AUTONOMIC NERVOUS SYSTEM Autonomic Nervous System Somatic Autonomic







































































- Slides: 79

AUTONOMIC NERVOUS SYSTEM • Autonomic Nervous System • Somatic & Autonomic Nervous System • Parasympathatic & Sympathatic nervous system • Neurohumoral Transmission • • Receptors -Cholinoceptors -Adrenergic receptors • Drugs affecting parasympathetic NS • Drugs affecting sympathetic NS

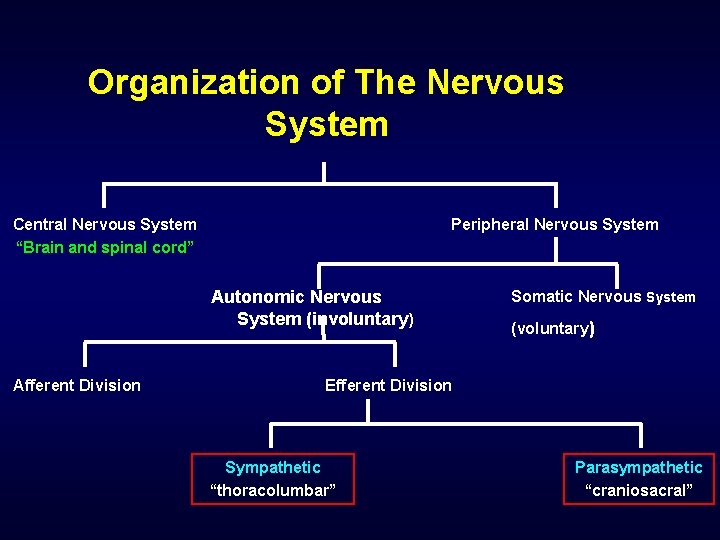
Organization of The Nervous System Central Nervous System “Brain and spinal cord” Peripheral Nervous System Autonomic Nervous System (involuntary) Afferent Division Somatic Nervous System (voluntary) Efferent Division Sympathetic “thoracolumbar” Parasympathetic “craniosacral”

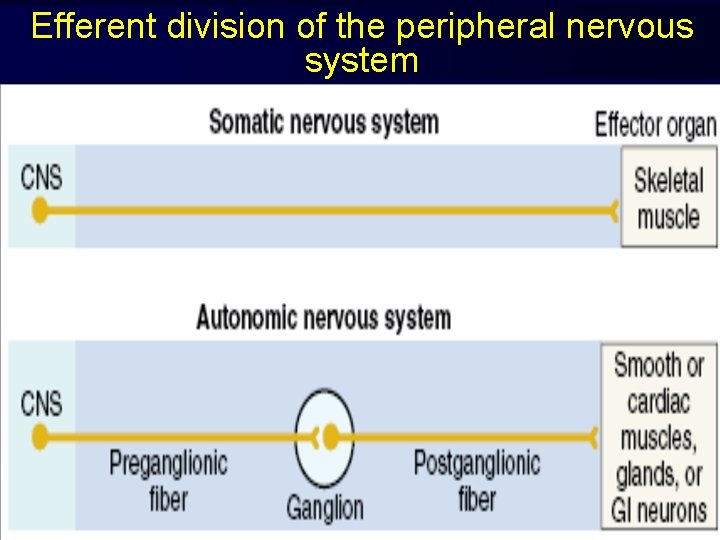
Efferent division of the peripheral nervous system

v. In the nervous system, chemical transmission occurs between nerve cells and their effector cells v. Chemical transmission takes place through the release of small amounts of transmitter substances from the nerve terminals into the synaptic cleft v. The transmitter crosses the cleft by diffusion and activates or inhibits the postsynaptic cell by binding to a specialized receptor molecule

Neurohumoral Transmission • It should be present in the presynaptic neurone (usually along with enzyme synthesizing it) • It should be released in the medium following nerve stimulation • Its application should produce responses identical to those produced by nerve stimulation • Its effects should be antagonized or potentiated by other substance which similarly alter effects of nerve stimulation

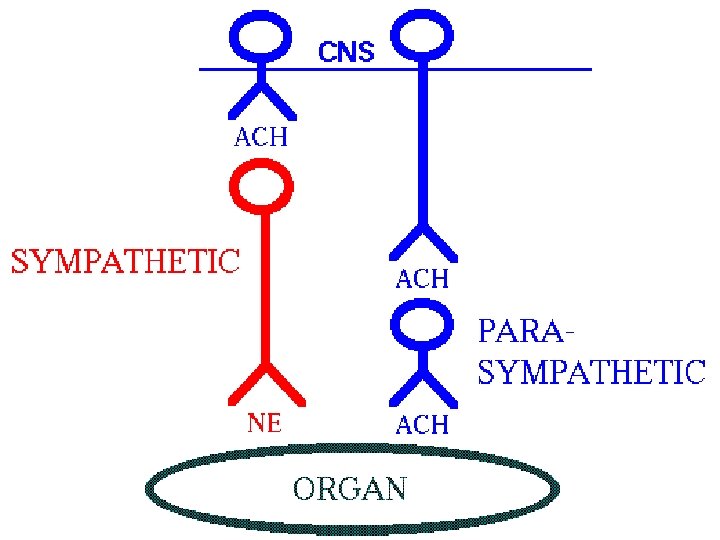
• Almost all autonomic nerves (Syp+Parasaymp) have relay centre in between called as ganglion Which lies outside the CNS Preganglionic Neuron Postganlionic neuron

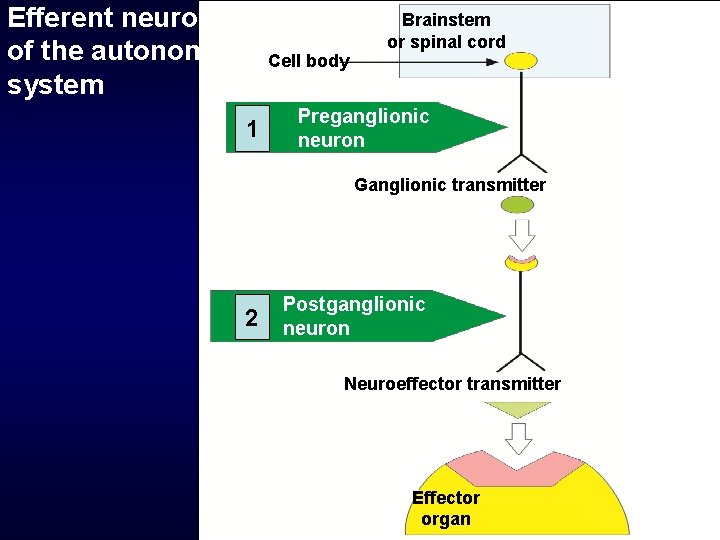
Efferent neurons of the autonomic system Cell body 1 Brainstem or spinal cord Preganglionic neuron Ganglionic transmitter 2 Postganglionic neuron Neuroeffector transmitter Effector organ

The Synapse í A functional connection between surfaces í Signal transmission zone í Synapse – synaptic cleft, presynaptic cell, and postsynaptic cell í Synaptic cleft – space in between the presynaptic and postsynaptic cell í Postsynaptic cell – neurons, muscles, and endocrine glands í Neuromuscular junction – synapse between a motor neuron and a muscle

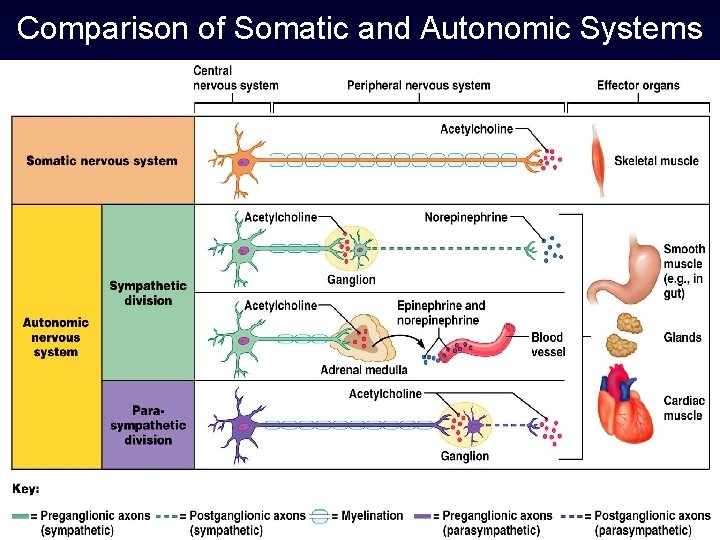
Comparison of Somatic and Autonomic Systems


Steps in neurohumoral transmission • Impulse conduction • Transmitter release • Transmitter action on postjunctional membrane -EPSP -IPSP • Post-junctional activity • Termination of transmitter action

• Presynaptically releases neurotrnsmitter is regulated by By homotropic receptor ineraction By heterotropic receptor ineraction

Sympathetic Responses to Fight-or-Flight Pupils should dilate HR and contractility increase Bronchials should dilate GI tract should shut down Bladder should be shut down Blood should be shunted from GI tract and skin to muscles Metabolism should increase supply of glucose

Parasympathetic Nervous System assimilation of food, conservation of energy

Parasympathetic Neurons & Synapses Preganglionic neurons • Long • Synapse with postganglionic neurons at or near organ • Release acetylcholine (ACh) to activate nicotinic receptors on postganglionic neurons Postganglionic neurons • Short • Synapse on the target organ • Release ACh to activate muscarinic receptors on the target organ Cholinergic fibers: i. e. , act by releasing acetylcholine. • Include: – all preganglionic efferent autonomic fibers – the somatic (non-autonomic) motor fibers to skeletal muscle – most parasympathetic postganglionic and a few sympathetic postganglionic fibers

Presynaptic autoinhibitory receptors • Presynaptic release of NT • Homotropic receptors interaction • Heterotropic receptors interaction

Cholinergic System & Drugs Synthesis Store & estruction Ach

Cholinestrase: Two types • True Acetylcholinestrase: • Location: neuronal membrane, RBC, Placenta • Plasma Cholinestrase (pseudocholinestrase, Butyrylcholine-estrase): Succinylcholine, Butyrylcholine, Ingested esters

• Muscarinic receptors: parasympathetic neuroeffector junction • M 1 Sympathetic ganglia, gastric glands, cerebral cortex • M 2 Myocardium, presynaptic terminal of peripheral & central neurones • M 3 Glandular & visceral smooth muscle • M 4 • M 5 • Nicotinic receptors • NM : Skeletal muscle end plate • NN: Ganglionic cells(SP &PSP), Adrenal medulla

Cholinoceptors • Muscarinic • AGONIST: Muscarine • ANTAGONIST: Atropine • • • M 1: Autonomic ganglia Gastric glands: histamine release CNS: learning, memories, motor function Agonist : Oxotremorine Antagonist: pirenzepine , telenzepine

• M 2: SA Node Rate of impulse generation Velocity of conduction ATRIUM Contractility VENTRICLE Contractility (SLIGHT) • AV Node • • • Visceral smooth muscle : Contraction • Agonist : Methacholine • Antagonist: Methoctramine,

• • • M 3: Visceral SM: Contraction IRIS: Constriction CILIARY MUSCLE: Contraction EXOCRINE GLANDS: Secretion Vascular endothelium: EDRF (NO) Vasodilatation Agonist : Bethanechole Antagonist: Hexahydrosiladifenidiol, Darifenacin

NICOTINIC RECEPTORS • NM • AGONIST • ANTAGONIST • NN PTMA, NICOTINE TUBOCURARINE AUTONOMIC GANGLIA AGONIST ANTAGONIST DMPP, NICOTINE HEXAMETHONIUM

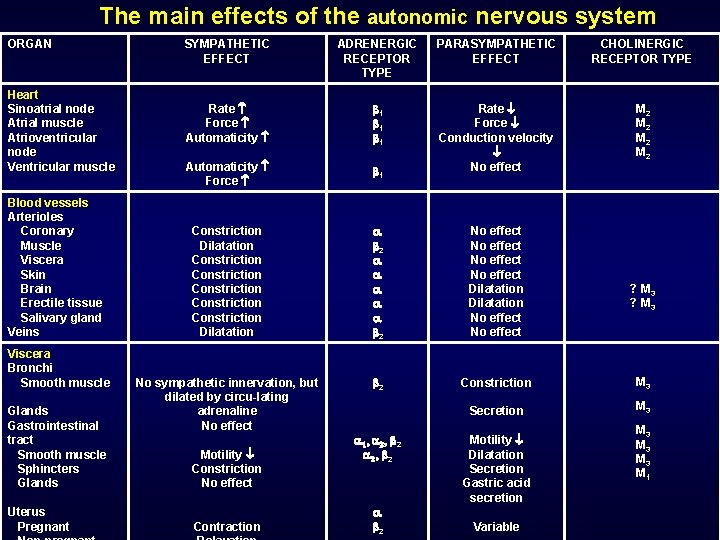
The main effects of the autonomic nervous system ORGAN Heart Sinoatrial node Atrial muscle Atrioventricular node Ventricular muscle Blood vessels Arterioles Coronary Muscle Viscera Skin Brain Erectile tissue Salivary gland Veins Viscera Bronchi Smooth muscle Glands Gastrointestinal tract Smooth muscle Sphincters Glands Uterus Pregnant SYMPATHETIC EFFECT ADRENERGIC RECEPTOR TYPE PARASYMPATHETIC EFFECT CHOLINERGIC RECEPTOR TYPE Rate Force Automaticity 1 1 1 Automaticity Force M 2 M 2 1 Rate Force Conduction velocity No effect Constriction Dilatation Constriction Constriction Dilatation 2 2 No effect Dilatation No effect No sympathetic innervation, but dilated by circu-lating adrenaline No effect 2 Constriction M 3 Secretion M 3 Motility Constriction No effect Contraction 1, 2 2, 2 2 Motility Dilatation Secretion Gastric acid secretion Variable ? M 3 M 3 M 3 M 1

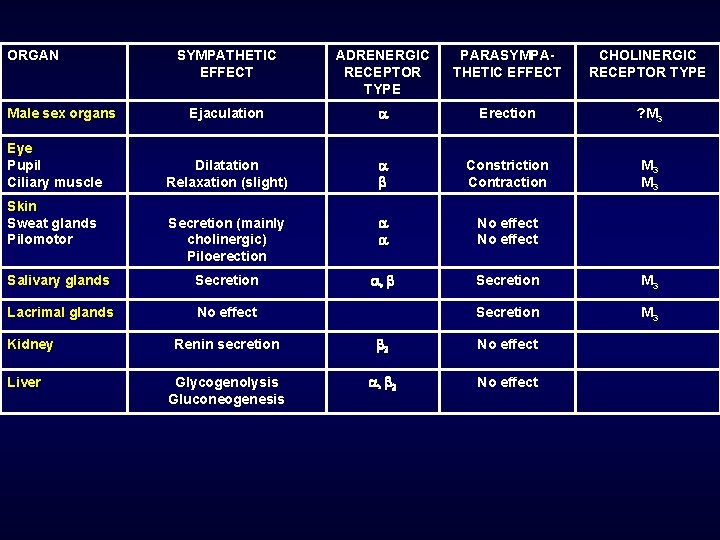
ORGAN SYMPATHETIC EFFECT ADRENERGIC RECEPTOR TYPE PARASYMPATHETIC EFFECT CHOLINERGIC RECEPTOR TYPE Ejaculation Erection ? M 3 Dilatation Relaxation (slight) Constriction Contraction M 3 Secretion (mainly cholinergic) Piloerection No effect Salivary glands Secretion , Secretion M 3 Lacrimal glands No effect Secretion M 3 Male sex organs Eye Pupil Ciliary muscle Skin Sweat glands Pilomotor Kidney Liver Renin secretion 2 No effect Glycogenolysis Gluconeogenesis , 2 No effect

• Heart M 2 Atria -ve chronotropic -ve ionotropic Decrease in conduction velocity RP (increase) Ventricular: Sweat glands: M 3 receptors Innervation sympathetic but cholinergic in nature

Classification of drugs affecting the ANS • Parasympathetic nervous system Mimic acetylcholine = cholinergic = muscarinic agonists = parasympathomimetic Block acetylcholine = anticholinergic = muscarinic antagonist = parasympatholytic • Sympathetic nervous system Mimic norepinephrine = adrenergic agonist =Adrenoceptors= sympathomimetic Block norepinephrine = antiadrenergic = adrenergic antagonist = sympatholytic

CHOLINERGIC AGONISTS CHOLINESTERS • ALKALOIDS • • • Muscarine • Pilocarpine • Arecoline Acetylcholine Methacholine Carbachol Bethanechol

ACTIONS (of ACh as prototype) • • Heart Smooth muscle Blood vessels Glands: Secretion from all parasympathetically innervated • Eye

Nicotinic: Autonomic ganglia Both sympathetic and parasympathetic ganglia are stimulated • This effects manifested at higher doses Skeletal muscles • Iontophoretic application of ACh to muscle endplate causes contraction of the fibres • High dose can cause twitching and fasciculations, buti. v. injection • CNS

Uses • • • Pilocarpine Acetylcholine Bethanechol Carbachol Methacholine

ANTICHOLINESTERASES • Reversible • Carbnmates • • Acridine • Tacrine Physostigmine(Eserine) Neostigmine Pyridostigmine Edrophonium Rivastigmine, Donepezil Galantamine lrreversible • Organophosphates • • • Dyflos (DFP) Echothiophate Parathion Carbamates • Carbaryl • Propoxur

• • Uses In glaucoma Myasthenia gravis Postoperative paralytic ileus/urinary retention Postoperative decurarization Belladona poisoning Alzheimer's disease

• ANTICHOLINERGIC DRUGS • (Muscarinic Receptor Antagonist, Parasympatholytics, • Atropine-like Drugs) Atropine, the prototype drug of this clas

• ANTICHOLINERGIC DRUGS Natural alkaloids: Atropine, Hyoscine (Scopolamine), Semisynthetic derivatives • Homatropine, Hyoscine butyl bromide, Ipratropium bromide, • Tiotropium bromide Synthetic compounds • (A) Mydriatics: Cyclopentolate, tropicamide • (B) Antisecretory-antispasmodics: • Quaternary compounds: Oxyphenonium, clidinium, glycopyrrolate • Tertiary amines: dicyclomine, pirenzipine • (C) Vesicoselective: oxybutynine, flavoxate, tolterodine • (D) Antiparkinsonian (central Anticholinergics): Biperiden, Trihexyphenidyl(benzhexol)

• CNS An overall stimulant action but not appreciable at low doses which • produce peripheral effects because of restricted entry • Hyoscine produces central depressant effects even at low doses • Atropine stimulates many medullar centers – • vagal, respiratory, and vasоmotor • Basalganglia, it suppresses tremor and rigidity in parkinsonism • High doses cause cortical excitation, rest • lessness, disorientation, hallucinations, and delirium • followed by respiratory depression and coma.

CVS • Atropine causes tachycardia, due to blockade of • M 2 -receptors on SA node • Tachycardia is more marked in young adults than in children and the elderly. • Atropine shortens the refractory period of AV conduction, • Atropine does not influence BP

• • Eye Topical instillation of atropine (0. 1%) causes mydriasis, abolition of light reflex, and cycloplegia, lasting 7– 10 days. Results in photophobia and blurring of near vision. Intraocular tension? Specially in narrow angle glaucoma

• Smooth muscles. • All visceral smooth muscles with parasympathetic innervation are relaxed (M 3 -blokade). • Tone and amplitude of GIT are reduced. • Spasm may be reduced, constipation may occur. • Peristalsis is only incompletely • Atropine causes bronchodilation and reduced airway. Inflammatory • mediators (histamine, PGs, and kinins) increase vagal • activity in addition to their direct action on bronchial • muscle and glands. Atropine attenuates their action • by antagonizing the reflex vagal component. It has a • relaxant action on urinary bladder • Urinary retention can occur in older men with prostatic hyperplasia.

Glands • Atropine decreases sweat, salivary, tracheo-bronchial, and lacrimal secretion (M 3 -blockade) • Eyes� dry, talking, and swallowing� difficult. • Atropine decreases less the secretion of acid and pepsin and more of the mucus in the stomach. Body temperature • Rise in body temperature occurs at higher doses, and is due to both inhibition of sweating as well as stimulation of the temperature regulating centre in the hypothalamus. • Children are highly susceptible.

• Local anaesthetic action. Atropine has a mild anaesthetic action on the cornea. • The sensitivity of different organs and tissues • to atropine varies and can be graded as • saliva, sweat, bronchial secretion > • bronchial muscles > heart > intestin • bladder smooth muscles > gastric g • and gastric smooth muscles

• Pharmacokinetics • Atropine and hyoscine are rapidly absorbed from • GIT. Applied to the eyes they penetrate the cornea. • Passage across BBB is somewhat restricted. 50% • of atropine is metabolized in the liver and excreted • unchanged in urine. It has t 1/2 3– 4 h. Hyoscine is • more completely metabolized and has better BBB • penetration. Some rabbits have a specific atropine • esterase which degrades atropine very rapidly.

Unwanted effects • Dry mouth, difficulty in swallowing and talking; • Dry and hot skin (especially over the face and neck); • fever difficulty in micturition; • Photophobia , blurring of near vision; • Palpitation • Contraindication:

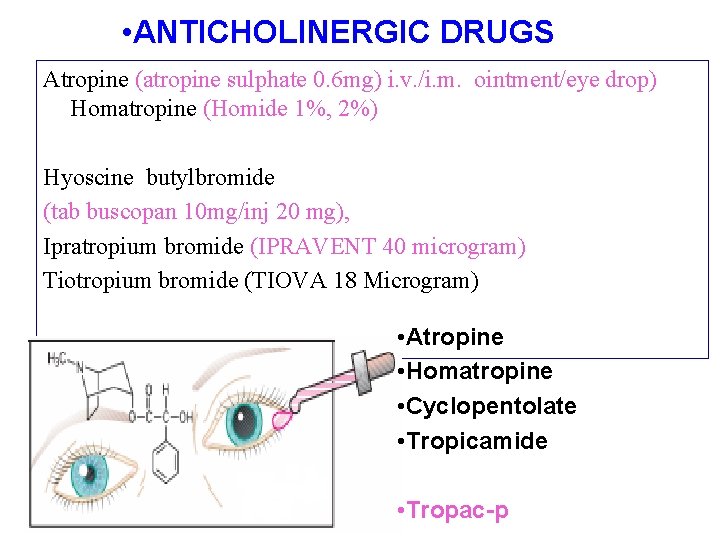
• ANTICHOLINERGIC DRUGS Atropine (atropine sulphate 0. 6 mg) i. v. /i. m. ointment/eye drop) Homatropine (Homide 1%, 2%) Hyoscine butylbromide (tab buscopan 10 mg/inj 20 mg), Ipratropium bromide (IPRAVENT 40 microgram) Tiotropium bromide (TIOVA 18 Microgram) • Atropine • Homatropine • Cyclopentolate • Tropicamide • Tropac-p

Clidinium (NORMAXIN 2. 5 mg, dicyclomine 10 mg, chlordiazepoxide) Glycopyrrolate (Pyroalte 0. 2 mg/ml, 10 ml vial) Tertiary amines: Dicyclomine (colimex drops 10 mg/ml with dimethicone) Pirenzipine Drotavarine (tab drotakind-M) VESICOSELECTIVE oxybutynine, flavoxate, tolterodine

USES • • • • Preanaesthetic medication Peptic ulcer Pulmonary embolism? ? ? COPD & Bronchial asthma As mydriatic agent for diagnosis refraction errors, Iridocycltis Adhesions between iris and lense Bradycardia Parkinsonism Motion sickness Lie detector test Relieve urinary frequency Dysmenorrhoea

CATECHOLAMINE n STORAGE OF CA n NA+ATP(4: 1 ) IS ABSORBED ON A n IN ADRENAL MEDULLA: NA DIFFUSES OUT n CYTOPLSM POOL OF CA IS KEPT LOW BY MAO CHROMOGRANIN OFCYTOPLASM METHYLATED TO ADR

RELEASE OF CAS ALONG WITH NA OR ADR+ATP+DOPAMINE HYDROXYLASE+CHROMAGRANIN n UPTAKE OF CAS n n AXONAL UPTAKE : ACTIVE AMINE PUMP NET TRANSPORT NA BY A Na+ coupled mechanism cocain, desipramine can block this pump n VESICULAR UPTAKE: VMAT (VESICULAR MONOAMINE TRANSPORTER) RESERPINE can block this pump METABOLISM CAS: n MAO IN CYTOPLASM n COMT (CATECHOLE-O-METHYL TRANSFERSE) LIVER & OTHER n VMA (VANILLYLMANDELIC ACID), 3 -METHOXY-4 -HYDROXY PHENYLETHYLENE GLYCOL, NORMETANEPHRINE, n 3, 4 DIHYDROXY MANDELLIC ACID CONJUGATION EXCRETION IN URINE n

Classification of drugs affecting the ANS n Parasympathetic nervous system Mimic acetylcholine = cholinergic = muscarinic agonists = parasympathomimetic Block acetylcholine = anticholinergic = muscarinic antagonist = parasympatholytic n Sympathetic nervous system Mimic norepinephrine = adrenergic agonist =Adrenoceptors= sympathomimetic Block norepinephrine = antiadrenergic = adrenergic antagonist = sympatholytic

ADRENALINE • HEART: increases HR by increasing slope of slow diastolic depolarization of cells in the SA node • Activates latent pacemaker in AV node • Cardiac contraction incraesed

• BLOOD VESSELS: vasoconstriction & vasodilation can occur depending on drug, dose, vascular beds • Cutaneous, mucus membrane, renal beds • Dose • Skeletal muscle •

• • RESPIRATION ADR NA ISPRENALINE

EYE • 1 vasoconstriction of ciliary muscle reduced aqueous fprmation • 2 reduced secretary activity of ciliary epithelium • 2 enhanced secretary activity of cilliary epithelium

GIT • • • Relaxation: & Bladder: Detruser relaxes & Trigone constricted 1 Uterus: Human: contraction nonpreg relaxation: pregnant • Skeletal muscle: neuromuscular transmission facilitated • CNS: • METABOLIC:

• • Adrenaline For systemic action, 0. 2 -0. 5 mg s. c. , i. m. , action lasts 1/2 to 2 hrs. ADRENALINE 1 mg/ml inj. As local vasoconstrictor, 1 in 200, 000 to 1 in 100, 000 added to lidocaine; in xylocaine with Adrenaline: lidocaine 21. 3 mg + adrenaline O. 005 mg/ ml. • Noradrenaline (levarterenol) • 2 -4 ug/min I. V. . infusion; local tissue necrosis occurs if the solution extravasates; • do not mix with Na. HCO 3 same bottle (rapid oxidation occurs); • Action starts declining within 5 min of discontinuing infusion. adrenor 2 mg (base)/2 ml amp. • Isoprenaline (Isoproterenol) 20 mg sublingual, 1 -2 mg i. m. , 5 -10 ug/min i. v. infusion; action lasts 1 -3 hrs. • It is occasionally used to maintain idioventricular rate till pacemaker is implanted. For bronchial asthma

• Adverse effects and contraindications: • Marked rise in BP cerebral haemorrhage, ventricular tachycardia/fibrillation, angina, MI doses • Adr is contraindicated in hypertensive, hyper-thyroid • AP patients. Adr not be given during anaesthesia halothane (risk of arrhythmias) • In patients receiving beta blockers (markecd rise in BP can occur due to unopposed action).

• • • • • THERAPEUTIC CLASSIFICATION OF ADRENERGIC DRUGS Pressor agents Noradrenaline Phenylephrine Ephedrine, Methoxamine Dopamjne, Mephentermine Cardiac stimulants Adrenaline, Dobutamine, Isoprenaline Bronchodilarors Salbutamol (Albuterol), Isoprenaline Terbutaline Salmeterol, Formoterol, Bambuterol Nasal decongestants Phenylephrine Naphazoline Xylometazoline Pseudoephedrine Oxymetazoline Phenyl propanolamine CNS stimulants Amphetamine Dexamphetamine Anorectics Fenfluramine, Sibutramine Dexfenfluramine Uterine relaxant and vasodilators Ritodrine, Salbutamol , Isoxsuprine, Terbutaline.

• Dopamine: (Dl and D 2) as well as adrenergic & 1 agonist. • D 1 1 1 action • Low dose of DA : Dl in renal & mesenteric BV are the most sensitive • Moderately doses : positive inotropic (direct 1 & Dl action + that due to NA release) & little chronotropic effect on heart. • Large doses infused: 1 action • At doses normally employed, it raises cardiac output and systolic BP with little effect on diastolic BP. • Does not penetrate BBB CNS effects. • DA : cardiogenic or septic shock and severe CHF to increase BP & urine outflow • i. v. infusion (0. 2 -1 mg/min): DOPAMINE, 200 mg in 5 ml amp

• Dobutamine: not a Dl or D 2 receptor agonist. • 1 (prominent action) + • At 2 -8 ug/kg/ min i. v. infusion: increased force of cardiac contraction and output, without significant change in heart rate, peripheral resistance • Dobutamine is 1 selctive agonist • Ephedrine: • Mainly acts indirectly but has some direct action on alpha and beta receptors also. • Repeated injections Tachyphylaxis • Resistant to MAO orally.

• Amphetamines • Central effects: alertness, jncreased concentration & attention span, euphoria, talkativeness, increased work capacity. Fatigue is allayed. Athletic performance is improved temporarily followed by deterioration • 'dope test' for athletes. • Reticular activating system is stimulated resulting in wakefulness and postponement of sleep deprivation • But short-lived & may be accompanied by anxiety, restlessness, tremor, dysphoria and agitation • Use in examinations can only be condemned • Potentiate antiepileptics, analgesics and anti motion-sickness drugs. Peripheral effects on heart and BP are not significant at the usual doses • Amphetamines are drugs of abuse & capable of producing marked psychological but little or no physical dependence

• Phenysephrine: selective 1 agonist, has negligible beta action • raises BP by causing vasoconstriction little cardiac action reflex bradycardia. Topical nasal decongestant Producing mydriasis when cycloplegia is not required. Phenylephrine tends to reduce IOT by constricting ciliary body blood vessels Orally administered nasal decongestant preparations. Central effects are not seen with usual clinical doses DECOLD PLUS 5 mg with paracetamol 400 mg + chlorpheniramine 2 mg + caffeine 15 mg DROSYN EYE DROPS 10%

• Methoxamine : 1 agonist • Mephentermine & +NA release • Not substrate for MAO &COMT

• SELECTIVE BETA-2 STIMULANTS • Salbutamol, Terbutaline, Salmeterol, Formoterol & Ritodrine • As uterine relaxant to delay premature labour (Ritodrine, Isoxsuprine) • In hyperkalemic familial periodic paralysis— BETA-2 agonists benefit by enhancing K+ uptake into muscles lowering plasma K+ levels • The most important side effect is muscle tremor; tachycardia

• • Nasal decongestants Phenylephrine Naphazoline Xylometazoline Pseudoephedrine Oxymetazoline Phenyl. Propanolamine • • • Anorectics Non adrenergic appetite centre Phenylpropanolamine Serotonergic satiety centre Fenfluramine, Dexfenfluramine Non adrenergic/Serotonergic : Sibutramine •

Therapeutic uses • • • • Hypotension Along with local anaesthetic agent As an styptics Nasal decongestant Cardiac arrest AV block: Isoprenaline CHF Bronchial asthma Mydriatic Hyperkinetic children Narcolepsy Obesity Uterine relaxant Insulin hypoglycemia Nocturnal enuresis in children

-ADRENERGIC BLOCKING DRUGS • adrenergic neurone blocking agents • - adrenergic blocking Drugs

• CLASSIFICATION • • Nonequilibrium type (non-competitive) Phenoxybenzamine • Equilibrium type (competitive) • A. Nonselective Ergot alkaloids: Ergotamine, Ergotoxine Hydrogenated ergot alkalolds: Dihydroergotamine, Dihydroergotoxine Imidazolines: Tolazoline, Phentolamine • B. 1 selective: Prazosin, Terazosin, Doxazosin, Tamsulosin • C. 2 selective: Yohimbine

• GENERAL EFFECTS OF BLOCKERS • Blockade of 1 TPR & VENOUS RETURN DECREASED & CO………. . BP? ? ? POSTURAL HYPOTENSION • Reflex tachycardia • Nasal stuffiness & miosis • Intestinal motility is increased • Hypotension reduce renal blood flow & g. f. r more complete reabsorption of Na & water increase in blood volume • Tone of s. m. in bladder trigone, sphincter & prostate is reduced( 1 blockade) improvement in BPH patients • • Contractions of vas deferens Ejaculation( response)

• Phenoxybenzamine • • Venodilatation is more prominent than arteriolar dilatation • In recumbent subjects cardiac output and blood flow to many organs are increased due to reduction in peripheral resistance & increased venous return • It tends to shift fluid from extravascular to vascular compartment. • Phenoxybenzamine is lipid soluble, penetrates brain and can produce CNS stimulation, nausea and vomiting on rapid i. v. injection • Oral doses produce, depression, tiredness and lethargy. postural hypotensiory , palpitation, nasal blockage, miosis, inhibition of ejaculation

• Phentolamine • Rapidly acting a blocker with short duration of action (in minutes). • 1 & 2 equally blockade • NA release increased and venodilatation predominates over arteriolar dilatation • Diagnosis & intraoperative management of Pheochromocytoma • and for control of hypertension due to clonidine withdrawal, cheese • Reaction • It is the most suitable a blocker for local infiltration to counteract vasoconstriction due to extravasated NA/DA

Prazosin • Highl selective 1: 2 100 o: 1 • Only mild tachycardia; NA released is not increased due to absence of 2 blockade • Prazosin dilates arterioles more than vein Postural hypotension is less marked • ‘first dose effect can be minimized by: • Starting with a low doses • Taking it at bedtime. • Prazosin is effective orally (bioavailab • -60%), highly bound to plasma proteins • Antihypertensive • BPH

• Tamsulosin • This uroselectivec 1 A / 1 D • 1 B BLOOD VESSEL • Tamsulosin : URIMAX,

USES OF BLOCKERS • • • Pheochromocytoma & Phentolamine test Hypertension Clonidine withdrawal & Cheese reaction Benign hypertrophy of prastate (EHP) Secondary shock Shock due to blood or fluid loss is accompamed by reflex vasoconstriction • Peripheral vascular disease • Papaverine & Phentolamine induced penile erection therapy for impotence (inj corpus cavernosum ) • Cangestive heart fatlure (CHF)? ? ?

CLASSIFICATION ADRENERGTCB LOCKTNGD RUGS • • • Nonselective ( 1 & 2) Without intrinsic sympathomimetic activity Propranolol, Sotalol, Timolol. With intrinsic sympathomimetic activity Pindolol With additional a blocking property Labetalol, Carvedilol Cardioselective ( 1 ) Metoprolol, Atenolol, Acebutolol, Bisoprolol Esmolol, Betaxolol, Celiprolol, Nebivolol

PHARMACOLOGICAL ACTIONS • Heart Propranolol decreases HR, FC (at relatively higher doses) & C. O. • Effects on a normal resting subject are mild, but become prominent under sympathetic over-activity (exercise, emotion). • Cardiac work & oxygen consumption are reduced • Coronary flow is reduced but this is largely restricted to the subepicardial region. • Overall effect in angina patients is improvement exercise tolerance is increased • The A-V conduction is delayed.

• Blood vessels Propranolol blocks vasodilatation • On prolonged administration BP gradually falls in hypertensive subjects but not in normotensive • Total peripheral resistance (t. p r. ) is increased • With continued treatment, resistance vessels graduallv adapt to chronically reduced c. o. so that t. p. r. decreases-both systolic and diastolic BP fall • • Reduced NA release from sympathetic terminals due to blockade of presynaptic beta -receptor mediated facilitation of the release process • Decreased renin release from kidney • Central action reducing sympathetic outflow.

• Respiratory tract: B 2 • • • CNS: anxiety & migrain Metabolic: Hypglycemia, HDL/LDL: (B 2) Skeletal muscle: B 2 Eye: Tremors: B 2 • PHARMACOKINETICS

• • • • Uses Hypertension AP Cardiac arrhythmias MI By preventing reinfarction By preventing sudden ventricular fibrillation at the second attack of MI Myocardial salvage during evolution of MI CHF THYROTOXICISIS MIGRAINE ESSENTIAL TREMORS BETA-2 action GLAUCOMA Anxiety Pheochromocytoma ADRs & contraindications