Basic Human Needs Oxygenation VentilationPerfusion Basic Needs Oxygenation

Basic Human Needs Oxygenation Ventilation/Perfusion
Basic Needs: Oxygenation

Oxygenation l l l Oxygen is required to sustain life, primary basic human need The cardiac & respiratory systems function to supply the body’s oxygen demands Cardiopulmonary physiology involves delivery of deoxygenated blood to the right side of the heart & to the pulmonary system
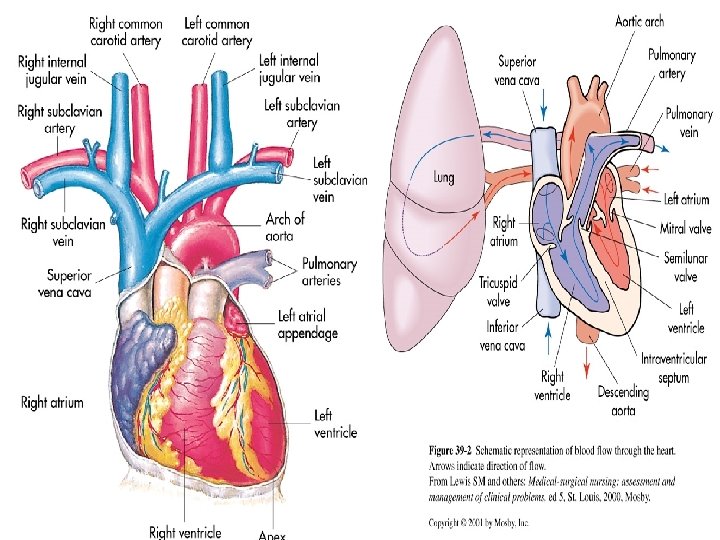
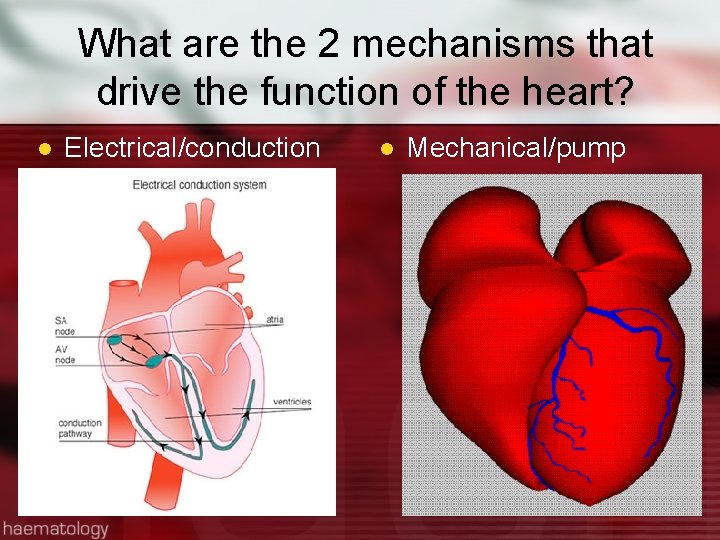
What are the 2 mechanisms that drive the function of the heart? l Electrical/conduction l Mechanical/pump

Myocardial Pumping action of heart is essential to maintenance of oxygen delivery l Decreased effectiveness of pumping action is a result of disease ( MI, CHF, Cardiomyopathy) l Results in diminished pumping action (stroke volume)

Myocardial Pump l Chambers of the heart fill during diastole & empty during systole l Myocardial fibers have contractile properties that enable them to stretch during filling l In healthy heart the stretch is proportionally related to the strength of contraction l Frank-Starling Law of the Heart

Myocardial Blood Flow l Unidirectional l 4 Heart valves ensure forward flow l Atrioventricular (mitral & tricuspid) l Open during ventricular filling (diastole), blood flows from atria into ventricles

Myocardial Blood Flow Review Semilunar valves (aortic & pulmonic) l Open during systolic phase l Closure of atrioventricular valves & closure of semilunar valves constitute normal heart sounds l “Lub” or S 1=Closing of atrioventricular valves just before the contraction of the ventricles (systole) l “Dub” or S 2=Closing of Semilunar valves after the ventricles have emptied and heart enters the filling phase (diastole) l
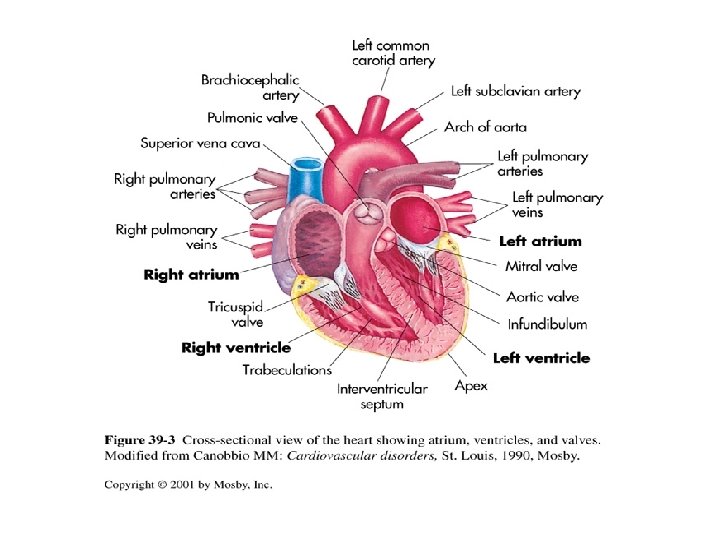

Coronary Artery Circulation l Right Coronary Artery l Left Coronary Artery l Circumflex
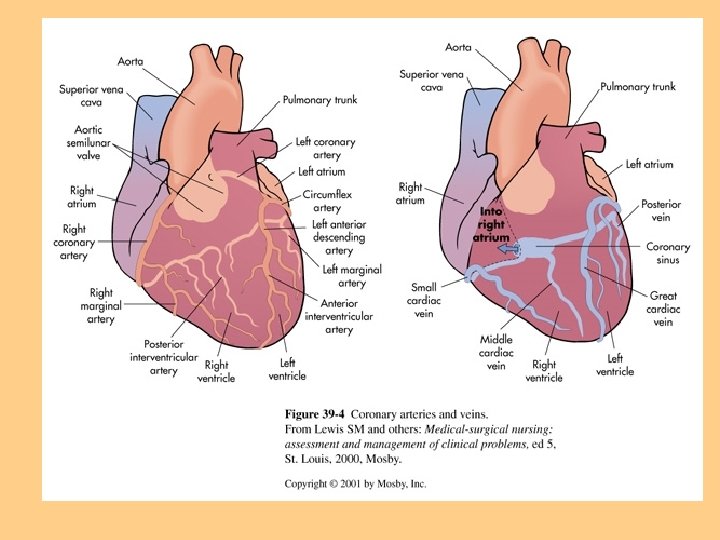
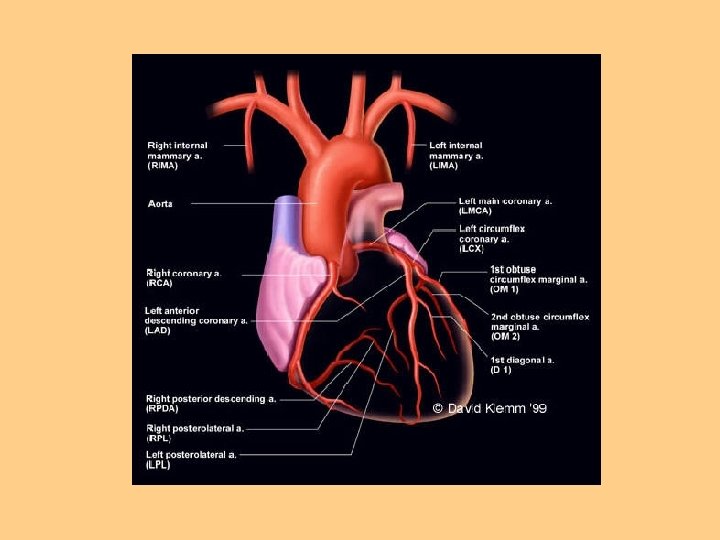

Systemic Circulation l LV to aorta to arteries to arterioles to capillaries l Oxygen exchange occurs at the capillary level l Waste product exchange occurs here also and exits via venous system back to lungs
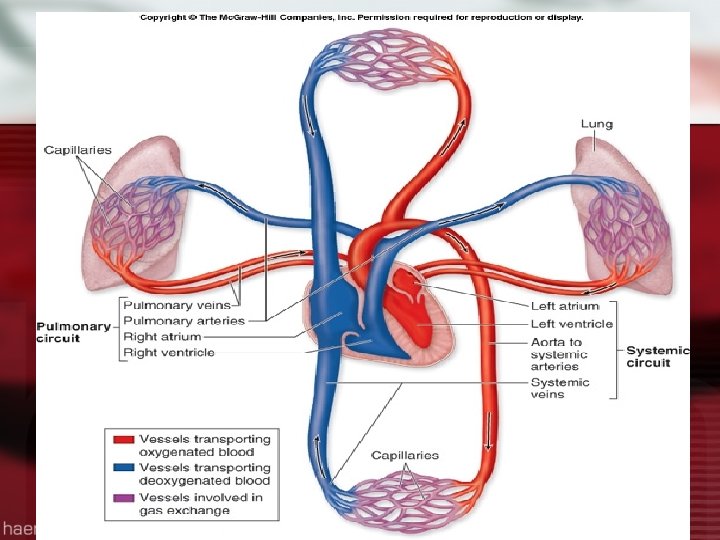

Blood Flow Regulation l Cardiac Output l Cardiac Index l Stroke Volume
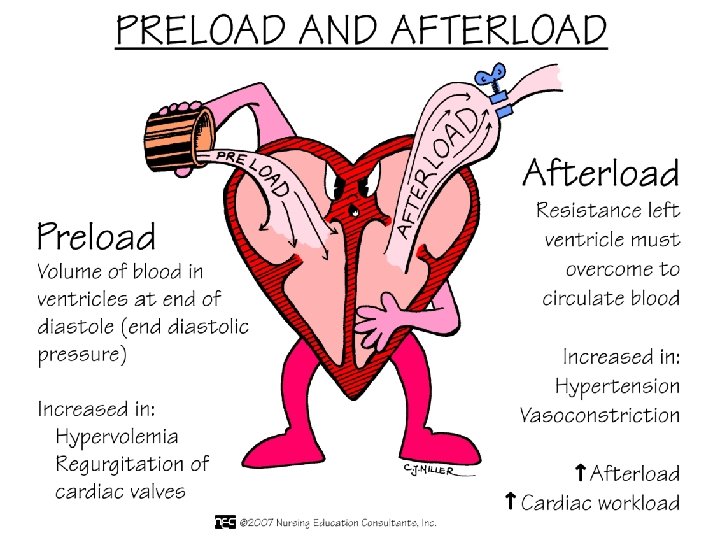
Stroke Volume l Preload l Myocardial Contractility l Afterload

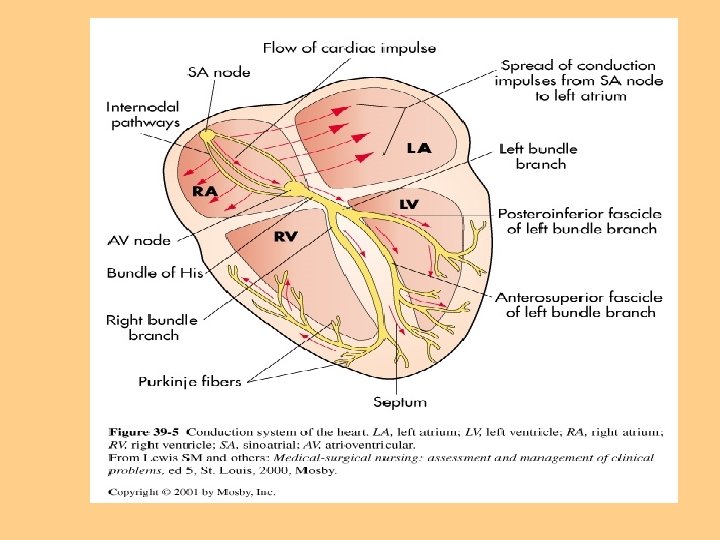
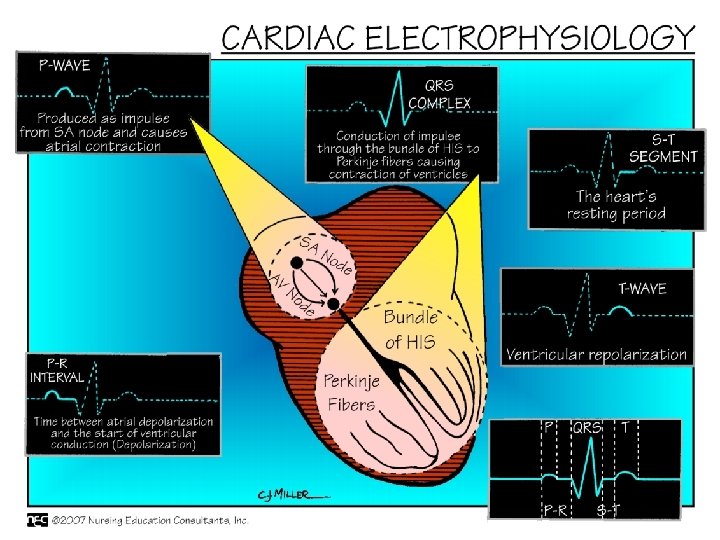
Conduction System l Rhythmic relaxation & contraction of atria & ventricles l Dependent on continuous transmission of electrical impulses l Influenced by ANS (Sympathetic & parasympathetic)

Conduction System l Originates in the sinoatrial node (SA node) l Intrinsic rate of 60 -100 beats per minute l Electrical impulses transmitted through atria along intra-nodal pathways to AV node

Conduction System l AV node mediates impulses between atria & ventricles l Intrinsic rate 40 -60 beats per minute l AV node assists atrial emptying by delaying the impulses before transmitting it through to the Bundle of His & Perkinje fibers

Conduction System l Intrinsic rate of Purkinje fibers 20 -40 beats per minute l EKG reflects the electrical activity of conduction system l Normal Sinus Rhythm l Physiology of NSR
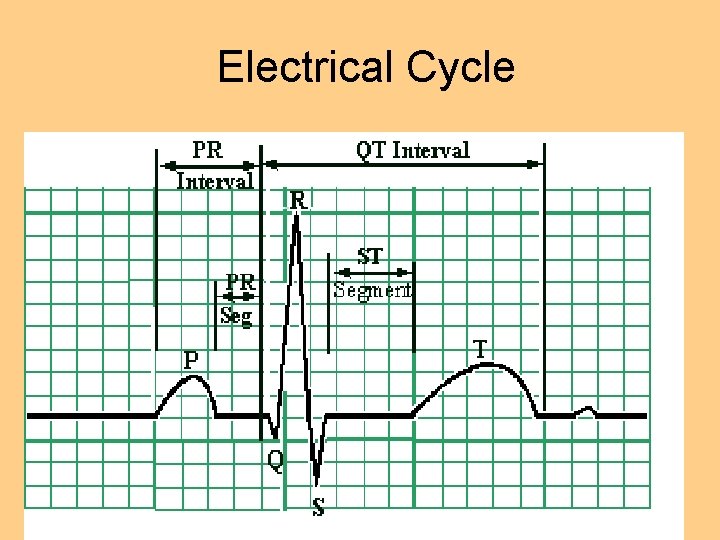
Electrical Cycle
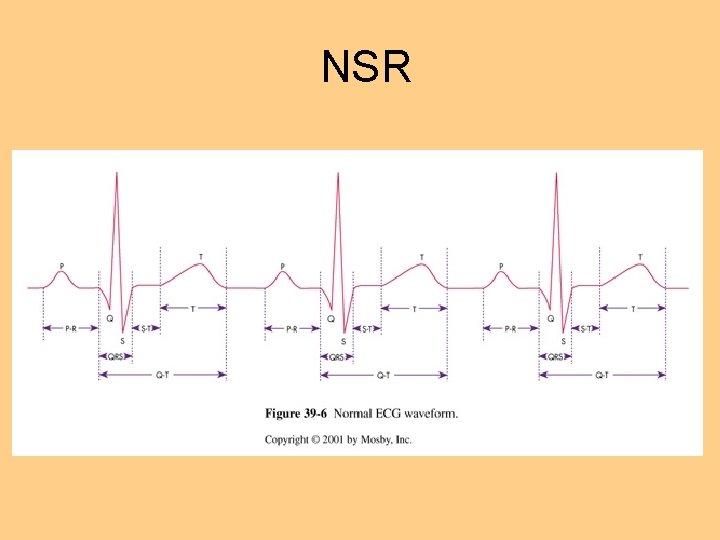
NSR
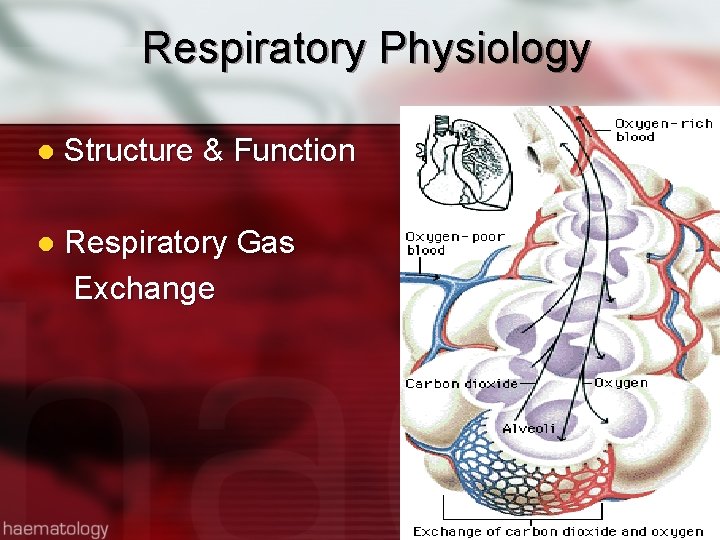
Respiratory Physiology l Structure & Function l Respiratory Gas Exchange

Structure & Function l Ventilation-Process of moving gases into and out of the lung l Requires coordination of the muscular & elastic properties of lungs & thorax as well as intact innervation l Diaphragm-Major muscle of inspiration, innervated by phrenic nerve (3 rd cervical vertebrae)
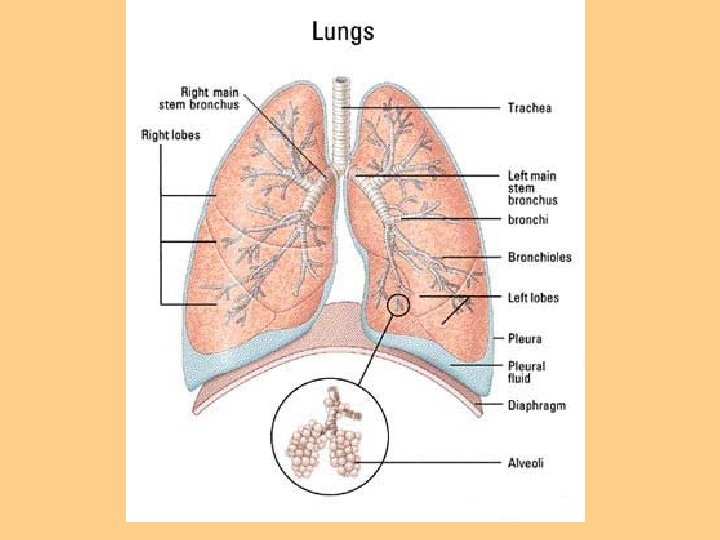

Structure & Function Work of Breathing l Degree of compliance of lungs l Airway resistance l Presence of active expiration l Use of accessory muscles of respiration
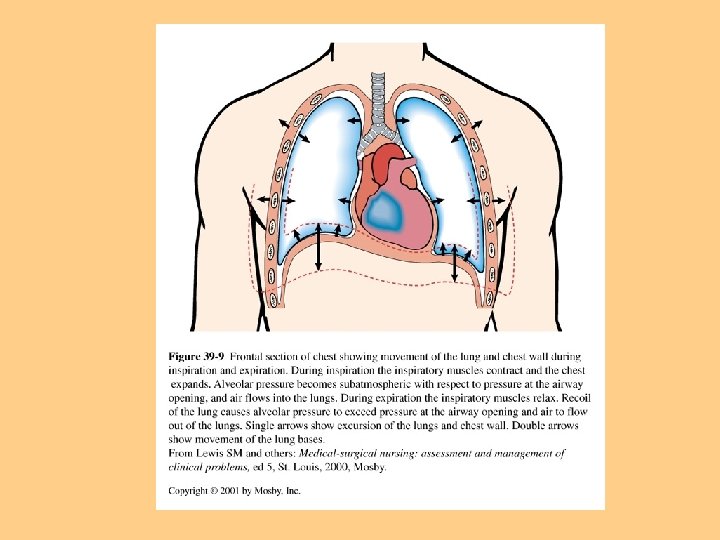

Lung Compliance Ability of lungs to distend or expand in response to increased intra-alveolar pressure, the ease in which lungs are inflated l Compliance is decreased in pulmonary fibrosis, emphysema l Lung compliance is affected by surface tension of alveoli, surfactant lowers surface tension. l

Airway Resistance l Pressure difference between the mouth & the alveoli in relation to the rate of flow of inspired gas l Airway resistance increased in airway obstruction, asthma, tracheal edema

Structure & Function Accessory Muscles Assist in increasing lung volume during inspiration l Scalene & sternocleidomastoid (inspiration) l COPD patients use these frequently l Abdominal muscles l Trapezius muscle and pectoralis play minor role l

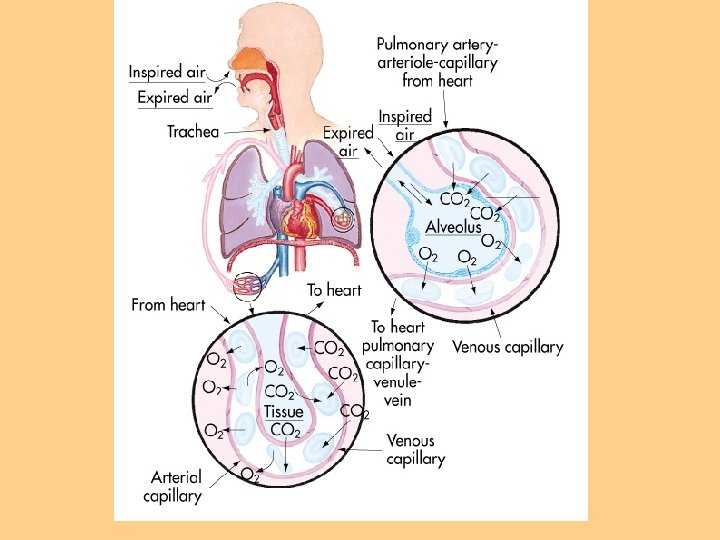
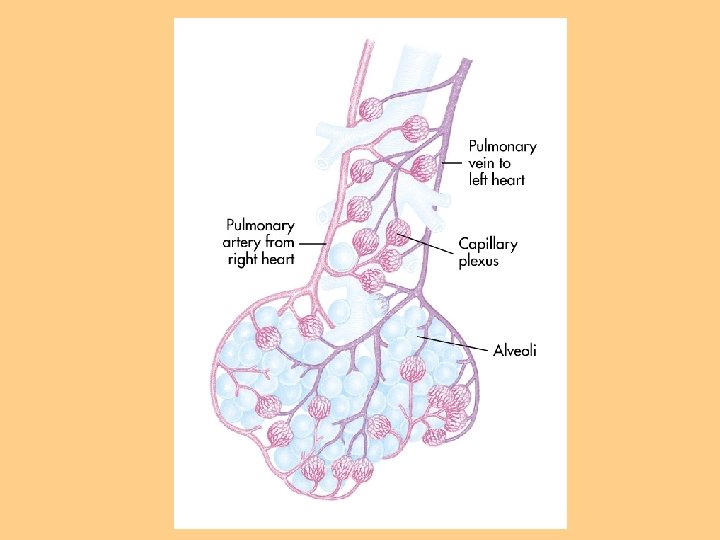
Pulmonary Circulation l Move blood to and from the alveolocapillary membrane for gas exchange l Begins at pulmonary artery which receives deoxygenated blood from RV l Flow continues to PA to pulmonary arterioles to pulmonary capillaries where blood comes in contact with alveolocapillary membrane

Respiratory Gas Exchange Diffusion-movement of molecules from an area of higher concentration to areas of lower concentration (oxygen & CO 2) l Occurs at the alveolocapillary level l Rate of diffusion affected by thickness of membrane l Increased thickness: COPD, pulmonary edema, pulmonary infiltrates, effusions l

Oxygen Transport l Consists of lung & cardiovascular system l Delivery depends on O 2 entering lungs (ventilation) l And blood flow to lungs & tissues (perfusion) l Rate of diffusion V/Q ratio l O 2 - carrying capacity

Oxygen Transport l O 2 transport capacity affected by hemoglobin l Oxyhemoglobin l CO 2 Transport-diffuses into RBC’s & is rapidly hydrated into carbonic acid

Regulation Of Respiration l CNS control rate, depth, & rhythm l Change in chemical content of O 2, CO 2 can stimulate chemorecptors which regulate neural regulators to adjust rate & depth of ventilation to maintain normal Arterial Blood Gases.

Factors Affecting Cardiopulmonary Functioning Physiological l Age l Medications l Stress l Developmental l Lifestyle l Environmental l

Factors Affecting Oxygenation: Physiologic Any factor that affects cardiopulmonary functioning directly affects the body’s ability to meet O 2 demands l l Physiologic factors include: decreased O 2 carrying capacity, hypovolemia, increased metabolic rate, & decreased inspired O 2 concentration

Conditions Affecting Chest Wall Movement Pregnancy l Obesity l Trauma l Musculoskeletal Abnormalities l Neuromuscular Disease l CNS Alterations l Influences of Chronic Disease l

Alterations in Cardiac Functioning l Disturbances in Conduction l Altered Cardiac Output l Impaired Valvular Function l Impaired Tissue Perfusion (Myocardial)

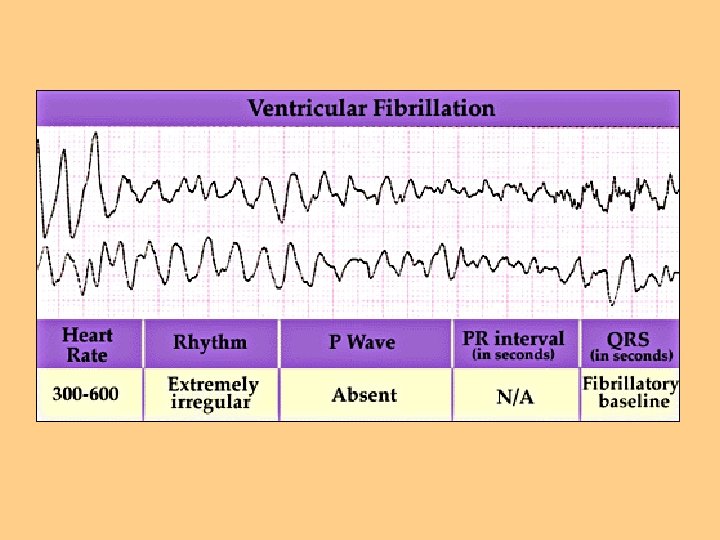
Disturbances of Conduction l l Dysrhythmias-deviation from NSR l Supraventricular dysrhythmias l Junctional Classified by cardiac response origin of impulse dysrhythmias l Tachycardia l Bradycardia l Ventricular dysrhythmias
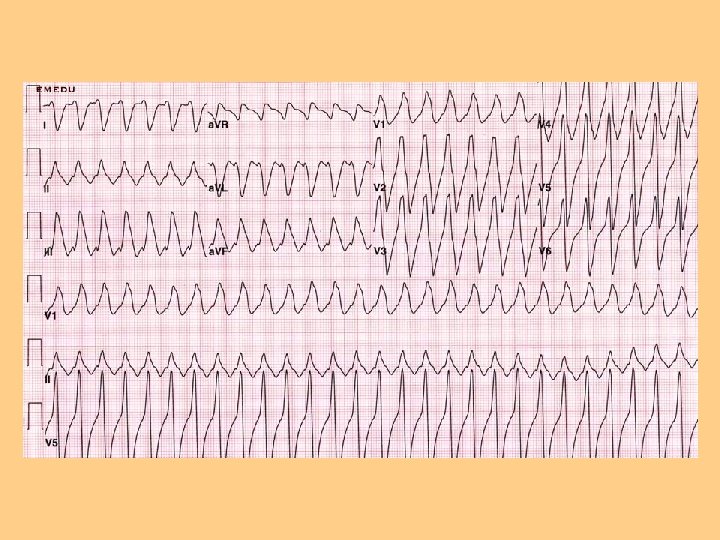
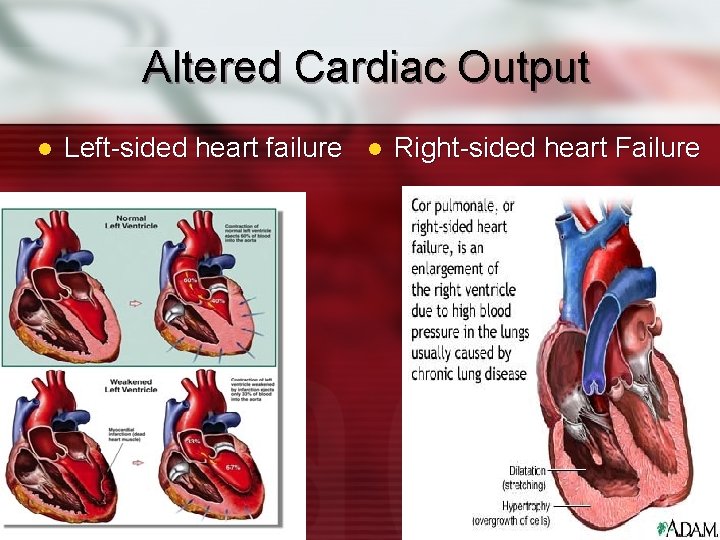
Altered Cardiac Output l Left-sided heart failure l Right-sided heart Failure
Impaired Valvular Function l Stenosis -Stenosis of valves can cause ventricles to hypertrophy (enlarge) l Obstruction of Flow l Valve Degeneration l Lead to Regurgitation of Blood
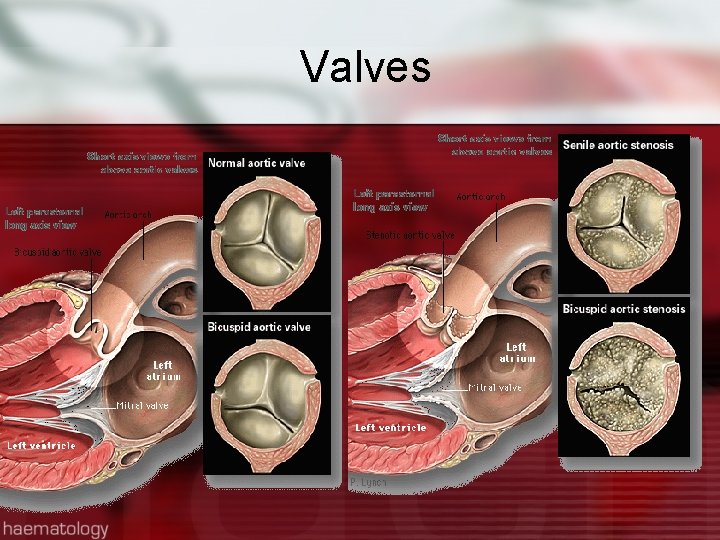
Valves

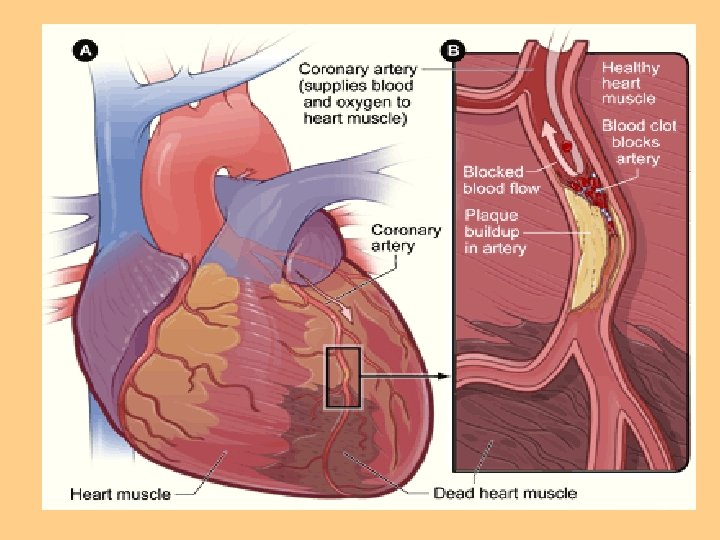
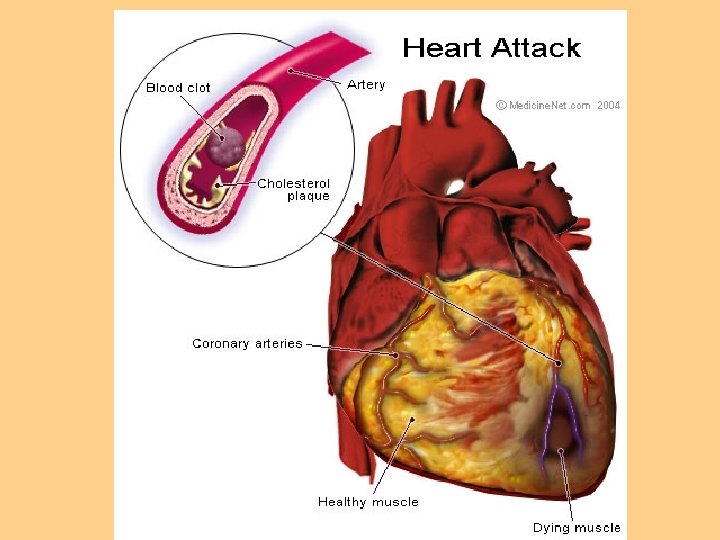
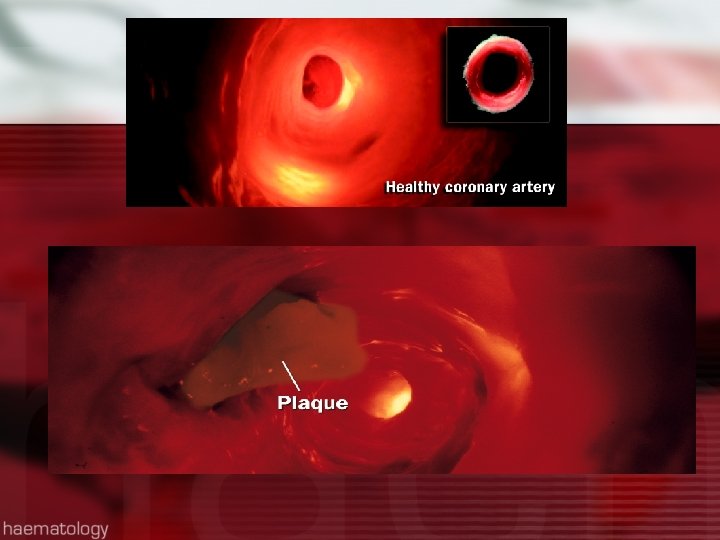
Impaired Tissue Perfusion: Myocardial l Insufficient blood flow from coronary arteries to meet heart O 2 demand l Manifested as angina, MI l Angina-transient imbalance between O 2 supply & demand’ resulting in chest pain l Atherosclerosis: most common cause of impaired blood flow to organs

Myocardial Ischemia l Myocardial Infarction-sudden decrease in coronary blood flow or an increase in myocardial oxygen demand without adequate perfusion l Infarction occurs because of ischemia (reversible) or necrosis (irreversible) of heart tissue
Impaired Tissue Perfusion Cardiac perfusion Cerebral perfusion (TIA, CVA) Peripheral vascular perfusion Incompetent valves Thrombus formation Blood alterations (anemia)
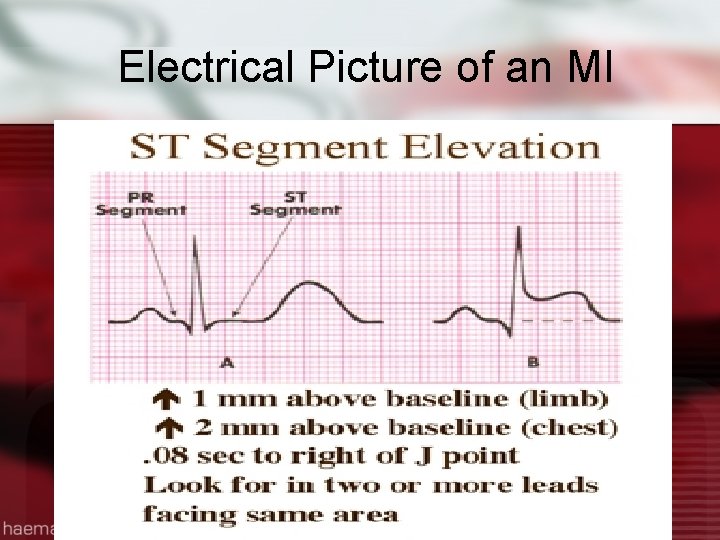
Electrical Picture of an MI
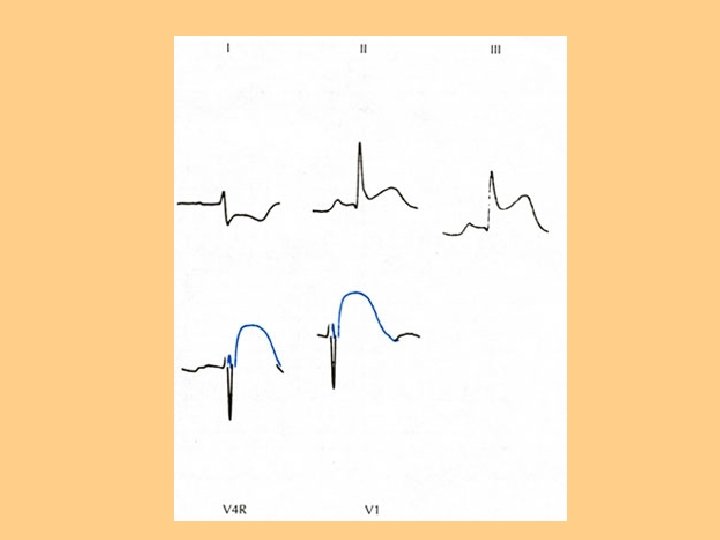

Alterations in Respiratory Function l Goal of ventilation is to produce a normal arterial CO 2 tension (Pa. CO 2) between 35 -45 mm. Hg and maintain normal arterial O 2 tension (Pa. O 2) between 95 -100 l Alterations affect ventilation or O 2 transport l Hyperventilation, Hypoxia

Alterations in Respiratory Function l Hyperventilation- state of ventilation in excess of that required to eliminate the normal venous CO 2 produced by cell metabolism l Anxiety, infection, drugs or acid-base imbalance can produce hyperventilation

Hyperventilation l l l l Lightheadedness Disorientation Dizziness Tachycardia Chest pain SOB Blurred vision Extremity numbness
Hypoventilation l Alveolar ventilation is inadequate to meet body’s O 2 demand l Pa. CO 2 elevates, Pa. O 2 drops l Severe atelectasis can cause hypoventilation l Hypoventilation and COPD


Hypoventilation l l l l Disorientation Lethargy Dizziness Headache Decreased ability to follow instructions Convulsions Coma Dysrhythmias, cardiac death

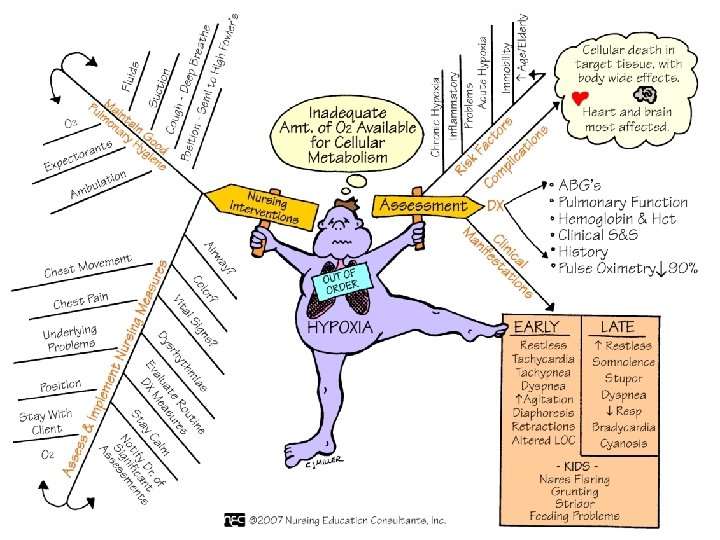
Hypoxia l Inadequate tissue oxygenation at the cellular level l Deficiency of O 2 delivery or O 2 utilization at cell level l Causes: Decreased Hgb, diminished concentration of inspired O 2, decreased diffusion poor tissue perfusion, impaired ventilation

Hypoxia l l l l Restlessness Inability to concentrate Decreased LOC Dizziness Behavioral changes Agitation Change in vital signs Cyanosis: Peripheral vs Central
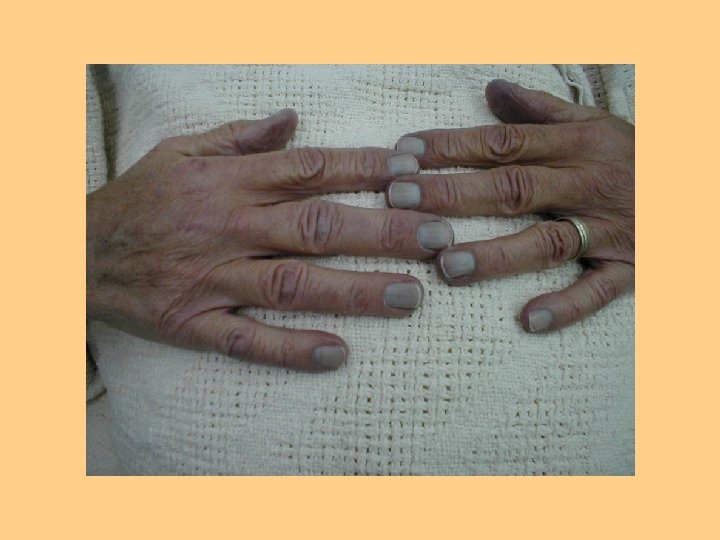

Other Factors Affecting Oxygenation Age l Environmental l Lifestyle l Medications l Stress l Infection l

Nursing Process Assessment History Physical Exam Diagnostic Tests Blood Studies

Assessment: Nursing History l l l Client’s ability to meet oxygen needs Pain Fatigue Smoking Dyspnea Orthopnea l l l l Environmental Exposure Respiratory Infections Allergies Health Risks Medications Cough Wheezing Altered breathing patterns

Physical Exam l Inspection l Palpation l Percussion l Auscultation

Inspection of Cardiopulmonary Status l l l l l Cyanotic mucous membranes Pursed lip breathing Jugular neck vein distention Nasal faring Use of accessory muscles Peripheral or central cyanosis Edema Clubbing of fingertips Altered breathing patterns Pale conjunctivae
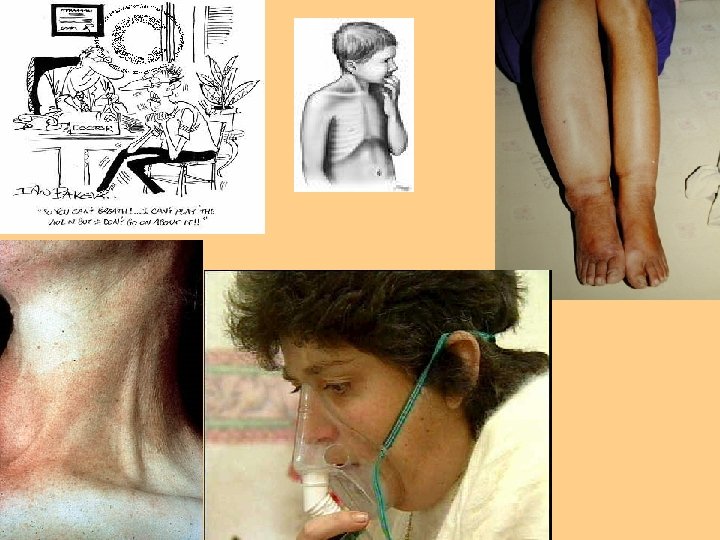
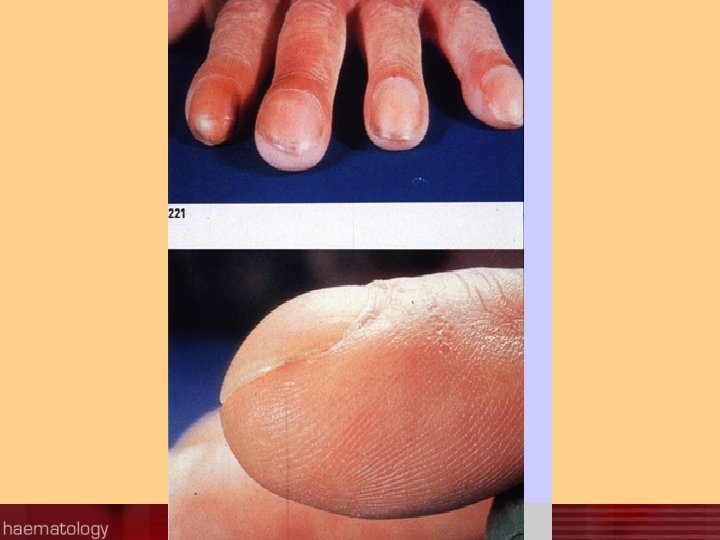
Marked clubbing of the nails.
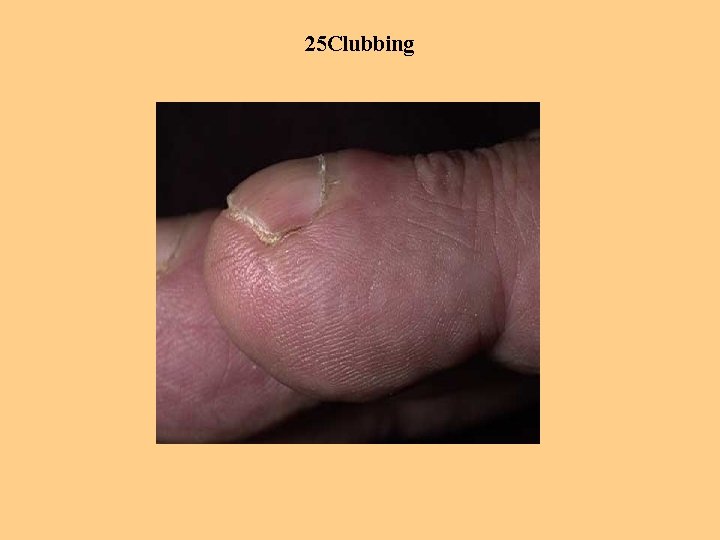
25 Clubbing Clubbing nails

Palpation Palpate for thoracic excursion l PMI l Palpation of peripheral pulses l Palpation for skin temperature, capillary refill l Palpation of lower extremities for peripheral edema l
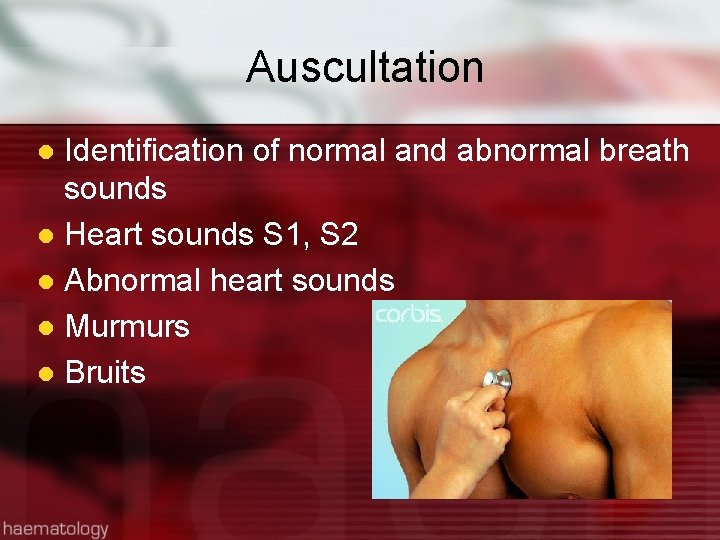
Auscultation Identification of normal and abnormal breath sounds l Heart sounds S 1, S 2 l Abnormal heart sounds l Murmurs l Bruits l

Diagnostic Tests l l l EKG Holter Monitor Stress tests Echocardiogram Cardiac cath TEE l l l l Pulmonary functions Chest x-ray Arterial blood gases Pulse ox Bronchoscopy Thoracentesis CT Scan/MRI Ventilation/Perfusion Scan
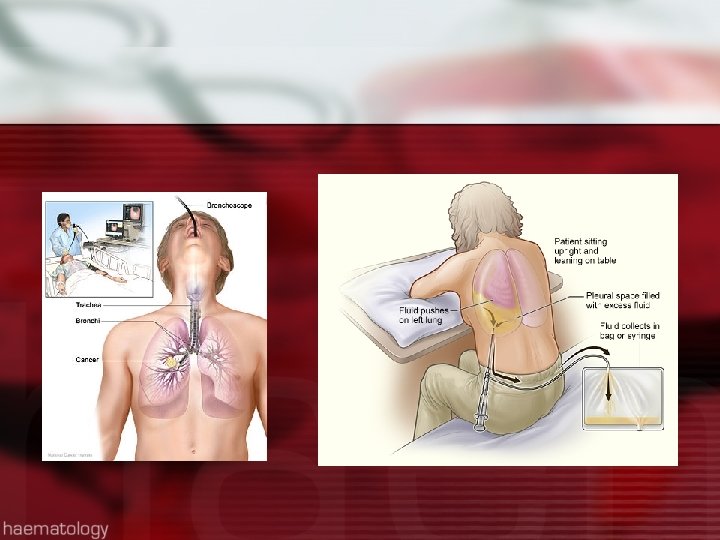

Lab Studies l l l l l Electrolytes Cardiac enzymes BNP Lipid Profile Coagulation Studies CBC Troponin D Dimer C reactive protein l l Sputum culture Throat culture AFB Cytology
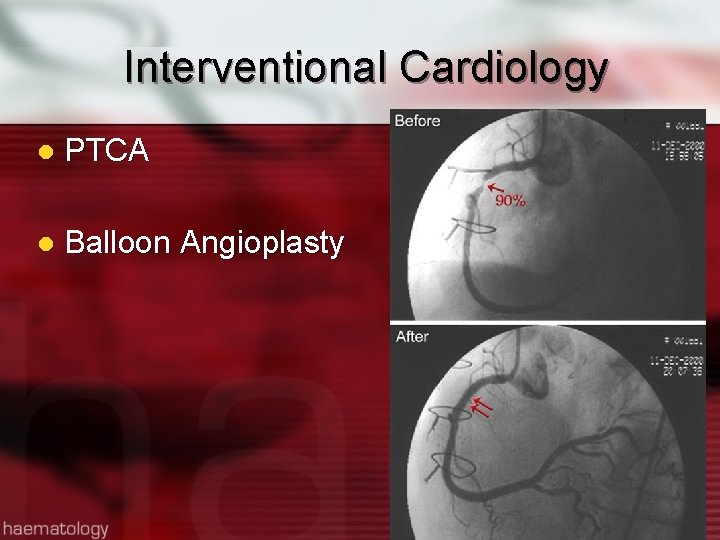
Interventional Cardiology l PTCA l Balloon Angioplasty
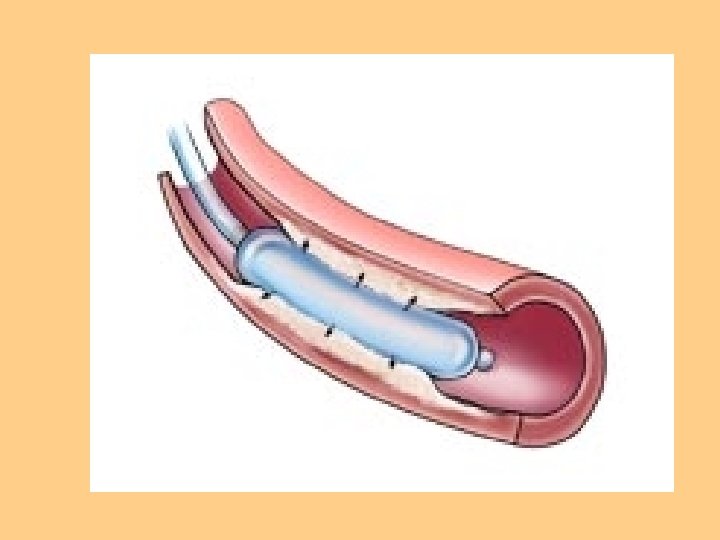
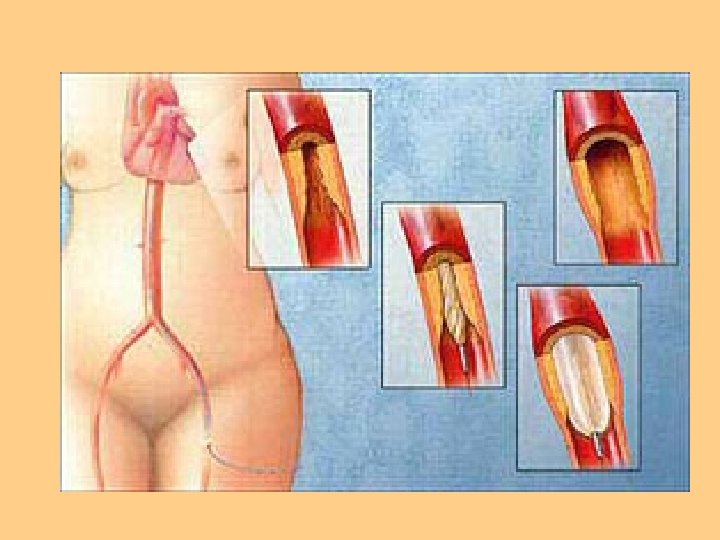
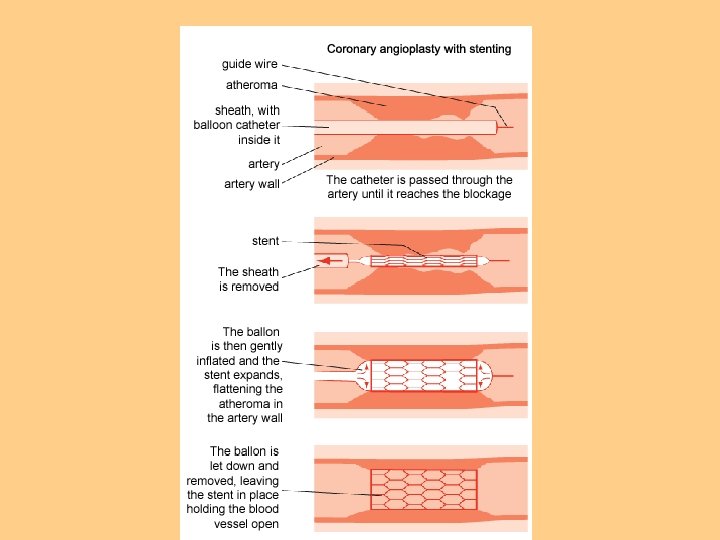

Nursing Diagnosis Activity Intolerance l Ineffective Tissue Perfusion l Decreased Cardiac Output l Impaired Gas Exchange l Ineffective Airway Clearance l Ineffective Breathing Pattern l Fatigue l Anxiety l

Planning for Care Develop goals and outcomes l Set Priorities l Select appropriate interventions l Collaborate l Involve patient and family in care l

Implementation: Health Promotion/Prevention l Vaccinations l Healthy Lifestyle l Environmental pollutants

Implementation: Acute Care Dyspnea Management l Airway Management l Mobilization of Airway Secretions l Maintenance and Promotion of Lung Expansion l Maintenance and Promotion of Oxygenation l Breathing Exercises l Hydration l

Dyspnea Management Treat underlying disease process and additional therapies as needed: l Pharmacological agents l Oxygen therapy l Physical techniques l Psychosocial techniques l

Airway Maintenance Mobilization of Secretions Hydration l Humidification l Nebulization l Coughing techniques l Chest PT l Postural drainage l Suctioning l Artificial airways l

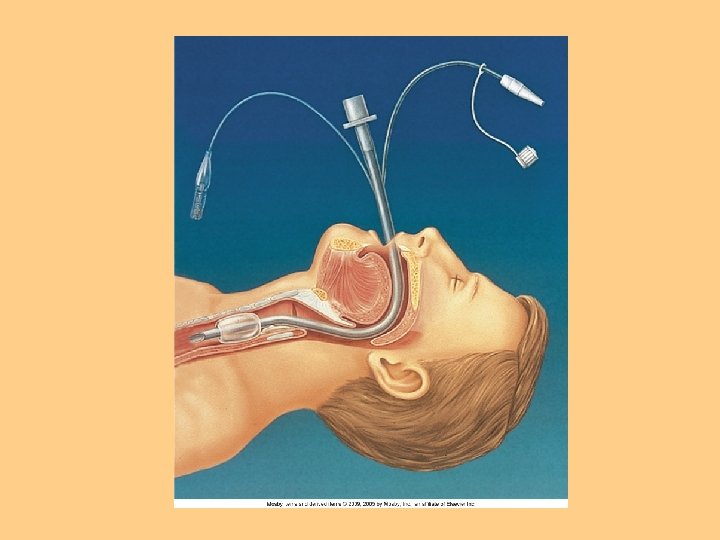


Suctioning l Oropharyngeal l Nasopharyngeal l Orotracheal l Nasotracheal l Tracheal
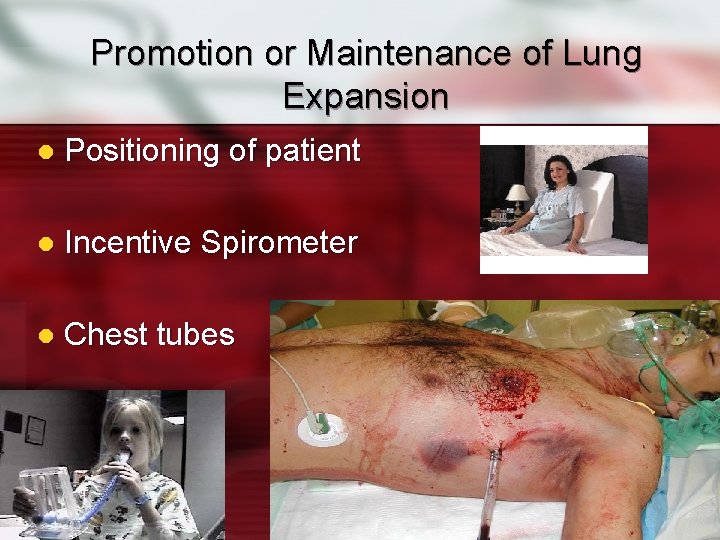
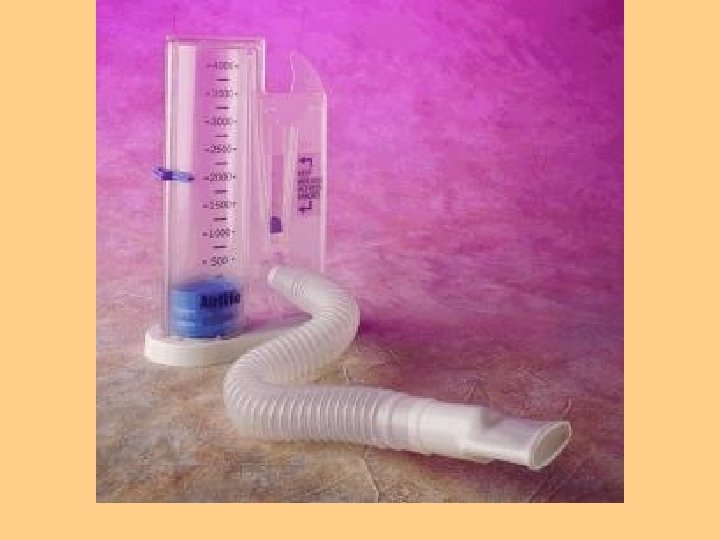
Promotion or Maintenance of Lung Expansion l Positioning of patient l Incentive Spirometer l Chest tubes
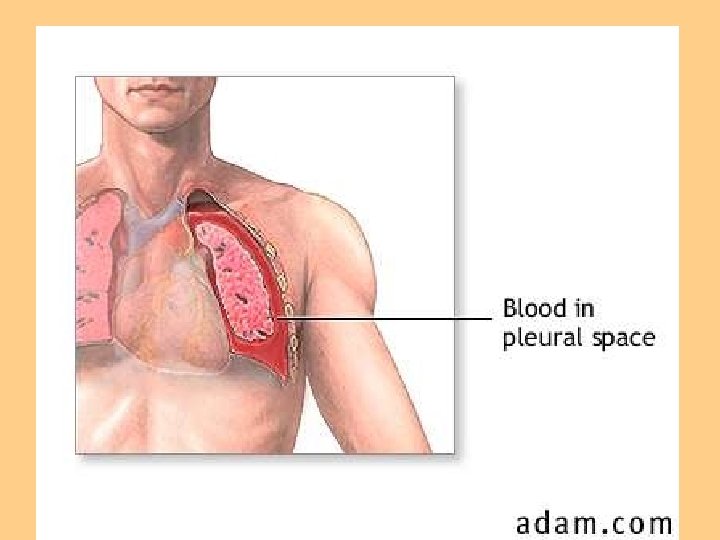
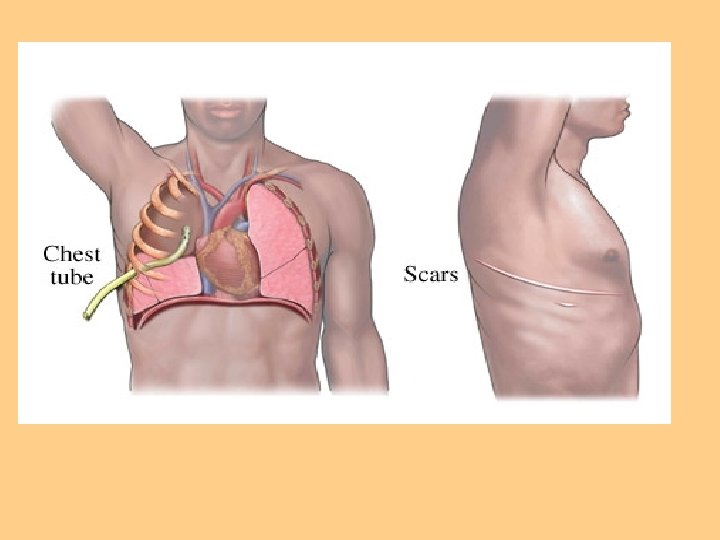
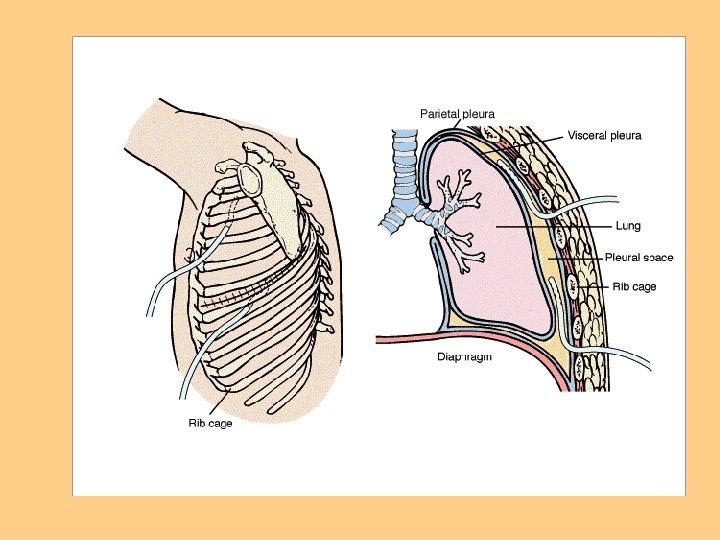


Oxygen Therapy l Goal is to prevent or relieve hypoxia l Not a substitute for other treatment l Treated as a drug l Safety precautions

Methods of O 2 Delivery l Nasal cannula-1 -4 liters/min l Oxygen Mask-Simple face mask, Venturi mask, Non-rebreather face mask, Rebreather mask l Home Oxygen Therapy



l
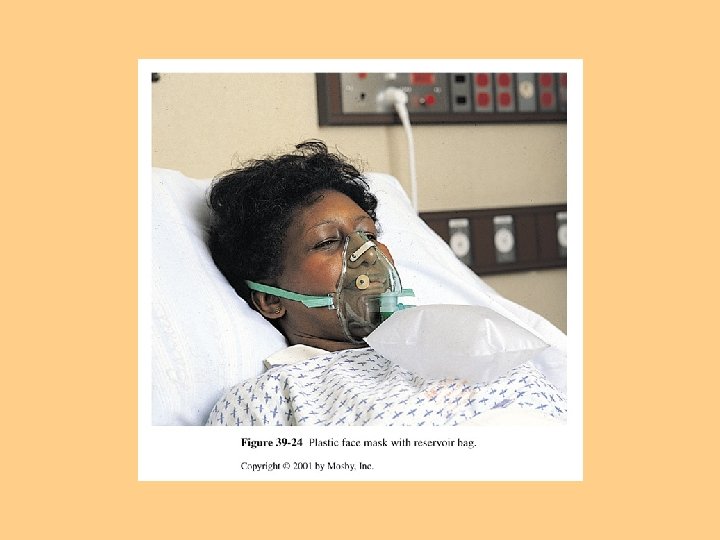
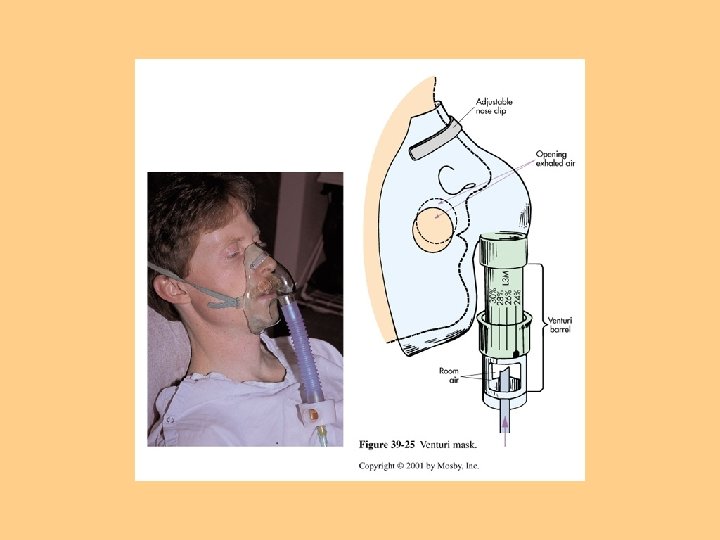

Medications Affecting Cardiopulmonary Functioning l Cardiovascular agents: Nitrates, Calcium Channel Blockers, Beta Blockers, ACE Inhibitors/Blockers Positive Inotropic Agents (Digoxin) Antiarrhythmic Agents Antilipemic Agents Bronchodilators Cough suppressants/expectorants Benzodiazepines/Narcotics l Diuretics l Anticoagulants/Antiplatelet Agents l l l

Acute MI Core Measures www. the jointcommission. org l Aspirin at arrival l Aspirin prescribed at discharge l ACE Inhibitor/ARB prescribed at discharge for left ventricular systolic dysfunction l Adult smoking cessation counseling l Beta Blocker prescribed at discharge l Beta Blocker at arrival l Thrombolysis within 30 minutes l Percutaneous coronary intervention within 90 minutes

Promoting Cardiovascular Circulation l Positioning l Medications l Preventing venous stasis l Cardiopulmonary Resusitation

Clicker Question During the first heart sound, S 1 or “Lub”, what valves are closing? l A. Aortic and pulmonic l B. Tricuspid and mitral l C. Aortic and mitral l D. Mitral and pulmonic l

Clicker Question Nursing care prior to cardiac catheterization includes all of the following except: l A. Assess for allergy to iodine l B. Evaluation of peripheral pulses l C. Informed consent l D. Clear liquids prior to the test l

Clicker Question Treatment of suspected myocardial infarction (MI) includes: l A. Oxygen, aspirin, morphine, nitroglycerin l B. Acetaminophen, bedrest, EEG l C. Oxygen, cardiac catheterization l D. Mechanical ventilation, CEA levels, acetaminophen l

Clicker Question Which of the following is an early sign of hypoxia? l A. Pallor l B. Restlessness l C. Difficulty breathing l D. Decreased heart rate l

Clicker Question l l l 3. When evaluating a postthoracotomy client with a chest tube, the best method to properly maintain the chest tube would be to: A. Strip the chest tube every hour to maintain drainage. B. Place the device below the client’s chest. C. Double clamp the tube except during assessment. D. Remove the tubing from the drainage device to check for proper suctioning. 40 - 120

Clicker Question 2. A client with a tracheostomy has thick tenacious secretions. To maintain the airway, the most appropriate action for the nurse includes: l A. Tracheal suctioning l B. Oropharyngeal suctioning l C. Nasotracheal suctioning l D. Orotracheal suctioning l 40 - 121

To have a persons Heart in Your Hands!!!!
- Slides: 122