Bedside Reporting Regis Student Nurses Melanie Bartels Erin

Bedside Reporting Regis Student Nurses Melanie Bartels, Erin Hoffman, Perry Horner, Natasha Montoya, Sarah Osag & Karina Rodriguez

What is a Handoff Report? ● Communication between shifts & caregivers ● A complex “transfer of information (along with authority & responsibility) during transitions in care across the continuum; to include an opportunity to ask question, clarify & confirm. ” (Friesen, White & Byers, p. 2 -1) ● Purpose o Convey essential information related to patient care. o Improved continuity of care & therapeutic goal achievement. o Ensure safe transfer of care to a competent & qualified nurse. o Opportunity for education, debrief, socialization, planning, organization & teamwork.

The Details ● Many types of nursing reports / handoffs o Shift change, Unit transfer, Unit to diagnostic area, Discharge / interfacility, Medication transfer reports ● Methods o Patient involvement? o From memory or with notes / brain sheet o Verbal - with or without notes § Bedside, telephone, audio recording, o Nonverbal § Handwritten bedside notes, electronic reports, computer printouts ● Influences o Culture of the organization - open communication? non-hierarchical? who they turn to for assistance. o Nurse experience - report ability, knowledge of what to include, resources for assistance.

Poor Handoff: Why does it matter? ● Components of a poor handoff o o o Omission of important information Distraction Limited / Illegible documentation & Lack of transfer form use Incomplete records or medication reconciliation Poor accessibility to information Limited guidelines o o Reduced therapeutic progression. Increased likelihood of adverse patient outcome. Essential information is not relayed. Compromised patient safety & lower quality of care. ● Consequences:

An Effective Handoff ● Unit customization required. ● Protocols / Standardized process & steps of hand off report. o Mnemonic Checklists § 5 P’s - Patient/project, plan, purpose, problems & precautions § A. I. D. E. T - Acknowledge, Introduced, Duration, Explanation & Thank you ● Attainment of Goals o Increased accuracy & inclusion in information. o Improved patient & nursing staff satisfaction. o Improved patient safety & outcome.

PICO Question Population: Patients and nurses on med/surg floors Intervention: Bedside Reporting Comparison: Report given outside patient’s room Outcome: Increase in patient safety, satisfaction, & outcome. Increase in nurse satisfaction. Research question: • On hospital med/surg floors, does patient safety, satisfaction, and outcome as well as nurse satisfaction increase when nurses do bedside report versus report given outside the patient’s room?

Research Methods ● Databases: CINAHL, Ebsco. Host, MEDLINE, and Pub. Med ● Keywords: bedside report, shift report, safety, nurse satisfaction, patient satisfaction ● Inclusion Criteria: Articles within 5 years, peer reviewed, evidence-based practice, studies performed within inpatient hospitals
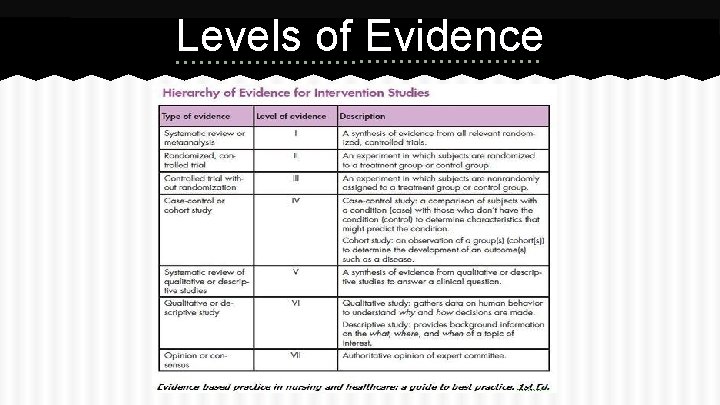
Levels of Evidence
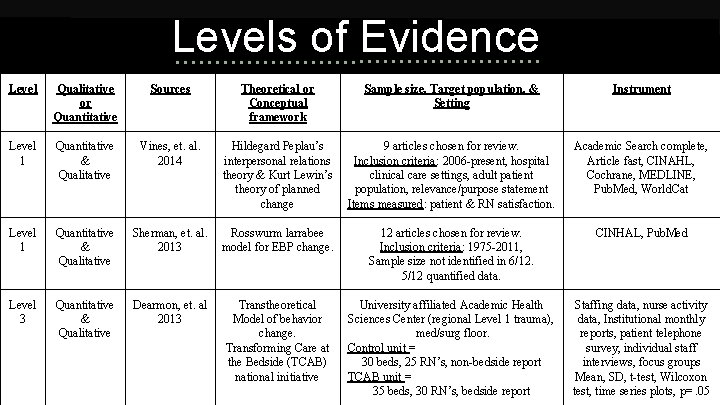
Levels of Evidence Level Qualitative or Quantitative Sources Theoretical or Conceptual framework Sample size, Target population, & Setting Instrument Level 1 Quantitative & Qualitative Vines, et. al. 2014 Hildegard Peplau’s interpersonal relations theory & Kurt Lewin’s theory of planned change 9 articles chosen for review. Inclusion criteria: 2006 -present, hospital clinical care settings, adult patient population, relevance/purpose statement Items measured: patient & RN satisfaction. Academic Search complete, Article fast, CINAHL, Cochrane, MEDLINE, Pub. Med, World. Cat Level 1 Quantitative & Qualitative Sherman, et. al. 2013 Rosswurm larrabee model for EBP change. 12 articles chosen for review. Inclusion criteria: 1975 -2011, Sample size not identified in 6/12. 5/12 quantified data. CINHAL, Pub. Med Level 3 Quantitative & Qualitative Dearmon, et. al 2013 Transtheoretical Model of behavior change. Transforming Care at the Bedside (TCAB) national initiative University affiliated Academic Health Sciences Center (regional Level 1 trauma), med/surg floor. Control unit = 30 beds, 25 RN’s, non-bedside report TCAB unit = 35 beds, 30 RN’s, bedside report Staffing data, nurse activity data, Institutional monthly reports, patient telephone survey, individual staff interviews, focus groups Mean, SD, t-test, Wilcoxon test, time series plots, p=. 05
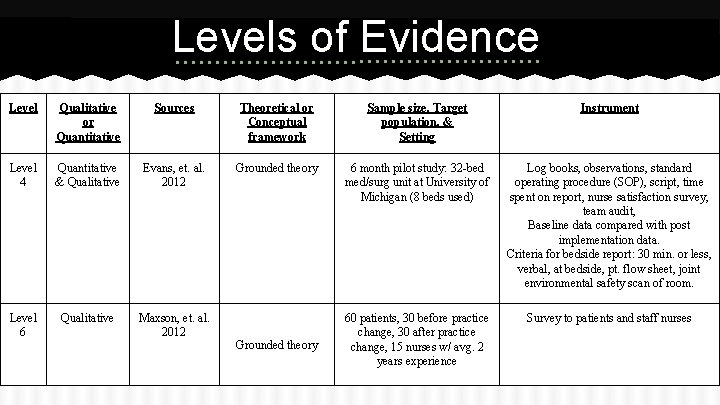
Levels of Evidence Level Qualitative or Quantitative Sources Theoretical or Conceptual framework Sample size, Target population, & Setting Instrument Level 4 Quantitative & Qualitative Evans, et. al. 2012 Grounded theory 6 month pilot study: 32 -bed med/surg unit at University of Michigan (8 beds used) Log books, observations, standard operating procedure (SOP), script, time spent on report, nurse satisfaction survey, team audit, Baseline data compared with post implementation data. Criteria for bedside report: 30 min. or less, verbal, at bedside, pt. flow sheet, joint environmental safety scan of room. Level 6 Qualitative Maxson, et. al. 2012 60 patients, 30 before practice change, 30 after practice change, 15 nurses w/ avg. 2 years experience Survey to patients and staff nurses Grounded theory

Critique of Evidence ● Applies to population ● Research question clearly defined ● Methods appropriate for studies ● Articles within the last 3 years ● Variety: Four different levels of evidence used

Results of Research: Nurse Impacts Advantages: ● Better prioritization & preparedness at the beginning of the shift ● Increased satisfaction and accountability ● Environmental safety scan ● Decreased use of subjective language during report, such as unclear acronyms, abbreviations forbidden by hospital policy ● Decreased report time o A 2006 study found that implementation decreased overtime by 100 hours in the first 2 pay periods & that handoff would only take 2 -5 min per patient.

Results of Research: Nurse Impacts Disadvantages : ● Nurses were slow to adopt the new process and needed constant reinforcement. ● Some patients monopolized the time so patient teaching regarding report was needed. ● Nurses were concerned about HIPAA violations for patients not in private rooms.

Results of Research: Patient Impact Benefits • Improved Patient Satisfaction / Perceptions o HCAHPS & Press Ganey scores increased post-implementation o Direct patient care begins sooner in shift o Felt informed of plan & of health care team members for the day o Felt involved in care, included in treatment decisions o Faster discharge times • Patient Safety o Decreased patient falls during shift change o Decreased medication errors o Improved timeliness of dressing & IV replacement

Results of Research: Patient Impact Disadvantages • Medical jargon can be difficult for patients to understand • Tiring repetition of information • Patient anxiety related to hearing about their illness & incorrect information • Lack of privacy

Results of Research: Patient Impacts Vines et al (2014) Research: ● 32 -Bed Surgical Unit: “Eight months after initiation, HCAHPS scores showed bedside report increased in client satisfaction within three key areas of communication: 1) nurses kept patients informed (5699%), 2) staff worked well together to provide care (98 -99%) and 3) staff included patients in decisions regarding treatment (58 -97%)” (Anderson & Mangino, 2006) ● 24 -Bed Telemetry Unit: “Press-Ganey satisfaction scores showed initiation of bedside report contributed to a 4. 4% increase in overall client satisfaction and a 5. 5% increase in client perceptions of being informed. ” (Freitag & Carroll, 2011) ● 592 -Bed Acute Care Hospital: “Within 6 months of implementation, HCAHPS scores within nursing communication increased 8%, confirming the positive influence of bedside report on client satisfaction. ” (Reinbeck & Fitzsimmons, 2013) Sherman, Sand-Jecklin & Johnson (2013) Findings: ● 34 -Bed Progressive Care Unit: Patient falls decreased (between 7 am and 7: 30 am) from 8 falls in the 6 month period pre-implementation to 1 fall in the 6 month period post-implementation. (Athwal et al, 2009)

Summary ● Published literature is highly positive but findings are not generalizable. ● Each study focused on diff potential benefits but there has been little reproduction. ● Other facilities may have had negative findings that were not published. ● Implementation requires a substantial change in how experienced nurses give report & unsuccessful implementation could be the result of an inherent problem with the bedside report process. ● Positive finding suggest beside nursing report may lead to improvements in patient outcomes, as well as patient & nursing satisfaction. ● Published evidence is highly anecdotal in nature ● Risks associated with this practice change are relatively low.

Future Research Needs ● More QUANTITATIVE research with adaquate sample sizes & details of previous method of handoff report. ● Comparative research related to bedside report’s impact on staff overtime, patient falls, discharge times, med errors, dressings & IV replacement times. ● What is the relationship between: o Whiteboard use during bedside report & patient / nurse satisfaction o Bedside report & the activation of rapid response / code teams ● Are there styles of bedside or hybrid report that are more effective than others?

P 2: A Case Study Current Similarities: o AIDET implemented o Offgoing & oncoming nurse greet patient together for introductions. - Oncoming nurse introduces self & updates whiteboard & reviews basic plan of care for the day - Offgoing nurse says goodbyes

P 2: A Case Study Current Differences: o Exchange of information between shifts performed away from patient bedside. o Patient not involved. o Friendly hand-off sheets are utilized.

Does the evidence justify changes at Rose? ● Patient Preferenceo Ratings from the hopsital compare tool on Medicare. gov report: § Patients who reported that their nurses "Always" communicated well - Rose Medical Center average: 77% - National & Colorado Average: 79% ● Scientific evidenceo Research suggests that bedside reporting has a positive impact on patient outcome & satisfaction. o Additional research needed. ● Clinical experienceo AIDET is currently in use at Rose

Implementation of Bedside Report on P 2 Prior to implementation ● Unit protocol of information included in bedside report. o AIDET, 5 P’s, friendly hand-off sheet, reporting by exception, NPSF bedside report model, etc. ● Launch date set 1 to 2 months out in order for preperation. ● Staff Training o Computer training for all staff prior to launch date o Charge nurses & mentors implement hands on training for nurses o Discussions & updates in morning huddles

Implementation of Bedside Report on P 2 During implementation & ongoing ● Inform patient population of upcoming change o Posters, website, newsletter, etc. ● Monitor feedback from nurses, patients, and administrators. ● Evaluate time spent, impact on patient safety/outcome and satisfaction among nurses & patients. ● Make necessary changes to improve initial process. ● Reevaluate: Does bedside reporting have a positive impact?

Steps to Implement Change ● Are we Ready to Change? ● Gather Multidisciplinary Team o Hospital & Nurse leaders, unit nurses, etc. o Patients & family members ● Identify Facilititators & Barriers to Success ● ● ● o Formulate Plan to Overcome Barriers Define Standardized Bedside Report Procedure Inform & Train Staff Implementation Evaluation & Refinement Reassess http: //www. ahrq. gov/professionals/systems/long-term-care/resources/pressure-

Transition to Bedside Reporting ● Barriers to Change o o o Comfort with current methods of handoff report. Reduced time for socialization Unsure of what to do & say Concerns related to talking about condition/disease in front of patient or family Increased time to complete shift change ● Facilitators of Change o o o Opportunity to increase patient satisfaction scores Poor communication of information at shift change Chance for improved prioritization Increased frequency & interaction with the patient & family Most nurses agree that bedside reporting has the potential to improve patient care

Successful Report Patient participation • Upon admission, educated on bedside report & what to expect. • Made aware of upcoming report 30 – 60 minutes before shift change. Bedside Report • • • AIDET guides interaction. SBAR format Verification of information Patient involvement Individualized goal setting Outline of the day’s plan of care National Paitent Safety Foundation (Currier, Joshi, & O’Brien, 2011)

Appendix A: Additional Patient Impact Data Vines et al (2014) Research, Continued: ● “Bedside report significantly impacted responses. Clients and family members reported that nurses made sure they knew who their nurse was and included them in shift report discussion. ” (178 clients, 72 family members) (Sand-Jecklin & Sherman, 2013) ● “For 6 months post implementation, client satisfaction scores increased by an average of 11. 1 points (Press-Ganey instrument). Longitudinal results (23 months after initiation of bedside reporting) showed an increase of 6. 9 points. (20 bed health center) (Wakefield et al, 2012) Maxson et al (2012) Findings - Sample of 60 patients: ● Patient Likert Scale survey results improved when patients were asked about their satisfaction with; a) being involved in plan of care communication, b) being informed , and c) experiencing open communication, teamwork and professional behaviors in report. (Pre-implementation mean 1. 5 -2. 0, Post -implementation mean of 1. 0)

Appendix A: Additional Patient Impact Data, cont. Evans et al (2012) - 32 Bed University of Michigan Hospital med-surg unit: ● “Improved prioritization: most acute patients are seen first after report, patients are seen within the first half hour of the shift and oncoming nurses are able to visualize the patient themselves rather than rely on colleague comments. ” ● “Many nurses believe the process violates patient confidentiality and they are not comfortable with bedside report. ” ● “Patients were more involved in their care and able to identify their caregivers for the shift, promoting client satisfaction. Bedside report increased direct care time to patients. ” Sherman, Sand-Jecklin & Johnson (2013): ● Time decreased from 30 -60 minutes in between nurses coming on shift and the first patient being seen to 11 minutes. (Federwisch, 2007)

Appendix B: Bedside Report Example Videos • Bedside Report Using SBAR : https: //www. youtube. com/watch? v=d. CLp 8 Kiiv 1 A • Nurse Bedside Report/Handoff: https: //www. youtube. com/watch? v=Leq_FV-g. Y 7 w • Bedside Handover: https: //www. youtube. com/watch? v=hbx. PR-ra 6 RE • Bedside Report Workshop Video: https: //www. youtube. com/watch? v=Id. IMfm. Ksn. Bg

References Currier, A. , Joshi, M. S. , & O’Brien, K. (2011). Bedside Change of Shift Reporting: A Strategy to Increasing Patient Safety. NPSF. Retrieved from: http: //www. npsf. org/wp-content/uploads/2011/11/PLS_1110_MJ. pdf Dearmon, V. , Roussel, L. , Buckner, E. B. , Mulekar, M. , Pomrenke, B. , Salas, S. , &. . . Brown, A. (2013). Transforming Care at the Bedside (TCAB): Enhancing Direct Care and Value-added Care. Journal Of Nursing Management, 21(4), 668 -678. doi: 10. 1111/j. 1365 -2834. 2012. 01412. x Evans, D. , Grunawait, J. , Mc. Clish, D. , Wood, W. , & Friese, C. R. (2012). Bedside Shift-to-Shift Nursing Report: Implementation and Outcomes. MEDSURG Nursing, 21(5), 281 -292. Friesen MA, White SV, Byers JF. Handoffs: Implications for Nurses. Rockville, M. D. : Agency for Healthcare Research and Quality 2008 [updated 2008; cited 2008 April 23]; Available from: http: //www. ahrq. gov/qual/nurseshdbk/docs/Friesen. M_HOIN. pdf. Maxson, P. , Derby, K. , Wrobleski, D. , & Foss, D. (2012). Bedside nurse-to-nurse handoff promotes patient safety. Medsurg Nursing: Official Journal Of The Academy Of Medical-Surgical Nurses, 21(3), 140 -144. Sherman, J. , Sand-Jecklin, K. , & Johnson, J. (2013). Investigating Bedside Nursing Report: A Synthesis of the Literature. MEDSURG Nursing, 22(5), 308 -318. Vines, M. M. , Dupler, A. E. , Van Son, C. R. , & Guido, G. W. (2014). Improving Client and Nurse Satisfaction Through the Utilization of Bedside Report. Journal For Nurses In Professional Development, 30(4), 166 -173. doi: 10. 1097/NND. 000000057 Wakefield, D. S. , Ragan, R. , Brandt, J. , & Tregnago, M. (2012). Making the transition to nursing bedside shift reports. Joint Commission Journal on Quality and Patient Safety, 38(6), 243 -253.

Thank You
- Slides: 31