Basics of Transfusion Therapy Resident Education Lecture Series

Basics of Transfusion Therapy Resident Education Lecture Series

Hemoglobin Level and Symptoms HGB (GM%) SYMPTOMS 9 -11 MINIMAL 7. 5 EXERTIONAL DYSPNEA 6. 0 WEAKNESS 3. 0 DYSPNEA AT REST 2 -2. 5 HEART FAILURE LINMAN NEJM 279: 812, 1968

RBC Transfusion: Indications n Acute Blood Loss n Symptomatic Anemia n Suboptimal O 2 Capacity n Exchange (SS, Co)
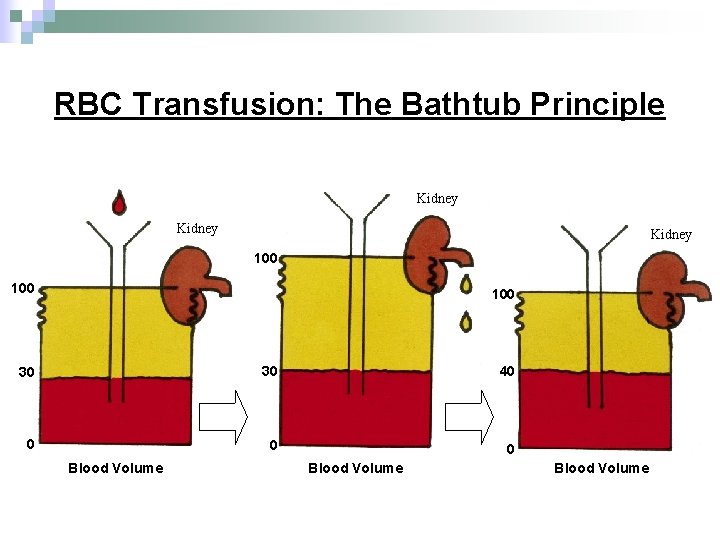
RBC Transfusion: The Bathtub Principle Kidney 100 100 30 30 40 0 Blood Volume

Pre-Transfusion Testing n BLOOD TYPING: ¨ ABO, D Antigens only (Other antigens are weak immunogens) n ANTIBODY SCREEN: ¨ Patient n serum vs. cell panel CROSSMATCH ¨ Major: Patient Serum vs. Donor Cells

RBC Products n PRBC MOST TRANSFUSIONS n WHOLE BLOOD ACUTE BLEEDING EXCHANGE PLASMA NEEDED n WASHED REMOVE PLASMA n FROZEN RARE RBC PHENOTYPE IRRADIATED CMV NEGATIVE IMMUNODEFICIENT SERONEGATIVE, NEONATE n n

RBC Transfusion Volume n Usual: Up to 15 cc/Kg in 3 -4 hours n Unusual: Acute Hemorrhage: replace ongoing losses Chronic Anemia, Heart Failure, îBP 2 cc/Kg/Gm HGB Diuretic Exchange

Transfusion Volume n 10 cc/Kg PRBC 10 cc/kg 2. 4 GM% n 2. 4 GM% in HGB = X cc/kg Desired HGB rise PRBC cc = Blood Volume x (HGBF- HGBI) HGBT BV=70 cc/KG, 80 -90 cc/KG newborn

Hemolytic Transfusion Reactions n Acute HTR ¨ Fatal n Acute HTR Delayed HTR 1/25, 000 1 -4/1, 000 1/5 -10, 000

Symptoms and Signs of Acute Hemolytic Reactions n n n n Severe Back Pain Substernal Tightness, Dyspnea Hypotension / Circulatory collapse Vomiting, diarrhea Icterus Hemoglobinuria Renal shutdown Diffuse Oozing from wounds/punctures

Response to Suspected Hemolytic Reaction n Stop Transfusion Hydrate Specimens to Blood Bank ¨ Unit/Bag ¨ Serum ¨ Red cells ¨ Urine

Acute Hemolysis: Diagnosis n n n Do a direct antiglobulin test on posttransfusion sample Obtain post-transfusion blood and urine and inspect visually Recheck paperwork Recheck ABO type of unit and pre-and posttransfusion specimens Run urinalysis - to check for hemoglobinuria

Cause of Acute HTR n ABO incompatibility: source of error ¨ 10% at phlebotomy/labeling ¨ 23% in Transfusion Lab ¨ 67% transfusion administration (at the bedside)

Nonhemolytic Transfusion Reactions n Leukocyte Associated n FNHTR ¨ Transfusion GVHD ¨ Neonatal Neutropenia Citrate Toxicity ¨ Hypothermia ¨ Circulatory Overload ¨ n Immunoglobulin Associated Urticaria/Fever ¨ Ig E ¨ TRALI ¨ n Platelet Associated Post transfusion Purpura ¨ Neonatal Thrombocytopenia ¨ Metabolic/ Physical ¨ n Massive Transfusions Haemostatic Abnormalities ¨ Metabolic complications ¨ Hgb-O 2 Curve Shift ¨
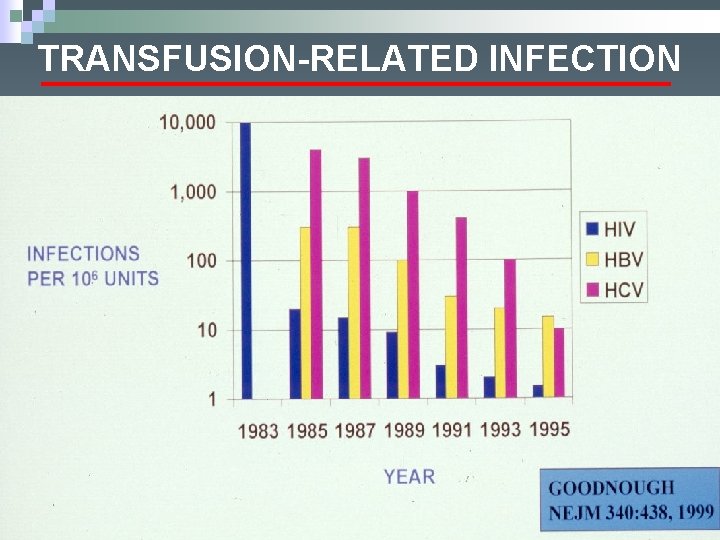
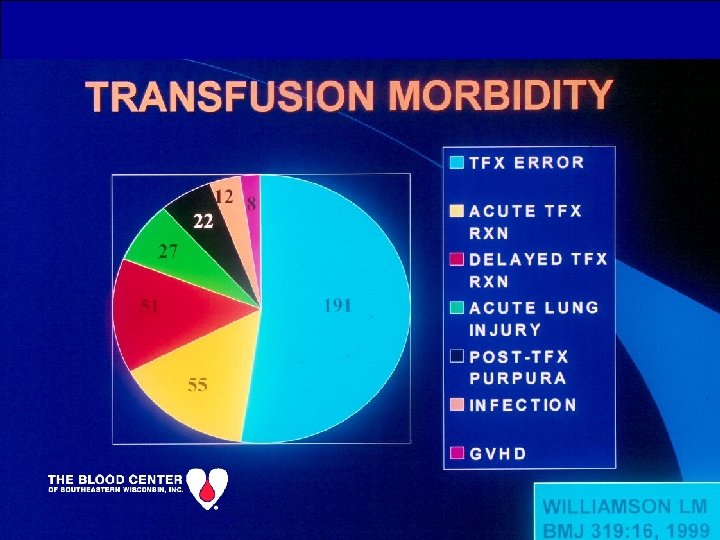
TRANSFUSION-RELATED INFECTION

Risk of Transfusion. Transmitted Infection HIV Hepatitis C Hepatitis B Hepatitis A HTLV I/II Bacteria 1 in 2, 000, 000 1 in 175, 000 Rare 1 in 3, 000 1/3, 000 (for platelets) Malaria, T Cruzi, Babesia, Yersinia, Syphilis, Lyme, CJD, West Nile Virus…? ?

Post Transfusion HCV Percent Incidence Chronic Cirrhosis 5 -10 50 20 Number 150 -300, 000 75 -150, 000 15 -30, 000
Neonatal Post Transfusion CMV n Incidence: 25% of seronegative infants receiving >50 ml CMV seropositive blood n Severity 50% severe or lethal manifestations

Neonatal Transfusion CMV Prevention by Filtering Blood Seroconvert/Total Filtered PRBC: 0/30 Unfiltered PRBC: 9/42 Gilbert, L 1: 98: 228, 1989

Prevention of Post Transfusion Infection n n n Don’t Transfuse Minimize Transfusion Limited Donors (dedicated units) Autologous Transfusions Erythropoetin Donor Screening: HIV Ab, HIV NAT, HCV Ab, HCV NAT, HBV Ag, Ab, HBc Ab, VDRL, West Nile NAT, HTLVI/II Ab, CMV Ab, Bacterial Culture (Platelets)

Strategies to Decrease Operative RBC Transfusion Hemostasis Hemodilution Cell salvage DDAVP Autologous Transfusion Erythropoetin
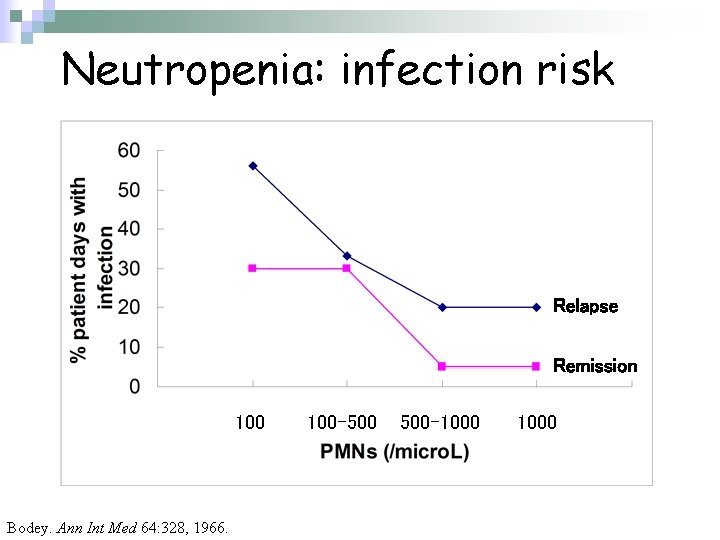
Neutropenia: infection risk Relapse Remission 100 Bodey. Ann Int Med 64: 328, 1966. 100 -500 500 -1000

WBC Indications 2004 n PMN: n Ly: Newborn Sepsis Congenital/Acquired Neutropenia PMN Dysfunction Refractory Gram Negative Sepsis Disseminated Varicella-Zoster

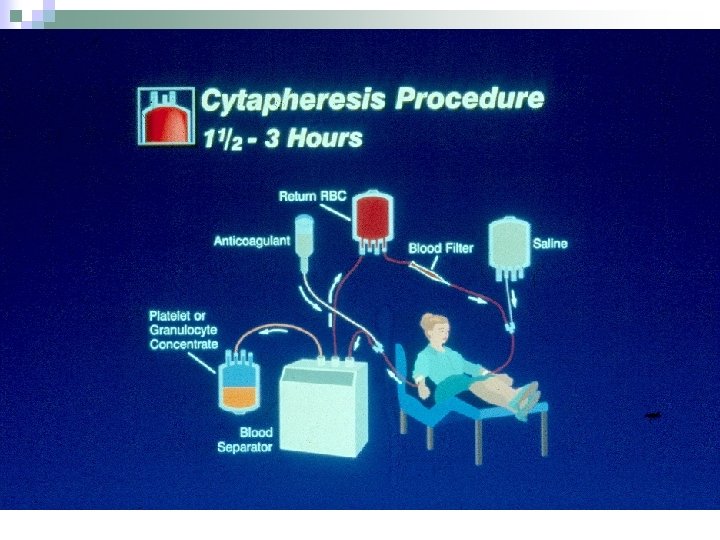
WBC transfusion: Logistics Donors Receive G-CSF +/- Decadron n 2 -3 Hour Cytapheresis n 1010 Cells by Standards n Donors pretested for ID markers n Cells decay rapidly: limited value at > 6 hours post-collection n Quantitative impact limited n

Fresh Frozen Plasma 200 -250 ml of plasma containing all clotting factors, AT III, Protein C & S. n Compatibility Important n Can Give: A plasma to A or O patient B plasma to B or O patient O plasma to O patient AB plasma to anyone n

Indications: FFP n Replacement of Coagulation Factors ¨ Abnormal Bleeding with coagulopathy n Multiple factor deficiency: ¨ ¨ n Isolated factor deficiency-no concentrate ¨ n Factor XI, XIII Replacement of regulatory proteins ¨ TTP, n Liver disease DIC Reversal of Warfarin Dilutional Hereditary angioedema Not indicated for: volume expansion, reversal of Heparin, correction of INR < 1. 5

Guidelines: FFP Use n n n Usual dosing: Adult 10 ml/Kg Peds 10 -15 ml/Kg 15 -20% rise in factor levels Usually does not correct laboratory coagulation status to “normal”
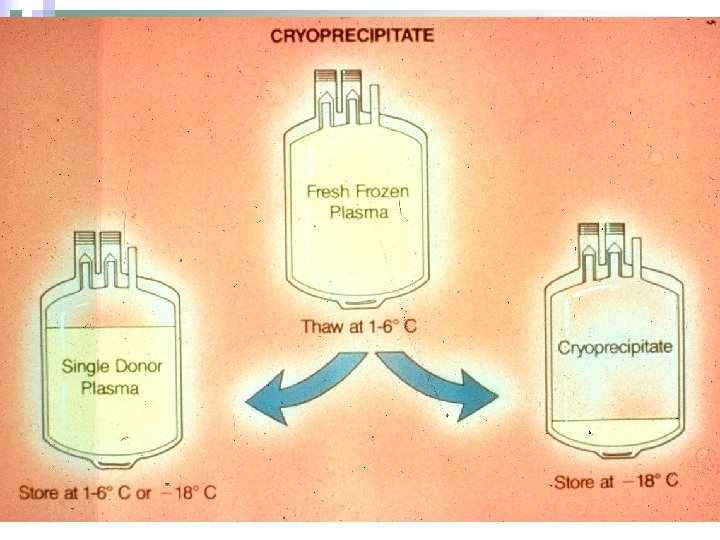

Cryoprecipitate n n n 10 -15 ml per unit (bag) Fibrinogen 250 mg Factor VIII 80 -120 units Von Willebrand Factor 40 -70% of FFP Factor XIII 20 -30% of FFP Fibronectin 20 -40 mg

Cryoprecipitate: Dosing n n n 1 -2 Units / 10 Kg Expect 60 -100 mg/dl rise in fibrinogen Goal: Fibrinogen 70 -100 mg/dl
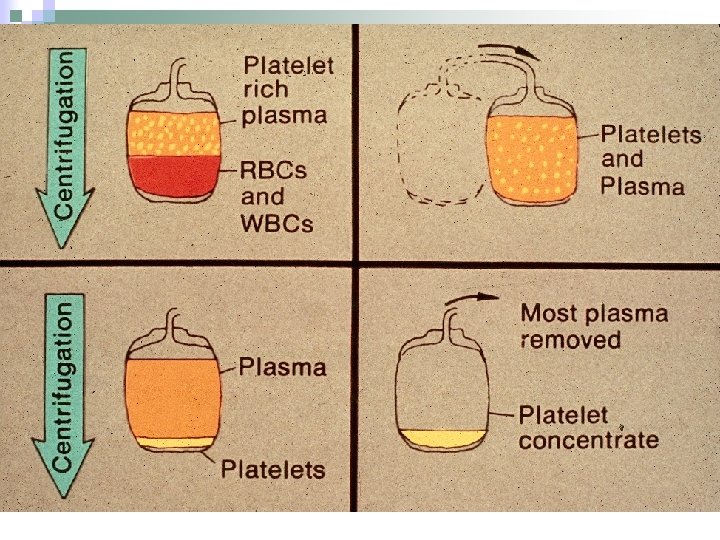

Platelets: Risk of Spontaneous Hemorrhage Count > 40, 000 20 -40, 000 5 -20 <5 Site Minimal GI Mucosa Skin, Mucus Membranes CNS, Lung
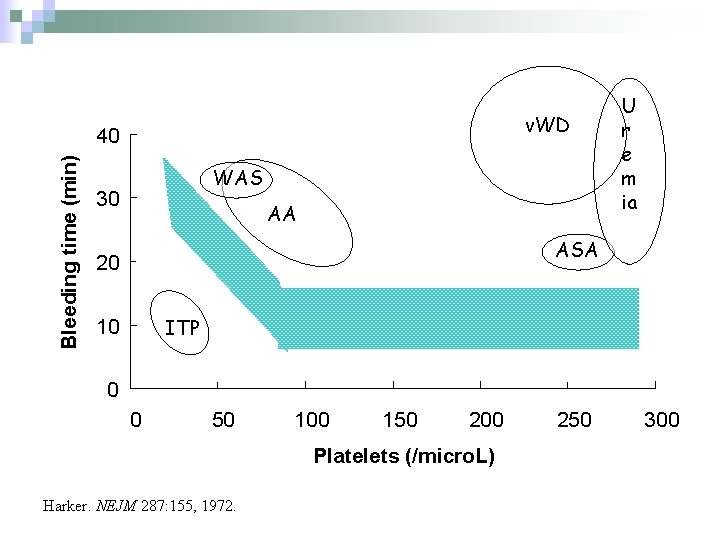
v. WD Bleeding time (min) 40 WAS 30 AA U r e m ia ASA 20 ITP 10 0 0 50 100 150 200 Platelets (/micro. L) Harker. NEJM 287: 155, 1972. 250 300

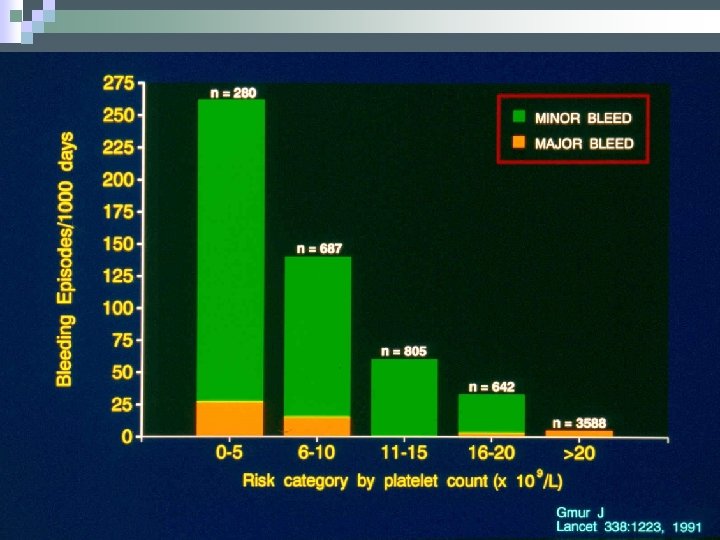
Prophylactic Platelet TX Guidelines Platelet Count/μl 0 -5, 000 5 -10, 000 11 -20, 000 >20, 000 Recommendation Always If Febrile of Minor Bleeding If coagulopathy or minor procedure If Major Bleed or invasive procedure

Transfused Platelets/Survival 6 units = 1 single donor unit (SDP); available as ¼, ½ and full SDP n Dose: child 1 unit/5 -6 kg n n n adult 1 unit/8 -10 kg Lifespan: 7 -10 Days Native 2 -3 Days Transfused Factors shortening Lifespan: ¨ Fever, Sepsis ¨ HLA, Platelet Specific Abs ¨ DIC ¨ Product Age?
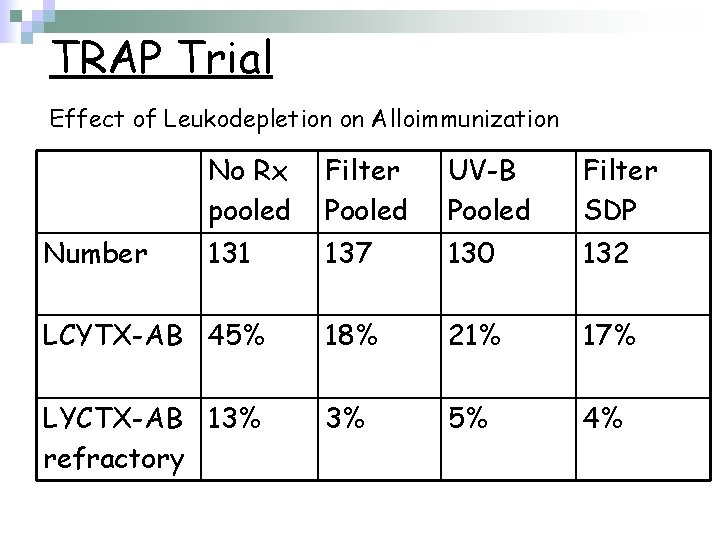
TRAP Trial Effect of Leukodepletion on Alloimmunization No Rx pooled Filter Pooled UV-B Pooled Filter SDP 131 137 130 132 LCYTX-AB 45% 18% 21% 17% LYCTX-AB 13% refractory 3% 5% 4% Number

When in Doubt: Call the Transfusion Service! 266 -2119


From ABP Certifying Exam Content Outline n 2. Transfusion and collection of blood n Understand the risk of transmitting infectious diseases during blood transfusion(s) n Recognize that erythrocyte transfusions may be associated with hemolytic, febrile, and urticarial reactions n Understand the role of erythrocyte transfusions in the management of anemia

Credits n Bruce Camitta MD M W Lankiewicz MD
- Slides: 43