Basic structures of the eye Learning Objectives Basic

Basic structures of the eye

Learning Objectives • Basic Visual Optics • Identification of the major anatomical structures of the eye • Functions of structures of the eye • Blindness & ocular morbidity
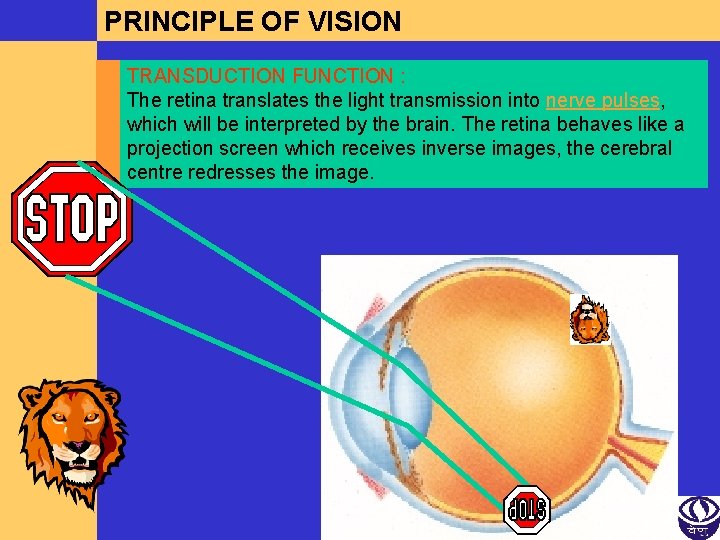
PRINCIPLE OF VISION TRANSDUCTION FUNCTION : The retina translates the light transmission into nerve pulses, which will be interpreted by the brain. The retina behaves like a projection screen which receives inverse images, the cerebral centre redresses the image.

Optical System of the Eye (60 D) • Cornea – 75% of refracting power (45 D) • Lens – 25% of refracting power (15 D)

Refractive Errors : “normal“ eye. • Emmetropia Axial length and refractive power of the eye fit together . • Ametropia eye requiring vision correction. Axial length and refractive power are not matching e. g. Myopia, Hyperopia, Astigmatism Source of picture : http: //www. e-sunbear. com/pp_page 2. html
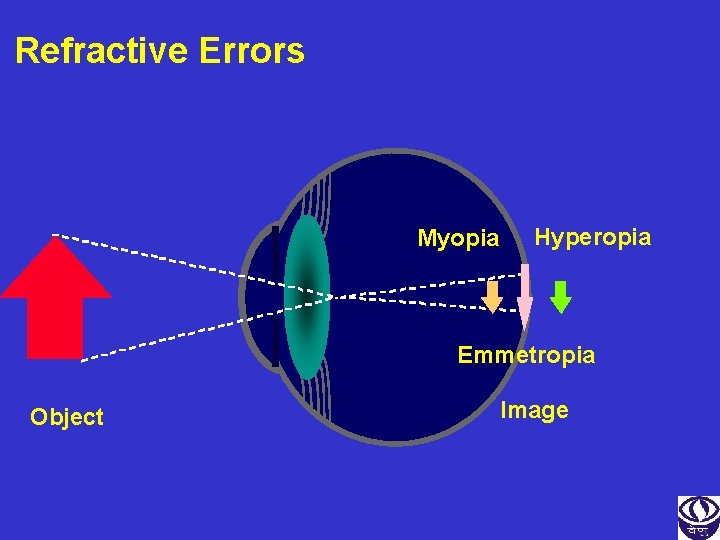
Refractive Errors Myopia Hyperopia Emmetropia Object Image
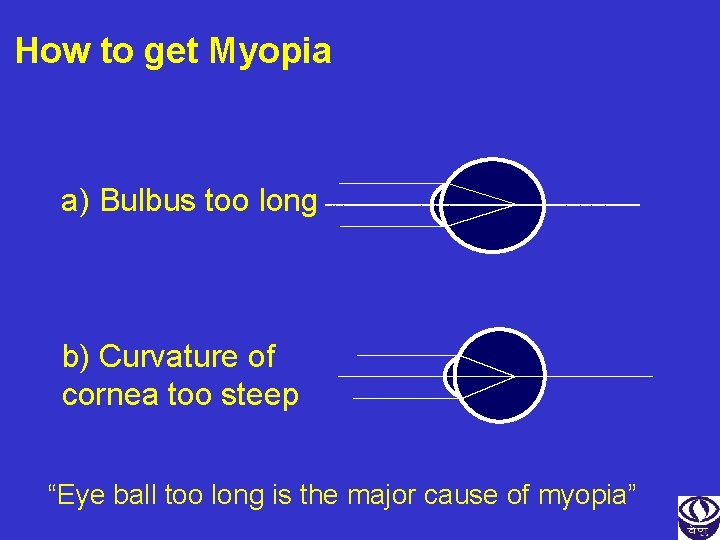
How to get Myopia a) Bulbus too long b) Curvature of cornea too steep “Eye ball too long is the major cause of myopia”
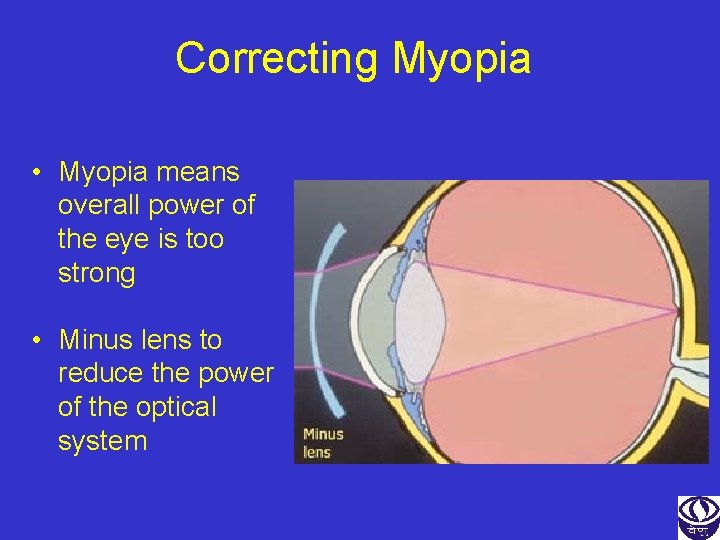
Correcting Myopia • Myopia means overall power of the eye is too strong • Minus lens to reduce the power of the optical system
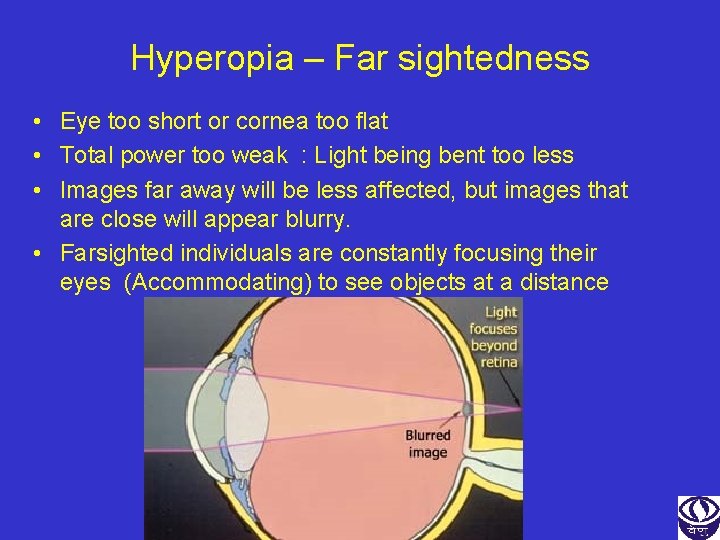
Hyperopia – Far sightedness • Eye too short or cornea too flat • Total power too weak : Light being bent too less • Images far away will be less affected, but images that are close will appear blurry. • Farsighted individuals are constantly focusing their eyes (Accommodating) to see objects at a distance
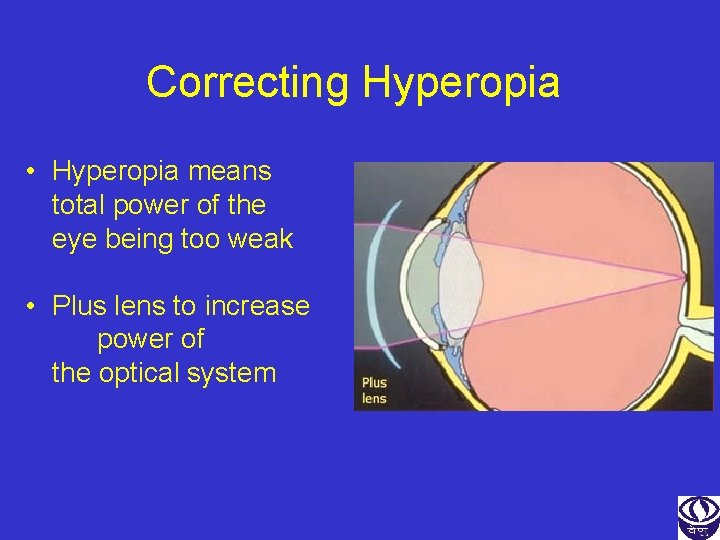
Correcting Hyperopia • Hyperopia means total power of the eye being too weak • Plus lens to increase power of the optical system

Focal Point – Plus Lens • Light passing through a convex lens will focus at one point called the focal point

Focal Point – Minus Lens • An imaginary or virtual focal point occurs in the front of a minus lens

Calculating the Power of a Lens • 1 Diopter = 1 Focal length of 1 meter • The focusing power of any lens in diopters can be calculated with the formula: D=1 f • D = power of lens • f = focal length in meters

Example #1 • If a lens has a focal length of 2 meters (f = 2 m), then: – Power = 1 / 2 m – Power = 0. 5 Example #2 • If lens has a focal length of 250 millimeters (f =. 25 m), then: – D = 1 / 0. 25 m – 4 D

Spherical Lenses (Sph) • Have the same curvature and same power in all directions • All light passing though a spherical lens will focus at the same point

Astigmatism • Cornea has non-spherical surface Spherical Toroidal
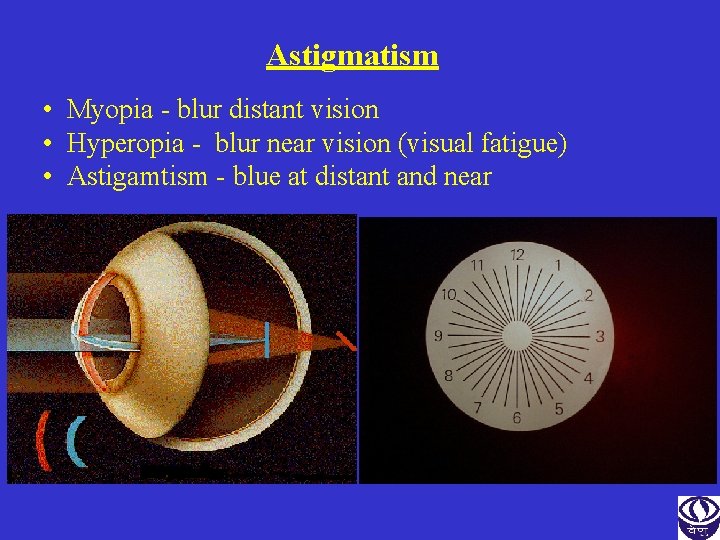
Astigmatism • Myopia - blur distant vision • Hyperopia - blur near vision (visual fatigue) • Astigamtism - blue at distant and near
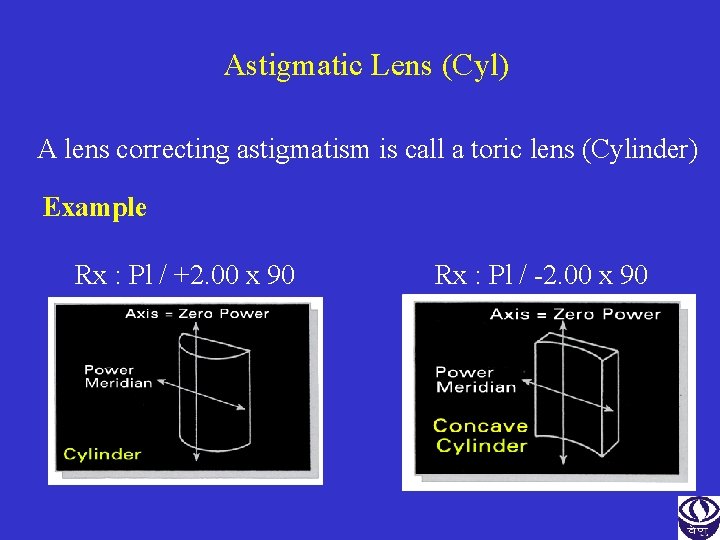
Astigmatic Lens (Cyl) A lens correcting astigmatism is call a toric lens (Cylinder) Example Rx : Pl / +2. 00 x 90 Rx : Pl / -2. 00 x 90
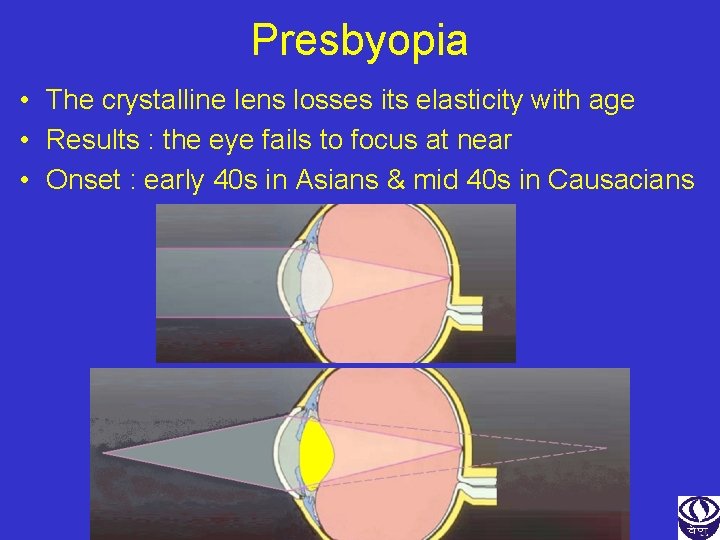
Presbyopia • The crystalline lens losses its elasticity with age • Results : the eye fails to focus at near • Onset : early 40 s in Asians & mid 40 s in Causacians
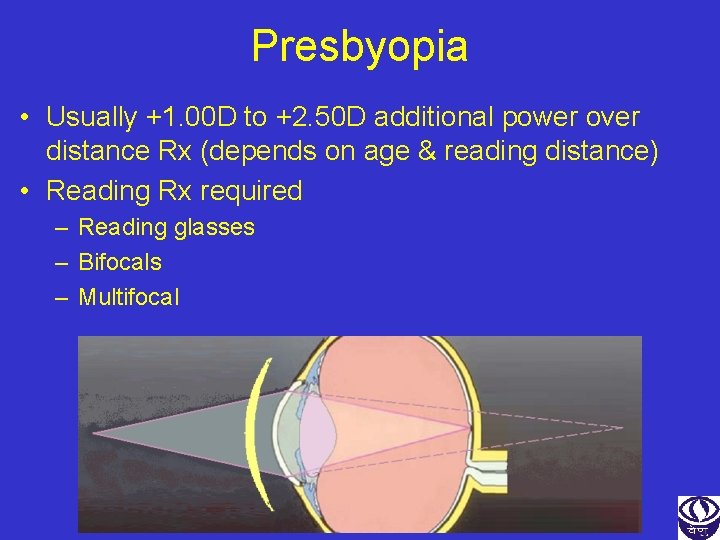
Presbyopia • Usually +1. 00 D to +2. 50 D additional power over distance Rx (depends on age & reading distance) • Reading Rx required – Reading glasses – Bifocals – Multifocal

Measuring Visual Acuity • Measured by Snellen chart • Measure of eye’s ability to resolve detail (resolution power)

Expressing Visual Acuity • Visual acuity is expressed as a fraction 20/20 or 6/6 or in decimal point (e. g. 0. 8 or 1. 0 etc) • 20/20 means patient can read the 20/20 line on chart at a distance of 20 feet • 6/6 means patient can read the 6/6 line at a distance of 6 meters

Visual Acuity • 6/18 = 20/60 = 0. 33 • Meaning the letter should be barely read at 18 m (60 ft) away is now read at 6 m (20 ft) away only • Vision is only 33% of a normal person • What does 6/4. 5 represents ?

Ocular structures • Part 1: Surrounding ocular structures • Part 2: Intra-ocular structures
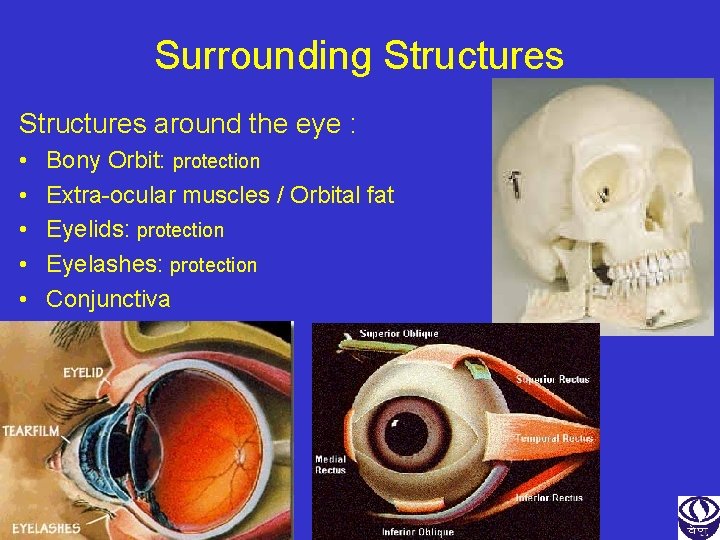
Surrounding Structures around the eye : • • • Bony Orbit: protection Extra-ocular muscles / Orbital fat Eyelids: protection Eyelashes: protection Conjunctiva
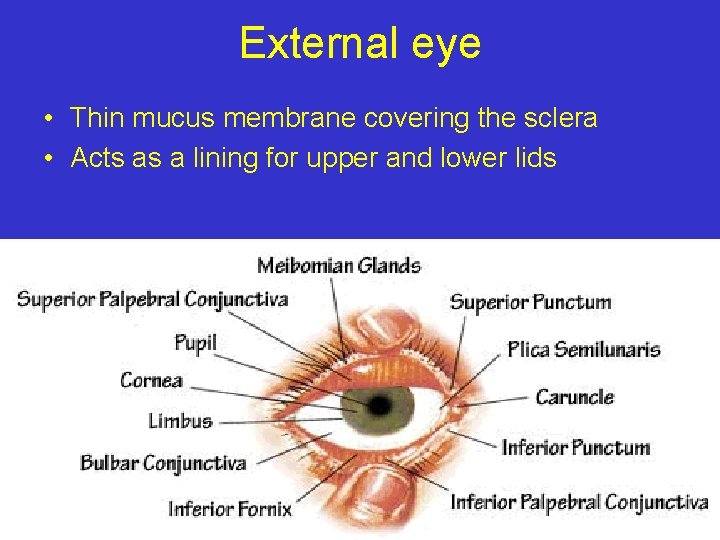
External eye • Thin mucus membrane covering the sclera • Acts as a lining for upper and lower lids
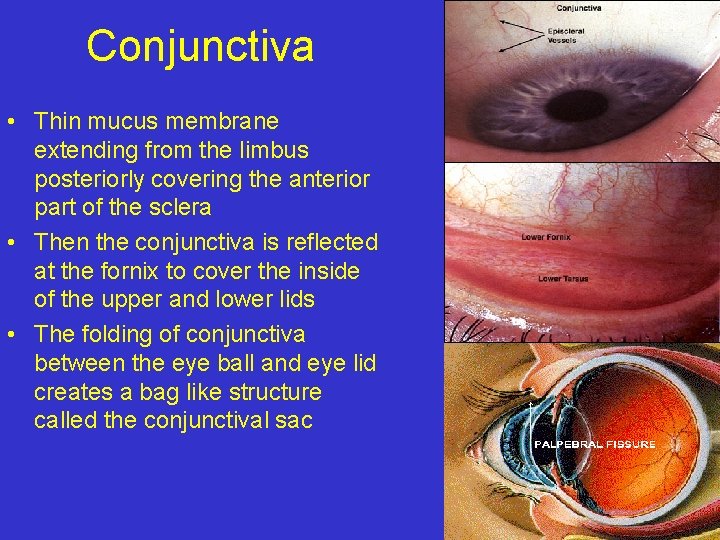
Conjunctiva • Thin mucus membrane extending from the limbus posteriorly covering the anterior part of the sclera • Then the conjunctiva is reflected at the fornix to cover the inside of the upper and lower lids • The folding of conjunctiva between the eye ball and eye lid creates a bag like structure called the conjunctival sac

Tearfilm • Produced by the tear & other glands • A layer of water, oils and nutrients that flow over the exposed surfaces of the eye • Approximately. 05 ml/1. 0 ml of tears are produced each day • Virtually no tears are produced during sleep
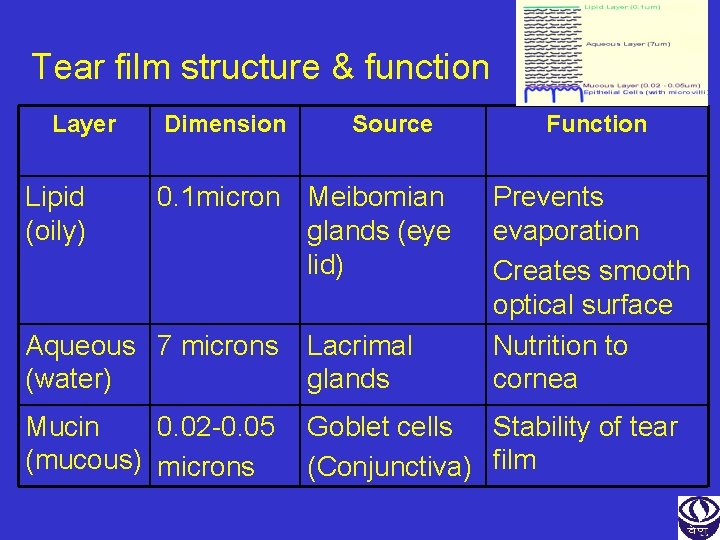
Tear film structure & function Layer Lipid (oily) Dimension Source 0. 1 micron Meibomian glands (eye lid) Function Prevents evaporation Creates smooth optical surface Nutrition to cornea Aqueous 7 microns (water) Lacrimal glands Mucin 0. 02 -0. 05 (mucous) microns Goblet cells Stability of tear (Conjunctiva) film
Part 2: The Eye
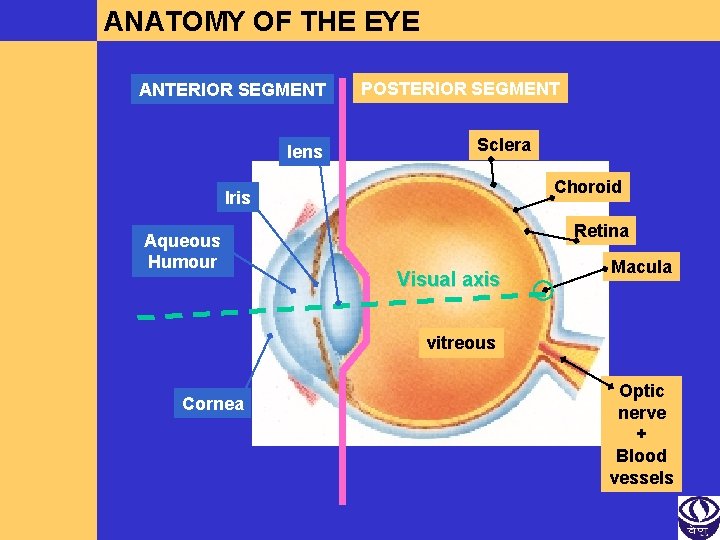
ANATOMY OF THE EYE ANTERIOR SEGMENT lens POSTERIOR SEGMENT Sclera Choroid Iris Aqueous Humour Retina Visual axis Macula vitreous Cornea Optic nerve + Blood vessels
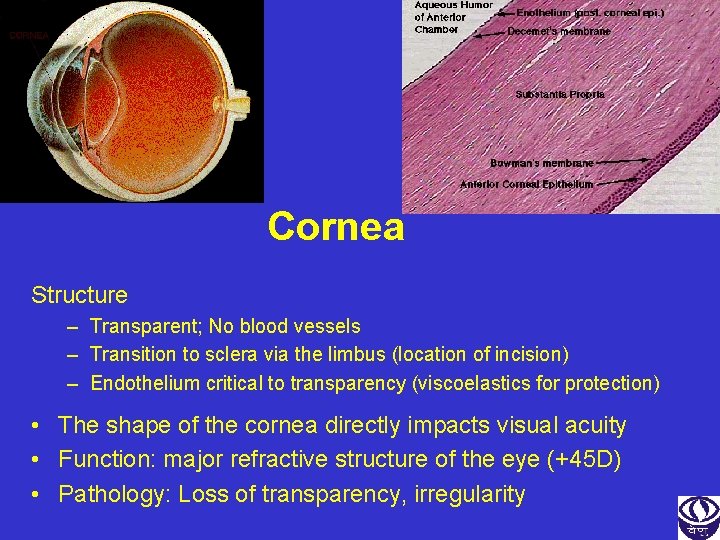
Cornea Structure – Transparent; No blood vessels – Transition to sclera via the limbus (location of incision) – Endothelium critical to transparency (viscoelastics for protection) • The shape of the cornea directly impacts visual acuity • Function: major refractive structure of the eye (+45 D) • Pathology: Loss of transparency, irregularity

Corneal structure 1. Epithelium 2. Bowman’s Membrane 3. Stroma 4. Descemet’s Membrane 5. Endothelium
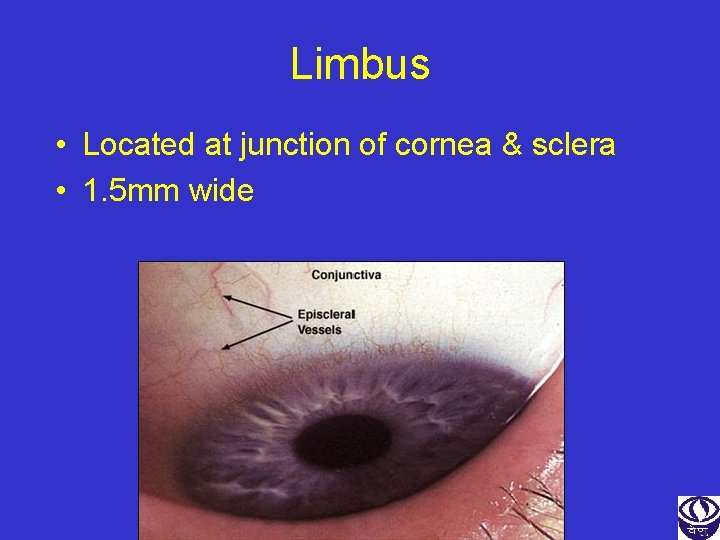
Limbus • Located at junction of cornea & sclera • 1. 5 mm wide

Sclera • “The White of the Eye” • Interwoven dense tissue – Tendons of extra-ocular muscles blend with it for insertion
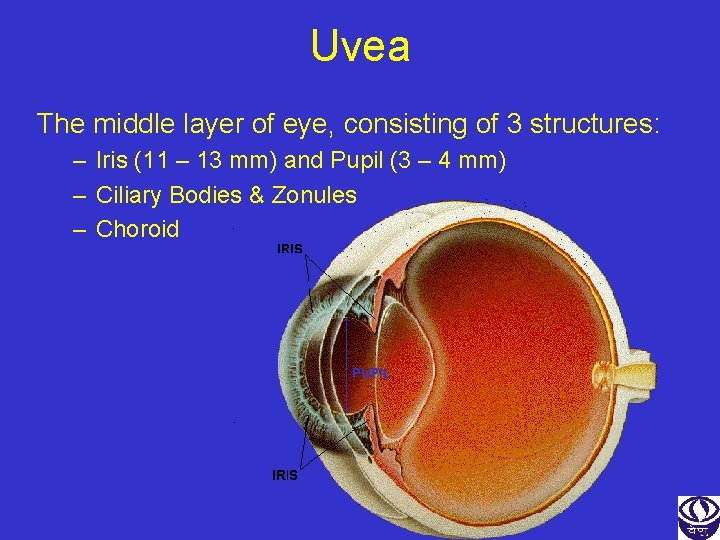
Uvea The middle layer of eye, consisting of 3 structures: – Iris (11 – 13 mm) and Pupil (3 – 4 mm) – Ciliary Bodies & Zonules – Choroid

Iris & pupil • Circular shaped diaphragm containing 2 sets of muscles to control the pupil size. (circular & radial muscles) • With pigment & non-pigmented cells. Many pigments = 'brown eyes'; some pigments = 'green eyes‘; very few pigments = 'blue eyes‘ • The pupil should be equally big & round and respond both to light & accommodation
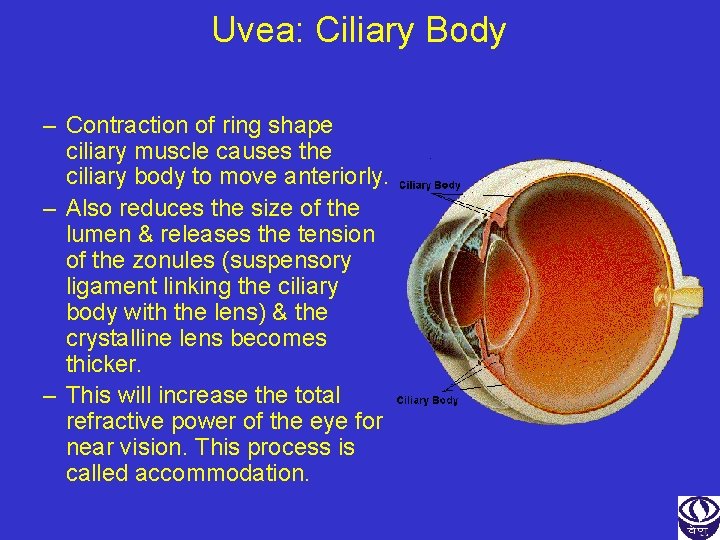
Uvea: Ciliary Body – Contraction of ring shape ciliary muscle causes the ciliary body to move anteriorly. – Also reduces the size of the lumen & releases the tension of the zonules (suspensory ligament linking the ciliary body with the lens) & the crystalline lens becomes thicker. – This will increase the total refractive power of the eye for near vision. This process is called accommodation.
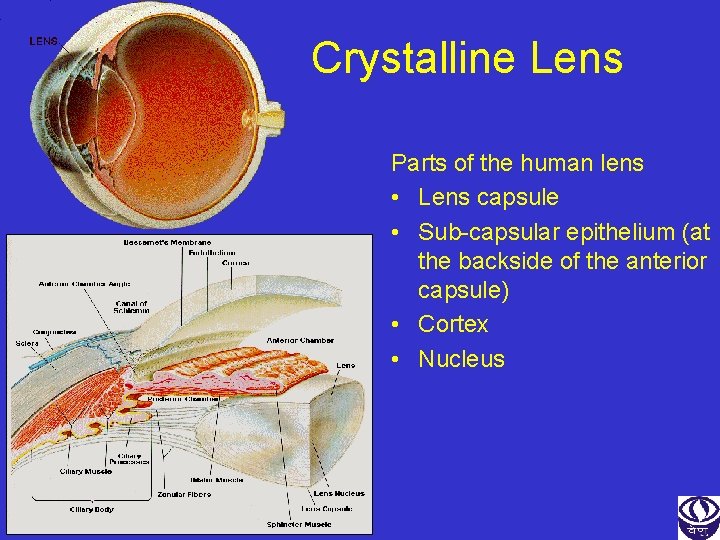
Crystalline Lens Parts of the human lens • Lens capsule • Sub-capsular epithelium (at the backside of the anterior capsule) • Cortex • Nucleus
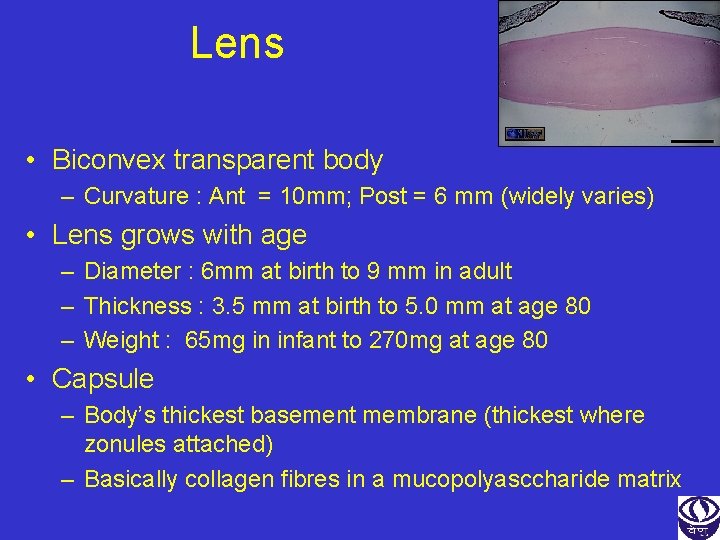
Lens • Biconvex transparent body – Curvature : Ant = 10 mm; Post = 6 mm (widely varies) • Lens grows with age – Diameter : 6 mm at birth to 9 mm in adult – Thickness : 3. 5 mm at birth to 5. 0 mm at age 80 – Weight : 65 mg in infant to 270 mg at age 80 • Capsule – Body’s thickest basement membrane (thickest where zonules attached) – Basically collagen fibres in a mucopolyasccharide matrix

Lens • Subcapular Lens epithelium – simple cuboidal in appearance, keep multiplying & elongates as they migrate from central region to the peripheral of the lens capsule. • Lens cortex – elongated columnar cells from epithelium (the lens is like an onion – with layers) – bulk of the substance of lens – As the newer cells (fibres) are formed, they will compress the older cell to the nucleus of the lens • Nucleus – Central hardened structure – Increases in size with age

Zonules • Zonules fibres pass from the basement membrane of the unpigemted ciliary epithelial cell to the lens capsule • Zonules fibres are 1 – 10 micron thick & are formed of collagen filaments about 20 nm in diameter • There are 2 major groups of zonular fibres (anterior & posterior capsular fibre sheets)

Aqueous humor • fills anterior chamber (0. 34 ml) – Composition not quite but similar to plasma (less protein, higher ascorbate, pyruvate, & lactate than plasma) – nourishes lens and other tissues • Produced by ciliary body • escapes at the corneo-scleral junction at the anterior angle of the eye (the angle between the iris and cornea) through the trabecular meshwork into the small blood vessels • Removal rate : 2 – 3 u. L / min
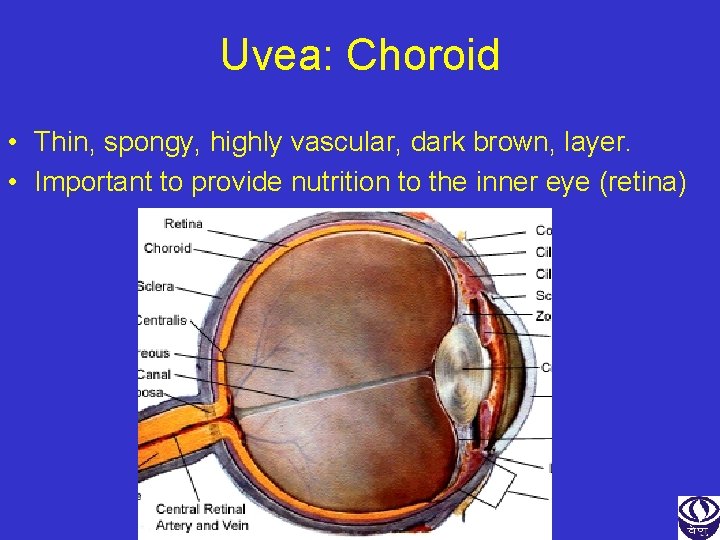
Uvea: Choroid • Thin, spongy, highly vascular, dark brown, layer. • Important to provide nutrition to the inner eye (retina)

Retina • Inner layer of eye containing the sensory receptors required for transmission of light • The retina can be divided into 10 layers & contains 120 millions photoreceptors & over 1 Million nerve fibres. It is a highly active structure and require a lot of nutrient supply – mainly from the choroid. • The retina has a average thickness of 200 um, 130 um in the centre of fovea to 550 um at the margin of the fovea. Total surface a • The retina is considered the extension of the brain.
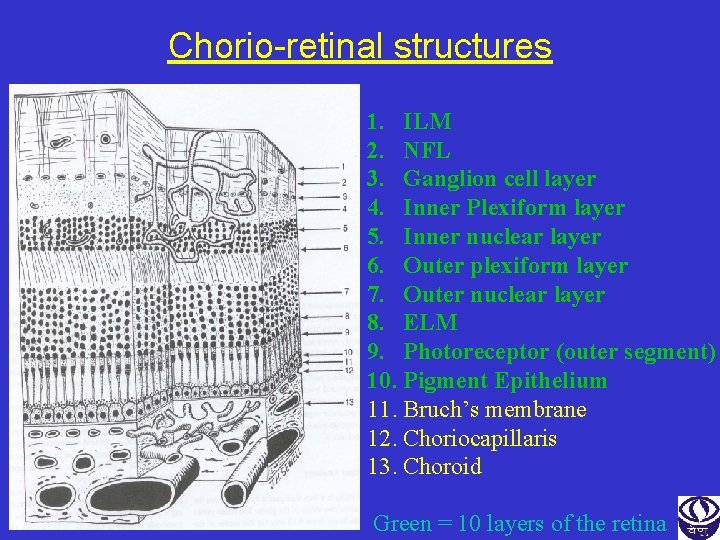
Chorio-retinal structures 1. ILM 2. NFL 3. Ganglion cell layer 4. Inner Plexiform layer 5. Inner nuclear layer 6. Outer plexiform layer 7. Outer nuclear layer 8. ELM 9. Photoreceptor (outer segment) 10. Pigment Epithelium 11. Bruch’s membrane 12. Choriocapillaris 13. Choroid Green = 10 layers of the retina
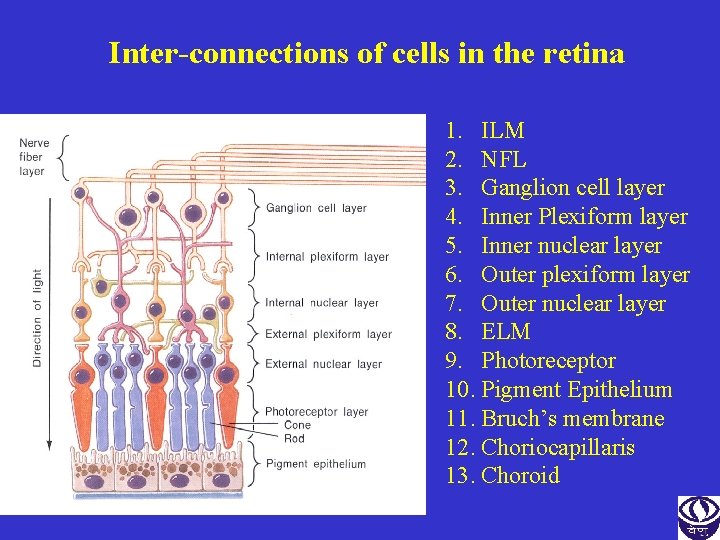
Inter-connections of cells in the retina 1. ILM 2. NFL 3. Ganglion cell layer 4. Inner Plexiform layer 5. Inner nuclear layer 6. Outer plexiform layer 7. Outer nuclear layer 8. ELM 9. Photoreceptor 10. Pigment Epithelium 11. Bruch’s membrane 12. Choriocapillaris 13. Choroid
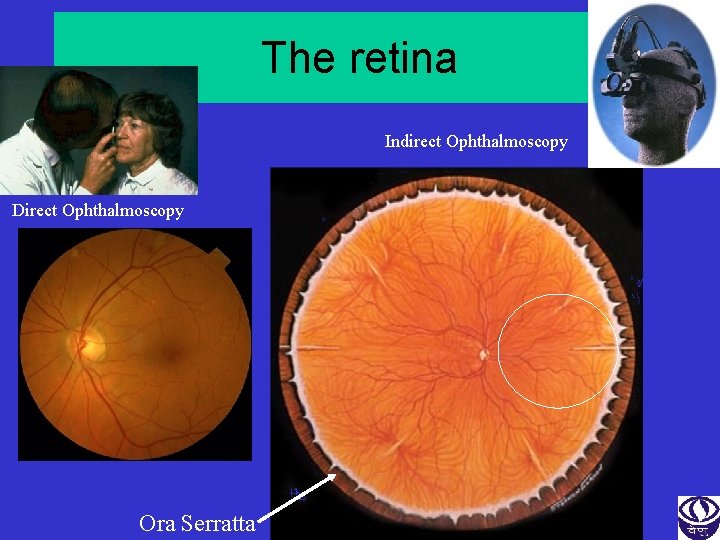
The retina Indirect Ophthalmoscopy Direct Ophthalmoscopy Ora Serratta

Examination of the retina Direct ophthalmoscopy • No pupil dilation • Magnified view • Can not exam the periphery of the retina • More use in examination of the macular & Optic nerve head Indirect ophthalmoscopy • Pupil dilation required • No / low magnification • Give a wider view of the retina (upto Ora Serrata) • Provide a stereoscopic (3 D) image • Use in thorough exam of the retina (retinal degeneration or detachment)

Retina • High myopia is highly associated with retinal degeneration • Elongation of eyeball stretches on the retina resulting in thinning of the retina especially in the midperipheral area resulting in choroidal & retinal degeneration • Thinning and degenerative retina may develop into retinal holes / tears which allows liquid in the vitreous to enter the sub-retinal space and resulting in retinal detachment • High myopic patients should have an annual dilated retinal examination by a Eye Care Practitioner using an indirect ophthalmoscope
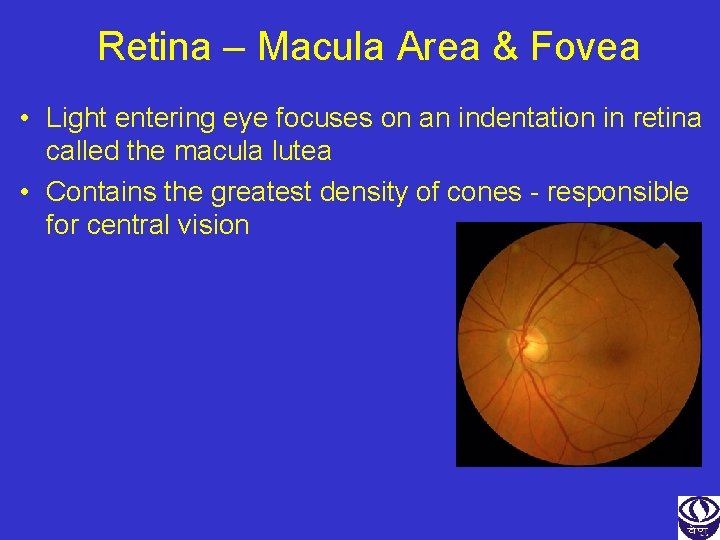
Retina – Macula Area & Fovea • Light entering eye focuses on an indentation in retina called the macula lutea • Contains the greatest density of cones - responsible for central vision
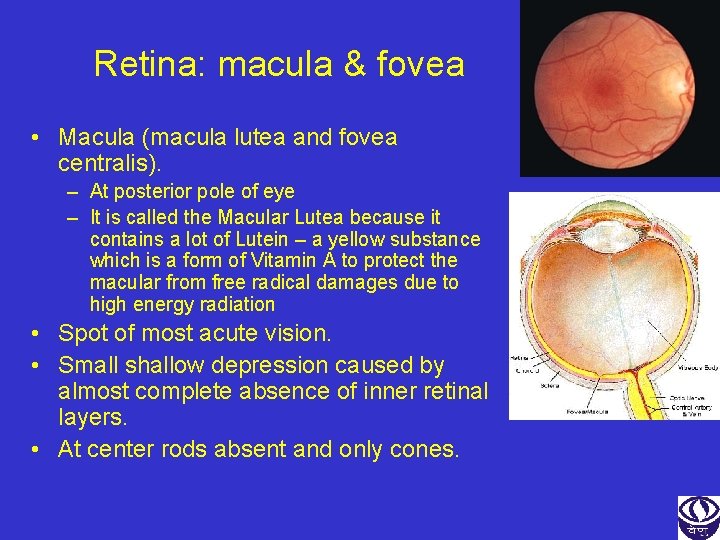
Retina: macula & fovea • Macula (macula lutea and fovea centralis). – At posterior pole of eye – It is called the Macular Lutea because it contains a lot of Lutein – a yellow substance which is a form of Vitamin A to protect the macular from free radical damages due to high energy radiation • Spot of most acute vision. • Small shallow depression caused by almost complete absence of inner retinal layers. • At center rods absent and only cones.
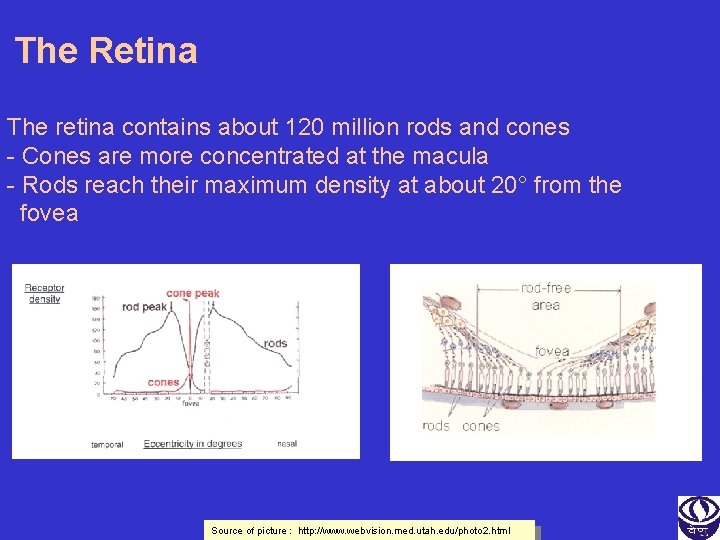
The Retina The retina contains about 120 million rods and cones - Cones are more concentrated at the macula - Rods reach their maximum density at about 20° from the fovea Source of picture : http: //www. webvision. med. utah. edu/photo 2. html
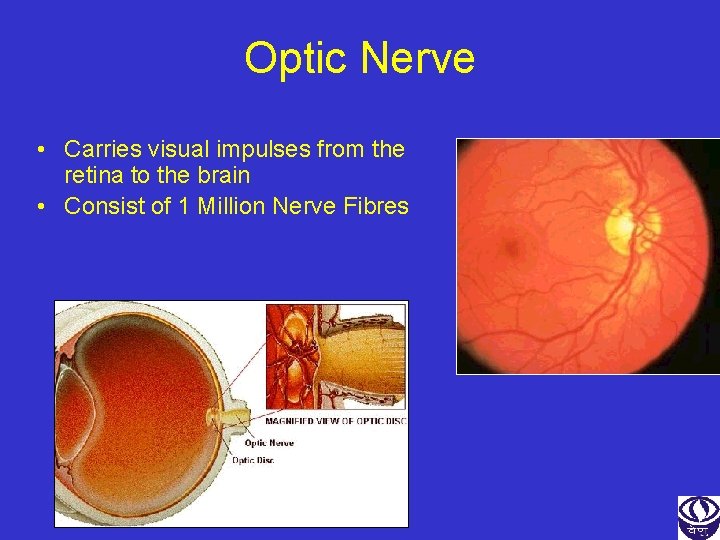
Optic Nerve • Carries visual impulses from the retina to the brain • Consist of 1 Million Nerve Fibres

Right Optic track Left Optic Nerve Optic Chiasma Image on the L side of the visual field (red) is focused on the R side of the retina in both eyes (red). All the nerve fibre in the nasal retina of the L eye (carrying the signal from the L visual field) cross over to join the temporal retina fibre of the R eye (also carrying signal of the L visual field). Then they travel together to the R visual cortex via the R Optic track (Left visual field is interpreted by the R side of the brain). Similarly, image on the R visual field will be sent to the L side of the brain.
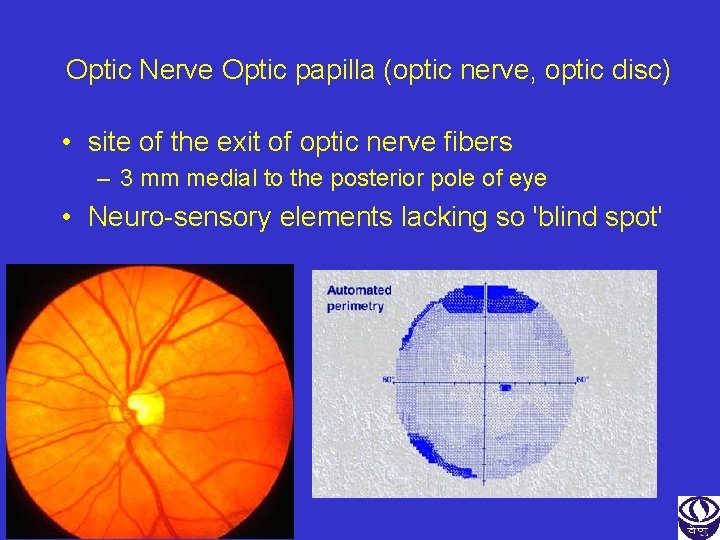
Optic Nerve Optic papilla (optic nerve, optic disc) • site of the exit of optic nerve fibers – 3 mm medial to the posterior pole of eye • Neuro-sensory elements lacking so 'blind spot'
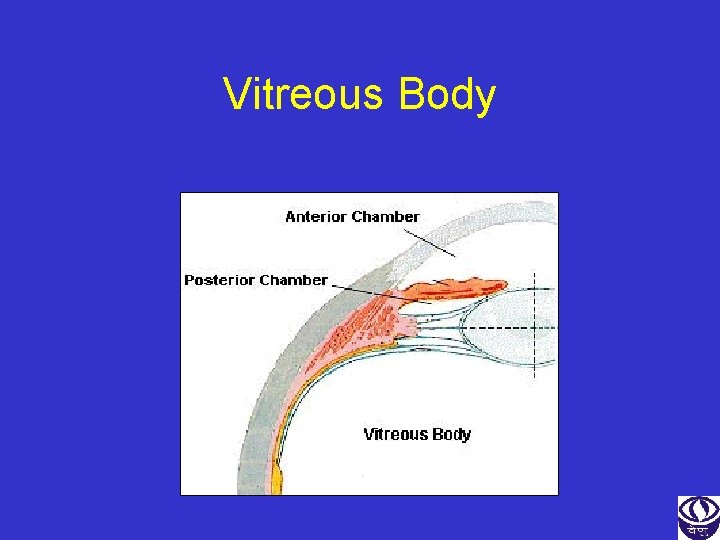
Vitreous Body

Vitreous Body • Fills the posterior chamber (4 ml) • Give support & shape to the eye ball • Composition – Colorless near structure-less, gelatinous mass – 99% water in a very fine network of collagen fibers • The vitreous fibre condensed on the surface forming a 100 um thick cortical vitreous • Degeneration of the vitreous can result in floaters (patient seeing black dots or thread like shadows floating around) or even traction to the retina • Vitrectomy is a surgical procedure to remove the problematic vitreous

Common Terminology related to anatomy • Superior/inferior, temporal/nasal, lateral/medial Anterior/posterior • Clock hours reference • OS: left eye: LE ; OD: right eye: RE; OU: both eyes • Unilateral / Bilateral • Extra-ocular, intra-ocular, retro-ocular

End For Further Queries Contact : Ms. Priyanka Singh Head – Optometry Service Email – optometry@venueyeinstitute. org
- Slides: 60