Bacillus anthracis Amanda Russell Anna Bossert Taxonomy Kingdom

Bacillus anthracis Amanda Russell Anna Bossert

Taxonomy • • Kingdom: Bacteria Phylum: Firmicutes Class: Bacilli Order: Bacillales Family: Bacillaceae Genus: Bacillus Species: anthracis

Basic Facts • Zoonotic Disease: usually carried by animals, can be transmitted to human hosts under natural conditions • Rod-shaped • monomorphic • Endospore-forming, remain viable in soil and animal products for decades • Gram-positive • Aerobic respiration • Exotoxin producing • Grows best at 24 -40⁰C • Incubation period: 1 to 15 days • Three forms: inhaltion, gastrointestinal, cutaneous

Virulence Factors • Encoded on two plasmids ▫ One encodes for the synthesis of a polyglutamyl capsule (inhibits phagocytosis by macrophages) ▫ Other bears genes encoding for the synthesis of exotoxins • Exotoxins: three proteins ▫ Protective antigen ▫ Edema Factor: adenylate cyclase activity, increases c. AMP, leads to cytoplasm loss after forming an edema ▫ Lethal Factor: interferes with transcription factor in genome (Nfk. B) which regulates immunity genes. Once these are no longer transcribed, immune response of macrophages will fade.

General Mode of Infection • B. anthracis spores enter the body (lungs, skin lesion, gastrointestinal) and germinate, giving rise to the vegetative form • The bacterium begins to produce capsules containing exotoxins, which will help evade the host’s immune system • The PA portion will bind to receptors on the membrane of macrophages, when seven complexes are combined they form a ring. This ring will pierce through the membrane and the macrophage will shuttle in the complex as an endosome

General Mode of Infection cont. • The PA molecules will form a pore that pierces the endosome membrane, releasing the EF and LF into the cytoplasm of the macrophage • EF and LF essentially kill the macrophage, and release the contents of the macrophage to the outside. • The endosome enzymes that were released will degrade surrounding tissues, resulting in the common symptoms of anthrax.

Cutaneous Anthrax • B. anthracis comes into contact with a skin lesion, or cut. • The spores germinate, producing bacteria, which produce exotoxins to evade the macrophages • Infection is manifested in a painless ulcer with a necrotic (dead) center • Transmission: coming in contact with infected animals or their products through a skin lesion

Symptoms of cutaneous anthrax • Boil-like skin lesion forming a painless ulcer • Swelling of the lymph glands • Fever • Headache

Inhalation Anthrax • The spores are inhaled and lodge in the alveolar spaces • Alveolar macrophages engulf the spores. • Spores germinate within macrophages after failed phagocytosis • Bacteria proceed to lymph nodes and spread into bloodstream, where they begin to release the exotoxins • Transmission: inhaling the spores of B. anthracis
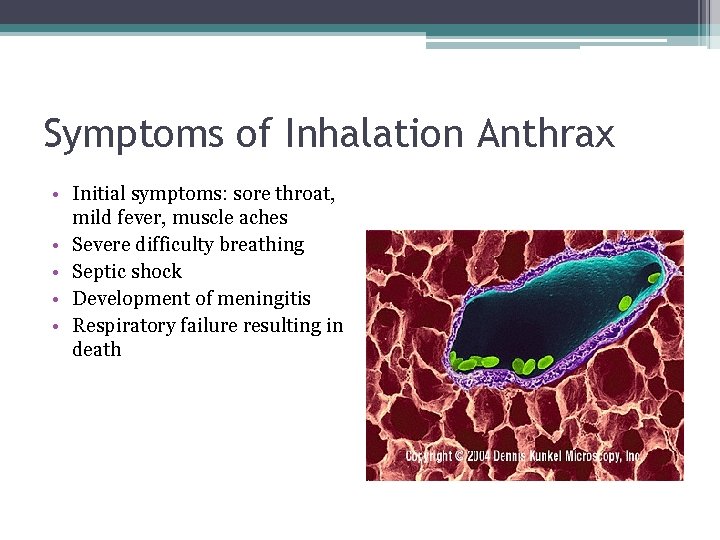
Symptoms of Inhalation Anthrax • Initial symptoms: sore throat, mild fever, muscle aches • Severe difficulty breathing • Septic shock • Development of meningitis • Respiratory failure resulting in death

Gastrointestinal Anthrax • Spores are consumed after eating undercooked meat • Spores can evade stomach acid due to their capsule • Once in the digestive tract, they begin to germinate and produce bacteria, which release exotoxins • After the macrophages have been lysed, the endosome enzymes begin degrading intestinal walls, allowing the bacteria to spread directly into the bloodstream • Transmission: Digesting undercooked meat containing spores

Symptoms of Gastrointestinal anthrax • • Serious gastrointestinal difficulty Nausea Fever Abdominal pain Vomiting of blood Severe bloody diarrhea Acute inflammation of intestinal tract Loss of appetite

Diagnosis • A diagnosis can be made by taking a smear of a skin lesion (if cutaneous anthrax) and gramstaining the sample. • Blood tests that show encapsulated, broad, gram -positive bacilli • Cultures: large, flat, nonhemolytic colonies, nonmotile, will test positive for catalse, positive for capsule production • Confirmatory Diagnosis: Serological tests for toxins at reference laboratories

Transmission • Bacillus anthracis is transmitted mainly through the contact of infected animals or their products, and humans, resulting in cutaneous anthrax • It cannot be spread from human to human. • 2001: Anthrax was sent in the form of a powder in letters, when the recipient of the letter opened them and inhaled the spores, they became infected. 5 out of 22 died. ▫ Biological Warfare Debate

Prevalence • In the past, anthrax was found all over the world. • Now, this bacterium is found mainly in underdeveloped countries lacking the means of disease control; such as the Middle East, Africa, Australia, southern and eastern Europe, South and Central America, Asia • It is not common in the United States, although small outbreaks periodically occur in agricultural areas on animals. • The last outbreak resulted in the death of 5 out of 22 people in 2001. ▫ 1987: 20 out of 22 had died • 2, 000 – 20, 000 human outbreaks annually

Susceptibility • All warm-blooded animals are susceptible to anthrax, especially herbivores ▫ Other domesticated animals such as horses and mules may also contract the disease.

Treatment • Cutaneous / gastrointestinal ▫ Antibiotic therapy for 7 – 14 days • Inhalation ▫ Antibiotic therapy for 30 days if used alone ▫ If vaccine is available, antibiotics can be discontinued after 3 doses of vaccine

Vaccine • Anthrax Vaccine Adsorbed (AVA) ▫ 6 -dose series at 0, 2, 4 weeks and 6, 12, 18 months ▫ Annual booster injections to maintain immunity • Who receives vaccine? ▫ Animals, mainly cattle ▫ People with high occupational risk �Military, people close to an outbreak

Prevention • Decontamination ▫ ▫ Wash down with anti-microbe effective soap Boil articles that came in contact with infected hosts Chlorine Burning articles • Early detection ▫ USPS installed Bio. Detection System • Antibiotics ▫ Penicillin ▫ Doxycycline

Current Research • New research has found that extracellular metalloproteases may play a role in the survival of the bacterium ▫ Aid in degradation of the LL-37 peptide. ▫ Other bacillus species showed no resistance to this peptide

Current Research cont. • Anti-protective antigen antibody has been shown to suppress the vegetative form of B. anthracis before it sporulates.

Current Research cont. • Research has also shown a new technique in identifying anthrax spores before a new outbreak occurs. ▫ Microwave-Accelerated Metal-Enhanced Fluorescence (MAMEF) (Metal-enhanced flulow power microwave heating) is used to accelerate DNA hybridization ▫ The DNA of the B. anthracis spores was detected almost immediately.

References • http: //www. ncbi. nlm. nih. gov/sites/entrez? Db=pubmed&Cmd=Show. Detail. View&Ter m. To. Search=17955147&ordinalpos=2&itool=Entrez. System 2. PEntrez. Pubmed. Pubme d_Results. Panel. Pubmed_RVDoc. Sum • Microbiology Lecture Textbook • http: //www. cdc. gov/ • http: //www. nlm. nih. gov/medlineplus/anthrax. html • http: //pathport. vbi. vt. edu/pathinfo/pathogens/Bacillus-anthracis. html • http: //www. ncbi. nlm. nih. gov/Taxonomy/Browser/wwwtax. cgi? id=191218&lvl=1 • http: //www. ncbi. nlm. nih. gov/sites/entrez • http: //www. bt. cdc. gov/agent/anthrax/lab-testing/#references
- Slides: 23