Before you prescribe psychotropics in primary care Kathryn

Before you prescribe psychotropics in primary care Kathryn Fraser, MD Professor of Psychiatry Medical Director of UNM Psychiatric Center START Clinic

Objectives 1. Know basic diagnostic criteria for common psychiatric disorders 2. Be aware of common medical disorders with “psychiatric symptoms” and understand effect of substance use on “psychiatric symptoms” 3. Know indications and relative contraindications of commonly used psychotropic medications

Psychiatric Disorders

Psychiatric HX • HPI focusing on psychiatric symptoms: mood, anxiety, sleep, appetite, concentration, suicidal thoughts/actions, homicidal thoughts/aggression, psychotic symptoms (delusions and hallucinations), hypomanic or manic symptoms. • Past Psych Hx (Medications tried, hospitalizations, suicide attempts); Check PMP and external rx • Current and past substance use (UDS helpful and/or review ER/PES records); • Family Psych and Substance Hx • Social Hx: support system, strengths; ask if in a safe living situation, any current/past legal problems

Mental Status Exam • • • General appearance and attitude Speech Mood Affect Thought process Suicidal thoughts/actions (get details) Homicidal thoughts/aggression (get details) Psychotic symptoms (delusions, hallucinations) Judgment/Insight Cognitive screen (orientation, short term memory, serial 7’s; Consider MOCA if memory seems impaired)

Before Making a Psychiatric Diagnosis • Consider if symptoms caused by medical illness(es): endocrine, anemia, vitamin def, obstructive sleep apnea • • ABC Mnemonic for organic mimics (Dorsey 2002) : A and B Airway and breathing (PE, CO poisoning, COPD) C CNS and CV ( head trauma, CVA, CNS neoplasms, MI) D Drugs and Meds (all illicit drugs/ETOH/benzo use/withdrawal, caffeine, corticosteroids, serotonin syndrome, phenothiazine anti-emetics) E Electrolytes and endocrinology (low glu/sodium/potassium, low/high calcium/thyroid/adrenal) F Fever and chills (UTI, pneumonia, endocarditis, meningitis, encephalitis G-Z Others (SLE, Parkinson’s, HIV dementia, pancreatic cancer, uremic/hepatic encephalopathy) • • • Consider if symptoms caused by substance use and/or withdrawal. Usually can be diagnosed by history, physical, labs, chart review, collateral history (if available). If you miss this and person doesn’t improve with treatment, re-consider ongoing/intermittent substance use Certainly possible to have Psych+Medical+Substance use as causes of symptoms Dorsey ST. Medical Conditions that Mimic Psychiatric Disease: A systematic approach for evaluation of patients who present with psychiatric symptomatology Emergency Medicine Reports Sept 22, 2002. AHCmedia. com.

Questions • As a group, what is the most common type of psychiatric disorder? • As a group what is the second most common type of psychiatric disorder? • As a group what is the third most common type of psychiatric disorder? • Kessler RC, et al Lifetime Prevalence and Age of Onset of DSM IV D/O in NCSR, Arch Gen Psych 62. 2005

Anxiety Disorders

General Thoughts • Anxiety is part of the human condition: autonomic arousal required for survival: flight, fight or freeze • Disorders have excessive symptoms and/or persist beyond developmental or cultural norms • Genetics 30 -40% and rest environmental: early life stress, attachment, sexual/physical/neglect abuse as child • Very common: 25% lifetime (second only to substance use d/o) although not diagnosed when due to a medical d/o or substance/med/another psych condition

Adult Anxiety Disorders (12 month prevalence) Specific phobia 7 -9% (often >1) Social anxiety (phobia) disorder 7% Generalized Anxiety d/o (GAD) 3% Panic disorder 2 -3% (with or without agoraphobia) • Substance/medication induced use/withdrawal • Anxiety due to another medical condition • •

Tips to Differentiate • Specific phobia: fear/anxiety responses to specific stimulus: spiders, snakes, etc. • Social phobia: fear/anxiety to parties, public speaking, etc. • GAD: at least 6 months of worries about almost everything most of the time (physical, cognitive, emotional symptoms) • Panic disorder: discrete episodes of anxiety that come on suddenly for no apparent reason and usually last no more than a few minutes-half hour; sometimes with fear of death, losing control, “going crazy”; end up in ER often first few times

Question: • A patient has hx of palpitations, sweating and intense anxiety. Panic disorder would be the most likely dx if her symptoms occur when she: • A. is reminded of a previous assault • B. must use a public restroom • C. attends a large party • D. is in any setting • E. must use an elevator

Cognitive Behavior Therapy (CBT) • Very effective for all forms of anxiety disorders (meta analysis of 43 controlled studies showed CBT more effective than medications for panic d/o 70%> 53% (although both together >70% response) • CBT: thoughts lead to feelings which cause distress; identify the thoughts and change them (over time) leading to change in feelings and reduced distress

Medications • Antidepressants (first line) • A. Selective Serotonin Reuptake Inhibitors (SSRIs) (fluoxetine, sertraline, citalopram, escitalopram, paroxetine) • B. Serotonin Norepinephrine Reuptake Inhibitors (SNRIs) • (second line) (venlafaxine, duloxetine) • C. Tricyclic (TCAs: imipramine, doxepin, amitriptyline, nortriptyline) • D. Others: trazodone, nefazodone, MAOIs • Benzodiazepines (second line, although sometimes used with antidepressants) (can interfere with CBT and problems with misuse/dependence) • Buspirone (especially useful in patients with ETOH/other substance use hx) • Others: neurontin, pregabalin, propranolol (especially for performance anxiety), hydroxyzine, clonidine, prazosin, seroquel)
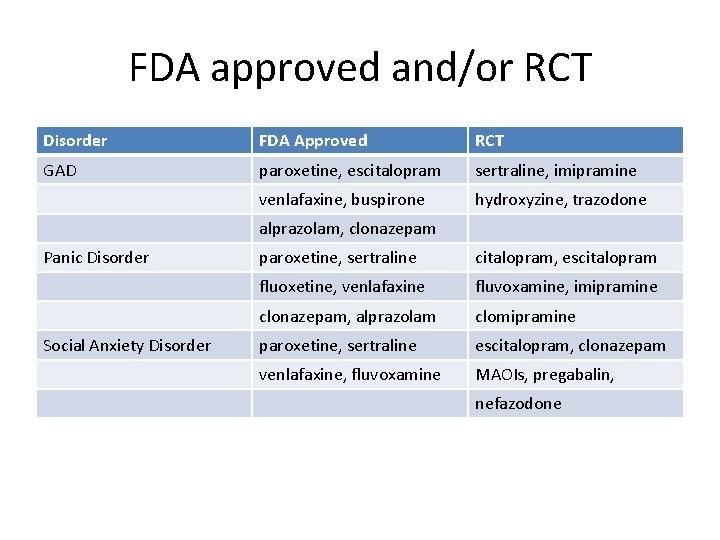
FDA approved and/or RCT Disorder FDA Approved RCT GAD paroxetine, escitalopram sertraline, imipramine venlafaxine, buspirone hydroxyzine, trazodone alprazolam, clonazepam Panic Disorder Social Anxiety Disorder paroxetine, sertraline citalopram, escitalopram fluoxetine, venlafaxine fluvoxamine, imipramine clonazepam, alprazolam clomipramine paroxetine, sertraline escitalopram, clonazepam venlafaxine, fluvoxamine MAOIs, pregabalin, nefazodone

Suggestions • GAD: two SSRIs: sertraline and fluoxetine (or others but not paroxetine) buspirone short term (hopefully) clonazepam/lorazepam Panic Disorder two SSRIs (as above) and venlafaxine clonazepam (possibly short term)

Before prescribing • Consider if pregnant: order pregnancy test (if pregnant avoid benzos and paroxetine/Paxil) • SSRIs: most common side effects: nausea, GI, sexual dysfunction; can cause anxiety and insomnia; if patient has Bipolar I or II could cause irritability or manic/hypomanic symptoms (can happen with any antidepressant) • Venlafaxine/Effexor: at higher doses (over 150 mg) can increase blood pressure and important to taper off slowly to avoid unpleasant discontinuation syndrome • If patient has ETOH use disorder don’t prescribe benzos for anxiety (be careful if has past use hx) • If chronically suicidal and/or hx suicide attempts don’t prescribe benzos and usually not TCAs

Question • A 35 year old woman has been on 20 mg of citalopram for the past 3 months for panic disorder and currently has hardly any symptoms. No prior psychiatric history. How long should she continue this medication? (36) • A. 4 weeks • B. 3 months • C. 1 year • D. 3 years • E. Indefinitely

Prognosis • Even with good treatment, for many these are chronic illnesses; about a third can get complete remission • Keep recommending psychotherapy if patients haven’t tried it; even a few sessions of CBT can be helpful and there are no side effects! • Be aware that anxiety as a symptom is a risk factor for suicide so always ask about that

PTSD and Acute Stress Reaction (Trauma and Stress Related Disorders) • • Acute stress reaction (common) 1. Suffering a trauma (as below) 2. Duration 2 days to one month 3. Symptoms similar to PTSD (see below) • • PTSD (more than half population with serious trauma but PTSD 8 -12% in US) 1. Suffering/witnessing a serious trauma (actual or threat of death, serious injury, sexual violence) 2. Indirectly by hearing that close relative or friend has died by accident or violence 3. Repeated direct exposure to consequences of above (first responders, OMI, professionals exposed to child abuse) Intrusive symptoms (nightmares, flashbacks), Persistent avoidance, Negative cognitions and mood, Hyperarousal and reactivity • • Symptoms persist beyond a month which cause distress and affect functioning; not caused by substance, medication or illness

Question • What is the leading cause of disability in the world for persons 15 -44 years old? (143) • A. Bipolar disorder • B. Schizophrenia • C. Self inflicted injuries • D. Unipolar major depression • E. Alcohol use

Depressive Disorders

Major Depressive Disorder • Must have either depressed mood or loss of pleasure/interest (or can have both) and at least 4 (if both of above) or at least 5 (if only 1 of above) of below: • Weight loss or gain or increased/decreased appetite • Insomnia or hypersomnia • Psychomotor agitation or retardation • Fatigue or loss of energy most of the time • Feelings of worthlessness or guilt • Poor concentration • Recurrent thoughts of death, recurrent suicidal ideation and/or specific attempt or plan to kill self • For at least 2 weeks causing significant dysfunction • Not attributable to substance use or another medical condition

Other considerations • Always as about suicidal thoughts/plans/previous attempts (and any protective factors) • Always ask about psychotic symptoms (auditory hallucinations and/or delusions) • Always ask about homicidal thoughts particularly towards children if they are caring for kids • Always ask about substance use and check labs, UDS if possible • Always ask about current/past hypomanic or manic symptoms (could indicate Bipolar d/o rather than Unipolar depression)

Epidemiology • 12 month prevalence: 7% all but higher in 1829 year olds, women • Lifetime: 16% ( approx. 10% for men and 20% for women) • Women more likely to attempt suicide but less likely to “succeed” (exception: women physicians and nurses)

Treatment • Ask again about substance use and if actively drinking, using meth, cocaine, opiates (? ) person may not have underlying MDD; needs treatment for substance use first • Safety: if in doubt send for mental health eval (PES) • Psychotherapy CBT (especially for mild-moderate depression)

Medication SSRIs (try two before switching to another med) SNRIs Mirtazapine, Trazodone, Buproprion TCAs Others: Nefazodone, Lithium Adequate dose for adequate time (2 months if possible at given dose) then treat for at least 6 months after the person has gone into remission-so up to 12 months total • Ideally see within 2 weeks of starting med and regularly afterwards, ie don’t give more than 2 -3 refills • • •

Question • A 3 day postpartum mother without prior psychiatric illness is concerned about feeling depressed. She has decreased energy, difficulty sleeping despite being tired, decreased appetite and frequent mood swings saying “One minute I’m fine and the next I’m crying. ” Which of the following is the most appropriate treatment? • A. Psychoeducation • B. Cognitive behavioral therapy • C. Pharmacotherapy • D. Hospitalization • E. Psychodynamic psychotherapy

Peripartum Depression • Major Depression can occur during pregnancy 13 -20% • After pregnancy 1. Baby blues up to 75% for several days after birth; symptoms end within 10 days 2. Postpartum depression 12% 3. Postpartum psychosis 1 -2 out of 1000

Schizophrenia

Schizophrenia • • • Slightly less than 1% of population (new onset 18 -24 men and 25 -35 in women) Criteria 1. Delusions 2. Hallucinations 3. Disorganized speech 4. Disorganized or catatonic behavior 5 Negative symptoms Two of 5 required and at least one must be in first three At least 6 months (at least 1 month of active symptoms) with social or occupational deterioration and not attributable to another condition (substance use for example) However, comorbid substance use is common (up to 50% with either ETOH or illicit drug dependence) Psychosocial rehabilitation treatment very helpful (UNM PSR-but must have psych evaluation to be referred)

Question • Demographic and clinical features associated with suicide in patients with schizophrenia include: • 1. Older age • 2. Female gender • 3. Higher cognitive status • 4. Lower socioeconomic status • 5. Good social support

Medication Treatment • • • Second generation antipsychotics 1. Risperidone (Risperdal) 0. 5 -6 mg 2. Quetiapine (Seroquel) 100 -800 mg 3. Olanzapine (Zyprexa) 2. 5 -40 mg 4. Ziprasidone (Geodon) 20 -120 mg 5. Aripiprazole (Abilify) 2 -30 mg First generation 1. Haloperidol (Haldol) 0. 5 -20 mg 2. Chlorpromazine (Thorazine) 100 -1000 mg 3. Fluphenazine (Prolixin) 2 -20 mg 4. Perphenazine (Trilfon) 4 -32 mg

Considerations in antipsychotic prescription • Check fasting lipids, Hg. A 1 c prior to prescription and every 6 months especially for olanzapine and quetiapine • Consider check EKG prior to Ziprasidone and Chlorpromazine (can elongate QRS) • For sedation: quetiapine/olanzapine>risperidone>ziprasido ne • For alertness: aripiprazole

Common side effects • Neuromuscular side effects (Extrapyramidal or EPS) (more common with risperidone and haloperiodol but can happen with any) • 1. Consider lower dose • 2. Consider change antipsychotic • 3. Add benztropine (0. 5 -3 mg)or diphenhydramine (25 -100 mg) • Akathesia (restlessness) • 1. Consider lower dose or changing med • 2. Propranolol (10 mg bid to 40 mg tid) or clonazepam 0. 5 mg bid to 2 mg bid • Excessive sedation • 1. Consider lower dose • 2. Consider change antipsychotic

Other side effects • 1. Risperidone: increased prolactin causing breast enlargement and/or galactorhea • 2. Any: dry mouth • 3. Weight gain Olanzapine>Quetiapine>Risperidone>Aripiprazole>Ziprazidone/Haloperidol • 4. Sexual dysfunction • 5. Tardive dyskinesia (check AIMS every 6 mo)

Non-Emergency Referrals from UNM Clinics to Psych Center • Ad Hoc on powerchart: must have tried minimum two antidepressants with minimal response before can be accepted (usually can be seen in 1 month once accepted) • If patient has substance problem, referral to ASAP or other community substance treatment agency • For psychotherapy, with UNM PCP, check to see if clinic has psychotherapist and refer (may get in quicker than Psych Center psychotherapy) • Or refer using Ad Hoc to psychotherapy at the Psych Center (usually 2 -3 month process)

Urgent/Emergent Referrals • Psych Urgent Care Clinic (PUCC) open Mon-Fri during the day. Walk in, staffed by CNP • Psychiatric Emergency Service (PES) open 24/7 staffed by two doctors (attending and resident) • Phone number PUCC and PES 272 -2920 -if in clinic, call PES Attending or resident to briefly discuss case; they can pass on info to next shift • Use Certificate of Evaluation (C of E) if person needs psych eval (danger to self or others or grave passive neglect) and refuses to go. Notify PES and fax to PES and to nearest police substation; requires a known patient location; only fill out on patients you or your clinic knows

Other Places to Refer and Information Sources • Community Substance Treatment options (see handout) • Community Behavioral Health Providers (see handout) • Community Psychotherapy Groups (see handout) • Web sites: www. mentalhealth. gov www. nimh. hih. gov www. psychiatry. org www. apa. org DSM 5 (Diagnostic Statistical Manual) FOCUS: the journal of lifelong learning in psychiatry Vol 2 DSM 5 Rev Ed • Questions: kfraser@salud. unm. edu
- Slides: 39