Benign prostatic hyperplasia BPH BPH is the most

Benign prostatic hyperplasia BPH

*BPH is the most common benign tumor in men. *Its age related disease. For Pathololgy mean cellular proliferation of stromal and epithelial elements of prostate For Radiologist mean an enlarged prostate > 30 cm For Urologsit represent acollection of lower urinary tract symptoms (LUTs) that develop in male population in association with aging and prostatic enlargement Pathology. The prostate composed of -stroma (smooth muscle & fibrous tissue) and -epithelium. BPH can arise from any one of them or in combination

Etiology. BPH need both Age +Androgen to develop Increase in cell number • Epithelial and stromal proliferation. • Impaired programmed cell death (apoptosis) Proposed factors that play role in aetiology include üAndrogens üEstrogens üStromal-epithelial interactions üGrowth factors üNeurotransmitters üGenetic(autosomal dominant) family history usually effect younger age group

Anatomically the prostate had 3 zones -peripheral (70%) commonest site for Ca, -central (25%) around ejaculatory duct, & -transitional (5%) periurethral. BPH uniformly originate from the transitional zone & as the nodule enlarge compress the outer zones of the prostate resulting in surgical capsule. Pathophysiology Increase urethral pressure lead tobladder wall hypertrophy so First : the changes that lead to decrease compliance causing frequency and urgency

Second : changes associated with decreased contractility causing decrease force of urinary stream, hestancy, intermittency and increase resudial volume Clinical features Either obstructive or irritative. obstructive symptoms -hesitancy, -decrease force & caliber of stream, -sensation of incomplete bladder emptying, -double voiding -straining to urinate, & post void dribbling.
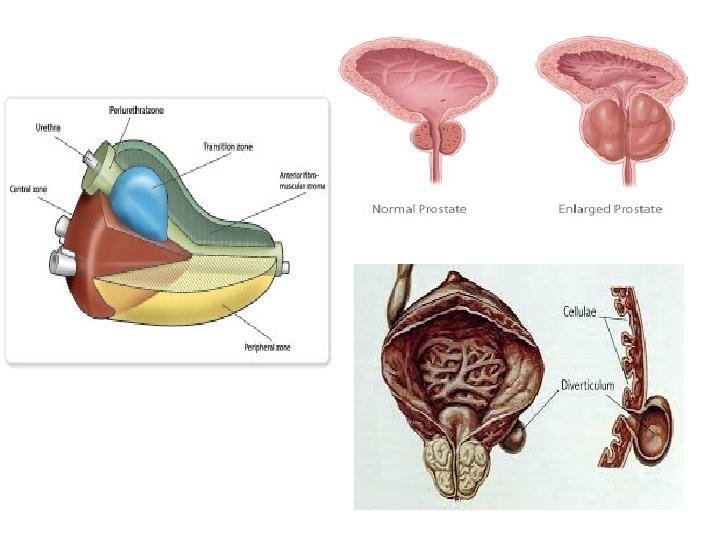

Irritative symptoms urgency, frequency, & nocturia. * The amount of post void residual urine is extremely variable in sequential evaluation of same patient. DRE, used to determine the size, consistency of the prostate -a smooth firm usually BPH while -induration signify the possibility of Ca & need further evaluation.

-retention may occur usually precipitated by prostatic infection or infarction, ingestion of diuretic, anticholenergic, antidepressant Symptom not related to prostatic size Investigation q. GUE, infection & hematuria. q. Renal function : b. urea & s. creatinine. q. PSA : is optional. prostatic tumor marker q Imaging : IVU &U/S is some time recommended. q. Cystoscopy. Used to choose surgical approach when surgery is indicated.

D. Dx. Obstructive condition of lower tract like -urethral stricture, -bladder neck contracture, -bladder stone, & -Ca prostate. irritative -UTI, -CIS, & -neurogenic bladder

Treatment Options v Watchful waiting v Medication v Surgical approaches TURP Invasive open procedures Minimal invasive A-Watchful waiting Idea is only 5% of BPH patients will develop retention • Mild symptoms with not very active life style • Follow up every 3 -6 months • Offer suggestions that reduce symptoms

B-Medical therapy. 1 -Alpha blocker: The human prostate & bladder neck contain alph-1 a receptors. Alpha blocker lead to smooth muscle relaxation & dilatation of bladder neck. Alpha blocker either nonselective act on alpha like phenoxybenzamine Selective which either short acting e. g prazosin or, long acting e. g terazosin & doxazosin. These need dose titration to decrease their side effect

side effect include -orthostatic hypotension, -dizziness, -tiredness, -retrograde ejaculation, -rhinitis, & -headach. Highly selective act on alpha 1 a receptors like Tamsolusin and Silodosin in both no need for dose titration because it had fewer side effect. mostly causing retro grad ejaculation

2 - 5 -alpa reductase inhibitor Finasteride and dutasteride are 5 alpha reductase inhibitors that block the conversion of testosterone to dihydrotestosteron. This drug act on epithelial component (adenoma) of the prostate reduce the size of the gland (20% reduction of weight in 6 months). side effect -decrease libido & -reduce PSA level to 50% complicating cancer detection.

B-Surgical management. Absolutetely Indicated in 1 -refractory retention (after at least 1 trial of catheter removal), 2 -recurrent UTI due to PBH 3 -recurrent gross hematuria, due to PBH 4 -bladder stone, 5 -renal insufficiency 6 -bladder diverticulum 7 - failure of medical treatment (medication not improving the quality of life) *provide these are from BPH.

1 -TURP (transurethral resection of the prostate) -resection of the prostate endoscopically into small pieces which removed by bladder wash. -Used in 95% of BPH. complications. Immediate -Bleeding -Capsular perforation with fluid extravasation -Infaction -TURP syndrom resulting from hypervolemic hyponatremic state due to absorption of hypotonic irrigating solution. Manifested by nausea, vomiting, confusion, hypertension, bradycardia, & visual disturbance

Late complication • Urethral stricture • Bladder neck contracture • Retrograde ejaculation • Impotence • Incontinence

2 -open simple prostatectomy. Indicated when TURP not performed due to 1 - large prostate >100 g. 2 - concomitant bladder pathology like stone or diverticulum, & 3 - when dorsal lithotomy positioning is not possible. Its either transvesical or retropubic.

3 -minimal invasiae therapy. 1 - laser therapy, 2 - electrovaporization of the prostate, 3 - transurethral needle ablation, 4 - high intensity focused ultrasound, 5 - intraurethral stent, 6 - balloon dilation of the prostate.
- Slides: 18