Berkshire West 10 Frail and Older People Pathway

Berkshire West 10 Frail and Older People Pathway Redesign Programme South Reading Patient Voice Group Stuart Rowbotham; Director of Adult Social Care, Wokingham Borough Council

Meeting aims To share with Reading Patient Voice: • the work undertaken as part of the Frail and Older People Project • the key findings to date of the project • the next steps in developing services BW 10 Integration Programme

Programme aims To build on the model of care developed with the Kings Fund in 2014 by: – creating a person centred, joined up response to meet Sam’s needs; – improving the experience of older people living in our communities; – enhancing the navigation of services across our system; and – using scarce resources more efficiently in the face of growing demand. BW 10 Integration Programme

Progress to date Care Model 1. 2. 3. 4. Carried out a gap analysis comparing the current pathway against “Sam’s Story”; Identified 11 areas of focus for improvement; Reviewed evidence of best practice against these 11 areas; Developed initial assumptions for testing through the financial model. Financial Model 1. 2. 3. Collected available data from all organisations involved in the current pathway; Developed analysed a detailed baseline of current service provision; Produced a first draft 5 year projection. BW 10 Integration Programme
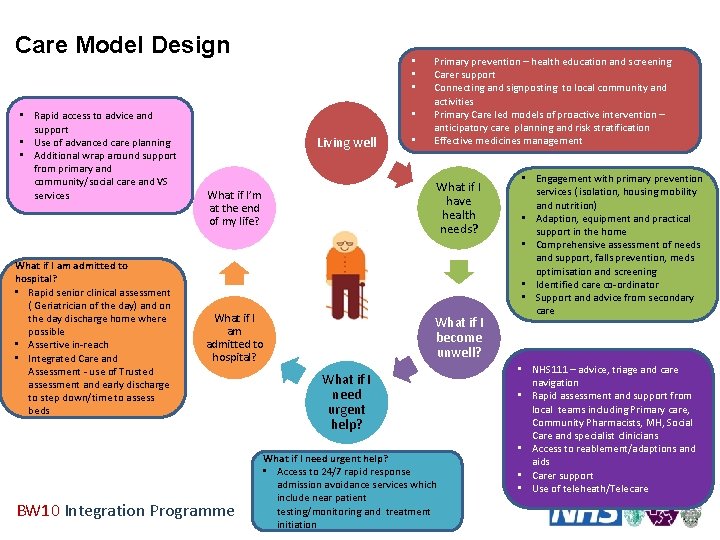
Care Model Design • Rapid access to advice and support • Use of advanced care planning • Additional wrap around support from primary and community/social care and VS services What if I am admitted to hospital? • Rapid senior clinical assessment ( Geriatrician of the day) and on the day discharge home where possible • Assertive in-reach • Integrated Care and Assessment - use of Trusted assessment and early discharge to step down/time to assess beds • • Living well • Primary prevention – health education and screening Carer support Connecting and signposting to local community and activities Primary Care led models of proactive intervention – anticipatory care planning and risk stratification Effective medicines management What if I’m at the end of my life? What if I have health needs? What if I am admitted to hospital? What if I become unwell? BW 10 Integration Programme What if I need urgent help? • Access to 24/7 rapid response admission avoidance services which include near patient testing/monitoring and treatment initiation • Engagement with primary prevention services ( isolation, housing mobility and nutrition) • Adaption, equipment and practical support in the home • Comprehensive assessment of needs and support, falls prevention, meds optimisation and screening • Identified care co-ordinator • Support and advice from secondary care • NHS 111 – advice, triage and care navigation • Rapid assessment and support from local teams including Primary care, Community Pharmacists, MH, Social Care and specialist clinicians • Access to reablement/adaptions and aids • Carer support • Use of teleheath/Telecare
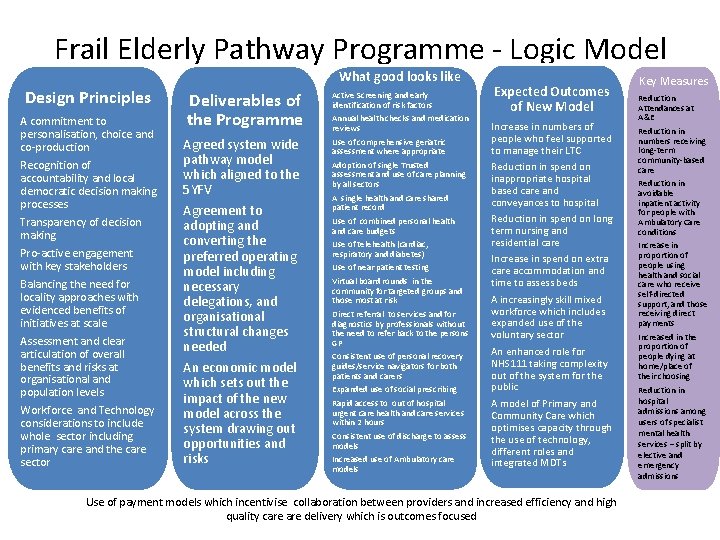
Frail Elderly Pathway Programme - Logic Model What good looks like Design Principles A commitment to personalisation, choice and co-production Recognition of accountability and local democratic decision making processes Transparency of decision making Pro-active engagement with key stakeholders Balancing the need for locality approaches with evidenced benefits of initiatives at scale Assessment and clear articulation of overall benefits and risks at organisational and population levels Workforce and Technology considerations to include whole sector including primary care and the care sector Deliverables of the Programme Agreed system wide pathway model which aligned to the 5 YFV Agreement to adopting and converting the preferred operating model including necessary delegations, and organisational structural changes needed An economic model which sets out the impact of the new model across the system drawing out opportunities and risks Active Screening and early identification of risk factors Annual health checks and medication reviews Use of comprehensive geriatric assessment where appropriate Adoption of single Trusted assessment and use of care planning by all sectors A single health and care shared patient record Use of combined personal health and care budgets Use of telehealth (cardiac, respiratory and diabetes) Use of near patient testing Virtual board rounds in the community for targeted groups and those most at risk Direct referral to services and for diagnostics by professionals without the need to refer back to the persons GP Consistent use of personal recovery guides/service navigators for both patients and carers Expanded use of social prescribing Rapid access to out of hospital urgent care health and care services within 2 hours Consistent use of discharge to assess models Increased use of Ambulatory care models Expected Outcomes of New Model Increase in numbers of people who feel supported to manage their LTC Reduction in spend on inappropriate hospital based care and conveyances to hospital Reduction in spend on long term nursing and residential care Increase in spend on extra care accommodation and time to assess beds A increasingly skill mixed workforce which includes expanded use of the voluntary sector An enhanced role for NHS 111 taking complexity out of the system for the public A model of Primary and Community Care which optimises capacity through the use of technology, different roles and integrated MDTs Use of payment models which incentivise collaboration between providers and increased efficiency and high quality care delivery which is outcomes focused Key Measures Reduction Attendances at A&E Reduction in numbers receiving long-term community-based care Reduction in avoidable inpatient activity for people with Ambulatory Care conditions Increase in proportion of people using health and social care who receive self-directed support, and those receiving direct payments Increased in the proportion of people dying at home/place of their choosing Reduction in hospital admissions among users of specialist mental health services – split by elective and emergency admissions

Next steps. 1. Agree the target changes in activity levels and financial impact modelling 2. Identify the service operating model and early quick wins or development opportunities for 16/17 3. Map and establish the links with NHS and Local Authority related projects • Primary Care Strategy and local plans • Better Care Fund Plans • CCG Operating Plans for 16/17 • Wider system Workforce Strategy • Connecting Care and expanding technology enabled care • CCG Transformation Board work programmes BW 10 Integration Programme
- Slides: 7