Bacterial and Curable STDs Gonorrhea Chlamydia Syphilis and

Bacterial and Curable STDs Gonorrhea, Chlamydia, Syphilis and Trichomoniasis Jeffrey D. Klausner, MD, MPH Professor of Medicine and Public Health Attending Physician Ronald Reagan Medical Center Program in Global Health and Division of Infectious Diseases David Geffen School of Medicine Department of Epidemiology Karin and Jonathan Fielding School of Public Health AAHIVU August 2014

Disclosures • • • Dr. Klausner is a faculty member of the University of California Los Angeles Dr. Klausner is a guest researcher with the US CDC Mycotics Diseases Branch Dr. Klausner is a member of the WHO STD Guidelines group Dr. Klausner is a board member of YTH, Inc, non-profit Dr. Klausner is medical advisor for Healthvana. com • In the past 12 months, Dr. Klausner has received: – Travel support for meeting coordination and speaking from Standard Diagnostics, Inc. – Research funding or donated supplies from the NIH, CDC, Hologic, Inc. , Alere, Inc. , Chembio, Inc. Cepheid, Standard Diagnostics, Inc. , and Med. Mira, Inc. JDKlausner@mednet. ucla. edu

Today’s talk • • Gonorrhea Chlamydia Syphilis Trichomoniasis
Case • 28 year old man with urethral discharge 4

Name of piercing ? a) Prince Charles b) Prince Harry c) Prince William d) Prince Albert

Prince Albert ring • • • The Prince Albert is one of the more common male genital piercings The Prince Albert is a ring-style piercing that extends along the underside of the glans from the urethral opening to where the glans meets the shaft of the penis Legend has it that Prince Albert used the ring to fix his penis to his thigh while wearing pants in court Ferguson, H. Body Piercing. BMJ 1999 6

Differential diagnosis of urethritis • Infectious Neisseria gonorrhoeae Chlamydia trachomatis Mycoplasma genitalium Trichomonas vaginalis Herpes simplex virus 1 and 2 Oral flora---streptococci, anaerobes, haemophilus sp. , adenoviruses • Non-infectious Trauma--physical or chemical (drugs), post-catheterization or sex-play related Autoimmune--Reiter’s syndrome
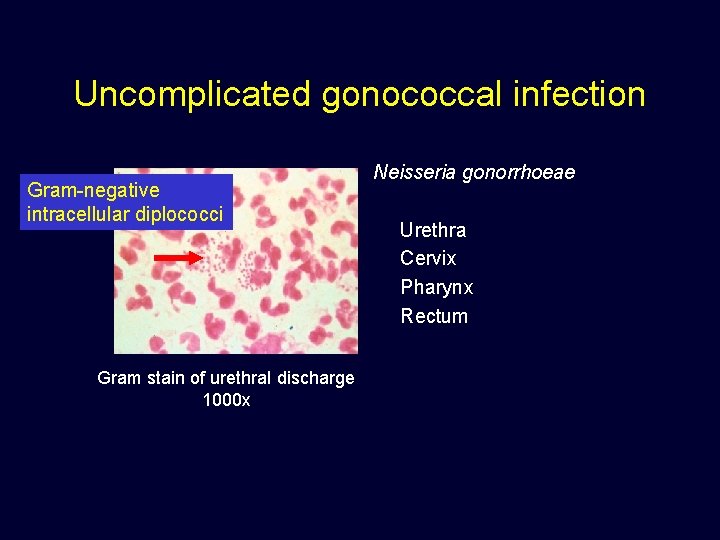
Uncomplicated gonococcal infection Gram-negative intracellular diplococci Gram stain of urethral discharge 1000 x Neisseria gonorrhoeae Urethra Cervix Pharynx Rectum

Detection of gonococcal infection § § Gram stain sensitivity specificity Culture sensitivity specificity 92% 90% 95% 99% • Nucleic acid amplification tests (NAATs) – PCR, SDA, TMA sensitivity 95% specificity >99. 7% -- NAATs FDA-cleared in urethra, cervix, urine, vagina, self-obtained vaginal specimens – Verified in pharynx and rectum

Gonorrhea—Rates, United States, 1941– 2012 -Fig 11. SR, Pg 19

Gonorrhea—Rates by County, United States, 2012 -Fig 20. SR, Pg 21

Gonorrhea—Rates by Age and Sex, United States, 2012 -Fig 21. SR, Pg 21

Gonorrhea—Rates by Race/Ethnicity, United States, 2008– 2012 †NHOPI = Native Hawaiian and Other Pacific Islanders. NOTE: Includes 38 states and the District of Columbia reporting race/ethnicity data in Office of Management and Budget compliant formats during 2008– 2012 -Fig 19. SR, Pg 23

Percentage of Isolates in Which Minimal Inhibitory Concentrations (MICs) of Cefixime Were 0. 25 μg/m. L or Higher, 2005– 2011 Bolan GA et al. N Engl J Med; Feb. , 2012 14

What is the current recommended treatment for gonorrhea? A) Ceftriaxone 250 mg IM once B) Ceftriaxone 250 mg IM once + azithromycin 1 gm PO once C) Ceftriaxone 250 mg IM once + doxycycline 100 mg PO once D) Cefixime 400 mg PO once E) Ciprofloxacin 500 mg PO once + azithromycin 1 gm PO once Plus partner treatment 15 MMWR CDC STD Treatment Guidelines Update, August 2012

Multi-drug treatment for gonorrhea Ceftriaxone 250 mg IM once AND azithromycin 1 gm PO once or doxycycline 100 mg PO twice daily x 7 days Plus partner treatment Retesting at 3 months 16 MMWR CDC STD Treatment Guidelines Update, August 2012

Penicillin, Tetracycline, and Ciprofloxacin Resistance Among Neisseria gonorrhoeae Isolates, 2012 NOTE: Pen. R = penicillinase producing Neisseria gonorrhoeae and chromosomally mediated penicillinresistant N. gonorrhoeae; Tet. R = chromosomally and plasmid mediated tetracycline-resistant N. gonorrhoeae; and QRNG = quinolone-resistant N. gonorrhoeae. 2012 -Fig 27. SR, Pg 27

Fluoroquinolone resistance in Neisseria gonorrhoeae 18
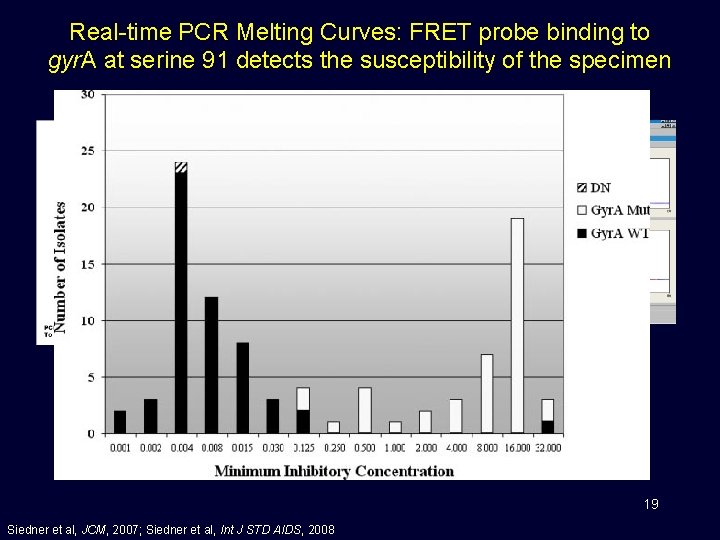
Real-time PCR Melting Curves: FRET probe binding to gyr. A at serine 91 detects the susceptibility of the specimen 19 Siedner et al, JCM, 2007; Siedner et al, Int J STD AIDS, 2008

Molecular-based resistance testing • Rapid detection of NG • Simultaneous detection of key antimicrobial resistance profile • Enable targeted treatment • Reduce antibiotic selection pressure • Decrease emergence of resistance UNDER DEVELOPMENT-R 21 AI 109005 20

Case 19 year old female used Sex. Info text message service (Text “Sex. Info” to 61827) and comes in for a check-up. She has one regular partner for 6 months and has no symptoms. What STD screening tests are appropriate?

Recommended STI screening in sexually active female < 25 years • Chlamydia trachomatis and Neisseria gonorrhoeae, annually • HIV test Consider Trichomonas vaginalis (increased risk) Herpes simplex virus type 2 antibody Avoid PAP smear (only if sexually active > 3 years) Syphilis USPSTF, 2013; AAP July 2014
Screening tests for chlamydial infection • Nucleic acid amplification tests – DNA amplification (Roche, Bayer, Abbott, BD, Seimens, Cepheid) – RNA amplification (Hologic)
Options for specimen collection 1) Cervical swab 2) Vaginal swab 3) Self-collected vaginal swab 4) Urine 5) Rectal swab 6) Self-collected rectal swab

Rectal Chlamydia Positivity, San Francisco (n=6, 861) Mean positivity 8. 4% (n=576+) 25
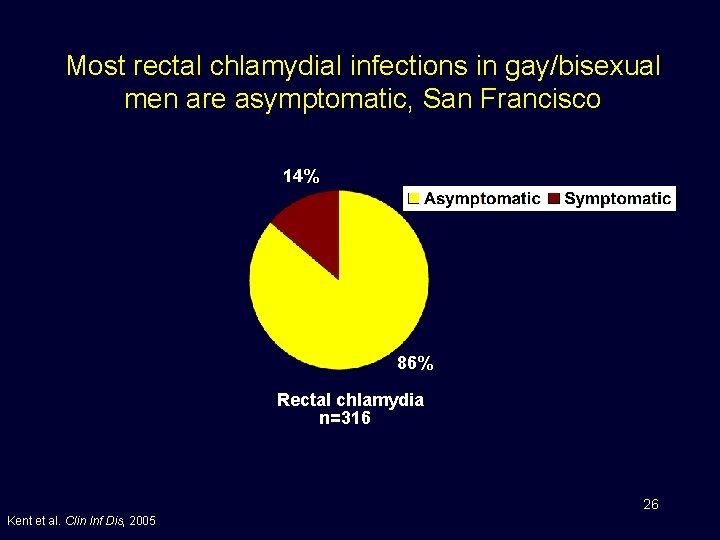
Most rectal chlamydial infections in gay/bisexual men are asymptomatic, San Francisco 14% 86% Rectal chlamydia n=316 26 Kent et al. Clin Inf Dis, 2005
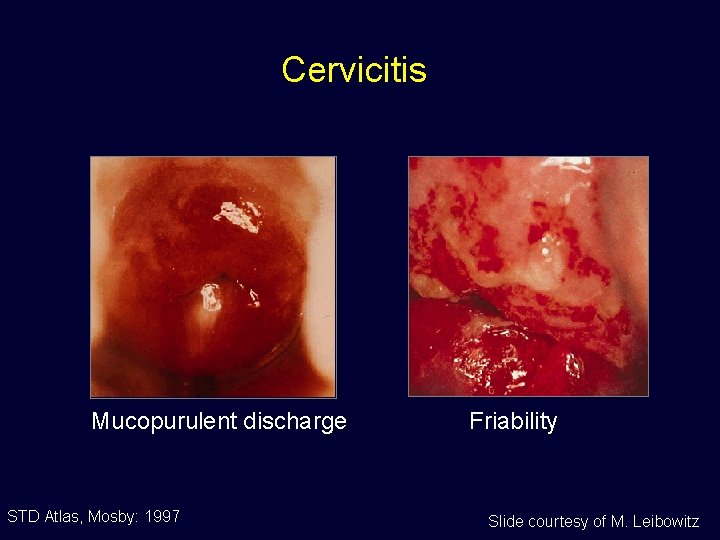
Cervicitis Mucopurulent discharge STD Atlas, Mosby: 1997 Friability Slide courtesy of M. Leibowitz
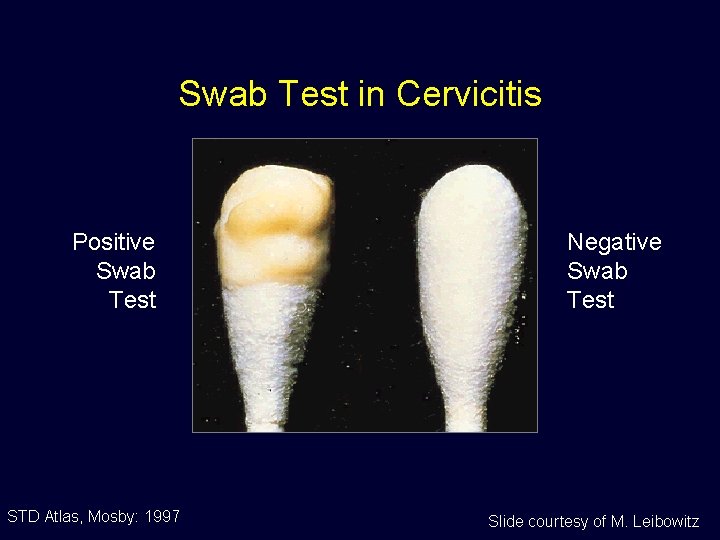
Swab Test in Cervicitis Positive Swab Test STD Atlas, Mosby: 1997 Negative Swab Test Slide courtesy of M. Leibowitz

What is best treatment for uncomplicated chlamydial infection? 1) 2) 3) 4) 5) Azithromycin 1 gm orally once Doxycycline 100 mg orally twice daily for 7 days Amoxicillin 500 mg po tid x 7 days Levofloxacin 500 mg po qd x 7 days None of the above

Treatment for uncomplicated chlamydial infection 1) 2) 3) 4) Azithromycin 1 gm orally once Doxycycline 100 mg orally twice daily for 7 days Amoxicillin 500 mg po tid x 7 days Levofloxacin 500 mg po qd x 7 days • Partner treatment 1) SB 648, CA Law January 2001 1) Re-testing at 3 months

Chlamydia—Rates by Sex, United States, 1992– 2012 NOTE: As of January 2000, all 50 states and the District of Columbia have regulations that require the reporting of chlamydia cases. 2012 -Fig 1. SR, Pg 9
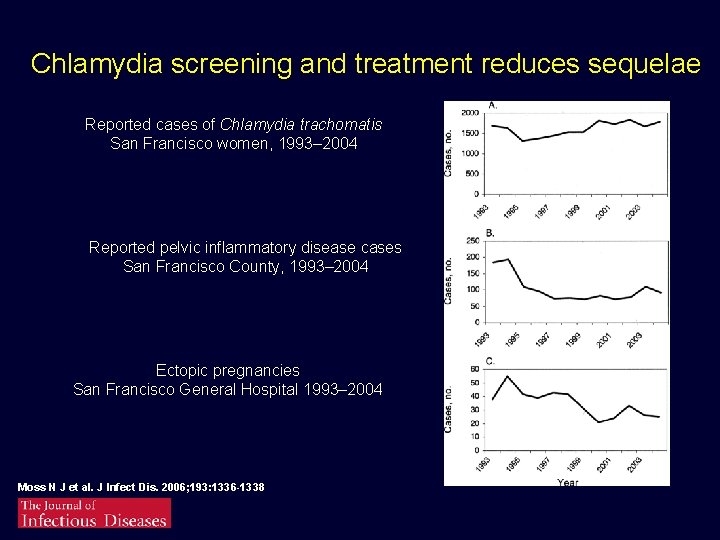
Chlamydia screening and treatment reduces sequelae Reported cases of Chlamydia trachomatis San Francisco women, 1993– 2004 Reported pelvic inflammatory disease cases San Francisco County, 1993– 2004 Ectopic pregnancies San Francisco General Hospital 1993– 2004 Moss N J et al. J Infect Dis. 2006; 193: 1336 -1338

Chlamydia—Prevalence Among Persons Aged 14– 39 Years by Sex, Race/Ethnicity, or Age Group, National Health and Nutrition Examination Survey, 2005– 2008 NOTE: Error bars indicate 95% confidence intervals. 2012 -Fig 10. SR, Pg 13
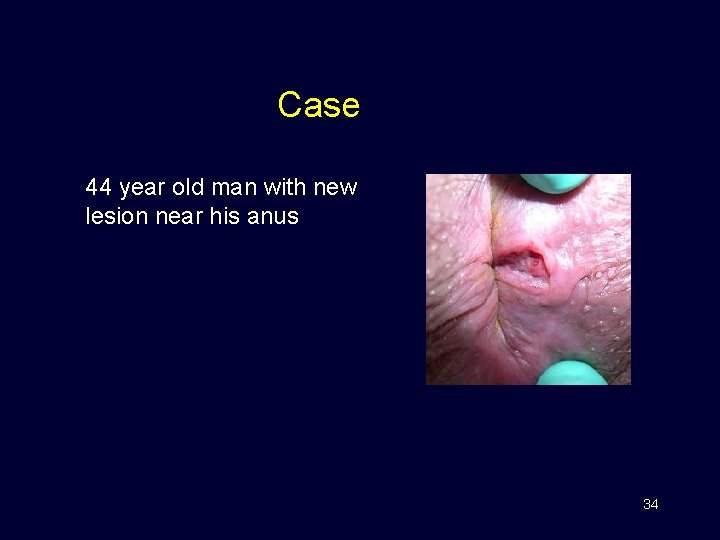
Case 44 year old man with new lesion near his anus 34

Differential diagnosis of anogenital ulcer Sexually transmitted diseases Other • Primary syphilis • Genital herpes • Chancroid • Fixed drug reactions – NSAIDs, tetracyclines, foscarnet • Skin flora infections • Autoimmune conditions
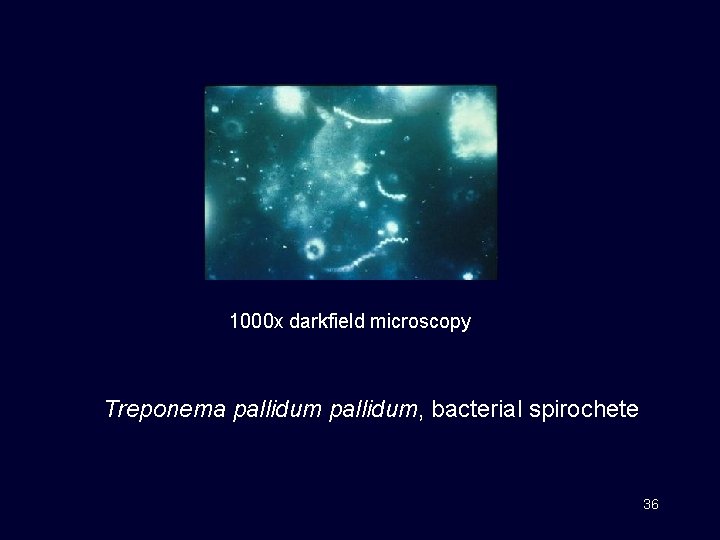
1000 x darkfield microscopy Treponema pallidum, bacterial spirochete 36

All those syphilis tests • Non-treponemal tests (RPR, VDRL) – – Antibody to cardiolipin-lecithin-phospholipids Rise and fall with infection and treatment over time 4 -fold change in titer (1: 2 to 1: 8 or 1: 64 to 1: 16) is significant Specificity = 98% (false-positives in IDU, auto-immune, etc) • Treponemal tests (FTA-Abs, TPPA, TP EIA) – – Antibody to Treponemal antigen More sensitive and develop earlier Stay positive for “life” (85%) Indicate past or current infection Klausner, Current STD Diagnosis and Management 2007 37
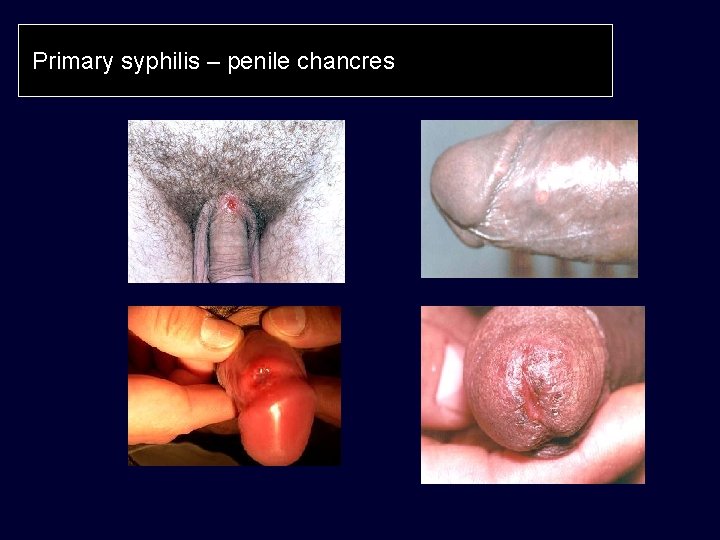
Primary syphilis – penile chancres
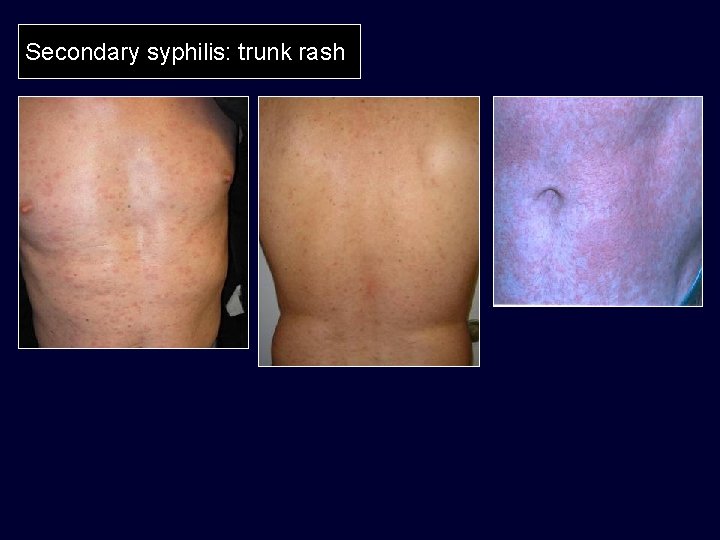
Secondary syphilis: trunk rash
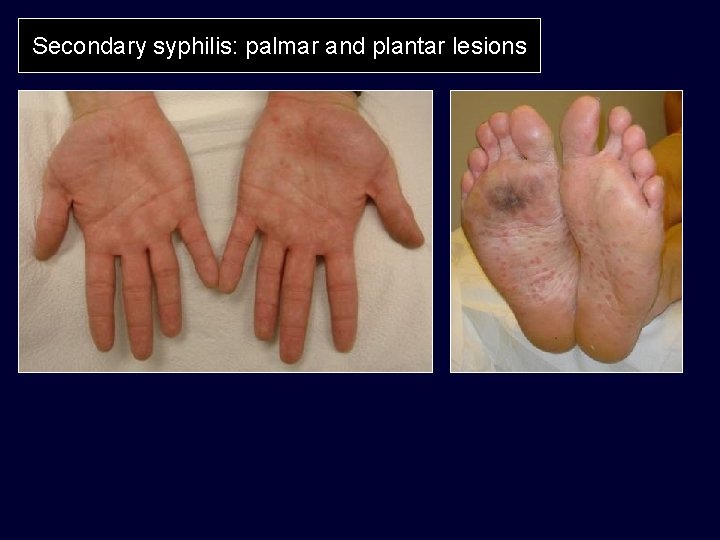
Secondary syphilis: palmar and plantar lesions
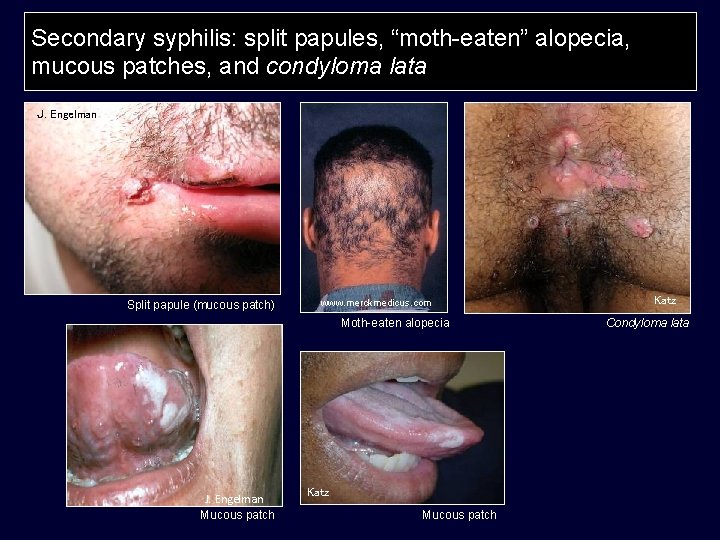
Secondary syphilis: split papules, “moth-eaten” alopecia, mucous patches, and condyloma lata J. Engelman Split papule (mucous patch) www. merckmedicus. com Moth-eaten alopecia J. Engelman Mucous patch Katz Condyloma lata

Latent syphilis This page intentionally left blank!
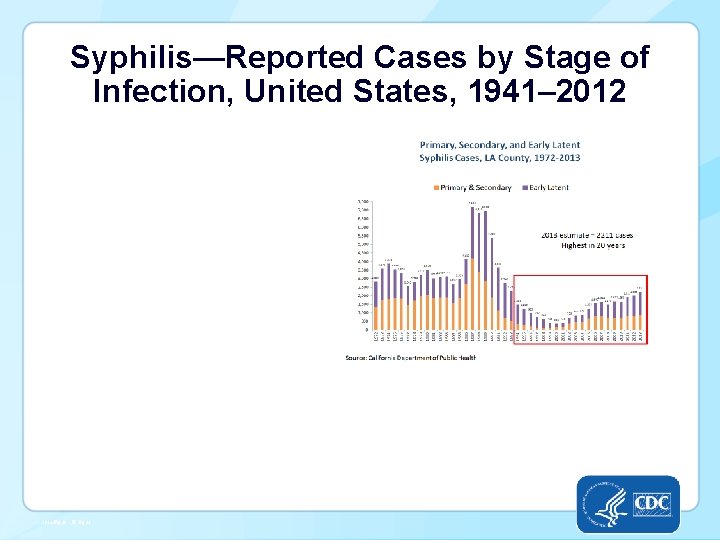
Syphilis—Reported Cases by Stage of Infection, United States, 1941– 2012 -Fig 29. SR, Pg 32

Primary and Secondary Syphilis—Rates by Age and Sex, United States, 2012 -Fig 35. SR, Pg 35

Primary and Secondary Syphilis—Rates by Race/Ethnicity, United States, 2008– 2012 * AI/AN = American Indians/Alaska Natives; NHOPI = Native Hawaiian and Other Pacific Islanders. NOTE: Includes 38 states and the District of Columbia reporting race/ethnicity data in Office of Management and Budget compliant formats during 2008 -2012 -Fig 38. SR, Pg 36

What is the recommended treatment for early syphilis? A) Azithromycin 1 gm PO once B) Azithromycin 1 gm weekly for 3 weeks C) Amoxicillin 500 mg PO tid x 7 days D) Penicillin G benzathine 2. 4 MU IM once E) Penicillin G aqueous 600, 000 U IV q 4 -6 x 10 days Plus partner treatment CDC STD Treatment Guidelines, 2010 46

Primary & Secondary and Latent < 1 year syphilis treatment HIV (-)/(+) 2. 4 million units of benzathine penicillin G-LA Pregnant 2. 4 million units of benzathine penicillin G-LA PCN-allergic: HIV(-)/(+) doxycycline 100 mg po bid x 14 d Pregnant desensitize, then benzathine penicillin G-LA • Prophylactic treatment: All contacts to syphilis within past 90 days should be treated regardless of serologic test result with benzathine penicillin G 2. 4 MU IM once CDC STD Treatment Guidelines, 2010

Syphilis and HIV infection • Multiple chancres • May present with overlapping primary and secondary manifestations • Rarely abnormal serology but slower decline • Increased risk neurosyphilis Zetola and Klausner, Clin Inf Dis 2007.
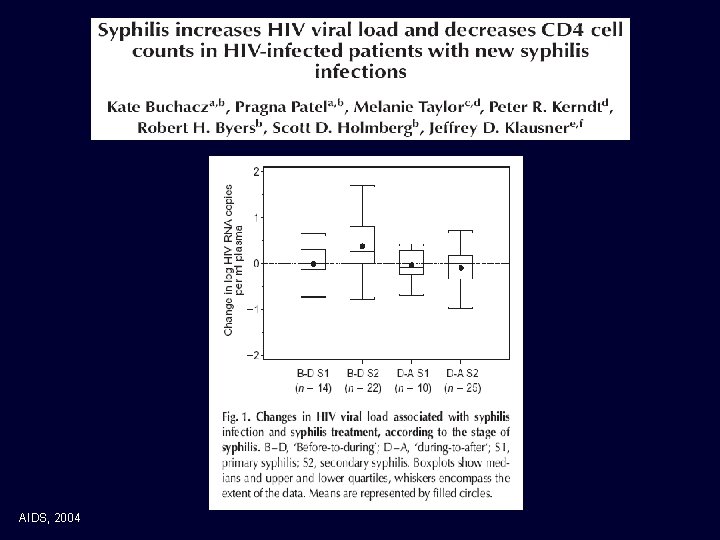
AIDS, 2004

San Francisco, 2009 San Francisco, early 2000 s Texas
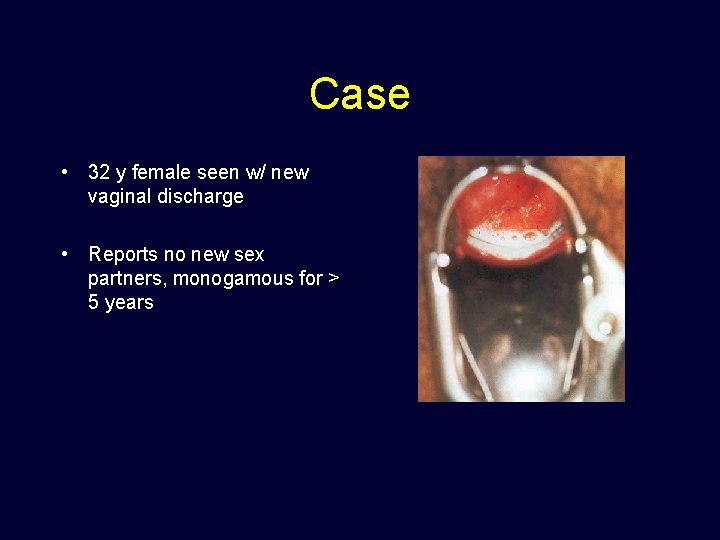
Case • 32 y female seen w/ new vaginal discharge • Reports no new sex partners, monogamous for > 5 years

Differential diagnosis of vaginal discharge • Infectious Vaginitis Trichomonas vaginalis Bacterial vaginosis Candida albicans and other Cervicitis Neisseria gonorrhoeae Chlamydia trachomatis Herpes simplex virus 1 and 2 • Non-infectious Mechanical, chemical or allergic irritation
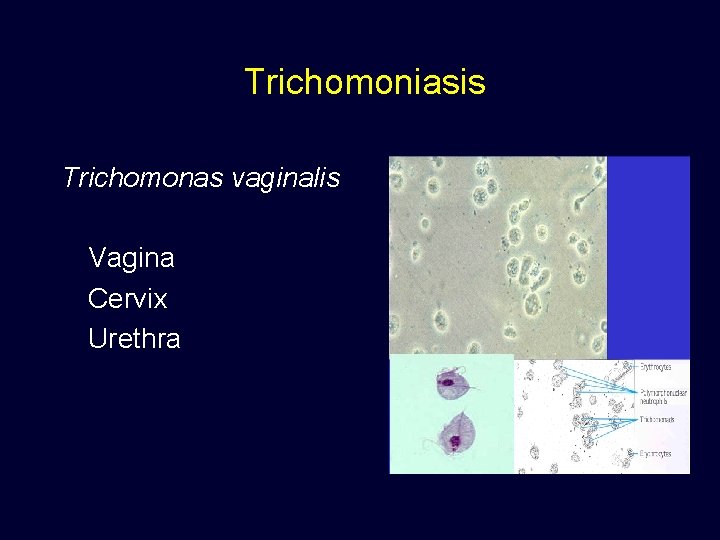
Trichomoniasis Trichomonas vaginalis Vagina Cervix Urethra
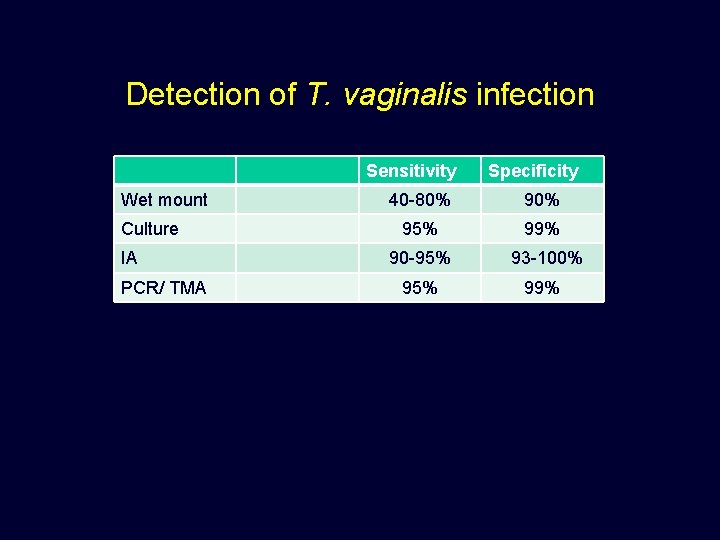
Detection of T. vaginalis infection Sensitivity Wet mount Culture IA PCR/ TMA Specificity 40 -80% 95% 99% 90 -95% 93 -100% 95% 99%

Treatment of trichomoniasis Metronidazole 2 gm po x 1 500 mg po bid x 5 -7 Cure rate 95% Partner management—Treat partners Hager D et al. , JAMA, 1980; Thin et al. , Br J Ven Dis, 1979.
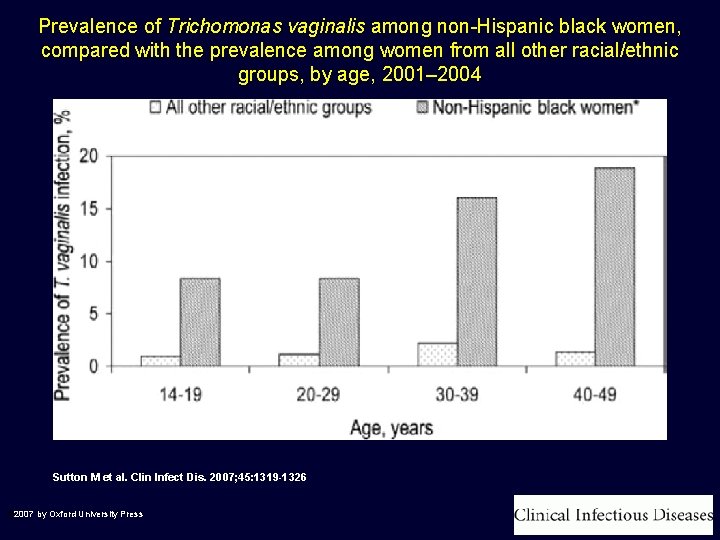
Prevalence of Trichomonas vaginalis among non-Hispanic black women, compared with the prevalence among women from all other racial/ethnic groups, by age, 2001– 2004 Sutton M et al. Clin Infect Dis. 2007; 45: 1319 -1326 © 2007 by Oxford University Press

Sources for more STD information • Me – JDKlausner@mednet. ucla. edu • CDC – www. cdc. gov/std • Current STD Management Textbook

Thank you
- Slides: 58