Basic Positions Supine Lithotomy Sitting Prone Lateral Complications

� Basic Positions: �Supine �Lithotomy �Sitting �Prone �Lateral

� Complications: �Joint dislocation �Postoperative musculoskeletal pain �Integumentary System Skin breakdown Necrosis �Peripheral nerve damage �Cardiovascular compromise �Respiratory compromise �Neuromuscular injury

� General anesthesia & Regional blocks prevents normal defense of pain from stretching, twisting and compression � Subsequent nerve and vascular structures are compromised � Extreme/Unnatural positions: lungs become engorged with blood, decreasing alveolar expansion, reducing oxygenated blood

� Respiratory �Unfavorable Compromise: positions reducing ability of thoracic cage to expand �Gas exchange reduced (hypoventilation, hypoxia, hypercarbia) �Lung expansion reduced from restriction of ribs or sternum �Diaphragm’s reduced ability to push against abdominal contents or from retractor use �Anesthetics cause vasodilatation, constriction, resulting in hypotension

� Cardiovascular �Ability compromise: of heart to contract reduced due to positioning and anesthetic agents �Decreased cardiac output �Positioning or pressure obstructing flow to legs results in potential for phlebothrombosis �Venous thrombosis resulting from pressure, straps, and position

� Neuromuscular Compromise: � Awake patient: pain and pressure are indicators � Anesthetized patient: unable to indicate pain, exaggerated ROM; exacerbates injury for neuromuscular compromise � Hyperextension injury can result from mild pain postoperatively to joint dislocation � Extremities should never be allowed to “hang” over the edge of OR table � Crushing and pressure injuries to fingers, toes, ears, nose are prevented by surgical team members visualizing involved body parts when positioning or re-positioning � Surgical team members should NEVER LEAN on patient

� Brachial �More Plexus Injury: common positioning injury �Results in improper positioning of arm/armboard (hyperextension or hyperabduction) �Never extend arm more than 90 degrees �Turn head toward extended arm, palm supinated to minimize pressure on brachial plexus

� Brachial Plexus Injury �Shoulder braces �Radial/Ulnar nerve damage Injured if elbow slips off mattress to OR table Compression of arm by OR team leaning on patient or draw sheet tucked in to tight Elbow not padded Malfunctioning automatic blood pressure cuff
� Integumentary Injuries: �Friction �Shearing �Pressure �May be superficial Microsoft clipart

� Friction: usually superficial, result in abrasion or blisters � Shearing: �Skin remains stationary while tissue is under is shifted �Can happen if blankets or linens are PULLED out from patient rather than lifted �Can happen if anesthetized patient is repositioned or slides down when OR table is re-adjusted �Can lead to development of pressure ulcer

� Pressure: �Occur mostly over boney prominences �Anesthetized patient immobile during procedure �Hypoxia of tissue leads to necrosis �Surgeries lasting from 2. 5 – 4 hours double the risk of skin changes and have 5 times the risk of pressure ulcer formations (Spry- pg 135)

� Pressure: �Ulcers can go unnoticed for hours or days, as skin is not visible immediately post-op �OR pressure ulcers typically appear as a bruise and progress to a pressure ulcer �Damage typically occurs deep and progresses outward �Areas at most risk are: Heels Elbows Scapula Sacrum Coccyx
� Prevention �Adequate �Relief of Ulcer Formation: padding (foam, gel pads, pillows) of pressure after 2 hours ©Steris, Used by permission

� Headrest � Padded Armboards � Shoulder Braces � Kidney Brace � Table Strap � Leg stirrups � Table extensions � Table attachment holders All pictures © Steris, Used by permission

� Height and Weight � Nutritional Status � Existing integumentary damage � Pre-existing injuries � Pre-existing conditions � Surgical Procedures �Lasting longer than 2 hours �Vascular Surgery �Prolonged traction

� Communication with Surgical Team � Procedure, Assessment, Data, Nursing Diagnosis serve as a basis for plan of care � Selection of appropriate positioning devices � Number of personnel needed to implement appropriate positioning
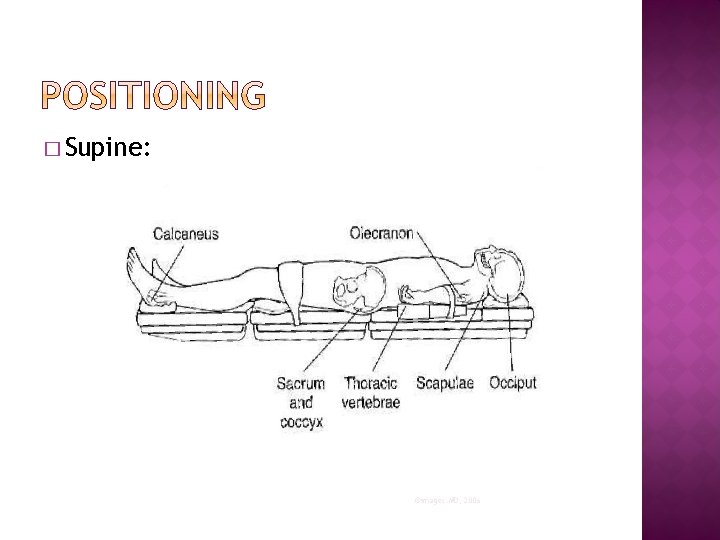
� Supine: ©images. MD, 2006

� Supine �Most common �Procedures include: abdominal, ENT, extremity, minimally invasive �Arms should be placed on armboards, palms up. Elbows must not be flexed or extend beyond the mattress. Pad elbow. �Arm secured with draw sheet �Table strap (safety strap) should be applied loosely over waist or mid-thighs. (At least 2” above the knees - prevent hyperextension) �Pad pressure points if surgery is anticipated to extend beyond 2 hours

� Supine Potential Pressure Points: �Occiput �Scapulae �Thoracic Vertebrae �Olecranon (elbow) �Sacrum and Coccyx �Calcaneus (heels)
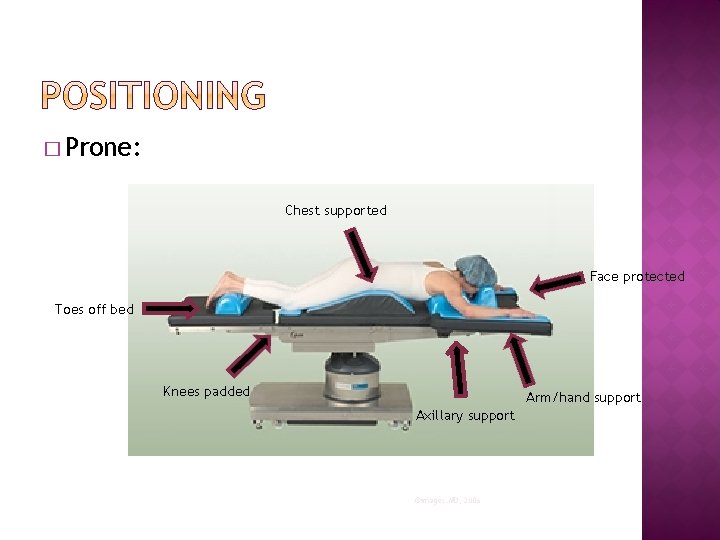
� Prone: Chest supported Face protected Toes off bed Knees padded Arm/hand support Axillary support ©images. MD, 2006

� Prone position: �Positioned on abdomen �Used for spine, back, rectum and posterior aspects of extremity surgical procedures �Initially positioned supine, following induction, anesthesia will secure ET tube and indicate readiness to place in prone position �Minimum of four persons is necessary to place in prone position �All equipment must be readily available

� Prone position (con’t) �Movement of patient is done slowly and gently �Anesthesia supports head, neck and protects airway �Once patient is turned: arms are brought down or forward (hands pronated, elbows padded) patients head turned to one side and supported Chest supported by rolls or special frames Pillow placed under ankles Place table strap/safety over the mid-thighs Small donut pads, placed under knees (protects patellas) Check soma if applicable- and pad as needed Check breasts (women) and genitalia (men) making sure no pressure exists

� Prone Pressure Points: �Cheek and Ear �Acromion Process �Breasts (women) �Genitalia (men) �Patella �Toes
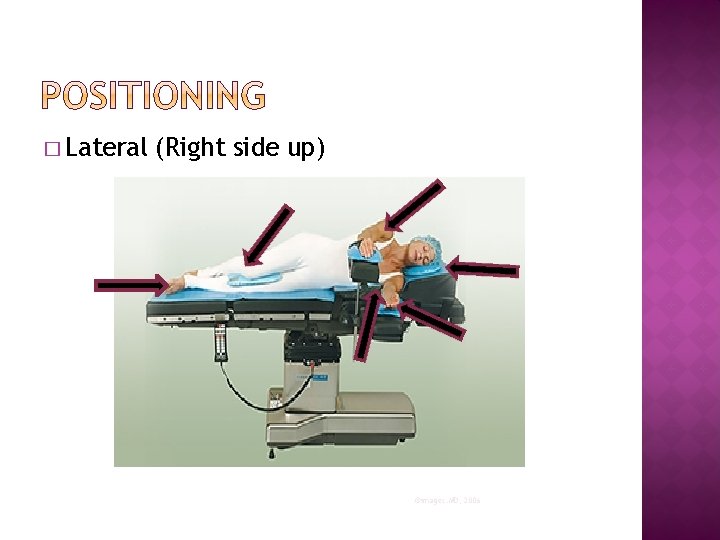
� Lateral (Right side up) ©images. MD, 2006
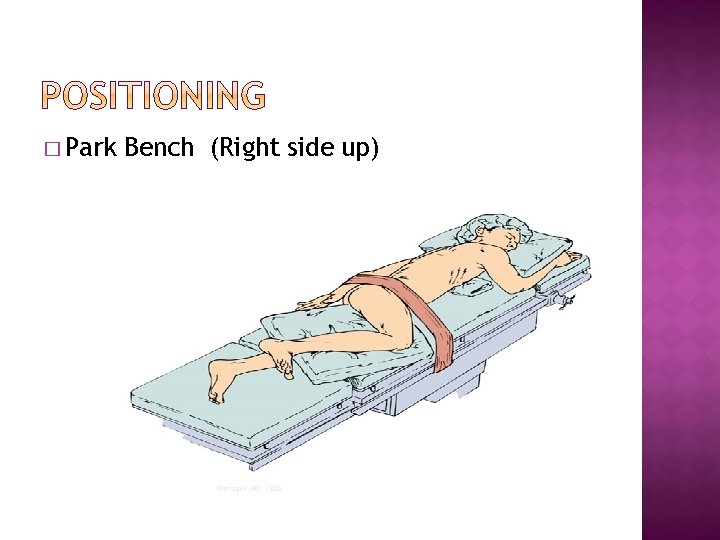
� Park Bench (Right side up) ©images. MD, 2006

� Lateral: �Patient lies on one side �Used for thorax, kidney, retroperitoneal space and hip surgical procedures �Initially place supine, until anesthetized, then lifted into place onto non-operative side �Place small roll or padding under patient’s lower axilla- relieves pressure on chest and axilla, allows for chest expansion and prevents brachial plexus �Kidney procedures: the kidney rest (in the middle of OR table) is elevated to provide exposure �Pay particular attention to eyes and ears as they are both at risk for damage

� Potential Pressure Points for Lateral and Park Bench position �Ear �Acromion process �Ribs �Ilium �Greater Trochanter �Medical and Lateral Condyles �Malleolus

� Sitting ©images. MD, 2006

� Sitting: �Used for cranial procedures �Initially positioned in supine position �Torso and shoulders supported by loose safety strap �Flex arms at elbows, rest on pillow �Pad pressure points �Anti-embolism or SCD hose should be placed on patient �Because of negative venous pressure in head and neck, sitting position patient are at risk for air embolism. CVP with doppler ultrasound is used to monitor the patient in this position to detect air

� Potential Pressure Points for Sitting Position: �Scapulae �Ischial Tuberosities �Back of Knee �Calcaneus (heels)
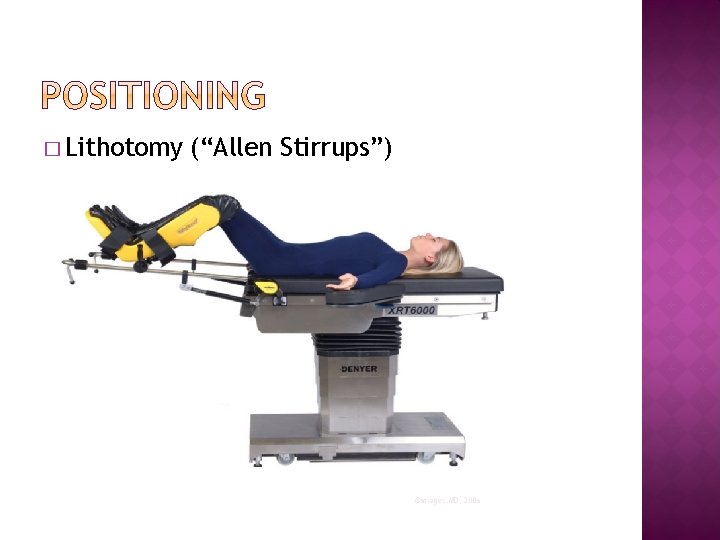
� Lithotomy (“Allen Stirrups”) ©images. MD, 2006
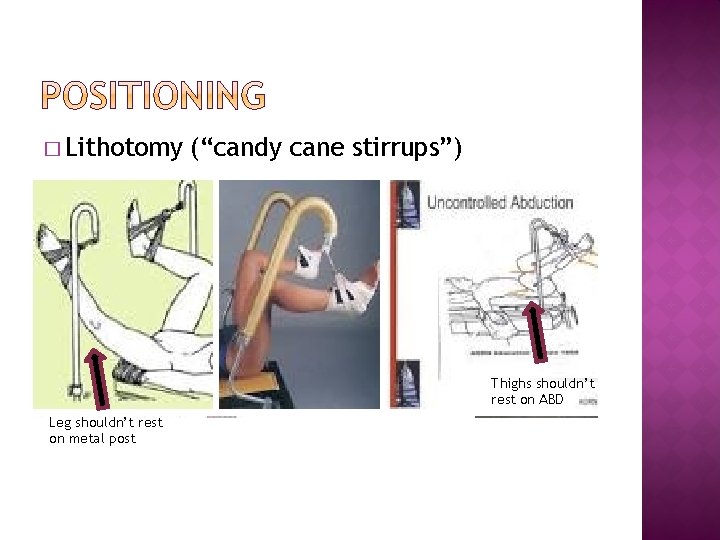
� Lithotomy (“candy cane stirrups”) Thighs shouldn’t rest on ABD Leg shouldn’t rest on metal post

� Lithotomy �Extreme modification of supine position- legs elevated, abducted and supported by stirrups �Used for procedures involving rectum, perineum, pelvic organs and genitalia �Secure arms on arm boards to prevent injury to fingers �Secure stirrups to table and position at equal height �Padding on portions of stirrups that contact legs is used to prevent external compression of nerves

� Lithotomy Potential Pressure Points: �Occiput �Scapulae �Olecranon (elbows) �Peroneal nerve �Posterior tibial nerve �Femoral obturator nerve �Sciatic nerves
� Lithotomy Peroneal Nerve: �On lateral aspect of knee �Injury can occur if nerve is compressed between the fibula and laterally on stirrup bar (injury results in foot drop) �Injury to posterior tibial nerve, damage will result in numbness of foot �Injury to sciatic nerve, can result in foot drop
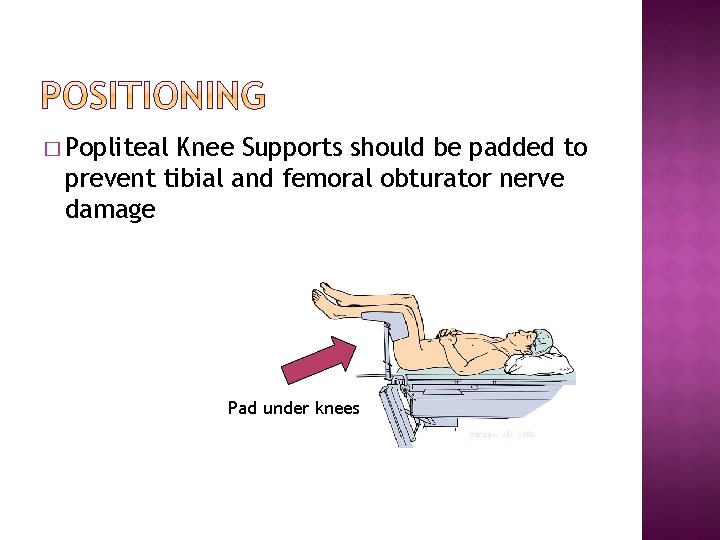
� Popliteal Knee Supports should be padded to prevent tibial and femoral obturator nerve damage Pad under knees ©images. MD, 2006
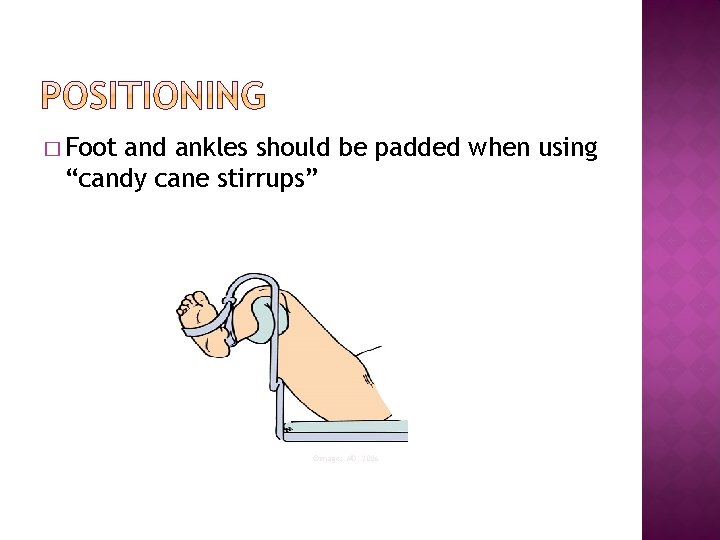
� Foot and ankles should be padded when using “candy cane stirrups” ©images. MD, 2006

� Improper placement of stirrups or improper movement of legs can result in: �Flexion �Compression �Stretching ALL causing damage to the lower extremity nerves

� During leg elevation, hold the foot with one hand, the lower part of the leg with the other. Legs are flexed SLOWLY & SIMULTANEOUSLY into the padded secured stirrup � Following the procedure, remove legs from stirrups (by two staff members) SIMULTANEOUSLY, extend fully to prevent abduction of hips and SLOWLY lowered to OR table

� Reduces respiratory efficiency due to pressure on thighs from abdomen, diaphragm, abdominal viscera restricting thoracic expansion � Vital capacity and tidal volume are decreased when lung tissue becomes engorged with blood

� Patient should be positioned supine with buttocks EVEN with the lower break of OR table � Stirrups pre-operatively should be attached to the table at equal height and adjusted to length of patient’s legs (once patient is in position on table adjust)

� Nursing �ROM Assessment: (range of motion) of hips Contractures ? Arthritis ? Prosthesis ? Other condition ? Communicate findings to Surgical Team (don’t forget Post-Operatively too!)

� Recommended Practice I: “Preoperative Assessment for positioning needs should be made before transferring the patient to the procedure bed. ” � Recommended Practice II: “Positioning devices should be readily available, clean and in proper working order before placing the patient on the procedure bed

� Recommended Practice III: “The perioperative nurse should actively participate in monitoring patient body alignment and tissue integrity based on sound physiologic principles. ” � Recommended Practice IV: “After positioning, the perioperative nurse should evaluate the patient’s body alignment and tissue integrity. ”

� ü ü Recommended Practice V: “Documentation of surgical positioning should be consistent with AORN’s “Recommended practices for documentation of perioperative nursing care. ” -”Documentation should include but not be limited to: Perioperative assessment Type and location of positioning and or padding devices Names and titles of persons positioning the patient Postoperative outcome evaluation”
- Slides: 45