BAKERS CYST Dr Isstelle Joubert 2 nd yr

BAKER’S CYST Dr Isstelle Joubert 2 nd yr M Sports and Exercise Medicine September 2012

PATIENT COMPLAINT • Mr. CG, 27 yo • rugby player playing lock forward – 1 st team, senior club level • pain at medial aspect of left knee – 6/52 Hx • pain progressed last 3/52 - VAS 6 -7/10

PATIENT COMPLAINT: PAI N • gradual in onset • daily when standing or sitting for extended periods • irritated when driving long distances: knee flexed • aggravated: bending to engage in scrums • relieved with occasional NSAIDs - returned within day

PATIENT COMPLAINT: • slight instability in L knee • “fullness”, especially in fully flexed position • mid-season - over-reaching during period before onset of pain • playing surfaces – not changed • footwear – not changed

PREVIOUS HISTORY: q partial tear in ACL of L knee – 2 seasons before • Rx: conservative, limited ROM brace • no meniscal injuries q No other medical history

CLINICAL EVALUATION: q Observation: • standing + supine: ü visible diffuse swelling ü postero-lateral aspect of popliteal fossa of L leg • walking: not much change in size / position • swelling visible bilateral to patellar tendon ant

CLINICAL EVALUATION: q Active movements • straight leg raise: normal • knee extension, flexion, tibial rotation: normal ROM • some discomfort: ü on full extension ü medially with tibial rotation ü “fullness”: knee full flexed position

CLINICAL EVALUATION: q Passive movements • extension, flexion, tibial rotation: minimal discomfort • hamstring stretch testing: marked discomfort • quad stretch testing: normal • Ober’s test: normal q Resisted movements • tibial rotation, knee flexion: marked discomfort

CLINICAL EVALUATION: q Functional testing • squatting and forward lunge: cause discomfort • jumping, hopping, stepping up and down step: normal

CLINICAL EVALUATION: q Palpation • gluteus medius: no trigger points • patellar tapping: mild ballotability - small effusion • patella glide test (all directions): no pain • palpation of patellar fat pad: normal • no synovial plica palpable • patella tracked perfectly within femoral trochlea • both VMO muscles palpated evenly in mass

CLINICAL EVALUATION: q Palpation • posterior popliteal fossa: diffuse swelling noted • direct pressure: ü elicited pain, mainly centrally in fossa ü radiated towards medial aspect of knee to point of pes anserinus bursa • not pulsating • auscultation: no vascular bruits
CLINICAL EVALUATION: q Special maneuvers • Stability testing for MCL and LCL: normal • Lachman’s test • Anterior Drawer test normal bilateral = ACL normal • Pivot Shift tests • Posterior Drawer test + with External Rotation reproduced pain - stability normal acc to R side • no posterior sagging

CLINICAL EVALUATION: • Reverse Lachman: negative - normal PCL • Patellar Apprehension testing: negative • Medial and Lateral Translations: not reproduce pain ? ? medial discomfort medial meniscus • Appley’s Posterior Grind test aspect of knee pathology • Mc. Murray’s test • Tell Sally test: marked discomfort on medial rotation

CLINICAL EVALUATION: q Referred Pain testing • Slump test no • Neural Thomas Stretch test pain • Straight Leg Raise with added Dorsiflexion q Lumbar Spine • Palpation + assessment: no pathology

CLINICAL EVALUATION: q Biomechanical Assessment • failed to show any signs of biomechanical problems predisposing to pain in L knee

DIFFERENTIAL DIAGNOSIS
• Baker’s Cyst • Pes Anserinus Bursitis • Torn Popliteus Muscle / Popliteus Tendinopathy • Hamstring Insertional Tendinopathy • Medial Meniscus Tear • Posterior Cruciate Sprain • Gastrocnemius Tendinopathy • Synovial Plica
SPECIAL INVESTIGATIONS

SPECIAL INVESTIGATIONS q Soft tissue Ultra-sound • large cystic mass - typical of Baker’s cyst • centrally in popliteal fossa • extending medially towards medial collateral lig area q X-rays • no abnormalities detected

SPECIAL INVESTIGATIONS q MRI • oval shaped, multi-lobulated cyst • medial in fossa • small neck: between medial gastroc head and semi-membranosis tendons • pressure on Pes Anserinus bursa • size: ü axially 36 x 15 mm ü cross sectionally 35 mm
SPECIAL INVESTIGATIONS • no free fluid accumulation in knee joint • no bone marrow edema or contusion • medial and lateral menisci: normal, no tears • medial and lateral collateral ligaments: normal • anterior and posterior cruciate ligaments: normal • quadriceps tendon, patellar tendon, other: normal

3 STAGE SUMMARY

3 STAGE SUMMARY q Biological / Clinical • Baker’s cyst due to unknown cause q Personal / Psychological • away from work due to post-operative pain • might be a career-ending injury q Social / Contextual • letting his team down mid-season

PROBLEM LIST

PROBLEM LIST q Active • Baker’s cyst with Pes Anserinus Bursa pressure • surgical repair indicated q Passive • None at this stage

PLAN & PROGRESSION

PLAN • patient discussed with orthopedic surgeon • plan: formal excision of cyst • surgery done in July 2012 • cyst found to be much larger than on MRI report

PROGRESSION • discharged 1 -day post-op with Robert Jones bandage • referred to physiotherapist • walking crutches for 5 days • during this period physiotherapist: ü isometric contraction exercises ü proprioceptive work replaces the multilayered system used not to fully extend knee – until ROS (day 8 post-op) with the traditional 'Robert scar fully healed Jones Dressing' • instructions: ü ü

PROGRESSION q Week 2 post-op: • physiotherapist: with Range of Motion (ROM) exercises • aim: to re-establish full knee extension ü active assisted knee slides against wall ü progressed to knee flexor stretching ü using sport cord and knee flexor stretch against a wall • after full ROM: ü active cycling to maintain aerobic fitness ü Isotonic Open-Chain-Kinetic Exercise - straight leg raises

PROGRESSION q Week 3 post-op: • Closed-Kinetic-Chain Strengthening Exercises • initial mini squats performed in 0 -40 degree range • progressing to standing wall slides • followed by straight line lunges • lunges done at different angles

PROGRESSION q Week 4 post-op: • start light leg presses in gym • incorporation of plyometric exercises q Week 5 post-op: • discharged to biokineticist • aim: ü maintain strength, proprioception and flexibility ü testing to return to play
Baker’s Cyst Discussion

DEFINITION • synovial fluid filled mass • in popliteal fossa • enlarged bursa located beneath medial head of gastroc + semimembranosus muscles • type of chronic knee joint effusion: herniates between two heads of gastroc Brukner & Khan, 2012

DEFINITION • 1 st Baker’s cyst: diagnosed in 1840 (dr Adams) • Dr William Morrant Baker ü 1877, (37 y later – published paper) ü 8 pt’s: peri-articular cysts caused by synovial fluid from knee joint new sac outside joint space ü associated with underlying conditions ü osteo-arthritis (OA) & Charcoat’s joints Baker, 1994

INCIDENCE

INCIDENCE • 2 peaks of age-incidence: 4 -7 y and 35 -70 y (Handy, 2001) • general population: 10 -41% (Janzen et al, 1994) • depends on diagnostic imaging: ü 5 -40% (MRI) in pt with OA or ? internal derangement ü 23 -32% with arthrography in similar population (Fielding et al, ‘ 91; Sansone et al, ‘ 95; Miller et al, ‘ 96; Hayashi et al, ‘ 10) • common associated meniscal lesions (83%) ü 43% were associated with articular cartilage damage ü 32% associated with ACL tears (Sansone et al 1995)
PATHO-PHYSIOLOGY
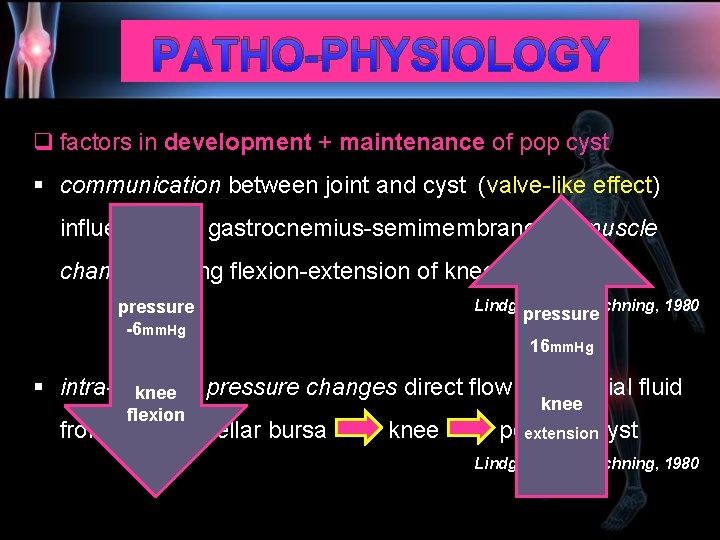
PATHO-PHYSIOLOGY q factors in development + maintenance of pop cyst § communication between joint and cyst (valve-like effect) influenced by gastrocnemius-semimembranosus muscle changes during flexion-extension of knee pressure -6 mm. Hg Lindgren & Rauschning, 1980 pressure 16 mm. Hg § intra-articular pressure changes direct flow of synovial fluid knee flexion knee from supra-patellar bursa knee popliteal cyst extension Lindgren & Rauschning, 1980

PATHO-PHYSIOLOGY § repeated micro-trauma of gastroc-semimem bursa: enlargement § joint capsule herniation into popliteal fossa (Handy, 2001) § trauma causative in 1/3 of cases (Miller et al, 1996) § co-existent joint disease in 2/3 of cases (Miller et al, 1996) ü osteo-arthritis ü rheumatoid arthritis ü meniscal tears ü infectious arthritis
SYMPTOMS & SIGNS
Sx & Tx q most cases: § small, asymptomatic, not found o/e § dx imaging studies for other indications § Sx from associated joint disorders / Kx q Sx & Tx of Cyst itself: § posterior knee pain § knee stiffness § swelling / mass palpable post – in extension § discomfort - prolonged standing / hyperflexion § symptoms worsened by physical activity
Sx & Tx due to Kx of the Cyst: enlargement into lower leg - DVT nerve entrapment: tibial and peroneal nerve (Jong-Hun Ji and Shafi et al, 2007) compartment syndrome, ant or post involvement (Klovning and Beadle, 2007) compression of popliteal vein: venous obstruction, pseudo-thrombophlebitis, thrombophlebitis (Drescher & Smally, 1997) occlusion of popliteal artery: ischemia of lower limb (Wachter et al, 2005)
Sx & Tx due to Underlying joint disorders: § instability of knee joint due to internal derangement: ü meniscal tears ü +/- ACL deficiencies § joint pain ü inflammatory arthritis ü osteo-arthritis ü cartilage damage

DIAGNOSIS
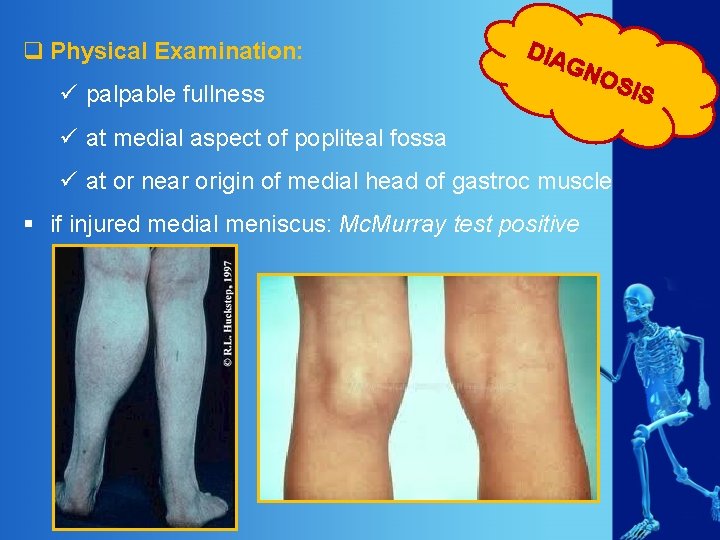
q Physical Examination: ü palpable fullness DIA GN OS ü at medial aspect of popliteal fossa ü at or near origin of medial head of gastroc muscle § if injured medial meniscus: Mc. Murray test positive IS
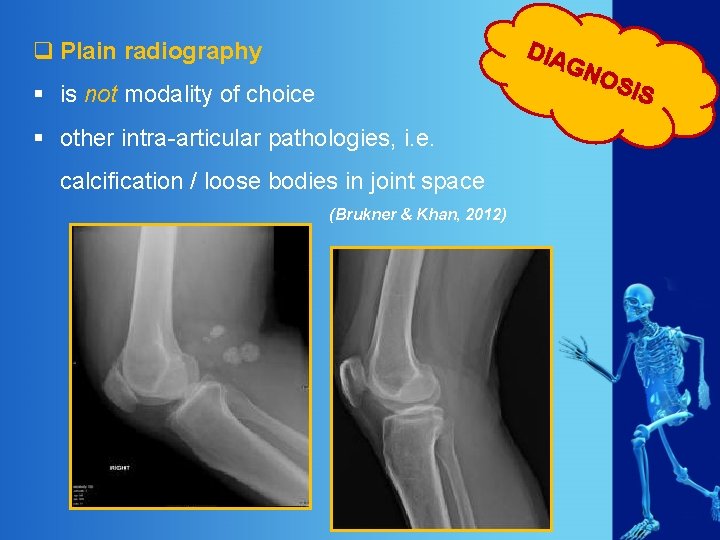
DIA q Plain radiography GN § is not modality of choice § other intra-articular pathologies, i. e. calcification / loose bodies in joint space (Brukner & Khan, 2012) OS IS
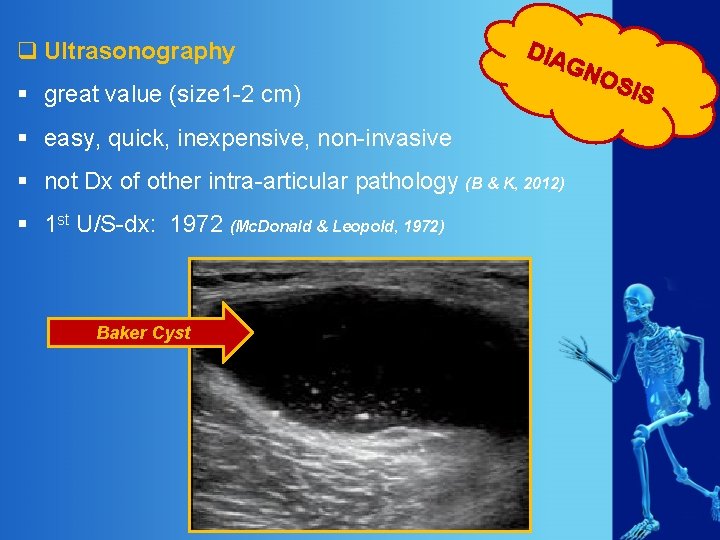
q Ultrasonography DIA § great value (size 1 -2 cm) § easy, quick, inexpensive, non-invasive § not Dx of other intra-articular pathology (B & K, 2012) § 1 st U/S-dx: 1972 (Mc. Donald & Leopold, 1972) Baker Cyst GN OS IS

q Ultrasonography DIA GN § sonographic diagnosis of Baker’s cyst OS IS ü presence of cystic soft tissue mass post of knee ü visualising of communicating anechoic or hypoechoic fluid between semimembranosus and medial gastrocnemius muscles (Ward and Jacobson, 2001) § distinguish Baker’s cyst from ü ganglion cysts ü popliteal aneurysm ü other popliteal masses
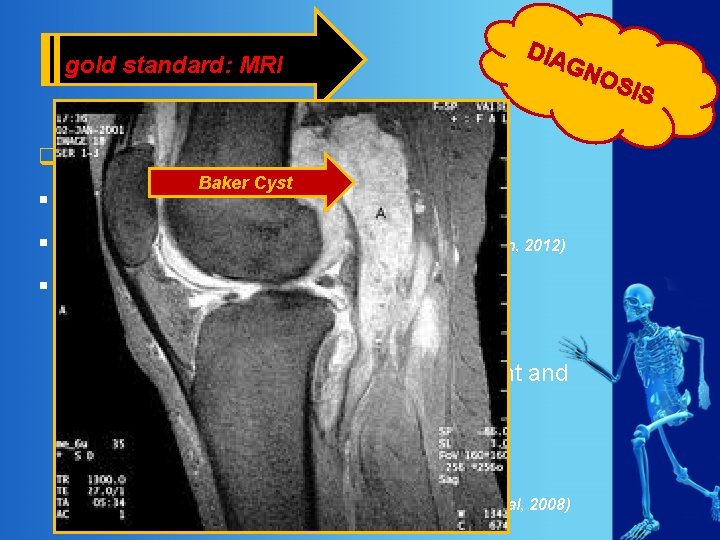
gold standard: MRI DIA GN q Magnetic Resonance Imaging (MRI) Baker Cyst § diagnosis Baker’s cyst § and intra-articular pathologies (Brukner & Khan, 2012) § indicated ü if ? internal derangement ü evaluate anatomical relationship to joint and surrounding tissues ü surgery is considered ü uncertain ultrasound-diagnosis (Marra et al, 2008) OS IS
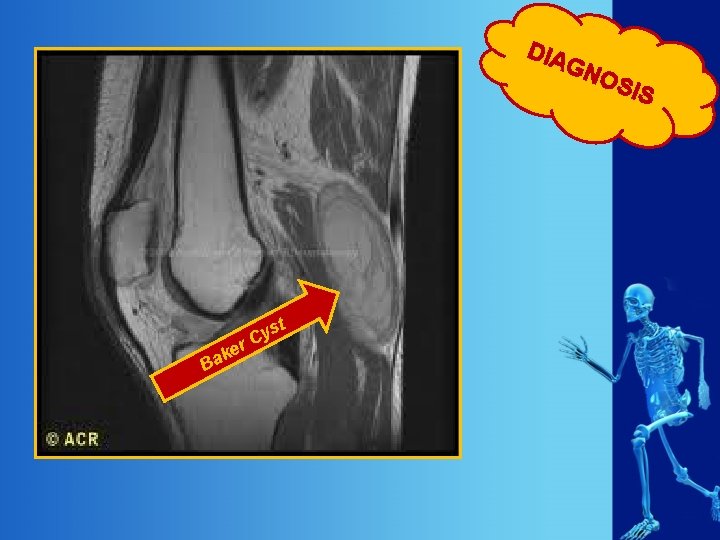
DIA GN t ys C er k Ba OS IS
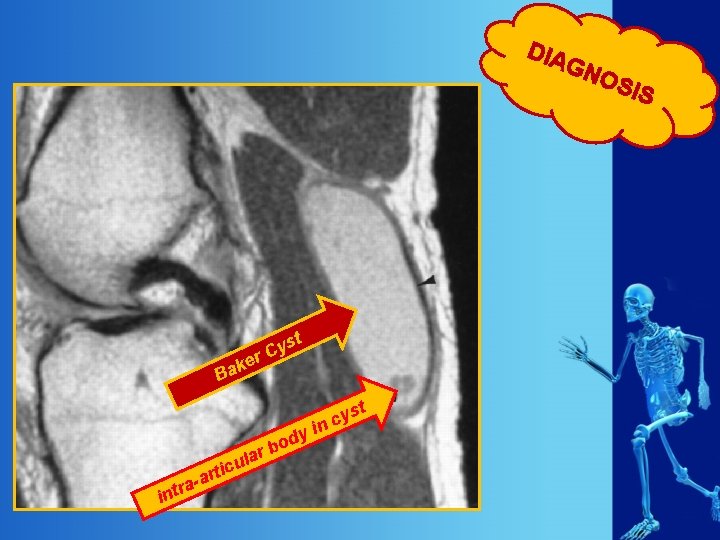
DIA GN st y r. C ke Ba od b r a a intr ul c i t -ar y yst c in OS IS
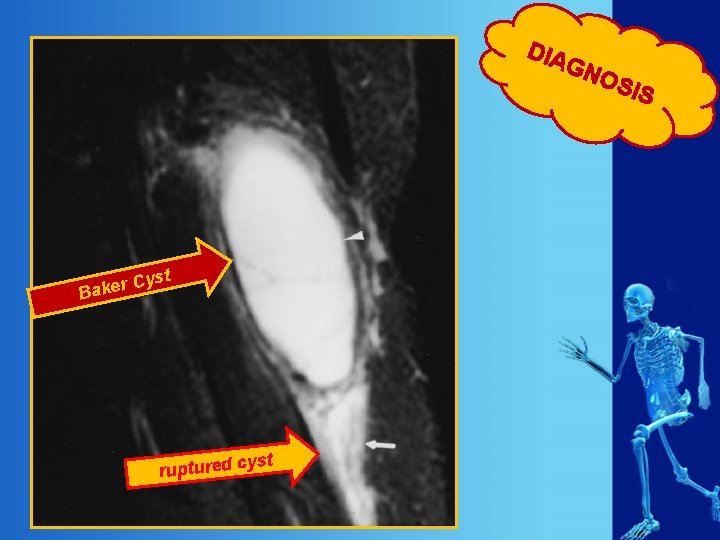
DIA GN yst C r e k Ba yst ruptured c OS IS

MANAGEMENT

MANAGEMENT v diagnosed incidentally: no treatment v advice: ü small risk of rupture ü seek medical advice if symptomatic v prevention not possible v advice on activities: ü regular exercise and weight Mx for OA ü no squatting, kneeling, heavy lifting, climbing

MANAGEMENT v initial Rx: ü arthrocentesis of knee ü aspiration ü intra-articular glucocorticoid injection of cyst expect ↓ in size and discomfort of cyst (two-thirds of pt) within 2 to 7 days • ↓ risk of recurrence • improvement of symptoms • controlling inflammation by glucocorticoid injections (Acebes et al, 2006)
MANAGEMENT § review diagnosis Ultrasound-guided § ? persistent underlying knee pathology § repeat of glucocorticoid injection direct cyst corticoid injection § arthroscopic knee surgery q indicated § non-communicating cysts: ü intra-articular injection of gluco-corticoids ü non-responsive to intra-articular injections failed to relief symptoms ü direct aspiration and glucocorticoid injection ü non-communicating Baker’s cysts § no joint pathology: surgical excision
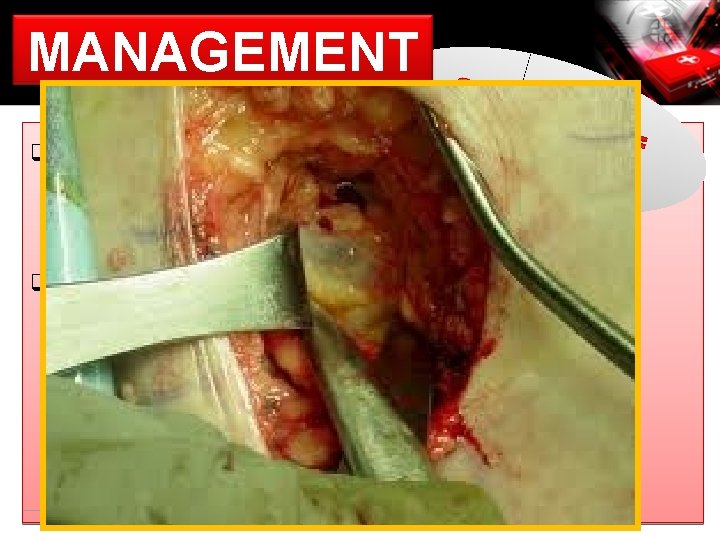
MANAGEMENT q indicated (if injections): § ++ painful § ↓ joint mobility q lengthy procedure § open procedure to excise cyst (Fritschy et al, 2006) § arthroscopic procedures ü repair of intra-articular pathology ü removal of cyst ü debridement of capsular openings (Ahn et al, 2010)

MANAGEMENT q Post-op Risks: § wound sepsis § synovial fistulae § recurrence: 2 y post-op f/u on MRI-study (Calvisi et al, 2007) ü disappeared: 64% ü reduced: 27% ü persisted: 9%

POST-OP REHABILITATION

POST-OP REHAB v aim: ↑ knee function v knee immobilizer § for comfort, with weight bearing q Supportive Management: v day 1 post-op: v P. R. I. C. E. regime § isometric exercises + straight leg raises v physical therapy: ↓ pain, preserve ROM v knee range of motion exercises v muscle strengthening: quads, patellar lig § wound stable § post-op inflammation subsided (Gonzalez & Lavernia, 2010) v wound healing complete before maximal extension

PROGNOSIS

PROGNOSIS q most asymptomatic – NO complications q some resolve spontaneously q most respond to Mx of associated disorders of knee


TAKE HOME MESSAGE differential diagnosis !! Ø NOT only Baker’s cyst / DVT • pleomorphic sarcoma • malignant giant cell tumors • myxoid liposarcomas (Arumilli et al, 2008) Ø early accurate / delayed dx affect overall prognosis Ø unnecessary use of anticoagulation therapy (if mistaken for DVT) could be dangerous!

REFERENCES

REFERENCES 1. Acebes JC, Sanchez-Pernaute O, Diaz-Oca A, et al. Ultrasonographic assessment of Baker’s cysts after inatrarticular corticosteroid injection in knee osteoarthritis. J Clin Ultrasound. 2006; 34: 113 2. Ahn JH, Lee SH, Yoo JC, et al. Arthroscopic treatment of popliteal cysts: clinical and magnetic resonance imaging results. Arthroscopy. 2010; 26: 1340 3. Arumilli BRB, Babu VL, Paul AS. Painful swollen leg - think beyond deep vein thrombosis or Baker’s cyst. World Journal of Surgical Oncology. 2008; (6): 6 4. Baker WM. On the formation of the synovial cysts in the leg in connection with disease of the knee joint. 1877. Clin Orthop Relat Res. Feb 1994; (299): 2 -10

REFERENCES 5. Calvisi V, Lupparelli S, Giuliani P. Arthroscopic all-inside suture of symptomatic Baker’s cysts: a technical option for surgerical treatment in adults. Knee Surgery, Sports Traumatology, Arthroscopy. 2007; 15(12): 1452 -1460 6. Brukner P, Khan K. Clinical Sports Medicine. 4 th Ed. 2012. p 731 -732 7. Drescher MJ, Smally AJ. Thrombophlebitis and pseudothrombo-phlebitis in the emergency department. Am J Emerg Med. 1997; 15: 683 -685 8. Fielding JR, Franklin PD, Kustan J. Popliteal cysts: a reassessment using magnetic resonance imaging. Skeletal Radiol. 1991; 20: 433

REFERENCES 10. Fritschy D, Fasel J, Imbert JC, et al. The popliteal cyst. Knee Surg Sports Traumatol Arthrosc. 2006; 14: 623 11. Gonzalez DM, Lavernia CJ. Cystic lesions about the knee: treatment and management. http: //www. emedicine. medscape. com/article/1250593 overview Jan 2010 12. Janzen DL, Peterfy CG, Forbes JR, et al. Cystic lesions around the knee joint: magnetic resonance imaging findings. AJR. 1994; 163: 155 -161 13. Jong-Hun Ji, Mohammed Shafi, et al. Compressive neuropathy of the tibial nerve and peroneal nerve by a Baker’s cyst: Case report. The Knee. 2007; 14(3): 249 -252 14. Handy JR. Popliteal cysts in adults: a review. Semin Arthritis Rheum. 2001; 31: 108

REFERENCES 15. Miller TT, Staron RB, Koenigsberg T, et al. MR imaging of Baker cysts: association with internal derangement, effusion, and degenerative arthropathy. Radiology. 1996; 201: 247 16. Hayashi D, Roemer FW, Dhina Z, et al. Longitudinal assessment of cyst-like lesions of the knee and their relation to radiographic osteoarthritis and MRI-detected effusion and synovitis in patients with knee pain. Arthritis Res Ther. 2010; 12: R 172 17. Klovning J, Beadle T. Compartment Syndrome secondary to spontaneous rupture of a Baker’s cyst. J La State Med Soc. 2007; 159(1): 43 -44 18. Lindgren PG, Rauschning W. Radiographic investigation of popliteal cysts. Acta Radiol Diagn (Stockh). 1980; 21: 657 19. Marra MD, Crema MD, Chung M, et al. MRI features of cystic lesions around the knee. Knee. 2008; 15: 423

REFERENCES 20. Mc. Donald DG, Leopold GR. Ultrasound B-scanning in the differentiation of Baker’s cyst and thrombophlebitis. Br J Radiol. 1972; 45: 729 21. Sansone V, De Ponti A, Palluello GM, et al. Popliteal cysts and associated disorders of the knee. Critical review with Magnetic Resonance Imaging. Int Orthop. 1995; 19(5): 275 -9 22. Ward EE, Jacobson JA. Sonographic detection of Baker’s cysts: Comparison with MR imaging. Am J Roëntgenol. 2001; 176(2); 373 -80
- Slides: 70