Behavioural health in primary care in rural and

Behavioural health in primary care in rural and remote contexts: Development of a new paradigm. Richard Taylor MACAPP Clinical Psychologist Management Consultant MBA advanced Univ WA Business School Foundation member of the Australian College of Advanced Postgraduate Psychologists www. acapp. net. au Foundation member of the Australian Clinical Psychology Association © R. Taylor 2014 1

Introduction This presentation is for rural and remote primary health care practitioners. It describes a collaborative person-centred methodology for behavioural health care built upon primary care values. The framework is called the Exploration Paradigm. It has two interrelated components: 1. A visual Formulation Map (covering assessment priorities, content, and process), and 2. A practice-based evidence process which draws on different services and resources as required over time. Notes on terminology The term behavioural health refers to anything to do with mental health in primary care. The terms ‘patient’ and ‘client’ are avoided where possible with the emphasis on the individual person as collaborator in their own care. © R. Taylor 2014 2

Primary care innovation can make a difference The vast majority of people consult a general practitioner (GP) for behavioural health issues and/or emotional distress. In 2010 approximately one in ten GP encounters in Australia (10. 7 million encounters nationwide) involved the management of mental health related problems (NACMH). Approximately 90 per cent of those with mental health problems, including 30 to 50 per cent of those with severe mental illness, are only seen in primary care (Lester, et al. 2004). The overall population effects of even small improvements in psychological and associated care would be enormous (Cape, et al. 2000). This would enable a flow on effect that positively influences the rates of prescribing psychotropic drugs, particularly given the lack of studies supporting combining drugs with psychological approaches (Sparks, et al. 2010). However, GPs sympathetic to alternative frameworks for understanding and responding to mental disturbance, and challenging the current attachment to the biomedical or biopsychological model, find that alternative theoretical and practical frameworks which fit within primary care do not exist. © R. Taylor 2014 3

Key reform challenge… ‘Despite calls from the World Health Organisation to integrate mental health care into primary care, clear theoretical or practical frameworks do not exist to guide this process globally. In addition, threats to generalism, and the traditional values of general practice, in what some call a reductionist age, suggest that perhaps it is time for primary care to define what core values, skills and priorities it proposes to offer to the community in mental health assessment’. (Lynch, et al. 2011, p. 143). © R. Taylor 2014 4

The benefits and the most effective means to improve health… ‘…integrating mental health services within primary care is the most practical way to advance a patient’s health, which can reduce hospitalizations and emergency visits, all resulting in decreased costs’. (Dr Parinda Khatri, American Psychological Association at a U. S. congressional briefing. APA Access, November 12, 2014). © R. Taylor 2014 5

Failed approaches to avoiding the dichotomy of ‘physical’ and ‘mental’ in primary health care: Coordination/collaboration/shared care - increased administration and decreased cost effectiveness usually results Co-location of mental health Care management model - outsourced psycho-education and medication compliance usually key features Consultation - liaison psychiatry - belongs in tertiary care Integration (jigsaw pieces) - never divorced from the paternalistic-medical ethos including evidence-based care derived from the medical model Need for a holistic approach, fusion, grounded in primary care values © R. Taylor 2014 6

The Exploratory Paradigm: Brief overview The Exploration Paradigm makes behavioural health a core function of primary care. It is built on the values and strengths of primary care. Hence fusion rather than integration is emphasized. An exploratory view of the consultation stresses a shared social interaction or interactive journey involving person-centred care. Variable outcomes result over time through a coconstructed exploratory process. Knowledge is shared to meet the needs of both practitioner and the individual. The process serves to support the creative capacity of individuals maintaining their daily lives (Reeve, 2010). Current constraints Unclear primary care values and availability of skills affect standards. The variability of competence, training and interest, influences the assessment of psychological distress and resultant priorities and outcomes. This often leads to prescribing medication or a referral elsewhere (Lynch, et al. 2012). Individuals often report an ad hoc, fragmented, and poorly communicated response to psychological distress. Even with the DSM GPs fail to diagnose many common mental disorders (Dew, et al. 2005). They often use diagnostic criteria loosely in a complex assessment process constrained by such things as time and resources (Armstrong & Earnshaw, 2004). However, routine GP consultations for psychological problems, involving a safe working and empowering relationship, empathy and listening, while making sense of experience and facilitating change, can have a powerful and positive impact (Buszewicz, et al. 2006). © R. Taylor 2014 7

Person-centred practice is a core value and involves: • The practitioner being open to the person’s full range of difficulties. • Understanding ‘meaning’ related to psychological suffering and illness. • Sharing of power and responsibility. • A relationship fostering trust, motivation, understanding, and confidence. • Practitioner self-awareness including values and assumptions. • Conscious attention to the present moment. People rarely report feeling at the centre of a consultation. Fear of loss of control, threats to existing coping strategies, and distrust of the wider system of which the GP is a part can compromise disclosure of mental health issues (Dew, et al. 2007). Person-centred practice can greatly assist align expectations and agendas in therapeutic relationship. Whole person-centred care built around the person’s perspective is central to primary care (Lynch, et al. 2012). © R. Taylor 2014 8

Foundations of innovation The design of the Exploration Paradigm, if to be successfully embedded in practice, has to be based on addressing ‘real’ problems from the perspective of the end user. Innovation must be person-centred: ‘The fundamental shift has to ensure we tackle the right issues by being well engaged with those seeking services. What is it that really matters and in what order? What are the simple things we can do to remove roadblocks so people can get on with their lives in the ways that it makes sense to them? ’ (Broadbent, 2013, p. 12). Extensive practice-based experience suggests people experiencing psychological distress and problems want: • Understanding (of relational/social contexts). • Focus on their identified issues and a ‘right’ outcome. • Restoration of personal meaning. • Tools to self-manage their own well-being. • Accessible language and cultural sensitivity. • To manage personal limitations and to build upon strengths and achievements. Successful innovation meets the needs of practitioners and those they help. It must be easily communicated, reliable, low cost, and not need an instruction manual. The process must be workable within limited consultation time. (blog - leanmedicine. co) For an innovation to become adopted in primary care there must be shared priorities about the nature of problems, possible actions and outcomes, with professional accountability and confidence in the health practitioner enhanced (May, 2007). © R. Taylor 2014 9

1. The Formulation Map is a practical tool that enables rural and remote practitioners to respond with a unified approach to the myriad types of behavioural health problems presented. It is a significant intervention in its own right and may set the person free on their own course. Formulation has been described as ‘the co-construction of a narrative that provides a specific focus for a learning journey’ (Corrie & Lane, 2010, p. 24). The initial assessment (formulation) depends upon a narrative and understanding the person’s story. It is about helping someone share an authentic account of where they are, how they got there, what needs to be accepted and what commitment to change needs to occur. Much psychological distress is undifferentiated and assessment involves skills to manage uncertainty and complexity. A whole person approach emphasizing both context and history is necessary. The Formulation Map (figure below) enables prioritizing action and desired outcomes while making choices and decisions transparent and explicit. It also facilitates interpersonal continuity of care which is a core primary care value. This includes continuity of information, cross boundary and team continuity and effective communication. © R. Taylor 2014 10

The Formulation Map incorporates: • Primary care values reflected in its architecture/design. • The possible role of trauma, abuse, and loss. • Unified transdiagnostic emotion-focused psychological assessment and intervention. • Relational contexts, social circumstances, quality of life. • Recovery factors and processes. • Attention to preventing onset and recurrence. • Previous experience with health services. • Advocacy, giving the person a voice. • Decision-criteria for psychotropic prescribing. © R. Taylor 2014 11
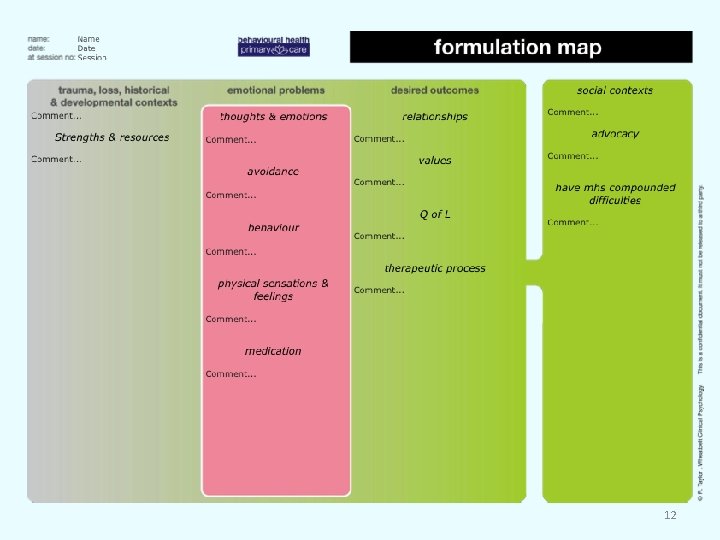
Figure 1 Formulation Map 12

Formulation and culture change Use of the formulation map in primary care is not just an alternative, but an antidote to psychiatric classification, diagnosis, and assumptions and their damaging effects including stigma, loss of meaning and medical and social consequences. Psychiatric values do not sit with the unique setting of primary care: ‘…using the psychiatric value system in mental health care conceptualisation and therapeutic decision making is not based on proven patient outcomes or alignment with primary care values or context’ (Moncrieff, quoted by Lynch, et al. 2012, pp. 145). Prescribing medication may too easily follow the use of diagnostic frameworks that medicalize problems of living and result in a narrowing of primary care tasks. When a formulation-based approach is embedded in primary care the exploratory process of change can be truly patient-centred, ‘It is a powerful instrument for culture change. It puts back what psychiatry takes out, and restores meaning, agency and hope, for staff and service users’ (Johnstone, 2014, p. 239). © R. Taylor 2014 13

‘What do we do instead of diagnosing people? ’ Response: ‘Stop diagnosing people’. The alternative: Ask people what their problems are and want they want help with, and give them the tools to explore change. Ask questions such as: ‘What is on your wish list? ’; ‘What is most important for you to change? ’, and ‘Do other people around you have a view on this? ’. A person with emotional difficulties seeks acceptance, acknowledgement, and a positive frame of reference. Development of a shared understanding of desired outcomes, relational and contextual goals, evolves over time. In this way the relationship and approach taken can be customized to the individual person and context…using what works and subjecting the relationship to constant measurement from feedback. © R. Taylor 2014 14

The Formulation Map in practice The Formulation Map in a live and interactive version permits the direct recording by practitioners of narrative and psychological insights. Linkages can be illustrated and made explicit. The Formulation Map deepens understanding. It provides a holistic or overall view previously not possible in constructing meaning and making sense of distress or dysfunction. It can be used by primary care team members for thinking and processing their feelings in response to a person’s life situation. From the outset different perspectives, expertise, and skills can be capitalised on. It can be used in a pro-active and preventative fashion. The impact of physical health problems and disease and disability can be incorporated. The Formulation Map is shared with the person involved who can also input and share new insights, understanding and importantly outcomes. Using a formulation approach can empower people to make informed decisions about medication through its collaborative framework and developmental, environmental, interactional, and sociocultural understandings (Sparks, et al. 2011). © R. Taylor 2014 15

2. Practice-based evidence process As a person explores self-managed changes in living their life the process involves constant feedback on how it is working and measuring progress. The problems of a person are addressed through engagement with and intervention in the person’s environment. The foundation of this process is based upon: • Qualitative approaches (human experience). • Feedback loops/action learning (Van de Ven, 2007). • Sequencing of goals (mutual exploration). • Mapping & targeting interventions. • Self-management of data collection, feedback, reflection, and action. • A systems approach involving levels of human-environment interactions. © R. Taylor 2014 16

Practice-based evidence is person centred and outcomes orientated… Evidence-based practice with emphasis upon the treatment itself is being replaced with practice-based evidence including measuring progress (monitoring) and feedback about the relationship (Hubble, et al. 2010). If psychological distress is not self-limiting then exploration in a pragmatic and incremental fashion will lead to an outcome criterion of ‘usefulness’ or ‘successful working’. This is getting a person’s behaviour to work successfully according to the person’s values and desired outcomes in the current context and taking account of all previous experiences (Bach & Moran, 2008). The individual’s efforts to live their life may be helped through often overlapping initiatives: e. g. • Adaptive emotional regulation skill development (psychological treatment) • Recovery work in a primary, community, or home environment. • Changes to the person’s quality of life and environment. Monitoring and feedback informs, guides, and evaluates person-directed exploration of change. This results in accountability and modification of the mix and timing of services in a person-centred fashion. © R. Taylor 2014 17

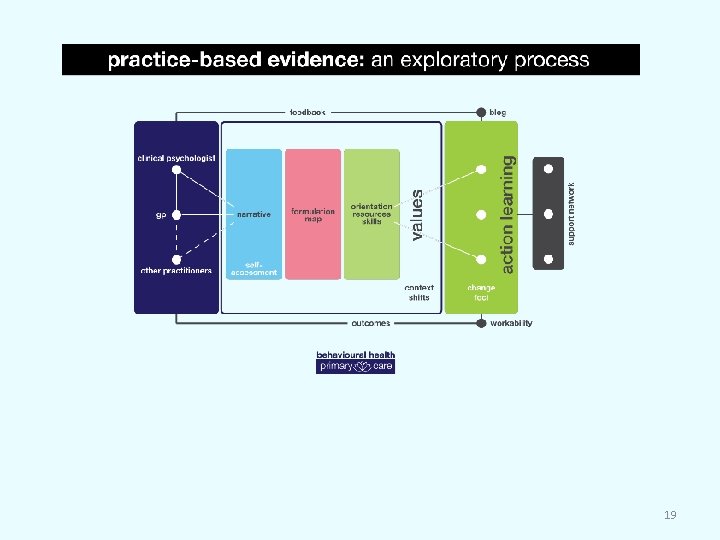
Practice-based evidence: Steps in the process The following are collaborative steps in an exploratory process (see Figure below): A shared narrative in non-technical language. Provision of generic and specific self-assessment tools as required. Completion of the Formulation Map. Orientation, resources & skills development (package – four basic tools). Drawing explicit links between behaviour, values and outcomes. Context-specific action learning. Outcome and relationship measurement and review, formal monitoring and feedback using blogs and new technologies is crucial. © R. Taylor 2014 18
19

Practice-based evidence: How it works Rather than diagnosis and efforts to predict behaviour the primary focus is a mutual exploration of what is required over time. This is predicated on responses to feedback, and continued and improved access to sufficient, appropriate, accessible, responsive and flexible resources and services. This exploratory process drives specific and context-dependent further action in collaboration with the GP and/or expert behavioural health, clinical or counselling psychologist consultant. In primary care a range of emotional problems are involved including self-limiting or relapsing episodes, emotional dysregulation in its various forms, and psychological components to presenting complaints, illness, and disability. Through the multi-modal formulation process the single rural practitioner or small primary care group can prioritize domains of help, and use remote clinical and other psychological disciplines and others to leverage behavioural and other skill sets. Cont… © R. Taylor 2014 20

How it works (cont. ) Problems with emotional regulation are addressed through clinical interventions drawn from ‘third wave’ behaviour and cognitive therapies such as acceptance and commitment therapy, mindfulness-integrated cognitive behaviour therapy, metacognitive therapy, and transdiagnostic treatment for emotional disorders. In supporting autonomy choice is provided, and individuals initiate actions themselves. Self management can be interpreted within the broader context within which people manage their conditions. It involves knowledge, goal setting and problem solving, resources mobilization, self-efficacy (coping and adapting), and collaboration (getting needs met). (Embrey, 2005). The formulation process in the health setting may not fit with the ‘stage’ model of the assessment, formulation, and intervention cycle and may be more recursive and ‘on-the-spot’ as interventions proceed (Cole, S. , 2014). New patterns may emerge quite quickly with new life skills (e. g. mindful awareness) and the link between behaviour and valued outcomes made apparent. Complexity and diversity is germane to working with people within their life context. © R. Taylor 2014 21

The overall task is to improve outcomes and involve service users… Jureidini (2012) has reminded us that success with distressed people is determined mostly by a combination of non-specific factors and natural recovery rather than the direct effects of any specific treatment, pharmacological or otherwise. ‘…more respect should be given to ‘watchful waiting’ – providing a careful assessment to exclude anything acutely dangerous, then monitoring the patient’s well-being without applying a specific intervention…Watchful waiting is different from doing nothing, with which it is often confused. It can be supplemented by a rehabilitation approach, with prescriptions for graded resumption of activities, exercise, healthy eating and other non-specific health enhancing interventions’. (p. 190) Recovery may be the dominant trajectory supported by other interventions: ‘A recovery-focused service requires a shift from professional interventions based on diagnostic labels and prescriptive treatments to individually tailored, consumer -directed planning…collaborative measurement and monitoring of progress provides a tangible way to support and include the consumer voice’ (Miller, et al. 2011, p. 426) © R. Taylor 2014 22

Exploration Paradigm: Value promotion and protecting resources through… • Formulation based on primary care values leading to skilled assessment. • Exploratory sequence reflecting patient priorities which is outcome oriented. • Effectively determining level/type of care and where to start. • A patient-centred focus emphasising functional contexts and self-management. • Quality of life focus and prospects for recovery. • Opportunities for health promotion. • Psychotropic medication and decision review. • Avoiding hospitalization. (Adapted from, Academy of Medical Royal Colleges UK, 2014) © R. Taylor 2014 23

Afterword ’It is said that to be a good clinician one must have a healthy dose of guilt, an obsession with details, and a drive to serve others. The ultimate goal of qualitative health and educational research is understanding the human experience of giving and receiving health care, and of learning, and to use that knowledge as scientists and citizens to improve our mutual lot’. Frankel & Devers (2000, p. 260) © R. Taylor 2014 24

References Academy of Medical Royal Colleges (2014). Protecting resources, promoting value: a doctor’s guide to cutting waste in clinical care. Armstrong, D. , & Earnshaw, G. (2004). What constructs do GPs use when diagnosing psychological problems? The British Journal of General Practice, 54 (505), 580 -583. Bach, P. A. , & Moran, D. J. (2008). ACT in practice: Case conceptualization in acceptance and commitment therapy. Oakland, CA: New Harbinger. Buszewicz, M. , Pistrang, N. , Baker, C. , Cape, J. , & Martin, J. (2006). Patients’ experiences of GP consultations for psychological problems: A qualitative study. The British Journal of General Practice, 56 (528), 496 -503. Broadbent, M. (2013). Innovative sector puts citizens first: Creative use of technology is helping tackle problems. The Weekend Australian, 23 -24 November, p. 12. Cape, J. , Barker, C. , Buszewicz, M. , & Pistrang, N. (2000). General practitioner psychological management of common emotional problems (11): A research agenda for the development of evidence-based practice. The British Journal of General Practice, 50, 396 -400. Cole, S. (2014). Using integrative formulation in health settings (pp. 243 -259). In L. Johnstone, & R. Dallos (Eds. ), Formulation in psychology and psychotherapy, Making sense of people’s problems. Hove, UK: Routledge. Corrie, S. , & Lane, D. (2010). Constructing stories, telling tales: A guide to formulation in applied psychology. London: Karnac. Dew, K. , Dowell, A. , Mc. Leod, D. , Collings, S. , & Bushnell, J. (2005). ‘This glorious twilight zone of of uncertainty’: Mental health consultations in general practice in New Zealand. Social Science and Medicine, 61 (6), 1189 -1200. Dew, K. , Morgan, S. , Dowell, A. , Mc. Leod, D. , Bushnell, J. , & Collings, S. (2007). ‘It puts things out of your control’: Fear of consequences as a barrier to patient disclosure of mental health issues to general practitioners. Sociology of Health and Illness, 29 (7), 1059 -1074. doi: 10. 1111/j. 1467 -9566. 2007. 01022 Embrey, N. (2006). A concept analysis of self-management in long-term conditions. British Journal of Neuroscience Nursing, 2, 507 -513. Van de Ven, A. H. (2007). Engaged scholarship: A guide for organizational and social research. Oxford: OUP. 25

Frankel, R. M. , & Devers, K. J. (2000). Study design in qualitative research-1: Developing questions and assessing resource needs. Education for health, 13 (2), 251 -261. Hubble, M. A. , Duncan, B. L. , Miller, S. D. , & Wampold, B. E. (2010). Introduction (pp. 23 -46). In B. L. Duncan, S. D. Miller, B. E. Wampold, & M. A. Hubble (Eds. ), The Heart and Soul of Change: Delivering what works in therapy. Washington: American Psychological Association. Johnstone, L. (2014). Using formulation in teams (pp. 216 -242). In L. Johnstone, & R. Dallos (Eds. ), Formulation in psychology and psychotherapy, Making sense of people’s problems. Hove, UK: Routledge. Jureidini, J. (2012). Explanations and unexplanations: Restoring meaning to psychiatry. Australia and New Zealand Journal of Psychiatry, 46 (3). 188 -191. doi: 10. 1177/0004867412437347 Lester, H. , Glasby, J. , & Tylee, A. (2004). Integrated primary mental health care: Threat or opportunity in the new NHS? British Journal of General Practice, 54, 285 -291. Lynch, J. M. , Askew, D. A. , Mitchell, G. K. , & Hegarty, K. L. (2012). Beyond symptoms: Defining primary care mental health clinical assessment priorities, content and process. Social Science and Medicine, 74, 143 -149. May, C. , Finch, T. , Mair, F. , Ballinin, L. , et al. (2007). Understanding the implementation of complex interventions in health care: The normalization process model. BMC Health Services Research, 7, 148. Miller, S. D. , Hubble, M. A. , Duncan, B. L. , & Wampold, B. E. (2011). Delivering what works (pp. 421 -429). In B. L. Duncan, S. D. Miller, B. E. Wampold, & M. A. Hubble (Eds. ), The Heart and Soul of Change: Delivering what works in therapy. Washington: American Psychological Association. National Advisory Council on Mental Health (NACMH) (2010). Fitting together the pieces: Collaborative care models for adults with severe and persistent mental illness (Final project report). Monash Alfred Psychiatry Research Centre, 1 -19. Reeve, J. (2010). Interpretative medicine: supporting generalism in a changing primary care world. Occasional paper series 88, 1 -62. London: Royal College of General Practitioners. Sparks, J. A. , Duncan, B. L. , Cohen, D. , & Antonuccio, D. O. (2011). Psychiatric drugs and common factors: An evaluation of risks and benefits for clinical practice (pp. 199 -235). In B. L. Duncan, S. D. Miller, B. E. Wampold, & M. A. Hubble (Eds), The Heart and Soul of Change: Delivering what works in therapy. Washington: American Psychological Association. 26

Contact details: Richard Taylor Clinical Psychologist MACAPP Wheatbelt Clinical Psychology 94 Stirling Terrace, Toodyay, Western Australia 6566 Postal address: PO Box 121, Toodyay, Western Australia 6566 M 0427 447 190 Email: richardt@iinet. au 27
- Slides: 27