Bacillary Dysentery shigellosis Definition Acute infectious disease of

Bacillary Dysentery (shigellosis)

Definition Acute infectious disease of intestine caused by dysentery bacilli(genus shigella) Place of lesion: sigmoid & rectum Pathological feature: diffuse fibrious exudative inflammation

Definition Clinical manifestation: fever, abdominal pain, diarrhea, tenesmus , stool mixed with mucus blood, & pus. shock, toxic-encepholopthy.

Etiology Causative organism: dysentery bacilli, genus shigella, gram-stained negative, non-motile short rod, Groups: 4 serogroups &47 serotypes

Etiology S. dysenteriae: the most severe S. flexneri: the epidemic group and easily turn to chronic S. boydii: tropical and subon S. sonnei: the most mild

Etiology Pathogenicity: - virulence endotoxin - exotoxin - invasiveness (attach-penetrate-multiply) Resistance: Strong, 1 -2 week in fruits, vegetable and dirty soil, heat for 60℃ 30 min

Epidemiology Source of infection: patients and carriers Route of transmission: fecal-oral route Suceptibility of population: immunity after infection is short and unsteady, no cross-immune

Epidemiology Epidemic features: season: summer & fall Flexneri, Soneii, dysentery age: younger children

Pathogenesis number of bacteria toxicity invasiveness attachment penetration multiplication immunity
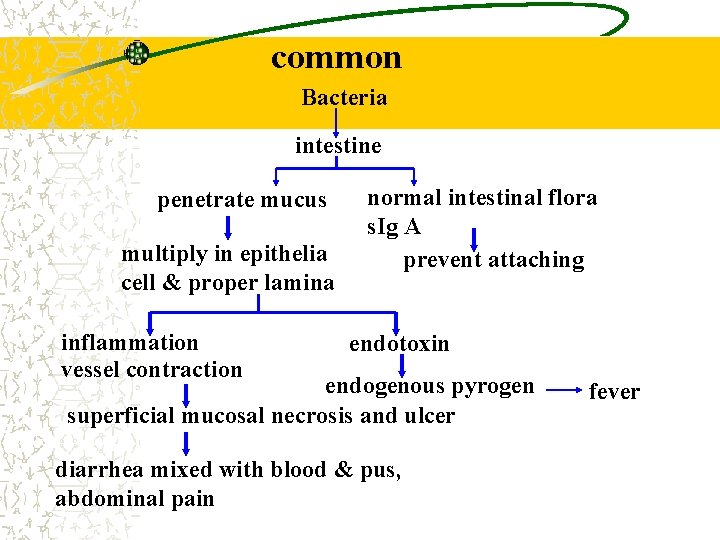
common Bacteria intestine penetrate mucus multiply in epithelia cell & proper lamina inflammation vessel contraction normal intestinal flora s. Ig A prevent attaching endotoxin endogenous pyrogen superficial mucosal necrosis and ulcer diarrhea mixed with blood & pus, abdominal pain fever

Pathogenesis-toxic strong - allergy to endotoxin demethyl-adrenaline micro-circulatory failure shock, cerebral edema cerebral hernia DIC

Pathology site of lesion: entire large bowelsigmoid colon & rectum feature: acute: diffuse fibrinous exudative inflammation,

Pathology hyperemia, edema, leukocyte infiltration, superficial necrosis, ulcer. chronic: edema, polypoid hyperplasia, toxic: colon: hyperemia, edema, micro- capillary was invaded

Clinical manifestation Incubation period: 1 -2 day, (hours to 7 days) Acute dysentery common type mild type toxic type

Clinical manifestation Øcommon type: (typical type) acute onset , shiver, high fever abdominal pain(tenderness) diarrhea: stool mixed with mucus, blood & pus tenesmus, 1 week

Clinical manifestation Ømild type: ( atypical type) caused by S. sonnei low fever or no fever abdominal pain is mild stool mixed with mucus, without blood & pus diagnosis by isolation of bacteria 3~7 d

Clinical manifestation Øtoxic type: age: 2 to 7 yrs. abrupt onset, high fever, T 40 o. C dysphoria, lethargy, convulsion repeatedly, coma. circulatory & respiratory collapse diarrhea mild or absent at beginning

Clinical manifestation shock form: septic shock brain form: dysphoria, lethargy, convulsion repeatedly, coma, brain hernia. respiratory failure mixed form

Clinical manifestation chronic dysentery: > 2 months chronic delayed type: chronic obscure type acute attack type

Clinical manifestation Øchronic delayed type: long-time and repeated abdominal pain, diarrhea, stool mixed with mucus, blood & pus. with fatigue, anemia, malnutrition.

Clinical manifestation Øchronic obscure type: acute history in 1 year, no symptoms, stool culture positive or sigmoidscopy Øacute attack type: same as common acute dysentery

Laboratory Findings Blood picture: WBC count increase, (10~20× 109/L) neutrophils increase Stool examination: gross examination: stool mixed with mucus, blood & pus.

Laboratory Findings direct microscopic examination: WBC, RBC, pus cells bacteria culture: PCR: DNA Sigmoidoscopy: chronic patients shallow ulcer scar polyp
- Slides: 23