Bacterial Infections 1 Classification of Antiinfective Drugs Antiinfective
Bacterial Infections 1

Classification of Anti-infective Drugs • • • Anti-infective Antibiotic Antibacterial Antimicrobial Bacteriocidal Bacteriostatic • Chemical class • Pharmacologic class 2

Goal of Antibiotic Therapy • Kill enough bacteria or slow growth of infection so natural body defense can overcome invading organism • Acquired Resistance • Health Care Acquired Resistance – MRSA – VRE 3

Describing and Classifying Bacteria • Staining Characteristics – Gram-positive bacteria – thick cell wall, retain purple color – Gram-negative bacteria – thinner cell wall, loose violet stain • Ability to use oxygen – Aerobic- with O 2 – Anaerobic- without O 2 • Cellular Shapes – Bacilli- rod shape – Cocci-spherical – Spirilla-spiral shape 4

Five Principles 1. Prevent infections 2. Use right drug for infections 3. Restrict use of antibiotics to conditions deemed medically necessary 4. Take full length of therapy 5. Prevent transmission –proper infection control 5

Widespread Use of Antibiotics • Resistance not caused by but is worsened by over prescription of antibiotics – Results in loss of antibiotic effectiveness • • • Only prescribe when necessary Long-time use increases resistant strains Nosocomial infections often resistant Prophylactic use sometimes appropriate Nurse should instruct client to take full dose 6

Acquired Resistance • Occurs when pathogen acquires gene for bacterial resistance – Through maturation • Antibiotics destroy sensitive bacteria • Insensitive (mutated) bacteria remain 7

Culture and Sensitivity (C&S) • Process of growing pathogen and identifying most effective antibiotic • Examination of specimen for microorganisms • Tested for sensitivity to different antibiotics • Bacteria may take several days to identify • Viruses may take several weeks to identify • Broad spectrum antibiotics may be started before lab culture completed 8

Superinfections • Secondary infections that occur when too many host flora are killed by an antibiotic – Host flora prevent growth of pathogenic organisms • Suspected if new infection appears while on antiinfective therapy – Signs and symptoms include diarrhea, bladder pain, painful urination, or abnormal vaginal discharge • Broad-spectrum antibiotics • Narrow-spectrum antibiotics (less effect on host flora) 9

Mechanism of Action • PROTEIN SYNTHESIS INHIBITOR • BACTERIAL DNA SYNTHESIS INHIBITOR • FOLIC ACID INHIBITOR 10

Prototype Drugs • Gentamycin (Garamycin) –aminoglycoside • Ciprofloxacin (Cipro) –fluoroquinolone • Trimethorpim-sulfamethoxazole (Bactrim) – sulfonamide 11

Role of the Nurse • Assessment – Obtain complete health history—allergies, drug interactions – Obtain specimens for culture and sensitivity before initiating therapy – Perform infection-focused physical examination— vital signs, WBC count 12

Role of the Nurse • Planning—patient will – Report diminished signs and symptoms of infection, decreased fever and fatigue, increased appetite – Be free from, or experiences minimal adverse effects 13

Role of the Nurse • Implementation – Monitor vital signs and symptoms of infection – Monitor for hypersensitivity reaction – Monitor for severe diarrhea – Administer drug around the clock – Monitor for superinfection – Monitor intake of OTC products – Monitor for photosensitivity 14

Role of the Nurse – Monitor labs values (WBC, antibiotic levels) – Monitor IV site for signs of tissue irritation, severe pain, extravasation – Monitor for side effects, renal function, symptoms of ototoxicity, compliance with antibiotic therapy 15

Role of the Nurse • Evaluation—patient – Reports diminished signs and symptoms of infection, decreased fever – Is free from, or experiences minimal adverse effects. – Verbalizes an understanding of the drug’s use, adverse effects and required precautions. – Demonstrates proper self-administration of the medication (e. g. , dose, timing, when to notify provider). 16

Role of the Nurse • After parenteral administration, observe closely for possible allergic reactions • Teach clients to – Wear medic-alert bracelets if allergic to antibiotics – Report symptoms of allergic reaction – Not stop taking drug until complete prescription has been taken 17
Viral Infections 18

Viruses • Nonliving agents • Intracellular • Infects organism and uses host cell to replicate (rapid mutation) 19

Challenges of Antiviral Therapy • Viruses mutate rapidly, and drug becomes ineffective • Difficult for drug to find virus without injuring normal cells • Each antiviral drug specific to one particular virus (narrow spectrum) 20

Therapy for Viral Infections • Most self-limiting; require no pharmacotherapy – Rhinovirus that causes common cold • Some viruses cause serious disease and require aggressive therapy – HIV, Hep B – Herpesviruses can cause significant pain and disability if left untreated 21

Basic Strategies for Antiviral Pharmacotherapy • Prevent viral infections through vaccinations • Treat active infections to interrupt replication cycle • Prophylaxis so virus latent = symptom free 22

HIV Pharmacotherapy • Antiretrovirals • No cure yet, but many new drugs developed • Some therapeutic successes – People live symptom-free longer – Rates of transmission from mother to newborn reduced – 70% decline in death rate in US 23

Therapeutic Goals • Reduce HIV related morbidity and prolong survival • Improve quality of life • Restore and preserve immune function • Promote max suppression of viral load • Prevent transmission from mother to child 24

Highly Active Antiretroviral Therapy (HAART) • Five drug classes used in various combinations – Nucleoside reverse transcriptase inhibitor (NRTI) – Nonnucleoside reverse transcriptase inhibitor (NNRTI) – Protease inhibitor (PI) – Nucleotide reverse transcriptase inhibitor (Nt. RTI) – Fusion (entry) inhibitor 25

Goal of HAART • Reduce plasma HIV RNA to lowest possible level. • Simultaneous use of drugs from several classes reduced probability that HIV will become resistant to treatment • Must be continued for lifetime of patient 26

Treatment Failure 1. 2. 3. 4. Inability to tolerate adverse effects Nonadherence to complex drug therapy Emergence of resistant HIV strains Genetic variability among patients 27

Prototype Drugs • Zidovudine (Retrovir, AZT) –antiretroviral • Nevirapine (Viramune) –antiretroviral • Acyclovir (Zoviraz) –antiviral for herpesvirus 28

Role of the Nurse • Assess patient’s ability to receive and understand instruction, • CD 4 Counts, Viral load • Instruct patient and/or family in proper selfadministration techniques followed by return demonstration • Ensure adequate nutrition and caloric intake • Encourage infection control and good hygiene measures • Be free from, or experience minimal adverse effects 29

Patients receiving pharmacotherapy for HIV-AIDS • Assessment – Note onset, duration, characteristics, presence or absence of fever or pain. – Evaluate : CBC, CD-4 count, HIV RNA assay, culture and sensitivity, hepatic and renal function studies, lipid levels, serum amylase, and glucose. – Assess patient’s ability to receive and understand instruction 30

Patients receiving pharmacotherapy for HIV-AIDS • Planning—patient will – Experience CD-4 counts and HIV RNA assays within acceptable limits, absence of signs and symptoms of concurrent infection, ability to maintain ADLs – Be free from, or experience minimal adverse effects 31

Patients receiving pharmacotherapy for HIV-AIDS • Planning—patient will – Verbalize an understanding of the drug’s use, adverse effects and required precautions. – Demonstrate proper self-administration of the medication (e. g. , dose, timing, when to notify provider). 32

Patients receiving pharmacotherapy for HIV-AIDS • Implementation – Monitor vital signs, especially temperature if fever is present – Monitor for hypersensitivity and reactions – Continue to monitor for hepatic and renal, toxicities – Monitor for dermatologic effects – Monitor client for signs of stomatitis 33

Patients receiving pharmacotherapy for HIV-AIDS • Implementation – Monitor : hepatic and renal function tests, CBC, CD-4 counts, HIV RNA assays, lipid levels, serum amylase, culture and sensitivity if concurrent infections are present, glucose. – Monitor for symptoms of pancreatitis – Monitor for signs and symptoms of blood dyscrasias 34

Patients receiving pharmacotherapy for HIV-AIDS • Implementation – Monitor for significant GI effects – Monitor for signs and symptoms of neurotoxicity – Administer drugs as per guidelines – Provide resources for medical and emotional support – Assess client’s knowledge level regarding use and effect of medication 35

Patients receiving pharmacotherapy for HIV-AIDS • Implementation – Monitor blood glucose – Ensure adequate nutrition and caloric intake – Encourage infection control and good hygiene measures – Instruct patient and/or family in proper selfadministration techniques followed by return demonstration 36

Patients receiving pharmacotherapy for HIV-AIDS • Evaluation—patient – Experiences CD-4 counts and HIV RNA assays within acceptable limits, absence of signs and symptoms of concurrent infection, ability to maintain ADLs – Is free from, or experiences minimal adverse effects – Verbalizes an understanding of the drug’s use, adverse effects and required precautions – Demonstrates proper self-administration of the medication (e. g. , dose, timing, when to notify provider). 37

Asthma and Other Pulmonary Disorders 38

Respiratory System • Bronchioles • The bronchial tree ends in dilated sacs called alveoli • Gases to readily move between the blood and inspired air via semipermeable membrane allows: – Oxygen to enter the blood – Carbon dioxide, and cellular waste products to leave the lungs 39
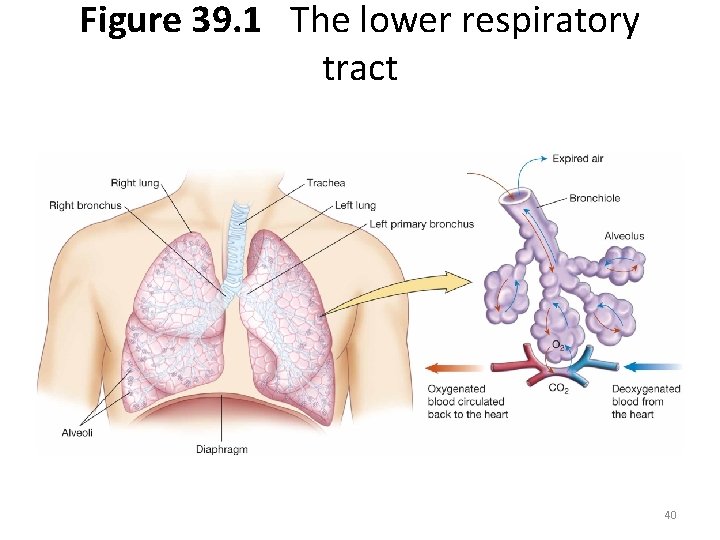
Figure 39. 1 The lower respiratory tract 40

Autonomic Control of Airways • Bronchioles – Lined with smooth muscle that controls amount of air entering lungs – Diameter of airways controlled by autonomic nervous system – The sympathetic branch activates beta 2 adrenergic receptors – Causes bronchiolar smooth muscle to relax – The airway diameter increases and decreases 41

Autonomic Control of Airways – Bronchodilation occurs: • Allows air to enter the lungs more freely • Increases the supply of oxygen to the body’s tissues. • The parasympathetic branch – Causes bronchiolar smooth muscle to contract – The airway diameter is narrowed • Bronchoconstriction occurs • Results in less airflow. 42

Administration by Inhalation • Common route of administration for pulmonary drugs • Rapid and efficient • Rich blood supply allows for quick absorption and onset of action • Delivers drugs directly to sites of action 43

Aerosol Therapy • Suspension of droplets or particles in a gas • Onset of action almost immediate • Drugs administered for local effect – Immediate relief of bronchospasm – Loosens thick mucus 44

Aerosol Therapy • Disadvantages of Aerosol Therapy – Difficult to measure precise dose – Usually, only 10– 50% of drug is placed – Instruction may be complicated for some clients – Side effects occur if client swallows drug or does not rinse mouth after inhalation 45

Devices Used for Aerosol Therapy • Nebulizer – Vaporizes liquid drug into fine mist – Uses small machine and face mask • Metered dose inhaler (MDI) – Propellant delivers measured dose of drug – Client times inhalation to puffs of drug • Dry powder inhaler (DPI) – Client inhales powdered drug – Device activated by inhalation 46

Asthma • Has both inflammatory and bronchospasm components • Symptoms occur – From exposure to triggers – Upon exertion (exercise induced) • Status asthmaticus—prolonged attack • Drugs used to – Prevent asthmatic attacks – Terminate attack in progress 47
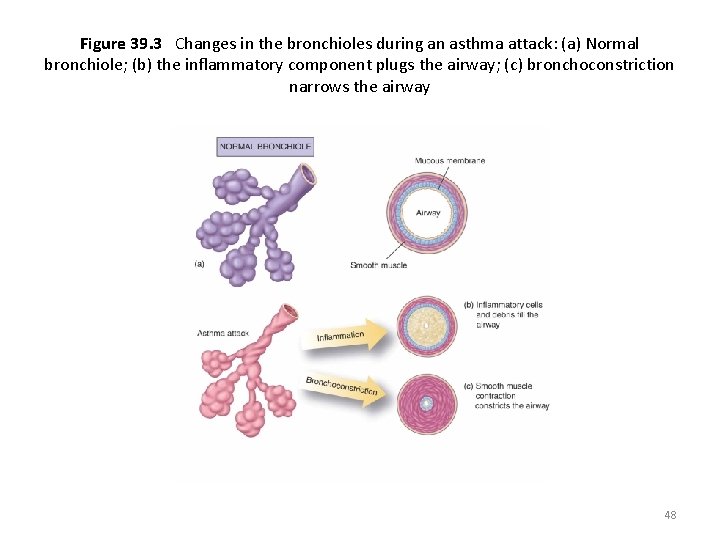
Figure 39. 3 Changes in the bronchioles during an asthma attack: (a) Normal bronchiole; (b) the inflammatory component plugs the airway; (c) bronchoconstriction narrows the airway 48

Goals of Therapy • Goals of drug therapy are twofold – To terminate acute bronchospasms in progress – To reduce the frequency of asthma attacks 49

Prototype Drugs • Salmeterol (Servent) –beta 2 -adrenergic agonist • Ipratropium (Atrovent) -anticholinergic 50

Anticholinergics • Block parasympathetic nervous system with bronchodilator effect • Occasionally used as alternative to beta-agonists in asthma therapy • Used in inhaled form • Ipratropium (Atrovent) is the most common anticholinergic prescribed for chronic obstructive pulmonary disease (COPD) and asthma • Most effective when used in combination with beta-agonist 51

Beta-Adrenergic Agonist • Most effective drugs for relieving acute bronchospasm • Activate beta 2 -receptors in bronchial smooth muscle to cause bronchodilation • Fewer cardiac side effects than older nonselective beta-adrenergics • Range from ultrashort to long acting 52

Role of the Nurse • Assessment – Obtain complete health history – Assess for symptoms related to respiratory deficiency – Assess for any recent changes if asthma are of new onset is of new onset – Obtain vital signs including pulse, blood pressure, respiratory rate and depth, and breath sounds. – Auscultate bilateral breath sounds for air movement and adventitious sounds – Assess pulmonary function with pulse oximeter, peak expiratory flow meter, and/or arterial blood gases 53

Role of the Nurse • Planning—patient will – Experience • • Increased ease of breathing, Improvement in pulmonary function studies, Normal sleep and eating periods, Ability to carry out ADLs to a level appropriate for condition 54

Role of the Nurse • Implementation – Instruct patient and/or family in proper selfadministration of drug 55

Role of the Nurse • Evaluation - Client – Experiences • • Increased ease of breathing Improvement in pulmonary function studies Normal sleep and eating periods Ability to carry out ADLs to a level appropriate for condition – Is free from, or experiences minimal adverse effects. – Verbalizes an understanding of the drug’s use, adverse effects and required precautions – Demonstrates proper self-administration of the medication (e. g. , dose, timing, when to notify provider 56
- Slides: 56