Av Med Health Plans Fraud Waste and Abuse

Av. Med Health Plans Fraud, Waste and Abuse Training 2009

Objectives • • • Define fraud, waste, and abuse Recognize the financial impact of fraud Identify where fraud can be committed Share examples of suspect fraud Understand preventive efforts Review Av. Med’s Anti-Fraud Plan 2

What is Fraud • Fraud – The intentional deception or misrepresentation that an individual or entity knows to be false or does not believe to be true and makes, knowing the deception could result in some unauthorized benefit to himself/herself or some other person. 3

What is Waste • Health care spending that can be eliminated without reducing the quality of care such as quality waste (overuse, underuse, and ineffective use) and inefficiency waste (redundancy, delays, and unnecessary process complexity) 4

What is Abuse • Abuse – Practices by facilities, physicians, and suppliers, while not usually considered fraudulent, are nevertheless inconsistent with accepted medical, business, and fiscal practices. 5
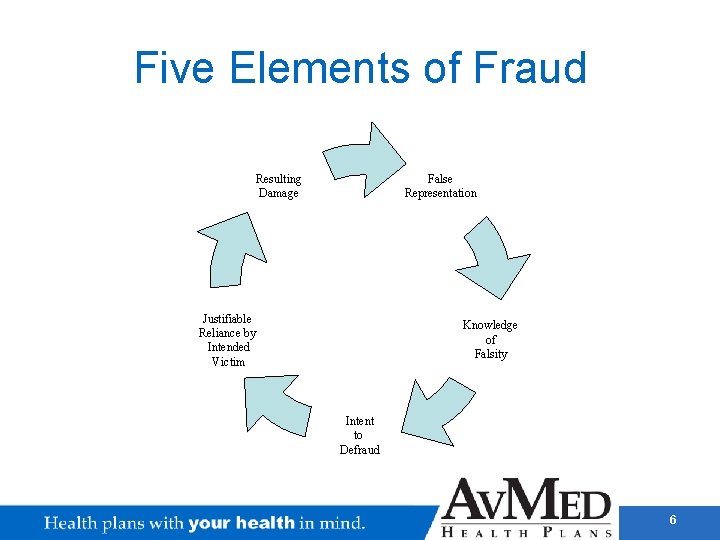
Five Elements of Fraud False Representation Resulting Damage Justifiable Reliance by Intended Victim Knowledge of Falsity Intent to Defraud 6

Audit vs. Investigation • • • Regular, recurring General Opinion Non-adversarial Financial data Professional skepticism • • • Non-recurring Specific allegation Determination Affix blame Interviews Proof to support allegation 7

Impact of Fraud • The United States spent in excess of $2. 2 trillion on health care in 2007 • Fraud is estimated to be between 3% 10% of health care dollars • If 5% is the average lost to health care fraud, that would equal to losing approximately $100 billion in 2007 or about $300 million per day 8

Vulnerabilities • Where can fraud and abuse occur? – Hospitals, Physicians, Members, Nursing Homes, Home Health Care, Ambulance Services, Office Staff, Chiropractors, Clinics, Brokers and Agents, Durable Medical Equipment, Laboratories, Accident Claims, Pharmacies, Employees, Drug Manufacturers, Pharmacy Benefit Managers, Group Enrollments, Wholesalers, Workers Compensation, to name a few… 9

Examples of Pharmacy Fraud • • Billing for higher supply than dispensed Employee fraud with dispensing Enhance revenue of brand vs. generic Kickbacks using manufacturers products Controlled drugs without physician service Outlier of reversal rates Prescription splitting 10

Examples of Pharmacy Fraud • • Altering prescriptions Drug diversion Pharmacist billing for “gang visits” Excessive quantity dispensed Prescription price with inflating AWP Prescription drug shorting True Out-of-Pocket (Tr. OOP) manipulation 11

Examples of Pharmacy Fraud • • Double billing No prescription on file Unauthorized refills Incorrect days of supply billed Unit billing issues Dispensing without validation of customer Dispensing expired prescription drugs 12

Examples of Facility Fraud • • Unbundled supplies and equipment Non-covered services hidden Inflating costs Charge master inconsistencies Up coding Unlicensed ambulatory surgical centers Skilled nursing failure of care 13

Examples of Facility Fraud • Failure to report credit balances • Seeking reimbursement for costs not related to patient care • Failing to disclose relationship between business entities • Diagnostic unnecessary testing 14

Examples of Member Fraud • • Stolen card falsification Misrepresentation on enrollment forms Stolen prescription pads Altering prescriptions Physician or pharmacy shopping Excessive visits for controlled substances Beneficiary ID card sharing 15

Examples of Physician Fraud • • • Coding (up, down, modifiers, rule playing) Place of service falsification Non-rendered or phantom billing Medically unnecessary or unbelievable Kickbacks or bribery Billing free services 16

Examples of Physician Fraud • • • Duplicate billing Waiver of co-pay or deductible Misrepresentation on claim Selling filled scripts on black market Prescribing to self or family Over prescribing to patients 17

Examples of Physician Fraud • Excessive scripts of controlled substances • Excessive quantities of controlled substances • Overutilization • Unlicensed office-based surgeries • Resubmission of denied claim with different code(s) • Medical treatment unrelated 18

Prevention • Combating Fraud is a Collaborative Effort – – – • • Av. Med Health Plans Anti-Fraud Program Department of Justice Federal Bureau of Investigation Office of Inspector General Centers for Medicare & Medicaid Services Education Administrative Sanctions Civil Litigation and Settlements Criminal Prosecution 19

Prevention • Develop a Compliance Program to include Fraud, Waste, and Abuse • System for monitoring claims for accuracy • Review medical records to validate documentation supports services rendered • Perform regular internal audits • Take action when an issue is identified 20

Av. Med’s Anti-Fraud Plan • Fiduciary Responsibility • Mission Statement • Compliance – – – Section 626. 9891(a)(b), Florida Statutes Section 626. 9891(3), Florida Statutes Rule Chapter 69 D-2. 001 -005, Administrative Code 42 C. F. R. 422. 503, Medicare Advantage Program 42 C. F. R. 423. 504(b)(4)(vi)(H), CMS Part D Federal Employees Health Benefit Program 21

Fiduciary Responsibility • The Board of Directors has a fiduciary responsibility to Av. Med specifically and to the broader health care community to resist criminal behavior, instances of false claims and improper billing and coding practices, and other schemes that adversely impact patient safety, the quality of health care services being delivered and that impose a tremendous financial burden on the health care system. 22

Mission Statement • Fraud and Abuse Program Mission Statement seeks to meet the customer’s expectation that we will reimburse only for services that are medically necessary and appropriate and that the benefits will be issued only to eligible subscribers and providers. 23
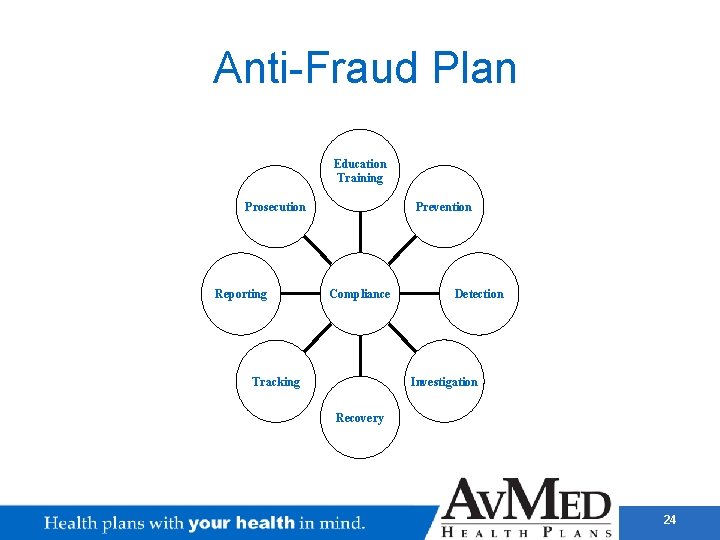
Anti-Fraud Plan Education Training Prevention Prosecution Reporting Compliance Detection Investigation Tracking Recovery 24

Resources • Tips • Websites – Internal – External – U. S. Government – Regional CMS Carrier – Professional Physician • Coding Texts – ICD-9 -CM, CPT, HCPCS • Data Mining and Profiling • National Health Care Anti. Fraud Association • American Medical Association • American Health Information Management Association • • Medicare Drug Contractors Law Enforcement Federal Bureau Investigation Office Inspector General Vendors Media Anonymous (Hotline) 25

Healthcare Fraud and You • Healthcare fraud is a menace to you, your family, and the future of your health care • It causes higher premiums or fewer benefits, higher taxes, and higher copayments • Your detection and referrals are critical to the success of all anti-fraud efforts 26

Training Attestation Now that you have completed Fraud, Waste, Abuse, and Compliance Training in accordance with CMS regulations, please click here to attest completion of the program. 27
- Slides: 27