Benign Prostatic Hyperplasia BPH and Prostatitis Matthew Lane

Benign Prostatic Hyperplasia (BPH) and Prostatitis Matthew Lane, Pharm. D, BCPS Associate Professor University of Kentucky

BPH • Common cause of urinary dysfunctional symptoms in elderly men • Due to proliferation of stromal and epithelial cells of the prostate gland

BPH • 75% of men who live up to age of 70 will experience symptoms • No evidence disorder predisposes patients to developing prostate cancer

Etiology • Testosterone metabolized to dihydrotestosterone (DHT) by 5 -alpha reductase • 5 -alpha reductase contained in prostatic epithelial cells • DHT is the obligate androgen responsible for normal and hyperplastic prostatic growth • Overactivity of bladder (50% incidence with BPH)

Clinical Presentation • Obstructive – Hesitancy, decrease in urinary force, urinary stream intermittency, terminal dribbling and incomplete bladder emptying • Irritative – Nocturia and daytime urinary frequency, urge incontinence and pain • Obstructive symptoms associated more with enlarged prostate, while irritative symptoms suggest voiding dysfunction

Clinical Presentation • Objective findings – Abdominal tenderness – Enlarged bladder – Enlarged, firm, rubbery prostate • Differential diagnosis – Urinary tract infection – Prostate CA – Hydronephrosis – bladder contractility or outlet obstruction

Studies • Urinalysis – Obtain urine specimen before digital rectal examination (DRE) • DRE – Large, palpable prostate with smooth mucosal surface rectally appreciated

Prostate CA • DRE – Presence of hard nodules or induration suggest prostate CA • Intravenous pyelogram (IVP) warranted only if hematuria present

Urodynamic Evaluation • Assesses urinary flow rate, bladder volume, detrusor pressure and visualization of voiding • Peak urinary flow rate is noninvasive and useful monitoring parameter • Cystoscopy – Used to rule out tumors and stones – Required only if hematuria or pelvic pain with voiding present
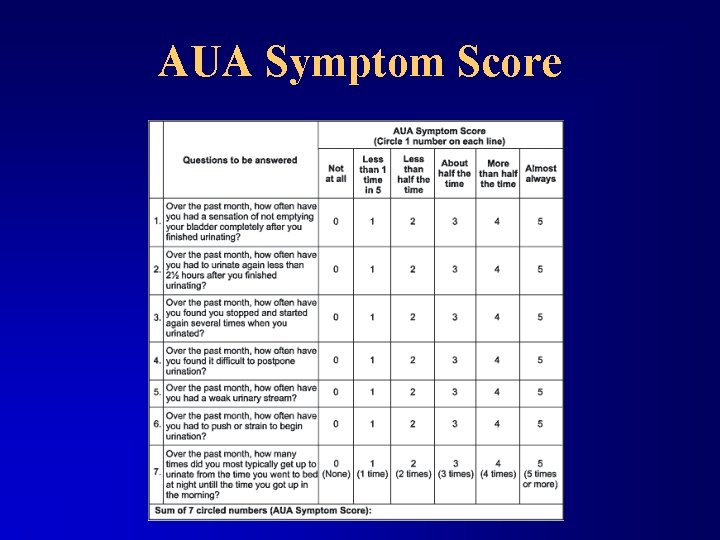
AUA Symptom Score

Complications • Urinary incontinence – With advanced disease secondary to large residual volume • Hydronephrosis with renal damage – Associated with abdominal discomfort and flank pain during voiding • Acute urinary retention – Alcohol, anticholinergics, alpha-adrenergic agents and neuroleptics may precipitate

Treatment • Goal is to relieve symptoms, maintain quality of life and prevent complications • Nonpharmacologic strategies – Transurethral resection of the prostate (TURP) – Transurethral incision of the prostate (TUIP) – Transurethral dilation of the prostate (TUDP) – Urethral stent

TURP • Treatment of choice for large prostate gland (> 30 g) +/- complications • Significant relief of symptoms in 75 -86% of patients up to 7 years after procedure • Initial adverse effects include postsurgical TURP syndrome (2%), voiding problems, hemorrhage and UTIs • Impotence, retrograde ejaculation and urinary incontinence may occur

TUIP and TUDP • Reasonable alternatives for men with smaller prostates (< 30 g) that cause bladder outlet obstruction • Incisions or balloon catheter relieve outlet obstruction and preserve antegrade ejaculation • Good choice in high-risk surgical patients (e. g. elderly) as it can be performed under local anesthesia

Drug Therapy • Used initially to treat mild to moderate symptoms of prostatism • Alpha-blockers – Prostatic capsule, BPH adenoma and bladder neck rich with alpha 1 receptors

Alpha Blockers • Agents reduce smooth muscle tone of prostate, bladder neck, urethra, improve voiding function and decrease symptoms • Receptor alpha 1 A subtype most important • Relieves irritative symptoms

Alpha-Blockers • Shown in clinical trials to improve urinary flow rate (3 m. L/s) and BPH symptoms (40%) • Most agents must be titrated in stepwise fashion due to postural hypotension and syncope • Administer first dose at bedtime • Blood pressure changes usually small in normotensive men

Alpha-Blockers • Patients experience improvement in symptoms within several weeks – Assess initial response after 1 month • Common side effects include dizziness and nasal congestion • Regimens – Terazosin 1 -20 mg/d – Doxazosin 1 -8 mg/d

Alpha Blockers • Tamsulosin – Higher affinity for alpha 1 A receptors potentially causing less dizziness and postural hypotension (10 x more specific for prostate than peripheral receptors) – Stepwise titration not necessary – 0. 4 -0. 8 mg/d (maximum benefit at 0. 4 mg/d) – Significant increase in ejaculatory disturbances – Not indicated for treatment of hypertension – Benefits seen over first few days/wk.

Alpha Blockers • Alfuzosin – Uroselective alpha adrenergic selective when used in the current extended release formulation – Lowest incidence of hypotension – Low risk of sexual side effects, unlike tamsulosin – Dosing: 10 mg extended release tab daily

Alpha Blockers • Silodosin (Rapaflo®) – Alpha 1 a receptor specific (minimal orthostasis effects) – Similar benefit in reducing LUTS compared to other agents – SE - Significant increase in ejaculatory disturbances – Dosing 8 mg/day with meal. • Dose reduce in renal insufficiency • Avoid strong CYP 3 A 4 inhibitors

5 -alpha Reductase Enzyme Inhibitors • 2 types of receptors – Type 1 located in skin and liver – Type 2 located in prostate • Blockage of DHT production leads to shrinkage of prostate and decreased LUTS • Advantageous in patients with large prostate size • Disadvantage – reduces PSA making cancer detection more challenging

Finasteride • Blocks conversion of testosterone to dihydrotestosterone by inhibiting 5 -alpha reductase enzyme (type II) • Long-term administration (5 mg/d) causes prostate shrinkage (25%) and is detected 3 -24 months after initiation • Improvement in urinary flow rate (2 m. L/s) and symptoms occur at 12 -18 months

Dutasteride • Inhibits both peripheral and prostate specific enzymes • High protein bound, high metabolism by CYT 3 A 4, t ½ - approx 5 weeks • Dosing - 0. 5 mg daily • Prostate size reduced 25. 7% @ 2 yrs • PSA reduced 50% @ 2 yrs • SE’s similar to finasteride • Dutasteride/Tamsulosin – Jalyn ®

VA Trial 359 • Compared terazosin, finasteride, terazosin + finasteride and placebo • Results – Terazosin superior to finasteride – Finasteride no more effective than placebo – Combination therapy was not synergistic • Subsequent meta-analysis of 6 finasteride clinical trials show agent only effective for prostates > 40 g

MTOPS • Evaluated combo alpha blockade and 5 AREI vs single agents and placebo • AUA scores declined 7 points during combo therapy over 4. 5 yrs. • Overall shows combo tx slows progression best • Demonstrates effectiveness of alpha blockers • Shows that prostate > 40 g and PSA > 4 respond best to combo tx. • Surgical rates similar between finasteride vs combo tx NEJM 2003; 349; 2387 -2398

Comb. AT Trial 4 year trial comparing tamsulosin, dutasteride or combo for moderate/severe BPH in 4000+ men Both arms using dutasteride were better at preventing acute urinary retention and need for prostate reduction sx. Reiterates men with enlarged prostates benefit best when using 5 AREI with or without alpha blocker • Eur Urol. 2010; 57(1): 123

Tadalafil • FDA approved for treatment of signs and symptoms of BPH • 5 mg daily • Comparable to tamsulosin in mild symptom control • Option for mild disease with concomitant erectile dysfunction • Cautions – Interaction with alpha blockers – St. Johns wort may decrease effectiveness

Approach to Drug Therapy • Patients with smaller prostates and significant symptoms should receive alpha-blocker agent alone • Patients with larger prostates (> 40 g) treated with alpha-blocker + finasteride to provide prompt symptom relief • Trials ongoing to assess treatment of overactive bladder (anticholinergics)

Other Agents • Flutamide – Nonsteroidal antiandrogen that inhibits binding of DHT to receptor – Limited effectiveness – Reserved for nonsurgical candidates, finasteride failures +/- alpha blocker therapy • Gn. RH agonists – High cost, toxicity and questionable effectiveness preclude use of leuprolide

Other Developments • Saw palmetto • Finasteride 1 mg/d – BPH prevention – Male-pattern baldness – Prostate CA prevention

• A 56 yo male with 2 year history of increasing voiding symptoms, his main complaint being he has to wake up multiple times nightly to urinate. • • AUA symptom score 18 • Peak flow rate: 15 ml • Post Void Residual: 10 ml • Prostate Volume: 25 ml • PSA level: 0. 9 ng/ml • • What would you recommend for initial treatment? • • A. None, recommend watchful waiting. • B. Terazosin • C. Finasteride • D. Terazosin and finasteride

Bacterial Prostatitis • Acute – Sudden onset of fever, tenderness and urinary/constitutional symptoms • Chronic – Urinating difficulty, low back pain, suprapubic discomfort – Recurring infection with same organism • Possible routes of infection are same as those of UTIs

Prostatitis • Gram-negative, enteric organism most frequent pathogens – E. coli occurring in 75% of cases • DRE reveals swollen, tender, warm, tense gland • Diagnosis made when number of bacteria in expressed prostatic secretions are 10 times that of urethral and midstream sample upon voiding

Treatment of Prostatitis • Acute – Trimethoprim-sulfamethoxazole – Fluoroquinolones – Cephalosporins – Duration of therapy 4 weeks to reduce risk of developing chronic prostatitis • Chronic – Cures rarely obtained – Trimethoprim and fluoroquinolones – Treat initially for 4 -6 weeks
- Slides: 35