Basics of Stem Cell Transplant Prof Ileana Constantinescu

Basics of Stem Cell Transplant Prof. Ileana Constantinescu

Background First successful transplants—late 1960 s n 30, 000 -40, 000 transplants performed yearly worldwide n >20, 000 patients have survived >5 years n Lazarus HM. Autologous and allogeneic transplantation procedures for hematologic malignancies. Manual of Clinical Hematology, 3 rd edition 2002: 399 -409

Graft Sources Allogeneic: from another person n Syngeneic: from an identical twin n Autologous: from the patient n n Choice of graft is based on disease type, patient condition, donor compatibility and health

Graft Sources n Autologous Transplant – No evidence of disease in the blood or bone marrow – Transplant related mortality (TRM) lowest with autos (<5%) – Relapse rates are higher depending on the disease – Absence of graft versus tumor effects Lazarus HM. Autologous and allogeneic transplantation procedures for hematologic malignancies. Manual of Clinical Hematology, 3 rd edition 2002: 399 -409

Graft Sources n Allogeneic Transplants – High TRM (30 -50%) – Lower relapse rates due to graft versus tumor effects – Graft versus host effects n Matched Related Donor (siblings) – 25% chance a sibling will be a match – The more siblings a patient has the better chance for a match Lazarus HM. Autologous and allogeneic transplantation procedures for hematologic malignancies. Manual of Clinical Hematology, 3 rd edition 2002: 399 -409

GRAFT VS. HOST DISEASE n This disease occurs when an immunologically competent foreign graft containing T cells reacts against the MHC antigens of an immunologically compromised host. In general, concerns regarding the outcome of transplantation represent a one-way street, namely the potential of the immune system of a transplant recipient or host to reject a transplant. An interesting reversal of the direction of the immune response occurs, however, when immunocompetent cells (spleen cells) are transplanted into a host whose immune system is not functioning properly (irradiated) and is, therefore, immunosuppressed. In this case, a phenomenon known as graft vs. host disease ensues, where the immunocompetent graft directs an immunological assault against the host, sometimes with fatal consequences. Graft vs. host disease is, therefore, of particular concern in cases of bone marrow transplantation, where immunocompetent T cells in the graft tissue can direct a graft rejection response against the cell surface MHC antigens of a frequently immunocompromised recipient or host. n 6

HLA Typing HLA typing became feasible in 1960 s n Linked on chromosome 6 n Inherited as haplotypes n 1 in 4 chance a sibling will be identical n Copelan EA. Hematopoietic stem-cell transplantation. NEJM 2006; 354: 18131826.

HLA alleles n The considerable polymorphism of HLA is wellknown. n HLA polymorphism is reflected by allelic substitution of many amino acid residues in the polypeptide chains, especially the external domains which contain the peptide binding site. n This affects the spectrum of antigenic peptides presented by the different allelic types of HLA molecules and the repertoire of responding Tcells.

The HLA genetics is complex n HLA polymorphism n Expression of HLA polymorphism –Typing n The transplanted graft represents a continuous source of HLA alleles that can induce a rejection response at any time post-transplant. n HLA matching can have a dualistic effect on transplant outcome: it reduces rejection but conversely, it may promote other HLA-restricted mechanisms of allograft injury.

HLA Matching n 6/6, 8/8, or 10/10 – HLA loci on chromosome 6 – HLA-A, HLA-B, HLA-C, HLA-DR, HLA-DQ, HLA-DP n ABO incompatibility is not an exclusion Lazarus HM. Autologous and allogeneic transplantation procedures for hematologic malignancies. Manual of Clinical Hematology, 3 rd edition 2002: 399 -409
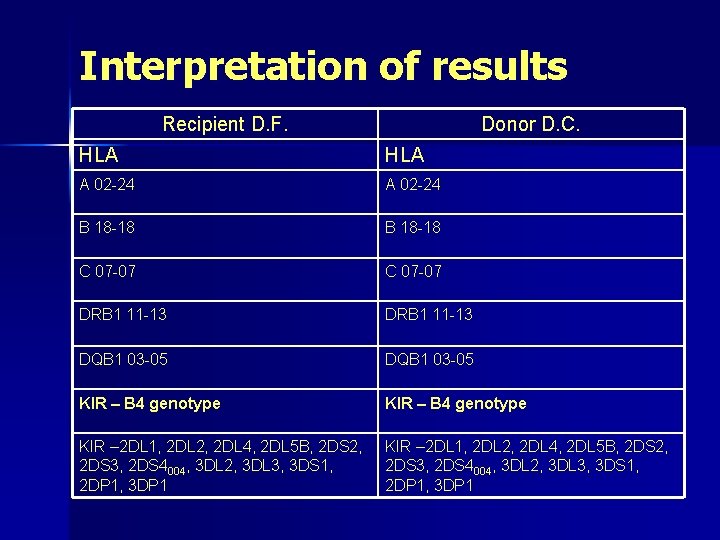
Interpretation of results Recipient D. F. Donor D. C. HLA A 02 -24 B 18 -18 C 07 -07 DRB 1 11 -13 DQB 1 03 -05 KIR – B 4 genotype KIR – 2 DL 1, 2 DL 2, 2 DL 4, 2 DL 5 B, 2 DS 2, 2 DS 3, 2 DS 4004, 3 DL 2, 3 DL 3, 3 DS 1, 2 DP 1, 3 DP 1
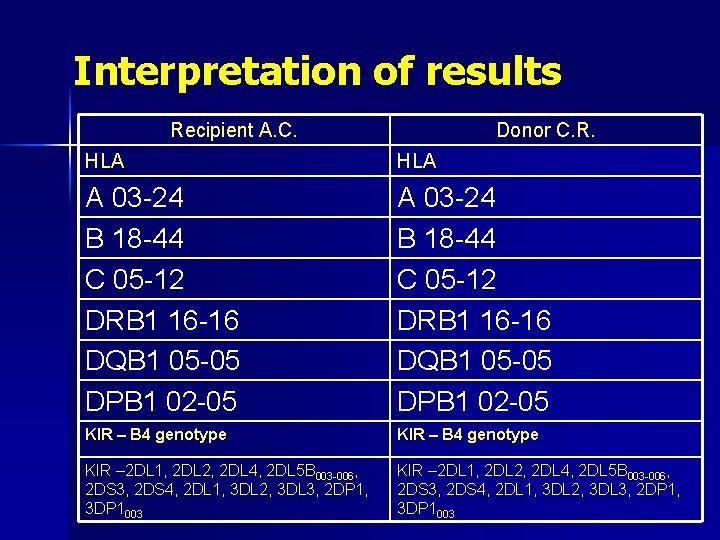
Interpretation of results Recipient A. C. Donor C. R. HLA A 03 -24 B 18 -44 C 05 -12 DRB 1 16 -16 DQB 1 05 -05 DPB 1 02 -05 KIR – B 4 genotype KIR – 2 DL 1, 2 DL 2, 2 DL 4, 2 DL 5 B 003 -006, 2 DS 3, 2 DS 4, 2 DL 1, 3 DL 2, 3 DL 3, 2 DP 1, 3 DP 1003
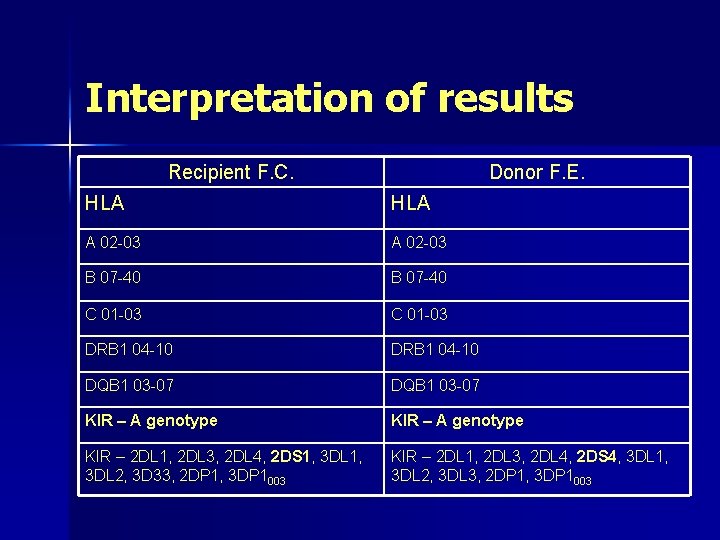
Interpretation of results Recipient F. C. Donor F. E. HLA A 02 -03 B 07 -40 C 01 -03 DRB 1 04 -10 DQB 1 03 -07 KIR – A genotype KIR – 2 DL 1, 2 DL 3, 2 DL 4, 2 DS 1, 3 DL 2, 3 D 33, 2 DP 1, 3 DP 1003 KIR – 2 DL 1, 2 DL 3, 2 DL 4, 2 DS 4, 3 DL 1, 3 DL 2, 3 DL 3, 2 DP 1, 3 DP 1003

Eligibility n Age < 65 – Autologous, mini-allo n Age < 55 – Myeloablative allogeneic n Exclusions – CHF, uncontrolled diabetes mellitus, active infections, renal insufficiency

Indications Autologous Transplant n n n n Multiple myeloma NHL Hodgkin’s disease AML Neuroblastoma Ovarian cancer Germ-cell tumors n n Autoimmune disorders Amyloidosis Copelan EA. Hematopoietic stem-cell transplantation. NEJM 2006; 354: 18131826.

Indications for Allogeneic Transplant n n n n n AML ALL CML MDS MPD NHL Hodgkin’s Disease CLL Multiple myeloma Juvenile CML n n n n n Aplastic anemia PNH Fanconi’s anemia Blackfan-Diamond Thalessemia major Sickle cell anemia SCID Wiskott-Aldrich Inborn errors of metabolism Copelan EA. Hematopoietic stem-cell transplantation. NEJM 2006; 354: 1813 -1826.

Preparative Regimens n Myeloablative – High doses of chemotherapy +/- radiation – 3 goals n Eliminate malignancy n Immunosuppression to allow engraftment n Decrease graft versus host effects Copelan EA. Hematopoietic stem-cell transplantation. NEJM 2006; 354: 1813 -1826. Lazarus HM. Autologous and allogeneic transplantation procedures for hematologic malignancies. Manual of Clinical Hematology, 3 rd edition 2002: 399 -409

Myeloablative Regimens n Myeloablative Regimens – Most common regimens n Cyclophosphamide/TBI n Busulfan/Cyclophosphamide n Stem cells are essential to restore marrow function Copelan EA. Hematopoietic stem-cell transplantation. NEJM 2006; 354: 1813 -1826. Lazarus HM. Autologous and allogeneic transplantation procedures for hematologic malignancies. Manual of Clinical Hematology, 3 rd edition 2002: 399 -409

Myeloablative Regimens Therapy is based on disease n Other drugs n – Etoposide, BCNU, cytarabine, melphalan n Graft versus leukemia effects in allogeneic donors Lazarus HM. Autologous and allogeneic transplantation procedures for hematologic malignancies. Manual of Clinical Hematology, 3 rd edition 2002: 399 -409 Copelan EA. Hematopoietic stem-cell transplantation. NEJM 2006; 354: 18131826.

Umbilical Cord Blood n 1 st UCB transplant 16 years ago – Child with Fanconi’s anemia n Cell dose is given per recipient weight – Lower patient weights the high the cell dose – 2 x 107 nucleated cells/kg – 1. 7 x 107 CD 34+ cells/kg n 4/6 match UCB with sufficient cells has a similar outcome to a matched or one antigen mismatched MUD Chao NJ, Emerson SG, Weinberg KI. Stem cell transplantation (Cord Blood Transplants). Am Soc Hematol Ed Book. 2004: 354 -371.

Umbilical Cord Blood n Umbilical Cord Blood – Cryopreserved – Small number of stem cells – Higher incidence of engraftment failure n Using more than one unit in adults – Lower risk of GVHD – Degree of matching not as stringent Chao NJ, Emerson SG, Weinberg KI. Stem cell transplantation (Cord Blood Transplants). Am Soc Hematol Ed Book. 2004: 354 -371.

Umbilical Cord Blood Lower GVHD n TRM not different than MUD n Can be used with myeloablative or nonmyeloablative conditioning (on a clinical trial) n Chao NJ, Emerson SG, Weinberg KI. Stem cell transplantation (Cord Blood Transplants). Am Soc Hematol Ed Book. 2004: 354 -371.

Complications n Early – Mucositis – Sinusoidal obstructive syndrome (VOD) n Fluid retention, jaundice, hepatomegaly – Transplant related infections n Damage to mouth, gut and skin n Prolonged neutropenia Copelan EA. Hematopoietic stem-cell transplantation. NEJM 2006; 354: 18131826.

Complications n Early – Pancytopenia n PRBC and platelet transfusions n Broad spectrum antimicrobials n Antifungals if prolonged fevers 3 -5 days Lazarus HM. Autologous and allogeneic transplantation procedures for hematologic malignancies. Manual of Clinical Hematology, 3 rd edition 2002: 399 -409

Complications n Early – Graft Versus Host Disease n Acute GVHD to day 100 – Skin, GI tract, liver Copelan EA. Hematopoietic stem-cell transplantation. NEJM 2006; 354: 18131826. Lazarus HM. Autologous and allogeneic transplantation procedures for hematologic malignancies. Manual of Clinical Hematology, 3 rd edition 2002: 399 -409

GVHD n In GVH diseases donor-derived immuno-competent lymphocytes react with HLA incompatible recipient cells and induce inflammatory responses in host tissues such as the skin and gastrointestinal tract. n GVH disease seems more likely in cases whereby the donor is well matched for the patient. n Direct and indirect HLA allorecognition mediate GVH reactions if immunocompetent donor cells recognize recipient incompatibilities. n During infection, microbial antigens are processed by APC and presented via HLA molecules to T-cells that elicit cytotoxic and DTHlike inflammatory reactions in the allograft.

Complications n Early – Graft Rejection n Host versus graft n Drug injury to marrow n Viral infections: CMV, HHV-6 & 8 – Interstitial Pneumonitis n Diffuse alveolar hemorrhage n Too few donor stem cells n ARDS often caused by CMV Lazarus HM. Autologous and allogeneic transplantation procedures for hematologic malignancies. Manual of Clinical Hematology, 3 rd edition 2002: 399 -409

Complications n Delayed – Chronic GVHD n Scleroderma or Sjogrens syndrome n Bronchiolitis n Keratoconjunctivitis n Malabsorption n Cholestasis n Esophageal stricture Copelan EA. Hematopoietic stem-cell transplantation. NEJM 2006; 354: 18131826.

Late Complications n n Secondary Tumors – – – Acute leukemias, solid tumors, MDS Months to years after transplant Increased incidence with TBI – – Bacterial, viral fungal Months after transplant Associated with GVHD Need repeat vaccinations Late Infections n Pneumovax, Hep B, Hemophilus influenza b, poliovirus, diphtheria/tetanus, flu Lazarus HM. Autologous and allogeneic transplantation procedures for hematologic malignancies. Manual of Clinical Hematology, 3 rd edition 2002: 399 -409

Human herpesvirus 6 infection in hematopoietic cell transplant recipients Human herpesvirus 6 (HHV-6) is a member of the Roseolovirus genus of the beta-herpesvirus subfamily of human herpesviruses. There are two HHV-6 variants, HHV-6 A and HHV-6 B. Based on their distinctive biological properties and genome sequences, the Herpesvirales Study Group of the International Committee on Taxonomy of Viruses has classified HHV-6 A and HHV-6 B as two distinct herpesvirus species. n The vast majority of documented primary infections and reactivation events are due to HHV-6 B. HHV 6 B infects most children within the first three years of life and, like other herpesviruses, it establishes latency after primary infection. HHV-6 B may reactivate in immunocompromised hosts, especially following allogeneic hematopoietic cell transplantation (HCT). Encephalitis is the most clearly established clinical manifestation of HHV-6 reactivation in allogeneic HCT recipients, and may result in substantial morbidity. Little is known about the epidemiology or clinical implications of HHV-6 A. n The epidemiology, clinical manifestations, diagnosis, and treatment of HHV-6 infections in HCT recipients will be discussed here. HHV-6 infections in patients who are not HCT recipients are presented separately. EPIDEMIOLOGY n Human herpesvirus 6 (HHV-6) reactivation occurs in 30 to 70 percent of patients undergoing allogeneic hematopoietic cell transplantation (HCT) , with encephalitis occurring in only a small subset of these patients. HHV-6 reactivation often manifests as HHV-6 viremia, and typically occurs between two and four weeks after transplantation. HHV-6 B accounts for most reactivations, with HHV-6 A accounting for fewer than 3 percent of cases. n Risk factors — Both demographic and clinical factors may influence the risk of HHV-6 reactivation. As an example, recipients of allogeneic HCT are at higher risk of HHV-6 reactivation than recipients of autologous HCT; among allogeneic HCT recipients, those who receive transplants from unrelated or HLA-mismatched donors are at particularly increased risk. n

Romanian BMR Started in 2003 n EFI Accredited in 2006 n Holds details of stem cell donors and cord donations from Moldavia, Transilvania, Banat, Black Sea Coast, Walachia. n We need to contiue to recruit more donors, particularly from ethnic communities n HLA DNA 2 digits typed for HLA A, B, C, DRB 1 and DQB 1 n
- Slides: 31