Basildon and Brentwood CCG Annual General Meeting 4

Basildon and Brentwood CCG Annual General Meeting 4. 30 pm 12 September 2019 Dr Boye Tayo, Chair Lisa Allen, Clinical Accountable Officer

Agenda Welcome and introductions Accountable Officer’s Report Dr Boye Tayo, Chair Lisa Allen, Clinical Accountable Officer Annual Report for 2018/19 including: Quality & Safety Report 2018/19 Geraldine Rodgers on behalf of Teresa Kearney, Chief Nurse Performance 2018/19 Emma Timpson, Director of Planning and Performance Annual Accounts 2018/19 Dee Davey, Interim Chief Finance Officer Patient and Community Reference Group Questions and closing remarks Robert Hackett, PCRG Member Dr Boye Tayo, Chair

Welcome and who we are • • CCG established 1 st April 2013 Serve 279, 000 residents across Basildon and Brentwood 2018/19 budget of £ 354 m CCG commissions hospital, community, mental health and children’s services • Key providers in the STP include; o Basildon and Thurrock Hospital o Southend Hospital o Mid Essex Hospital (Broomfield) o Barking, Havering and Redbridge Hospital (Queens) o North East London Foundation Trust (Community and Children's Mental Health services) o Essex Partnership University Trust (Mental Health) o East of England Ambulance Service
Working as part of the Mid and South Essex STP
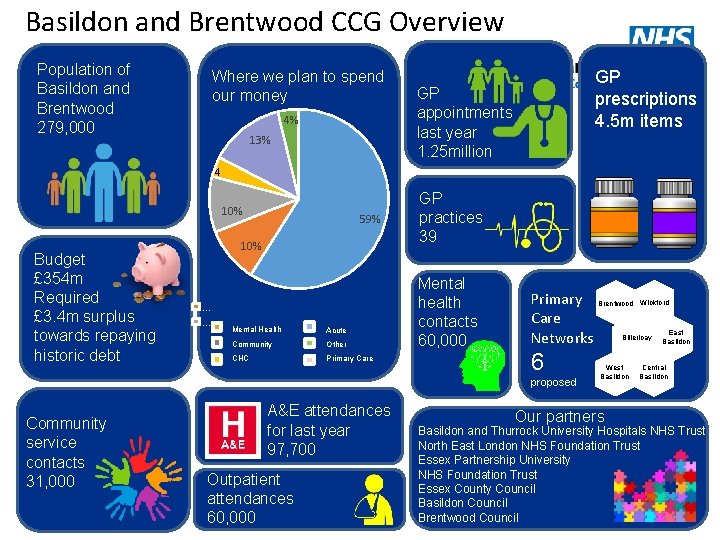
Basildon and Brentwood CCG Overview Population of Basildon and Brentwood 279, 000 Where we plan to spend our money 4% 13% GP prescriptions 4. 5 m items GP appointments last year 1. 25 million 4 10% Budget £ 354 m Required £ 3. 4 m surplus towards repaying historic debt 59% 10% . . . Mental Health Acute Community Other CHC Primary Care GP practices 39 Mental health contacts 60, 000 Primary Brentwood Wickford Care East Networks Billericay Basildon 6 proposed Community service contacts 31, 000 A&E attendances for last year 97, 700 Outpatient attendances 60, 000 West Basildon Our partners Central Basildon and Thurrock University Hospitals NHS Trust North East London NHS Foundation Trust Essex Partnership University NHS Foundation Trust Essex County Council Basildon Council Brentwood Council

TBC Overarching Focus • 2018/19 saw the early impact of the CCG’s work that focuses on the out of hospital model and in particular the transformation of primary care. • The CCG has worked closely with primary care colleagues to support the establishment of Primary Care Networks and new models for delivering primary care services such as the Acute Home Visiting Service. • In addition, the CCG has worked collaboratively with local partners to develop a common vision and priorities for the future.
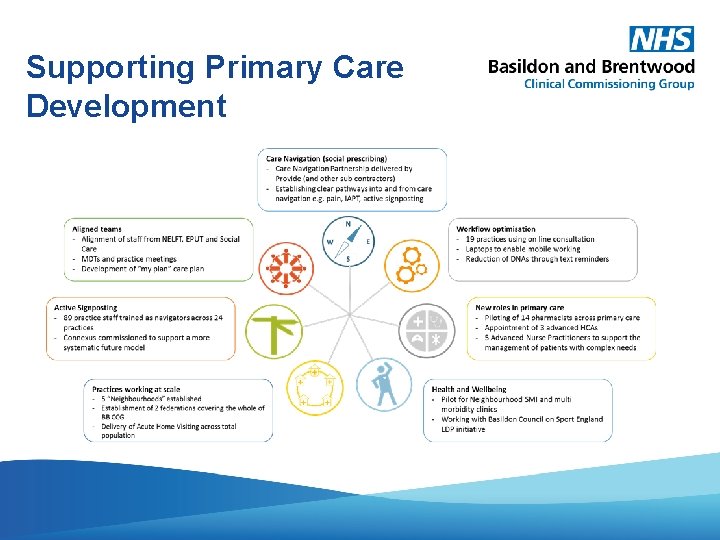
TBC Supporting Primary Care Development

Clinical Accountable Officer’s Report Lisa Allen, Clinical Accountable Officer

Achievements • Further development and implementation of the Aligned Team Model • Implemented a new “Acute Home Visiting Service” that provides a consistent approach to the delivery of primary care home visits across the whole CCG. • Worked with the four other CCGs and other stakeholders within the STP to develop a Primary Care Strategy and investment plan • Commission of signposting across primary care to offer suitable alternatives to seeing GPs. • Piloted new roles in primary care including pharmacists, Advanced Nurse Practitioners and advanced Health Care Assistants

Achievements • Alongside Essex County Council, we have; • Embedded a Trusted Assessor Model within Basildon Hospital • Supported the Frailty Assessment model at Basildon Hospital by funding additional therapists and a coordinator role • Invested additional therapy capacity in intermediate care wards improving outcomes for patients. • Working with stakeholders, we have supported a 25% reduction in the number of patients spending more than 21 days in hospital • Successfully procured a new provider of Improving Access to Psychological Therapies services

Achievements • Embedding of social prescribing across key stakeholders • Working with partners, implemented a comprehensive Mental Health Rapid Assessment Service in Basildon Hospital • Implemented a new Cows Milk Protein Allergy pathway across primary, community and acute paediatric services. • Significantly improved compliance with the four hour A&E standard despite increased A&E Activity As a CCG we achieved a ‘Good’ rating from NHSE/I against the indicators in the CCG Improvement and Assessment Framework • Implementation of an Organisational Development programme • Internal and external audit rating of ‘satisfactory’ • Improved staff survey • Improved 360 stakeholder survey

Plans for 2019/20 • Operational Plan ‘Transforming Together’ set out CCG ambitions for next two years: - Primary Care Networks to be at the heart of local health transformation - Community services integrated and aligned around Primary Care Networks - Implementation of Integrated Care System from April 2021 - Single management team for five CCGs in Mid & South Essex - Infrastructure, IT and Estates, supports new models of working • CCG working within the STP will set out it’s plans over the next five years to meet the challenges set out in the NHS Long Term Plan
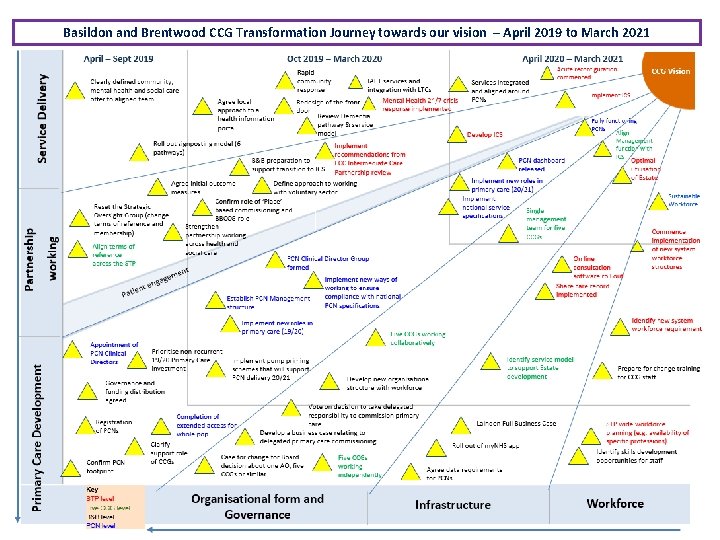
Basildon and Brentwood CCG Transformation Journey towards our vision – April 2019 to March 2021

Operational Plan Summary 2019/20 Objectives We will: • Work in partnership with our communities to enable people to live full, active, and independent lives, promoting self-care and building resilience • Lead and enable our partners to deliver safe, high quality, equitable care with less variation • Give clear and consistent messages on the availability of health services and fund the things we know will work and reduce waste • Be an organisation of clinical and managerial leaders who have the necessary skills, capacity and capability to lead positive change for the communities we serve. Transformation Programme Primary Care development: change how care is delivered by moving towards GP led services supported by a wider range of roles, delivered at scale through Primary Care Networks Partnership working: move towards an Integrated Care System (ICS) that improves the health and well being of our local population Service delivery: transform out of hospital care and align services where possible around Primary Care Networks. Reconfigure acute hospital services to create larger specialist teams (STP led) • • • Enablers • • • Organisational form & governance: adapts to the changing commissioning and ICS landscape whilst supporting CCG staff through the change Workforce: create a modern health workforce that attracts and retains staff Infrastructure: provision of digital solutions, IT, data analytics and Estates that supports new models of care within available resources Cross Cutting Programme • Urgent & Emergency Care Ensure patients receive the right care in the right place • Mental Health Improve access to services and crisis response services • Children & Young People Establish system wide plan • Maternity Improve safety, choice and personalisation • Transforming Care Improve services and support for people with learning disabilities • Continuing Healthcare & PHBs Adoption of best practice including Personal Health Budgets • Medicines Management Ensure optimal prescribing • Cancer and Elective Care Improve access and patient pathways (STP led) Outcomes • • - Finance Move towards financial balance Achieve QIPP savings Support overall system sustainability Effective use of investment Deliver Mental Health Investment Standard Quality Better experience of care Improved access Better Health outcomes for people with long term conditions, cancer and mental health issues Sustainable workforce Performance Achieve constitutional standards Deliver NHSE Targets on Mental Health, Primary Care and LD Reduction in activity growth in acute sector Our values B Be Honest B Be Accountable C Clinically Led C Compassionate and Respectful G Growing Together

Partnership Working The CCG recognises that we cannot fulfil our ambitions without our partners and as such, we have worked closely with a broad range of partners throughout 2018/19. Our approach to partnership working is across three tiers; 1). At an STP level, the CCG has worked closely with fellow CCGs, councils and trusts to develop a cross organisational vision and key outputs such as the Primary Care Strategy. 2). At a CCG level, the CCG has engaged key partners from health, social care and local authorities to begin the implementation of a local model of care. 3). At a more local level, the CCG has worked with localities and the emerging PCNs to form strong partnerships with primary care and patients to ensure that local variation is addressed within any service change

Quality and Safety Report 2018/19 Geraldine Rodgers, Deputy Chief Nurse on behalf of Teresa Kearney, Chief Nurse

CCG Responsibility • The CCG is accountable for the monitoring of patient safety and the quality of services. • The commissioned providers range from the local maternity services, community care, continuing healthcare plans through to end of life care services.

Areas of focus this past year • Harm Free Care Agenda - Working collaboratively with health care partners • The Learning Disability Mortality Review (Le. De. R) • Special Educational Needs & Disability (SEND) • Discharge to Assess (D 2 A) • Engaging people and communities • Safeguarding for vulnerable adults and children

Local Maternity System (LMS) Maternity Transformation Programme Recommendation from Better Births: Each pregnant woman will have consistency in having the same midwife or clinical team throughout the three phases of her maternity journey

2019/20 Quality Priorities Learning Disability and Autism Local Maternity Services Workforce Enhanced Care Homes Linking with the Long Term Plan 2019– making sure everyone gets the best start in life, delivering world class care for major health problems and supporting people to age well.

Performance 2018/19 Emma Timpson, Director of Planning, Performance & Demand Management

Delivery in 2018/19 – A&E 95. 7% patients seen within 4 hours at Basildon Hospital (March 19) 80. 9% patients seen within 4 hours at Basildon Hospital (March 18) 7, 429 17, 041 more attendances than in 2017/18 more people seen within 4 hours than in 2017/18 South West A&E Delivery Board led improvement programme 7, 880 less people waited 4 hours or longer compared with 2017/18
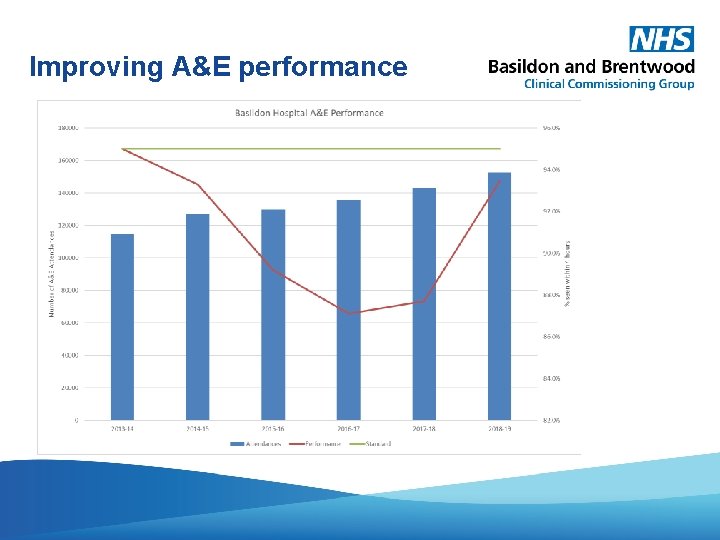
Improving A&E performance

Delivery in 2018/19 – Constitutional Standards Referral to Treatment (RTT) 81. 9% patients treated within 18 weeks (target 92%) Diagnostics 97. 1% of diagnostic tests take place within 6 weeks of referral (target 99%) • Basildon Hospital missed the RTT and diagnostic standard for 2018/19 year. • The Hospital continues to implement a recovery plan focusing on reducing its waiting list size to less than the March 2018 position by March 2020 to meet the national guidance. • Throughout 2018/19 the commissioning Quality Team worked with BTUH to ensure that all significant patient waits beyond 52 weeks were subject to a robust clinical harms review. • Commissioners have expanded capacity with community providers and supported outsourcing patients in particular stretched specialties.
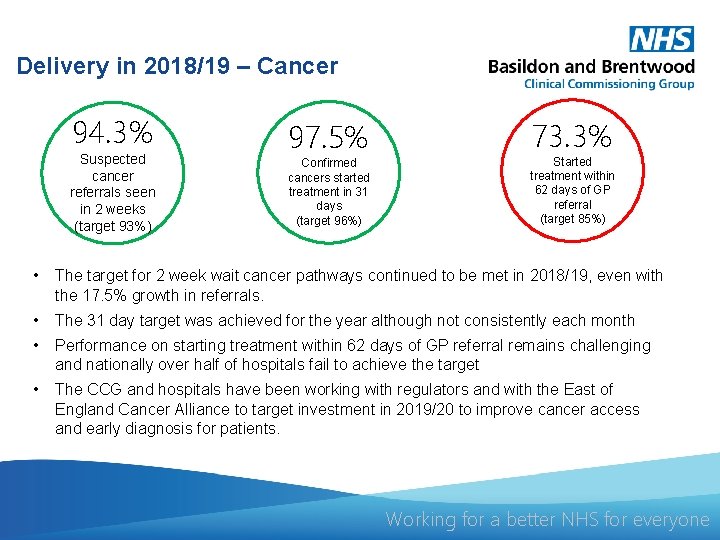
Delivery in 2018/19 – Cancer 94. 3% Suspected cancer referrals seen in 2 weeks (target 93%) 97. 5% Confirmed cancers started treatment in 31 days (target 96%) 73. 3% Started treatment within 62 days of GP referral (target 85%) • The target for 2 week wait cancer pathways continued to be met in 2018/19, even with the 17. 5% growth in referrals. • The 31 day target was achieved for the year although not consistently each month • Performance on starting treatment within 62 days of GP referral remains challenging and nationally over half of hospitals fail to achieve the target • The CCG and hospitals have been working with regulators and with the East of England Cancer Alliance to target investment in 2019/20 to improve cancer access and early diagnosis for patients. Working for a better NHS for everyone

Delivery in 2018/19 – Mental Health Improving Access to Psychological Therapies 16. 35% Adults with anxiety and depression entering psychological therapies (target 17. 8%) 51. 5% Of people entering psychological therapies who reported recovery (target 50%) 99. 5% Of patients seen within 6 weeks of referral (standard 75%) 100% Of patients seen within 18 weeks of referral (Standard 95%) • The CCG achieved the recovery and waiting time standards for Psychological Therapies for 2018/19 year. • However, the % of patients accessing the service fell short of the target. This was due to reduced capacity in March 19 to support the transition to the new service provider from 1 April 19.

Delivery in 2018/19 – Mental Health 65. 5% Dementia register size against estimated size (target 67%) 31. 4% Access to community mental health services for children & young people (target 32%) Dementia Whilst the dementia diagnosis rate continues to improve the CCG fell below the standard. Our focus for the next year is on: • Support provided to patients and carers post diagnosis • End of life pathway; • Patients diagnosed previously with mild cognitive impairment. Children & Young People The numbers of Children & Young People accessing mental health services increased in 2018/19 and the CCG was close to meeting the target. There has also been an increase in the number of referrals to the Eating Disorder service: • 100% of children were seen within 4 weeks of referral • 66. 7% of children needing to be seen urgently were seen within a week

Annual Accounts 2018/19 Dee Davey, Interim Chief Finance Officer

Finance Review 2018/19 Publicly funded, from taxation, based upon an assessed need to spend We started the year with an accumulated deficit of £ 8. 4 m We were required to repay £ 3. 4 m of the deficit in 2018/19 We received £ 356. 9 m to meet service and management costs and to cover our required debt repayment = £ 1, 284 per head of population
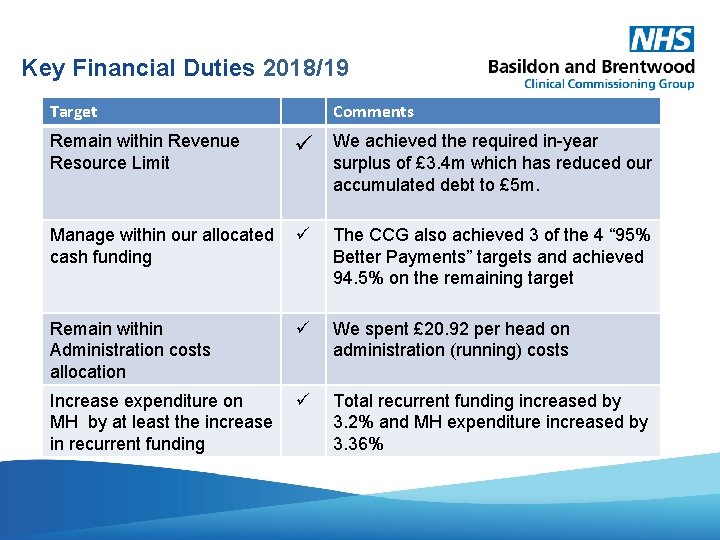

Key Financial Duties 2018/19 Target Remain within Revenue Resource Limit Comments We achieved the required in-year surplus of £ 3. 4 m which has reduced our accumulated debt to £ 5 m. Manage within our allocated cash funding The CCG also achieved 3 of the 4 “ 95% Better Payments” targets and achieved 94. 5% on the remaining target Remain within Administration costs allocation We spent £ 20. 92 per head on administration (running) costs Increase expenditure on MH by at least the increase in recurrent funding Total recurrent funding increased by 3. 2% and MH expenditure increased by 3. 36%

Finance Review 2018/19 £ 14. 8 m savings delivered Unqualified audit opinion on the 2018/19 accounts External Audit concluded that the CCG has adequate arrangements in place to secure economy, efficiency and effectiveness on the CCG’s use of resources – known as the “value for money conclusion”
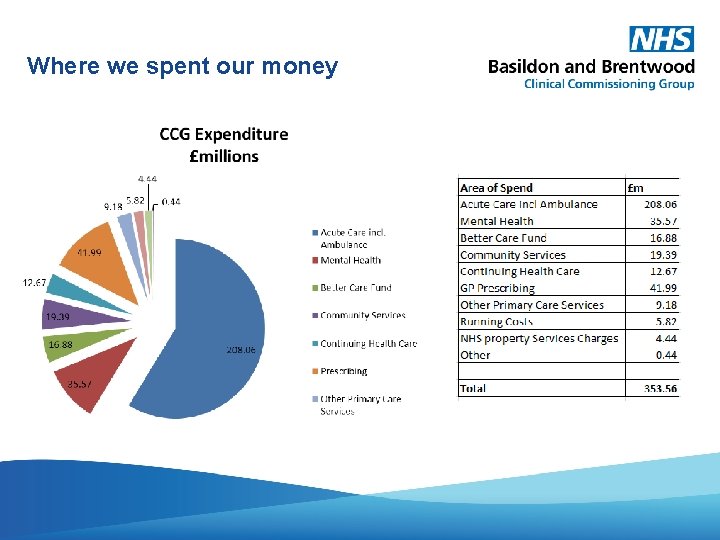
Where we spent our money

Patient and Community Reference Group Bob Hackett, PCRG Member

Who are we? Brentwood Care Centre July 2018 Basildon Town Centre 2010

Who are we? • Demographics • People power • Change • = PATIENTS

Our fit? The CCG Governing Body will seek the views of the Patient & Community Reference Group (PCRG) in respect of commissioning developments or changes they are considering and will take these views into account in their decision making

Our fit? A CRITICAL FRIEND - Challenge - Support - Argue Constructively - Offer Alternatives And to make sure that policy makers have the ‘patients /service users’ view point, and best interests, at the centre of their decision making!

How are we doing? Achievements 2018/19 MSK Connect: Patient Survey IAPT: Improving Access to Psychological Therapy: Vita Minds Winter Communications Integrated Care for M&SE Community Teams Mental Health Pathway in A&E Workshops/ Focus groups Freestyle Libre/ Retinal Eye screening

How are we doing? Achievements 2018/19 MSK Connect: Patient Survey Patient complaints Met with providers Surveyed changes Followed up IAPT: Improving Access to Psychological Therapy: Vita Minds Presentations from provider Followed up feedback following launch

Patient Participation is… • • • • Patients who are Active in taking Responsibility for their health and work as a Team with their practice to ensure that patients are well Informed about health matters which affect the Community, Individual patients and the Practice, look to raise Awareness of wider issues in the NHS, including the use of Technology. Involved and can have influence in improving the quality of care. Objectives are to improve the patient experience in primary care in the NHS

We need you

Any Questions? • Please speak to any of the PCRG members during the breaks if you wish further discussion • Thank you – Bob Hackett, PCRG member, Basildon and Brentwood CCG

Closing remarks and Questions?
- Slides: 43