Basics of Mechanical Ventilation Origins of mechanical ventilation

Basics of Mechanical Ventilation

Origins of mechanical ventilation • Negative-pressure ventilators (“iron lungs”) • first used in Boston Children’s Hospital in 1928 • Used extensively during polio outbreaks in 1940 s – 1950 s The iron lung created negative pressure in abdomen as well as the chest, decreasing cardiac output. Iron lung polio ward at Rancho Los Amigos Hospital in 1953.

Era of intensive care begun with this Positive-pressure ventilators Invasive ventilation first used at Massachusetts General Hospital in 1955 l Now the modern standard of mechanical ventilation l

Outline • Modes • Ventilator Settings • Indications to intubate • Indications to extubate • Trouble shooting

Pressure ventilation vs. volume ventilation Pressure-cycled modes: -deliver a fixed pressure at variable volume Volume-cycled modes: -deliver a fixed volume at variable pressure

Ventilator settings 1. 2. 3. 4. 5. 6. 7. 8. Ventilator mode Respiratory rate Tidal volume or pressure settings Inspiratory flow I: E ratio PEEP Fi. O 2 Inspiratory trigger
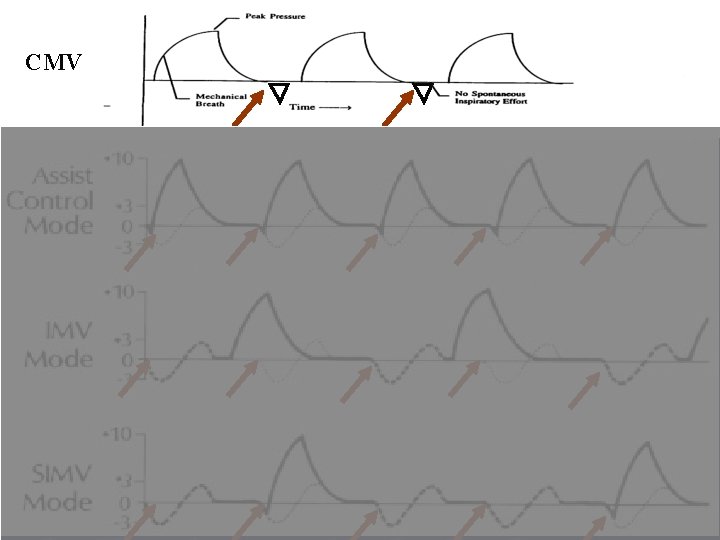
CMV
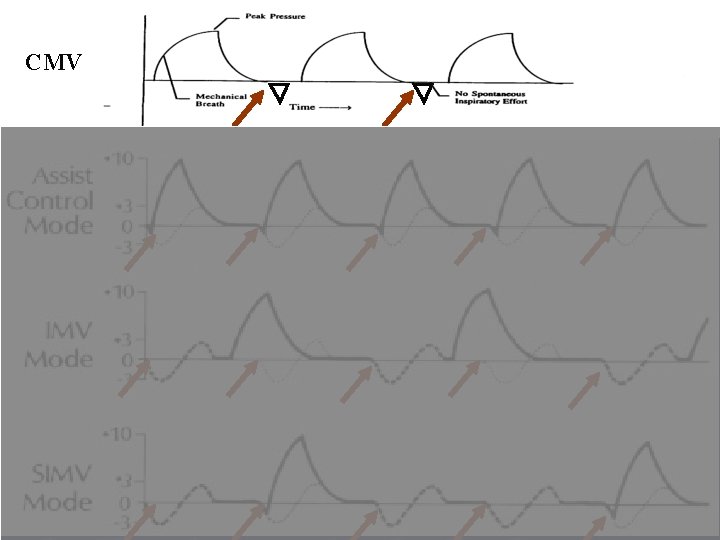
CMV
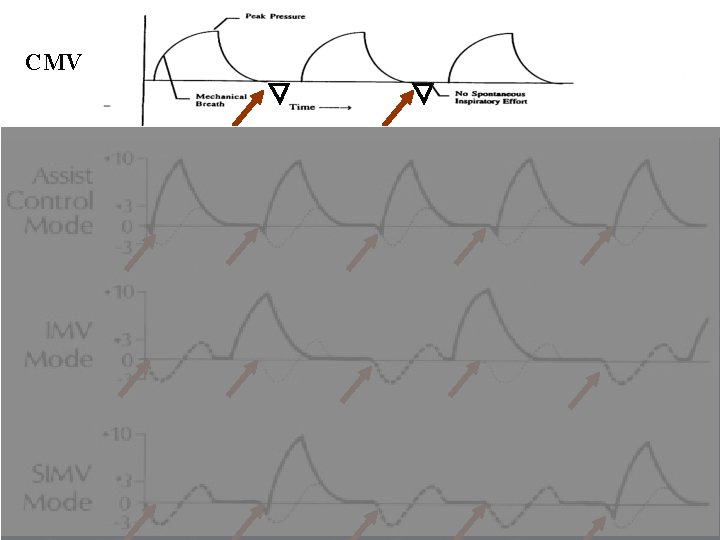
CMV
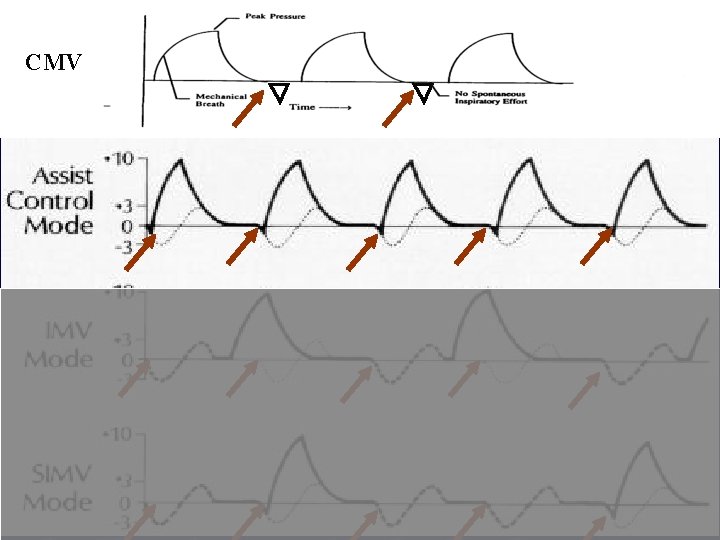
CMV
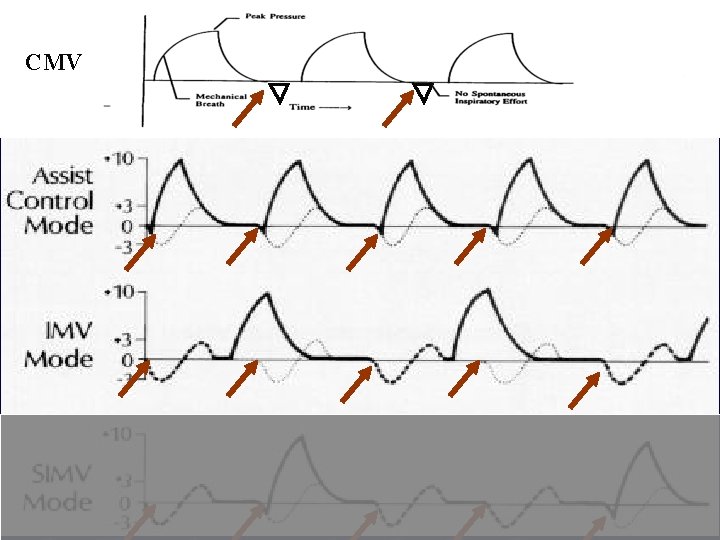
CMV
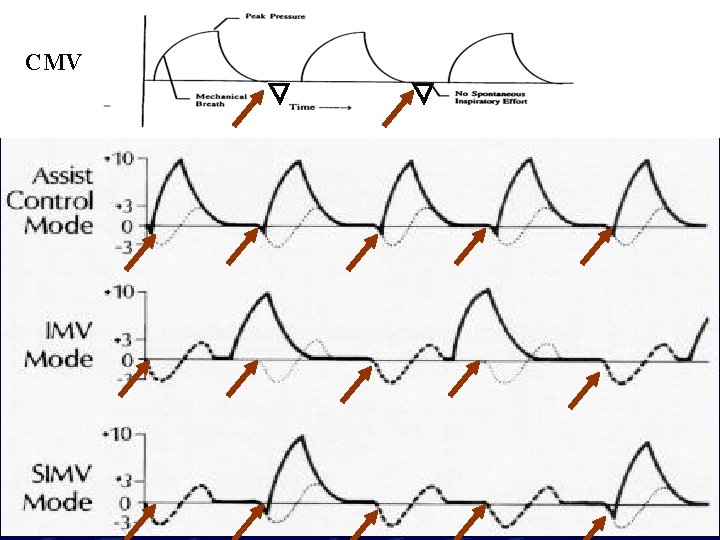
CMV
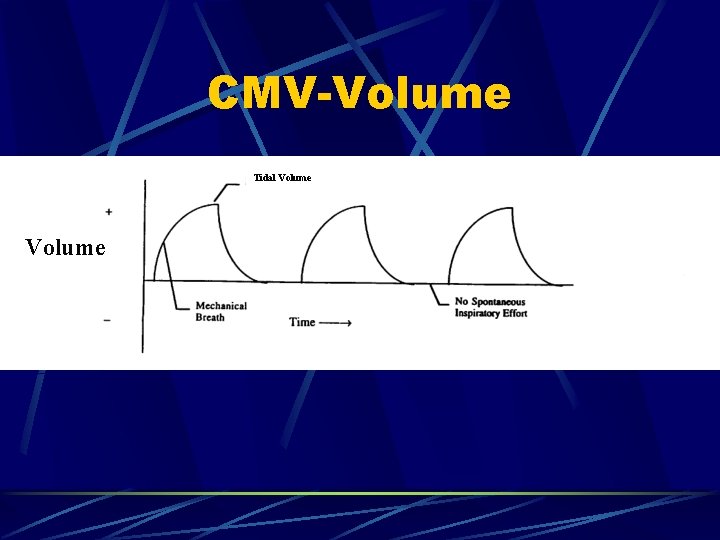
CMV-Volume Tidal Volume
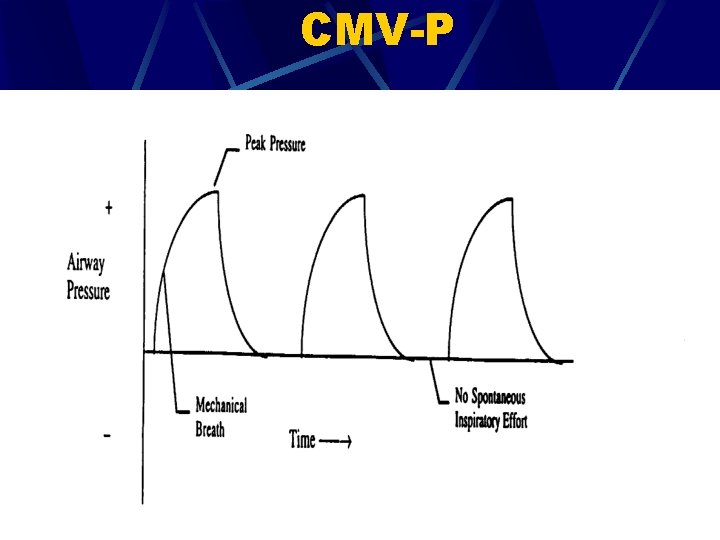
CMV-P
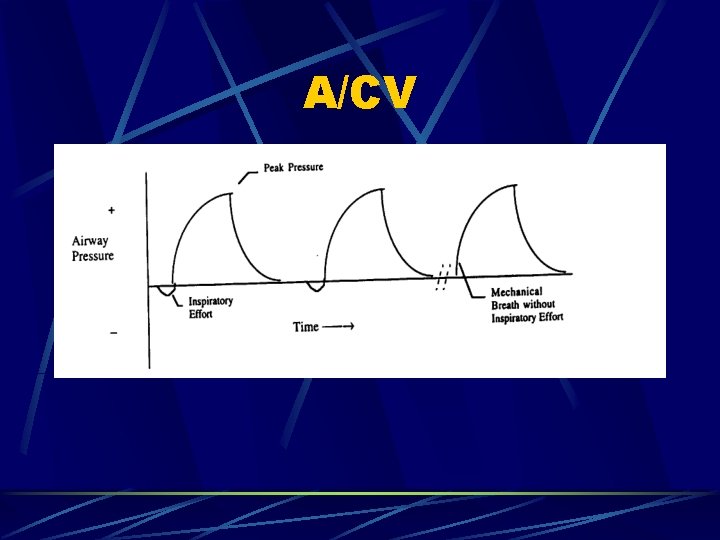
A/CV
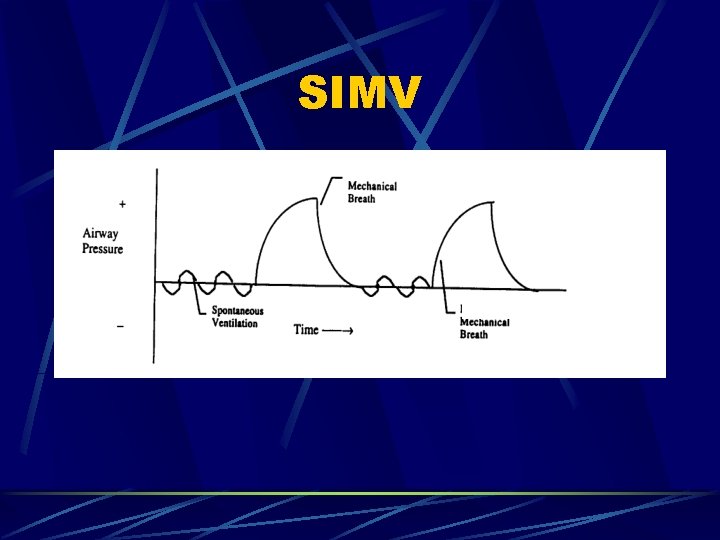
SIMV
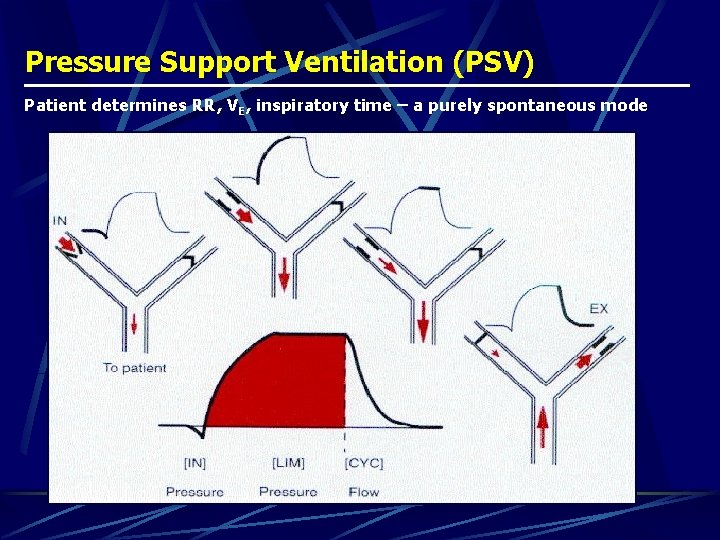
Pressure Support Ventilation (PSV) Patient determines RR, VE, inspiratory time – a purely spontaneous mode

CPAP and Bi. PAP CPAP is essentially constant PEEP; Bi. PAP is CPAP plus PS • Parameters · CPAP – PEEP set at 5 -10 cm H 2 O · Bi. PAP – CPAP with Pressure Support (5 -20 cm H 2 O) · Shown to reduce need for intubation and mortality

Respiratory Rate 10 -12/Min – Adult 20+_ 3 - Child 30 - 40 - New born

Respiratory Rate Increase – Hypoxia Hypercapnoea / Resp. Acidosis Decrease Hypocapnoea Resp. Alkalosis Asthma / COPD
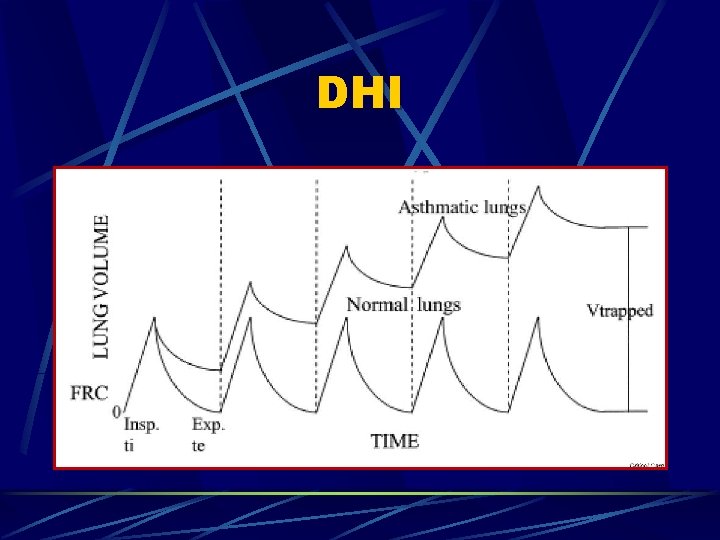
DHI

Hey not always the same buddy

Tidal Volume or Pressure setting Optimum volume/pressure to achieve good ventilation and oxygenation without producing alveolar overdistention Max = 6 -8 cc/kg

Inspiratory Trigger Normally set automatically 2 modes: Airway pressure l Flow triggering l

I: E Ratio Normaly 1: 2 Asthma/COPD 1: 3, 1: 4, … Severe hypoxia ARDS/ALI Pul. Edema 1: 1 , 2: 1

FIO 2 Goal – to achive Pa. O 2 > 60 mm. Hg or a sat >90% Start at 100% aim 40%

Vent settings to improve <oxygenation> PEEP and Fi. O 2 are adjusted in tandem • FIO 2 • Simplest maneuver to quickly increase Pa. O 2 • Long-term toxicity at >60% • Free radical damage • Inadequate oxygenation despite 100% Fi. O 2 usually due to pulmonary shunting • Collapse – Atelectasis • Pus-filled alveoli – Pneumonia • Water/Protein – ARDS • Water – CHF • Blood - Hemorrhage

Positive End-expiratory Pressure (PEEP) What is PEEP? Positive pressure measured at the end of expiration. What is the goal of PEEP? l l Improve oxygenation Recruit lung in ARDS Prevent collapse of alveoli Diminish the work of breathing

PEEP- Indications. If a Pa. O 2 of 60 mm. Hg cannot be achieved with a Fi. O 2 of 60% If the initial shunt estimation is greater than 25% Pulmonary edema ARDS/ALI Atelectosis

PEEP What are the secondary effec`ts of PEEP? Barotrauma l Diminish cardiac output l Regional hypoperfusion l Augmentation of I. C. P. ? l Paradoxal hypoxemia l Hypercapnoea and respiratory acidosis l

PEEP Contraindication: Barotrauma l Airway trauma l Hemodynamic instability l I. C. P. ? l Bronchospasm? l

Collapse/ atelectosis/ ARDS Increases Surface area for gas exchange Opens the collapsed lung PEEP Collapsed alveoli After PEEP
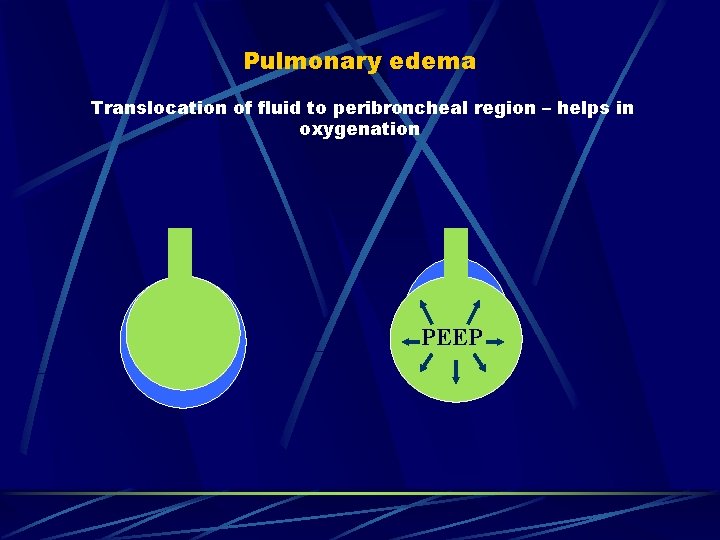
Pulmonary edema Translocation of fluid to peribroncheal region – helps in oxygenation PEEP

Trouble Shooting

DOPE D- Disposition of ETT O- Obstruction / kinking P- Pneumothorax E- Equipment failure
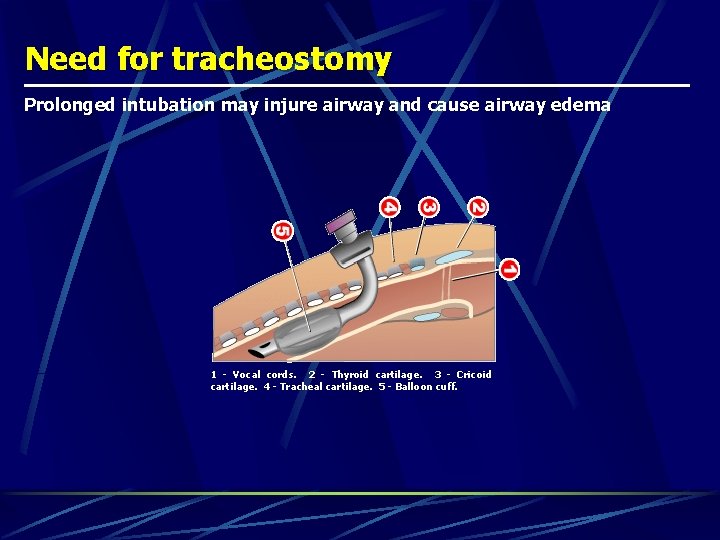
Need for tracheostomy Prolonged intubation may injure airway and cause airway edema 1 - Vocal cords. 2 - Thyroid cartilage. 3 - Cricoid cartilage. 4 - Tracheal cartilage. 5 - Balloon cuff.
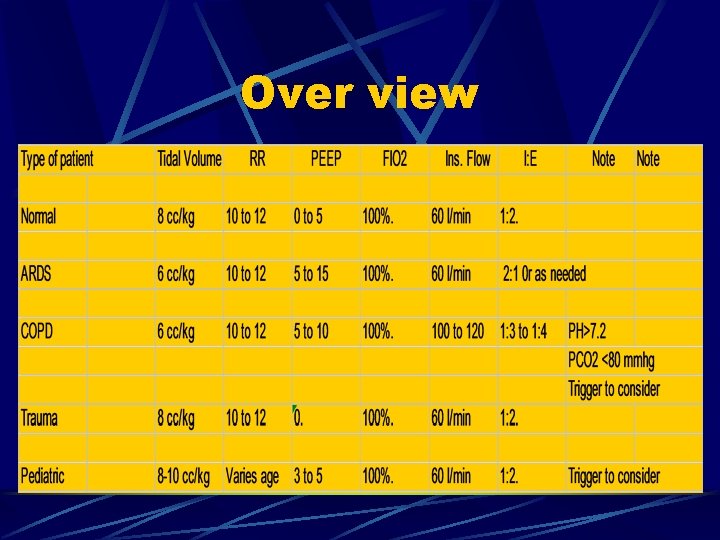
Over view

- Slides: 38