Back pain Pathways Common spinal problems Assessment strategies

Back pain & Pathways • Common spinal problems • Assessment strategies • Evidence based approach to treatment • Financial aspects • Pathway design and delivery
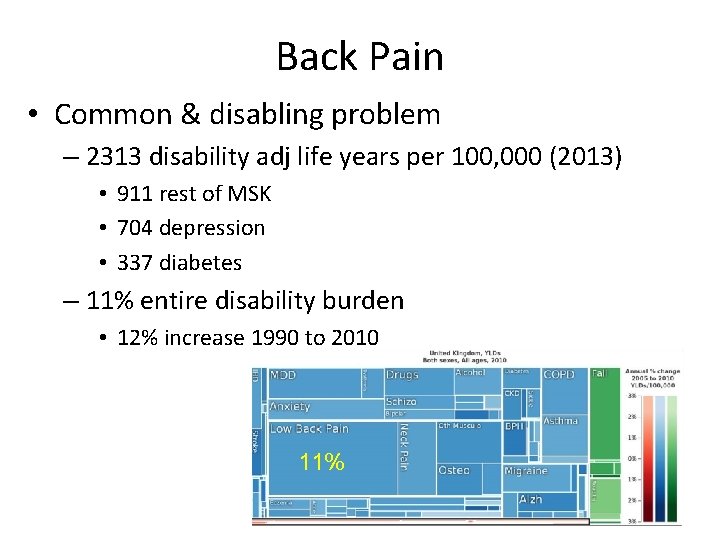
Back Pain • Common & disabling problem – 2313 disability adj life years per 100, 000 (2013) • 911 rest of MSK • 704 depression • 337 diabetes – 11% entire disability burden • 12% increase 1990 to 2010 11%

Case for Change: Back Pain Costs CG 88 NICE estimated that the cost of Back Pain to the NHS in 2008 was: £ 2. 1 billion Which is: £ 4, 133, 858. 20 per 100, 000

When to refer? • 3 priority levels of referral – Emergency = Phone call NOW to Orthopaedic Sp. R (at NGH) – Urgent = Faxed referral to NGH – Acute Spinal Clinic x 2 each week – Routine = SPA

When to refer? • 3 priority levels of referral – Emergency = Phone call NOW to Orthopaedic Sp. R (at NGH) – Urgent = Faxed referral to NGH – Acute Spinal Clinic x 2 each week – Routine = SPA

When to refer? • 3 priority levels of referral – Emergency = Phone call NOW to Orthopaedic Sp. R (at NGH) – Urgent = Faxed referral to NGH – Acute Spinal Clinic x 2 each week – Routine = SPA
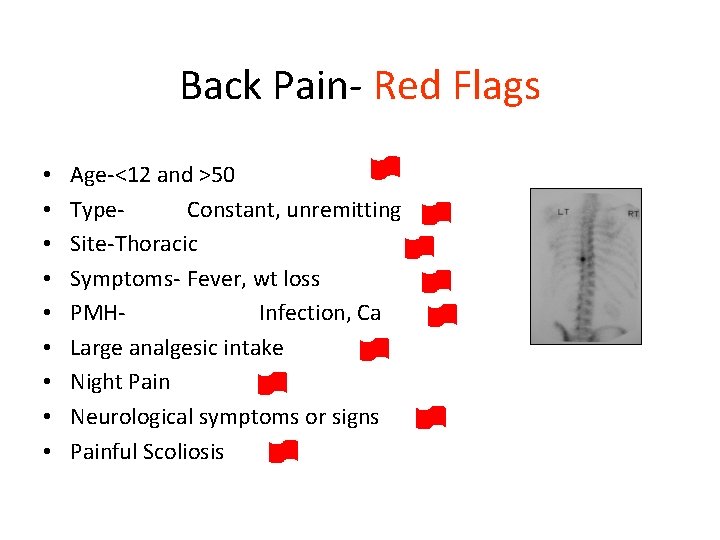
Back Pain- Red Flags • • • Age-<12 and >50 Type. Constant, unremitting Site-Thoracic Symptoms- Fever, wt loss PMHInfection, Ca Large analgesic intake Night Pain Neurological symptoms or signs Painful Scoliosis

CES • • • Back pain Bilateral leg weakness & numbness Saddle numbness Reduced anal tone, sensation, squeeze Retention of urine- leading to incontinence

Infection • Pyogenic – Discitis • • St Aureus, E Coli IVDU Elderly Immunocompromised • Non-Pyogenic – TB

Back Pain • 99% “non-specific” – Mechanical cause somewhere! – Not serious – Not curable – Reassure – Exercise – Reassure – Lose weight/ analgesia – Reassure
Axial and Radicular pain • General principles – Analgaesia – Reassure • 85% settle in 2 -3 month • Pain is not damaging – Stay mobile – CES warnings if radicular pain – No imaging • Reassess – Getting better? – Any radicular pain ? – Red flags? – Rheumatological presentation?

All in the History • Where is the pain – Back (Neck) – Buttock – Leg (Arm): distribution – % back v % leg eg 80% right leg: 20% back • How long • How severe is it and how disabling • Weakness • Bladder / Bowel function • Medical co-morbidities
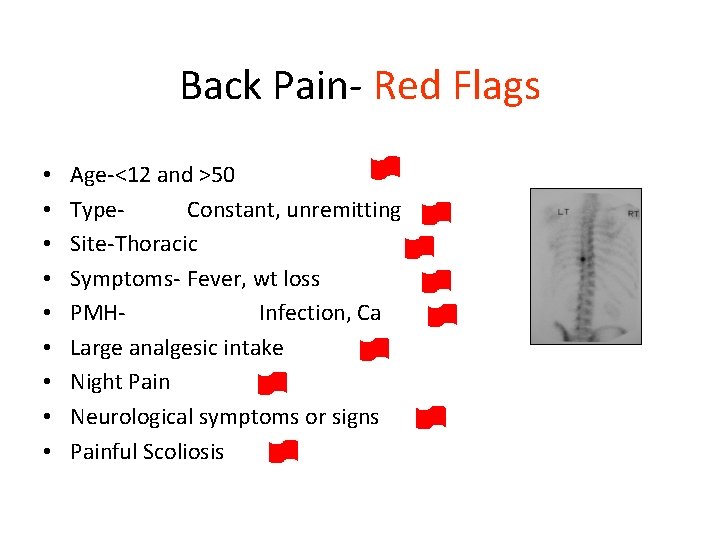
Back Pain- Red Flags • • • Age-<12 and >50 Type. Constant, unremitting Site-Thoracic Symptoms- Fever, wt loss PMHInfection, Ca Large analgesic intake Night Pain Neurological symptoms or signs Painful Scoliosis

Back Pain- Yellow flags • Beliefs- Pain is dangerous • Inappropriate illness behaviour • Compensation • Mood • Employer issues
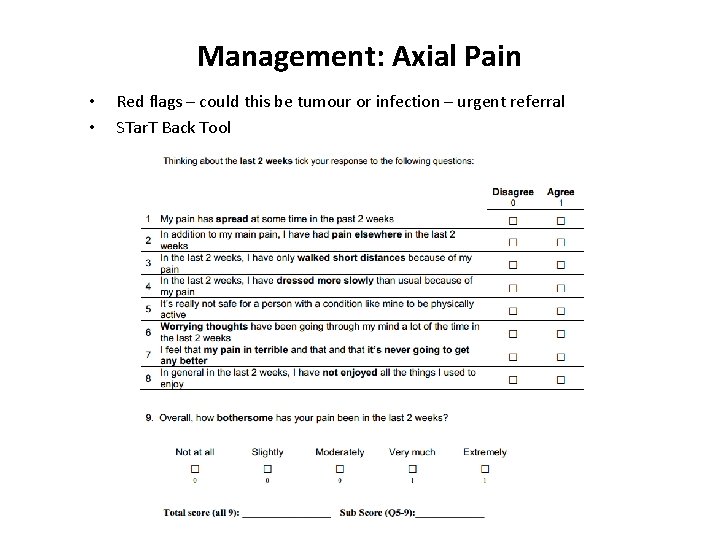
Management: Axial Pain • • Red flags – could this be tumour or infection – urgent referral STar. T Back Tool

STar. T Back Scoring Single session manual therapy & advice Manual therapy & advice 10 -12 sessions Low intensity combined physical and psychological programme
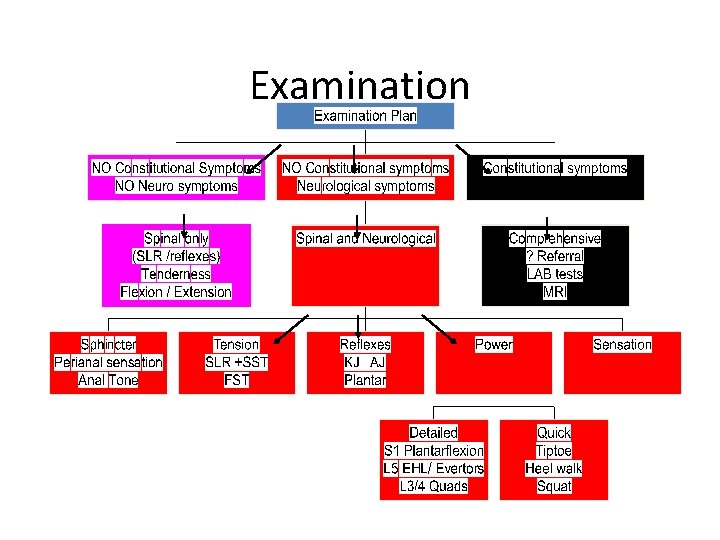
Examination
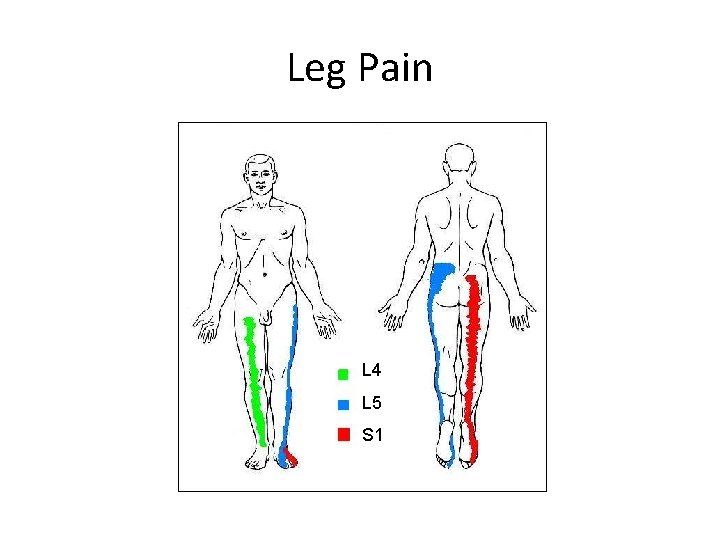
Leg Pain L 4 L 5 S 1

History - extra • Myelopathy – Clumsy hands – Unsteady legs (ataxia) • Spinal Stenosis – Buttock, thigh, calf pain / aching / heaviness / deadness / numbness on standing and walking – Eases with sitting / bending forward – few mins
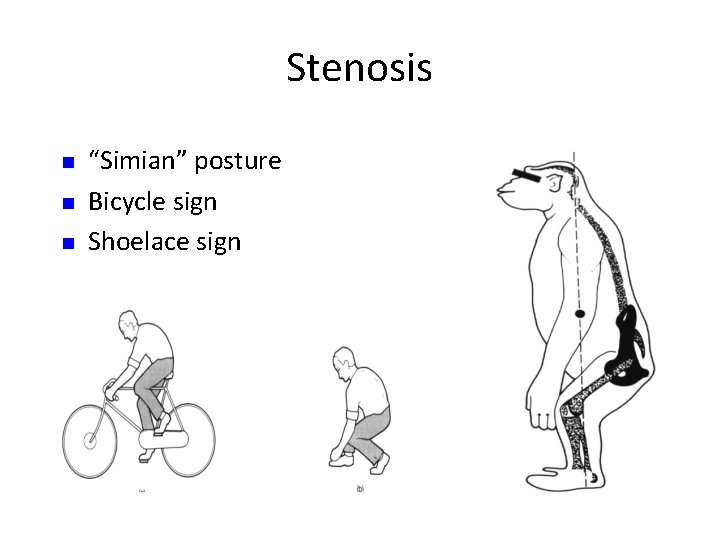
Stenosis n n n “Simian” posture Bicycle sign Shoelace sign
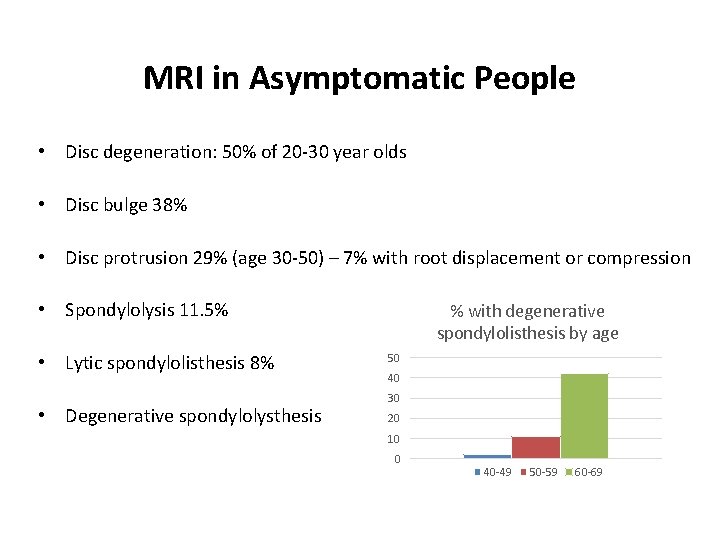
MRI in Asymptomatic People • Disc degeneration: 50% of 20 -30 year olds • Disc bulge 38% • Disc protrusion 29% (age 30 -50) – 7% with root displacement or compression • Spondylolysis 11. 5% • Lytic spondylolisthesis 8% • Degenerative spondylolysthesis % with degenerative spondylolisthesis by age 50 40 30 20 10 0 40 -49 50 -59 60 -69

Back Pain • 99% “non-specific” – Mechanical cause somewhere! – Not serious – Not curable – Reassure – Exercise – Reassure – Lose weight/ analgesia – Reassure

Back pain- Causes • • Tumour Infection Fracture Degenerate disc Spondylolysis/ spondylolisthesis Stenosis Facet degeneration

Tumour • Metastasis – Breast, prostate, renal, lung • Primary – Osteoid osteoma, osteosarcoma, chondrosarcoma • Haematogenous – Myeloma, lymphoma, leukaemia

Infection • Pyogenic – Discitis • • St Aureus, E Coli IVDU Elderly Immunocompromised • Non-Pyogenic – TB

Fracture • Traumatic • Pathological – Tumour – Osteoporosis

Degenerative • Disc Herniation – – 1 st episode 90% get better and stay better 2 nd episode 90% get better and 50% recur 3 rd episode 90 % get better and almost all recur By 3 months should be improving • 10% do not recover – 90% relief with surgery
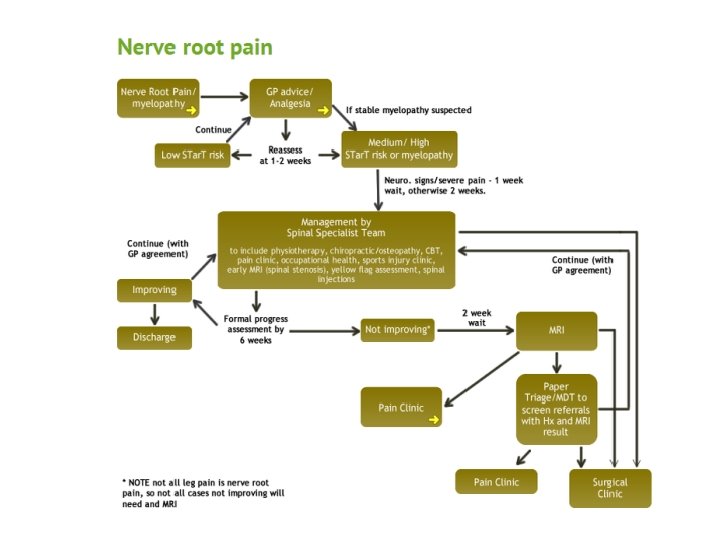

Referral to MSK Services (SPA) • Suspected CES / spinal cord compression - EMERGENCY • Severe radicular pain at any time despite analgaesia – URGENT (2 w) • Radicular weakness – URGENT (2 w) • Non-tolerable radicular pain at 6 weeks – not improving • Non-tolerable axial pain – depends on STar. T Back score

Referral to Spinal Surgeon - Back Pain • Reassurance • Investigation for possible surgery if short history (<2 yrs) and well motivated. Must have failed conservative measures including CPPP: – Spondylolisthesis – Localised degenerative change

Pathway – Benefits Realisation • Average performing CCG savings of £ 250, 000 per 100, 000 population per annum by reductions in referrals and ‘surgery’

Can I Help? • Comprehensive Spinal Service – NGH – 8 Consultant Surgeons + Fellow – 24/7 Consultant On-Call – 24/7 Imaging – Fast access clinic – Extended Scope Physios
- Slides: 32