BEACHSIDE NURSING CENTER 24 Hours Skilled Nursing Facility

BEACHSIDE NURSING CENTER 24 - Hours Skilled Nursing Facility with Rehabilitation Services

OVERVIEW Courteous and compassionate quality of care Facility is rated 5 stars by DHS/Medicare 59 Bed Facility Great team of…. Nurses, Rehabilitation Experts, PT/OT, Dietitian, Support Staff, Volunteers Various Amenities and Activities Facility was in Survey window towards the last 3 weeks of my internship

ESMERALDA SALCIDO, MS, RD Registered Dietitian Previous Experience in Acute Care Now works at Beachside Nursing as the RD and Food Service Manager Manages the Kitchen On Site Coordinates resident care with other disciplines Ensure patient satisfaction in relation to food intake and preferences Conduct necessary Nutrition Assessment

OTHER STAFF Administrator – Nathan Beck Director of Nursing Director of Rehabilitation Director of Staff Development Social Services Dietary - Esmeralda Maintenance

POLICY AND PROCEDURE BINDER Guiding Principles for the Care of Patients and Operating the Facility Important for inspections with DHS Purchasing, Inservice & Orientation, Menus, Meal Service, Nutrition Care, Food Preparation, Sanitation and Infection Control, Safety, Emergency Procedures, Quality Improvement Policies and Procedures are very patient centered and revolve around resident rights

DIETARY DIRECTIONS INC. Company located in Fresno, California Company of RDN consultants, that provide services to health care and food service facilities Provide Menu’s, Diet Manuals, and Food Service Policy and Procedures Manuals for the Facility

LONG TERM CARE COMPETENCIES

REVIEW THE MOST RECENT STATE INSPECTION RESULTS D. H. S. Surveys and HIPAA Notice There were no deficiencies from last year Some examples of deficiencies found in the facility were… Using Nasal Swabs on patients without verbal or written consent A deficiency was found in regards to the care plan of a patients hypertension. Traction tape in Showers Last survey was end April 2017 Facility kept 5 star rating Facility is currently in the survey window

COMPLETE 5 MDS QUARTERLY ASSESSMENTS Assisted with 2 in the beginning of the rotation Completed 1 on 2/2/2019 Completed 2 on 2/22/2018

PROJECTS - MDS are to be completed within 5, 14, 30, 60, 90 days after admission for Medicare resident/patients and within 14 days and quarterly thereafter for non-Medicare Residents and patients on intake MDS must be completed using a 3 day observation period as noted on the MDS DSS or RD should complete the MDS based on the nutrition assessment Identified triggers should be noted on Care Area Assessment (CAA) Admission Record, Monthly & Weekly Wts, Pressure Ulcers, Enteral/Parenteral Feedings, Significant Problems and Follow Up
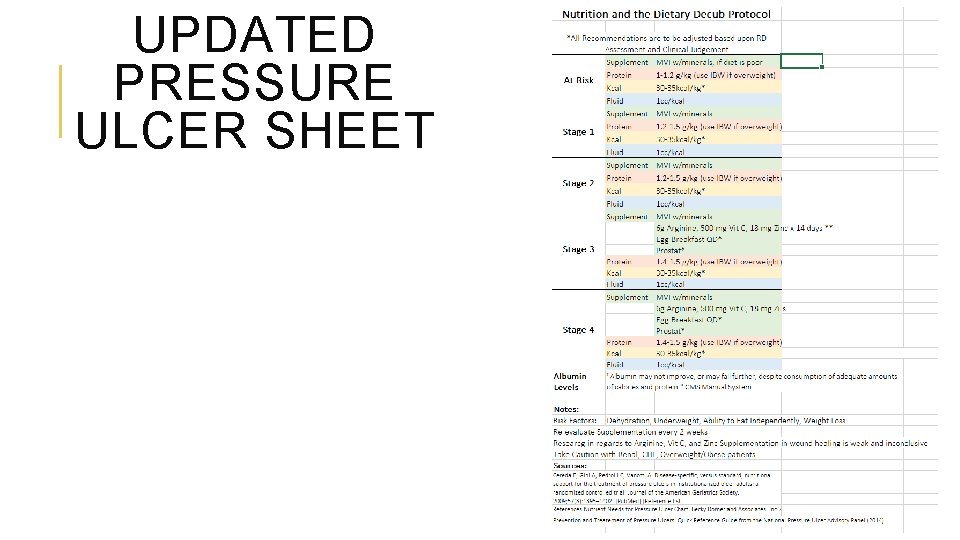
UPDATED PRESSURE ULCER SHEET

CASE STUDY – 69 YO FEMALE Admitted on: 2/23/2018 HTN (blood pressure controlled) BMI 16 Meds: 57” 74# IBW 84 – 93 – 102 80% IBW Estimated needs: Laxative if needed Aspirin 81 mg Atorvastatin Calcium 40 mg for HLD Varvediolol for HTN Lansoprazole, for GI prophylaxis Warfarin QD x 30 days Tamiflu Est kcal need: 1177 -1345 kcal (35 -40 m. L/kg) Pro 1. 2 g/kg = 40 g 1 cc/kcal = 1200 m. L Skin Diet: RD Recs 2/27/2018 increase feeding to 40 cc x 20 hr to meet nutritional needs and for weight gain Isosource 1. 5 ml x 35 m. L x 20 hours. On 12 pm to 8 am Dietetic Inter Rec: increase to 40 m. L/hr x 20 hr Water flush 30 m. L/hr x 20 hr PEG NKA Presents with: generalized muscle weakness, Dysphagia oropharyngeal phase, Acute MI, Gastrostomy status, Hyperlipidemia, Sacrococcygeal Pressure Injury Stage 1 SLP Consult Machine – Vitalstim which is a neuromuscular ele

REVIEW MINIMUM DATA SAT AND CARE AREA TRIGGERS (CATS) AND CARE AREA ASSESSMENTS (CAAS) PROTOCOLS MDS – Section K for nutrition Triggers: Swallowing, changes in weight (significant wt loss), Meeting kcal/pro needs (more 50% needs tube feedings) Care Area Assessment – LTC MDS assessment done on quarterly patient If Medicare pt here longer than 3 months, each discipline will review chart on quarterly and annual basis. Use blue nutrition assessment page

COMPLETE FOLLOW UP / REASSESSMENT DOCUMENTATION Completed Follow Up and Reassessment Documentation on patients. Initial admissions and MDS follow ups with patients Weight Variance patients

COMPLETE MEAL ROUNDS, RECORD CALORIC INTAKE AND RECOMMENDED DIET CHANGES AS NEEDED Upon Admission look at Doctors Orders, Diagnosis, Medications, Supplements, Age About 3 days after Admission, a Nutrition Assessment will take place Food Preferences, Weight Hx, Chewing and Swallowing, Weight Goals, Allergies, Activity Level, Estimated Needs, Supplements, RD Recommendations, Review Lab Values, Wounds, Incisions Make RD Recommendation’s based upon resident assessment regarding above factors

MEDICAL AND SKIN CARE ROUNDS There is a Wound Doctor that comes once a week to look at patients wounds and ulcers Nutrition Recommendations change depending on severity Increased Kcal and protein needs I did not have a chance to observe the wound care doctor

COORDINATE THE DESIGN OF MENUS AND MODIFICATIONS FOR THERAPEUTIC DIETS Reformatted the Alternative Menu The Alternative Menu provides alternates to what is on the scheduled cycle menu for the day When doing assessment, make recommendations for diet changes for resident

ALTERNATIVE MENU

ATTENDED INTERPROFESSIONAL MEETINGS, DEVELOPED NUTRITION CARE PLANS FOR Safety Committee meetings ASSIGNED RESIDENT Interdisciplinary Meetings prepare Survey Weight Variance Meetings In each of these meetings we collaborated with other heads of departments to agree upon a care plan moving forward for the resident

SAFETY COMMITTEE MEETING Feb 21, 2018 Safety meeting betweed the Administrator, Director of Nursing, Director of Rehab, Maintinance Director, Dietary, and Director Staff Development Discussed… Dietary – Dishwasher, needs to be ran 3 times in the morning before it reaches proper temperatures, and Checking Sanitizer with Strip Shower Room Safety, and Traction Matts Smoking – weighing patient rights, safety concerns, and procedure/policy Discussed 11 pm-7 am shift and concerns Rehab- clutter, compliance regarding power plugs, and creating a more comfortable environment with blinds

MONITOR ENTERAL FEEDINGS Monthly Check up for Medicare Check weight, if they are meeting their nutritional needs, or may need changes in formula Balance Enteral Feedings with PO intake, adjust as necessary

DISCUSS NEEDED CHANGES IN NUTRITION SUPPORT ORDERS WITH OTHER DISCIPLINES AS NEEDED Care Conferences Discuss Care with Family, DON, PT, Social Services Ex. Resident, at risk aspiration, on nectar thick liquids but not getting PO intake. Weight costs/benefits of G-Tube.

REFER RESIDENTS TO OTHER PRIMARY CARE PROVIDERS AS APPROPRIATE During an assessment there was a resident with very high Blood Sugar, at 370. Resident has a recent history of significant wt loss, CKD, and CHF Discussed results with the assigned Nurse and made recommendations for Hyperglycemia medication to the Doctor Resident was then discharged to the hospital after a fainting incident, and returned a couple days after on Metformin I felt like this was a good example where there may have been a lack of communication or interdisciplinary collaboration among the health care team, because this patient had lost a significant amount of weight, unintentionally, over the course of 2 years Resident was d/c after a fainting incident, and then was readmitted on a hyperglycemia medication Lab Initial Admin 2/14 Readmin 2/20 Blood Sugar 470 69

REFER RESIDENTS TO OTHER PRIMARY CARE PROVIDERS AS APPROPRIATE When nutrition recommendations are made they are referred to nursing, which approves orders through the doctor
- Slides: 24