Basic HIV Course for Health Professionals Session 3

Basic HIV Course for Health Professionals Session 3 a: HIV Testing Services (HTS)

Learning Objectives By the end of this session participants should be able to: • Explain what HIV testing services (HTS) are • Define the different modalities under HTS • Describe the guiding principles of HTS • Describe the different HTS service delivery platforms • Describe the HIV testing process • Outline different HIV tests results • Describe equipment required to conduct an HIV rapid test • Explain importance of linkage to care following a HIV positive diagnosis and the services that patients should expect to receive

Group Discussion What are the benefits of knowing one’s HIVstatus?

Definition: HIV Testing Services (HTS) • HIV testing services (HTS) embrace full range of services provided with HIV testing: • Counselling (pre‐test information, post-test counselling) • Linkage to HIV prevention, treatment and care services and other clinical and support services • Coordination with lab services to support quality assurance and the delivery of correct results

A Rights-Based Approach • Human rights-based approach that prioritises: • universal health coverage • gender equality and • health-related rights such as • • accessibility availability acceptability and quality of services • essential for success of HTS programme This Photo by Unknown Author is licensed under CC BY-SA

The 5 Cs: The Foundation of Effective HTS Consent People who receive testing must: • Counselled and consent to be tested • be informed of HTS process and of right to decline testing Confidentiality • Discussions between HTS provider and client should not be disclosed to anyone without consent of person being tested • Encourage shared confidentiality with partner or family members • Pre-test information can be done in group setting, but provide individuals with a private setting for individuals with questions they do not wish to share with others • Follow HIV testing with high-quality post-test counselling • Quality assurance (QA) mechanisms are essential to ensure people receive a correct diagnosis • Linkage to prevention, treatment and care services and effective and appropriate follow-up should be provided Counselling Correct Connection
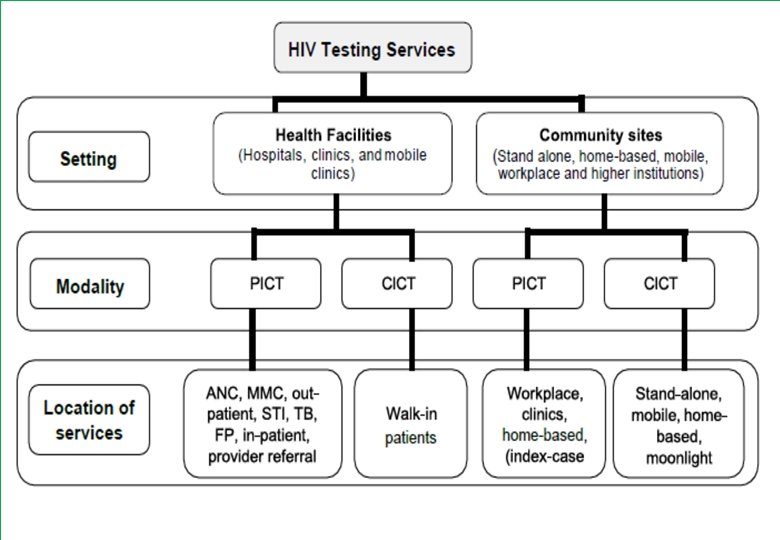

CICT - Client Initiated Counselling and Testing • For client-initiated counselling and testing, (CICT), individual voluntary requests (previously VCT)an HIV test and counselling at health facility and other areas where HTS services are offered. • Those receiving CICT provide signed consent, which should always be documented by provider in patient’s file

PICT - Provider Initiated Counselling and Testing • Also known as Routine offer of Voluntary Counselling and testing • In this model, provision of HIV counselling and testing is offered and recommended by health care providers to all patients attending health facilities - standard component of medical care • All patients that receive PICT should provide, at a minimum, written consent for HIV testing

HIVSS- Self-Screening • Person voluntarily collects own specimen and performs an HIV screening and interprets the result • Not recommended for users with known HIV status who are taking ARV drugs - may lead to an incorrect self-test result (false non-reactive)
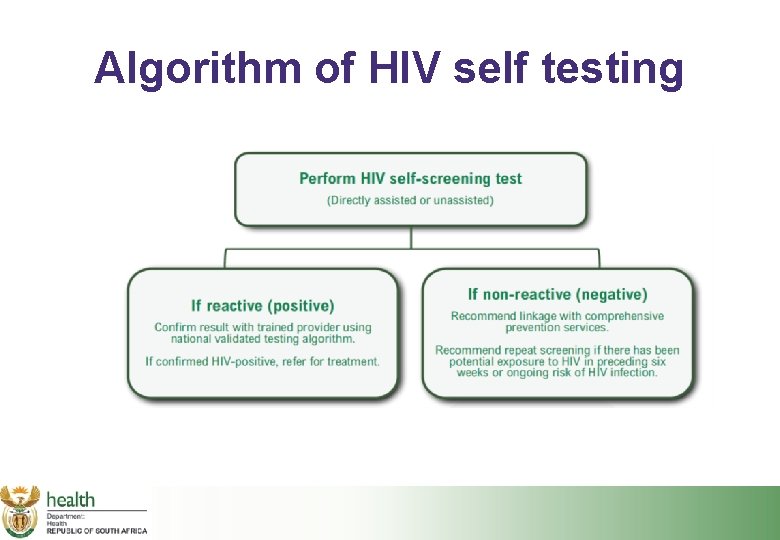
Algorithm of HIV self testing

Points to note for HIV self-testing

Index testing • Index testing: voluntary process where counsellors and/or health care workers ask index clients to list all of their: (1) sexual or injecting drug partners within the past year, and (2) biologic children. • Index client: an individual newly diagnosed as HIV-positive and/or an HIV-positive individual who is enrolled in HIV treatment services

Index testing process • If the index client agrees, each listed partner and child is: (1) contacted, (2) informed that they need an HIV test, and (3) offered voluntary HIV testing services (HTS). • Goal of index testing is to break the chain of HIV transmission by offering HTS to persons who have been exposed to HIV and linking them to: • HIV treatment, if positive, or • Prevention services (e. g. VMMC, Pr. EP, condoms), if negative.
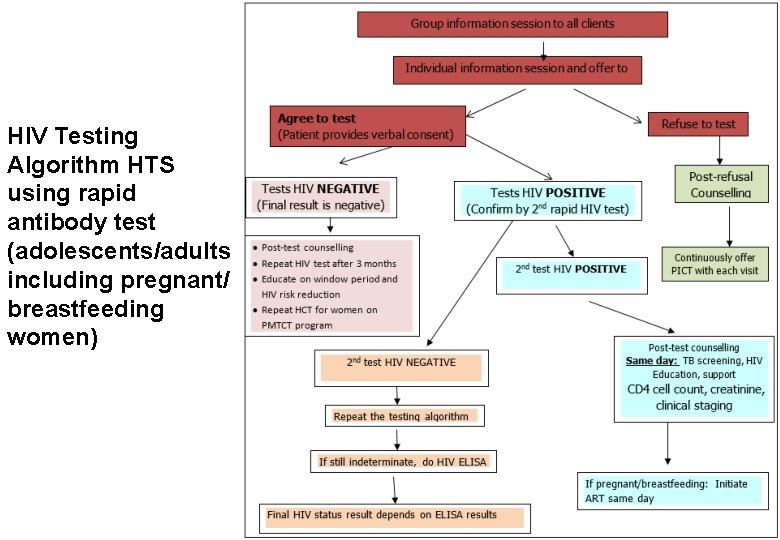
HIV Testing Algorithm HTS using rapid antibody test (adolescents/adults including pregnant/ breastfeeding women)
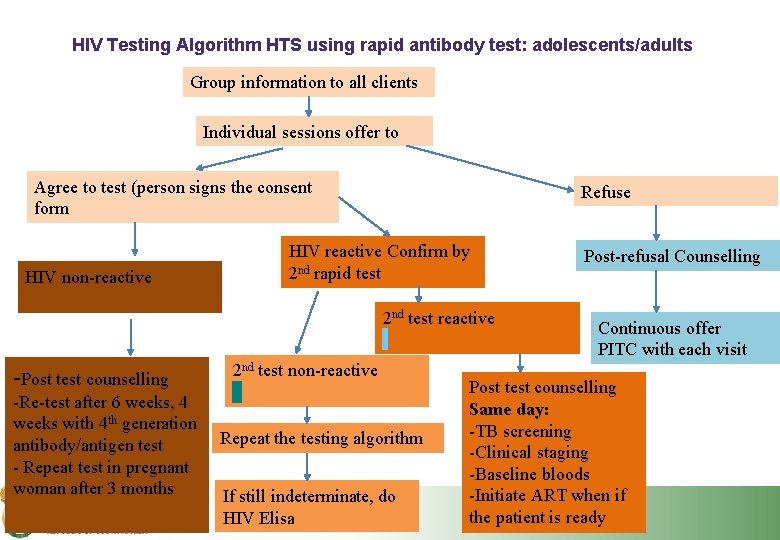
HIV Testing Algorithm HTS using rapid antibody test: adolescents/adults Group information to all clients Individual sessions offer to Agree to test (person signs the consent form HIV non-reactive Refuse HIV reactive Confirm by 2 nd rapid test 2 nd test reactive -Post test counselling -Re-test after 6 weeks, 4 weeks with 4 th generation antibody/antigen test - Repeat test in pregnant woman after 3 months 2 nd test non-reactive Repeat the testing algorithm If still indeterminate, do HIV Elisa Post-refusal Counselling Continuous offer PITC with each visit Post test counselling Same day: -TB screening -Clinical staging -Baseline bloods -Initiate ART when if the patient is ready

Rapid Testing: Principles of Testing Process must be: • Completely voluntary; • Conducted with informed consent • Confidential • Protective of person who tested • All forms of HTS should be voluntary, adhere to five Cs • Children may self-consent to HIV testing if 12 years of age and above, and child is of sufficient maturity to understand benefits, risks, and implications of HIV test

Components of Testing 1. Informed consent 2. Consent formed signed 3. Collecting the necessary equipment 4. Performing the test 5. Interpreting and providing the result This Photo by Unknown Author is licensed under CC BY-NC-SA

Consent • No person may undergo testing without full information of what test is about • It is vitally important prior to testing that patient has signed for informed consent • Consent may either be written or verbal

Pre-test Information • Must be age-appropriate through either individual or group information session • Followed by individual one-on-one session to assess whether information communicated in group session has been understood and remaining questions answered, with aim to clarify misunderstandings, address concerns

Collecting the Necessary Equipment Checklist of Supplies and Materials Hand washing soap Sharps container Paper towels Red bag for soiled materials Surgical Gloves Clear plastic bag for unsoiled materials Alcohol swabs Band-Aids or plasters Sterile Lancets Spray/Wash bottle Cotton gauze / wool Pens for labelling Transfer pipettes Disinfectant HIV Rapid Test Kit(s) Log book or register Diluent Standard Operating Procedures Timer, clock, or watch Positive and Negative Controls

Steps Involved in Performing the HIV Test (1) • Introduction • Introduce yourself, explain your role, HTS process • Discuss confidentiality • Contracting

Steps Involved in Performing the HIV Test (2) • Motivation for testing and risk reduction • Explore reasons for testing, knowledge of HIV/AIDS and client history • Discuss client’s sexual risk behaviour and risk reduction options • Discuss advantages and disadvantages of testing • Explain window period and seroconversion and their impact on results • Check client’s understanding of the above and invite questions

Steps Involved in Performing the HIV Test (3) • Basic HIV/AIDS education • Explain and discuss: what HIV and AIDS are, HIV transmission, prevention measures (condom use, Pr. EP etc. ), HIV symptoms and myths

Steps Involved in Performing the HIV Test (4) • Anticipation of the reaction to HIV test results • Discuss feelings about possible results • Discuss imagined consequences of a positive and negative result • Discuss and identify possible supportive people • Discuss disclosure • Provide referral, wellness and support options

Steps Involved in Performing the HIV Test (5) • Testing procedure and readiness to test • Discuss type of test, what it measures, accuracy, confirmatory tests and how results are given • Discuss readiness to test • Explain procedure to client • Get consent; signed consent is adequate • Open test kit in front of client • Label test kit using client registration number or name • Position hand palm-side up • Choose whichever finger is least calloused

Performing the Rapid Test: Testing Procedure Summary • • • Wash hands, put on gloves Position hand palm-side up, assess fingers, choose least calloused Apply intermittent pressure to finger to help blood flow Clean fingertip using alcohol swab, allow area to dry for 30 seconds Hold finger firmly and firmly press lancet to puncture fingertip Wipe away first drop of blood Collect blood using pipette Lower finger to below elbow to encourage blood flow Apply pressure to puncture site using cotton wool to stop bleeding Dispose of needle in sharps container

Clients who Test HIV-Negative • Post-test counselling session should focus on: • keeping individual negative and • active linkage to appropriate prevention services • • Educate person on window period Educate about Pr. EP Educate about VMMC is male patient Provide person with condoms and lubricants

Post-Test Services • All clients, regardless of the outcome of the HIV test, should be offered and should receive post-test counselling based on their test result • All results must be communicated clearly

Post-test Services for People Testing HIV-Negative • Those testing HIV-negative should receive health information about test result including: • risk reduction counselling • recommendations on uptake of preventive behaviours including consistent condom use • Post-test counselling session should focus on keeping individual negative • Provide active linkage to appropriate services

Services for People with Discrepant Test Results • An HIV-inconclusive/indeterminate result means: first reactive test results were not confirmed by subsequent testing using an HIV rapid test • Clients with an HIV-inconclusive status should be told a definitive diagnosis cannot be provided that day and • Whole blood should be drawn and sent to lab for ELISA testing as a tie breaker; give clients a clear plan for follow-up testing • Encourage them to return within seven days for ELISA results to confirm diagnosis

Managing Discrepant HIV Rapid Testing ELISA/EC HIV screening Test HIV REACTIVE HIV NON-REACTIVE ELISA HIV confirmation Test REACTIVE NONREACTIVE Report as HIV POSITIVE Report as HIV DISCREPANT and request client to return to facility after six weeks for rapid testing Report as HIV NEGATIVE
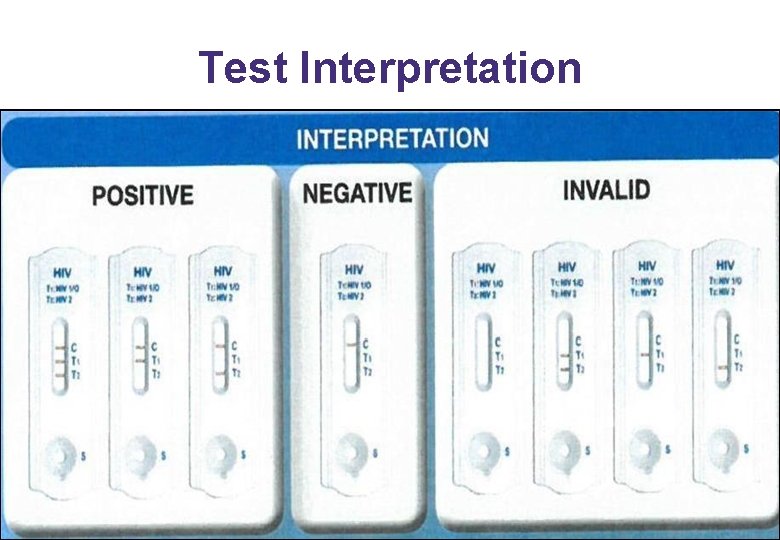
Test Interpretation

When to repeat the HIV test WHO WHEN Pregnant/breastfeedi Every full BANC visit ng women Postnatal health care encounter throughout breastfeeding (to detect HIV sero(monthly testing recommended – aligned to EPI expanded conversion) programme of immunisation) Routinely at labour/delivery At 6 -week mother/child visit Couple counselling and testing recommended HIV-exposed babies At Birth (do not repeat test if Around 10 weeks (and 18 weeks for those on 12 week AZT & infant confirmed to be NVP) HIV-infected) At 18 months 6 weeks after complete cessation of breastfeeding All children Anytime if child has symptoms suggestive of HIV General population 6– 12 -monthly depending on risk Adolescents 6– 12 -monthly if sexually active or more frequently if they have new sexual partner/s or if having unprotected intercourse If exposed to HIV After 6– 12 weeks for window period Key populations Every 3– 12 months (MSM and sex

Recommended Testing Intervals for Infants and Children – HIV PCR Test AT BIRTH • ALL HIV-exposed neonates • These infants can be regarded as high-risk cases that need an urgent diagnosis so should receive HIV PCR as soon as possible after birth • Repeat HIV PCR testing at 10 weeks or 18 weeks should be done on all HIV-exposed infants without confirmed HIV infection, regardless of earlier testing • Any infant with a positive birth PCR should be urgently referred/ discussed telephonically for ART initiation by a paediatric HIV expert • • At 10 weeks: All HIV-exposed infants At 18 weeks: All infants who received 12 weeks of NVP prophylaxis

Recommended Testing Intervals for Infants and Children – Rapid HIV Antibody (1) AT 18 MONTHS • All HIV exposed infants Breastfed infants: (6 weeks post cessation of breastfeeding) • All HIV exposed infants- age appropriate: if • <18 months old- do HIV PCR >18 months old – do rapid HIV Antibody test Family and social history (at all times) • Parental request to test the child • Father or sibling with HIV infection • Death of mother, father or sibling • When mother’s HIV status is unknown, her whereabouts are unknown, or she is unavailable to be tested
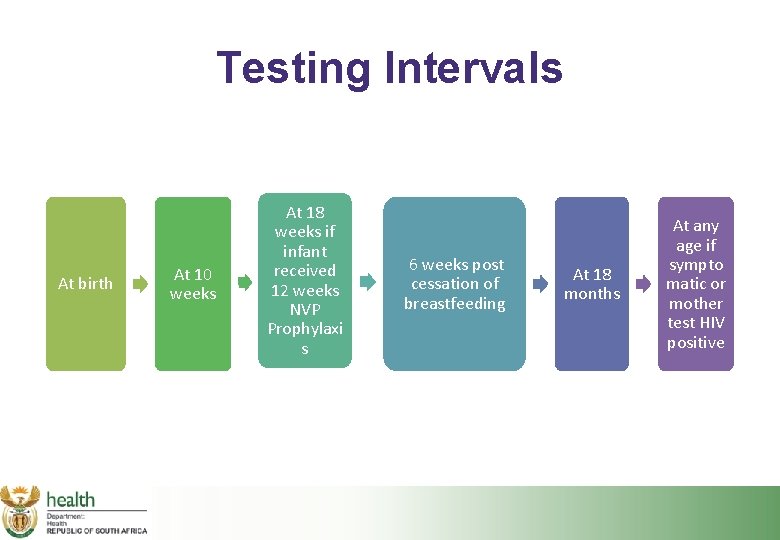
Testing Intervals At birth At 10 weeks At 18 weeks if infant received 12 weeks NVP Prophylaxi s 6 weeks post cessation of breastfeeding At 18 months At any age if sympto matic or mother test HIV positive

Recommended Testing Intervals for Infants and Children – Rapid HIV Antibody (2) All children (at all times) with: • Clinical features suggestive of HIV infection • Acute, severe illness • IMCI classification of Suspected symptomatic HIV infection • IMCI classification of Possible HIV infection • TB diagnosis or history of TB treatment • Risk of sexual assault • Wet-nursed or breastfed by a woman with unknown or HIV-positive status • Children considered for fostering

Linkage to Care (1) • Activities that support people testing for HIV and people diagnosed with HIV to engage with prevention, treatment and care services • For people with HIV, period begins with HIV diagnosis and ends with enrolment in care or treatment • Responsibility of all HTS providers to ensure that clients are connected to appropriate care • HIV testing alone is of limited value unless linked with other services

Linkage to Care (2) Services include: • Treatment, care, support, disease management Sexual and reproductive health • Testing for partners and families • includes partner notification and index case testing • HIV prevention, including education on condom use and lubricants, and voluntary medical male circumcision (VMMC) • other clinical and supportive services

Any Questions? Thank you!
- Slides: 41