Behavioral Gerontology Linda Le Blanc and Allison Jay

Behavioral Gerontology Linda Le. Blanc and Allison Jay 1

Aging in America ¨ The proportion of the population over age 65 in the U. S. has risen from 4% to 13% in the 20 th Century – Predicted to be 20% of the population by 2030 ¨ Many factors contribute – Medical advances have increased life expectancy • 1900: 47. 3 years • 1950: 67 years • 2000: 76 years – Aging of Baby Boomers 2

Effects of Aging ¨ Living longer means a substantial portion of elders live with chronic illness and disability – Higher total cost of care – Greater care needs – Potentially lower quality of life 3

Behavioral Gerontology ¨ Application of behavioral theory and principles to aging issues – Clinical/Rehabilitation Issues – OBM/Staff Training Issues ¨ Small sub-field of behavior analysis that needs new interested students – Check out the Behavioral Gerontology SIG at ABA ¨ Different approach to aging from typical medical model of inevitable biological decline 4

Behavioral Gerontology ¨ From a behavioral perspective, when a person ages – Fewer discriminative stimuli control behavior – Different establishing operations are likely – Contingencies of reinforcement tend to support the wrong behaviors ¨ Leads to behavioral deficits like – memory problems, incontinence, overdependence ¨ And behavioral excesses like. . . 5

Need For Behavioral Gerontology ¨ Behavior Excesses (Behavior Problems): – Aggression, Wandering, Repetitive vocalizations ¨ Behavior problems are – Major cause of caregiver stress – The most common cause of institutionalization • Not a health decline but “can’t take it anymore” on the part of the caregiver – Very common in nursing homes • 64% have significant problems (Zimmer et al, 1984) • Can lead to high staff turnover 6

Obstacles to widespread behavioral services ¨ Practitioners are reluctant to serve elders – no training ¨ Older people and caregivers perceive stigma for accessing mental health services – Older adult: means “I’m crazy” – Caregiver: “a good son/daughter/wife/husband” could handle it without help ¨ Medical Model Myths – Psychotropic medications are the only thing that will work - most common intervention – Once a skill is lost it cannot be regained ¨ Cost and effort constraints – Simple and/or cheap will always be selected 7

Common mental health problems for elders ¨ Depression and Anxiety ¨ Dementia related behaviors – Losses or declines in memory, conversation, socialization, and activity engagement – Incontinence – Increases in problem behaviors • Aggression • Repetitive Vocalizations • Wandering 8

Anxiety and Depression ¨ Often undetected in elders because – Physicians and patients fail to recognize it • Focus on physical symptoms rather than mental health • Emotional issues are reported as physical symptoms (e. g. , fatigue, heart rate problems) • View it as typical aging to be sad and worried ¨ Anxiety – About 6% of healthy elders have clinical anxiety (APA, 1998) – Higher rates in elders with medical conditions ¨ Depression – Occur in 2 - 10% of older adults; 2 x more in women – 30 -50% of people in nursing homes 9

Behaviorally. . . why ¨ Depression and anxiety might increase because. . . – Motivative operations – Reinforcer availability/loss – Discriminative stimuli – Others 10

Behavior Therapy ¨ Individual or group based therapy that focuses on the role of: – Activity and social engagement – Access to reinforcers for non-depressed behaviors – Negative self-statements – Problem – solving skills ¨ Elders who complete therapy tend to benefit as much or more than younger adults – Often a preference for group therapy 11

Nursing Homes ¨ Depressed affect can increase risk of nursing home placement (Cohen-Mansfield & Wirtz, 2007) ¨ Nursing homes – Absence of meaningful opportunities for engagement – No social interaction or conversations – Increased depression and memory problems – High rates of problem behavior – Excess disability ¨ Behavioral gerontologists have tackled each of these problems successfully 12

Bourgeois (1993) ¨ “Effects of memory aids on dyadic conversations of individuals with dementia” ¨ Patients with dementia appear incoherent in conversation because they – Substitute vague words for specifics – Drop out content and theme – Cannot spontaneously generate topics ¨ Interventions such as memory wallets result in better conversations 13

My Nieces: Caroline, Courtney, Jessica 14

My favorite color is blue. My cat is Mr. Snuffles and he is a Siamese. 15

I live at 427 Bloomfield Ave 16

Bourgeois (1993) ¨ Two demented patients in conversation ¨ Participants: 5 women & 1 man at adult day care centers ¨ Memory aid for one of the two was used in each conversation – Interviewed family members to develop list of facts and topics – Took corresponding pictures to include in wallet ¨ 5 minute conversations 3 times per week – Measured on-topic statements and statements related to the memory aid 17

18

Bourgeois (1993) ¨ Research design = – Reversal (BAB) ¨ Effects – Noticeably more on-topic statements related to aids and to other areas (except one) for target client – Also more for the partner - it wasn’t their aid! – Least effects were when both partners were extremely impaired ¨ Social Validity – 13 Speech Staff listened to tapes and rated quality – Aided conversations rated higher on staying on topic, ambiguity, comfortability, 19

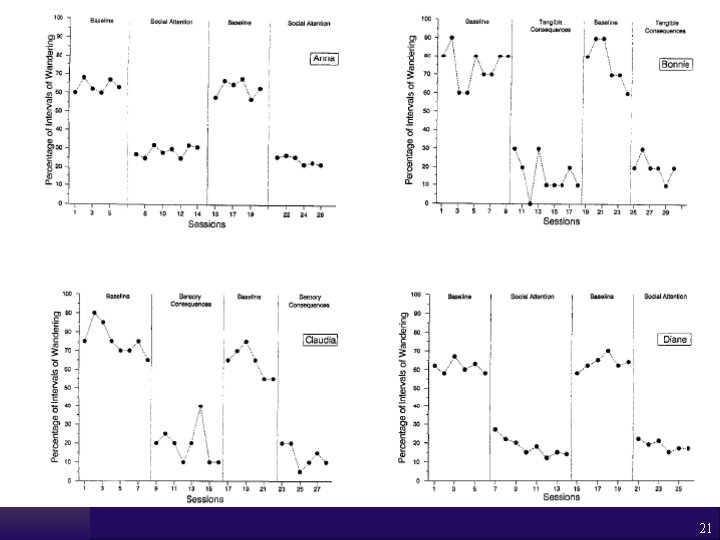
Heard & Watson (1999) ¨ Targeted wandering in demented individuals in nursing homes using a functional behavioral approach ¨ Tracked wandering in 35 -40 minute episodes; in how many intervals did it occur ¨ Found different reasons or functions for why wandering occurred – Attention – Access to food – Sensory stimulation ¨ Used that reinforcer in a DRO procedure to decrease wandering 20
21

¨ Research Design = – Reversal (ABAB) ¨ Effects = – Clear effects for each participant – Decreased intervals with wandering by ½ for each participant • What implication for this continued level of behavior? 22

The Intersection of Gerontology and OBM ¨ Direct care staff in nursing homes – Are called CNAs (Certified Nursing Assistant) – Are often receiving low pay and working long hours – Have many potentially unpleasant aspects to their job – Are often kind people who sincerely want to help – Often have no idea that their actions are directly contributing to an environment that • Suppresses independence and activity • Reinforces problematic behavior 23

The Intersection of Gerontology and OBM ¨ Staff training and performance monitoring are a critical part of providing good care in nursing home settings ¨ Staff will often acquire knowledge of procedures in in-service then fail to use the procedures when they interact with clients – No system in place to make it worthwhile or feasible to maintain new procedures 24

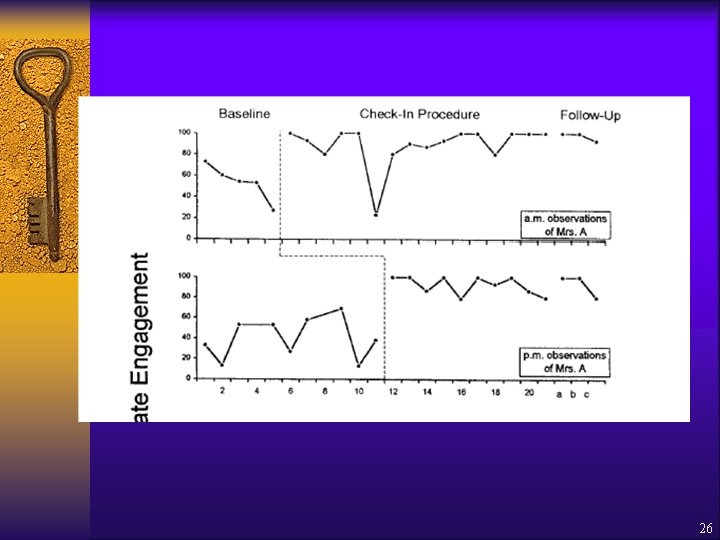
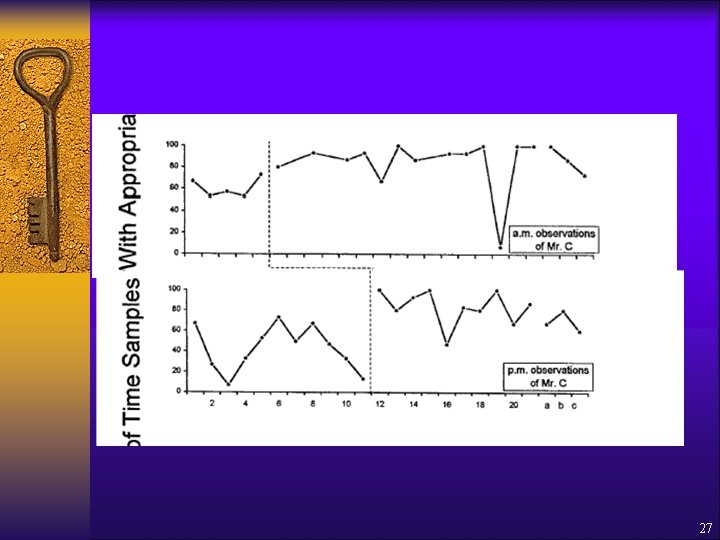
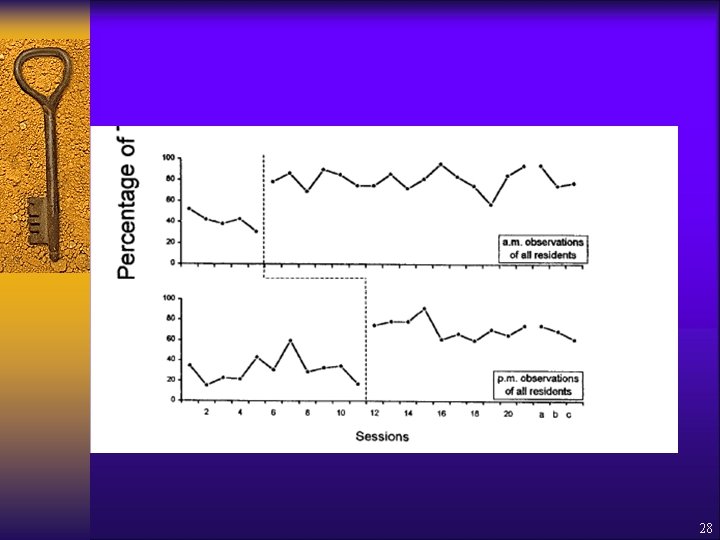
Engelman, Altus & Mathews (1999) ¨ Increasing engagement in daily activities ¨ 5 residents with dementia ¨ Intervention: – CNA training to get staff • Interacting with each client every 15 min • Offering activity choices • Praising activity – Written feedback on CNA performance ¨ Measured appropriate engagement, inappropriate engagement, no engagement ¨ Research Design = 25
26
27
28

Engelman, Altus & Mathews (1999) ¨ Results = – All participants experienced increased appropriate engagement • over 80% of intervals in morning • over 70% of intervals in afternoon – Greater diversity of activities • 7 in baseline, over 20 in intervention 29

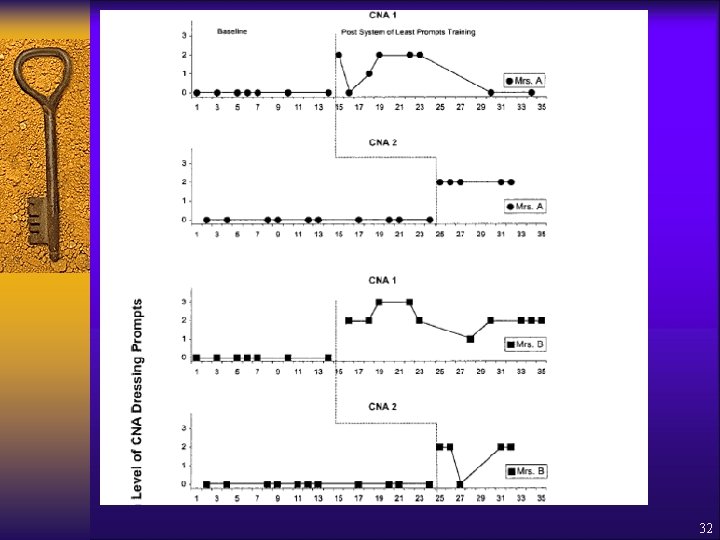
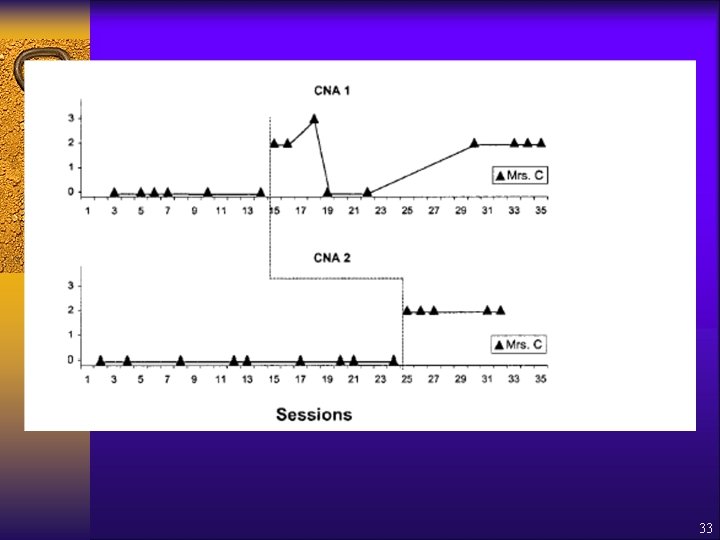
Engelman, Altus, Mosier & Mathews (2003) ¨ Well meaning staff may increase resident dependence by doing everything for them ¨ System of “Least to Most” Prompts ensures opportunity to perform independently – Verbal – Gestural – Physical ¨ Intervention – Interactive 30 min training on SLP (model, rehearse, feedback) – Feedback on job; Daily Monitoring of Client Performance by CNA 30

Engelman, Altus, Mosier & Mathews (2003) ¨ Participants: 2 CNAs; 3 elders with dementia ¨ Measured – CNA use of SLP – Time it took to dress*** ¨ Research Design = multiple baseline across participants ¨ Results = – Prompts increased for all CNAs across elders – No increase in time it took to dress elder (6. 7 vs. 6. 5 min) 31
32
33

Conclusions ¨ Increasing need for professionals with experience and expertise in aging ¨ Opportunity to create new models for service delivery that allow individuals to retain independence as long as possible ¨ Allows you to blend clinical and OBM interests 34

Practicum in Behavioral Gerontology ¨ New model of service delivery – Day program so they live at home longer – Respite for caregivers – Activities and care for participants ¨ Physical, Medical, Cognitive Disabilities ¨ Active Behavioral Programming – Increased engagement, decreased problem behavior ¨ Advanced Practicum if you do well – OBM and clinical opportunities 35

¨ Practicum for Psychology Students - WMU – Year round – 3 credit hours Contact Allison. Jay@wmich. edu http: //wmu. aging. practicum. googlepages. com/home 36
- Slides: 36