Barcelona 20 22 January 2011 MODULE FOR NUCLEAR

Barcelona, 20 -22 January 2011 MODULE FOR NUCLEAR MEDICINE Prepared by: Marta Sans-Mercè University Hospital Center and University of Lausanne, Switzerland Mercè Ginjaume Universitat Politècnica de Catalunya, Spain This training material has been developed in the framework of the Research project ORAMED, Optimization of Radiation Protection of Medical staff, funded by the European Atomic Energy Community's Seventh Framework Programme (FP 7/2007 -2011) under grant agreement n° 211361. Workshop on optimization of Radiation Protection of Medical Staff ORAMED SPECIFIC TRAINING

USE AND DISCLAIMER l This is a Power. Point file. l It may be downloaded free of charge. l It is intended for teaching and not for commercial purposes. l It is based on the results and guidelines derived from the “ORAMED, Optimization of Radiation Protection of Medical staff” project, funded by the European Atomic Energy Community's Seventh Framework Programm.

Objectives Framework: it is based on lessons learned from the ORAMED project, it mainly concentrates on extremity dosimetry in nuclear medicine After the training participants should be able to 1. - know the physical characteristics of the different sources of exposure in nuclear medicine and the limits of exposure. 2. - identify the organs at risk for the different diagnostic/ therapy procedures. 3. - recognize and apply radiation protection means to ensure an adequate protection of staff. 4. - select the best dosimetric system and to implement the best monitoring procedure (type of dosemeter, position of use, interpretation of dosemeter reading). 5. - identify good and bad practices, in order to adapt, if needed, changes in the procedures, to improve the daily practice.

General structure 1. - Introduction/revision: (what should be known: Aims of the medical speciality, different types of procedures, types of radiation sources, characteristics + workers dose-limit) 2. - Radiological risks (based on ORAMED results, the critical procedures, organs at risk and associated doses are highlighted). 3. - Staff monitoring: available dosemeters (Different types of available dosemeters together with the recommendations on their use depending on the type of procedure are presented). 4. - Radiation protection means (Based on ORAMED measurements and simulations results, a description of available RP means, shielding, type of syringe, distance, time are shown; first recommendations are presented). 5. - Guidelines, recommendations to optimize radiation protection (summary of previous observations) To confirm knowledge, several questions are introduced in the presentation. When available they can be used with interactive systems.

CHAPTER 1: INTRODUCTION / REVISION

Nuclear medicine definition Nuclear medicine is a branch of medicine dealing with the use of (un-sealed) radioactive materials in the diagnosis and treatment of disease. Ref: Merriam-Webster's Medical Dictionary, © 2007 Merriam-Webster, Inc.

Most common radionuclides in nuclear medicine For diagnostic Gamma emitters 99 m. Tc, 111 In, 123 I, 131 I, 201 Tl, 133 X, … + emitters (and annihilation photons) 18 F, 11 C, 13 N, 15 O, (64 Cu, 82 Rb, 86 Y, 124 I, …) For therapy - emitters 90 Y, 131 I, 32 P, 89 Sr, 153 Sm, 169 Er, 177 Lu, 186 Re, …
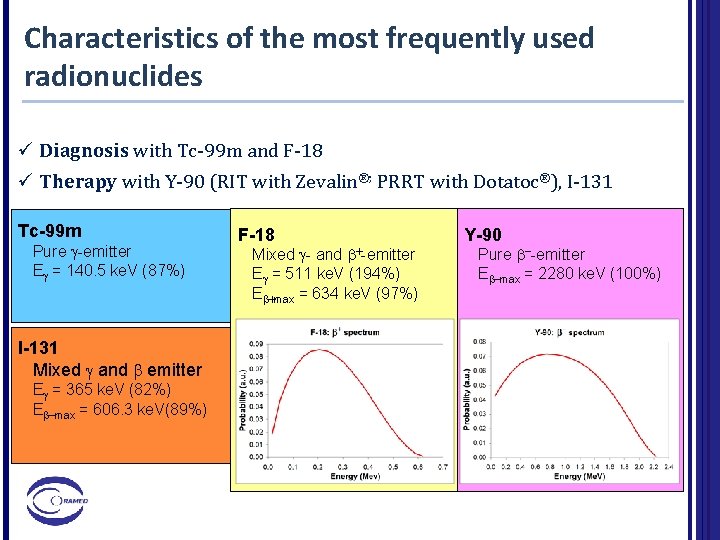
Characteristics of the most frequently used radionuclides ü Diagnosis with Tc-99 m and F-18 ü Therapy with Y-90 (RIT with Zevalin®; PRRT with Dotatoc®), I-131 Tc-99 m Pure g-emitter Eg = 140. 5 ke. V (87%) I-131 Mixed g and emitter Eg = 365 ke. V (82%) E -max = 606. 3 ke. V(89%) F-18 +-emitter Mixed g- and Eg = 511 ke. V (194%) E +max = 634 ke. V (97%) Y-90 Pure --emitter E -max = 2280 ke. V (100%)

Radionuclides characteristics Q 1. Typical activities per patient per diagnostic procedures are of the order of 500 MBq for Tc-99 m, 400 MBq for F-18. For Y-90 therapy the activity is 1 GBq. Which is the dose rate in contact of a 5 ml unshielded syringe? A. The lowest dose-rate is for Y-90. B. For Y-90 is 34 times larger than for Tc-99 m and 5 times larger than for F-18. C. The largest dose-rate is for F-18. D. The largest dose-rate is for Y-90, then for Tc-99 m and finally for F-18.
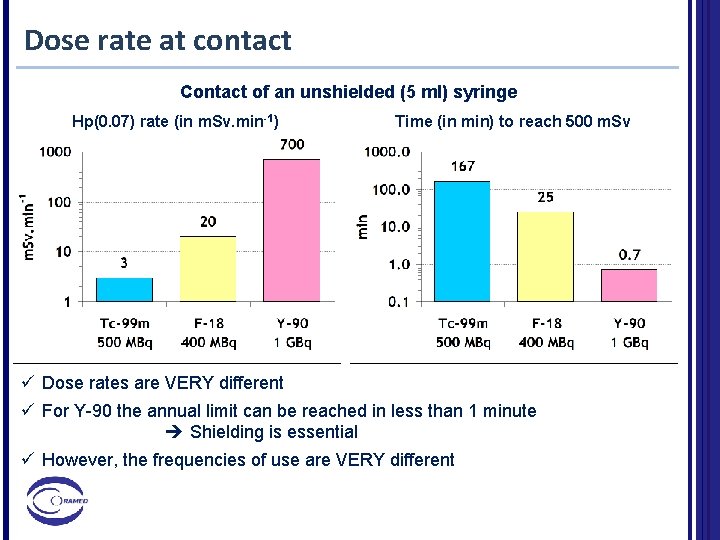
Dose rate at contact Contact of an unshielded (5 ml) syringe Hp(0. 07) rate (in m. Sv. min-1) Time (in min) to reach 500 m. Sv ü Dose rates are VERY different ü For Y-90 the annual limit can be reached in less than 1 minute Shielding is essential ü However, the frequencies of use are VERY different

Radionuclides characteristics Q 2. As regards the range/penetration of the most typical radiopharmaceuticals. Which is the correct statement? A. The half-value layer in tissue of F-18 is of the order of 7. 5 cm. . B. The half-value layer in tissue for Tc-99 m is of the order of 2 cm. C. The range of Y-90 in tissue is of the order of 5 cm. D. The range of Y-90 in air is of the order of 10 cm.
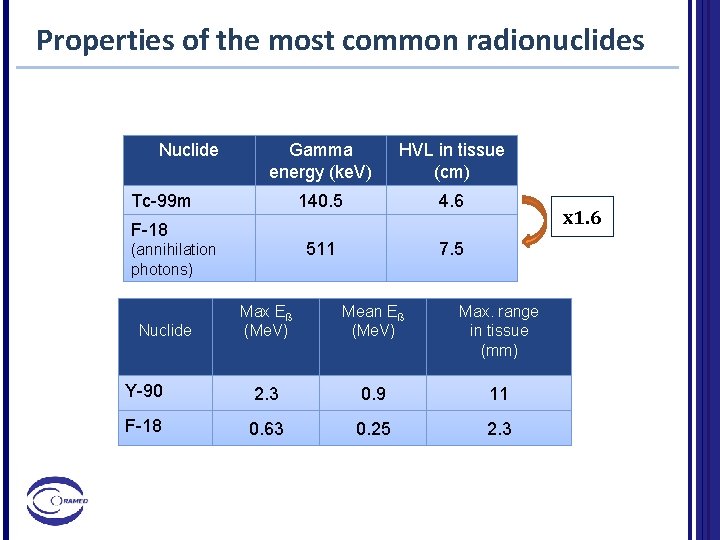

Properties of the most common radionuclides Nuclide Gamma energy (ke. V) HVL in tissue (cm) 140. 5 4. 6 511 7. 5 Tc-99 m F-18 (annihilation photons) x 1. 6 Max Eß (Me. V) Mean Eß (Me. V) Max. range in tissue (mm) Y-90 2. 3 0. 9 11 F-18 0. 63 0. 25 2. 3 Nuclide

Dose limits Q 3. As regards the dose limits for extremity dosimetry in nuclear medicine Which is the correct statement? A. No need for routine extremity monitoring , dose limit is never reached. B. The annual dose limit for the skin is 20 m. Sv averaged over 1 cm 2 C. The annual dose limit for the skin is 500 m. Sv averaged over 1 cm 2 D. The annual dose limit for the skin is 500 m. Sv averaged over the hand

Dose limits for the extremities ICRP 60 recommendations : Annual equivalent dose in the skin 500 m. Sv for 12 months averaged over 1 cm 2 area regardless of the exposed surface European directive 96/29: All workers likely to receive an extremity dose larger than 3/10 of the annual limit dose must wear an extremity dosemeter

CHAPTER 2: RADIOLOGICAL RISKS Staff
Radiological risks: Sources of exposure of nuclear medicine workers Nuclear medicine implies the manipulation of unsealed radioactive sources §Risk of internal contamination • Valid for all radionuclides and specially for iodine (volatile) and. . . D 0 / 202

Radiological risks: Sources of exposure of nuclear medicine workers §Risk of external irradiation • Whole body (WB) and extremities irradiation when manipulating radioactive sources Generator Elution vial Labelling with Tc-99 m Labelling vial Injection in diagnostics The hands are particularly exposed in nuclear medicine • Whole body irradiation from the patient

Radiological risks Q 4. As regards nuclear medicine technologists’ annual dose, the main source of exposure, compared with annual limits is related to : A. The WB exposure during preparation and administration of radiopharmaceuticals. B. The WB exposure when assisting and accompanying the patient. C. The extremity exposure during preparation and administration of radiopharmaceuticals. D. The extremity exposure when assisting and accompanying the patient.
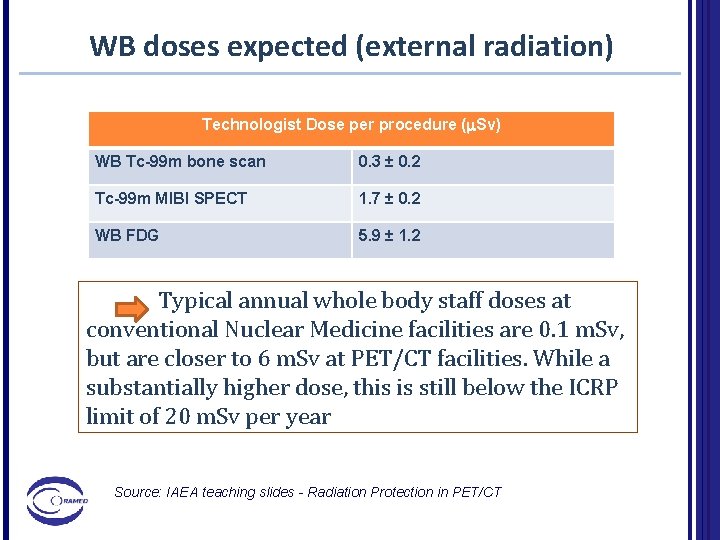

WB doses expected (external radiation) Technologist Dose per procedure (m. Sv) WB Tc-99 m bone scan 0. 3 ± 0. 2 Tc-99 m MIBI SPECT 1. 7 ± 0. 2 WB FDG 5. 9 ± 1. 2 Typical annual whole body staff doses at conventional Nuclear Medicine facilities are 0. 1 m. Sv, but are closer to 6 m. Sv at PET/CT facilities. While a substantially higher dose, this is still below the ICRP limit of 20 m. Sv per year Source: IAEA teaching slides - Radiation Protection in PET/CT
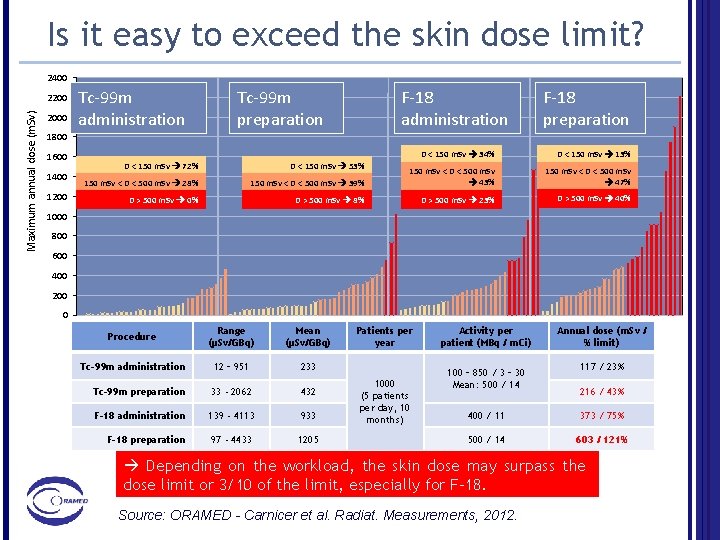
Is it easy to exceed the skin dose limit? 2400 Maximum annual dose (m. Sv) 2200 2000 Tc-99 m administration Tc-99 m preparation F-18 administration F-18 preparation 1800 1600 1400 1200 D < 150 m. Sv 34% D < 150 m. Sv 13% 150 m. Sv < D < 500 m. Sv 39% 150 m. Sv < D < 500 m. Sv 43% 150 m. Sv < D < 500 m. Sv 47% D > 500 m. Sv 8% D > 500 m. Sv 23% D > 500 m. Sv 40% D < 150 m. Sv 72% D < 150 m. Sv 53% 150 m. Sv < D < 500 m. Sv 28% D > 500 m. Sv 0% 1000 800 600 400 200 0 Procedure Range (µSv/GBq) Mean (µSv/GBq) Tc-99 m administration 12 – 951 233 Tc-99 m preparation 33 - 2062 432 F-18 administration 139 - 4113 933 F-18 preparation 97 - 4433 1205 Patients per year 1000 (5 patients per day, 10 months) Activity per patient (MBq / m. Ci) 100 – 850 / 3 – 30 Mean: 500 / 14 Annual dose (m. Sv / % limit) 117 / 23% 216 / 43% 400 / 11 373 / 75% 500 / 14 603 / 121% Depending on the workload, the skin dose may surpass the dose limit or 3/10 of the limit, especially for F-18. Source: ORAMED - Carnicer et al. Radiat. Measurements, 2012.

Radiological risks Q 5. What are the procedures at risk for nuclear medicine technologists in diagnostic nuclear medicine, regarding the doses to the extremities? For the same activity, the maximum skin dose. . . A. Is usually higher for the preparation of Tc-99 m than for the administration of F-18. B. Is usually higher for the preparation of F-18 than for the administration of F-18. Can be higher for the preparation of Tc-99 m than for the preparation of F-18. D. All are correct.
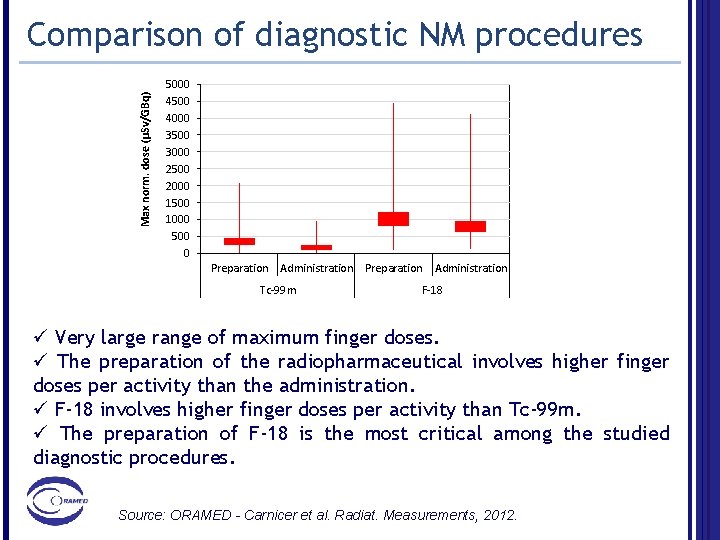
Max norm. dose (µSv/GBq) Comparison of diagnostic NM procedures 5000 4500 4000 3500 3000 2500 2000 1500 1000 500 0 Preparation Administration Tc-99 m Preparation Administration F-18 ü Very large range of maximum finger doses. ü The preparation of the radiopharmaceutical involves higher finger doses per activity than the administration. ü F-18 involves higher finger doses per activity than Tc-99 m. ü The preparation of F-18 is the most critical among the studied diagnostic procedures. Source: ORAMED - Carnicer et al. Radiat. Measurements, 2012.
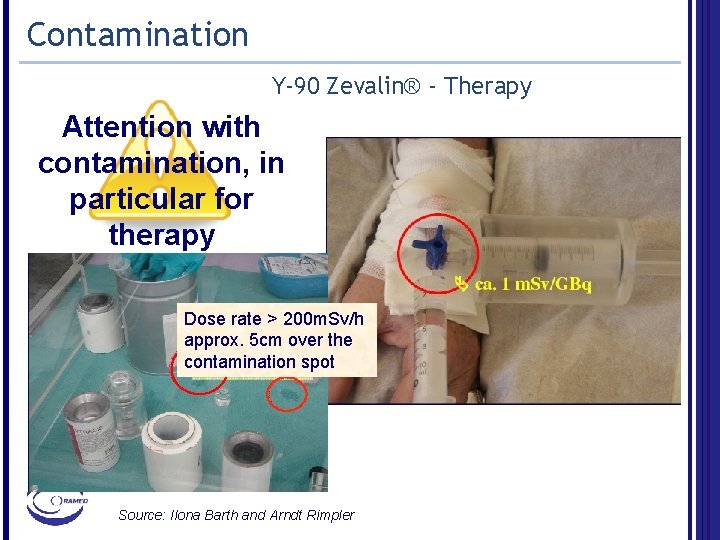
Contamination Y-90 Zevalin® - Therapy Attention with contamination, in particular for therapy Dose rate > 200 m. Sv/h approx. 5 cm over the contamination spot Source: Ilona Barth and Arndt Rimpler

CHAPTER 3: STAFF MONITORING 24
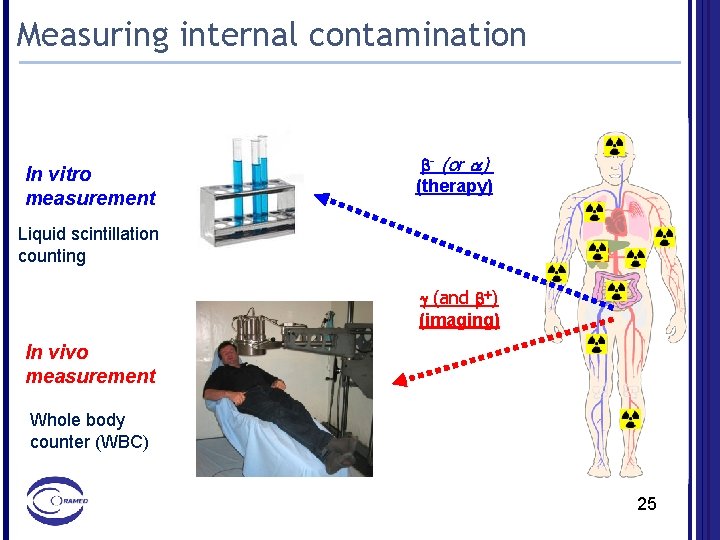
Measuring internal contamination In vitro measurement b- (or a) (therapy) Liquid scintillation counting g (and b+) (imaging) In vivo measurement Whole body counter (WBC) 25

Routine external monitoring Routine whole body monitoring with TLDs Quantity to be measured Hp(10) Extremity routine monitoring with TLDs Quantity to be measured Hp(0, 07) In practice ring or wrist dosemeter are used Should be worn at the most exposed position in the hands 26

Type of TLD Ø Whenever one can be sure that the workplace does not include lowenergy beta particles, the use of TLD-100 would be advisable because of its better performance and ease of use (1). ØIf the contribution of positrons to Hp(0. 07) for PET workers cannot be neglected. Thin TL detectors, such as MCP-Ns, are more appropriate for this type of dosimetric application. If thin TL detectors are not used, an underestimation of the order of 30% could be envisaged for 18 F handling. This difference should be added to the underestimation of Hp(0. 07) because of the position of the dosemeter (2). (1) Ginjaume et al. Comparison of two extremety dosemeters based on Li. F: Mg, Cu, P thin detectors for mixed beta-gamma fields. Radiat. Prot. Dosim. 120, No. 1 -4, 316– 320 (2006). (2) Ginjaume et al. Comparison of TLD-100 and MCP-Ns for use as an extremity dosemeter for PET nuclear medicine staff. Radiat. Prot. Dosim. 43, 607– 610 (2008). 27

Staff monitoring Q 6. Which statement would you consider if you were to recommend some type of extremity dosemeter for nuclear medicine workers? A. - The ring dosemeter always provides a higher dose reading. Use a ring dosemeter. B. – You can use either a ring or a wrist dosemeter. But it is important to use 2 dosemeters. C. - There are no significant differences between wrist and ring. Use a wrist dosemeter in the dominant hand (right) because it is more confortable. D. -There are no significant differences between wrist and ring. Use a wrist dosemeter in the non dominant hand (left). 28
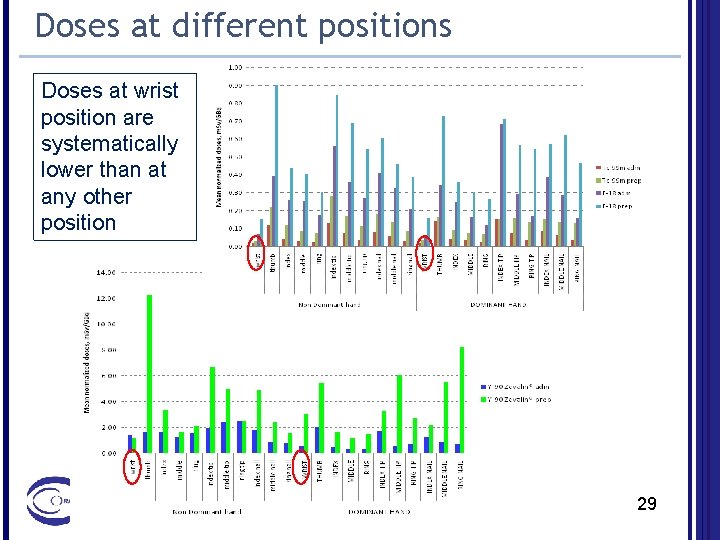
Doses at different positions Doses at wrist position are systematically lower than at any other position 29

Staff monitoring The ring dosemeter is recommended to the wrist dosemeter in nuclear medicine. Q 7. In which position should it be worn? A. Base of the ring finger of dominant hand (external side) B. Base of the ring finger of dominant hand (palm side) C. Base of the index finger of non-dominant hand (external side) D. Base of the index finger of non-dominant hand (palm side) 30

Staff monitoring The ring dosemeter should be worn as close as possible to the most exposed part of the hand. However this is not easy to do in practice. Q 8. How much do you underestimate the maximum skin dose when monitoring it with a ring dosemeter worn in the base of the index (palm side) non-dominant hand? A. You don’t underestimate. B. Up to a factor of 2 C. Around a factor of 6 D. Around a factor of 10 E. Up to a factor of 100 when you manipulate beta sources. 31
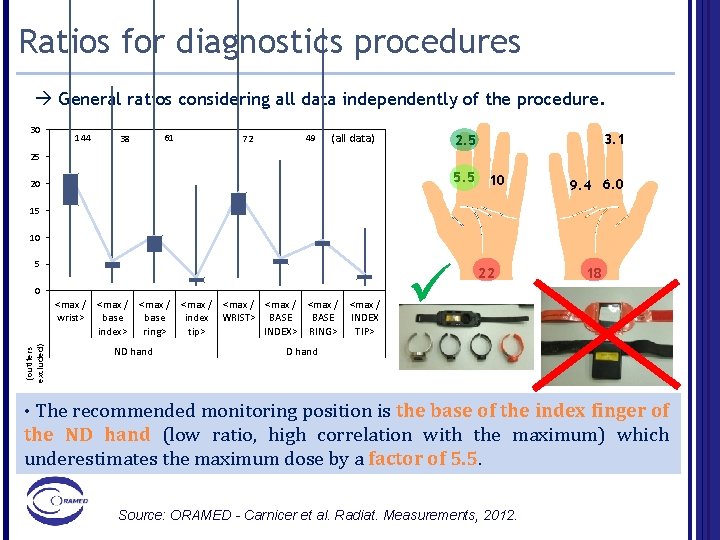
Ratios for diagnostics procedures General ratios considering all data independently of the procedure. 30 144 61 38 72 49 (all data) 3. 1 2. 5 25 5. 5 10 20 9. 4 6. 0 15 10 5 0 (outliers excluded) <max / wrist> <max / base index> <max / base ring> ND hand <max / index WRIST> BASE tip> INDEX> RING> <max / INDEX TIP> ü 22 18 D hand The recommended monitoring position is the base of the index finger of the ND hand (low ratio, high correlation with the maximum) which underestimates the maximum dose by a factor of 5. 5. • Source: ORAMED - Carnicer et al. Radiat. Measurements, 2012.
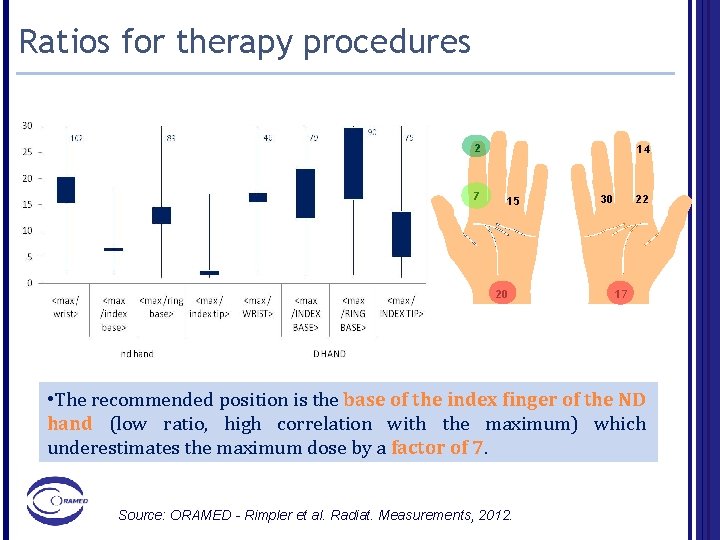
Ratios for therapy procedures 2 7 14 15 20 30 22 17 • The recommended position is the base of the index finger of the ND hand (low ratio, high correlation with the maximum) which underestimates the maximum dose by a factor of 7. Source: ORAMED - Rimpler et al. Radiat. Measurements, 2012.

CHAPTER 4: RADIATION PROTECTION MEANS 34

Radiation protection means How to reduce the skin dose? Q 9. What are the 3 most important parameters (in order of importance) influencing the maximum skin dose in nuclear medicine? A. Distance – Shielding – Dose monitoring B. Distance – Time – Shielding C. Shielding – Distance - Training D. All of the above 35
3 basic principles in Radiation protection • Shielding • Distance • Time (training) 36

Shielding Personal Protective equipment Syringe shield Vial Shield Lead gloves Room Protective Equipment Lead box Activimeter in the lead box 37
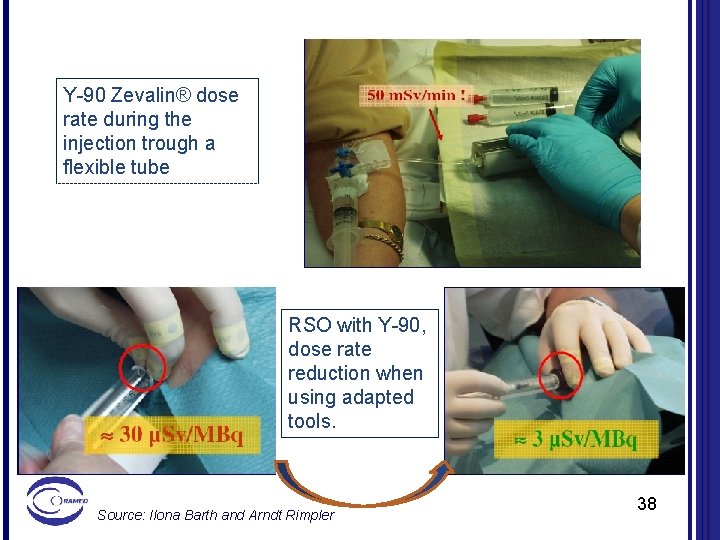
Y-90 Zevalin® dose rate during the injection trough a flexible tube RSO with Y-90, dose rate reduction when using adapted tools. Source: Ilona Barth and Arndt Rimpler 38

Radiation Protection means Q 10. Concerning shielding when injecting a radiopharmaceutical. . A. All shieldings have the same reduction factor independently of the radionuclide B. No need of shielding since the injection procedure is fast C. 2 mm Tungsten and 3 mm lead are equivalent for 99 m. Tc D. 5 mm of tungsten is the minimum required shielding 99 m. Tc 39
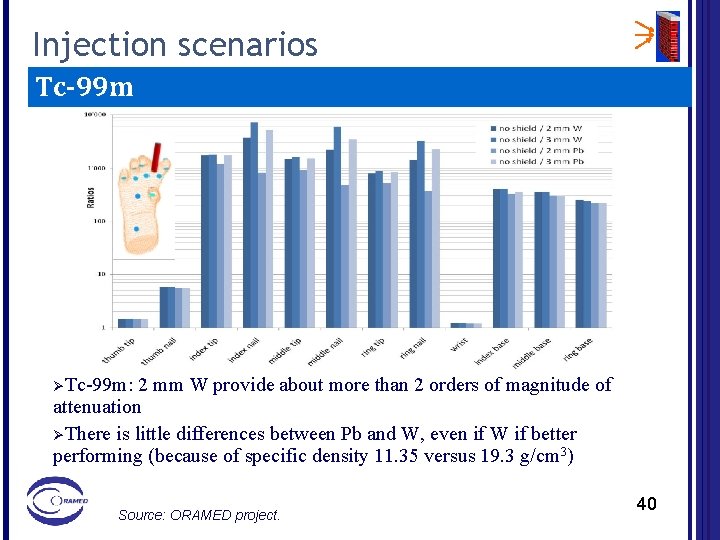
Injection scenarios Tc-99 m ØTc-99 m: 2 mm W provide about more than 2 orders of magnitude of attenuation ØThere is little differences between Pb and W, even if W if better performing (because of specific density 11. 35 versus 19. 3 g/cm 3) Source: ORAMED project. 40
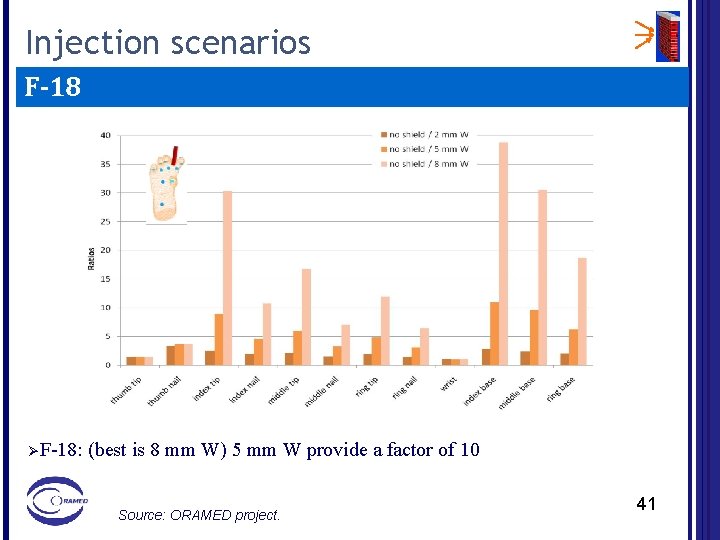
Injection scenarios F-18 ØF-18: (best is 8 mm W) 5 mm W provide a factor of 10 Source: ORAMED project. 41
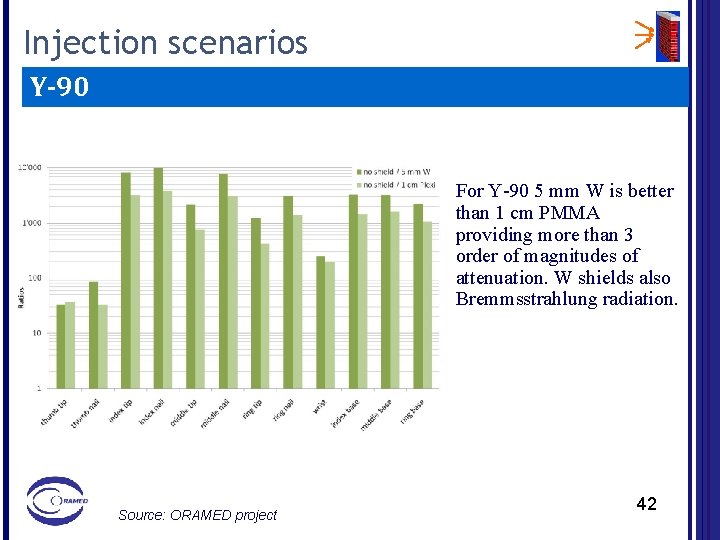
Injection scenarios Y-90 For Y-90 5 mm W is better than 1 cm PMMA providing more than 3 order of magnitudes of attenuation. W shields also Bremmsstrahlung radiation. Source: ORAMED project 42
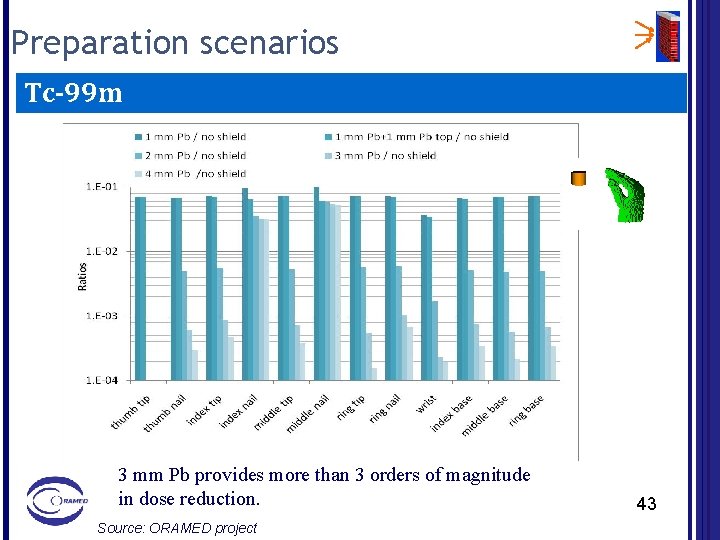
Preparation scenarios Tc-99 m 3 mm Pb provides more than 3 orders of magnitude in dose reduction. Source: ORAMED project 43
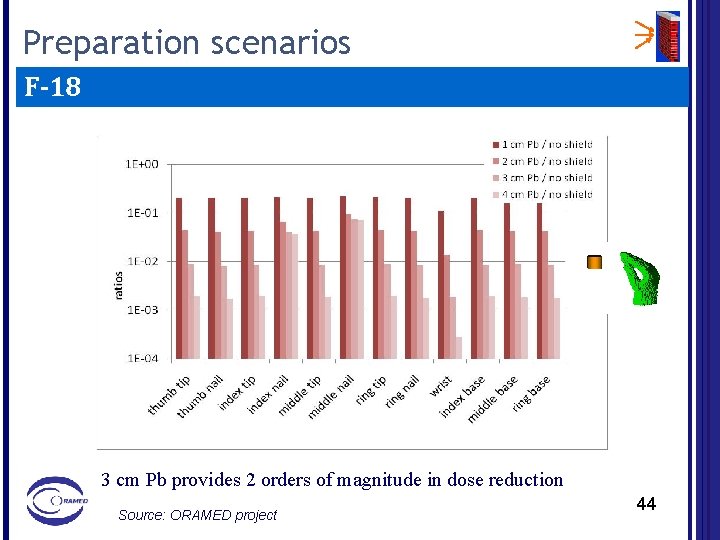
Preparation scenarios F-18 3 cm Pb provides 2 orders of magnitude in dose reduction Source: ORAMED project 44
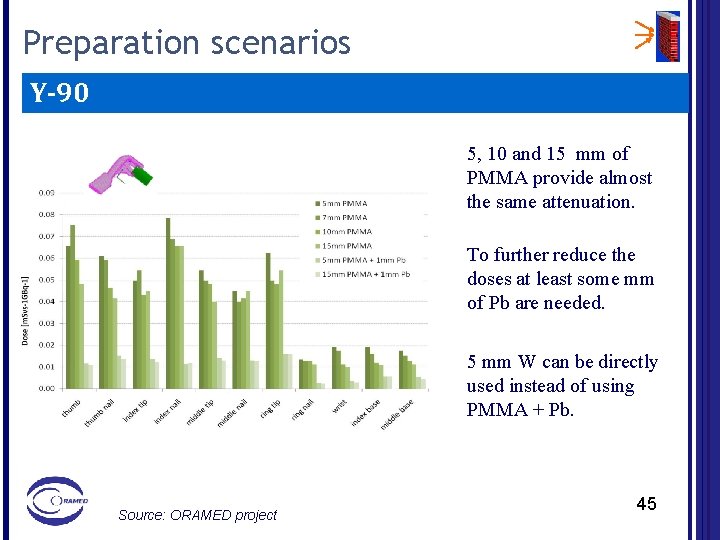
Preparation scenarios Y-90 5, 10 and 15 mm of PMMA provide almost the same attenuation. To further reduce the doses at least some mm of Pb are needed. 5 mm W can be directly used instead of using PMMA + Pb. Source: ORAMED project 45

Summary shielding recommendations For the injection (syringe shielding): Ø 2 mm W (or Pb) for Tc-99 m give a dose reduction of at least 2 order of magnitudes; Ø 5 mm W provides up to a factor 10 in dose reduction for F-18 (8 mm W up to a factor 40). For Y-90 10 mm PMMA completely shield beta radiation, nevertheless 5 mm shielding of tungsten provides a better shielding cutting down bremsstrahlung radiation too. Ø For the preparation (vial shielding): ØFor F-18, 3 cm of Pb provides 2 order of magnitudes on dose reduction. The same attenuation for Tc-99 m is obtained with 2 mm Pb. Ø For Y-90 an acceptable shielding is obtained with 10 mm PMMA with an external layer of few mm of lead or alternatively 5 mm of W. 46
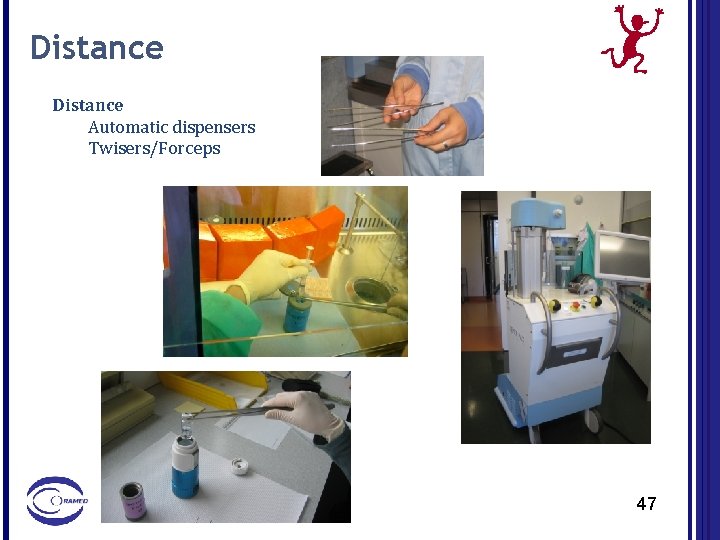
Distance Automatic dispensers Twisers/Forceps 47
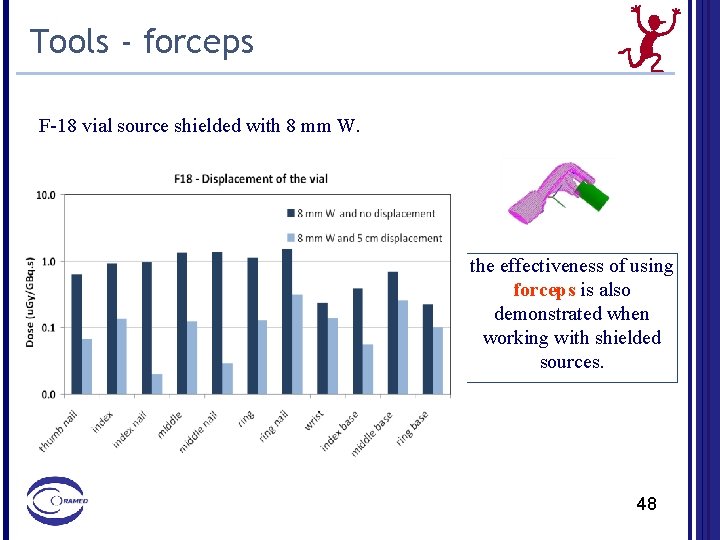
Tools - forceps F-18 vial source shielded with 8 mm W. the effectiveness of using forceps is also demonstrated when working with shielded sources. 48

Radiation Protection means When handling an Y-90 syringe for RTPE the position of the fingers is very important. The dose rate along the syringe varies dramatically. . Q 11. How many times can the doses at the fingers be reduced if the contact with the shielded syringe is in position A (no pharmaceutical, below)? C A. More than 1500 from B to A B. Up to a factor of 100 times from B to A C. Up to a factor of 1000 times from C to A D. More than 10000 times from C to A E. (A) and (D) are correct B A 49

Dose rates (in m. Sv/h) at the different positions in a syringe filled with Y-90 50

Time It is very difficult to correctly estimate the influence of time to a complete procedure, especially for the preparation of radiopharmaceuticals. (Different steps, very different dose rates in each step, usually for trained workers, the use of shield or the distance are parameters more determinant). 51

Radiation Protection means Q 12. How many years of experience a worker needs to keep his annual maximum hand dose below the annual limit of 500 m. Sv? A. More than 1 year B. After 6 months the worker has acquired enough experience C. Minimum 5 years D. The experience is not always related to low doses 52
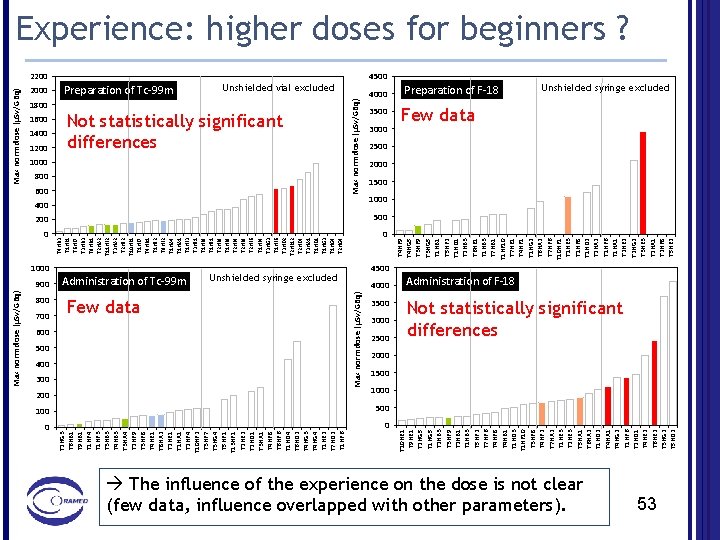
1200 900 800 700 Not statistically significant differences 1000 800 600 400 1000 Administration of Tc-99 m Unshielded syringe excluded Few data 600 500 400 300 200 4000 3500 3000 200 500 0 0 4000 3500 3000 2500 100 500 0 0 T 4 HF 9 T 4 HG 5 T 3 HF 9 T 3 HG 5 T 1 HB 1 T 5 HF 2 T 1 HD 1 T 2 HB 3 T 6 HE 1 T 1 HB 3 T 7 HB 1 T 1 HF 10 T 7 HE 1 T 4 HF 1 T 1 HG 2 T 6 HA 2 T 7 HF 6 T 10 HF 1 T 1 HE 3 T 1 HF 8 T 1 HD 2 T 2 HA 2 T 1 HF 6 T 1 HA 1 T 2 HE 2 T 2 HG 2 T 3 HE 3 T 2 HA 1 T 2 HF 8 T 5 HE 2 1400 Unshielded vial excluded T 10 HE 1 T 9 HE 1 T 2 HG 5 T 1 HG 5 T 2 HB 3 T 3 HF 9 T 2 HB 1 T 1 HB 3 T 5 HF 2 T 7 HF 6 T 4 HF 8 T 4 HB 1 T 1 HD 3 T 1 HF 10 T 3 HF 8 T 4 HF 2 T 7 HA 2 T 1 HE 3 T 2 HE 3 T 5 HA 1 T 6 HA 2 T 1 HD 2 T 4 HA 1 T 4 HG 2 T 1 HF 6 T 2 HD 1 T 4 HE 2 T 6 HE 2 T 3 HG 2 T 5 HD 2 1600 Preparation of Tc-99 m Max norm dose (µSv/GBq) 2200 Max norm dose (µSv/GBq) 1800 T 4 HB 3 T 1 HF 1 T 6 HF 7 T 3 HB 3 T 8 HB 1 T 2 HA 2 T 11 HF 2 T 3 HA 2 T 2 HE 2 T 10 HF 1 T 1 HF 7 T 4 HB 1 T 1 HE 2 T 9 HF 2 T 1 HA 4 T 1 HA 1 T 1 HF 3 T 3 HE 1 T 1 HF 8 T 1 HE 1 T 2 HF 9 T 1 HF 9 T 2 HF 4 T 2 HF 8 T 2 HF 6 T 1 HF 4 T 3 HG 3 T 1 HF 6 T 3 HD 2 T 2 HF 12 T 2 HD 4 T 3 HA 1 T 1 HD 1 T 1 HG 3 T 1 HG 4 T 2 HG 4 Max norm dose (µSv/GBq) 2000 T 2 HG 3 T 6 HB 1 T 9 HB 1 T 1 HF 4 T 1 HF 3 T 3 HB 3 T 4 HB 3 T 3 HA 4 T 2 HF 9 T 3 HF 8 T 4 HE 1 T 8 HA 2 T 2 HE 1 T 1 HA 1 T 2 HF 4 T 10 HF 2 T 3 HF 7 T 3 HG 4 T 5 HF 1 T 13 HF 1 T 2 HE 2 T 2 HD 1 T 3 HA 1 T 4 HF 8 T 6 HF 6 T 1 HD 4 T 6 HD 2 T 4 HG 3 T 4 HG 4 T 1 HE 2 T 7 HD 2 T 1 HF 6 Max norm dose (µSv/GBq) Experience: higher doses for beginners ? 4500 Preparation of F-18 Unshielded syringe excluded Few data 2500 2000 1500 1000 4500 Administration of F-18 Not statistically significant differences 2000 1500 1000 The influence of the experience on the dose is not clear (few data, influence overlapped with other parameters). 53

ü The accumulated dose is directly proportional to the time. A reduction of 2 in time implies a reduction of 2 in doses. ü Training is very important to ensure a quick and correct handling of radiopharmaceuticals. However, experience is not always related with good training and good practice. There are cases of bad habits. 54

CHAPTER 5: SUMMARY RECOMMENDATIONS 55

General observations Ø Wide ranges of individual exposures (min/max) for similar procedures, different equipment, radiation protection means and tools. Ø Skin dose limit (500 m. Sv/y) can be exceeded by numerous workers in hospitals where RP standard is low Ø There is adequate potential to further improve radiation protection and decrease exposures Ø Adequate skin dose monitoring is urgently needed in nuclear medicine 56

What we have learned Ø The choice of TLD and TLD position is important for an adequate dose assessment Ø Shielding of vials and syringes are essential and a precondition but not a guarantee for low exposures. Ø Other RP tools and measures (e. g. pincers, forceps, time etc. ) significantly influence the exposure. Ø Also subjective factors e. g. risk awareness and training affect exposures. Especially in therapy, participants have reduced extremity dose during the project due to the feedback of the measurement results on the RP standard. Ø Working fast is often not sufficient 57
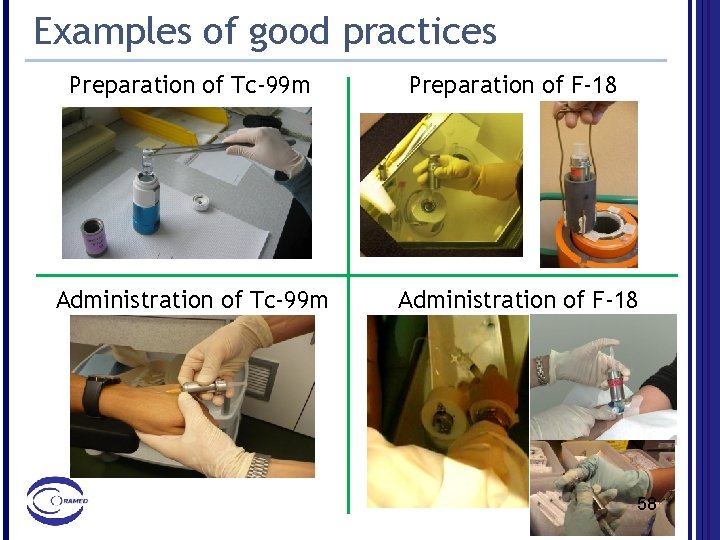
Examples of good practices Preparation of Tc-99 m Preparation of F-18 Administration of Tc-99 m Administration of F-18 58
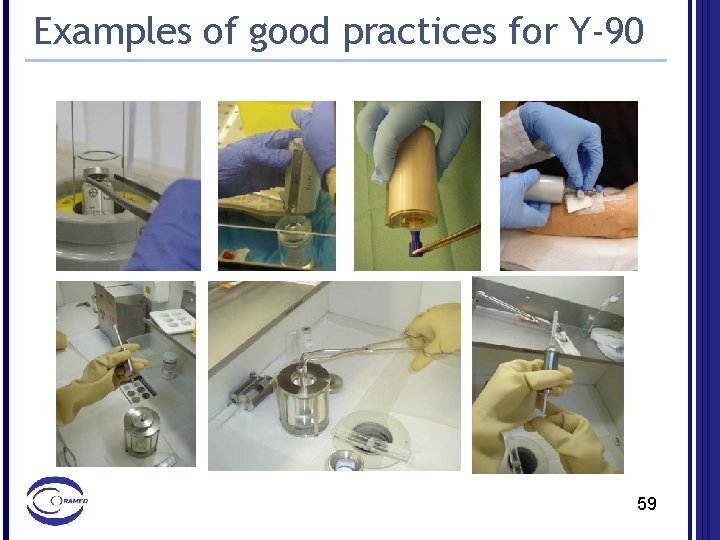
Examples of good practices for Y-90 59
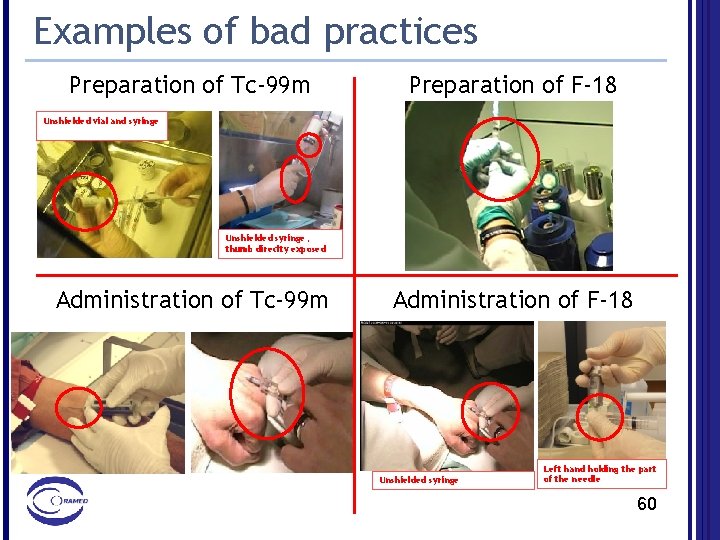
Examples of bad practices Preparation of Tc-99 m Preparation of F-18 Unshielded vial and syringe Unshielded syringe, thumb direclty exposed Administration of Tc-99 m Administration of F-18 Unshielded syringe Left hand holding the part of the needle 60

Examples of bad practices for Y-90 Example of bad RP practice The maximum skin dose for this worker is 52 times the mean of the 30 participants 61

Examples of bad practices for Y-90 The maximum skin dose for this worker is 16 times the mean of the 30 participants T 7 HF 2 62

Outcome The final outcome of the ORAMED project is to propose, on the basis of the results of measurement and simulation campaign performed, the guidelines in order to minimise radiation risk to medical staff in nuclear medicine. Directed to: • physicians • nurses • technicians • radiation protection officers • authorities in the field The following recommendations concern only radiation protection aspects.
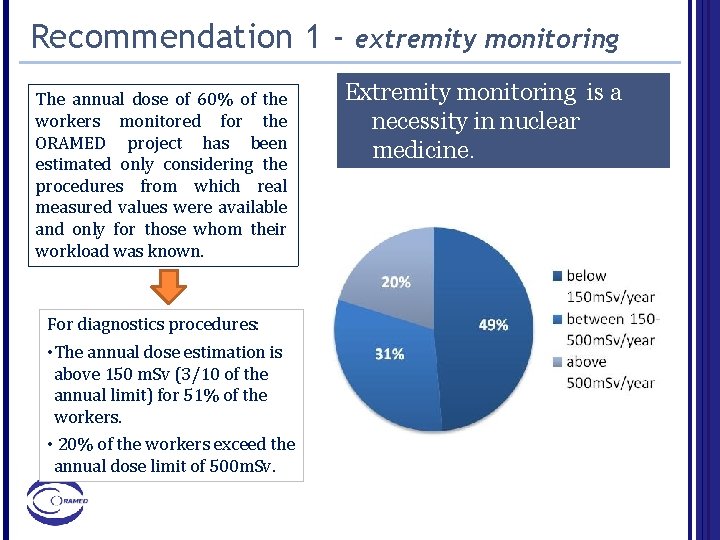
Recommendation 1 The annual dose of 60% of the workers monitored for the ORAMED project has been estimated only considering the procedures from which real measured values were available and only for those whom their workload was known. For diagnostics procedures: • The annual dose estimation is above 150 m. Sv (3/10 of the annual limit) for 51% of the workers. • 20% of the workers exceed the annual dose limit of 500 m. Sv. extremity monitoring Extremity monitoring is a necessity in nuclear medicine.

Recommendation 2 - routine monitoring The base of the index finger of the non dominant hand with the detector (TLD) placed towards the inside of the hand is the recommended position for routine extremity monitoring in nuclear medicine. 30 144 38 61 72 49 25 (all data) 20 15 10 5 0 Best monitoring position: index tip of the non dominant hand BUT not feasible for routine monitoring with ring dosemeters <max / <max / wrist> base index WRIST> BASE INDEX index> ring> tip> INDEX> RING> TIP> ND hand Recommended monitoring position: base index finger of non dominant hand with TLD directed to the inner side • low ratio • high correlation with the maximum • comfortable for manipulating
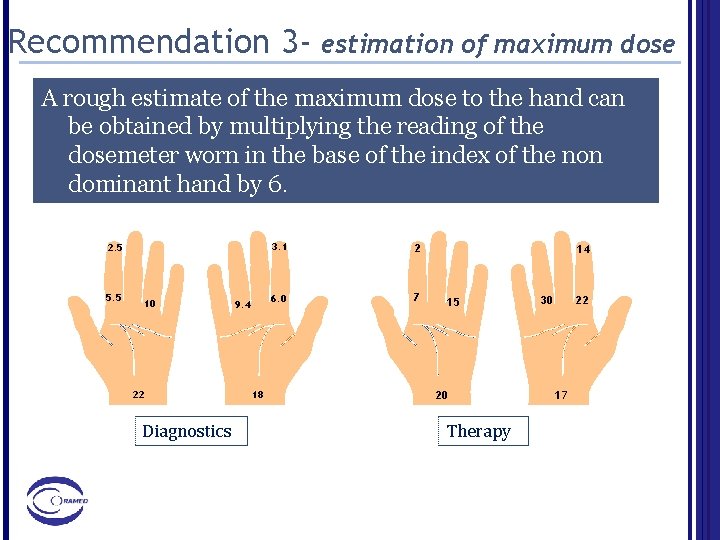
Recommendation 3 - estimation of maximum dose A rough estimate of the maximum dose to the hand can be obtained by multiplying the reading of the dosemeter worn in the base of the index of the non dominant hand by 6. 2. 5 5. 5 10 22 Diagnostics 9. 4 18 3. 1 2 6. 0 7 14 15 20 Therapy 30 22 17
Recommendation 4 - shielding Shielding of vials and syringes are essential and a precondition but not a guarantee for low exposures.

Recommendation 5 – minimum syringe shield The minimum acceptable shielding required for a syringe is 2 mm of tungsten for 99 m. Tc and 5 mm of tungsten for 18 F. For 90 Y 10 mm PMMA completely shield beta radiation, nevertheless 5 mm shielding of tungsten provides a better shielding cutting down bremsstrahlung radiation too.

Recommendation 6 – minimum vial shield The minimum acceptable shielding required for a vial is 3 mm and 3 cm lead for 99 m. Tc and 18 F respectively. For 90 Y an acceptable shielding is obtained with 10 mm PMMA with an external layer of few mm of lead.

Recommendation 7 – training and education Training and education on good practice (e. g. procedure planning, repeating procedures using non radioactive sources) are more relevant parameters than the experience of the worker. Procedure planning: preparation of tools, estimation of doses to be received (dose estimation tool), first trial with inactive sources.
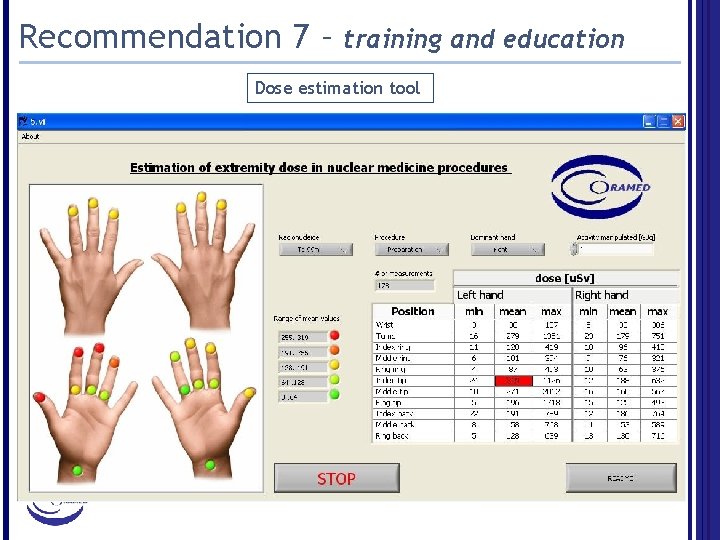
Recommendation 7 – training and education Dose estimation tool

Recommendation 8 – radiation protection tools All tools increasing the distance (e. g. forceps) between the hand/finger and the source are very effective for dose reduction. the effectiveness of using forceps is also demonstrated when working with shielded sources.

Recommendation 9 – time Working fast is not sufficient, the use of shields or increasing the distance are more effective than pushing on the working speed. It is very difficult to correctly estimate the influence of time on the dose during a complete procedure, especially for the preparation of radiopharmaceuticals. Different steps, very different dose rates in each step, usually for trained workers the use of shields or increasing the distance are more effective than pushing on the working speed.

Recommendations (summary 1/2) 1. Extremity monitoring is a necessity in nuclear medicine. 2. The base of the index finger of the non dominant hand with the detector (TLD) placed towards the inside of the hand is the recommended position for routine extremity monitoring in nuclear medicine. 3. A rough estimate of the maximum dose to the hand can be obtained by multiplying the reading of the dosemeter worn in the base of the index of the non dominant hand by 6. 4. Shielding of vials and syringes are essential and a precondition but not a guarantee for low exposures. 5. The minimum acceptable shielding required for a syringe is 2 mm of tungsten for 99 m. Tc and 5 mm of tungsten for 18 F. For 90 Y 10 mm PMMA completely shield beta radiation, nevertheless 5 mm shielding of tungsten provides a better shielding cutting down bremsstrahlung radiation too.

Recommendations (summary 2/2) 6. The minimum acceptable shielding required for a vial is 3 mm and 3 cm lead for 99 m. Tc and 18 F respectively. For 90 Y an acceptable shielding is obtained with 10 mm PMMA with an external layer of few mm of lead. 7. Training and education on good practice (e. g. procedure planning, repeating procedures using non radioactive sources) are more relevant parameters than the experience of the worker. 8. All tools increasing the distance (e. g. forceps) between the hand/finger and the source are very effective for dose reduction. 9. Working fast is not sufficient, the use of shields or increasing the distance are more effective than pushing on the working speed.

ACKNOWLEDG MENTS Special thanks to all the workers and hospitals that have collaborated Acknowledgment to the European Atomic Energy Community's Seventh Framework Programme for funding the ORAMED project under grant agreement n° 211361.
- Slides: 76