Bell Work Grab a note taker from the


Bell Work • Grab a note taker from the front table • Discuss in your groups what you already know about concussions. Be ready to share in 7 minutes

WHAT is a CONCUSSION • Definition: “Complex pathophysiological process affecting the brain, induced by traumatic biomechanical forces” • Usually defined as any change in neurologic function • Often referred to as mild traumatic brain injury (MTBI) • Only about 10% of concussions involve loss of consciousness • 80 -90% resolve in 7 -10 days • CT and MRI often normal • 15% may have symptoms lasting >1 year Mc. Crory P et al. Consensus statement on Concussion in Sport-the 3 rd International Conference on Concussion in Sport held in Zurich, November 2008. J Sci Med Sport 2009; 12: 340 -351

Defined as the result of the forceful motion of the head causing a brief change in mental status for less than 30 minutes.

Why the increased focus recently on sports-related concussions? • Evolving definition of concussion • Concussion is common in sports and increasing • Potential for catastrophic outcomes • Development of tools to describe postconcussive dysfunction

WHY INCREASED FOCUS? • EVOLVING DEFINITION of concussion to reflect alteration in brain function, even without loss of consciousness • Pre-participation counseling, testing PRIOR to the athlete’s season • Checklists and screening tools now available • Recent media reports highlight the potential for rare but catastrophic outcomes in young healthy individuals • Legislative efforts, such as Lystedt Laws, to prevent repeat injuries and tragic consequences • i. Phone APPS!!! Meehan WP, et al. High School concussions in the 2008 -2009 Academic Year: Mechanisms, Symptoms and Management. A J Sports Med. 2010; 38(12): 2405 -2409. Mc. Crory P, et al. Consensus statement on Concussion in Sport-the 3 rd International Conference on Concussion in Sport held in Zurich, November 2008. J Sci Med Sport 2009; 12: 340 -351
Why increased focus on sports concussion? • All sports and recreation-related concussion in U. S. 1. 63. 8 million/year • Concussion is COMMON in youth sports: 8. 9% of high school athletes • Concussions appear to be increasing, especially among high school athletes Meehan WP, et al. High School concussions in the 2008 -2009 Academic Year: Mechanisms, Symptoms and Management. A J Sports Med. 2010; 38(12): 2405 -2409. Langlois JA, et al. The epidemiology and impact of traumatic brain I njury: a brief overview. J Head Trauma Rehabil 2006; 21: 375 -8. Bakhos LL, et al. Emergency Department visits for concussion In young child athletes. Pediatrics. 2010 Sep. 126(3): e 550 -556.

Why increased focus? • Development of tools to describe postconcussive dysfunction Collins MW. , et al. Relationship between concussion and neuropsychological performance in college football players. JAMA. 1999; 282(10)964 -970.

SIGNS AND SYMPTOMS OF ACUTE CONCUSSION • Symptoms-somatic, cognitive or emotional – Somatic • Headache, nausea, vomiting, dizziness, – Cognitive • Feeling slowed down, difficulty concentrating/remembering – Emotional • Involuntary crying, sadness, anxious, nervous

Concussion Symptoms • Various symptoms may occur, may be intermittent and may not be noticed immediately. Common symptoms include: l Confusion l Nausea or vomiting l Headache l Bothered by light or l Difficulty remembering or paying attention l Balance problems or dizziness l Feeling sluggish, hazy, foggy or groggy l Feeling irritable, more emotional or “down” noise l Double or blurry vision l Slowed reaction time l Sleep problems l Loss of consciousness www. cdc. gov/concussioninyouthsports

EVALUATION • Standard emergency management, especially with C-spine • Team personnel remove the athlete from play • No athlete should return to play until assessed by appropriate LHCP • Imaging NOT helpful for sports related concussion – CT used to R/O more serious TBI if LOC, amnesia, persistently altered mental status, or clinical deterioration • Player should not be left alone and should have serial monitoring over initial few hours

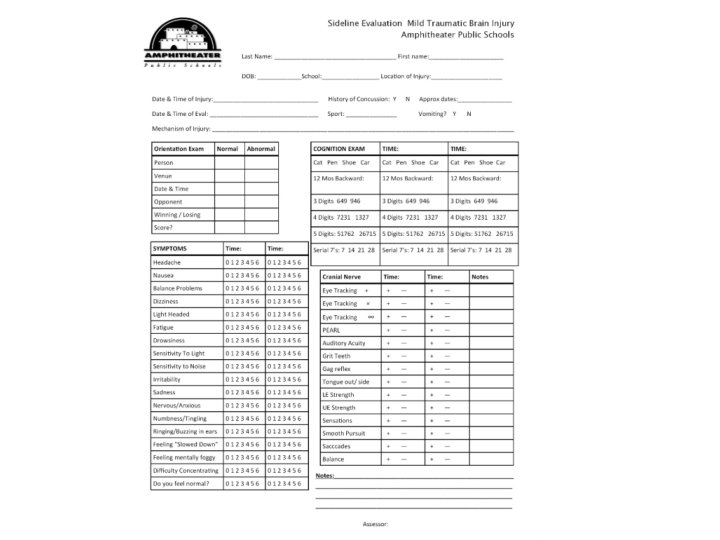
SIDELINE EVALUATION • Neurological Exam – Assessment of sensory and motor responses (reflexes, sensation, cranial nerves) • Cognitive Exam – A series of tests to determine brain function (orientation, months backwards, serial 7 s) • Physical Exam – Medical history, physical history, inspection of further injuries (open wounds/closed wounds)

TREATMENT • Physical rest: refrain from strenuous aerobic activities • Cognitive rest: minimize activities that require concentration and attention • Recommendations are based on best available science and consensus Mc. Crory P, et all. Consensus statement on Concussion in Sport-the 3 rd International Conference on Concussion in Sport held in Zurich, November 2008. J Sci Med Sport 2009; 12: 340 -351

RETURN TO PLAY? ? • Ongoing symptoms should preclude return to play – Includes practice! • Gradual return to activity ONLY after symptoms have resolved – Walk/Bike – Jog-Run-Jog – Run and sprints

RETURN TO PLAY • No single diagnostic test to determine concussion resolution • Clinical determination based on history, exam, etc. • Pre-injury baseline neurocognitive testing is helpful for a post-injury comparison • Progressive physical activity

How You Can Help Minimize Risk Factors in Sports Concussions • Teach safe techniques in practice and play • Encourage recognition and reporting of concussion symptoms • Be aware that injuries are more common in younger athletes • Use available assessment tools • Monitor developments at advanced levels of play and legislative efforts • Head and spine injury prevention programs

Teach Safe Techniques • Greater emphasis needs to be placed on teaching fundamentals and techniques, such as proper and safe blocking and tackling • https: //www. youtube. com/watch? v=91 vg. E_uj. VHM

Encourage Recognition and Reporting of Symptoms

Be extra vigilant with younger players, who are more likely to be injured

http: //www. discnw. org/youth/lystedt. html Encourage passage of Lystedt Laws Named in honor of 13 yo Zachery Lystedt, injured in October, 2006, when he returned to a football game after a concussion and was permanently injured. • Coaches are required to sign a statement indicating that they have been educated as to the nature and risk of head injuries. "When it doubt, sit them out. " A player that has been removed from competition cannot return to play until (s)he has been evaluated by a LHCP trained in the evaluation and management of concussion and has received written clearance to return to play from that health care provider. • Parents/Guardians are required to review and sign an annual concussion and head injury information sheet prior to their children's participation in athletic events. • Athletes are required to review and sign an annual concussion and head injury information sheet prior to their participation in athletic events. If they suspect a head injury in themselves or a teammate, they are encouraged to tell their coach.

All Concussions Are Serious • • Don’t hide it Report it Take time to recover It’s better to miss one game than the whole season

Conclusion • Traumatic injuries affect more patients than all other neurological conditions COMBINED • At present, the best treatment is PREVENTION • Athletic Trainers are experts in evaluation, treatment and prevention of concussion and traumatic brain injury. https: //www. youtube. com/watch? v=cyx. Vq. L 7 n. AZ 4 https: //www. youtube. com/watch? v=F 4 fo. Y 1 Etm. Ko https: //www. youtube. com/watch? v=edp. TZsd. YFL 4 https: //www. youtube. com/watch? v=9 Tr. CZcs. Sy. A 8&t=308 s
- Slides: 23