BC Newborn Resuscitation Record PSBC 1980 June 2019

BC Newborn Resuscitation Record (PSBC 1980) June 2019 Guide for Completion

Overview 1. Advantages of a Standardized Resuscitation Record 2. The Recorder 3. Summary of Changes 4. Completion of the Form 5. Case Study 6. Summary 7. Questions 2
Advantages of a Standardized Resuscitation Record Facilitates clear, concise, factual, objective, timely documentation Information recorded can guide continuing care Identifies Quality Assurance issues May assist in answering questions from family/ clinicians Guides resource allocation (staff, supplies, equipment) Identifies staff learning needs Provides data for research 3

The Recorder • Identify the “recorder” ASAP, preferably prior to birth • Recorder should be an experienced team member with a good working knowledge of the Neonatal Resuscitation Program (NRP) Algorithm • Clinical documentation should be the recorder’s only role Responsibilities of the Recorder: • Document care provided by all health care professionals • Maintain an accurate record of the timing of all assessments and interventions • Communicate with the Team Leader and provide decision support by prompting assessments and interventions based on NRP algorithm 4

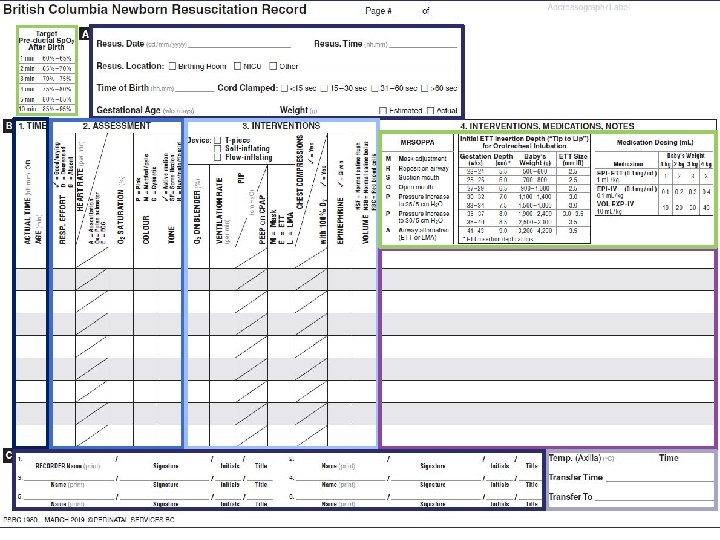
British Columbia Newborn Resuscitation Record (March 2019) 5

WHAT’S NEW? • New fields to record: – Time of cord clamping – Axillary temperature – Transfer time and location • Separate columns to record epinephrine and volume • Only one time column – recorder will decide what time source to use • Codes added to enhance standardization of documentation 6
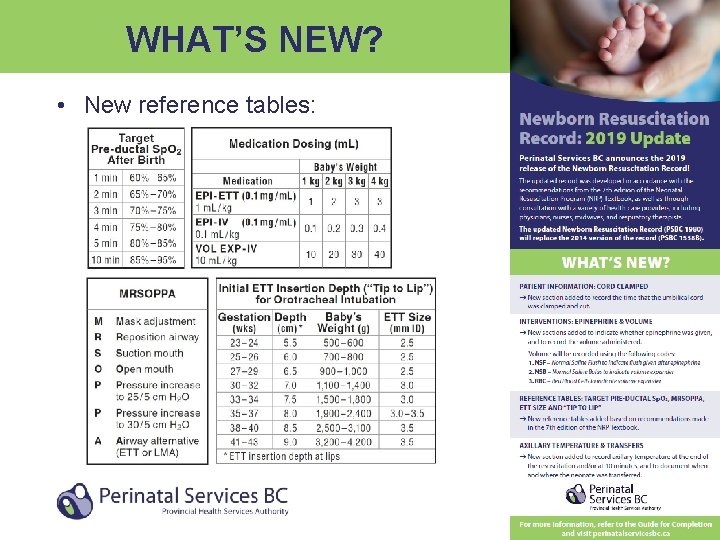
WHAT’S NEW? • New reference tables: 7

How to complete the BC Newborn Resuscitation Record (PSBC 1980) 8

A. Demographics and Background 1 16/07/2018 3 14: 36 14: 35 36/4 2000 • Top section of record can be completed anytime during the resuscitation event, including prior to, during, or immediately after the resuscitation event 9

Patient Identification 1 16/07/2018 3 14: 36 14: 35 36/4 2000 • Affix patient addressograph or label in indicated space • If not available, record patient’s Surname, Sex, and Birth Order (if multiple pregnancy) 10
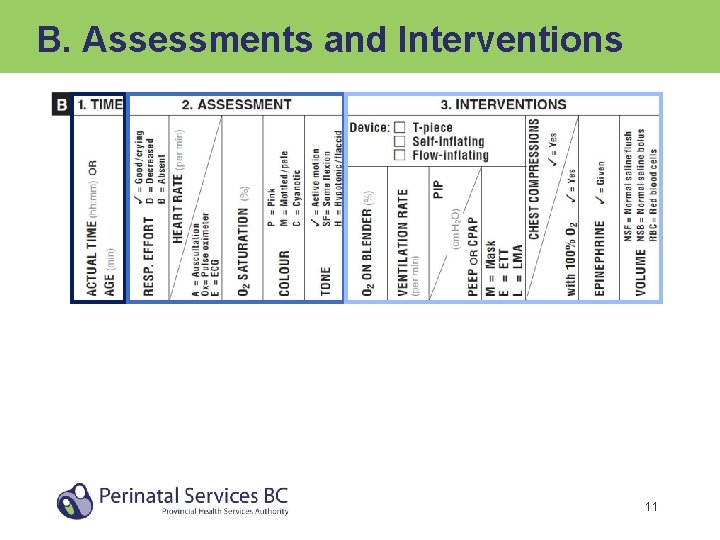
B. Assessments and Interventions 11

1. TIME • Record timing of all major events (e. g. , assessments and interventions) and decisions • Use a single time reference – Either actual time on a wall clock or baby’s age (in minutes) from an Apgar timer – Indicate time source by circling either ACTUAL TIME or AGE in column header • The more complex the resuscitation, the more entries should be recorded 12
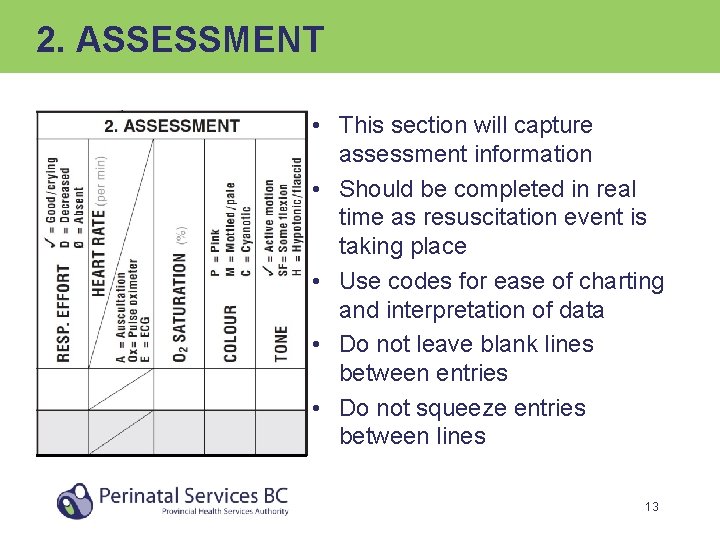
2. ASSESSMENT • This section will capture assessment information • Should be completed in real time as resuscitation event is taking place • Use codes for ease of charting and interpretation of data • Do not leave blank lines between entries • Do not squeeze entries between lines 13

RESPIRATORY EFFORT • Record respiratory effort by noting one of the following codes: ✓ = Good / crying D = Decreased (defined as breathing that is so shallow or slow that it is unable to meet needs of the body) Ø = Absent Go to #4. INTERVENTIONS, MEDICATIONS, NOTES • Record if respiratory effort is laboured (e. g. , tachypnea, grunting, retractions) 14
![HEART RATE • [Top-left] Record heart rate • [Bottom-right] Record method by which heart HEART RATE • [Top-left] Record heart rate • [Bottom-right] Record method by which heart](http://slidetodoc.com/presentation_image_h/1aab72505320aa09e8c7b03100ef016f/image-15.jpg)
HEART RATE • [Top-left] Record heart rate • [Bottom-right] Record method by which heart rate was obtained by noting one of the following codes: A = Auscultation Ox = Pulse oximeter E 120 143 146 A Ox E = Electrocardiography (ECG) • If the baby has a low heart rate or poor perfusion, a pulse oximeter is not a recommended method for measuring the heart rate • Palpation of the cord is not a recommended method to measure the heart rate 15

O 2 SATURATION • Record the preductal (right hand or wrist) oxygen saturation as per the pulse oximeter • Compare oxygen saturation with target saturations Alert team leader if there is a need to administer additional oxygen to meet target saturations Note: Target pre-ductal saturation 63 values are only applicable in the immediate newborn period; After one hour of birth oxygen saturation should be ≥ 95% 16
COLOUR • Record colour of the baby by noting one of the following codes: P = Pink M = Mottled / pale C = Cyanotic 17

TONE • Record tone of the baby by noting one of the following codes: ✓ = Active motion SF = Some flexion H = Hypotonic / flaccid 18
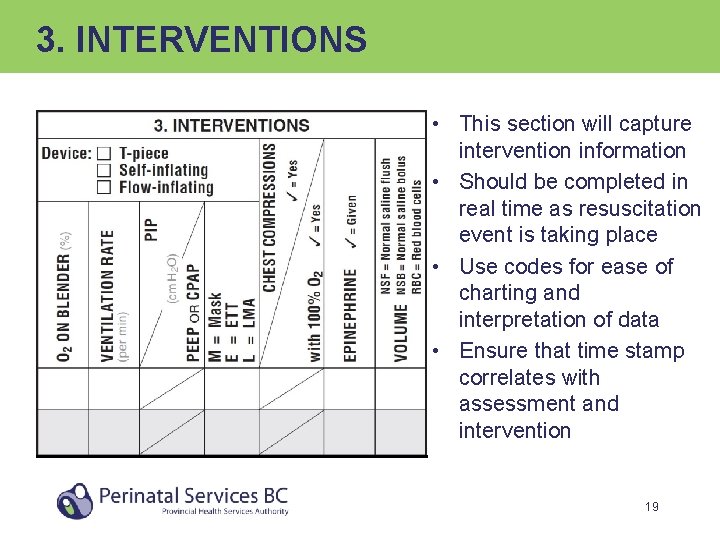
3. INTERVENTIONS • This section will capture intervention information • Should be completed in real time as resuscitation event is taking place • Use codes for ease of charting and interpretation of data • Ensure that time stamp correlates with assessment and intervention 19
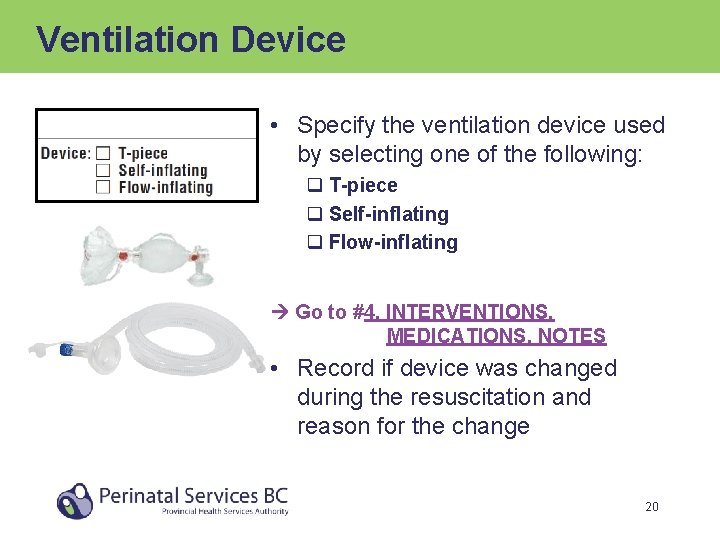
Ventilation Device • Specify the ventilation device used by selecting one of the following: q T-piece q Self-inflating q Flow-inflating Go to #4. INTERVENTIONS, MEDICATIONS, NOTES • Record if device was changed during the resuscitation and reason for the change 20

O 2 % ON BLENDER • Record amount of oxygen delivered as per air/oxygen blender • This will include Positive Pressure Ventilation (PPV), Continuous Positive Airway Pressure (CPAP) or free-flow oxygen administration 21
VENTILATION RATE • Record number of administered breaths per minute 22
![PPV OR CPAP • If Positive Pressure Ventilation (PPV) used: – [Top-left] Record Peak PPV OR CPAP • If Positive Pressure Ventilation (PPV) used: – [Top-left] Record Peak](http://slidetodoc.com/presentation_image_h/1aab72505320aa09e8c7b03100ef016f/image-23.jpg)
PPV OR CPAP • If Positive Pressure Ventilation (PPV) used: – [Top-left] Record Peak Inspiratory Pressure (PIP) – [Bottom-right] Record Positive End-Expiratory Pressure (PEEP) • If Continuous Positive Airway Pressure (CPAP) used: – [Top-left] *leave blank* – [Bottom-right] Record pressure 20 5 5 23

Interface Device • Record interface device used by noting one of the following codes: M = Mask E = Endotracheal Tube (ETT) L = Laryngeal Mask Airway (LMA) 24
Interface Device Go to #4. INTERVENTIONS, MEDICATIONS, NOTES • If ETT or LMA used, document the following: – – – – Whether insertion was successful/ unsuccessful Name of person who performed procedure Number of attempts ETT/ LMA size Insertion depth (for ETT) Confirmation method Timing of procedure (should be ≤ 30 seconds) 25
![CHEST COMPRESSIONS • [Top-left] Indicate whether chest compressions were administered by noting ‘✓’ if CHEST COMPRESSIONS • [Top-left] Indicate whether chest compressions were administered by noting ‘✓’ if](http://slidetodoc.com/presentation_image_h/1aab72505320aa09e8c7b03100ef016f/image-26.jpg)
CHEST COMPRESSIONS • [Top-left] Indicate whether chest compressions were administered by noting ‘✓’ if they were • [Bottom-right] Indicate whether oxygen was turned up to 100% by noting ‘✓’ if it was Alert team leader if oxygen has not been turned up to 100% ✓ ✓ 26

EPINEPHRINE • Indicate whether epinephrine was administered by noting ‘✓’ if it was Go to #4. INTERVENTIONS, MEDICATIONS, NOTES • If epinephrine administered, document the following: – – – Concentration Dose Route Prescriber Effect 27
VOLUME • Record type of volume administered by noting one of the following codes: NSF = Normal saline flush (indicating flush given after epinephrine) NSB = Normal saline bolus (indicating normal saline given as volume expander) RBC = Red blood cells (indicating red blood cells given as volume expander) 28
VOLUME Go to #4. INTERVENTIONS, MEDICATIONS, NOTES • If volume administered, document the following: – – Dose Route Prescriber Effect 29
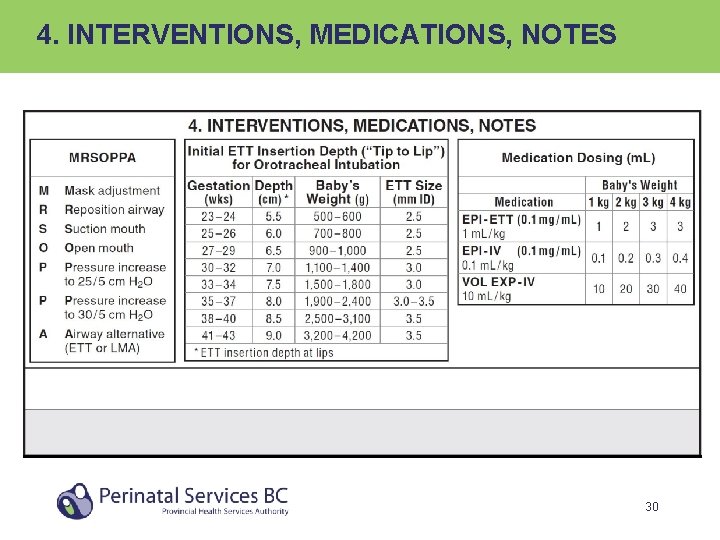
4. INTERVENTIONS, MEDICATIONS, NOTES 30

4. INTERVENTIONS, MEDICATIONS, NOTES • If resuscitation occurred at birth, specify the following in first entry: – Mode of delivery – Number of babies delivered (multiple gestation) – Information about pertinent delivery complications 31

4. INTERVENTIONS, MEDICATIONS, NOTES • Record other important information pertaining to resuscitation event that was not captured in previous sections, including: – Name of person who performed invasive interventions – Baby’s response to interventions performed – Type of suctioning performed (i. e. , oropharyngeal or tracheal) and type/ amount of secretions (e. g. , meconium, mucus, etc. ) – Umbilical Venous Catheter (UVC) size, insertion depth, confirmation method, and name of person who inserted it – Procedures or diagnostic tests performed, including volume of blood taken for test, and results (if available/ reported) – Time of arrival and designation of additional health care providers who present to resuscitation event – Baby’s condition post-resuscitation – How baby was transported post-resuscitation 32
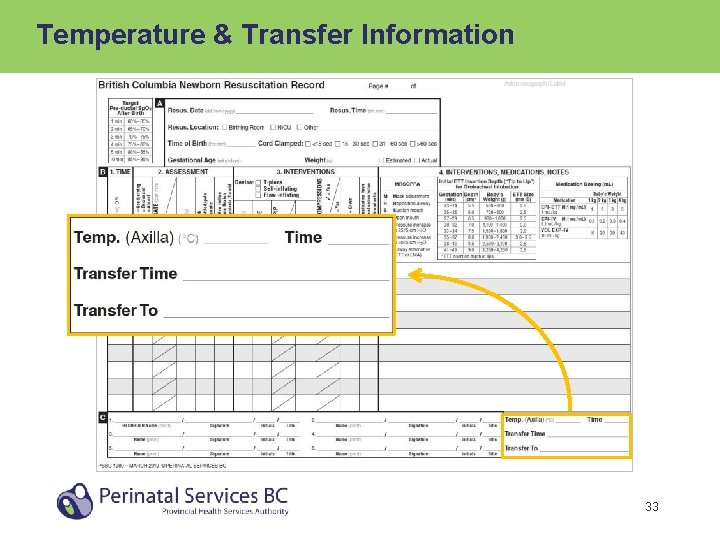
Temperature & Transfer Information 33

Temperature & Transfer Information • Record baby’s axillary temperature at end of resuscitation or at 10 minutes, whichever is first • Record time when baby’s axillary temperature was assessed Go to #4. INTERVENTIONS, MEDICATIONS, NOTES • If a servo temperature probe applied to the baby, record temperature at 5 minute intervals 34
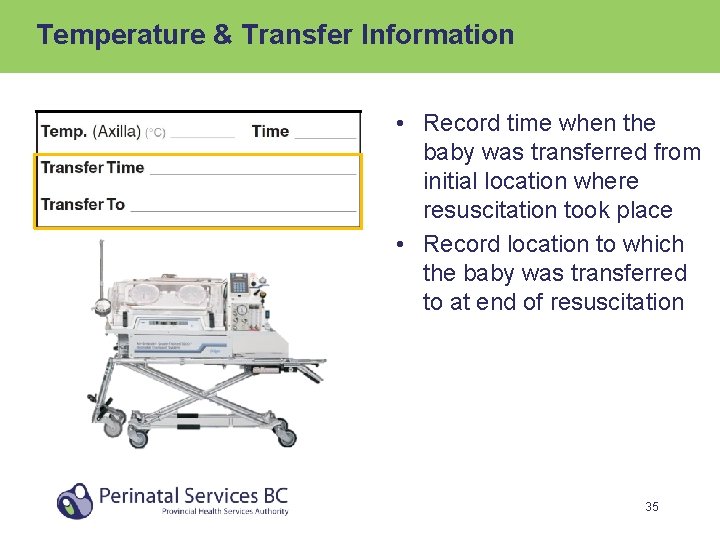
Temperature & Transfer Information • Record time when the baby was transferred from initial location where resuscitation took place • Record location to which the baby was transferred to at end of resuscitation 35

5. ADDITIONAL NARRATIVE NOTES (Page 2) • Following the neonatal resuscitation, record a retrospective narrative summary of event to supplement real-time documentation of assessments and interventions (Sections 1 -4) 36

C. Sign-Offs • This section identifies all those present at the resuscitation event, including the Recorder • Should be completed after resuscitation event • The recorder and all other personnel present must print, sign, initial and indicate their profession in the designated fields – A signature indicates that the individual has read and is in agreement with everything as it is documented on the Newborn Resuscitation Record – The recorder’s information should be specified in the first entry 37

CASE STUDY 38

Case Study You are asked to be the recorder at the vaginal delivery of a 41 + 5 week baby. The mother is 31 years old, G 1 P 1. Induction of labour has been started 10 hours ago. Membranes ruptured spontaneously 3 hours ago. The fetal heart tracing is atypical and the amniotic fluid now shows some thick meconium staining. 39

Case Study • • After collecting a copy of the Newborn Resuscitation Record, a clipboard and a pen, you position yourself where you are able to see and hear everything the team will do in the event of a resuscitation. While the team is preparing for the imminent birth you have time to complete some parts of Section A: Demographics and Background of the Newborn Resuscitation Record: 1 13/02/2019 40/5 Baby Doe Since the addressograph will not be available until after the birth of the baby you document the baby’s surname (maternal surname). SVD, atypical fetal tracing, thick meconium present. 40

30 Seconds • • The baby is born at 14: 35. The team announces that it is a boy. Baby appears apneic and limp, so the team dries and stimulates the baby. At 30 seconds the baby is still apneic and limp, the cord is clamped and cut, and the baby is brought over to the warmer. 1 Baby Doe 13/02/2019 Male 14: 35 40/5 15 sec Ø H SVD, atypical fetal tracing, thick meconium present. Baby dried and stimulated. 30 sec Ø H Cord cut at 30 sec and baby brought to warmer. 41
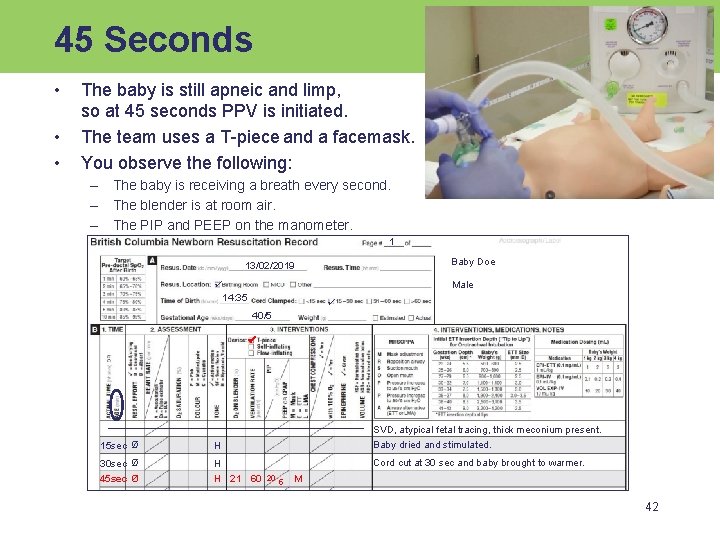
45 Seconds • • • The baby is still apneic and limp, so at 45 seconds PPV is initiated. The team uses a T-piece and a facemask. You observe the following: – The baby is receiving a breath every second. – The blender is at room air. – The PIP and PEEP on the manometer. 1 Baby Doe 13/02/2019 Male 14: 35 40/5 15 sec Ø H SVD, atypical fetal tracing, thick meconium present. Baby dried and stimulated. 30 sec Ø H Cord cut at 30 sec and baby brought to warmer. 45 sec Ø H 21 60 20 5 M 42
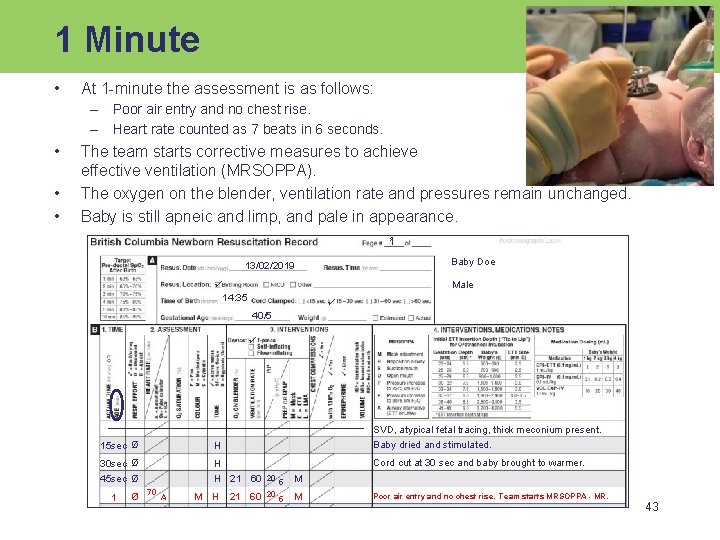
1 Minute • At 1 -minute the assessment is as follows: – Poor air entry and no chest rise. – Heart rate counted as 7 beats in 6 seconds. • • • The team starts corrective measures to achieve effective ventilation (MRSOPPA). The oxygen on the blender, ventilation rate and pressures remain unchanged. Baby is still apneic and limp, and pale in appearance. 1 1 Baby Doe 13/02/2019 Male 14: 35 40/5 15 sec Ø H SVD, atypical fetal tracing, thick meconium present. Baby dried and stimulated. 30 sec Ø H Cord cut at 30 sec and baby brought to warmer. 45 sec Ø 1 Ø 70 A M H 21 60 20 H 20 21 60 5 M Poor air entry and no chest rise. Team starts MRSOPPA - MR. 43

1 Minute 20 Seconds • At 1 -minute 20 -seconds the assessment is as follows: – Poor air entry and some chest rise. – Heart rate counted as 7 beats in 6 seconds. – The rest of the parameters remain the same. • Team moves to SO of MRSOPPA: – Thick mucus and meconium removed from airway when suctioned. 1 1 Baby Doe 13/02/2019 Male 14: 35 40/5 15 sec Ø H SVD, atypical fetal tracing, thick meconium present. Baby dried and stimulated. 30 sec Ø H Cord cut at 30 sec and baby brought to warmer. 45 sec Ø 1: 20 Ø 70 70 A A M M H 21 60 20 5 M Poor air entry and no chest rise. Team starts MRSOPPA - MR. 5 M Poor air entry, some chest rise. SO - suction, thick mucus, mec. 44
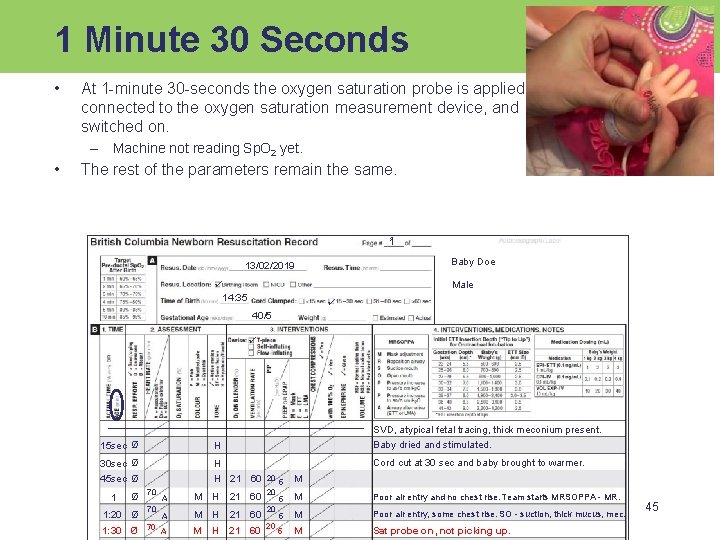

1 Minute 30 Seconds • At 1 -minute 30 -seconds the oxygen saturation probe is applied, connected to the oxygen saturation measurement device, and switched on. – Machine not reading Sp. O 2 yet. • The rest of the parameters remain the same. 1 1 Baby Doe 13/02/2019 Male 14: 35 40/5 15 sec Ø H SVD, atypical fetal tracing, thick meconium present. Baby dried and stimulated. 30 sec Ø H Cord cut at 30 sec and baby brought to warmer. 45 sec Ø 1: 20 Ø 1: 30 Ø 70 70 70 A M H 21 60 20 H 20 21 60 A M H 21 60 20 20 5 M Poor air entry and no chest rise. Team starts MRSOPPA - MR. 5 M Poor air entry, some chest rise. SO - suction, thick mucus, mec. 5 M Sat probe on , not picking up. 45

1 Minute 40 Seconds • • At 1 -minute 40 -seconds the team reports that the baby is making respiratory efforts. Air entry has improved, there is chest rise, and the heart rate is 9 beats in 6 seconds. The ventilation rate is decreased to 40 breaths per minute. The team reports that the baby’s tone is improving. You notice that the O 22 saturation is 58%, so you alert the team leader to consider administering additional oxygen to meet target saturations. The team leader orders oxygen to be increased to 30%. No change in other parameters. 1 1 Baby Doe 13/02/2019 Male 14: 35 40/5 [Previous entries omitted from view. ] 1: 40 90 A 58 M SF 30 40 20 5 M Baby starting to make some respiratory efforts. 46
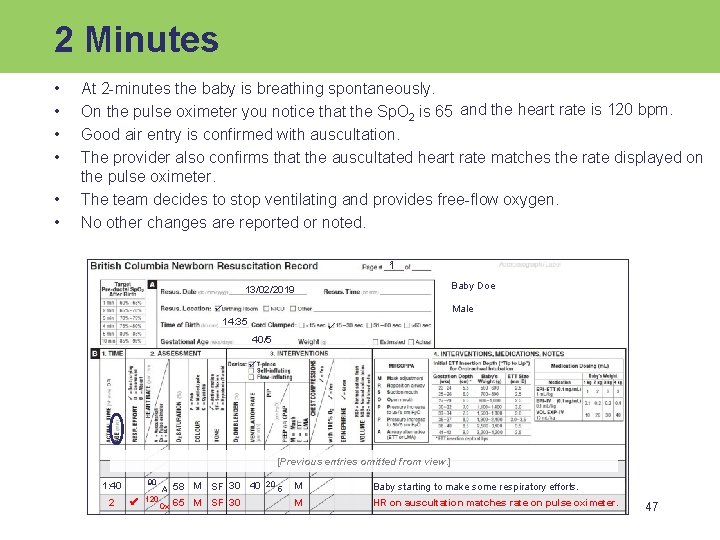

2 Minutes • • • At 2 -minutes the baby is breathing spontaneously. On the pulse oximeter you notice that the Sp. O 2 is 65 and the heart rate is 120 bpm. Good air entry is confirmed with auscultation. The provider also confirms that the auscultated heart rate matches the rate displayed on the pulse oximeter. The team decides to stop ventilating and provides free-flow oxygen. No other changes are reported or noted. 1 1 Baby Doe 13/02/2019 Male 14: 35 40/5 [Previous entries omitted from view. ] 1: 40 90 2 120 A Ox 58 M SF 30 40 65 M SF 30 20 5 M Baby starting to make some respiratory efforts. M HR on auscultation matches rate on pulse oximeter. 47
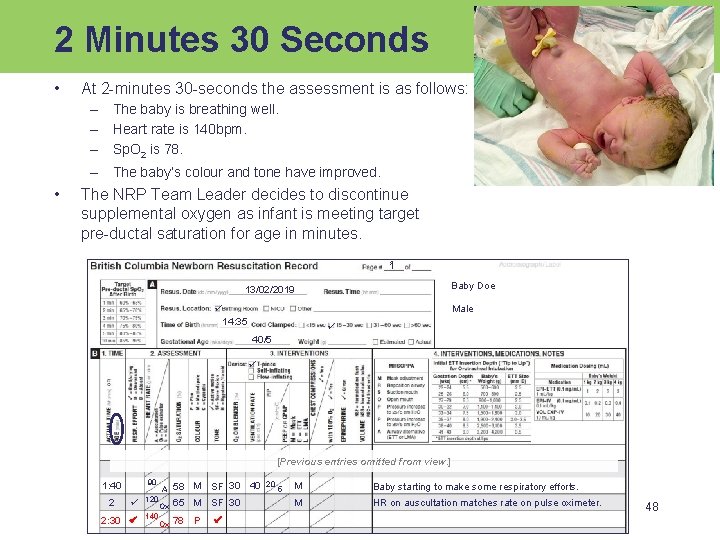
2 Minutes 30 Seconds • At 2 -minutes 30 -seconds the assessment is as follows: – The baby is breathing well. – Heart rate is 140 bpm. – Sp. O 2 is 78. – The baby’s colour and tone have improved. • The NRP Team Leader decides to discontinue supplemental oxygen as infant is meeting target pre-ductal saturation for age in minutes. 1 1 Baby Doe 13/02/2019 Male 14: 35 40/5 [Previous entries omitted from view. ] 1: 40 90 2 120 2: 30 140 A 58 M SF 30 40 Ox 65 M SF 30 Ox 78 P 20 5 M Baby starting to make some respiratory efforts. M HR on auscultation matches rate on pulse oximeter. 48

Completion of Newborn Resuscitation Record 1 1 Complete: • End of Section B • Section C • Page # section 1 Baby Doe 13/02/2019 Male 14: 35 40/5 15 sec Ø H 30 sec Ø H 45 sec Ø 1 Ø 70 70 1: 20 Ø 1: 30 Ø 1: 40 2 2: 30 70 90 A M A A A 120 Ox 140 Ox Best Recorder RT Breath M SVD, atypical fetal tracing, thick meconium present. Baby dried and stimulated. Cord cut at 30 sec and baby brought to warmer. H 21 60 M H 21 60 58 M SF 30 40 20 20 20 5 M M Poor air entry and no chest rise. Team starts MRSOPPA - MR. 5 M Poor air entry, some chest rise. SO - suction, thick mucus, mec. 5 M M Sat probe on, not picking up. Baby starting to make some respiratory efforts. M HR on auscultation matches rate on pulse oximeter. 5 5 65 M SF 30 78 P Best Recorder BR RN RT Breath RTB RT Dr. Very Nice VN MD 36. 8 14: 42 49
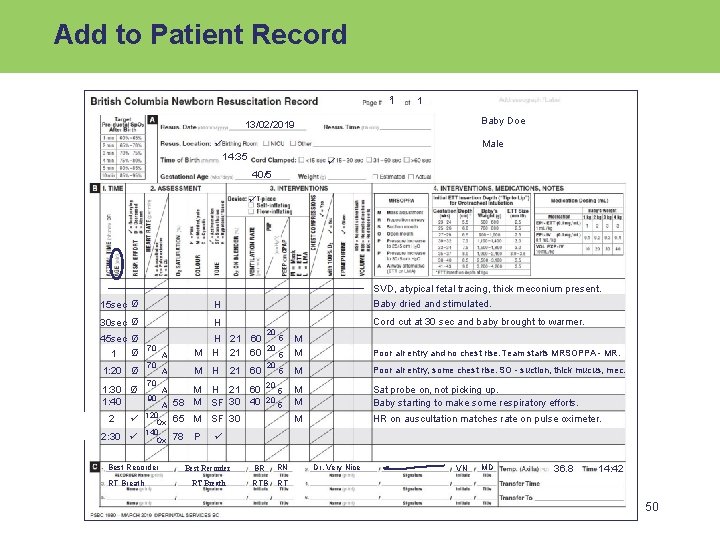

Add to Patient Record 1 1 1 Baby Doe 13/02/2019 Male 14: 35 40/5 15 sec Ø H 30 sec Ø H 45 sec Ø 1: 20 Ø 1: 30 Ø 1: 40 2 2: 30 70 70 70 90 RT Breath A M A A A 120 Ox 140 Ox Best Recorder M SVD, atypical fetal tracing, thick meconium present. Baby dried and stimulated. Cord cut at 30 sec and baby brought to warmer. H 21 60 M H 21 60 58 M SF 30 40 20 20 20 5 M M Poor air entry and no chest rise. Team starts MRSOPPA - MR. 5 M Poor air entry, some chest rise. SO - suction, thick mucus, mec. 5 M M Sat probe on, not picking up. Baby starting to make some respiratory efforts. M HR on auscultation matches rate on pulse oximeter. 5 5 65 M SF 30 78 P Best Recorder BR RN RT Breath RTB RT Dr. Very Nice VN MD 36. 8 14: 42 50

SUMMARY 51
52
QUESTIONS
- Slides: 53