Behavioral Health Homes Plus Matthew Hurford M D

Behavioral Health Homes Plus Matthew Hurford, M. D. | Melissa Michael, R. N. October 15, 2015 © 2015 Community Care Behavioral Health Organization

Objectives • Community Care overview • Describe the national landscape of physical and behavioral integration • Share lessons learned from Behavioral Health Homes Plus initiative – Quality improvement approaches from a nonprofit managed care organization © 2015 Community Care Behavioral Health Organization 2

Community Care • Behavioral health managed care company founded in 1996; part of UPMC and headquartered in Pittsburgh • Federally tax exempt nonprofit 501(c)(3) • Major focus is publicly-funded behavioral health care services; currently doing business in PA • Licensed as a Risk-Assuming PPO in PA; NCQAAccredited Quality Management Program • Serving over 1. 6 million individuals in 39 counties through a statewide network of over 1, 800 providers © 2015 Community Care Behavioral Health Organization 3
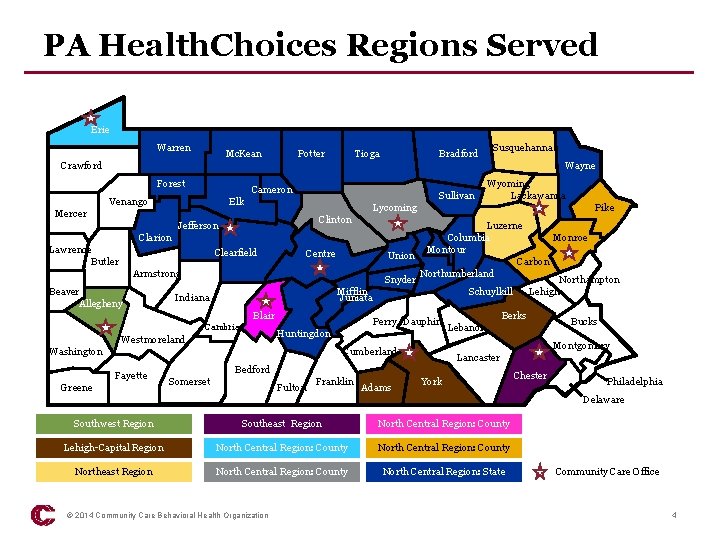
PA Health. Choices Regions Served Erie Warren Mc. Kean Potter Tioga Bradford Susquehanna Crawford Wayne Forest Cameron Venango Sullivan Elk Lycoming Mercer Clinton Jefferson Clarion Lawrence Butler Clearfield Centre Armstrong Beaver Allegheny Mifflin Juniata Indiana Blair Cambria Huntingdon Westmoreland Greene Berks Lebanon Lancaster Bedford Fulton Franklin Adams Bucks Montgomery Cumberland Somerset Pike Luzerne Columbia Monroe Montour Union Carbon Northumberland Snyder Northampton Schuylkill Lehigh Perry Dauphin Washington Fayette Wyoming Lackawanna York Chester Philadelphia Delaware Southwest Region Southeast Region North Central Region: County Lehigh-Capital Region North Central Region: County Northeast Region North Central Region: County North Central Region: State © 2014 Community Care Behavioral Health Organization Community Care Office 4

Mission and Vision • Improve the health and well-being of the community through the delivery of effective and accessible behavioral health services • Improve the quality of services through a stakeholder partnership focused on outcomes • Support high-quality service delivery through a nonprofit partnership with public agencies, experienced local providers, and involved members and families © 2015 Community Care Behavioral Health Organization 5

Integrate Quality Improvement into Health Initiatives © 2015 Community Care Behavioral Health Organization

New Models of Care Delivery • New models of care delivery are important for behavioral health: – World Health Organization ranks depression, alcohol, and tobacco use among the top causes of disability – Individuals may be at higher risk for health conditions due to the psychiatric medications or other medications they are prescribed – Individuals who have a serious mental illness (SMI) have a mortality rate that is higher than comparison groups – mostly due to medical conditions, such as cardiovascular disease or diabetes © 2015 Community Care Behavioral Health Organization 7

The Need for Integrated Systems 68% of adults with mental health (MH) conditions also have medical conditions People with MH conditions: 25% of adult population 68% of adults with mental health conditions have medical conditions © 2015 Community Care Behavioral Health Organization People with medical conditions: 58% of adult population 29% of adults with medical conditions have mental health conditions http: //www. integration. samhsa. gov/workfor ce/mental_disorders_and_medical_comorb idity. pdf
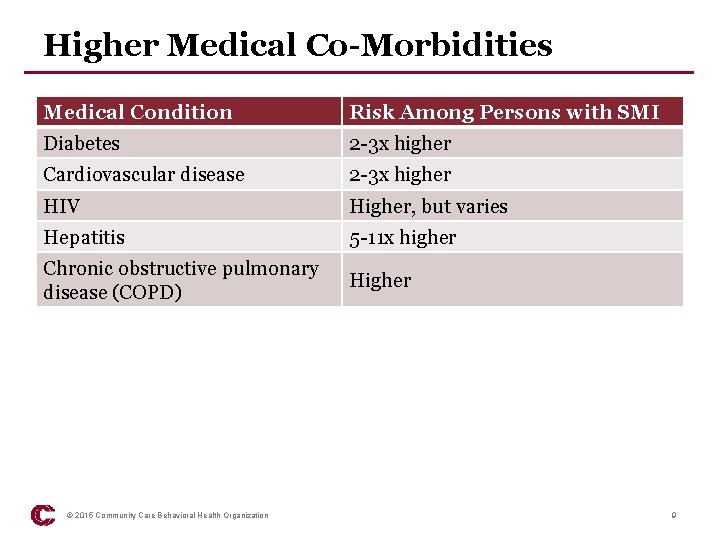
Higher Medical Co-Morbidities Medical Condition Risk Among Persons with SMI Diabetes 2 -3 x higher Cardiovascular disease 2 -3 x higher HIV Higher, but varies Hepatitis 5 -11 x higher Chronic obstructive pulmonary disease (COPD) Higher © 2015 Community Care Behavioral Health Organization 9

Key Points • Increased morbidity & mortality associated with SMI – Largely due to preventable medical conditions: metabolic disorders, cardiovascular disease & high prevalence of modifiable risk factors (e. g. , obesity, smoking) • Some psychiatric medications contribute to risk • Traumatic stress exposure can lead to both mental & medical illness • Established monitoring & treatment guidelines to lower risk are underutilized in SMI populations • Co-morbid substance abuse can increase burden of medical illness • Social factors are key contributors to medical status © 2015 Community Care Behavioral Health Organization 10

Behavioral Health Home Model © 2015 Community Care Behavioral Health Organization

Behavioral Health Home Plus • Designed to demonstrate the efficacy of care coordination of PH/BH services for individuals with SMI & co-occurring medical conditions • Successful collaboration with Community Care and BH providers in PA over the past six years: – Creating health homes in BH agencies – Development of a wellness culture through wellness coaching training – Case managers, certified peer specialists, and nurses as health navigators – Web portal with wellness tools and resources © 2015 Community Care Behavioral Health Organization 12

Community Care’s Approach • Enhance PH competencies in BH delivery system • Use a collaborative model • Ensure financial feasibility • Outcomes oriented, data-informed • Guided by mission and values – Recovery – Resilience – Empowerment © 2015 Community Care Behavioral Health Organization 13

Financing Strategy for BHH • Fee-for-service • Pay for Participation (P 4 P) – Provide an incentive for providers to report data and to participate in a collaborative quality improvement initiative (e. g. , attendance at training) – Initial payment, once letter of commitment is signed by provider (50% of total amount), then the remaining 50% once providers have completed the following implementation steps © 2015 Community Care Behavioral Health Organization 14

Pay for Participation (P 4 P) • Agency develops leadership team who will participate in BHH planning and implementation • Agency will hire/appoint a wellness nurse to serve as the Lead Health Navigator as the agency’s internal leader for Behavioral Health Home implementation • Agency staff participating in BHH activities will have Web access to: – Access patient level health info, wellness self-management tools – Gather outcomes information about participants in BHHP • Agency will support integration of wellness coaching into usual clinical activities • Agency will establish collaborative relationships with PCP/medical specialty offices © 2015 Community Care Behavioral Health Organization 15

Melissa Michael, RN Behavioral Health Home Model © 2015 Community Care Behavioral Health Organization

Community Care BHHP • Behavioral Health Home Plus (BHHP) • Initially developed by Community Care in 2009 with teams in the North Central region of PA • Designed to integrate PH/BH services for individuals with SMI & co-occurring medical conditions © 2015 Community Care Behavioral Health Organization 17

The BHHP Model • Provide a person-centered system of care • Develop “virtual team” for each individual to coordinate physical, behavioral, and supportive services • Use wellness coaching – Develop person-centered plan with individual – Enhanced PH competencies in BH team – Promote health, wellness, recovery, use of personal medicine, and self-management © 2015 Community Care Behavioral Health Organization 18

BH Home Key Components • Wellness nurse • Health navigators • Member registry and a Web portal • Comprehensive care team • Program tools for members and providers © 2015 Community Care Behavioral Health Organization 19

Member Registry • Information provided by Community Care to identify members who have both physical health and mental health needs • Population identification • Stratification • Pharmacy and BH data © 2015 Community Care Behavioral Health Organization 20

Health Home Team Members • Member and their family • Wellness nurse • Health navigator • Primary care provider • Psychiatrists and mental health clinicians • Community Care specialized care manager • Health Plan special needs resource specialist © 2015 Community Care Behavioral Health Organization 21

Health Home Team Members • Wellness coaching/health navigators – Certified peer specialist • Assists with engaging member and securing informed consent; if requested, accompanies member to appointments and coaches member to support his/her own advocacy within health care system – Case manager • Provides enhanced case management services accessing and coordinating both physical and behavioral health services © 2015 Community Care Behavioral Health Organization 22

Health Home Team Members • Trained in wellness coaching in order to: – Apply wellness principles and coaching techniques – Assist individuals to identify strengths to achieve wellness goals – Model wellness and recovery – Advocate for unmet needs – Accompany individual to community appointments if asked – Provide peer support through stages of change – Create environments that promote wellness and recovery practices © 2015 Community Care Behavioral Health Organization 23

Health Home Team Members • Wellness nurse – Provides clinical consultation/interface with PH and BH clinicians and member – Identifies high-risk people in care – Assures completion of wellness physical assessment – Uses disease registry to monitor progress for each person participating – Coordinates and collaborates with PCP and specialty medical providers – Supervises wellness coach process by HN – Wellness education for people in care, families and staff © 2015 Community Care Behavioral Health Organization 24
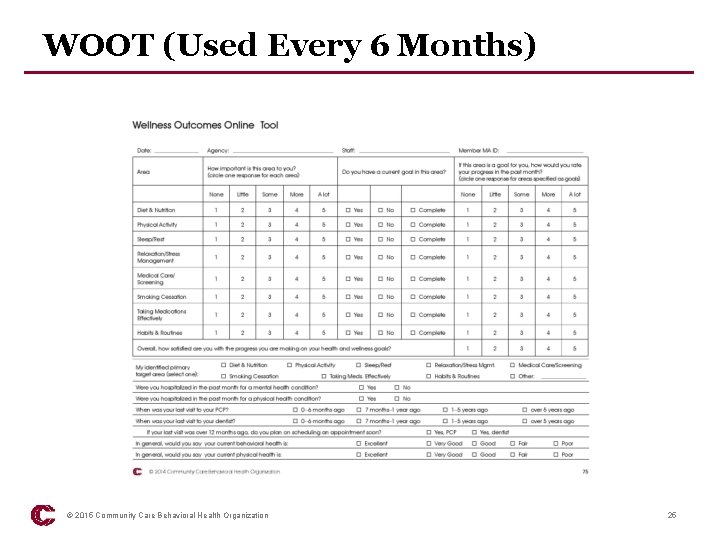

WOOT (Used Every 6 Months) © 2015 Community Care Behavioral Health Organization 25

Health Home Team Members • Primary physical health provider (virtual team member) – Provides physical health clinical services; has access to behavioral health team services and supports – Ongoing reciprocal communications with all team members © 2015 Community Care Behavioral Health Organization 26

Health Home Team Members • Community Care specialized care manager – A high risk care manager from community care that provides assistance to the health home regarding members strengths, care history and treatment plans. © 2015 Community Care Behavioral Health Organization 27

Health Home Team Members • Health Plan special needs resource specialist – High risk care manager from the physical health plan who assists with coordination for physical health needs – Can provide members strengths, physical needs, past physical treatments, and medication lists. © 2015 Community Care Behavioral Health Organization 28

Health Home Team Members • Member and their family – Choose an area for self-management – Develop new self-management strategies – Set a SMART goal and create action plan – Implement plan with intention of meeting goal – Monitor how plan is working – Adjust plan as needed © 2015 Community Care Behavioral Health Organization 29

Tools for Members and Providers • Self-management toolkits: – Diet and nutrition – Physical activity – Sleep – Stress management – Medical and behavioral care and recommended screenings (“know your numbers”) – Smoking cessation – Taking medications effectively © 2015 Community Care Behavioral Health Organization 30

Other Components of BHHP • BHHPE learning collaborative • Psychiatric provider physical health webinars – DM, HTN, CVD, COPD, HIV/HEPATITIS C, preventative health, tobacco cessation, metabolic syndrome, stress & physical health • Outcomes monitoring • Case conferences to support best practice © 2015 Community Care Behavioral Health Organization 31

Implementing the BHHP 1. Engaging stakeholders 2. Pay for Performance 3. Training: IHI learning collaborative implementation model – Wellness coaching training – Secure member portal training – Self-management toolkits – Physician(psychiatrist) training 4. Quality Improvement Processes © 2015 Community Care Behavioral Health Organization 32

Community Care’s Role • Analyze and stratify the population • Standardize the model across behavioral health providers, including training and technical assistance • Utilization and outcomes reporting • Facilitate information exchange and provide notice of key events • Provide specialized high-risk care management, including pharmacy management, with: – Oversight/consultation of person centered planning – Facilitation of data and information sharing with the health home team © 2015 Community Care Behavioral Health Organization 33

The Learning Collaborative Structured approach for change Adopt best practices in multiple settings Time-limited learning process © 2015 Community Care Behavioral Health Organization Uses adult learning principles & techniques Shared learning and collaboration 34

BHHPE LC Mission • The mission of the LC is the primary purpose or focus of the quality improvement effort – To implement behavioral health homes to improve the whole health and wellness of members with complex health conditions – To increase engagement and activation of the person in their care – To improve collaboration between PH/BH providers © 2015 Community Care Behavioral Health Organization 35
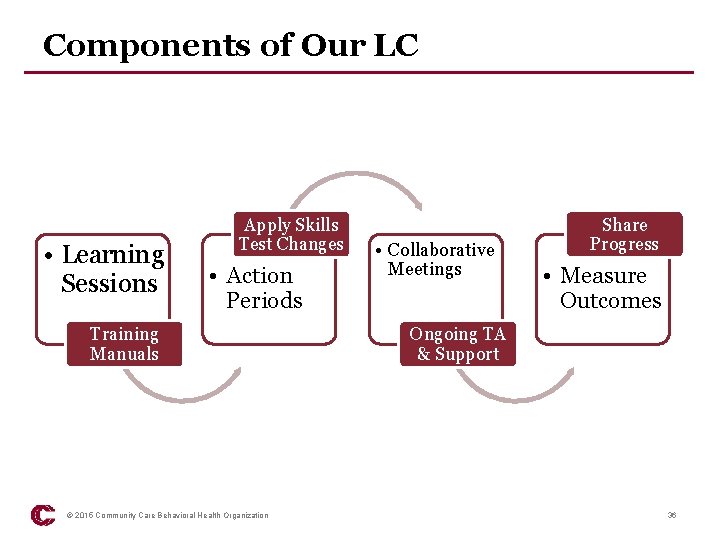
Components of Our LC • Learning Sessions Apply Skills Test Changes • Action Periods Training Manuals © 2015 Community Care Behavioral Health Organization • Collaborative Meetings Share Progress • Measure Outcomes Ongoing TA & Support 36

Quality Improvement Processes • Measure coordination of care with primary care providers • Engagement of members in physical health and wellness programs who had not previously attended to those issues • Documentation of decreased emergency department and acute medical service utilization • Enhance medication adherence to specific medications for chronic medical illnesses © 2015 Community Care Behavioral Health Organization 37

Initial Results: Positive Engagement • Strong engagement by members • PH and wellness concerns become routine part of recovery plan • Nurses and case managers partner to address PH concerns © 2015 Community Care Behavioral Health Organization 38

Learning Collaborative Aims • Process Aim 1: Wellness – By September 2015, 80% of all individuals presenting with complex needs will have completed the wellness planning tool • Process Aim 2: Assessment – By September 2015, 80% of all individuals presenting with complex needs will have completed a health assessment • Outcome Aim: Involvement – By September 2015, 80% of individuals engaged in BHHPE will report being highly involved (rated a 9 or 10) in working with their behavioral health service provider on physical health and wellness as measured by a 10 -point involvement question © 2015 Community Care Behavioral Health Organization 39
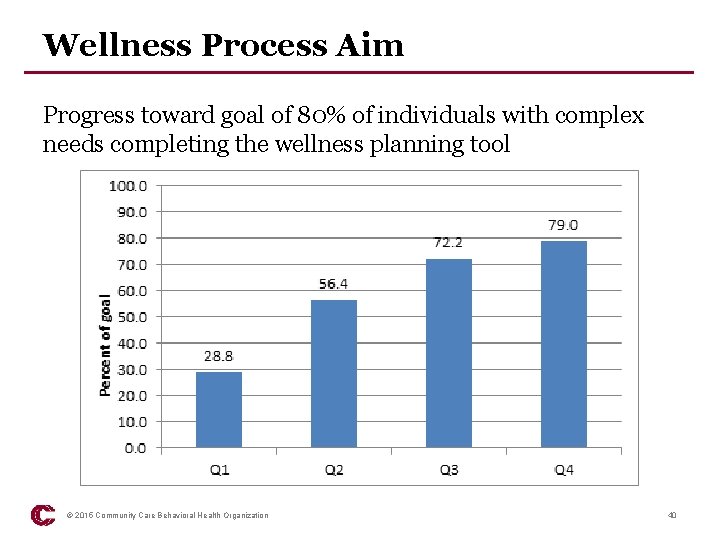
Wellness Process Aim Progress toward goal of 80% of individuals with complex needs completing the wellness planning tool © 2015 Community Care Behavioral Health Organization 40
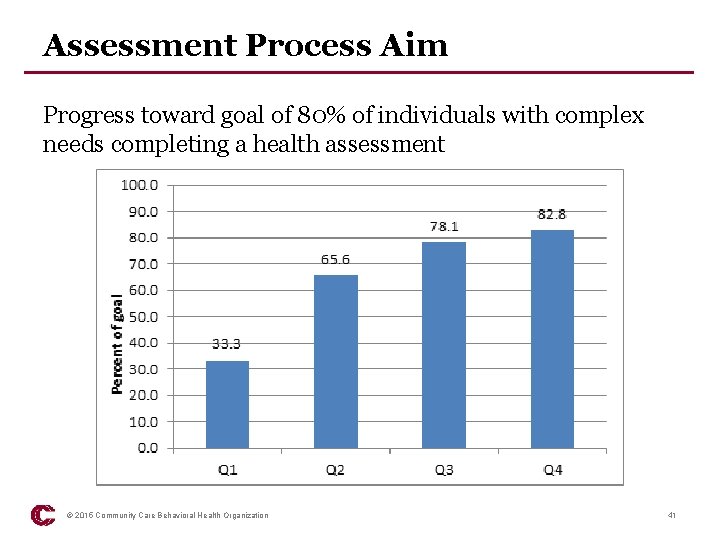
Assessment Process Aim Progress toward goal of 80% of individuals with complex needs completing a health assessment © 2015 Community Care Behavioral Health Organization 41
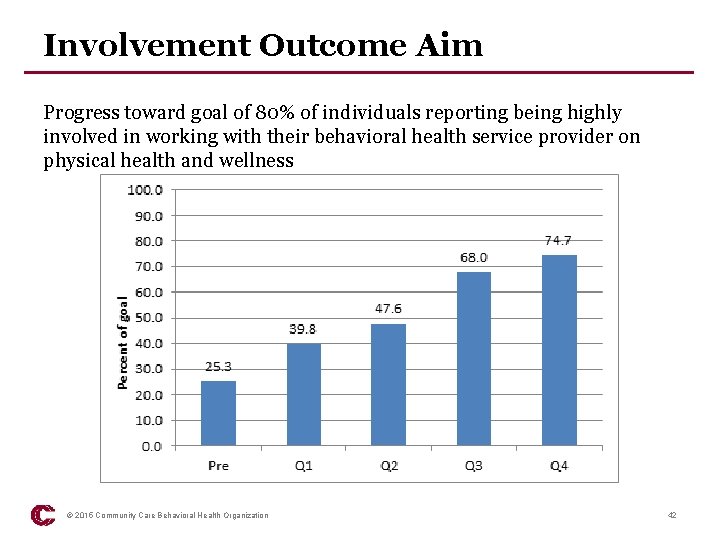
Involvement Outcome Aim Progress toward goal of 80% of individuals reporting being highly involved in working with their behavioral health service provider on physical health and wellness © 2015 Community Care Behavioral Health Organization 42

Lessons Learned: What Worked • BHHPE learning collaborative • Psychiatric provider physical health webinars – DM, HTN, CVD, COPD, HIV/HEPATITIS C, preventative health, tobacco cessation, metabolic syndrome, stress & physical health • Use of disease registry • Outcomes monitoring • Case conferences to support best practice © 2015 Community Care Behavioral Health Organization 43

Lessons Learned: Challenges • Implementing population management • Ongoing psychiatrist/prescriber involvement • Need for EMR (electronic medical records) • Some provider not having computer access • Staff turnover: need for additional wellness coach training • Provider and member commitment to a new wellness culture © 2015 Community Care Behavioral Health Organization 44
- Slides: 44