Avoidable utilization of hospital care among elderly patients

Avoidable utilization of hospital care among elderly patients with significant health care needs Limitations in the use of process and outcome measures to incentivize quality improvements in primary care. Anders Anell & Anna H Glenngård
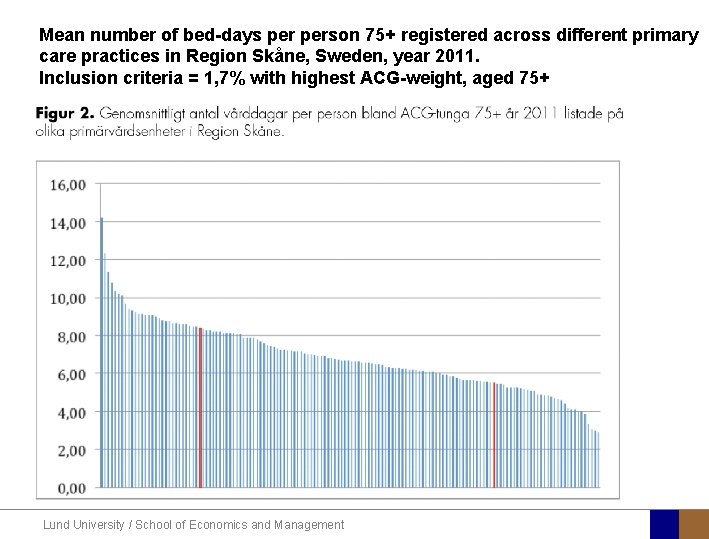
Mean number of bed-days person 75+ registered across different primary care practices in Region Skåne, Sweden, year 2011. Inclusion criteria = 1, 7% with highest ACG-weight, aged 75+ Lund University / School of Economics and Management

Possible indicators for pay-for-performance (P 4 P) • Outcome indicators – Visits to hospital emergency units without admission per 1000 registered – Utilization of in-patient care, re-admissions within 30 days • Process indicators – Continuity – Drug reviews – Individual patient plans (in collab. with community staff) Outcome is explained by: - evidence of interventions process - quality of implementation - riskfactors och patient attributes - randomnes Lund University / School of Economics and Management Type I (false positive) and type II (false negative) error when assessing practices

Data and Metod • Qualitative study – step 1 – Blinded interviews with eight practices and community staff – Assessment of case finding, continuity, access, coordination and collaboration between primary and community care – Summarizing index compared with hospital utilization and socioeconomic status of registered individuals • Quantitative study – step 2 – Data from 150 practices in regression analysis – Dependent variables: Mean beddays person 75+; Visits at emergency care units without admission per 1000 registered 75+ – Independent variables: location, CNI (socioeconomic status), private or public, continuity, drug reviews, individual patient plans, direct admissions Lund University / School of Economics and Management

Assessment of case finding, continuity, access, coordination and collaboration between primary and community care Name of providers (anonymous ) Casefinding Continuity towards patient Accessibilit y towards patient Collaboration between primary and community care Coordination of care based on individual needs Author assessmen t (interview data) Continuity in three consecutive visits (registered data) Author assessmen t (interview data) Author assessment of formal structure (interview data) Author assessment of accessibility and continuity (interview data) Self-rated by primary care Self-rated by community care Number of individual patient plans (registered data) Number of drug reviews (registered data) Tärnan *** *** *** * - ** 22 Doppingen ** ** ** * * - - 15 Måsen ** *** *** ** * - - 19 Svalan ** ** * - ** 14 Lommen ** ** * * *** 17 Vadaren * ** ** ** * - *** 18 Svanen *** *** *** *** 27 Falken ** ** *** ** ** - * 18 Lund University / School of Economics and Management Sum
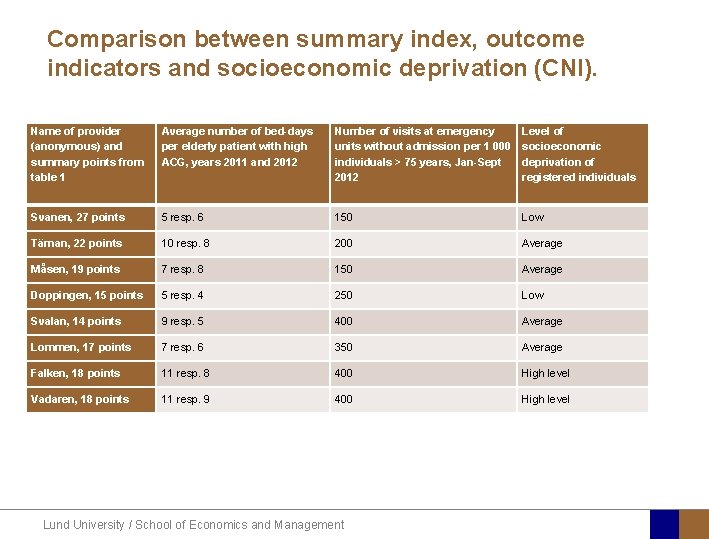
Comparison between summary index, outcome indicators and socioeconomic deprivation (CNI). Name of provider (anonymous) and summary points from table 1 Average number of bed-days per elderly patient with high ACG, years 2011 and 2012 Number of visits at emergency units without admission per 1 000 individuals > 75 years, Jan-Sept 2012 Level of socioeconomic deprivation of registered individuals Svanen, 27 points 5 resp. 6 150 Low Tärnan, 22 points 10 resp. 8 200 Average Måsen, 19 points 7 resp. 8 150 Average Doppingen, 15 points 5 resp. 4 250 Low Svalan, 14 points 9 resp. 5 400 Average Lommen, 17 points 7 resp. 6 350 Average Falken, 18 points 11 resp. 8 400 High level Vadaren, 18 points 11 resp. 9 400 High level Lund University / School of Economics and Management

Reflections • Insufficient routines to handle elderly in ordinary housing • Lack of coordination based on individual needs • Gap between formal responsibility and practical work • Insufficient information flow between different care givers • Continuity compensate for poor coordination and cooperation Lund University / School of Economics and Management

Results from regression analysis • Two models – mean number of bed-days and visits at emergency units without admission per 1000 • Significant correlation with location of practices in both models – Increased CNI results in increased mean number of bed-days and number of visits – Lower number of visits in two out of five districts • Higher percent of direct admissions reduces mean number of bed-days • The model with bed-days as dependent variable explains less of variance Lund University / School of Economics and Management
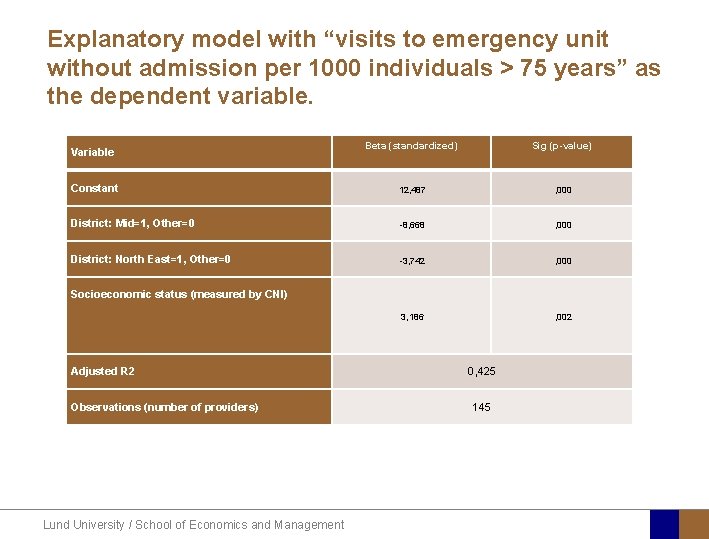
Explanatory model with “visits to emergency unit without admission per 1000 individuals > 75 years” as the dependent variable. Beta (standardized) Sig (p-value) Constant 12, 487 , 000 District: Mid=1, Other=0 -8, 668 , 000 District: North East=1, Other=0 -3, 742 , 000 3, 186 , 002 Variable Socioeconomic status (measured by CNI) Adjusted R 2 Observations (number of providers) Lund University / School of Economics and Management 0, 425 145
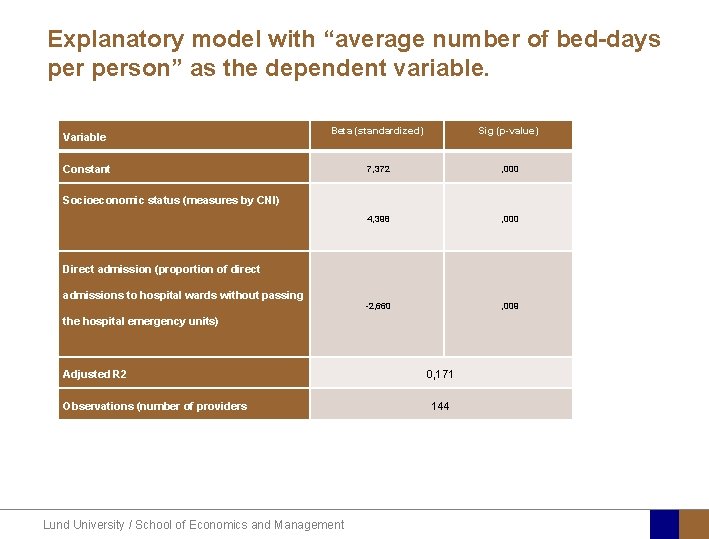
Explanatory model with “average number of bed-days person” as the dependent variable. Variable Beta (standardized) Sig (p-value) 7, 372 , 000 4, 398 , 000 -2, 660 , 009 Constant Socioeconomic status (measures by CNI) Direct admission (proportion of direct admissions to hospital wards without passing the hospital emergency units) Adjusted R 2 Observations (number of providers Lund University / School of Economics and Management 0, 171 144

Limitations of indicators • Wrong practices may be rewarded when using outcome meausers – Need to adjust for patient attributes (e. g. CNI) – Limitations when number of patients are limited (randomness) – Several factors may influence outcomes (attribution problem) • But process indicators have important limitations as well – Evidence base? – Often easy to manipulate – ”Box ticking”, ”treat-to-test”, ”reaching target but missing the point” – Need to secure quality in implementation Lund University / School of Economics and Management
- Slides: 11