BACTERIAL AND VIRAL INFECTIONS Dr Spandana P Hegde

BACTERIAL AND VIRAL INFECTIONS Dr Spandana P Hegde Senior Resident Dept of Dermatology

BACTERIAL INFECTIONS § § § Introduction Classification Primary pyodermas • Superficial folliculitis • Impetigo • Ecthyma • Furuncle • Carbuncle • Erysipelas • Cellulitis • Paronychia • Staphylococcal scalded skin syndrome § Secondary pyodermas § Management principles

INTRODUCTION § Bacterial infection of skin. § Caused by mainly 2 Gram positive organisms: • Staphylococcus aureus : Intact skin • Group A beta-hemolytic Streptococci : Traumatic skin § Other bacteria: • Corynebacteria • Pseudomonas
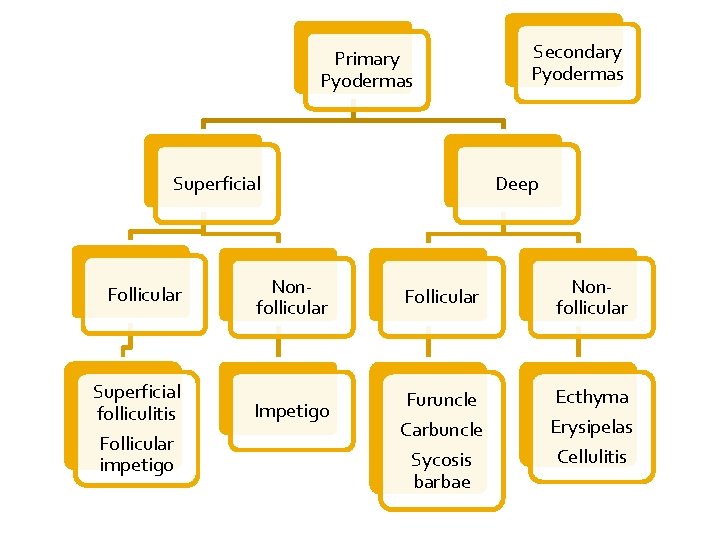
Primary Pyodermas Superficial Follicular Superficial folliculitis Follicular impetigo Nonfollicular Impetigo Secondary Pyodermas Deep Follicular Furuncle Carbuncle Sycosis barbae Nonfollicular Ecthyma Erysipelas Cellulitis
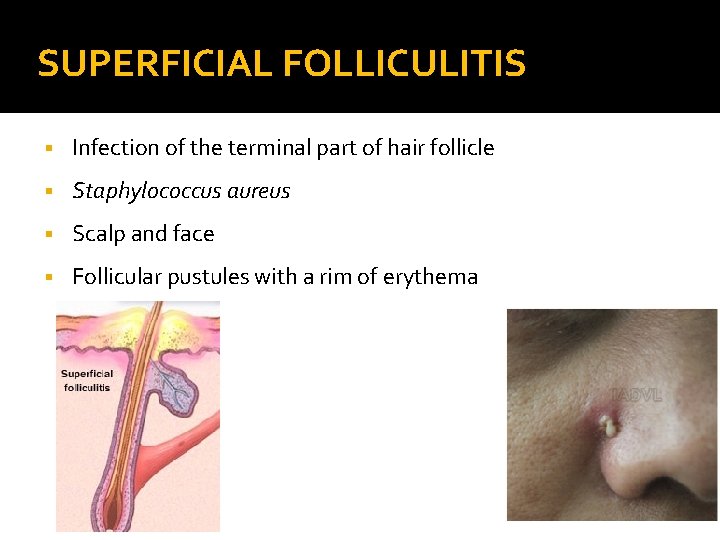
SUPERFICIAL FOLLICULITIS § Infection of the terminal part of hair follicle § Staphylococcus aureus § Scalp and face § Follicular pustules with a rim of erythema
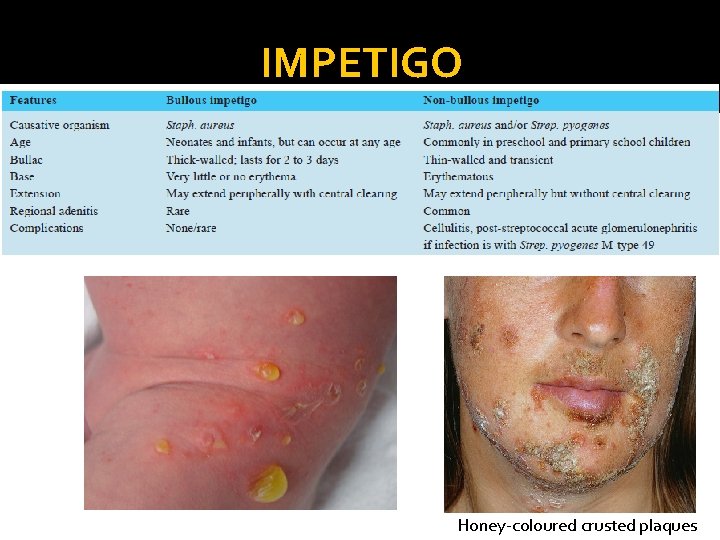
IMPETIGO Honey-coloured crusted plaques
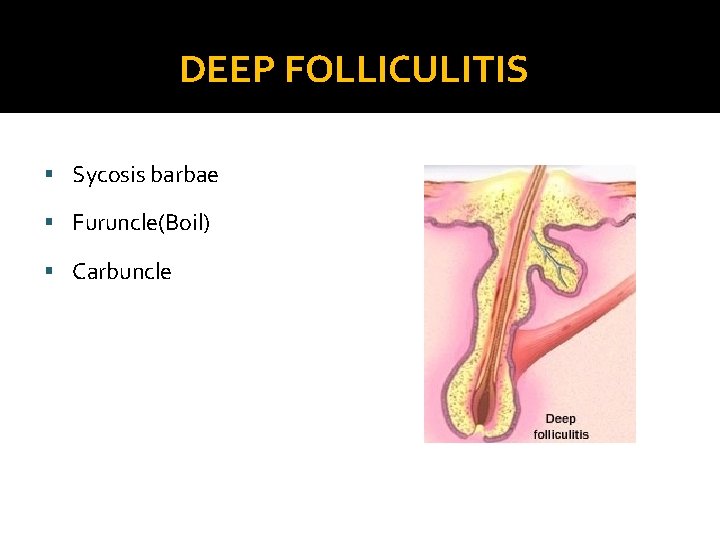
DEEP FOLLICULITIS § Sycosis barbae § Furuncle(Boil) § Carbuncle
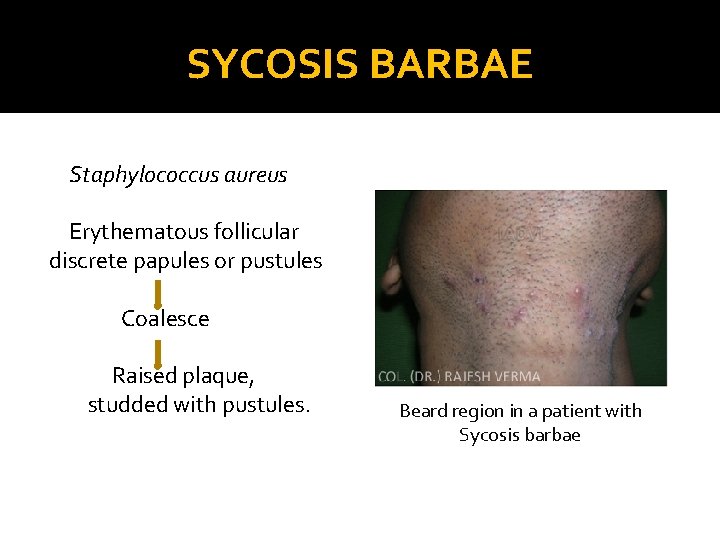
SYCOSIS BARBAE Staphylococcus aureus Erythematous follicular discrete papules or pustules Coalesce Raised plaque, studded with pustules. Beard region in a patient with Sycosis barbae
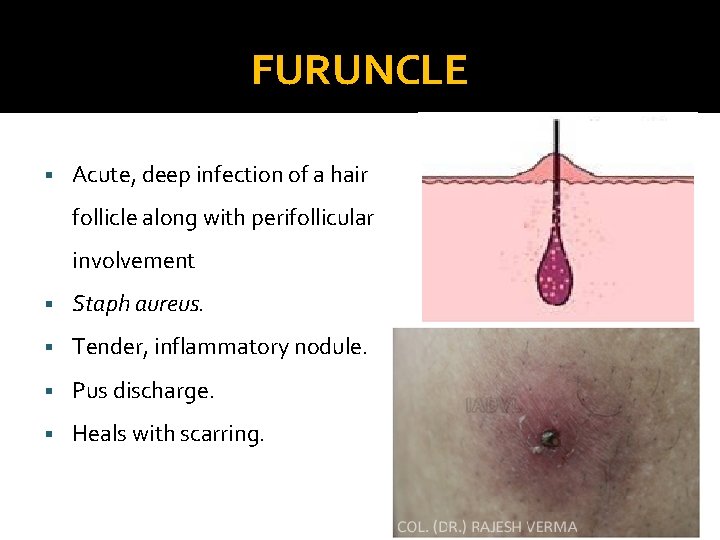
FURUNCLE § Acute, deep infection of a hair follicle along with perifollicular involvement § Staph aureus. § Tender, inflammatory nodule. § Pus discharge. § Heals with scarring.
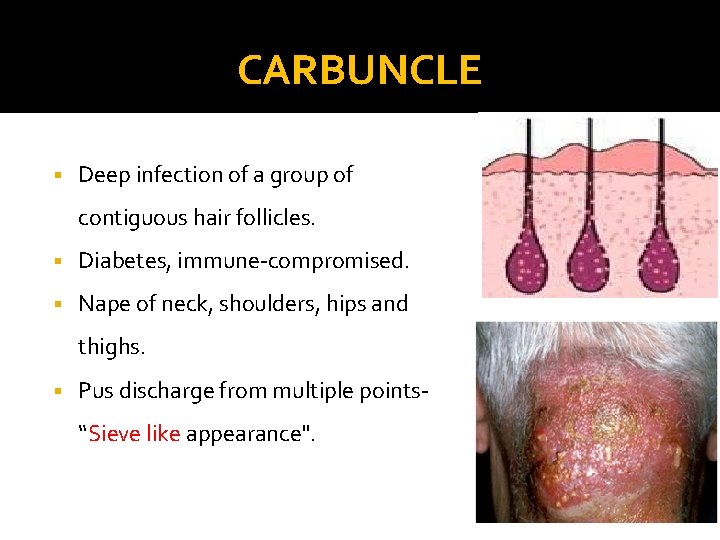
CARBUNCLE § Deep infection of a group of contiguous hair follicles. § Diabetes, immune-compromised. § Nape of neck, shoulders, hips and thighs. § Pus discharge from multiple points“Sieve like appearance".
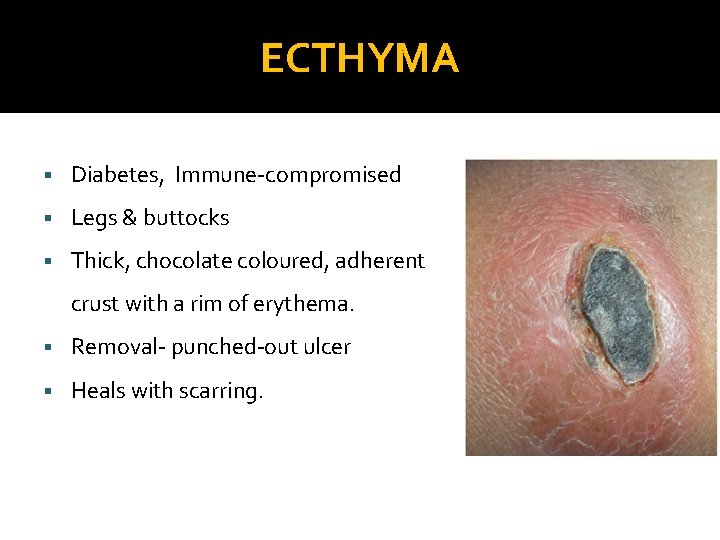
ECTHYMA § Diabetes, Immune-compromised § Legs & buttocks § Thick, chocolate coloured, adherent crust with a rim of erythema. § Removal- punched-out ulcer § Heals with scarring.
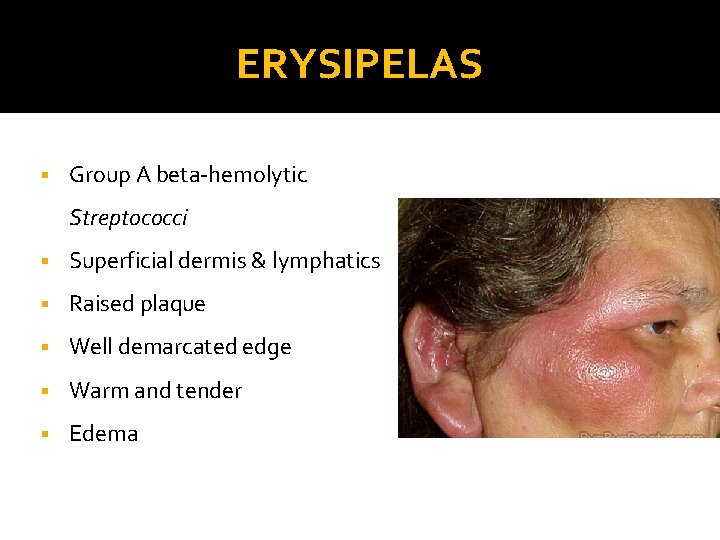
ERYSIPELAS § Group A beta-hemolytic Streptococci § Superficial dermis & lymphatics § Raised plaque § Well demarcated edge § Warm and tender § Edema
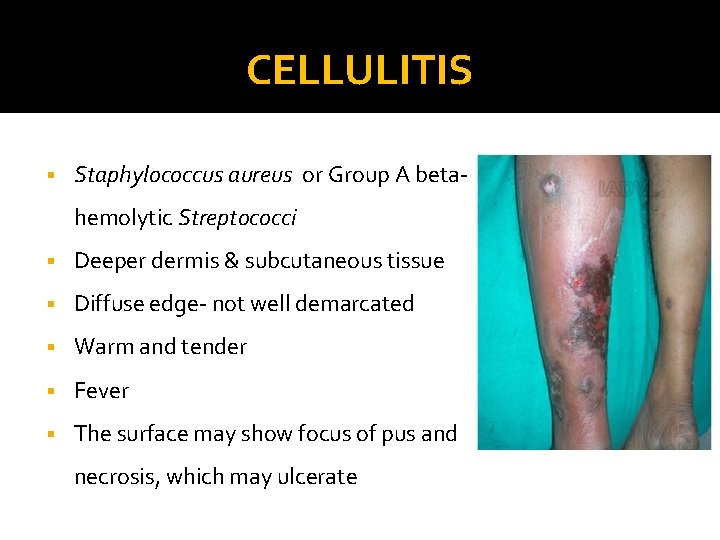
CELLULITIS § Staphylococcus aureus or Group A betahemolytic Streptococci § Deeper dermis & subcutaneous tissue § Diffuse edge- not well demarcated § Warm and tender § Fever § The surface may show focus of pus and necrosis, which may ulcerate
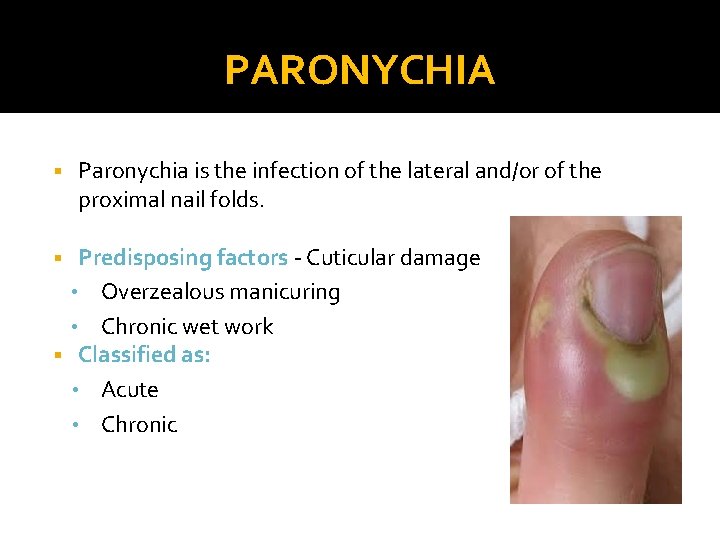
PARONYCHIA § Paronychia is the infection of the lateral and/or of the proximal nail folds. Predisposing factors - Cuticular damage • Overzealous manicuring • Chronic wet work § Classified as: • Acute • Chronic §
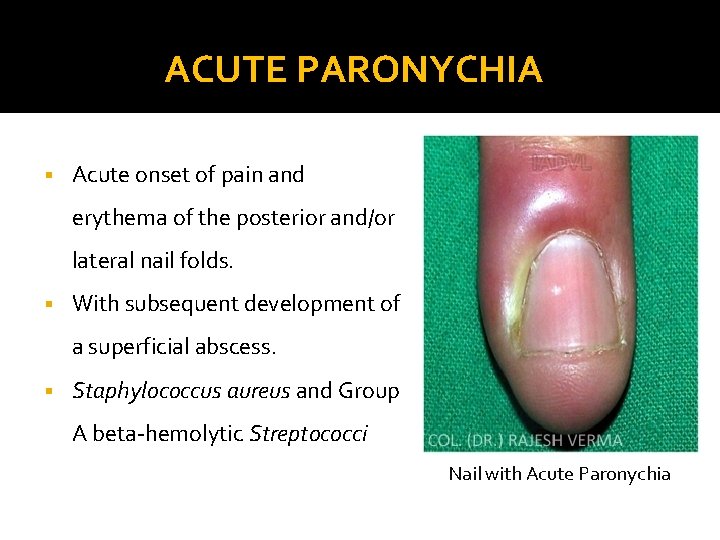
ACUTE PARONYCHIA § Acute onset of pain and erythema of the posterior and/or lateral nail folds. § With subsequent development of a superficial abscess. § Staphylococcus aureus and Group A beta-hemolytic Streptococci Nail with Acute Paronychia

ACUTE PARONYCHIA § Treatment: • Topical : – Warm compresses or soaks – Topical antibiotics • Systemic antibiotics & NSAIDs • Systemic : – Antibiotics – NSAIDs • Surgical : – Incision and drainage. without abscess with abscess

CHRONIC PARONYCHIA § Etiology : • Damage to cuticle of nail • Chronic Eczema • Chronic Candida infection § Treatment : • Keeping hands as dry as possible • Avoid irritants and allergens • Anti-fungals and corticosteroids
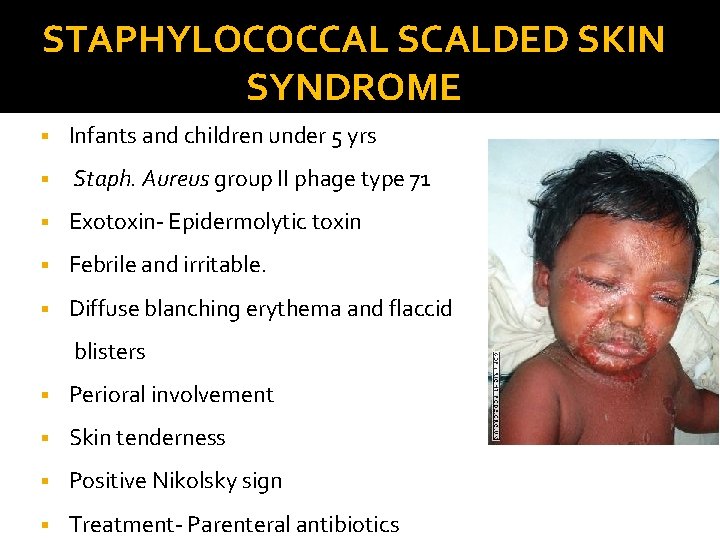
STAPHYLOCOCCAL SCALDED SKIN SYNDROME § Infants and children under 5 yrs § Staph. Aureus group II phage type 71 § Exotoxin- Epidermolytic toxin § Febrile and irritable. § Diffuse blanching erythema and flaccid blisters § Perioral involvement § Skin tenderness § Positive Nikolsky sign § Treatment- Parenteral antibiotics

MANAGEMENT PRINCIPLES § Identify and assess the predisposing factors : • Poor hygiene • Malnutrition • Recurrent trauma • Diabetes mellitus • Pre existing skin diseases • Congenital and acquired Immunodeficiency § Investigations : • Work up for any predisposing factors. • Smear, Culture and Antibiotic Sensitivity test (SCABS).

MANAGEMENT PRINCIPLES : TOPICAL THERAPY § § Soaks / compresses : Condy’s solution (KMNO 4) Topical antibiotics: • Mupirocin • Fusidic acid • Framycetin • Nadifloxacin • Bacitracin Topical agents used in the treatment of Pyodermas

MANAGEMENT PRINCIPLES : SYSTEMIC THERAPY § • • • Indications of systemic therapy : Fever, tachycardia Regional lymphadenopathy Danger area of face Pyodermas not responding to topical therapy Rapidly progressing pyodermas Available systemic agents : Semi-synthetic Penicillins Cephalosporins Macrolides Tetracyclines Quinolones
VIRAL INFECTIONS § Molluscum contagiosum § Human papilloma virus infection § Herpes simplex infection § Herpes zoster infection § Oral hairy leukoplakia
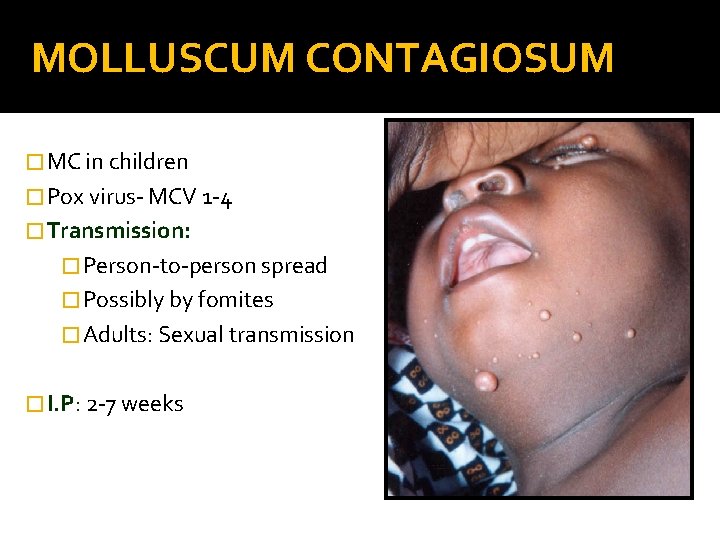
MOLLUSCUM CONTAGIOSUM � MC in children � Pox virus- MCV 1 -4 � Transmission: � Person-to-person spread � Possibly by fomites � Adults: Sexual transmission � I. P: 2 -7 weeks
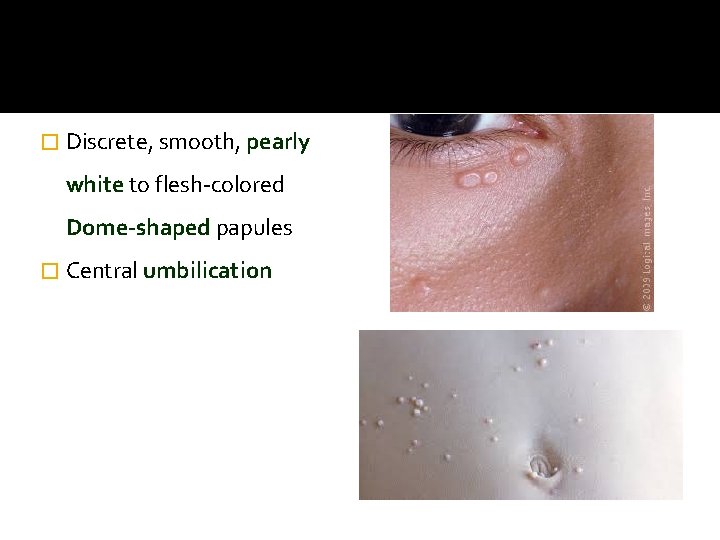
� Discrete, smooth, pearly white to flesh-colored Dome-shaped papules � Central umbilication

� Intracytoplasmic inclusion bodies: Molluscum bodies or Henderson-Paterson bodies � Treatment: � Curettage � 10 % KOH, 0. 5 % podophyllotoxin, Imiquimod cream � Cryotherapy with liquid nitrogen

VIRAL WARTS � Human papilloma virus- more than 100 types � Benign proliferations of the skin and mucosa § Transmission : direct or indirect contact (nail biters, shaving, occupational, swimming pool) § Sexual transmission : genital / perianal wart § Autoinoculation
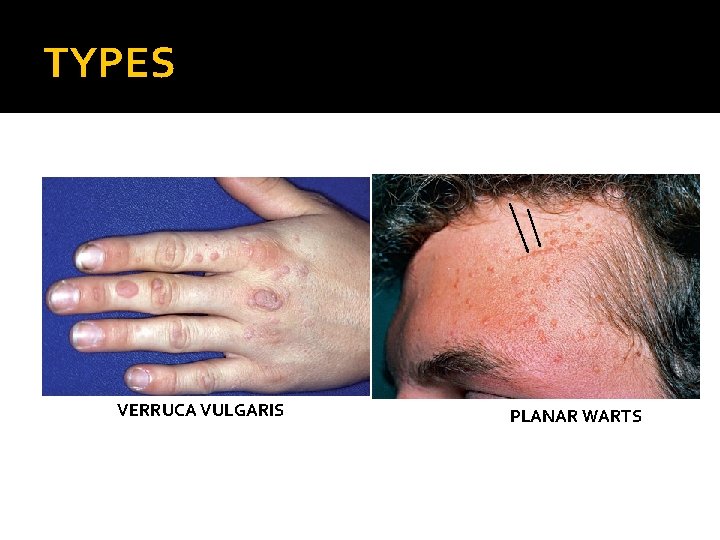
TYPES VERRUCA VULGARIS PLANAR WARTS
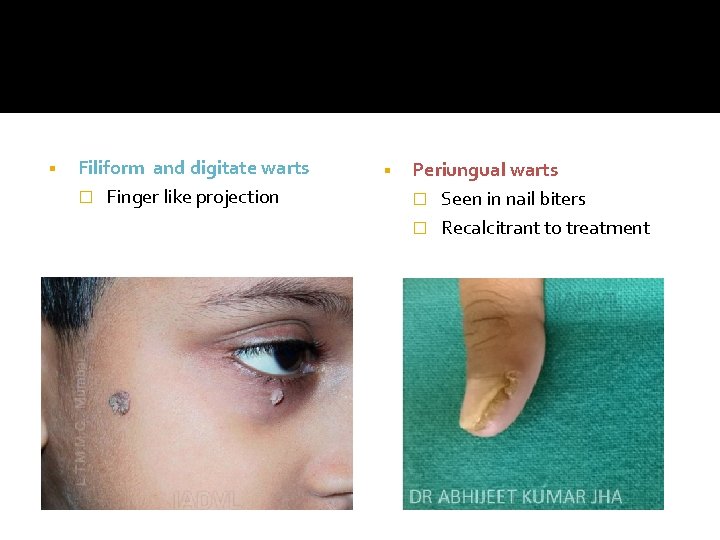
§ Filiform and digitate warts � Finger like projection § Periungual warts � Seen in nail biters � Recalcitrant to treatment
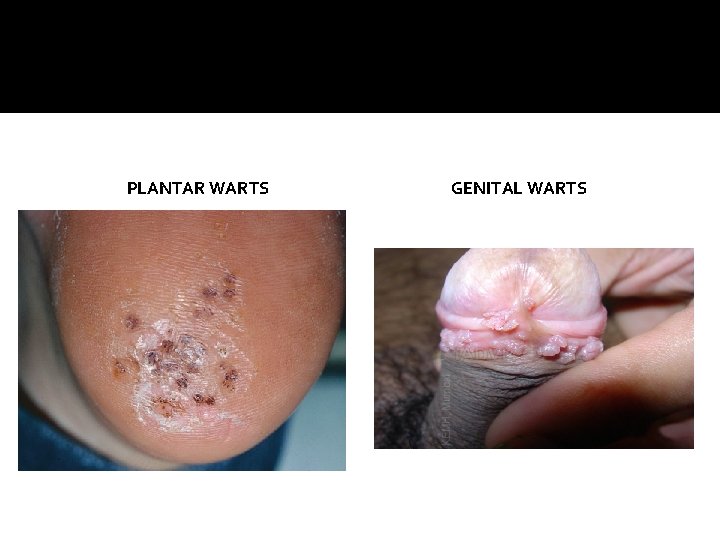
PLANTAR WARTS GENITAL WARTS

Treatment � Electrocautery � Cryotherapy � Topical salicylic acid � CO 2 laser � Podophyllin application for genital warts � Risk of development of carcinomas- HPV 16, 18

HERPES VIRUS INFECTIONS 1. Herpes simplex virus 1(HSV-1) 2. Herpes simplex virus 2 (HSV-2) 3. Varicella Zoster Virus (VZV) 4. Epstein Barr virus (EBV)- Oral Hairy Leukoplakia 5. Cytomegalovirus (CMV) 6. HHV 6 (exanthem subitum or roseola infantum) 7. HHV-7 8. HHV 8 (Kaposi's sarcoma-associated herpes virus).
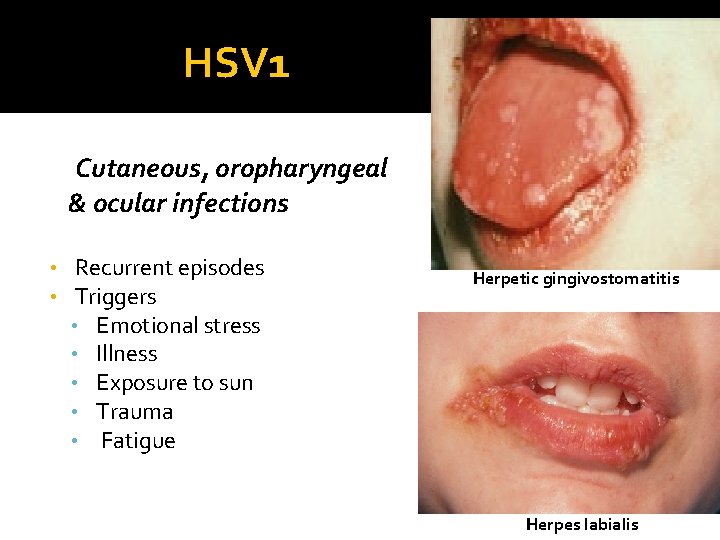
HSV 1 Cutaneous, oropharyngeal & ocular infections • • Recurrent episodes Triggers • Emotional stress • Illness • Exposure to sun • Trauma • Fatigue Herpetic gingivostomatitis Herpes labialis
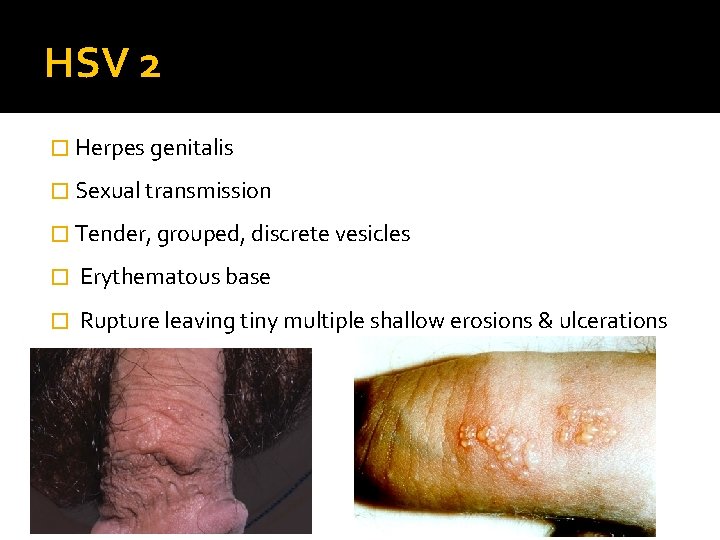
HSV 2 � Herpes genitalis � Sexual transmission � Tender, grouped, discrete vesicles � Erythematous base � Rupture leaving tiny multiple shallow erosions & ulcerations
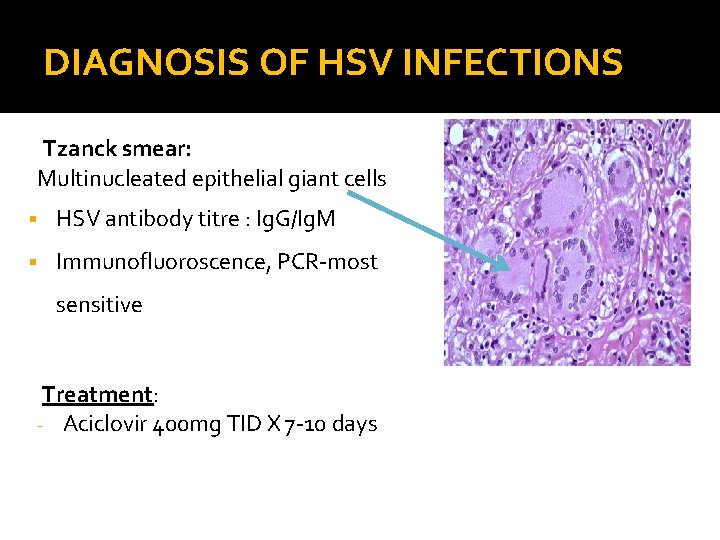
DIAGNOSIS OF HSV INFECTIONS Tzanck smear: Multinucleated epithelial giant cells § HSV antibody titre : Ig. G/Ig. M § Immunofluoroscence, PCR-most sensitive Treatment: - Aciclovir 400 mg TID X 7 -10 days
VARICELLA ZOSTER VIRUS � Varicella: � Primary infection with a viremic stage � Persistence of the virus in dorsal nerve root ganglion � Zoster: Reactivation of this residual latent virus. � Route of transmission: Droplet infection � Infectious period: 2 days- Rash -5 days
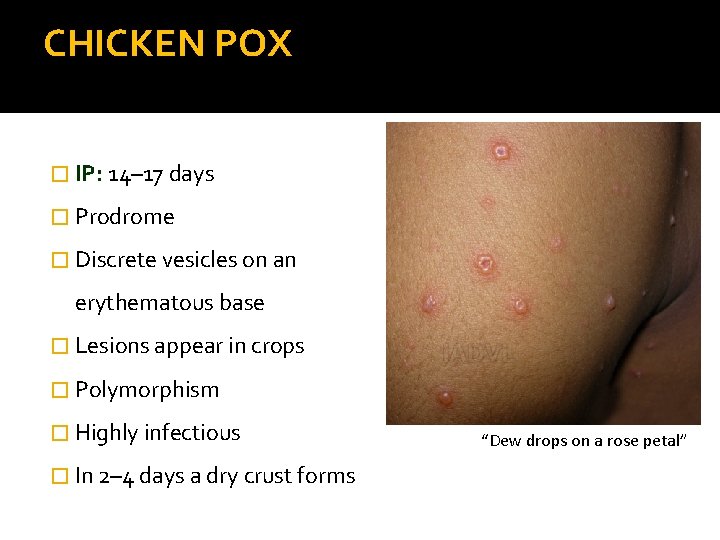
CHICKEN POX � IP: 14– 17 days � Prodrome � Discrete vesicles on an erythematous base � Lesions appear in crops � Polymorphism � Highly infectious � In 2– 4 days a dry crust forms “Dew drops on a rose petal”

§ Secondary bacterial infection may result in scarring. § Other complications : � § Pneumonia : neonates and adults (1/400) Treatment : � Acyclovir (800 mg 5 times a day/1 week) for severe cases, high risk individuals and adults (>13 years). � Isolate from immunocompromised.
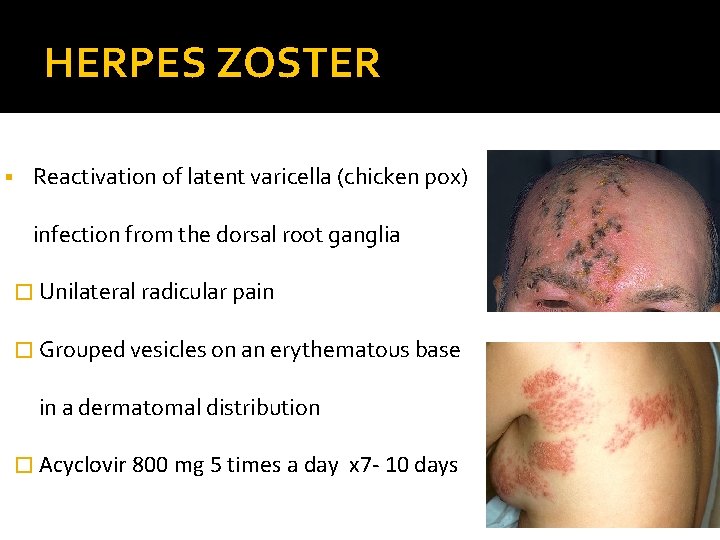
HERPES ZOSTER § Reactivation of latent varicella (chicken pox) infection from the dorsal root ganglia � Unilateral radicular pain � Grouped vesicles on an erythematous base in a dermatomal distribution � Acyclovir 800 mg 5 times a day x 7 - 10 days

Disseminated Zoster § Defined as >20 vesicles outside dermatome. § Elderly or Immunocompromised § Hemorrhagic/gangrenous lesions with outlying vesicles or bullae. § Systemic symptoms include fever, meningeal irritation. Complications: Post-herpetic neuralgia
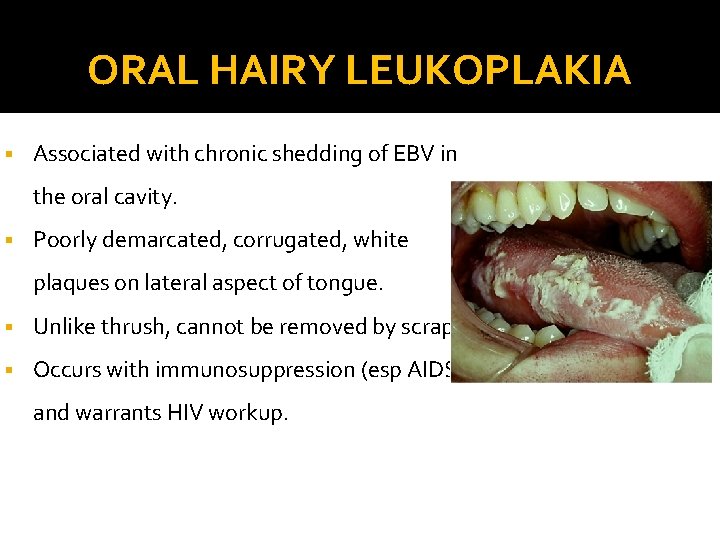
ORAL HAIRY LEUKOPLAKIA § Associated with chronic shedding of EBV in the oral cavity. § Poorly demarcated, corrugated, white plaques on lateral aspect of tongue. § Unlike thrush, cannot be removed by scraping. § Occurs with immunosuppression (esp AIDS) and warrants HIV workup.

THANK YOU
- Slides: 41