Autoimmune Encephalitis Morning Report 22218 Jessica MagidBernstein MD

Autoimmune Encephalitis Morning Report 2/22/18 Jessica Magid-Bernstein, MD, Ph. D

Definition v. Immune mediated encephalitis includes paraneoplastic and autoimmune types v. Paraneoplastic encephalitidies v Always cancer related v. Autoimmune encephalitidies v Associated with antibodies against neuronal cell surface and synaptic proteins v May or may not be cancer-associated

Clinical Presentation v. Wide clinical spectrum v. Typical limbic encephalitis – evolves over days to weeks v. Acute or subacute mood and behavior changes v. Short term memory problems v. Focal seizures with impaired awareness v. Cognitive dysfunction v. Hypothalamic dysfunction may occur – hyperthermia, somnolence, endocrine abnormalities v. Complex neuropsychiatric symptoms v. Deficits of memory, cognition, psychosis, seizures, abnormal movements, or coma
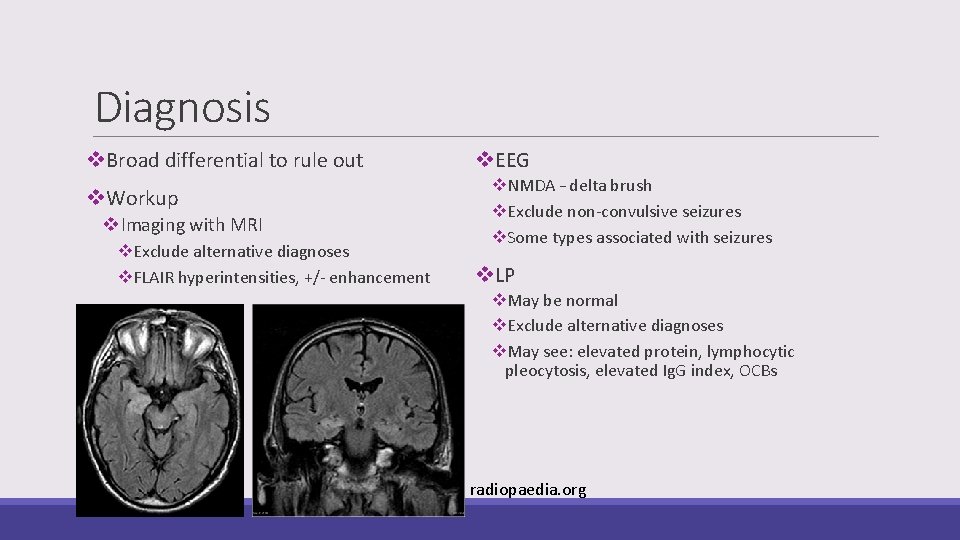
Diagnosis v. Broad differential to rule out v. Workup v. Imaging with MRI v. Exclude alternative diagnoses v. FLAIR hyperintensities, +/- enhancement v. EEG v. NMDA – delta brush v. Exclude non-convulsive seizures v. Some types associated with seizures v. LP v. May be normal v. Exclude alternative diagnoses v. May see: elevated protein, lymphocytic pleocytosis, elevated Ig. G index, OCBs radiopaedia. org

Diagnosis – antibody testing v. Test serum and CSF v. Be weary of serum Abs only, more likely to be false positive v. Correlate with clinical syndrome

Specific syndromes v. Anti-NMDA – prominent psychiatric manifestations; most associated with ovarian teratoma v. Anti-LGI 1 (previously attributed to VGKC Abs) – memory problems, confusion, FBD seizures; CSF often normal v. Anti-CASPR 2 (previously attributed to VGKC Abs) – older men, slower course, usually a/w thymoma v. Anti-AMPA – usually women, limbic encephalitis +/- seizures, 2/3 a/w neoplasm (lung, thymus, breast) v. Anti-GABA-A – rapid and progressive, a/w status epilepticus and/or EPC, 50% in children v. Anti-GABA-B – adults; often includes seizures, ataxia, or opsoclonus-myoclonus; 50% a/w SCLC v. Anti-Ig. LON 5 – REM and non-REM parasomnias, OSA, very poor prognosis, p. Tau on autopsy v. DPPX-associated – central hyperexcitability; CSF lymph pleocytosis; often relapse

Treatment v. Treat as soon as infection is ruled out v. Damage occurs rapidly and is often irreversible v. Immunotherapy is gold standard v. IVIg v. Glucocorticoids v. PLEX v. Cyclophosphamide v. Rituximab v. Antibody titers often do not correlate with disease v. Treat seizures aggressively – often do not require long-term AEDs v. Variable prognosis – depends on timing of diagnosis/treatment, also specific syndrome

References v. Dalmau, J. & Rosenfeld, M. (2018). Paraneoplastic and autoimmune encephalitis. In A. F. Eichler (Ed. ), Up. To. Date. Retrieved February 21, 2018, from https: //www. uptodate. com/contents/paraneoplastic-and-autoimmune-encephalitis v. Van Sonderen, A, et al. (2016). Anti-LGI 1 encephalitis: Clinical syndrome and long-term follow up. Neurology. 87: 1449 -1456. v. Van Sonderen, A, et al. (2016). From VGKC to LGI 1 and Caspr 2 encephalitis: The evolution of a disease entity over time. Autoimmunity Reviews. 15: 970 -974.

Questions?
- Slides: 9