Badger Care Plus Affordable Care Act 2021 Badger

Badger. Care Plus & Affordable Care Act 2021

Badger. Care Plus

BC+ and Turning 65 • Typical EBS clients with BC+ are in one of these coverage groups: • Adults ages 19 -64 who are not receiving Medicare and who do not have dependent children (“Childless adults”) • Parents and caretaker relatives of children younger than 18 years old and dependent 18 -year-olds – can be over 65 • BC+ does not always recognize when beneficiaries turn 65 • Best to be proactive and report this to Income Maintenance • Beneficiaries are required to report changes in insurance coverage within 10 days of occurrence (BC+ Handbook 27. 2) – includes Medicare enrollment 3

Note on Caretaker Relatives • Non-legally responsible relative of the child under his or her care • Caretaker relative must have a qualifying relationship to the child (under age 19), and the child must be under the care of that relative • Qualifying relationships: • Stepfather or stepmother (when the parent is deceased or divorced/separated from the stepparent) • Natural full brother or sister, legally adopted, half- or stepbrother or sister • Grandmother or grandfather, aunt or uncle, first cousin, nephew or niece, or any preceding generation denoted by the prefix grand-, great-, or great-great, and including those through adoption • Spouse of any of the above and the spouse of a child’s parent, even after the marriage ends by death, divorce, or separation • Being "under the care” means the caretaker exercises primary responsibility for the child’s care and control, including making plans for him or her. • Once a child marries, he or she can no longer be considered under the care of a caretaker relative. • Spouse of caretaker relative can also be eligible for BC+ 4

BC+ and Social Security Retirement • Many clients want to delay SSR benefits for as long as possible in order to maximize benefits, but federal law requires beneficiaries to take “all necessary steps to obtain any annuities, pensions, retirement, and disability benefits to which they are entitled. ” (42 CFR § 435. 608) • If it is known that a BC+ recipient is eligible for income: • If the amount is known, count the income as if the person is receiving it. • If the amount is unknown, ignore the income. (BC+ Handbook 16. 1. 2) 5

Long-Term Care for BC+ Childless Adults • A person who is not eligible for EBD Medicaid will be eligible for LTC Medicaid benefits under BC+ (see BC+ Handbook section 42): • No monthly patient liability can be charged • No asset limit • Those ages 55 and older are subject to estate recovery; however, a lien cannot be placed on their home. • If/when a person becomes eligible for EBD Medicaid, patient liabilities, asset limits, and regular estate recovery rules apply • Note: Once institutionalized and considered out of the home, a parent would be considered a childless adult and may qualify for long-term care as a childless adult. 6

BC+ Changes in 2020 • Section 1115 Badger. Care Reform Demonstration Waiver Amendment request submitted to CMS and approved October 2018 • Changes start going into affect February 1, 2020 (or at renewal): • Establish monthly premiums of $8 for households, or less depending on income and healthy behaviors • Establish emergency room visit copays of $8 for non-emergency use • Optional health survey upon application; members who report healthy behaviors can reduce monthly premium • Mandatory drug treatment needs question – answer will not affect health benefits • Affects childless adults ages 19– 64 • Does not affect EBD population or caregivers, children, and pregnant women (except for expanded access to substance abuse treatment) • Still pending: • Community engagement requirement, including limiting benefit eligibility to 48 months for non-compliance (childless adults ages 18 -49 only) • Coverage of residential substance use disorder treatment 7
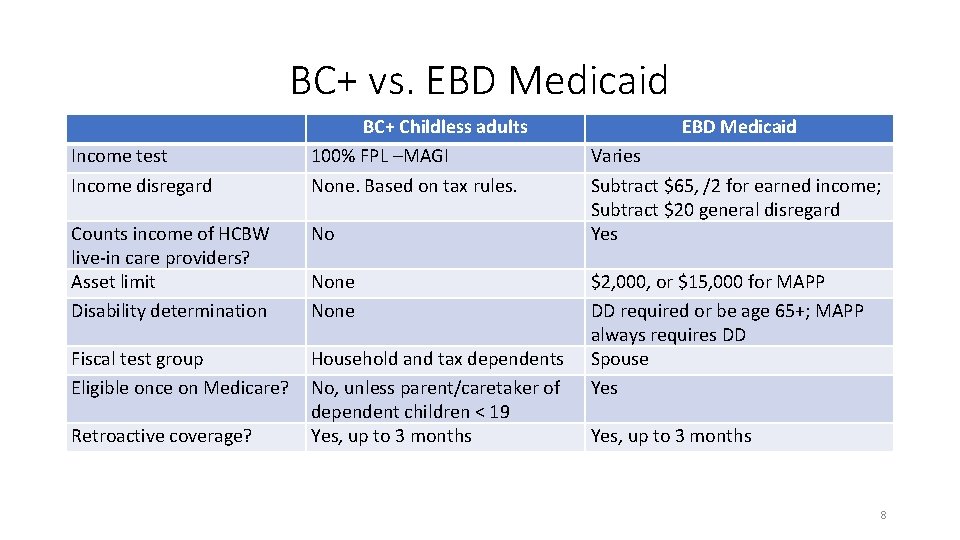

BC+ vs. EBD Medicaid Income test Income disregard BC+ Childless adults 100% FPL –MAGI None. Based on tax rules. Counts income of HCBW live-in care providers? Asset limit Disability determination No Fiscal test group Eligible once on Medicare? Household and tax dependents No, unless parent/caretaker of dependent children < 19 Yes, up to 3 months Retroactive coverage? None EBD Medicaid Varies Subtract $65, /2 for earned income; Subtract $20 general disregard Yes $2, 000, or $15, 000 for MAPP DD required or be age 65+; MAPP always requires DD Spouse Yes, up to 3 months 8
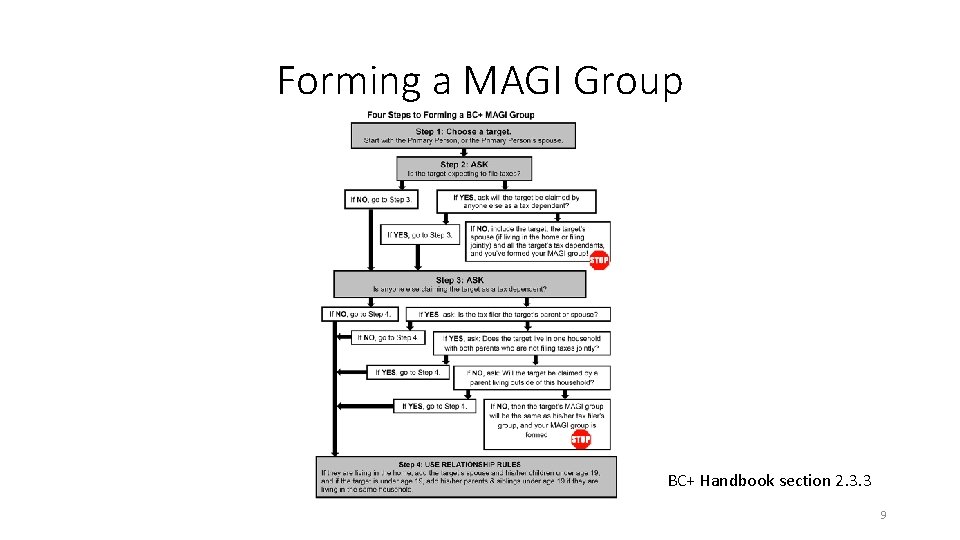
Forming a MAGI Group BC+ Handbook section 2. 3. 3 9

MAGI for an Extended Family Household 10

Gomez is applying for BC+ for his family. In addition to his wife, Morticia, and children, Wednesday and Pugsley, several people live in the house on Cemetery Lane: Grandmama, Uncle Fester, Cousin Itt, and Lurch, the butler. In addition to Wednesday and Pugsley, Gomez and Morticia claim Uncle Fester and Cousin Itt as dependents on their taxes. Who is in Gomez’s MAGI group? A. Gomez, Morticia, Wednesday, Pugsley, Grandmama, Uncle Fester, Cousin Itt, & Lurch B. Gomez, Morticia, Wednesday, Pugsley, Grandmama, Uncle Fester, & Cousin Itt C. Gomez, Morticia, Wednesday, Pugsley, Uncle Fester, & Cousin Itt D. Gomez, Morticia, Wednesday, & Pugsley 11

Uncle Fester & Cousin Itt Uncle Fester, who has severe headaches, and Cousin Itt, who is blind, are applying for BC+. They do not plan to file taxes, as their only income is from non-taxable SSDI benefits. Who is in their MAGI group(s)? A. One MAGI group: Uncle Fester and Cousin Itt B. One MAGI group: Uncle Fester, Cousin Itt, and Gomez C. Separate MAGI groups: Uncle Fester in one and Cousin Itt in another D. Separate MAGI groups: Uncle Fester and Gomez in one and Cousin Itt and Gomez in another 12

Grandmama Although she was only supposed to move in for two weeks, after twelve years, Grandmama, who is 72, is ready to move out. Tired of her brother, Wednesday moves in with Grandmama’s Social Security Retirement benefits are $1, 000/month, but she has significant assets. Is Grandmama eligible for BC+? A. No, because she’s over 65 and receiving Medicare. B. Yes, because Wednesday is under her care. 13

Lurch Uncle Fester is approved for Family Care. He hires Lurch to be his live-in caregiver. Lurch is happy to be earning some extra money, but he’s worried about losing his BC+. If Lurch earns $800/month from his butler duties, and an additional $500/month caring for Uncle Fester, what is his countable income for BC+? A. $1, 300/month B. $1, 000/month C. $800/month D. $500/month 14

Affordable Care Act

Affordable Care Act 16

1. What is the Health Insurance Marketplace? • A way to shop for health insurance • A place to find health insurance that works for you and your family • A place to compare health insurance plans and costs on an “apples-to-apples” basis • All of the above 17

2. How can I apply for coverage in the Health Insurance Marketplace? • Online • By phone • By mail • All of the above 18

3. Until what age can a young adult stay on a parent's health insurance plan? • 18 • 21 • 23 • 26 19

4. Who is able to purchase health insurance through the Health Insurance Marketplace? • Uninsured people • Small business owners • Self-employed people • All of the above 20

5. Which of the following consumer protections were included in the Affordable Care Act? • Insurance companies can't stop coverage just because a person becomes sick • Insurance companies can't deny coverage due to a child's medical history • Insurance companies can't deny coverage due to an adult's medical history • All of the above 21

6. Which of the following were covered by Medicare and most health insurance plans as a result of the ACA? • Screenings for diabetes • Mammograms • Colonoscopies • All of the above 22

7. How often can people with Medicare receive a free wellness exam? • Every year • Every 2 years • Every 5 years • Never 23

8. In what year was the Medicare Part D "doughnut hole" drug coverage gap completely closed? • 2014 • 2017 • 2019 • 2020 24

9. How many full-time workers can a business employ without facing fines for not providing health insurance? • 25 • 50 • 100 • 500 25

Marketplace and Retiree Health Insurance • If someone has retiree coverage and wants to buy a Marketplace plan instead, they can, but: • Can’t get premium tax credits and other savings based on income if they’re actually enrolled in retiree coverage. If they’re eligible for but not enrolled in retiree coverage, they may qualify for premium tax credits and lower out-of-pocket costs based on household size and income. • If they voluntarily drop retiree coverage, they won’t qualify for a special enrollment period to enroll in a new Marketplace plan. They won’t be able to enroll in health coverage through the Marketplace until the next Open Enrollment period. 26

Marketplace and COBRA • Can someone drop COBRA and get Marketplace coverage instead and qualify for lower costs based on my income? Maybe. • If COBRA coverage ends outside Open Enrollment, they qualify for a special enrollment period and can enroll in a Marketplace plan outside the annual Open Enrollment Period. • However, someone can’t choose to drop COBRA coverage outside Open Enrollment and enroll in a Marketplace plan instead – the special enrollment period applies only if COBRA coverage ends. • During the annual Open Enrollment Period, someone can drop COBRA coverage even if it’s not ending and replace it with a Marketplace plan. 27

Medicare & Marketplace • It is illegal to sell a Medicare beneficiary a Marketplace plan. • Medicare Part A alone meets the standard for Minimum Essential Health Coverage. • A person is not eligible for any Marketplace subsidies if he/she gets premium-free Medicare Part A. • People need to affirmatively drop a Marketplace plan prior to starting Medicare. It is not automatic!

Changing from the Marketplace to Medicare • If someone <65 has a Marketplace plan, they can keep it until Medicare coverage starts • Once Medicare Part A coverage starts, they won’t be eligible for a premium tax credit or other savings for a Marketplace plan – will have to pay full price for plan! • Medicare Part B is not considered minimum essential coverage. • Typically want to end Marketplace coverage once eligible for Medicare 29

Ending Marketplace Coverage • Can end coverage for everyone on the Marketplace plan or just some people on the plan. • The best way to make sure coverage ends on the right date is to contact the Marketplace Call Center and request the change – coverage will not end automatically when Medicare starts! • For step-by-step instructions, please see: https: //www. healthcare. gov/medicare/changing-from-marketplace-tomedicare/ 30

Choosing Marketplace over Medicare? • Fewer than 1% of people—talk to BSSA! • Typically will be people who have to pay a premium for Part A • Most people have better coverage at a more affordable price with Medicare. • People who receive premium-free Medicare Part A are NOT eligible for Marketplace subsidies. • Medicare late-enrollment penalties (Parts B & D) will apply.

People on Medicare should NOT go to the Marketplace to pick out any plans.

Marketplace/Medicare Equitable Relief • For individuals who delayed enrolling in Medicare Part B so that they could stay in their Marketplace plan or who could have enrolled in Part B using the Part B Special Enrollment Period but chose to enroll in Marketplace coverage instead • Does not include SHOP Marketplace plans • Individuals are eligible if they are or were enrolled in a Marketplace plan, are enrolled in premiumfree Part A, and: • Their Initial Enrollment Period (IEP) began between April 1, 2013 and March 1, 2020 • They were notified of retroactive premium-free Part A between October 1, 2013 and June 30, 2020 • Or, they had a Part B SEP that ended between October 1, 2013 and June 30, 2020 • If they want to request that their Part B late enrollment penalty (LEP) be eliminated or reduced, they must have received the penalty after enrolling in Part B during the Medicare General Enrollment Period between 2015 and 2020. • If they’re eligible, equitable relief will let them enroll in Medicare Part B without penalty or eliminate or reduce their Part B LEP. • Note that they are not eligible to request equitable relief for Marketplace enrollees if: • They delayed Part B enrollment to stay in SHOP. • They pay a premium for Part A (because they can choose to disenroll from Part A and continue to use Marketplace coverage). • They can currently enroll in Part B because they’re in their IEP or Part B SEP (because they can enroll in Part B without penalty). 33

Medicare and SHOP Marketplace • If someone has Medicare, can they get health coverage from an employer through the SHOP Marketplace? • Yes. Coverage from an employer through the SHOP Marketplace is treated the same as coverage from any job-based health plan. • If someone is getting health coverage from an employer through the SHOP Marketplace, can they delay enrollment in Part B without a penalty? • Yes. Someone can delay Part B enrollment if they’re getting health coverage through the SHOP Marketplace based on their own or their spouse’s job. • They’ll have a special enrollment to sign up for Part B without penalty: • Any time they’re still covered by the job-based health plan based on their own or their spouse’s current employment • During the 8 -month period that begins the month after the job or the coverage ends, whichever happens first • If they don’t sign up during the special enrollment period, they may have to pay a late enrollment penalty for Part B for as long as they have Medicare. 34

Marketplace and Prescription Drug Coverage • Is prescription drug coverage through the Marketplace considered creditable prescription drug coverage for Medicare Part D? Maybe. • While prescription drug coverage is an essential health benefit, prescription drug coverage in a Marketplace or SHOP health plan isn’t required to be at least as good as (creditable) Medicare Part D coverage. • All private plans offering prescription drug coverage, including Marketplace and SHOP plans, must report to members in writing if their prescription drug coverage is creditable each year. 35

ACA Litigation • NFIB v. Sebelius (2012): U. S. Supreme Court says individual mandate is constitutional under Congress’ power to tax • 2017: Various attempts in Congress to “repeal and replace, ” “repeal and delay, ” and “skinny repeal” • Tax Cuts and Jobs Act (2017): Congress sets shared responsibility payment (tax penalty for not having coverage) at $0 starting 1/1/2019 • U. S. House of Representatives v. Texas (2019): District Court judge says entire ACA is invalid; 5 th Circuit Court of Appeals says that the individual mandate is unconstitutional now that there’s no tax penalty and sends case back to the district court to see how much of the ACA can stay (“severability”) in light of that decision (also question about whether states and individual plaintiffs have standing to sue); U. S. Supreme Court heard California v. Texas in November 2021 • Next steps: ? ? ? but plans sold for 2021 are a contract for the entire year 36

EBS role with Marketplace/ACA • Client education, including the risks of going without health coverage • Marketplace is a good option for health insurance • Discuss transition to Medicare at age 65 • Refer clients to navigators or assistors for enrollment – EBS do not enroll • Private insurance agents can enroll too (commission) • Reassure clients that Marketplace plans are under contract with CMS to provide health insurance through the end of the year
- Slides: 37