B 260 FUNDAMENTALS OF NURSING Medication Administration Medication

B 260 FUNDAMENTALS OF NURSING Medication Administration

Medication: Pharmacokinetics • Route: how enter the body • Absorption: from site into blood • Distribution: from blood into cells, tissues, or organs • Action: alter physiological functions • Metabolism: changed to prepare for excretion • Excretion: how they exit the body • Action: how medications act This knowledge is used when selecting timing, route, risks, and evaluating the response

3 In your group… answer the following questions regarding the assigned medication administration route… 1. Nursing actions & safety implications regarding assigned medication administration route 2. Advantages & Disadvantages of route 3. Teach a patient or family member how to administer a medication by the assigned medication administration route.
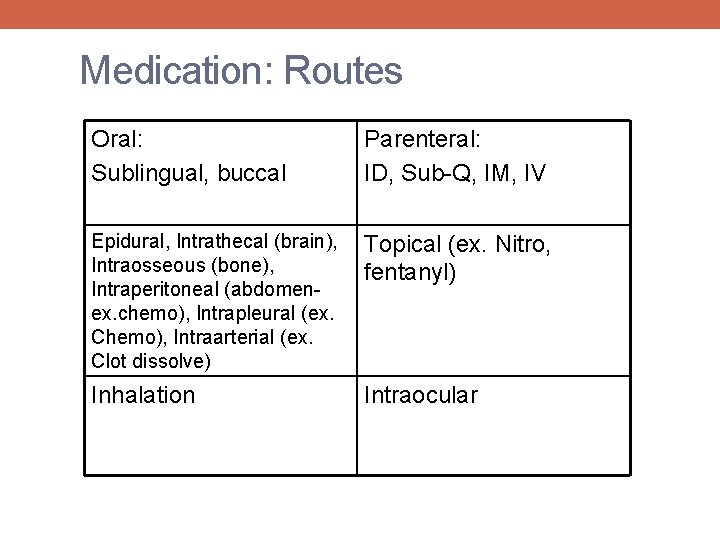
Medication: Routes Oral: Sublingual, buccal Parenteral: ID, Sub-Q, IM, IV Epidural, Intrathecal (brain), Intraosseous (bone), Intraperitoneal (abdomenex. chemo), Intrapleural (ex. Chemo), Intraarterial (ex. Clot dissolve) Topical (ex. Nitro, fentanyl) Inhalation Intraocular

Medication: Factors Influencing Routes • Oral: convenience vs. tolerance, easy to give, often produces local or systemic effects • Injections: infection risk, needle, bleeding, rapid absorption • Skin/topicals: painless, caution w/abrasions, provides local effects • Transdermal: prolonged systemic effects • Mucous membranes: sensitive, less pleasant, • Inhalation: provides rapid effect for local respiratory effect, potential serious side effects

Medication: Forms • Caplet – coated for easier swallowing • Capsule – powder, liquid or oil in gelatin shell • Tablet – compressed powder • Enteric coated – dissolves in small intestine • Time release – granules with different coatings, or some tablets that dissolve slowly • Lozenge – dissolves in mouth • Elixir – mixed with water or alcohol and a sweetener • Syrup – sugar solution

Medication: Forms • Suspension – drug particles in a liquid medium • Solution – mixed in water – can be sterile for dressing changes (Normal saline), or for IM, SQ, or IV routes • Lotion – liquid suspension for skin • Ointment – semisolid (salve another name) • Paste – semisolid, but thicker than ointment – slower absorption • Transdermal disk or patch – semi-permeable membrane disk or patch with drug applied to skin • Suppository – solid drug mixed with gelatin inserted into body cavity to melt (rectum or vagina)
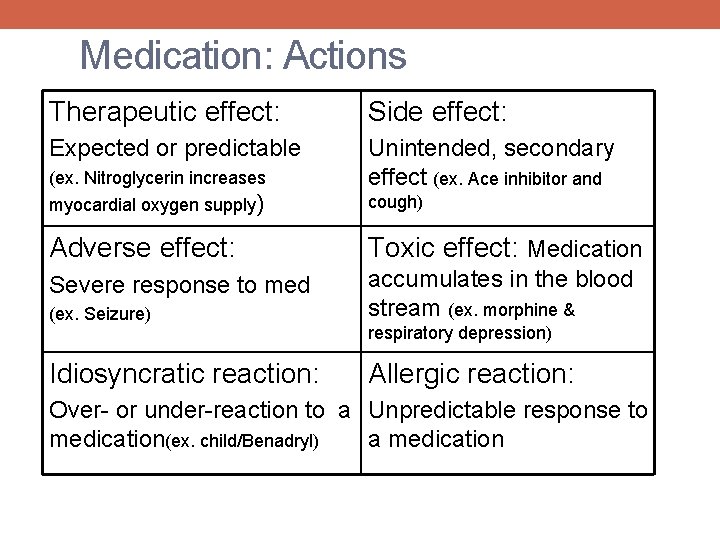
Medication: Actions Therapeutic effect: Side effect: Expected or predictable Unintended, secondary effect (ex. Ace inhibitor and (ex. Nitroglycerin increases myocardial oxygen supply) cough) Adverse effect: Toxic effect: Medication Severe response to med (ex. Seizure) accumulates in the blood stream (ex. morphine & Idiosyncratic reaction: Allergic reaction: respiratory depression) Over- or under-reaction to a Unpredictable response to medication(ex. child/Benadryl) a medication

Medication: Interactions • Occur when one medication modifies the action of another • A synergistic effect occurs when the combined effect of two medications is greater than the effect of the medications given separately
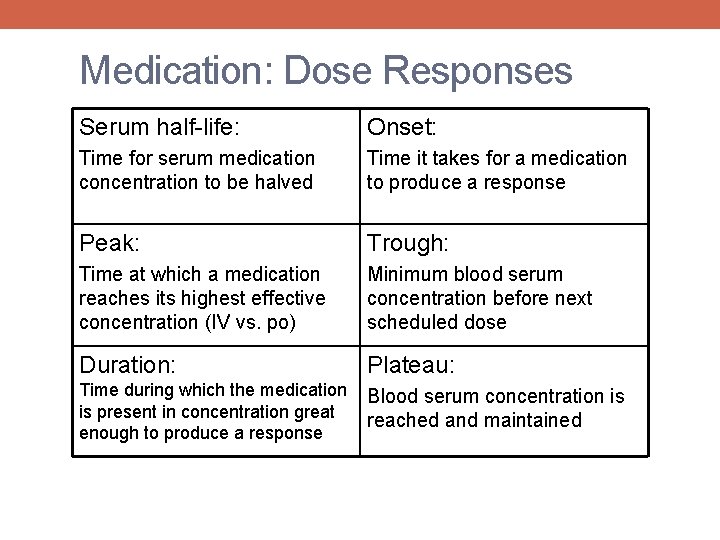
Medication: Dose Responses Serum half-life: Onset: Time for serum medication concentration to be halved Time it takes for a medication to produce a response Peak: Trough: Time at which a medication reaches its highest effective concentration (IV vs. po) Minimum blood serum concentration before next scheduled dose Duration: Plateau: Time during which the medication is present in concentration great enough to produce a response Blood serum concentration is reached and maintained

Administering via Inhalation • Aerosol spray, mist, or powder via handheld inhalers; used for respiratory “rescue” and “maintenance” • Pressurized metered-dose inhalers (p. MDIs) • Need sufficient hand strength for use • Breath-actuated metered-dose inhalers (BAIs) • Release depends on strength of patient’s breath. • Dry powder inhalers (DPIs) • Activated by patient’s breath • Produce local effects such as bronchodilation • Some medications create serious systemic side effects.

Administering via Inhalation • Inhalers: spacer used when pt. unable to do correctly
13 Administering via Inhalation

Prescriber’s Role • Prescriber can be physician, nurse practitioner, or physician’s assistant. • Orders can be written (hand or electronic), verbal, or given by telephone. • The RN Role in Computerized provider order entry (CPOE) • The use of abbreviations can cause errors; use caution. • Each medication order needs to include the patient’s name, order date, medication name, dosage, route, time of administration, drug indication, and prescriber’s signature.
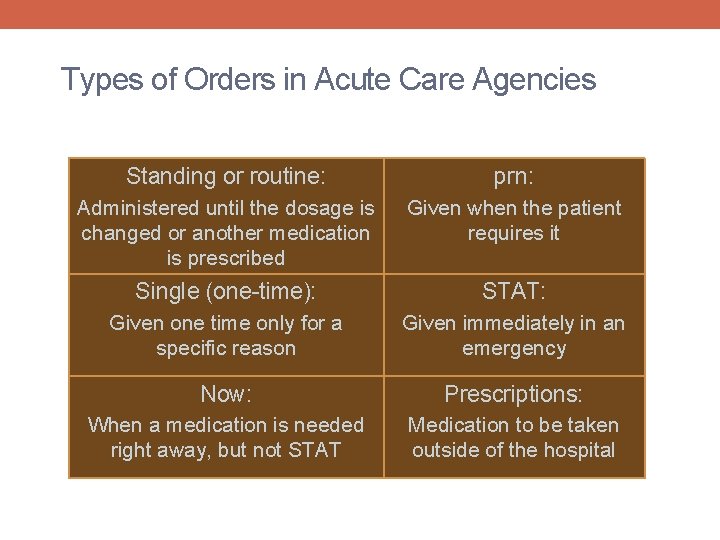
Types of Orders in Acute Care Agencies Standing or routine: prn: Administered until the dosage is changed or another medication is prescribed Given when the patient requires it Single (one-time): STAT: Given one time only for a specific reason Given immediately in an emergency Now: Prescriptions: When a medication is needed right away, but not STAT Medication to be taken outside of the hospital

Medication Administration • Pharmacist’s role • Prepares and distributes medication • Distribution systems (unit dose or automatic medication dispensing system [AMDS]) • Area for stocking and dispensing medication • Nurse’s role • Assess patient’s ability to self-administer, determine whether patient should receive, administer medication correctly, and closely monitor effects; do not delegate this task. • Medication error

Automated Medication Dispensing System • Automated: control the dispensing of medications, may be networked with computerized medical record, may include controlled substances

Medication Errors • Report all medication errors. • Patient safety is top priority when an error occurs. • Documentation is required. • The nurse is responsible for preparing a written occurrence or incident report: an accurate, factual description of what occurred and what was done. • Nurses play an essential role in medication reconciliation.

Medications: Seven Rights • Right patient: 2 identifiers (compare name/ID with MAR) • Right drug: need order, match MAR • Right dose • Right route • Right time: institutional • Right documentation: after it is given • Right to refuse

Medication: Nurse Role 1. 2. 3. 4. 5. 6. 7. 8. 9. 10. Follow 7 rights Read labels 3 x and compare to MAR Use at least 2 patient identifiers Avoid interruption Double check calculations, verify with another RN, follow policy Question unusual doses Record after medication given Report errors, near-misses Participate in programs designed to reduce error Patient education about medications
Right Patient

Maintaining Patients’ Rights • To be informed about a medication • To refuse a medication • To have a medication history • To be properly advised about experimental nature of medication • To receive labeled medications safely • To receive appropriate supportive therapy • To not receive unnecessary medications • To be informed if medications are part of a research study

Medication: Orders Patients full name • Date and time order written • Drug name • Dosage • Route • Time and frequency • Signature of provider
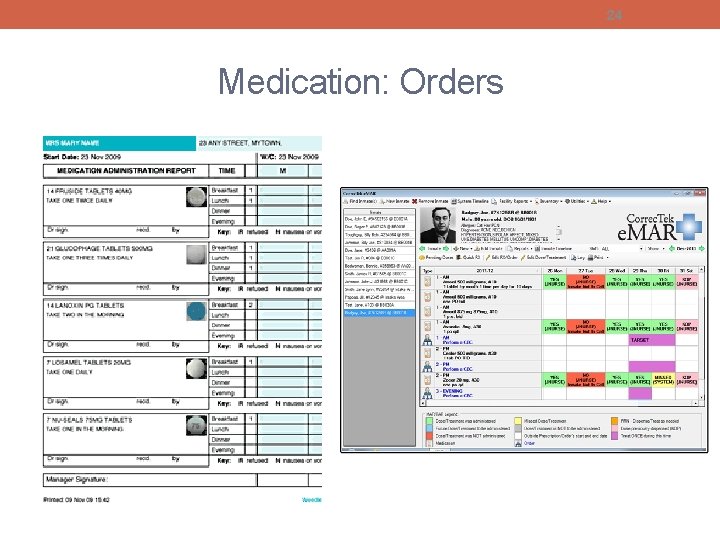
24 Medication: Orders

Essential Components of Medication Administration: • • Check chart for new orders first! Medical history Drug Allergies/Interactions Tolerance/Appropriateness of route Ordered diet Clients knowledge, educate if necessary And…. All 7 Rights prior to administration

Nursing Diagnoses related to medication administration… • Knowledge deficit regarding drug therapy related to unfamiliarity with information resources • Noncompliance regarding drug therapy related to limited economic resources (or health beliefs) • In effective management of therapeutic regimen related to complexity of drug therapy (or knowledge deficit). • Impaired swallowing related to neuromuscular impairment
- Slides: 26