Benign tumors of the Female Reproductive Tract n


Benign tumors of the Female Reproductive Tract n Pelvic mass A pelvic mass may be gynecologic in origin or it may arise from the urinary tract or bowel. n The gynecologic causes of a pelvic mass may be uterine, adnexal, or more specifically ovarian. n
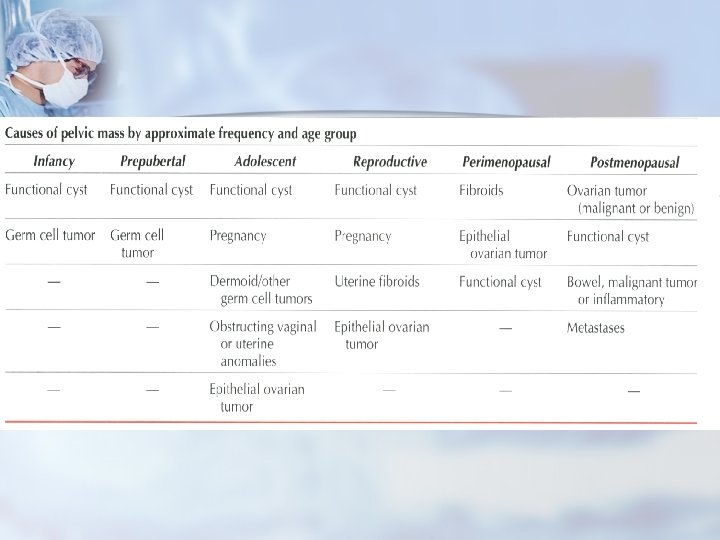

Prepubertal Age Group - Differential Diagnosis n < 5% of ovarian malignancies n Germ cell tumors make up 1/2 to 2/3 n 35% of all ovarian neoplasms occurring during childhood and adolescence were malignant n < 9 y/o, 80% malignant n

Prepubertal Age Group - Differential Diagnosis n n n Symptoms: abdominal or pelvic pain Pelvic mass very quickly becomes abdominal in location as it enlarges because of the small size of the pelvic cavity. Diagnosis is difficult because of the rarity of the condition (and therefore a low index of suspicion) Many symptoms are nonspecific Acute symptoms are more likely to be attributed to more common entities such as appendicitis.

Prepubertal Age Group - Differential Diagnosis Abdominal palpation n bimanual rectoabdominal examination n Abdominal in location: can be confused with other abdominal masses n Acute pain: torsion. n The ovarian ligament becomes elongated as a result of the abdominal location, thus creating a predisposition to torsion.

Prepubertal Age Group - Diagnosis and Management Ultrasonography n Unilocular cysts are virtually always benign and will regress in 3 to 6 months do not require surgical management with oophorectomy or oophorocystectomy. n
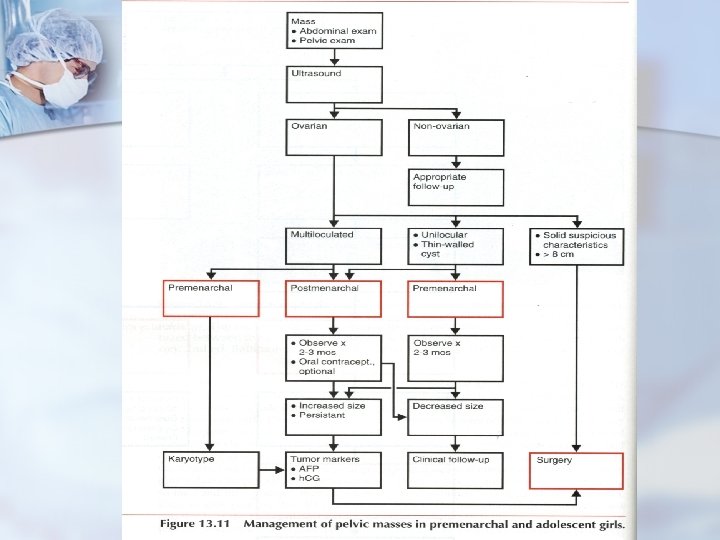

Prepubertal Age Group - Diagnosis and Management n n Close observation recommended (discuss risk of ovarian torsion with the child's parents. ) Recurrence rates after cyst aspiration 50%. Attention: long-term effects on endocrine functioning, future fertility, preservation of ovarian tissue Premature surgical therapy - ovarian and tubal adhesions that can affect future fertility.

Prepubertal Age Group - Diagnosis and Management Additional imaging : CT, MRI, Doppler flow studies. n Risk of a germ cell tumor is high, the finding of a solid component mandates surgical assessment. n

Adolescent Age Group n Differential n Ovarian Diagnosis Masses n Uterine Masses n Inflammatory Masses n Pregnancy

Adolescent Age Group - Ovarian masses n n The risk of malignant neoplasms lower. Germ cell tumors - most common tumors of the first decade of life but occur less frequently during adolescence. Epithelial neoplasms - increasing frequency with age. Mature cystic teratoma - most frequent neoplastic tumor of children and adolescents, accounting for > 1/2 of ovarian neoplasms in women < 20 y/o

Adolescent Age Group - Ovarian masses Neoplasia can arise in dysgenetic gonads. n 25% of dysgenetic gonads of patients with a Y - malignant. n Gonadectomy - recommended for patients with XY gonadal dysgenesis or its mosaic variations. n

Adolescent Age Group - Ovarian masses n Functional ovarian cysts n Incidental finding on examination n Pain caused by torsion, leakage, or rupture. n Endometriosis is less common during adolescence than in adulthood. n In series of adolescents referred with chronic pain, 50% to 65% have been found to have endometriosis.

Adolescent Age Group - Ovarian masses Most adolescents with endometriosis do not have associated obstructive anomalies. n In young women, endometriosis may have an atypical appearance, with nonpigmented or vesicular lesions, peritoneal windows, and puckering. n
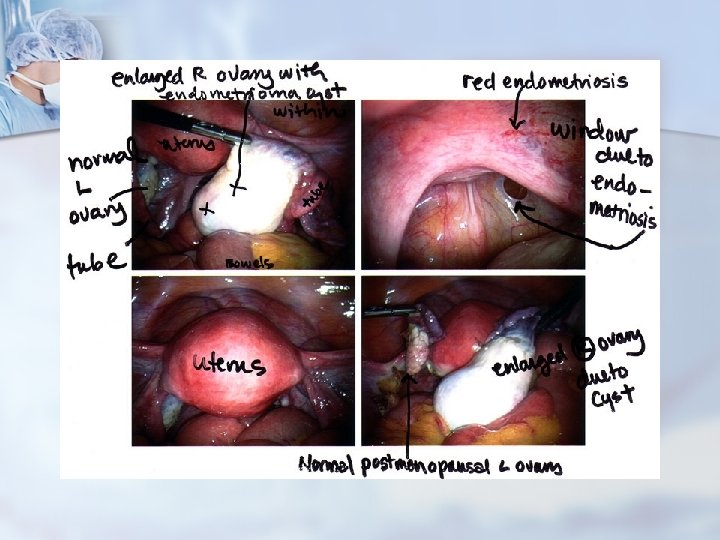

Adolescent Age Group - Uterine Masses Uterine leiomyomas - not common n Obstructive uterovaginal anomalies occur during adolescence, at the time of menarche, or shortly thereafter. n The diagnosis is frequently neither suspected nor delayed, particularly when the patient is seen by a general surgeon. n

Adolescent Age Group - Uterine Masses n n n Uterine anomalies - imperforate hymen, transverse vaginal septa, vaginal agenesis with a normal uterus and functional endometrium, vaginal duplications with obstructing longitudinal septa, and obstructed uterine horns. Cyclic pain, amenorrhea, vaginal discharge, or an abdominal, pelvic, or vaginal mass. Hematocolpos, hematometra
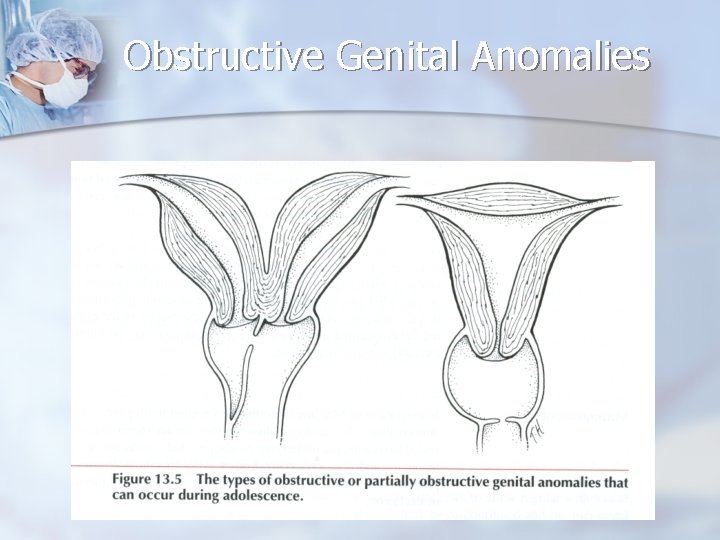
Obstructive Genital Anomalies
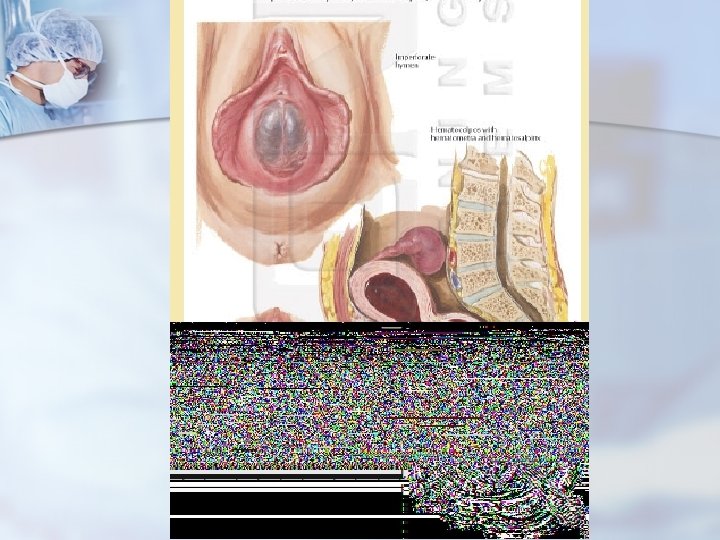
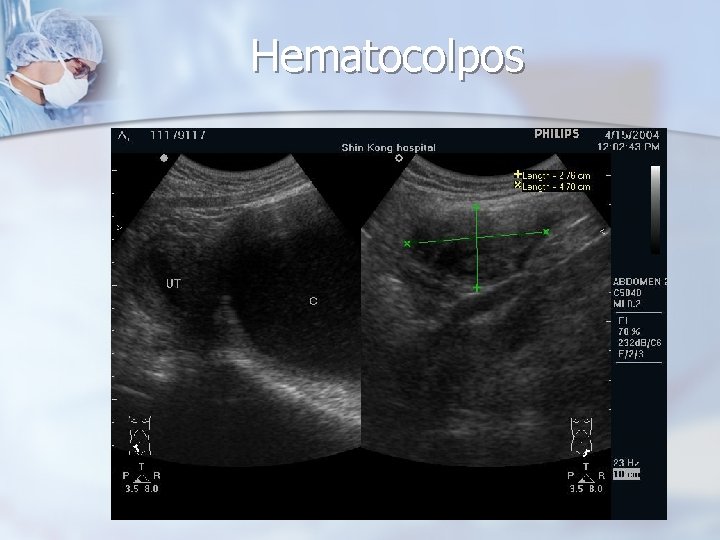
Hematocolpos
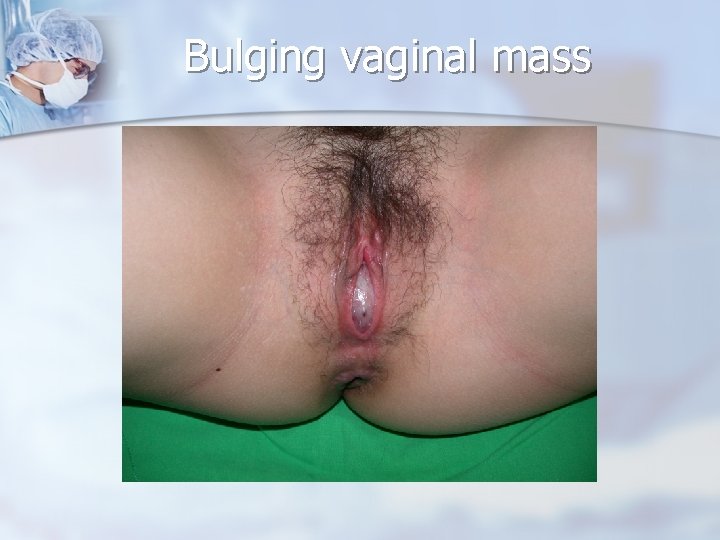
Bulging vaginal mass
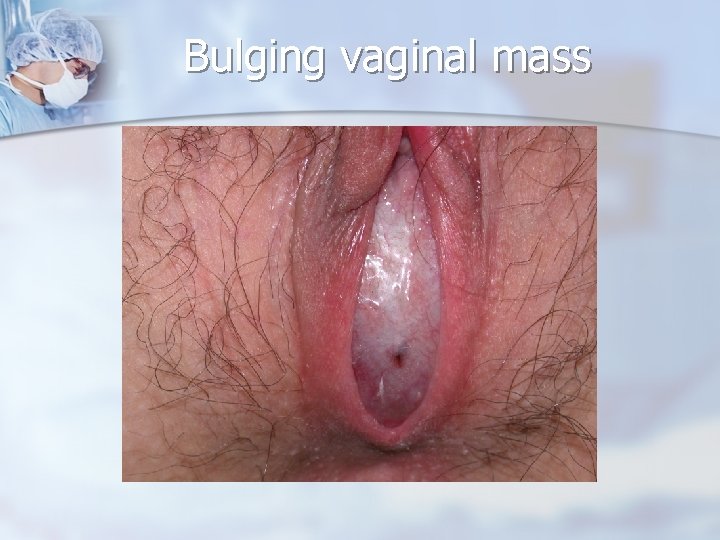
Bulging vaginal mass
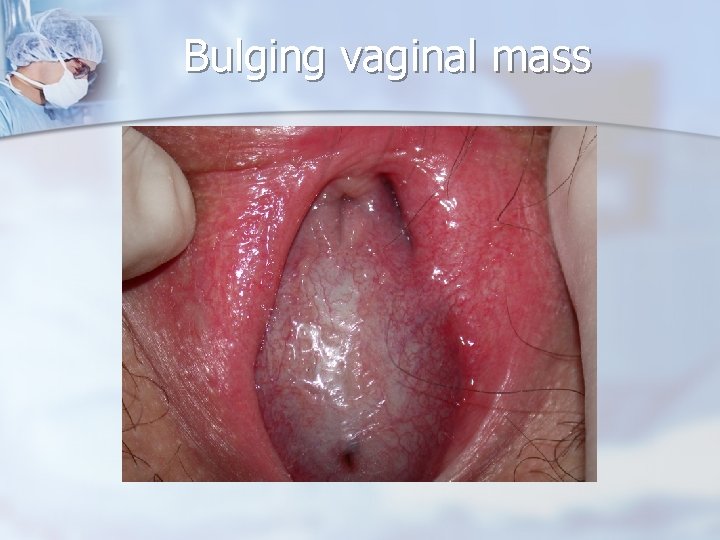
Bulging vaginal mass
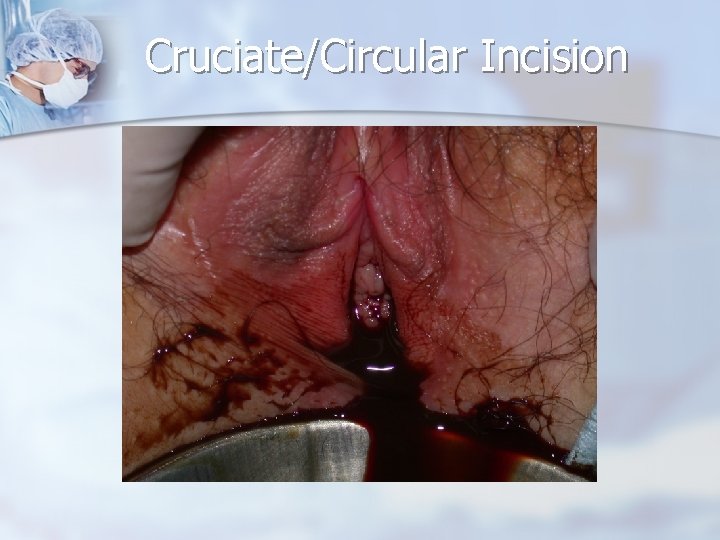
Cruciate/Circular Incision
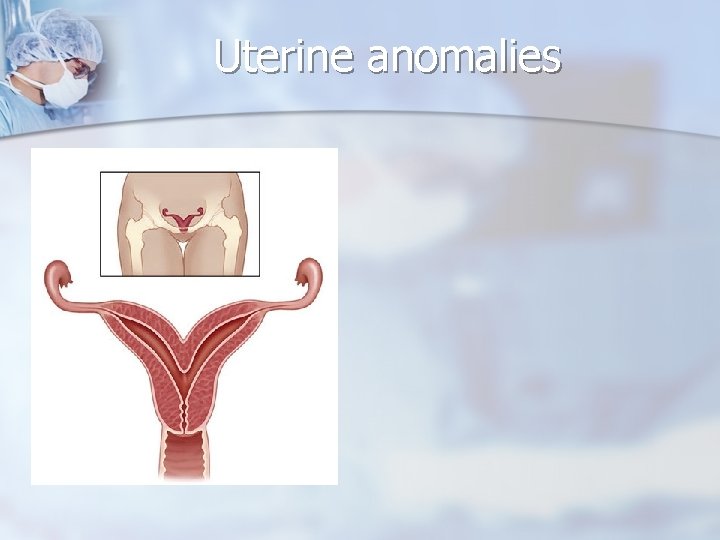
Uterine anomalies

Adolescent Age Group - Inflammatory Masses n n n Adolescents have the highest rates of PID An adolescent who has pelvic pain may be found to have an inflammatory mass. The diagnosis is primarily clinical, based on the presence of lower abdominal, pelvic, and adnexal tenderness; cervical motion tenderness; a mucopurulent discharge; elevated temperature, white blood cell count, or sedimentation rate

Adolescent Age Group - Inflammatory Masses Associated with the risks STD n Inflammatory masses may consist of n n Tuboovarian complex n Tuboovarian abscess n Pyosalpinx n Hydrosalpinx
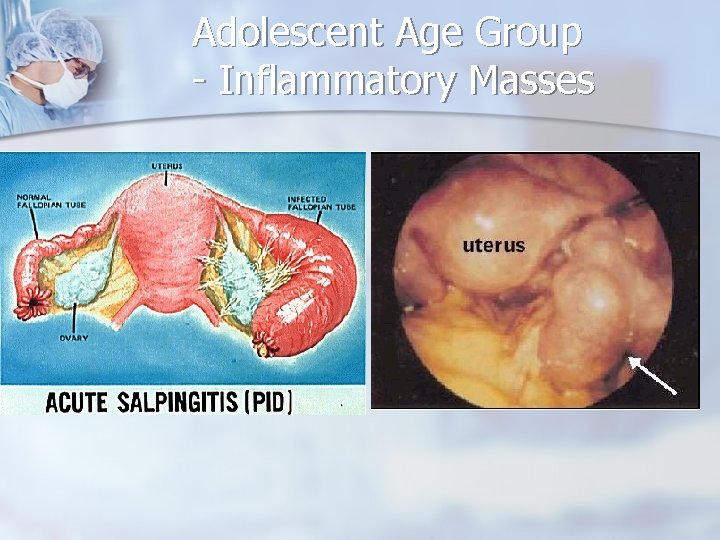
Adolescent Age Group - Inflammatory Masses

Adolescent Age Group - Pregnancy n n Pregnancy should always be considered Adolescents more likely to deny the possibility of pregnancy. Ectopic pregnancies may cause pelvic pain and an adnexal mass. Quantitative measurements of b-h. CG, ectopic pregnancies are being discovered before rupture, allowing conservative management with laparoscopic surgery or medical therapy with methotrexate.

Adolescent Age Group - Diagnosis A history and pelvic examination n Anxiety associated with a first pelvic examination n Issues of confidentiality related to questions of sexual activity. n Always include a pregnancy test (regardless of stated sexual activity) n CBC/DC. n Tumor markers (AFP, h. CG…) n

Adolescent Age Group - Diagnosis Ultrasonography. n TVS provide more detail than Abd sonography n TVS may not be well tolerated by adolescents n CT or MRI n

Adolescent Age Group - Management Laparoscopy n Acute PID to confirm the diagnosis n Persisted symptoms in patient with the clinical diagnosis of PID or TOA n The surgical management of inflammatory masses is rarely necessary in adolescents, except ruptured TOA or failure of medical management with broad-spectrum antibiotics n

Reproductive Age Group n Differential n Uterine Diagnosis Masses n Ovarian Masses n Nonneoplastic Ovarian Masses n Other Benign Masses n Neoplastic Masses n Other Adnexal Masses

Reproductive Age Group - Uterine Masses Uterine leiomyomas - most common benign uterine tumors. n Usually diagnosed on physical examination. n Incidence: 20% (reproductive age) n 40% to 50% of women older than 35 years of age. n
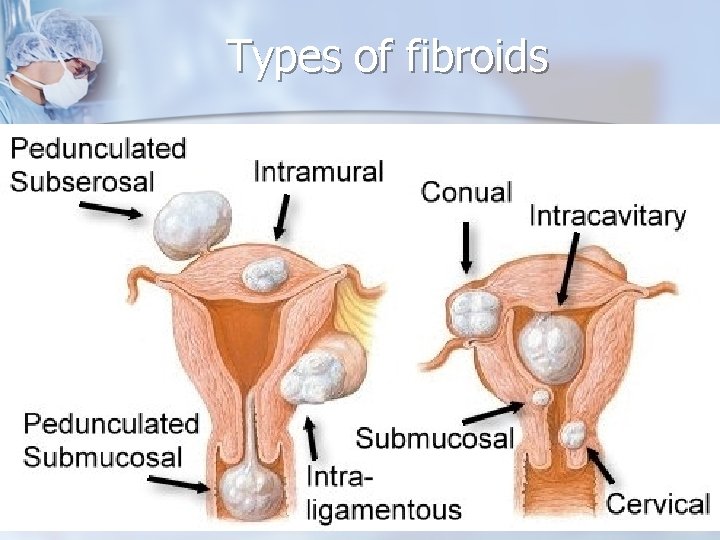
Types of fibroids

Reproductive Age Group - Uterine Masses Malignant degeneration < 0. 5% n Leiomyosarcoma -rare malignant neoplasm composed of cells that have smooth muscle differentiation. n Most diagnoses are determined (postoperatively) after microscopic examination. n

Reproductive Age Group - Uterine Masses n Symptoms n Menorrhagia n Chronic pelvic pain n Acute pain n Urinary symptoms: Frequency, Partial ureteral obstruction, complete urethral obstruction n Infertility

Reproductive Age Group - Uterine Masses n Symptoms n Rectosigmoid compression, with constipation or intestinal obstruction n Prolapse of a pedunculated submucous tumor n Venous stasis of the lower extremities and possible thrombophlebitis secondary to pelvic compression n Polycythemia n Ascites

Reproductive Age Group - Uterine Masses Management of Leiomyomas n Nonsurgical Management n n Intervention is reserved for specific indications and symptoms. n Periodic examinations n Gn. RH agonists

Reproductive Age Group - Uterine Masses Gn. RH agonists n 40% to 60% decrease in uterine volume n Hypoestrogenism: reversible bone loss and symptoms: hot flashes. n limited to short-term use n Regrowth of leiomyomas within a few months after stopping therapy in about 1/2 women treated

Reproductive Age Group - Uterine Masses n n n n Indications for Gn. RH agonist: 1. Preservation of fertility in women with large leiomyomas before attempting conception, or preoperative treatment before myomectomy 2. Treatment of anemia to allow recovery of normal hemoglobin levels before surgical management, minimizing the need for transfusion or allowing autologous blood donation 3. Treatment of women approaching menopause in an effort to avoid surgery 4. Preoperative treatment of large leiomyomas to make vaginal hysterectomy, hysteroscopic resection or ablation, or laparoscopic destruction more feasible 5. Treatment of women with medical contraindications to surgery 6. Treatment of women with personal or medical indications for delaying surgery.

Reproductive Age Group - Uterine Masses Indications for surgery : n n n Abnormal uterine bleeding - anemia, unresponsive to hormonal management Chronic pain with severe dysmenorrhea, dyspareunia, or lower abdominal pressure or pain Acute pain, as in torsion of a pedunculated leiomyoma, or prolapsing submucosal fibroid Urinary symptoms or signs such as hydronephrosis after complete evaluation Infertility, with leiomyomas as the only abnormal finding Markedly enlarged uterine size with compression symptoms or discomfort.

Reproductive Age Group - Uterine Masses n Indications for surgery because of the inability to exclude uterine sarcoma: n Rapid enlargement of the uterus during premenopausal years n or any increase in uterine size in a postmenopausal woman

Reproductive Age Group - Uterine Masses n n n Hysterectomy has long been viewed as the definitive management of symptomatic uterine leiomyomas. Myomectomy is an alternative to hysterectomy for patients who desire childbearing, who are young, or who prefer that the uterus be retained. Recent studies suggest that the morbidity of abdominal myomectomy and hysterectomy are similar Laparoscopic myomectomy minimizes the size of the abdominal incision, although several small incisions are required.

Reproductive Age Group - Uterine Masses n n Vaginal myomectomy is indicated in the case of a prolapsed pedunculated submucous fibroid. Hysteroscopic resection of small submucous leiomyomas The recurrence risk for leiomyomas has been reported to be as high as 50% after myomectomy, with up to 1/3 requiring repeat surgery. Endometrial ablation can decrease bleeding for women with primary intramural fibroid
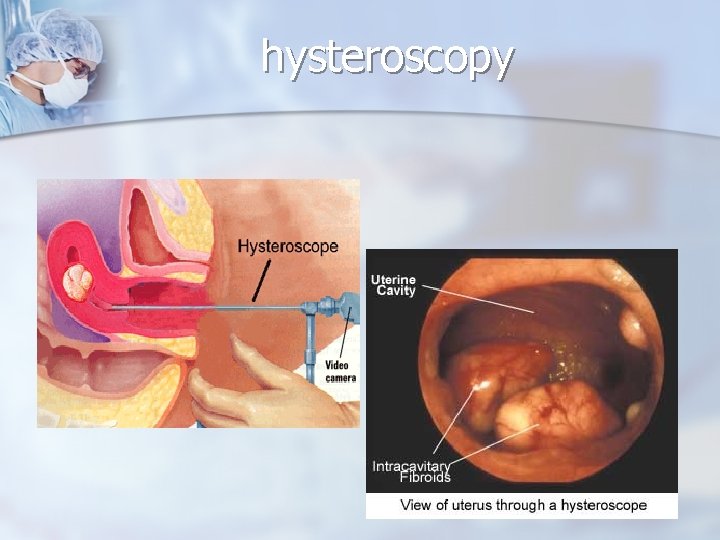
hysteroscopy

Reproductive Age Group - Uterine Masses n Nonextirpative approaches: n n n Myolysis - use of lasers to coagulate or needle electrodes to deliver an electrical current to individual leiomyomas Uterine artery embolization - have serious consequences, including infection, massive bleeding, and necrosis requiring emergency surgery. Still consider investigational. Long-term safety and efficacy have not yet been demonstrated.

Reproductive Age Group - Ovarian Masses n n During the reproductive years, the most common ovarian masses are benign. About 2/3 ovarian tumors are encountered during the reproductive years. Most ovarian tumors (80% to 85%) are benign, and 2/3 of these occur in women between 20 and 44 y/o. The chance that a primary ovarian tumor is malignant in a patient < 45 y/o is less than 1 in 15.

Reproductive Age Group - Ovarian Masses Pelvic findings in patients with benign and malignant tumors differ. n Benign - unilateral, cystic, mobile, and smooth n Malignant -bilateral, solid, fixed, irregular, and associated with ascites, cul-de-sac nodules, and a rapid rate of growth n

Reproductive Age Group - Nonneoplastic Ovarian Masses n Functional ovarian cysts include n n follicular cysts n corpus luteum cysts n theca lutein cysts n All are benign and usually do not cause symptoms or require surgical management.

Reproductive Age Group - Nonneoplastic Ovarian Masses n Follicular cyst n the most common functional cyst n cystic follicle can be defined as follicular cyst when diameter > 3 cm. n found incidental to pelvic examination n usually resolve in 4 to 8 weeks, seldom rupture causing pain and peritoneal signs

Reproductive Age Group - Nonneoplastic Ovarian Masses n Corpus luteum cysts n less common than follicular cysts. n may rupture, leading to a hemoperitoneum and requiring surgical management. n High risk - anticoagulant therapy. n Rupture - more often on the right side and during intercourse. n Most ruptures on cycle days 20 to 26.

Reproductive Age Group - Nonneoplastic Ovarian Masses n n n Combination monophasic oral contraceptive therapy has been reported to markedly reduce the risk of functional ovarian cysts. It appears that, in comparison with previously available higher-dose pills, the effect of cyst suppression with current lowdose oral contraceptives is attenuated. Most studies have suggested that the use of triphasic oral contraceptives is not associated with an appreciable increased risk of functional ovarian cysts.

Reproductive Age Group - Ovarian Masses Other Benign Masses n Women with endometriosis may develop ovarian endometriomas (“chocolate” cysts), which can enlarge to 6 to 8 cm in size. n A mass that does not resolve with observation may be an endometrioma. n
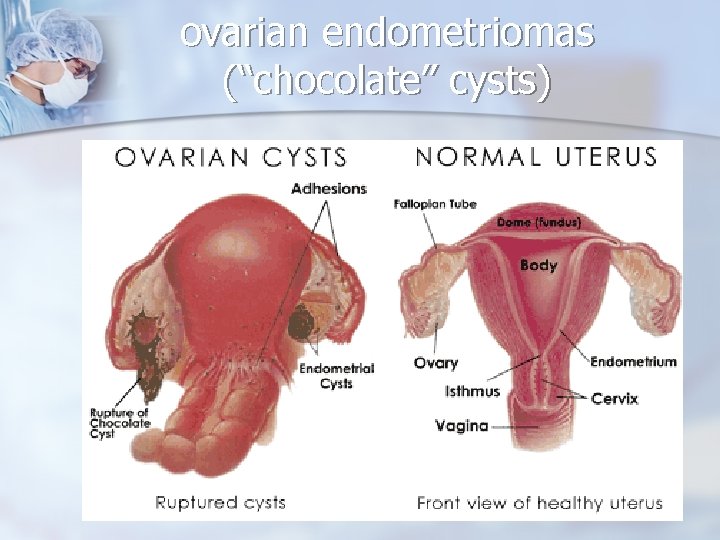
ovarian endometriomas (“chocolate” cysts)
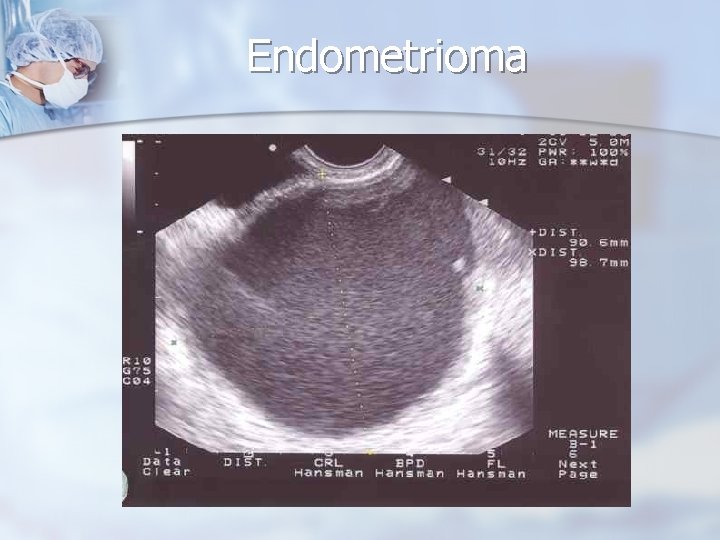
Endometrioma
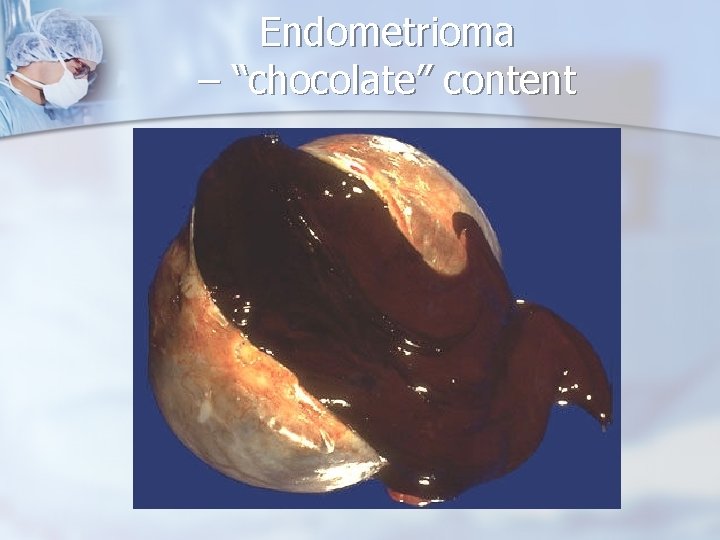
Endometrioma – “chocolate” content

Reproductive Age Group - Ovarian Masses n n n In one study, 257 volunteers were examined with ultrasonography; 22% were found to have polycystic ovaries. The finding of bilateral generously sized ovaries on examination or polycystic ovaries on ultrasonographic examination should prompt evaluation for the full-blown syndrome which includes hyperandrogenism and chronic anovulation as well as polycystic ovaries. Therapy for PCOS is medical and generally not surgical.
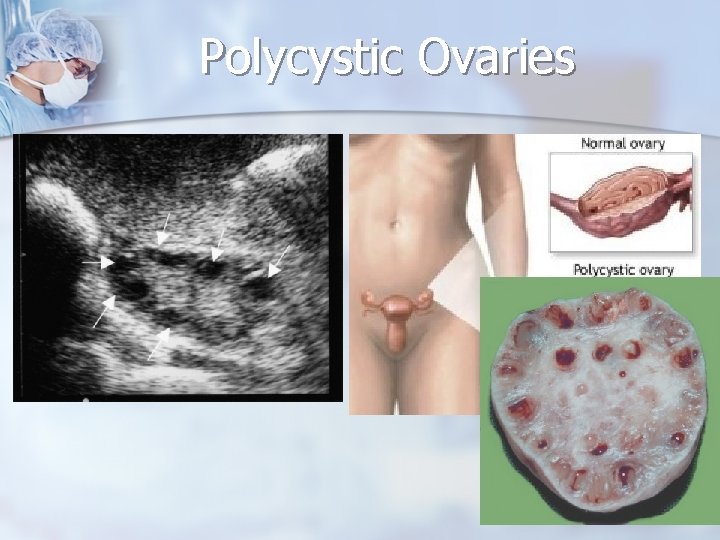
Polycystic Ovaries

Reproductive Age Group - Neoplastic Ovarian Masses n More than 80% of benign cystic teratomas (dermoid cysts) occur during the reproductive years, although dermoid cysts have a wider age distribution than other ovarian germ cell tumors.

Reproductive Age Group - Neoplastic Ovarian Masses Benign cystic teratomas have an admixture of elements. n comprising more than a single cell type derived from more than one germ layer, usually all 3. n Cells differentiate along various germ lines, essentially recapitulating any tissue of the body. Examples include hair, teeth, fat, skin, muscle, and endocrine tissue n

Reproductive Age Group - Neoplastic Ovarian Masses Malignant transformation: < 2% n Bilateral: 10% n Torsion: 15%, it occurs more frequently than with ovarian tumors because the high-fat content allowing them to float within the abdominal and pelvic cavity. n As a result, frequently is anterior in location. n

Reproductive Age Group - Neoplastic Ovarian Masses n n Cystectomy is almost always possible, even if it appears that only a small amount of ovarian tissue remains. Preserving a small amount of ovarian cortex in a young patient with a benign lesion is preferable Laparoscopic cystectomy is often possible, Intraoperative spill of tumor contents is rarely a cause of complications.
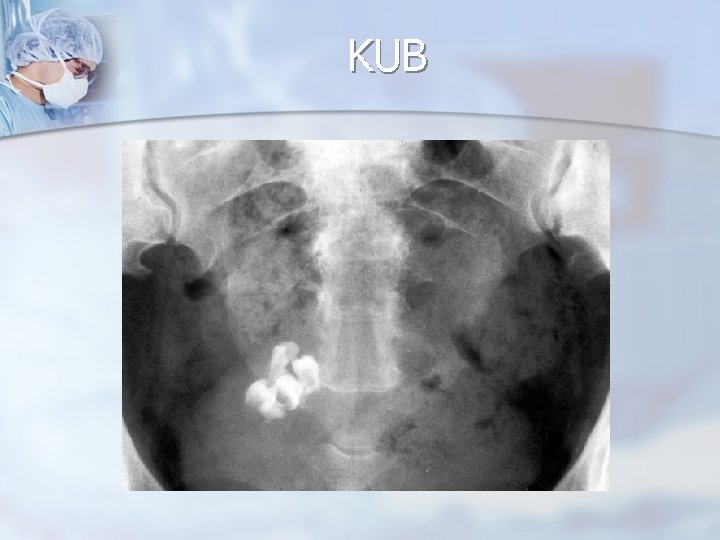
KUB
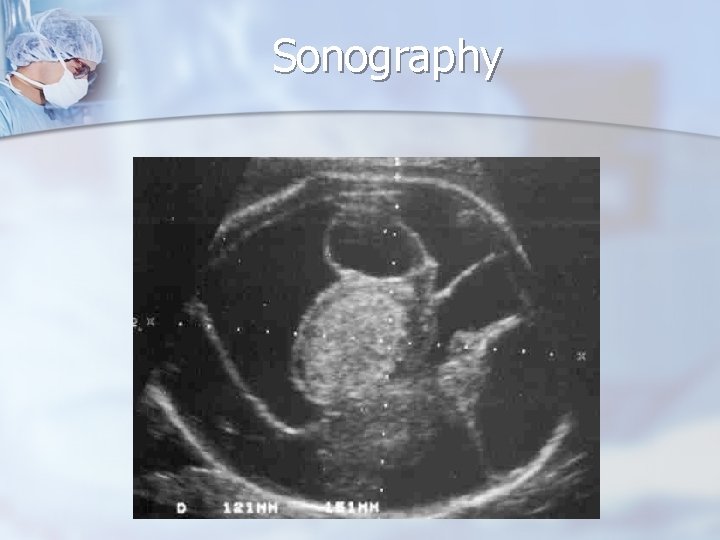
Sonography
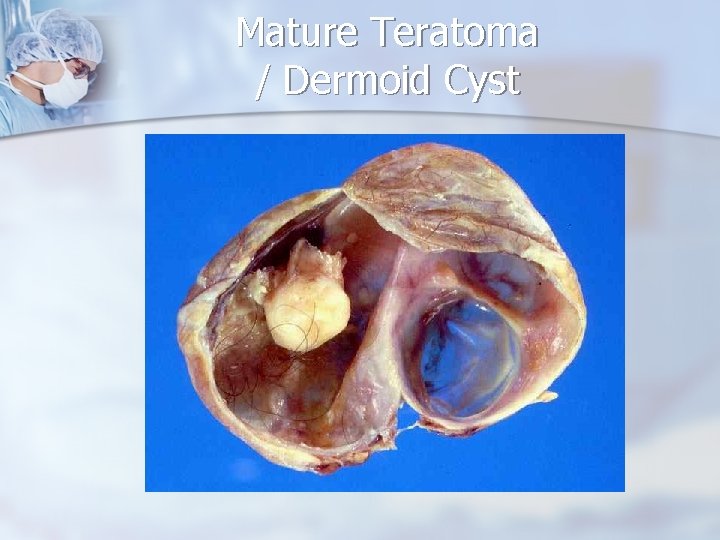
Mature Teratoma / Dermoid Cyst
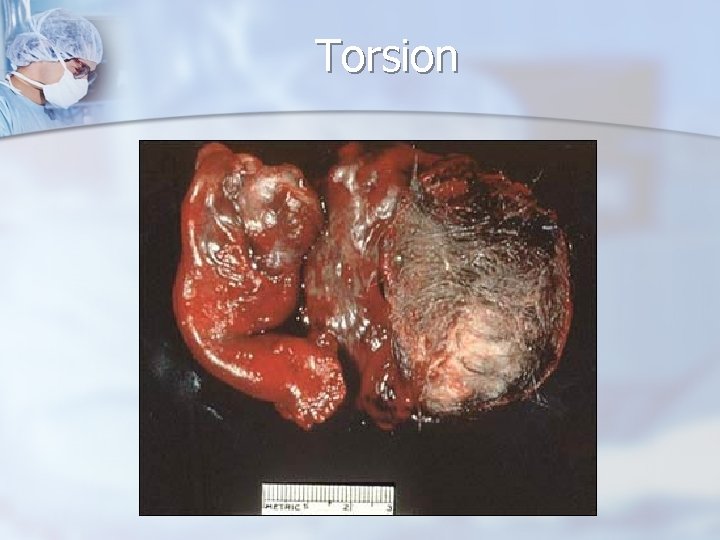
Torsion
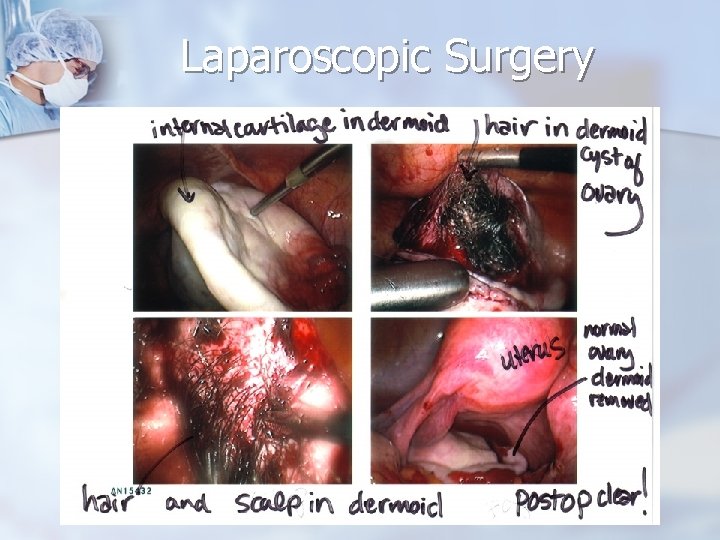
Laparoscopic Surgery
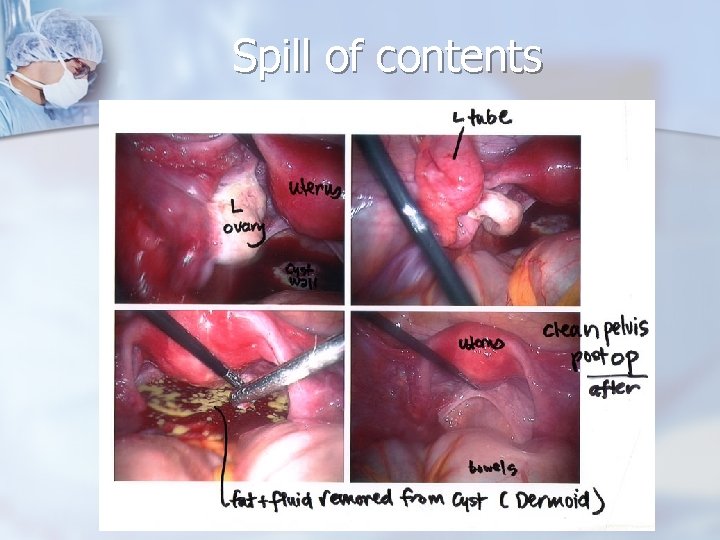
Spill of contents

Reproductive Age Group - Neoplastic Ovarian Masses n serous cystadenomas n The risk of epithelial tumors increases with age n 5% to 10% have borderline malignant potential n 20% to 25% are malignant n often multilocular, sometimes with papillary components.

Reproductive Age Group - Neoplastic Ovarian Masses n n n Surface epithelial cells secrete serous fluid, resulting in a watery cyst content. Psammoma bodies areas of fine calcific granulation, may be scattered within the tumor and are visible on radiograph. Frozen section is necessary to distinguish between benign, borderline, and malignant serous tumors, because gross examination alone cannot make this distinction.
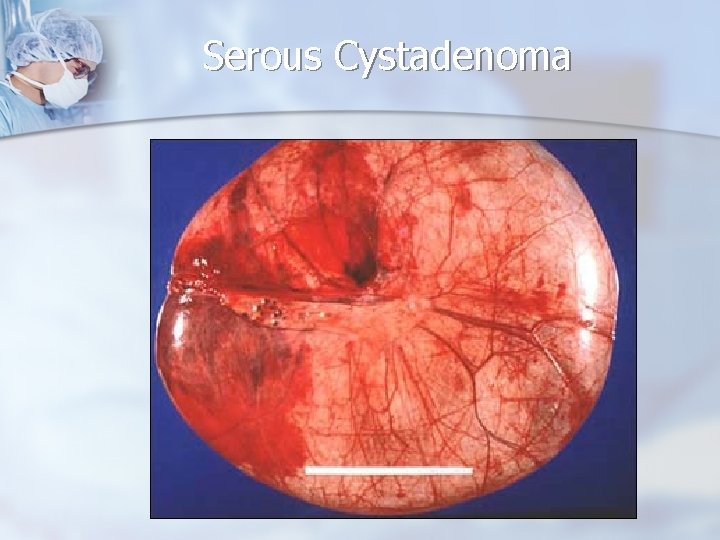
Serous Cystadenoma
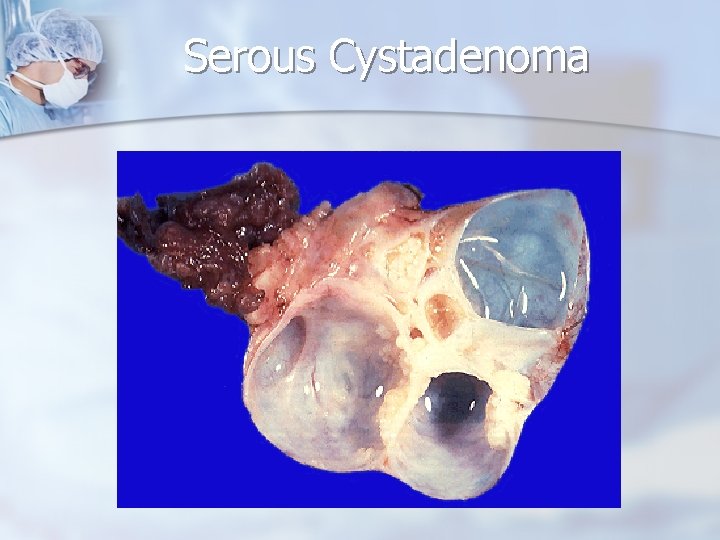
Serous Cystadenoma
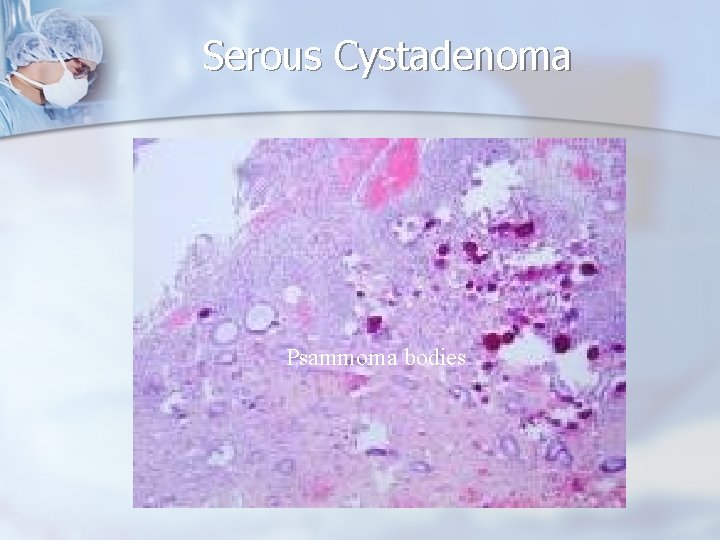
Serous Cystadenoma Psammoma bodies

Reproductive Age Group - Neoplastic Ovarian Masses n Mucinous n may ovarian tumors grow to large dimensions n lobulated, smooth surface, multilocular n Bilateral in up to 10% of cases n Five to ten percent of mucinous ovarian tumors are malignant.

Reproductive Age Group - Neoplastic Ovarian Masses Mucoid material is present within the cystic loculations n may be difficult to distinguish histologically from metastatic gastrointestinal malignancies n
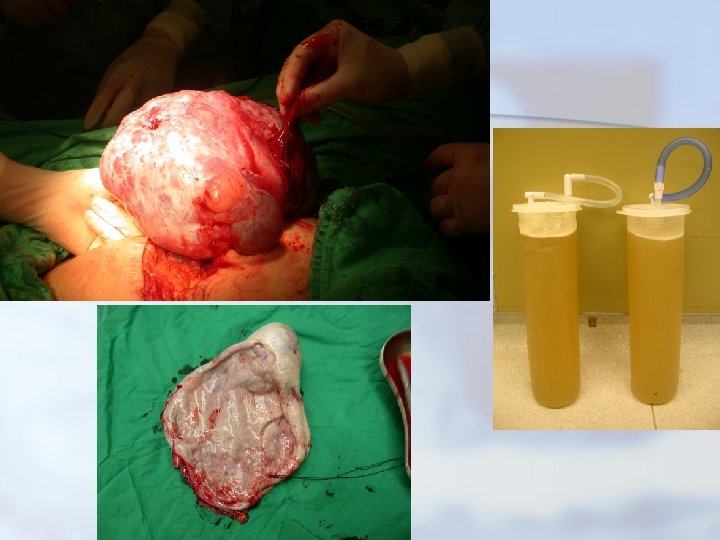
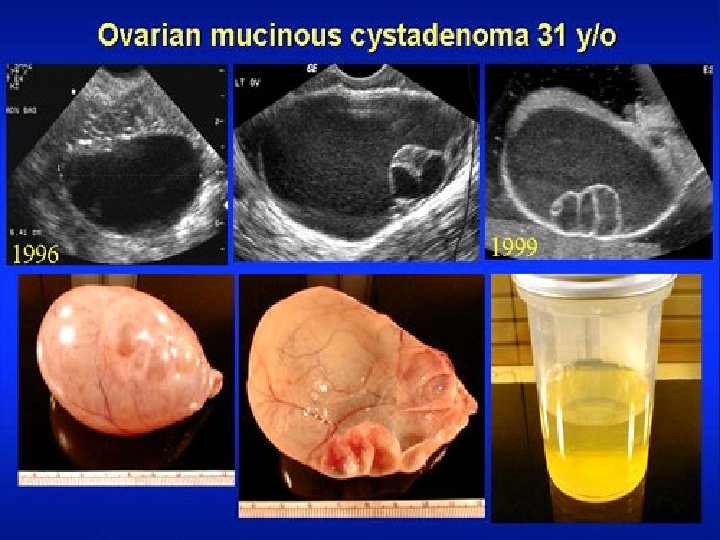

Reproductive Age Group - Neoplastic Ovarian Masses n Other benign ovarian tumors include fibromas (a focus of stromal cells), Brenner tumors (which appear grossly similar to fibromas and which are frequently found incidentally), and mixed forms of tumors such as the cystadenofibroma.
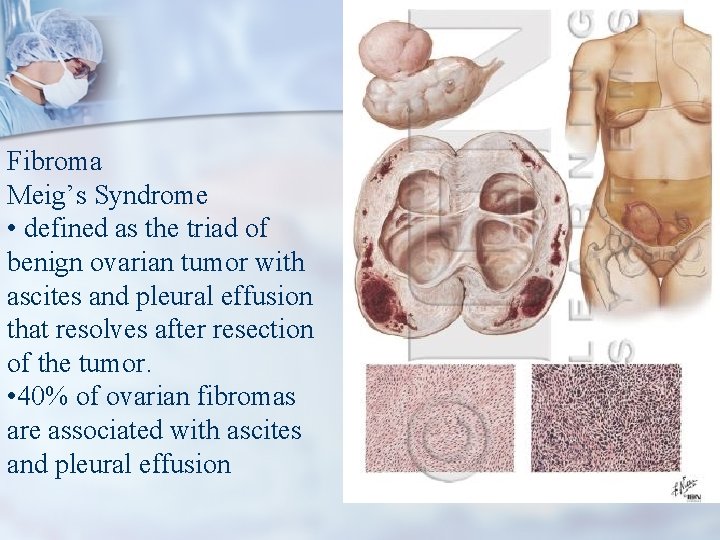
Fibroma Meig’s Syndrome • defined as the triad of benign ovarian tumor with ascites and pleural effusion that resolves after resection of the tumor. • 40% of ovarian fibromas are associated with ascites and pleural effusion
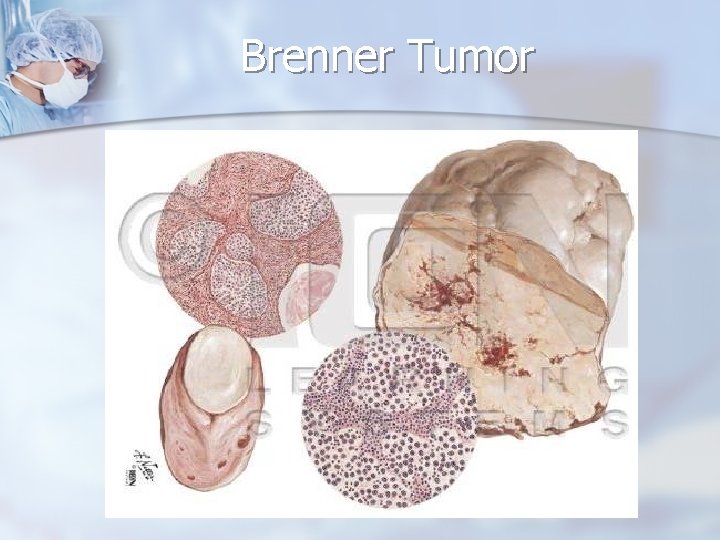
Brenner Tumor
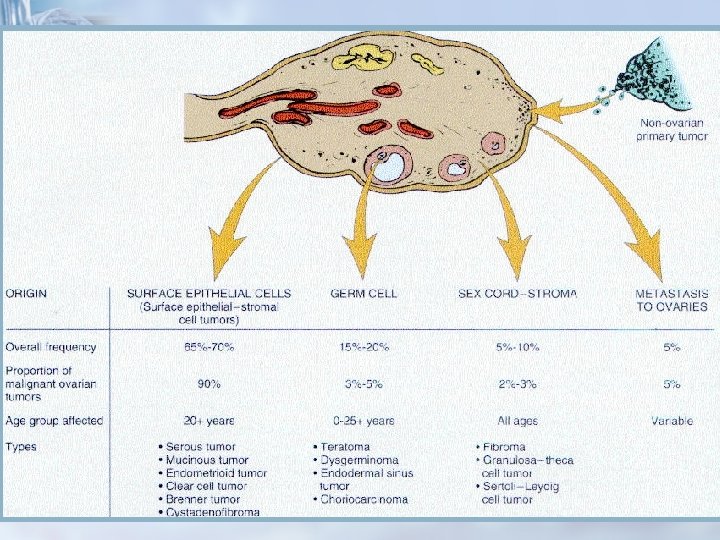

Postmenopausal Age Group Differential Diagnosis of Ovarian Masses n n During the postmenopausal years, the ovaries become smaller. Before menopause, the dimensions are approximately 3. 5 × 2 × 1. 5 cm. In early menopause, the ovaries are approximately 2 × 1. 5 × 0. 5 cm. In late menopause, they are even smaller: 1. 5 × 0. 75 × 0. 5 cm.

Postmenopausal Age Group n n Barber has described the postmenopausal palpable ovary (PMPO) syndrome, suggesting that any ovary that is palpable on examination beyond the menopause is abnormal and deserves evaluation Ovarian cancer is predominantly a disease of postmenopausal women; the incidence increases with age, and the average patient age is about 56 to 60 years
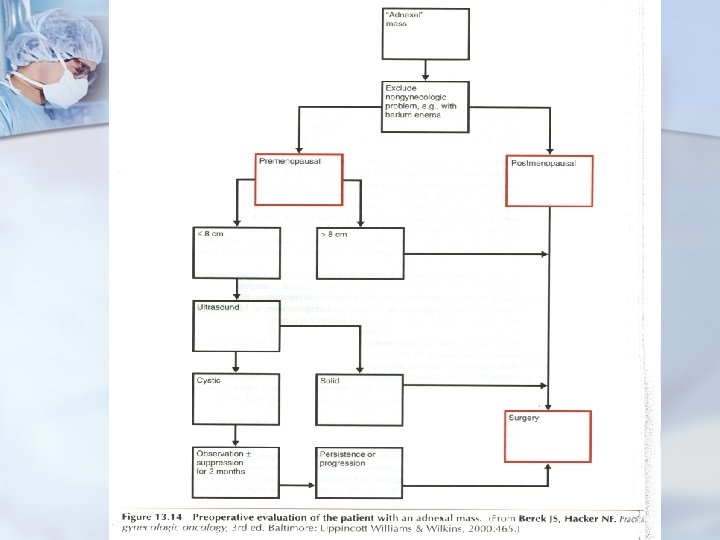

References Novak's Gynecology: Jonathan S. Berek, 2002 by Lippincott Williams & Wilkins. 13/e n Atlas of Human Anatomy, Student Edition, 3 rd Edition By Frank H. Netter, MD n
- Slides: 88