Attenuation Differences in Subdural Effusion and Acute Subdural
Attenuation Differences in Subdural Effusion and Acute Subdural Hematoma Following Administration of Iodinated Contrast e. P-123 R. Phelps Kelley, Jason Talbott, Alina Uzelac University of California, San Francisco Zuckerberg San Francisco General Hospital

Disclosures • Jason Talbott is a member of data monitoring committee (DMC) for Stem. Cells, Inc.

Introduction (1) • 3 types of traumatic subdural collections have been classified [1, 2, 5, 6]: • Acute trauma: • 1. Hematoma (SDH) – tear in bridging veins causes hemorrhage into subdural space • 2. Hygroma (SDG) – tear in arachnoid mater causes flow of cerebrospinal fluid (CSF) into subdural space • Remote trauma: • 3. Effusion (SDE) – CSF-density collections in absence of arachnoid tear, arising weeks to months after trauma

Introduction (2) • Timely, accurate diagnosis of a given subdural entity affects management and outcomes: • SDH may require decompressive craniotomy; delay in operative management is associated with high mortality [9, 10] • SDG/E are often asymptomatic and infrequently require surgical intervention [7, 8]

Introduction (3) • In the trauma setting, NCCTH is often performed in conjunction with subsequent contrast-enhanced CT (CECT) of the chest, abdomen, pelvis or extremities for polytrauma • Contrast can extravasate into SDH [3], SDG and SDE [4, 5]. • NCCTH is often repeated within 24 hours in the setting of acute findings on baseline NCCTH or in patients on anticoagulation

Introduction (4) • Contrast extravasation may lead to confusion, with enhancing SDG/E mimicking acute SDH • Correct diagnosis of subdural entities may avoid delayed or unnecessary repeat imaging and intervention.

Purpose 1. To characterize the enhancement and washout of subdural collections compared to baseline NCCTH following the administration of intravenous contrast 2. To evaluate whether enhancement characteristics allow the accurate differentiation of SDH from SDG/E on NCCTH 3. To determine the utility of blood pool attenuation measured in the superior sagittal sinus (SSS) as internal reference standard of enhancement

Materials & Methods (1) • Retrospective analysis of blunt head trauma patients at major level I trauma center between 2010 and 2015 who met the following criteria: • Baseline NCCTH obtained in the emergency department, with SDH, SDG or SDE documented in the final radiology report • Subsequent CECT (of any body part) prior to repeat NCCTH • Repeat NCCTH within 24 hours of the baseline NCCTH • 34 patients met inclusion criteria: • 23/34 patients underwent a third NCCTH within 24 hours, which was also included in the study

Materials & Methods (2) • NCCTH exams were stratified by time since administration of contrast: • Pre-contrast • 3 -8. 5 hours post-contrast (mean time: 5. 8 h) • 8. 5 -24 hours post-contrast (mean time: 14. 9 h) • For each NCCTH, the following were measured: • Attenuation in Hounsfield Units (HU) and size in millimeters (mm) of subdural collections • Attenuation in HU of CSF within the lateral ventricles and of blood pool within the SSS

Materials & Methods (3) • Subdural collections were retrospectively characterized as SDH if pre-contrast baseline attenuation was >40 HU, and as SDG/E if <40 HU • The unpaired two-tailed Student’s t-test was used to test for the difference in the mean attenuation of SDH vs. SDG/E at each timepoint, with p<0. 05 considered significant • The paired two-tailed Student’s t-test was used to test for the difference in mean attenuation in SDH or SDG/E between timepoints
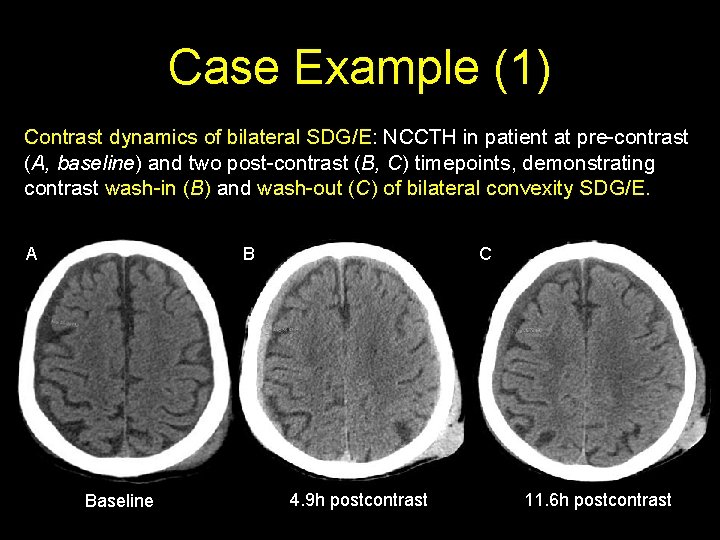
Case Example (1) Contrast dynamics of bilateral SDG/E: NCCTH in patient at pre-contrast (A, baseline) and two post-contrast (B, C) timepoints, demonstrating contrast wash-in (B) and wash-out (C) of bilateral convexity SDG/E. A B Baseline C 4. 9 h postcontrast 11. 6 h postcontrast
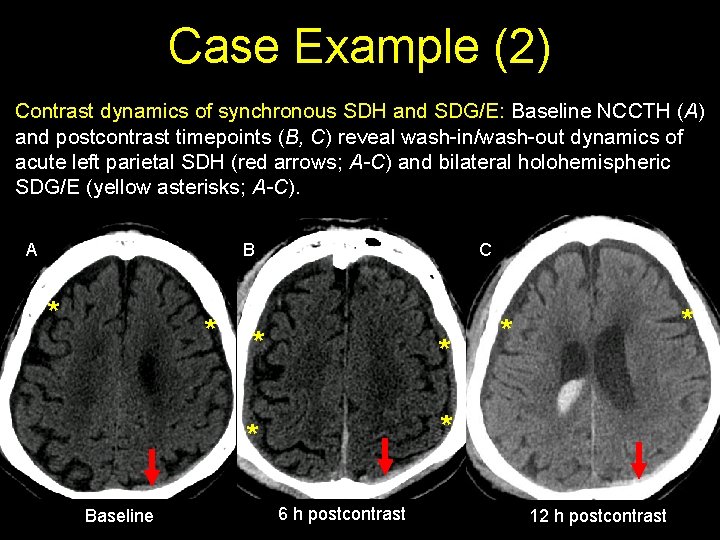
Case Example (2) Contrast dynamics of synchronous SDH and SDG/E: Baseline NCCTH (A) and postcontrast timepoints (B, C) reveal wash-in/wash-out dynamics of acute left parietal SDH (red arrows; A-C) and bilateral holohemispheric SDG/E (yellow asterisks; A-C). A B * * Baseline C * * 6 h postcontrast * * 12 h postcontrast
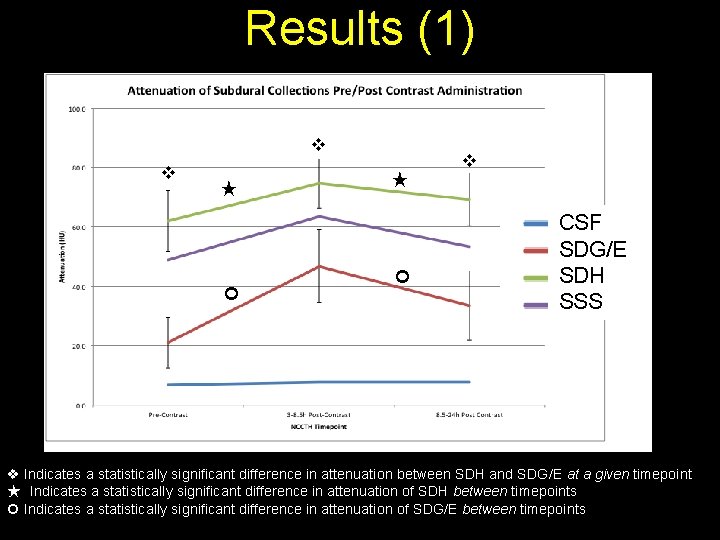
Results (1) ★ ★ CSF SDG/E SDH SSS Indicates a statistically significant difference in attenuation between SDH and SDG/E at a given timepoint ★ Indicates a statistically significant difference in attenuation of SDH between timepoints Indicates a statistically significant difference in attenuation of SDG/E between timepoints
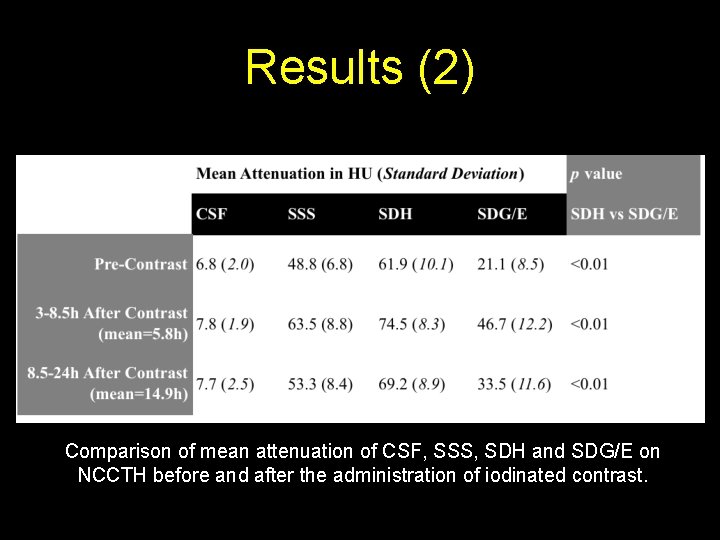
Results (2) Comparison of mean attenuation of CSF, SSS, SDH and SDG/E on NCCTH before and after the administration of iodinated contrast.

Results (3) • Following contrast administration, SDG/E and SDH significantly enhance (compared to baseline NCCTH) at 3 -8. 5 h (p<0. 01) and significantly washout 8. 5 -24 h post-contrast (p<0. 01) • SDH has significantly higher attenuation than SDG/E at all time points (all p<0. 01) • The wash-in/wash-out of SDG/E is not associated with a significant change in size (mean axial short axis: 6. 3 mm pre-contrast, 6. 5 mm at 3 -8. 5 h, and 7. 7 mm at 8. 5 -24 h; all p>0. 1)

Results (4) • Enhancing SDH is always HYPERDENSE to SSS at precontrast, 3. 5 -8 h postcontrast and 8. 5 -24 h postcontrast timepoints • Enhancing SDG/E is always HYPODENSE to SSS at precontrast, 3. 5 -8 h postcontrast and 8. 5 -24 h postcontrast timepoints

Conclusions • Enhancing SDG/E may mimic acute SDH at 3. 58 h post contrast administration (mean HU 46. 7). • In order to avoid mistaking enhancing SDG/E for interval acute SDH, it is important to account for recent contrast administration. • Blood pool (SSS) attenuation provides an internal reference for distinguishing SDH from SDG/E - Enhancing SDG/E always HYPODENSE to SSS - Enhancing SDH always HYPERDENSE to SSS

References 1. Liu Y, Gong J, Li F, et al. Traumatic subdural hydroma: Clinical characteristics and classification. Injury 2009; 40: 968 -72 2. Ohno K, Suzuki R, Masaoka H, et al. Chronic subdural haematoma preceded by persistent traumatic subdural fluid collection. J Neurol Neurosurg Psych 1987; 50: 1694 -7 3. Yasui T 1, Komiyama M, Kishi H, et al. Angiographic extravasation of contrast medium in acute "spontaneous" subdural hematoma. Surg Neurol. 1995 Jan; 43(1): 61 -7. 4. Zamora CA, Lin DD. Enhancing subdural effusions mimicking acute subdural hematomas following angiography and endovascular procedures: report of 2 cases. J Neurosurg 2015; 123: 1184 -7 5. Mori K, Maeda M. Delayed magnetic resonance imaging with Gd. D-DTPA differentiates subdural hygroma and subdural effusion. Surg Neurol 2000; 53: 303– 11

References 6. Lee KS, Bae WK, Bae HG, et al. The Computed Tomographic Attenuation and the Age of Subdural Hematomas. J Korean Med Sci. 1997 Aug; 12(4): 353 -9. 7. Lee KS, Bae WK, Park YT, Yun IG. The pathogenesis and fate of traumatic subdural hygroma. Br J Neurosurg 1994; 8: 551– 558. 8. Ishibashi A, Yokokura Y, Miyagi J. Clinical analysis of nineteen patients with traumatic subdural hygromas. Kurume Med J 1994; 41: 81– 85. 9. Dent DL 1, Croce MA, Menke PG, et al. Prognostic factors after acute subdural hematoma. J Trauma. 1995 Jul; 39(1): 36 -42; discussion 42 -3. 10. Seelig JM, Becker DP, Miller JD, et al. Traumatic acute subdural hematoma: major mortality reduction in comatose patients treated within four hours. . N Engl J Med. 1981 Jun 18; 304(25): 1511 -8.
- Slides: 19