BC Provincial Pediatric Early Warning System PEWS Education

BC Provincial Pediatric Early Warning System PEWS Education Session

This Session Will • Explain The Provincial Pediatric Early Warning System Ø PEWS score Ø Situational Awareness Factors Ø Provincial Escalation Aid Ø SBAR Communication Tool • Describe & review the Provincial PEWS flowsheet • Demonstrate how to calculate a PEWS score • Identify supports & resources available to assist you in using PEWS • Provide an opportunity for you to apply the components of PEWS using case scenarios

What is PEWS? üA clinical tool for frontline staff üAn evidence informed system to support improved recognition and response to pediatric deterioration üA system we can and are implementing across BC’s hospitals that provide care to children

PEWS is: • • For all patients regardless of acuity A complete system-not just a score A support for clinical decision making Provides a common language to support effective communication PEWS is not a substitute for clinical judgment

Why do we need earlier warning of a child’s compromise? ü~63 to 89% of children do not survive cardiac arrest üMorbidity in survivors remains high despite advances in resuscitation training, technology and treatment üEvidence indicates prevention is possible üPediatric patients may demonstrate physiologic and behavioral symptom deterioration up to 24 hours prior to cardiopulmonary arrest Early Recognition Early Intervention Improved outcomes

Provincial Approach § A variety of PEWS tools are in use internationally § Child Health BC has been working with Provincial Health Authority Planners to develop a PEWS that will work across the province § The provincial approach will include the Brighton Scoring Tool and the Cincinnati Situational Awareness Model

Who is Child Health BC? A provincial networking collaboratively to build an integrated, accessible system of health services for children and youth. ü All 7 Health Authorities, including First Nations HA ü UBC Department of Pediatrics ü The three child serving ministries (Mo. E, MCFD & Mo. H) ü Research (Maternal Infant Child Youth Research Network) ü BC Pediatric Society ü Doctors of BC ü Society of General Practitioners of BC 7

The Purpose of the PEW System ü Identify pediatric patients who are at risk of deterioration ü Mitigate the risk (through clinical and procedural response) ü Escalate to a higher level of care if mitigation is unsuccessful … and do it all sooner!
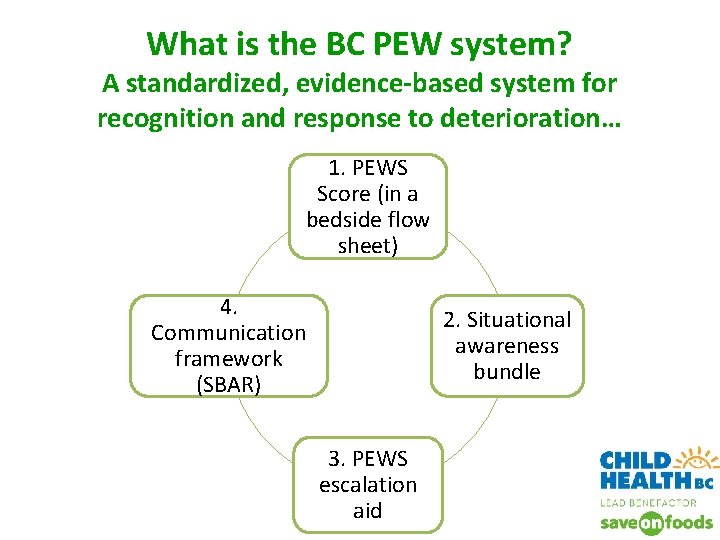
What is the BC PEW system? A standardized, evidence-based system for recognition and response to deterioration… 1. PEWS Score (in a bedside flow sheet) 4. Communication framework (SBAR) 2. Situational awareness bundle 3. PEWS escalation aid

1. PEWS Score The Brighton PEWS score can range between 0 and 13 Higher PEWS scores are associated with higher risk of clinical deterioration There are 6 flowsheets: ü 0 -3 months ü 4 -11 months ü 1 -3 years ü 4 -6 years ü 7 -11 years ü 12+ years
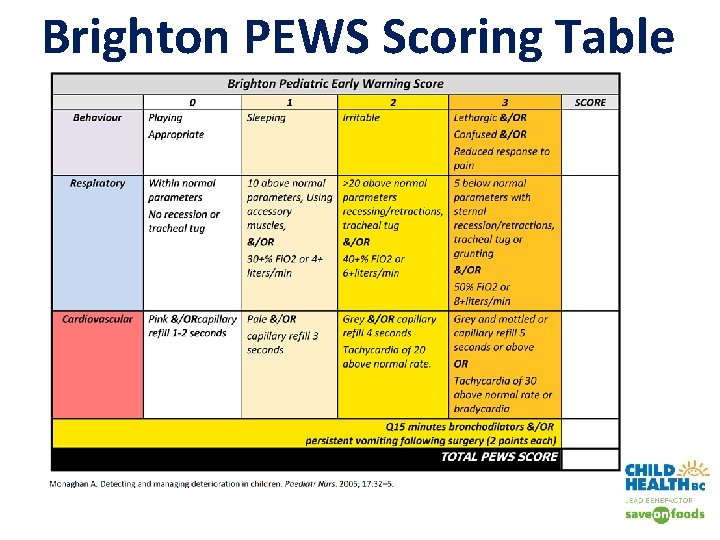
Brighton PEWS Scoring Table

Flow Sheet & PEWS Score PEWS Scoring Legend 0 1 2 3 Age- specific vital signs norms based on CTAS 2013

2. Situational Awareness -factors that contribute to the risk of pediatric clinical deterioration Caregiver Concern Unusual therapy PEWS score 2+ Watcher patient Communication breakdown Cincinnati Children’s found these factors to be 100% sensitive predictors of serious deterioration. Addressing all five on a regular basis helped teams improve predicting & preventing deterioration 13

Situational Awareness • Let’s review the poster… • Here is a short video from Cincinnati Children’s http: //www. riskybusiness. com/video. php? video id=74 • How can we engage patient’s and their families in the PEWS process?
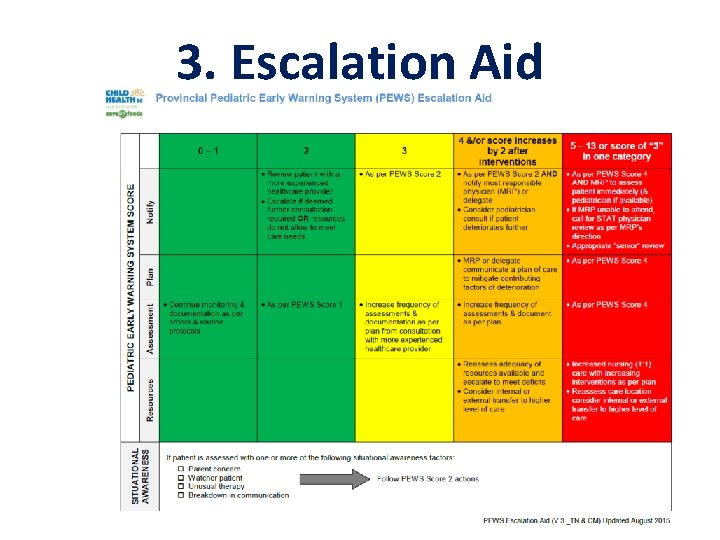
3. Escalation Aid

4. Standardizing Communication (SBAR) What is SBAR? SBAR (Situation-Background-Assessment. Recommendation) technique provides a framework for communication between members of the health care team about a patient's condition

SBAR Communication Tool Situation: What is the situation you are calling about? I am (name), a nurse on ward (X) I am calling about (patient X) I am calling because I am concerned that… (e. g. BP is low/high, pulse is XX, temperature is XX, PEWS score is X) Background: Pertinent Information & Relevant History Patient (X) was admitted on (XX date) with…(e. g. respiratory infection) They have had (X procedure/investigation/operation) Patient (X)’s condition has changed in the last (XX mins) Their last set of vital signs were (XXX) Assessment: What do you think the problem is? I think the problem is (XXX) and I have…(e. g. applied oxygen/given analgesia, stopped the infusion) OR I am not sure what the problem is but the patient (X) is deteriorating OR I don’t know what’s wrong but I am really worried Recommendation: What do you want to happen? I need you to… Come to see the child in the next (XX mins) AND Is there anything I need to do in the meantime? (give a normal saline bolus/repeat vitals/start antibiotics) Ask receiver to repeat key information to ensure understanding S B A R

Creating a Common & Clear Picture of Risk Visual cues for all healthcare providers to recognize patients at risk of deterioration Standardized check-in processes between charge nurse and RNs Example: patient room number coloured in red on white board

Example Baby Smith: • 5 -month-old admitted with RSV • Previously vigorous in her activity-now lethargic with a sunken fontanel • RR 70 with increased use of accessory muscles • Sa. O 2 is 95% on 1 L/min via NP • HR 160, she is pale, cap refill is 4 seconds, BP 82/46 • No wet diapers for 10 hours.

How to Score: Respiratory PEWS Scoring Legend x 0 1 2 3 95% 1 L NP x 2 Always use the score from the highest descriptor per category
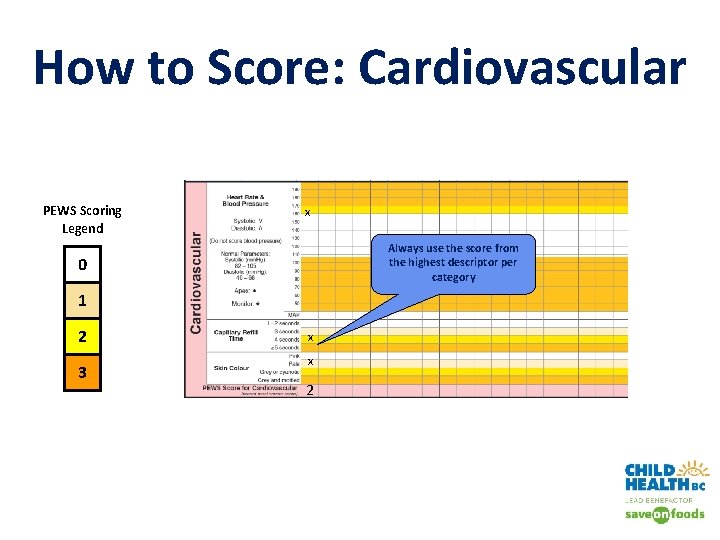
How to Score: Cardiovascular PEWS Scoring Legend x Always use the score from the highest descriptor per category 0 1 2 3 x x 2

How to Score: Behavior PEWS Scoring Legend 0 1 x 2 3 3

How to Calculate Total PEWS Score 2 2 3 0 0 7

Case Study 1 Maria is: • 2 -years-old, recently diagnosed with Leukemia • Resp rate of 55, Sa. O 2 is 92% on room air • Developed a fever last night 38. 8 o. C axilla • She is lethargic and confused • Tachycardic at 155 BPM, pale, cap refill is 5, BP 98/55 • Persistent vomiting • Her mom is extremely worried about her • Has not voided since the previous afternoon.

Case Study 1 2 3 3 8

Case Study 2 • 4 -years-old, newly diagnosed diabetic • Transferred to your unit from the ED with an initial PEWS Score of 0 • Respiratory rate 50, Sa. O 2 90% on room air • Heart rate 90, pale, cap refill 3 seconds, BP 110/78 • You find her irritable and increasingly lethargic
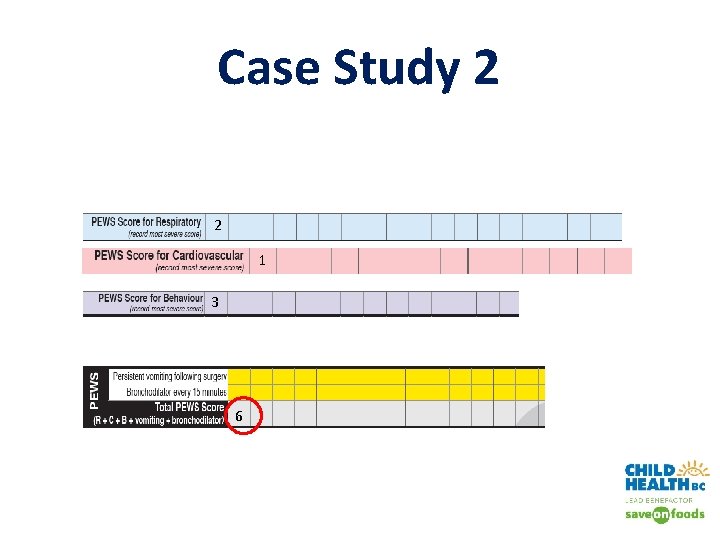
Case Study 2 2 1 3 6

Do the PEWS tools work? What has research found? • Nearly 50% decrease in rates of UNSAFE ICU transfers • Potentially provides advanced time of >11 hours • Positive directional trends in improved clinical outcomes • Enhanced multi-disciplinary team work, communication and confidence • There are no negative outcomes reported in the literature related to the use of PEWS 28

How will we know if PEWS is working? 15 sites PEWS ? ü Mixed method, pre-post evaluation design: chart reviews, interviews, focus groups and surveys at all phase 1 sites. 29

Who to Contact for Information? Insert PEWS Trainer(s) Name & Contact Information for your site here
- Slides: 30