Being Successful Under Bundled Payments What Weve Learned

Being Successful Under Bundled Payments; What We’ve Learned So Far December 11, 2015 1

What is the Bundled Payments for Care Improvement Initiative (BPCI) Models 1, 2, 3 and 4 Model 1: • inpatient stay; discounted IPPS Models 2 and 3: • retrospective bundled payment arrangement; FFS with reconciliation Model 4: • single, prospective payment to hospital to pay all costs of inpatient stay 2

What Is It and How It Works Models 2 and 3 48 Bundles Based upon DRGs Choose which bundles 1 to 48 bundles 30 – 60 – 90 day risk Longer risk had greater pricing Pricing is a combination of own historical data and regional data Fee for service Paid to all providers during the bundle Costs accrue Some exclusions Reconciliation 3

Model 2 vs. Model 3 Bundles 2 • Includes the initial hospitalization plus 30, 60, or 90 days post discharge • Hospital or operating/attending physicians can initiate the bundle 3 • Bundle starts after patient discharged from the hospital • HHAs, SNFs, operating/attending physicians can initiate the bundle • HHAs and SNFs only initiate the bundle if they are the first site of service post discharge • If patient goes to SNF first and then HHA, the HHA does not initiate the bundle 4

Precedence Rules • Model 2 bundles almost always trump Model 3 bundles • If hospital initiates the bundle, SNF or HHA cannot initiate the bundle • Model 2 bundle cannot pass on a bundle in which they are participating • Still need PAC providers who understand managing patients under a bundled payment model • Risk sharing/gain sharing opportunities • Model 2 and Model 3 bundles trump CJR • “AS IF” the CJR event did not occur; exclude the CJR event from the hospital’s reconciliation • Hospitals paid fee for service; no risk • Risk sharing/gain sharing opportunities 5
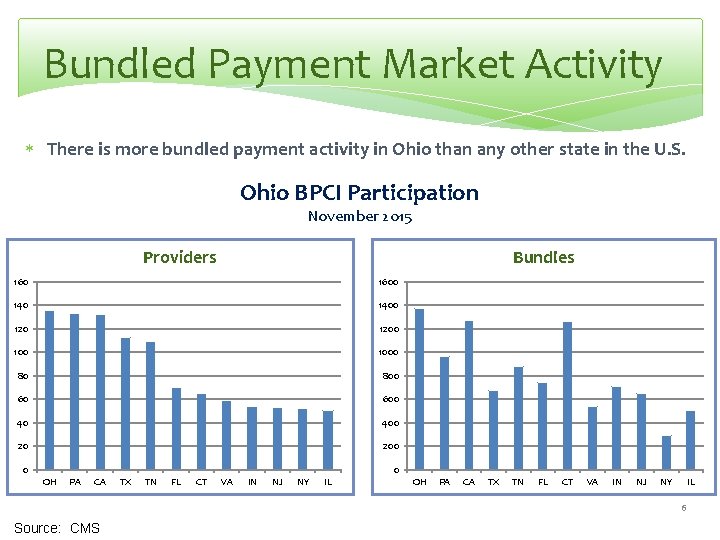
Bundled Payment Market Activity There is more bundled payment activity in Ohio than any other state in the U. S. Ohio BPCI Participation November 2015 Providers Bundles 1600 1400 1200 1000 80 800 60 600 40 400 20 200 0 0 OH PA CA TX TN FL CT VA IN NJ NY IL 6 Source: CMS
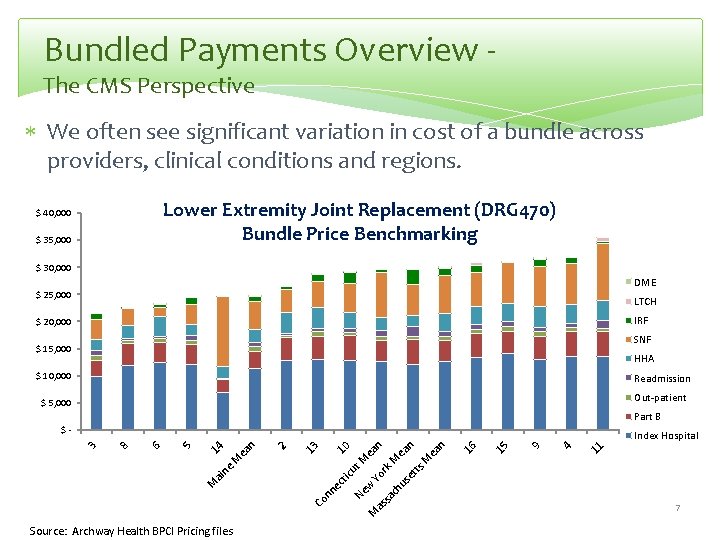
Bundled Payments Overview The CMS Perspective We often see significant variation in cost of a bundle across providers, clinical conditions and regions. Lower Extremity Joint Replacement (DRG 470) Bundle Price Benchmarking $ 40, 000 $ 35, 000 $ 30, 000 DME $ 25, 000 LTCH IRF $ 20, 000 SNF $ 15, 000 HHA $ 10, 000 Readmission Out-patient $ 5, 000 Part B $- 11 4 9 15 16 ut Co nn ec tic ai n M Source: Archway Health BPCI Pricing files Ne M w ea M Yo n as rk sa M ch ea us n et ts M ea n 10 13 2 ea n e M 14 5 6 8 3 Index Hospital 7
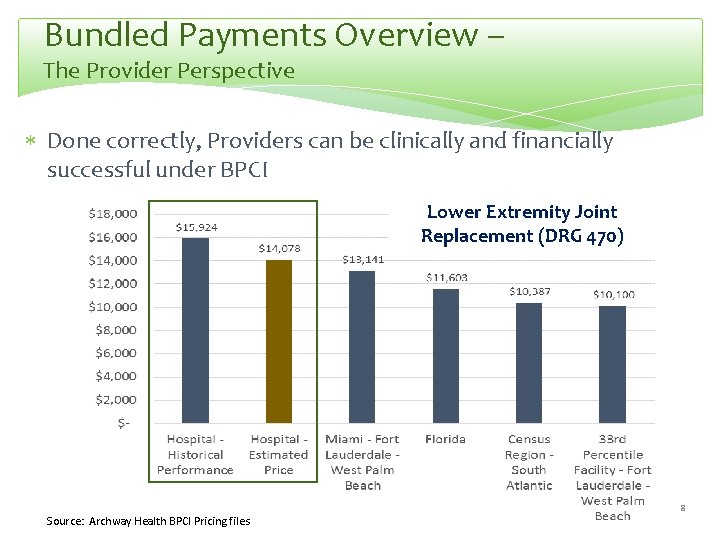
Bundled Payments Overview – The Provider Perspective Done correctly, Providers can be clinically and financially successful under BPCI Lower Extremity Joint Replacement (DRG 470) Source: Archway Health BPCI Pricing files 8

Bundled Payment Overview – The Provider Perspective There a number of strategic benefits for providers to participate in bundled payment programs. Increase Net Revenue Significantly increase net revenue opportunity Low Risk Low risk way to prepare for other alternative payment initiatives Increase Patient Satisfaction Enhance long term relationship with patients Enhance Provider Alignment Opportunity to enhance alignment and loyalty of upstream and downstream providers Network Development Facilitates development of a network of preferred providers • Does not conflict with patient choice 9

Case Study Cedar Village 10

Bundled Payment for Care Improvement Initiative • Triple Aim • Better Health • Better Experience • Lower cost • Care Improvement Focus • Bundled Payments align incentives 11

How To Be Successful in Bundled Payments Care Transitions Program/Coordinators Assist with providing quality care in a safe, cost-effective setting Software Data Analytics to drive process improvement Reduce avoidable readmissions Manage to appropriate length of stay Real time data Inclusive system available to all providers along the continuum 12
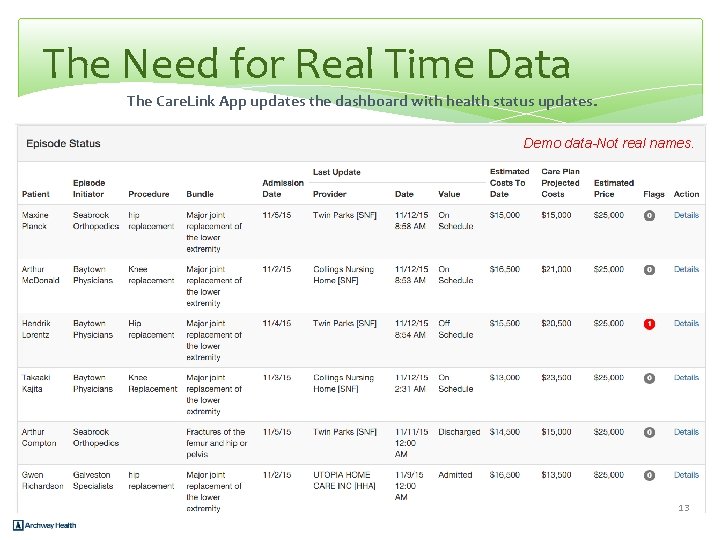
The Need for Real Time Data The Care. Link App updates the dashboard with health status updates. Demo data-Not real names. 13

Cedar Village - Critical Factors for Success • Case Management – real time tracking tools • Inter-disciplinary Team – daily monitoring • Nursing, Therapy, Social Services • Comprehensive 30 -day Care Plans • Discharge Planning begins at admission • Home Care involved early • Warm hand offs between settings 14
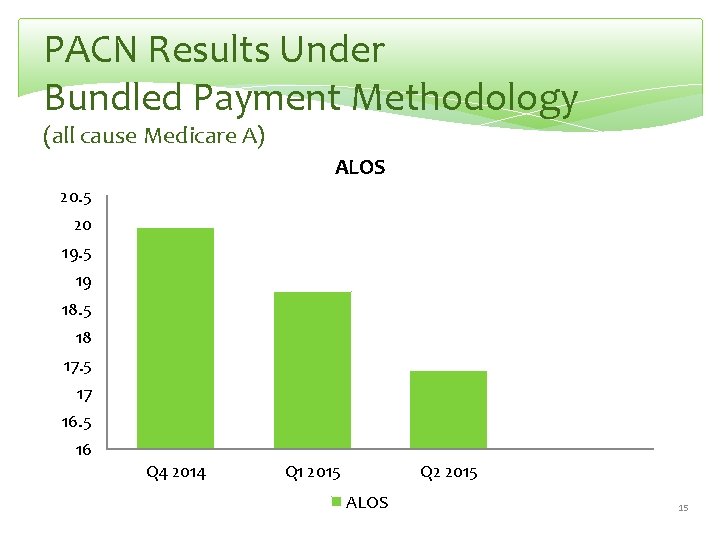
PACN Results Under Bundled Payment Methodology (all cause Medicare A) ALOS 20. 5 20 19. 5 19 18. 5 18 17. 5 17 16. 5 16 Q 4 2014 Q 1 2015 Q 2 2015 ALOS 15
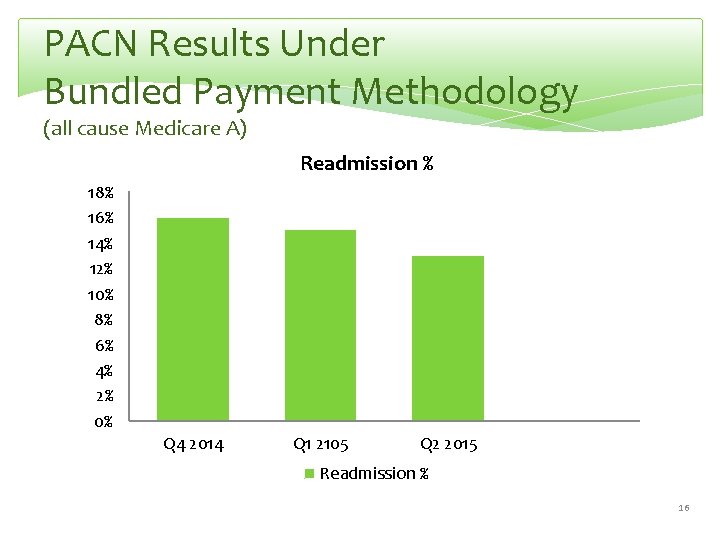
PACN Results Under Bundled Payment Methodology (all cause Medicare A) Readmission % 18% 16% 14% 12% 10% 8% 6% 4% 2% 0% Q 4 2014 Q 1 2105 Q 2 2015 Readmission % 16
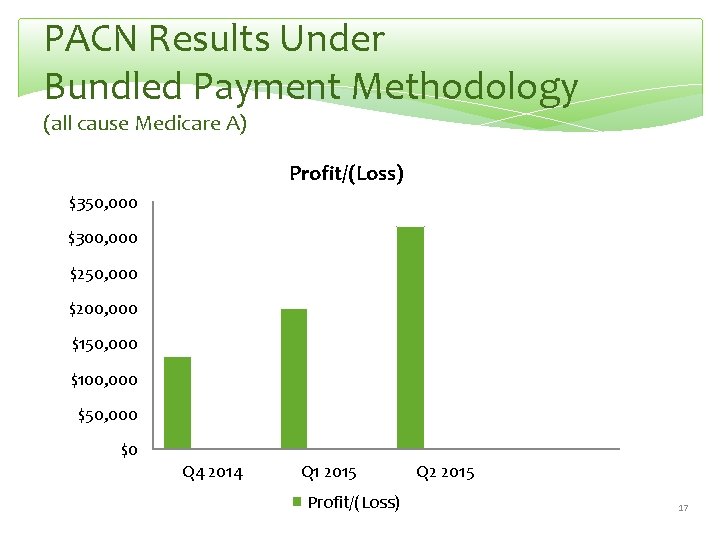
PACN Results Under Bundled Payment Methodology (all cause Medicare A) Profit/(Loss) $350, 000 $300, 000 $250, 000 $200, 000 $150, 000 $100, 000 $50, 000 $0 Q 4 2014 Q 1 2015 Profit/(Loss) Q 2 2015 17

Tippy Canoes Current – Per Diem Future – Bundled Payment 18
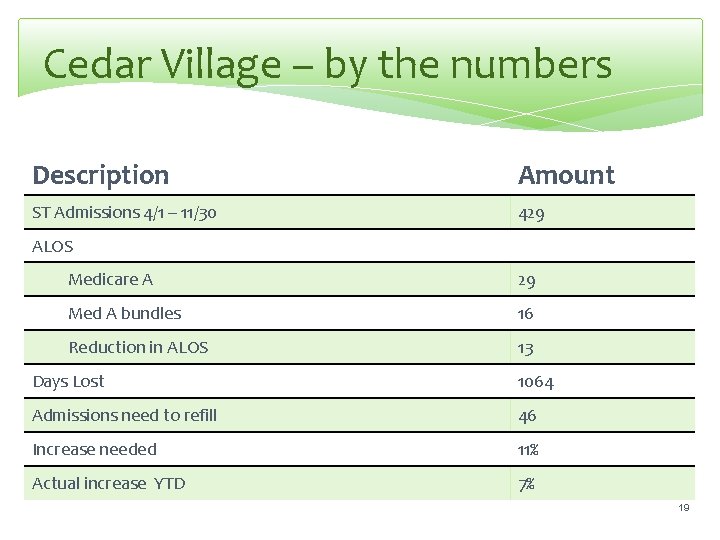
Cedar Village – by the numbers Description Amount ST Admissions 4/1 – 11/30 429 ALOS Medicare A 29 Med A bundles 16 Reduction in ALOS 13 Days Lost 1064 Admissions need to refill 46 Increase needed 11% Actual increase YTD 7% 19

Straddling the Tippy Canoes Short Run Long Run Reducing LOS reduces revenue Gains under BPCI is shared between Convener and Episode Initiator Gain sharing payments are delayed 9 months Success depends on increasing admission to refill the beds Early adopters are learning to manage under the new payment model Begin restructuring to adapt to shorter LOS Success depends on managing the full 30 -day episode and avoiding readmissions 20

Recap Bundled Payments are not coming, they are already here Precedence Rules are somewhat complicated • Model 2 almost always trumps a Model 3 • Model 2 and Model 3 trump CJR By 2018, CMS wants 50% or $330 B of the Medicare spend in alternate payment models (mainly BPCI, CJR, and some ACO’s) Success can only be achieved through acute care/post-acute care providers partnering with a clear focus on CMS’s Triple Aim 21

Don Berwick, MD “Moving from the concept that the best bed is a full bed to the concept that the best bed is an empty one – that’s a major transition. ” Donald M. Berwick, MD, former Administrator of the Centers for Medicare and Medicaid Services (CMS). Former President and Chief Executive Officer of the Institute for Healthcare Improvement[1. Berwick is Clinical Professor of Pediatrics and Health Care Policy in the Department of Pediatrics at the Harvard Medical School and Professor of Health Policy and Management at the Harvard School of Public Health. [17] He is also a pediatrician, Adjunct Staff in the Department of Medicine at Children's Hospital Boston, and a Consultant in Pediatrics at Massachusetts General Hospital. 22

Don Berwick, MD “Everybody is doing what makes sense to them individually. We pay hospitals to be full, so they try to be full. We pay doctors to see patients, so they see a lot of patients. We create a public expectation that more is better, (which isn’t actually true) so people seek more. Everybody is doing their jobs; we just designed the jobs wrong. ” 23

Don Berwick, MD We have a long way to go. Board, executives and finance leaders still need to really convince themselves that the best way to contain costs is to improve care. 24

Atul Gawande, MD The Cost Conundrum – “The lesson of the high quality, low cost communities is that someone has to be accountable for the totality of care. Otherwise the system has no brakes. ” 25

Contact Information Tim Grimes Jan Wooles, CPA, MBA Executive Director Post-Acute Care Network 6279 Tri-Ridge Blvd. Loveland, Ohio 45140 Cell: 937 -307 -4474 Office: 513 -719 -3502 Chief Financial Officer Cedar Village Retirement Community 5467 Cedar Village Drive Mason, Ohio 45040 Office: 513 -754 -3100 Tim. grimes@pacnllc. com jwooles@cedarvillage. org 26
- Slides: 26