Beltox Advanced Toxicology Seminar Clinical and other observations

Beltox Advanced Toxicology Seminar Clinical and other observations in animal toxicity studies Koen Van Deun

Outline • Clinical observations • Body weight , weight gain & food consumption • Ophthalmology • Other observations • Discussion & conclusion

Clinical observations (1) OECD 407, 408, 409, 451, 452, 453 • General clinical observations (health condition): at least once daily – preferably at the same time(s) each day – considering peak period of anticipated effects (peak time? ) • Moribundity & mortality: at least twice daily • Detailed clinical observations (outside the home cage): once before exposure & at least once a week – – • Changes in skin, fur, eyes, mucous membranes, secretions. . . Autonomic activity (e. g. piloerection, pupil size, respiration) Changes in gait, posture, response to handling Bizarre behaviour (e. g. self-mutilation, walking backwards)

Clinical observations (2) Volumetric pump Dosing Observation at dosing Computer Observation at peak period Balance • Additional observations in rodents: – Sensory reactivity to different stimuli: towards the end of the study auditory, visual & proprioceptive stimuli assessment of grip strength motor activity assessment – Functional observations (90 -day study; optional in 4 -week study)

Clinical observations (3) FDA Redbook 2000 • Individual records should be maintained for each animal – the time of onset and the characteristics and progression of any effects should be recorded, preferably using a scoring system. • Tumor development (long-term studies) – the time of onset, location, dimensions, appearance and progression of each grossly visible or palpable tumor should be recorded. • Toxic and pharmacologic signs during the study – may suggest the need for additional clinical tests or expanded post-mortem examinations.

Clinical observations (4) Examples • from the cage From the cage exterior Rats are sleeping. Hair coat normal. https: //www. aalaslearninglibrary. org Cage Wirelid off Rats are alert. Normal reaction.

Clinical observations (5) Examples • Handling Malocclusion Not test article related! Normal rat Sedation Test article related! Pharmacodynamic? Adverse? Chromodacryorrhea Dirty skin Skin lesions Test article related! Adverse!
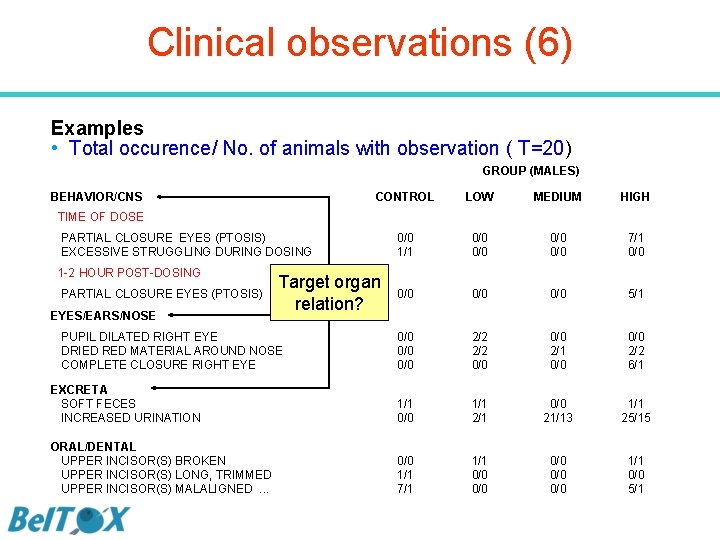
Clinical observations (6) Examples • Total occurence/ No. of animals with observation ( T=20) GROUP (MALES) BEHAVIOR/CNS CONTROL LOW MEDIUM HIGH 0/0 1/1 0/0 0/0 7/1 0/0 0/0 5/1 0/0 0/0 2/2 0/0 2/1 0/0 2/2 6/1 EXCRETA SOFT FECES INCREASED URINATION 1/1 0/0 1/1 2/1 0/0 21/13 1/1 25/15 ORAL/DENTAL UPPER INCISOR(S) BROKEN UPPER INCISOR(S) LONG, TRIMMED UPPER INCISOR(S) MALALIGNED. . . 0/0 1/1 7/1 1/1 0/0 0/0 0/0 1/1 0/0 5/1 TIME OF DOSE PARTIAL CLOSURE EYES (PTOSIS) EXCESSIVE STRUGGLING DURING DOSING 1 -2 HOUR POST-DOSING PARTIAL CLOSURE EYES (PTOSIS) EYES/EARS/NOSE Target organ relation? PUPIL DILATED RIGHT EYE DRIED RED MATERIAL AROUND NOSE COMPLETE CLOSURE RIGHT EYE

Clinical observations (7) • Relation to target organs? * Group Example Organs/systems likely involved 1. Respiratory Cyanosis (Cardio)pulmonary insufficiency 2. Motoric Somnolence CNS sleep center 3. Convulsions Clonic CNS, respiratory failure, neuromuscular, autonomic 4. Reflexes No normal righting CNS, sensory, neuromuscular 5. Ocular Myosis Autonomic (parasympathomimetic) 6. Cardiovascular Tachycardia Autonomic (sympathomimetic, (Cardio)pulmonary insufficiency * The toxicologist’s pocket handbook M. J. Derelanko, 2008 (ISBN 978 -1 -4200 -5138 -4)

Clinical observations (8) • Relation to target organs? * Group Example Organs/systems likely involved 7. Salivation Excessive Autonomic (parasympathomimetic) 8. Piloerection Rough hair Autonomic (sympathomimetic) 9. Analgesia Decreased reaction to Sensory, CNS pain (e. g. hot plate) 10. Muscle tone Hypertonia Autonomic (sympathomimetic) 11. Excretion Red urine (hematuria) Damage in kidney 12. Skin Redness (erythema) Immunity (inflammation, sensitization. . . ) * The toxicologist’s pocket handbook M. J. Derelanko, 2008 (ISBN 978 -1 -4200 -5138 -4)

Clinical observations (9) • Signs indicative of pain, suffering & distress in animals * – Appearance & physical signs: chromodacryorrhea piloerection, dehydratation, dirty skin, skin lesions rapid & laboured respiration excessive salivation hunched posture – Movement & behaviour gait irregularity, ataxia abnormal aggressive behaviour, restlessness, agitation abnormal reaction to handling, vocalisation on handling tremors, writhing lethargy, decreased activity, reluctance to move licking, scratching, self mutilation * The toxicologist’s pocket handbook M. J. Derelanko, 2008 (ISBN 978 -1 -4200 -5138 -4) Picture: AALAS Learning Library https: //www. aalaslearninglibrary. org

Clinical observations (10) • Signs indicative of moribundity as criteria for sacrifice * – – – – – Prolonged impairment of locomotion, preventing access to food/water Continued difficult, laboured breathing Continued severe diarrhea Severe dehydration Eyes fixed or sunken Severe self mutilation Significant blood loss Excessive weight loss (> 25% over 7 days or more) Evidence of irreversible major organ failure (see further) Sustained 10% decrease in body temperature * The toxicologist’s pocket handbook M. J. Derelanko, 2008 (ISBN 978 -1 -4200 -5138 -4)

Body weight and food consumption (1) OECD 407, 408, 409, 451, 452, 453 • Body weight: measured at least once a week (up to week 13; every 4 weeks thereafter) • Food consumption: measured at least every weekly (up to week 13; every 4 weeks thereafter) • water consumption: measured at least weekly if the test substance is administered via the drinking water FDA redbook 2000 • Attempt to quantify spillage of feed by test animals, and to determine if spillage is greater with test diets than with control diets. Appropriate discussions of feed spillage should be included in the study report.
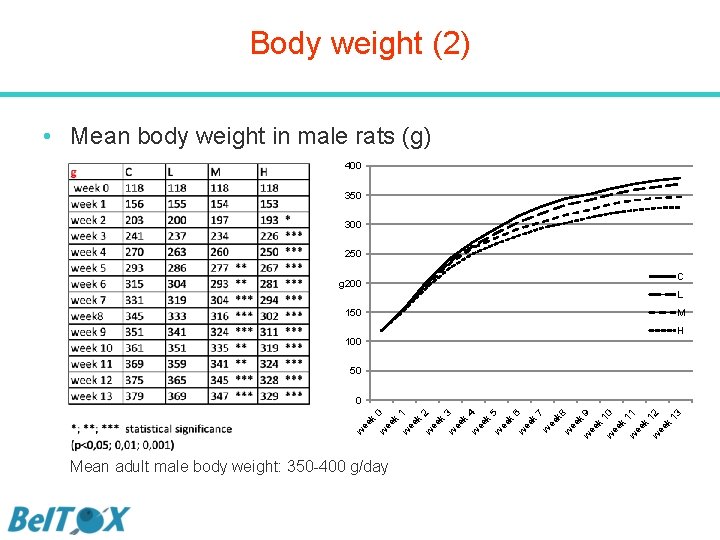
Body weight (2) • Mean body weight in male rats (g) 400 350 300 250 C g 200 L 150 M H 100 50 7 ee k w 8 ee k 9 w ee k w 10 ee k w 11 ee k w 12 ee k 13 w k 6 k w ee 5 k 4 ee w k 3 k w ee 2 k 1 ee k Mean adult male body weight: 350 -400 g/day w ee w w ee k 0 0
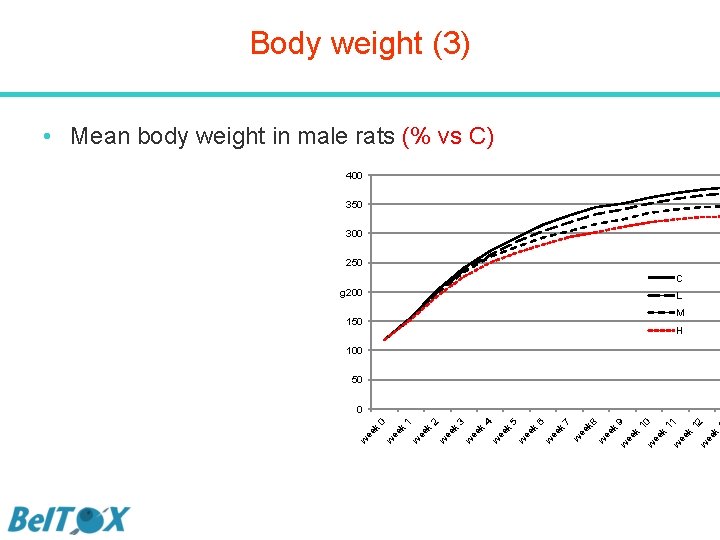
Body weight (3) • Mean body weight in male rats (% vs C) 400 350 300 250 C g 200 L M 150 H 100 50 ee k 12 w 11 ee k w 10 ee k w 9 ee k k w ee k 8 7 w k 6 ee w k ee w ee k k 5 4 w 3 ee w k 2 ee k ee w w ee k 1 0 0
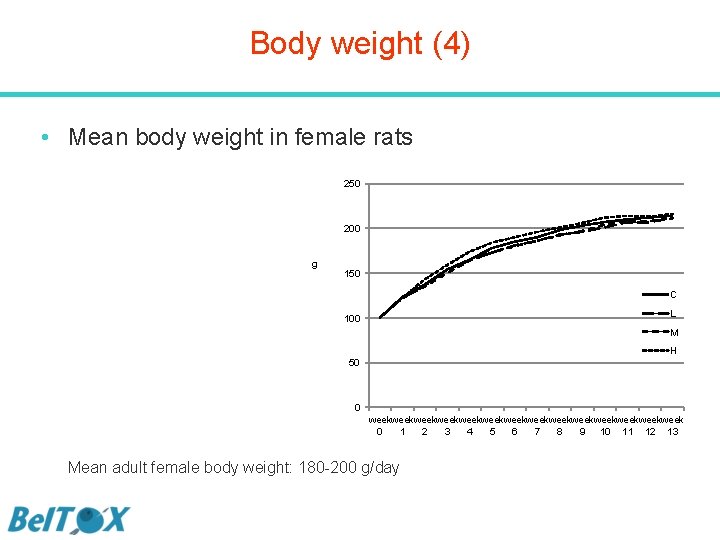
Body weight (4) • Mean body weight in female rats 250 200 g 150 C L 100 M H 50 0 weekweekweekweekweekweekweek 0 1 2 3 4 5 6 7 8 9 10 11 12 13 Mean adult female body weight: 180 -200 g/day
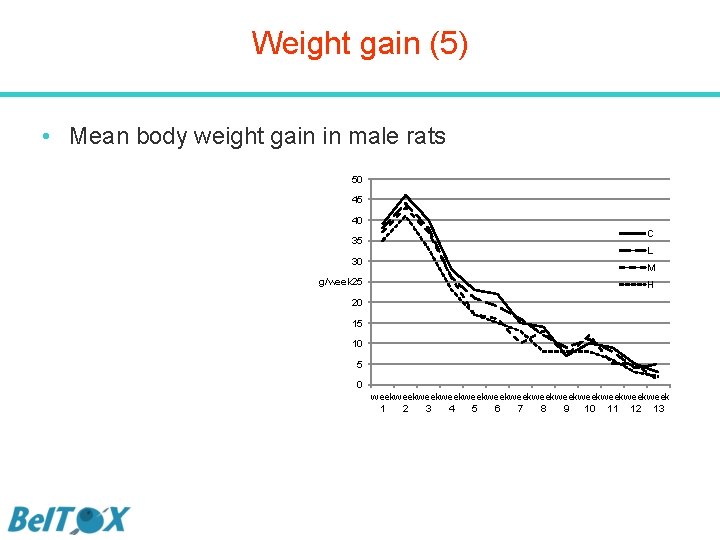
Weight gain (5) • Mean body weight gain in male rats 50 45 40 35 30 g/week 25 C L M H 20 15 10 5 0 weekweekweekweekweekweekweek 1 2 3 4 5 6 7 8 9 10 11 12 13
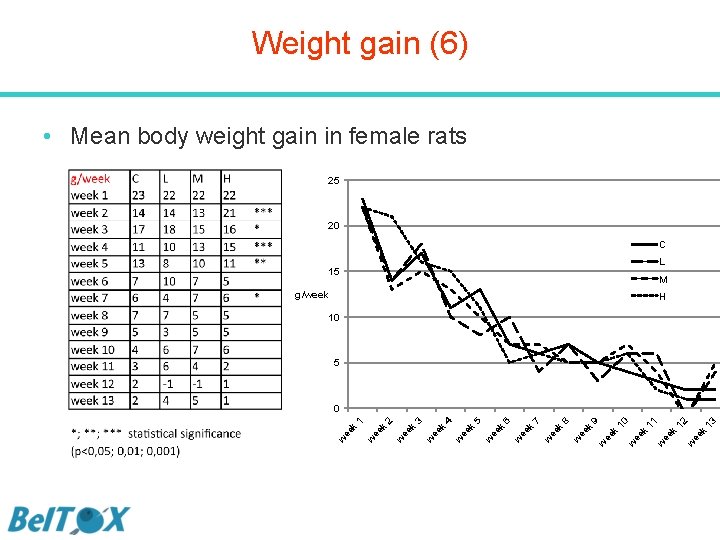
Weight gain (6) • Mean body weight gain in female rats 25 20 C L 15 M g/week H 10 5 13 ee k w ee k 12 11 w ee k 10 w 9 ee k k w ee w k ee w ee k 8 7 6 w ee k 5 w ee w k 4 3 k ee w w ee k 1 2 0
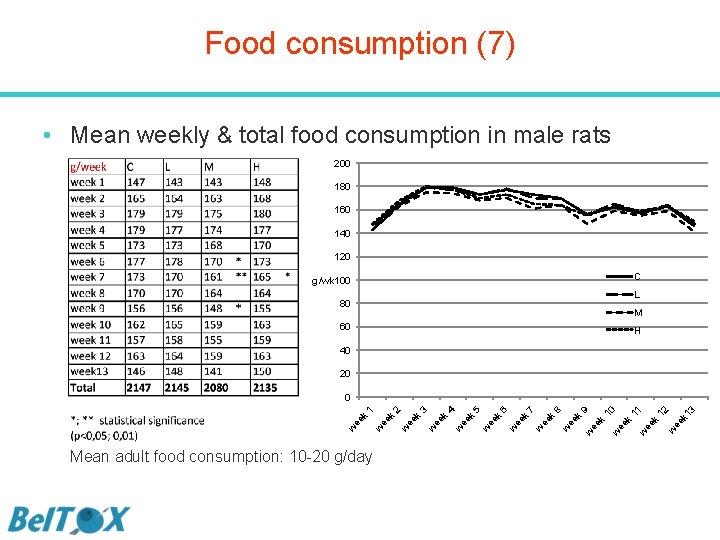
Food consumption (7) • Mean weekly & total food consumption in male rats 200 180 160 140 120 C g/wk 100 L 80 M 60 H 40 20 Mean adult food consumption: 10 -20 g/day 3 k 1 12 w ee 11 ee k w ee k 10 ee k w w 9 8 k w ee k 7 w 6 ee w k 5 ee w k 4 3 k 2 ee w k ee w w ee k 1 0
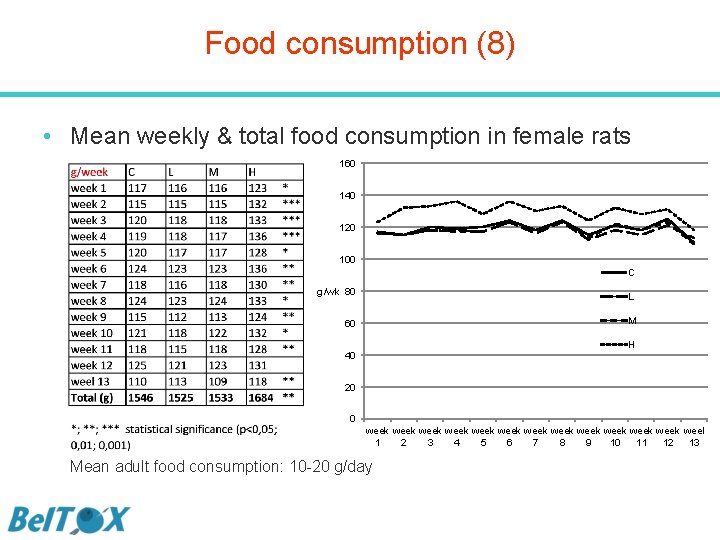
Food consumption (8) • Mean weekly & total food consumption in female rats 160 140 120 100 C g/wk 80 L M 60 H 40 20 0 week week week weel 1 2 3 4 5 6 7 8 9 10 11 12 13 Mean adult food consumption: 10 -20 g/day

Opthalmology (1) OECD 408, 409: • Opthalmological examination: prior to the administration and at termination of the study – Preferably in all animals of control and high dose group – If changes are detected, all animals should be examined • Practically: – Visual inspection: conjunctiva, sclera, cornea, iris, lens and fundus – After induction of mydriasis (e. g. atropine sulphate 1%), eyes are examined by use of a slit lamp biomicroscope.
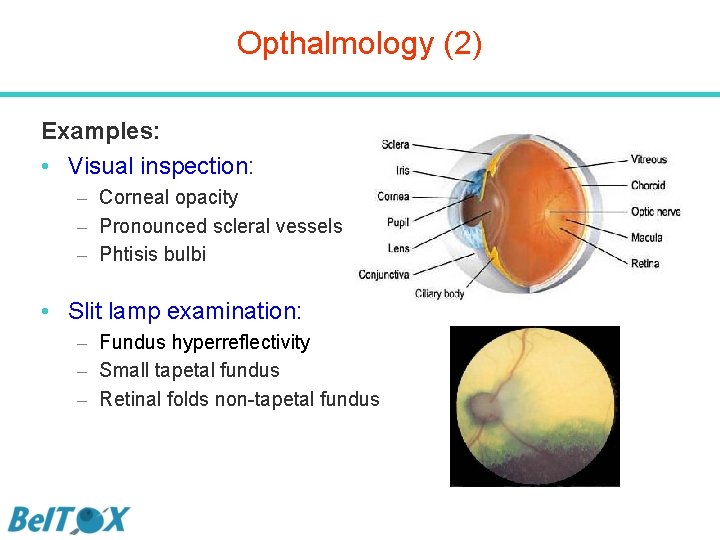
Opthalmology (2) Examples: • Visual inspection: – Corneal opacity – Pronounced scleral vessels – Phtisis bulbi • Slit lamp examination: – Fundus hyperreflectivity – Small tapetal fundus – Retinal folds non-tapetal fundus
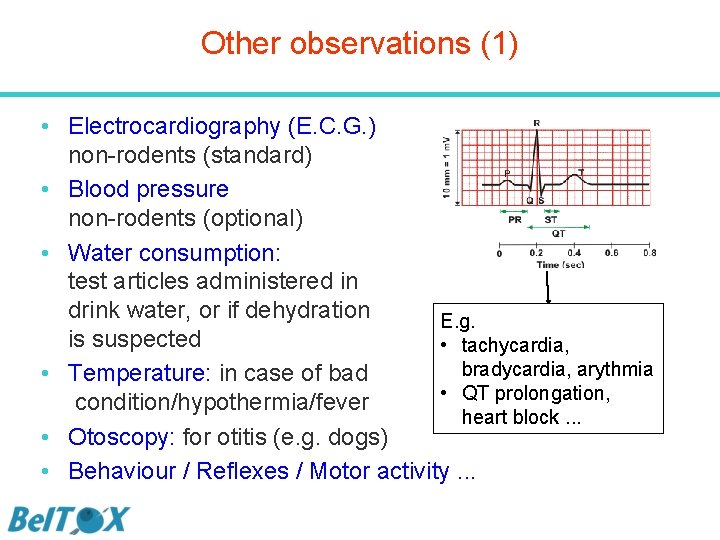
Other observations (1) • Electrocardiography (E. C. G. ) non-rodents (standard) • Blood pressure non-rodents (optional) • Water consumption: test articles administered in drink water, or if dehydration E. g. is suspected • tachycardia, bradycardia, arythmia • Temperature: in case of bad • QT prolongation, condition/hypothermia/fever heart block. . . • Otoscopy: for otitis (e. g. dogs) • Behaviour / Reflexes / Motor activity. . .
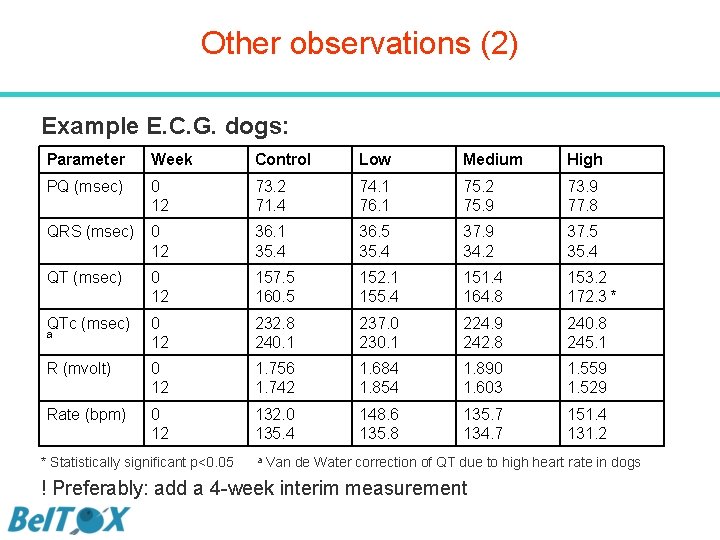
Other observations (2) Example E. C. G. dogs: Parameter Week Control Low Medium High PQ (msec) 0 12 73. 2 71. 4 74. 1 76. 1 75. 2 75. 9 73. 9 77. 8 QRS (msec) 0 12 36. 1 35. 4 36. 5 35. 4 37. 9 34. 2 37. 5 35. 4 QT (msec) 0 12 157. 5 160. 5 152. 1 155. 4 151. 4 164. 8 153. 2 172. 3 * QTc (msec) 0 12 232. 8 240. 1 237. 0 230. 1 224. 9 242. 8 240. 8 245. 1 R (mvolt) 0 12 1. 756 1. 742 1. 684 1. 854 1. 890 1. 603 1. 559 1. 529 Rate (bpm) 0 12 132. 0 135. 4 148. 6 135. 8 135. 7 134. 7 151. 4 131. 2 a * Statistically significant p<0. 05 a Van de Water correction of QT due to high heart rate in dogs ! Preferably: add a 4 -week interim measurement

Discussion & Conclusion Thank You! 25
- Slides: 25