam) 20 Gy at the surface of the applicator 5 -6 Gy at 1 cm NICE-approved ……for now • Mammosite: • • Afterloading catheters Placed intra- or post-operatively 2 balloon sizes, cavity is stretched over surface 34 Gy at 1 cm in 10 # (BD) 5/7 • Intra-operative Electrons: • • • EIO Milan Dedicated theatre Linac Post quadrantectomy & SNB Initially developed as a boost In phase III trial as sole therapy (ELIOT) 21 Gy as a single fraction to 90% isodose (calculated to be 56 Gy equivalent) • External Beam • Conformal/ IMRT

Partial Breast Radiotherapy – long term data • TARGIT • ELIOT • Very short follow-up (median follow-up of 2 years and 5 months) • 10 year results poor (not published) • Clearly not effective for pts not on endocrine therapy • Trend towards increased risk LR in TARGIT arm – no impact on OS expected • TARGIT concurrently with lumpectomy (prepathology, n=2298) had much the same LR expected from no radiotherapy : • • At medium follow-up of 5· 8 years, 35 (4. 4%) patients in the IORT and 4 (0. 4%) patients in the external RT group had an IBTR (p<0· 0001 • Most recurrences near tumour bed 2· 1% (1· 1– 4· 2) versus 1· 1% (0· 5– 2· 5; p=0· 31) • What happens when pts complete endocrine therapy? • Well tolerated (as is external beam RT) Lancet Oncology, 2013 Intraoperative radiotherapy versus external radiotherapy for early breast cancer (ELIOT): a randomised controlled equivalence trial. Veronesi U et al. • HDR Brachytherapy • Budapest Trial • 258 patients randomized • Partial breast RT delivered by electrons in 30% cases • 10 yr LR was 5. 9% vs 5. 1% in PBI and WBI arms, respectively (p = 0. 77) • rate of excellent-good cosmetic result was 81% in the PBI, and 63% in the control group (p < 0. 01) • External Beam • Results pending: • NSABP-B-39/RTOG -0413: 4, 300 participants randomly assigned to WBI or APBI using 3 D-CRT or balloon-catheter or interstitial brachytherapy • IMPORT low

Use of Boosts • EORTC “boost versus no boost” trial • 5318 patients with no tumour at margin • Whole breast 50 Gy in 25# (2 Gy) ± 16 Gy boost in 8# or implant (9%) • 20 year recurrence 13% (no boost) vs. 9% (boost) HR 0· 65 (99% CI 0· 52– 0· 81, p<0· 0001) • Age 40 local relapse 36% (NB) 24. 4%(B), p=0. 003 • Age 41 -50 local relapse 19. 4%(NB) 13. 5%(B), p=0. 007 • Age 51 -60 local relapse 13. 2%(NB) 10. 3%%(B) NS • Age >60 local relapse 12. 7%(NB) 9. 7%%(B) NS • Young age most important risk factor for local recurrence • Cosmetic results not as good in boost arm • No impact on overall survival Whole-breast irradiation with or without a boost for patients treated with breast-conserving surgery for early breast cancer: 20 -year follow-up of a randomised phase 3 trial. Bartelink H et al. Lancet Oncology 2015
Use of Clips • Facilitate accurate localization for tumour bed boost • Avoid mis-placement of tangents • No evidence of clip migration • Help with treatment verification • LCA audit: • Clinical findings alone were used to define tumour bed in 2/180 (1. 1%) cases and CT abnormality alone in 14/180 (7. 7%) cases. Clips were inserted and used in 164/180 (91. 2%) cases. The median number of clips inserted was 5 (minimum 2) - S Dadhania, S Cleator.

Appropriate Use of Bolus • Variation in use: • 1035 responses to survey- Vu T et al, Clin Oncol 2007 • • • 642 from the Americas - 82% use bolus 327 from Europe - 31% 66 from Australasia - 65% - (P < 0. 0001) • Variation in the schedule of application • • every day [33%] alternate days [46%]) < 1 cm [35%] > or = 1 cm [48%]) • Adds to toxicity: • Retrospective cohort study of 254 patients treated with adjuvant postmastectomy radiotherapy, 1993 -2003 (Tieu M, Int Radiat Oncol Biol Phys, 2011) • • • 143 patients received radiotherapy with whole chest wall bolus 88 patients with parascar bolus 23 with no bolus. • Twenty patients did not complete radiotherapy because of acute skin toxicity: • • 17 in the whole chest wall bolus group (12%) 2 in the parascar bolus group (2%) 1 in the group not treated with bolus (4%) On multivariate analysis, whole chest wall bolus and chemotherapy were found to be significant predictors for early cessation of radiotherapy resulting from acute skin toxicity • 19 chest wall failures • • 13 in the whole chest wall bolus group (9%) 4 in the parascar bolus group (4. 5%) 2 in the no-bolus group (9%) On multivariate analysis, lymphovascular invasion and failure to complete radiotherapy because of acute skin toxicity were associated with chest wall recurrence
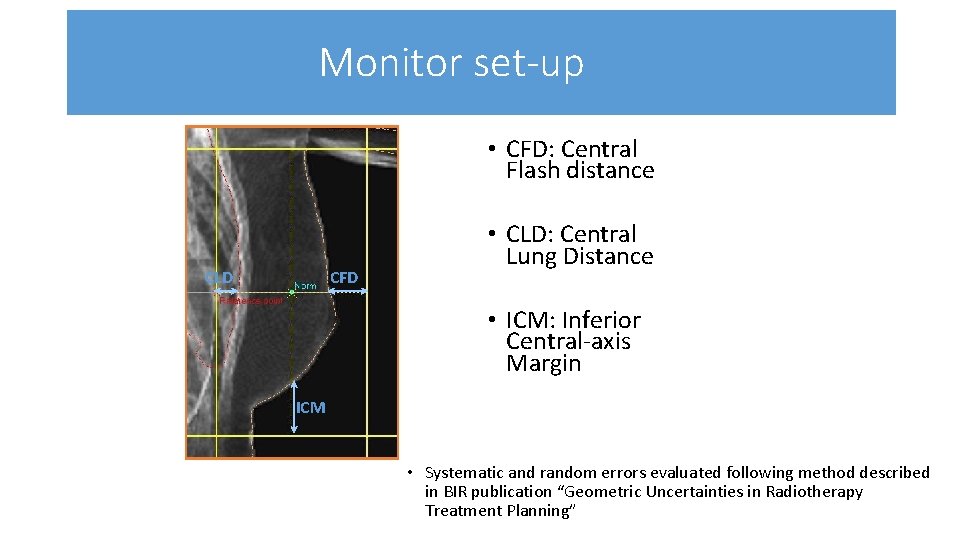
Monitor set-up • CFD: Central Flash distance CFD CLD • CLD: Central Lung Distance • ICM: Inferior Central-axis Margin ICM • Systematic and random errors evaluated following method described in BIR publication “Geometric Uncertainties in Radiotherapy Treatment Planning”
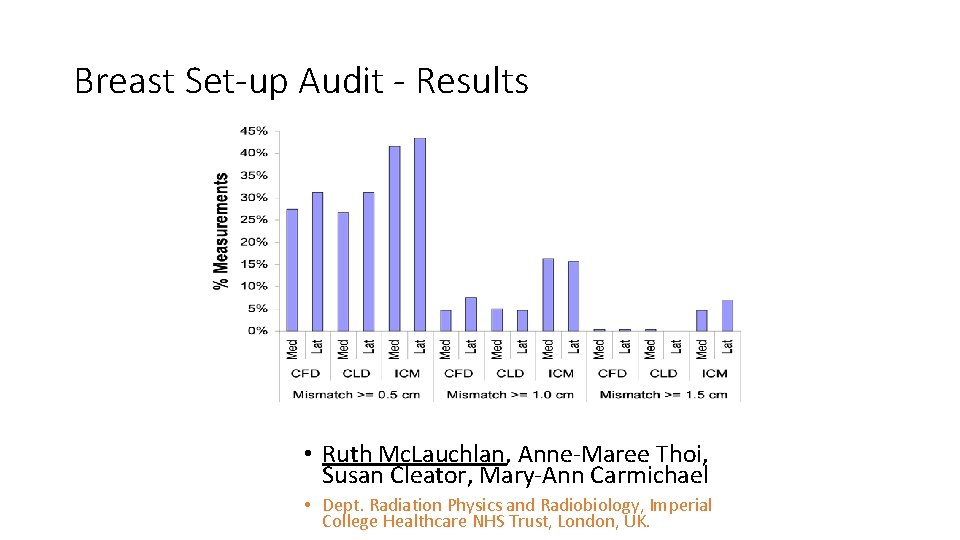
Breast Set-up Audit - Results • Ruth Mc. Lauchlan, Anne-Maree Thoi, Susan Cleator, Mary-Ann Carmichael • Dept. Radiation Physics and Radiobiology, Imperial College Healthcare NHS Trust, London, UK.

Window for Radiotherapy • 18 050 women ≥ 65 with stage 0 -II breast cancer diagnosed in 19912002 who received, BCS, RT but no chemotherapy (SEER database) • Interval between surgery and starting RT of > 6 weeks associated with increased likelihood of local recurrence • hazard ratio 1. 19, 95% confidence interval 1. 01 to 1. 39, P=0. 033 • Continuous relationship association • hazard ratio 1. 005 per day, 1. 002 to 1. 008, P=0. 004) • intervals over six weeks were associated with a 0. 96% increase in recurrence at five years (P=0. 026).
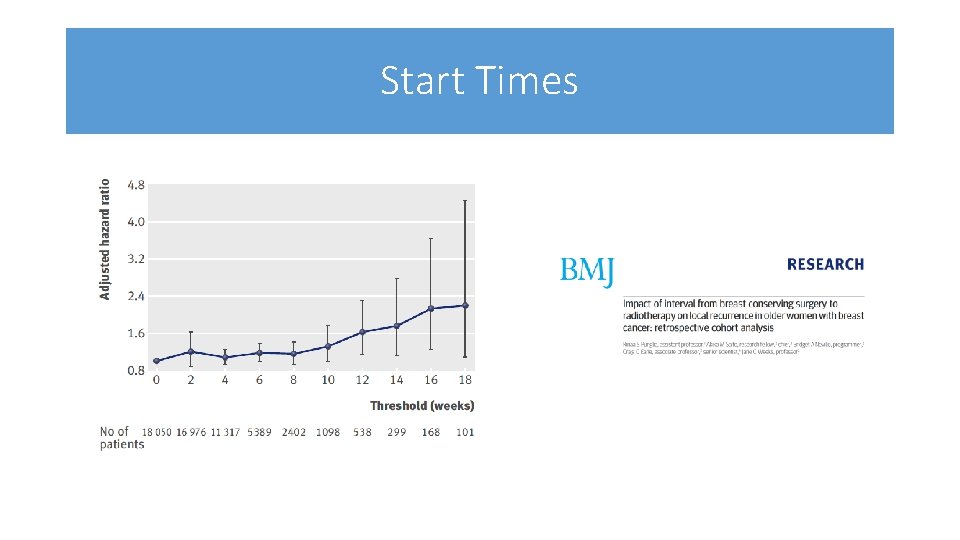
Start Times

How to deliver safe radiotherapy • Avoid use of 50 Gy in ‘START Trial’ population • Avoid cardiac toxicity • Avoid increasing risk of second malignancy • Avoid boost were not necessary • Avoid radiotherapy where possible • PRIME 2 population • Low-risk post-mastectomy patients • Employ IMRT to minimize dose to normal tissues in complex cases
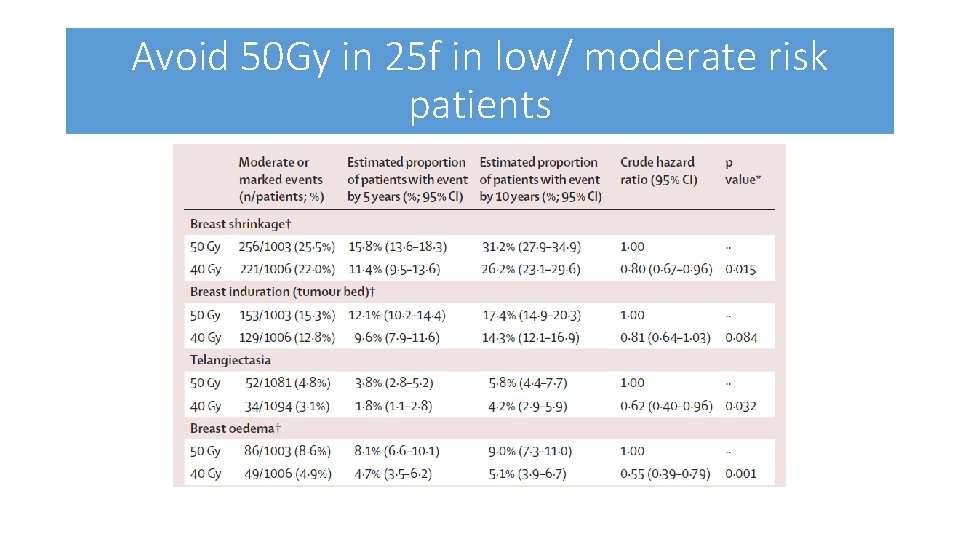
Avoid 50 Gy in 25 f in low/ moderate risk patients
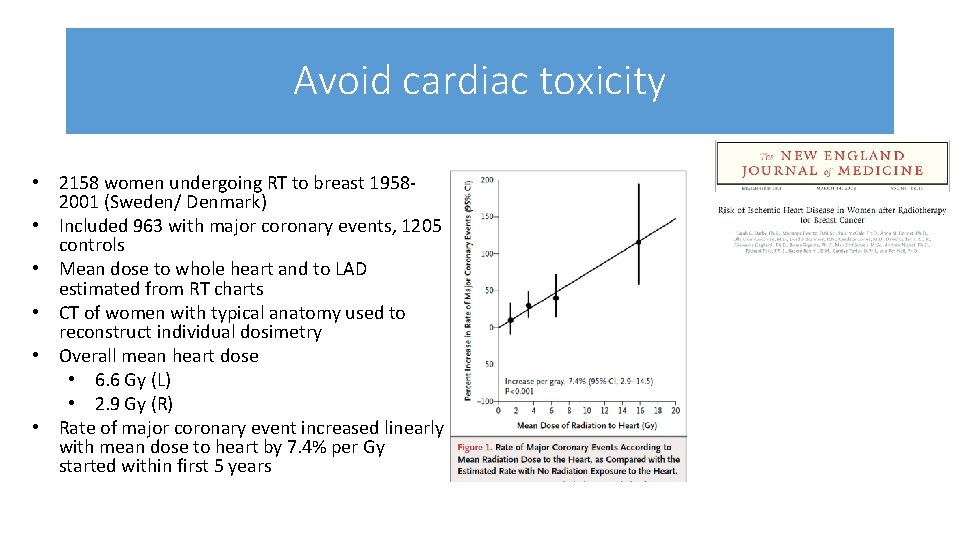
Avoid cardiac toxicity • 2158 women undergoing RT to breast 19582001 (Sweden/ Denmark) • Included 963 with major coronary events, 1205 controls • Mean dose to whole heart and to LAD estimated from RT charts • CT of women with typical anatomy used to reconstruct individual dosimetry • Overall mean heart dose • 6. 6 Gy (L) • 2. 9 Gy (R) • Rate of major coronary event increased linearly with mean dose to heart by 7. 4% per Gy started within first 5 years
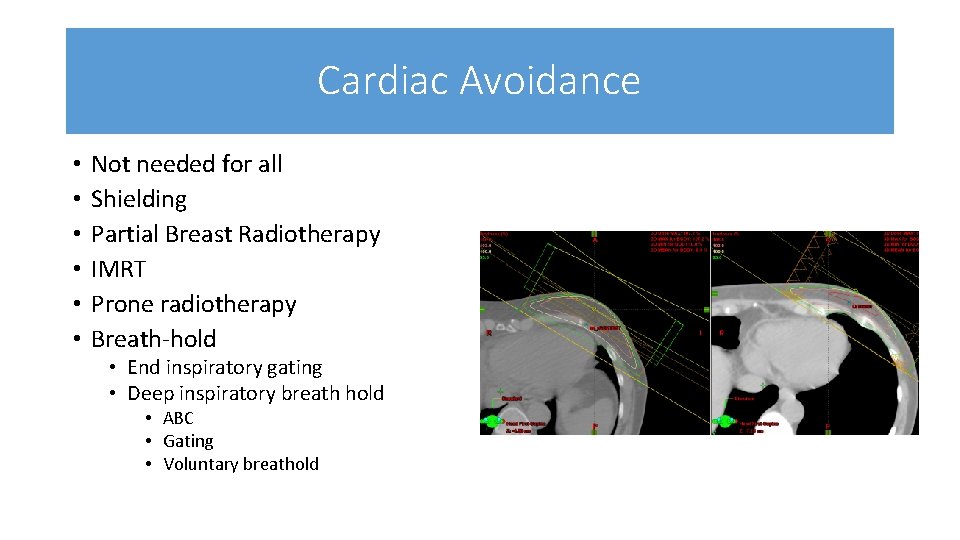
Cardiac Avoidance • • • Not needed for all Shielding Partial Breast Radiotherapy IMRT Prone radiotherapy Breath-hold • End inspiratory gating • Deep inspiratory breath hold • ABC • Gating • Voluntary breathold

Avoid second malignancy • Thirteen studies comprising 762, 468 breast cancer patients included in meta-analysis • ≥ 5 yrs after breast cancer diagnosis radiotherapy was significantly associated with an increased risk of • • second non-breast cancer RR 1. 12 (95% confidence interval [CI] 1. 06– 1. 19) second cancer of the lung RR 1. 39 (95% CI 1. 28– 1. 51) esophagus RR 1. 53 (95% CI 1. 01– 2. 31) second sarcomas RR 2. 53 (95% CI 1. 74– 3. 70) • The risk increased over time, and was highest 15 or more years after breast cancer diagnosis • for second lung RR 1. 66 (95% CI 1. 36– 2. 01) • and second esophagus cancer RR 2. 17 (95% CI 1. 11– 4. 25) • Second lung cancer after radiotherapy for breast cancer is associated with the delivered dose to the lung (Grantzau T et al. Risk of second primary lung cancer in women after radiotherapy for breast cancer. Radiother Oncol 2014; 111: 366– 73) • It has been estimated by Hall et al. , that IMRT would almost double the incidence of second cancers compared to conventional 3 DCRT (Hall EJ, Wuu CS. Radiation-induced second cancers: the impact of 3 D-CRT and IMRT. Int J Radiat Oncol Biol Phys 2003; 56: 83– 8)

Avoid boost where possible • Cumulative incidence of severe fibrosis at 20 years • 5· 2% (99% CI 3· 9– 6· 4) in the boost group • versus 1· 8% (1· 1– 2· 5) in the no boost group (p<0· 0001). S • The cumulative incidence of any degree of fibrosis (minor, moderate, or severe) • 71· 4% (69· 0– 73· 7) versus 57· 2% (54· 6– 59· 8; p<0· 0001).

Consider with-holding radiotherapy in PRIME 2 population • Several randomized studies • CALBG • PRIME 2 • • March 2015, Lancet (Kunkler et al) >65 yrs, ER pos, node neg Median F/U 5 yrs, IBR was 1· 3% vs 4· 1% (p=0· 0002) HR for IBR, 5· 19 (95% CI 1· 99 -13· 52; p=0· 0007) • ASCO endorse withholding of radiotherapy in elderly low risk (has not been adopted) • More work needed to selection of patients at very low risk of recurrence; Canadian LUMINA study (NCT 01791829)

Select patients carefully post-mastectomy • Many of the trials were undertaken decades ago • Management of axilla was often suboptimal • Contemporary series suggest risk of LR low if 1 -3 LN positive • Contemporary series suggest risk of LR low if T 3 N 0 • Current ASCO and LCA guidance: • RT of T 3/ T 4 • RT if >3 LN positive/ single LN mass≥ 3 cm • Awaiting results from SUPREMO study • Post mastectomy, RT vs no RT, intermediate risk cases
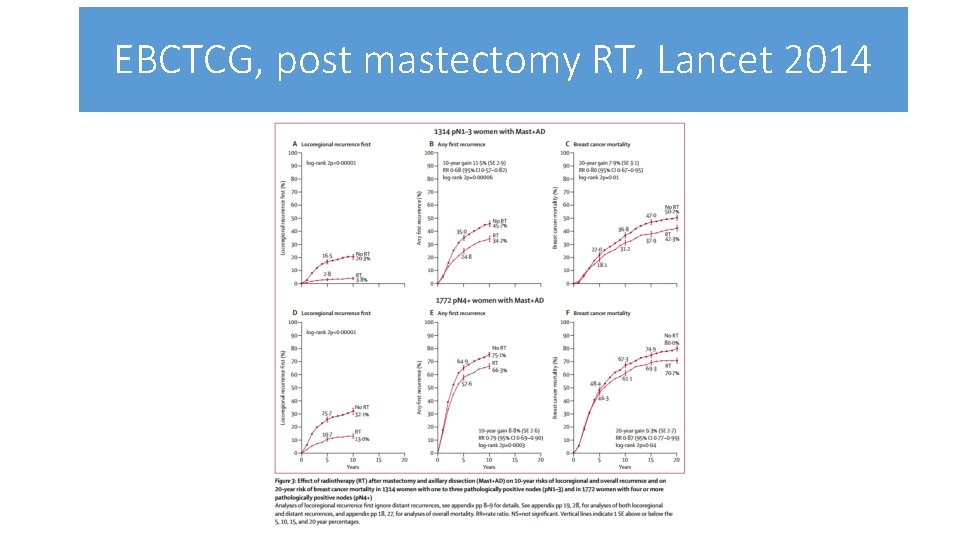
EBCTCG, post mastectomy RT, Lancet 2014


Employ IMRT when indicated • Medial tumours • Unusual chest anatomy • Internal mammary irradiation • Dose homogeneity for whole breast RT can usually be achieved by CT forward planned IMRT (extra segments)

What can be measured • Clear guidance/ gold standard: • • Set up Use of clips Appropriate fractionation Timeliness • Controversial: • Use of boosts • Post mastectomy radiotherapy • For the future: • Use of cardiac sparing radiotherapy (mean cardiac dose) • ? ? ? LOCAL CONTROL…………. .
- Slides: 28