ATS TRAINING COURSE Intraoperative blood salvage To Start

ATS TRAINING COURSE Intraoperative blood salvage
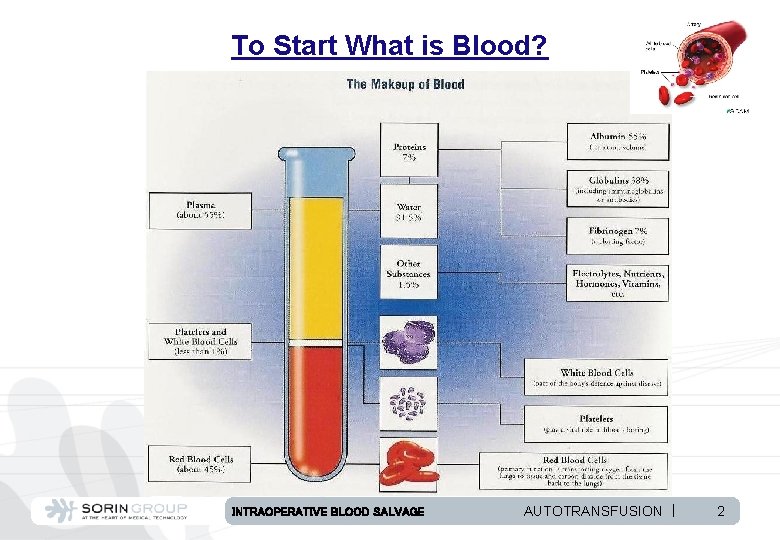
To Start What is Blood? INTRAOPERATIVE BLOOD SALVAGE AUTOTRANSFUSION | 2

AUTOTRANSFUSION FOR A BETTER PATIENT OUTCOME … 1 - DEFINITION : Autotransfusion is a process when a person receives their own blood for a transfusion, instead of banked donor blood. Blood can be pre-donated before a surgery, or can be collected during and after the surgery using a device commonly known as the Cell Salvage device. The Cell Salvage device is utilized in surgeries where there is expected a large volume blood loss. For example, aneurysm, total joint replacements and spinal surgeries. INTRAOPERATIVE BLOOD SALVAGE AUTOTRANSFUSION | 3

AUTOTRANSFUSION FOR A BETTER PATIENT OUTCOME … 2 - HISTORY OF AUTOTRANSFUSION : The first documented use of the procedure was in 1818 (James Blundell ), and interest in the practice continued until the Second World War, at which point blood supply became less of an issue, due to the increased number of blood donors. Later, interest in the procedure returned with new automated machinery being developed for it. Autotransfusion is used in a number of cardiac, trauma and orthopedic cases, amongst others, and it carries advantages, including the reduction of infection risk and the provision of more functional cells. INTRAOPERATIVE BLOOD SALVAGE AUTOTRANSFUSION | 4

AUTOTRANSFUSION FOR A BETTER PATIENT OUTCOME … 3 - INDICATIONS FOR AUTOTRANSFUSION: Autotransfusion is intended for use in situations characterized by the loss of one or more units of blood and may be particularly advantageous for use in cases involving rare blood groups, risk of infectious disease transmission, restricted homologous blood supply or other medical situations for which the use of homologous blood is contraindicated. Autotransfusion is commonly used intraoperatively and postoperatively. Intraoperative autotransfusion refers to recovery of blood lost during surgery or the concentration of fluid in an extracorporeal circuit. Postoperative autotransfusion refers to the recovery of blood in the extracorporeal circuit at the end of surgery or from aspirated drainage. INTRAOPERATIVE BLOOD SALVAGE AUTOTRANSFUSION | 5

AUTOTRANSFUSION FOR A BETTER PATIENT OUTCOME … 4 - IN WHICH OPERATION CAN WE USE AUTOTRANSFUSION: Cardiac: Cardiothoracic, Coronary Artery Bypass, Cardiac Valvular Repair / Replacement, Aortic Arch Aneurysms, Thoracic Trauma, Cardiac Transplantation l Trauma: Subdural Hematoma, Chest Injuries, Liver Fractures, Kidney Fractures, Major Vessel Lacerations, Aneurysms, Gun Shot Wounds, Stab Wounds, Extremity Reimplantations, Splenectomy, Blunt Trauma (Thoracic or Abdominal) l Orthopedic: Spinal Instrumentation, Spinal Fusion, Discectomie, Laminectomy, Total shoulder replacement, Total hip replacement, Total knee replacement, Femur Fractures, Open Reduction Internal Fixation Pelvic Fractures, IM Rodding l Other: Ectopic Pregnancy, Liver Resection (Non-Malignant), Porto-Caval Shunts, Liver Transplant, Nephrectomy (Non-Malignant), Speno-Renal Shunts, Abdominal Aortic Aneurysm, Aorto-Femoral Reconstruction, Major Vessel Resection, Hysterectomy (Non. Malignant), Cerebral Aneurysms, Craniotomy (Non-Malignant), Thoracotomy (Non. Malignant) l INTRAOPERATIVE BLOOD SALVAGE AUTOTRANSFUSION | 6

AUTOTRANSFUSION FOR A BETTER PATIENT OUTCOME … 5 - Contraindications The use of blood recovered from the operative field is contraindicated in the presence of bacterial contamination or malignancy. The use of autotransfusion in the presence of such contamination may result in the dissemination of pathologic microorganisms and / or malignant cells. The following statements reflect current clinical concerns involving autotransfusion contraindications. INTRAOPERATIVE BLOOD SALVAGE AUTOTRANSFUSION | 7

AUTOTRANSFUSION FOR A BETTER PATIENT OUTCOME … 5. 1 - Exceptions to those contraindications are under investigations: 5. 1. 1 - Malignancy: Blood irradiation for intraoperative autotransfusion in cancer surgery demonstration of efficient elimination of contaminating tumor cells. Hansen E, Knuechel R, Altmeppen J, Taeger K. Department of Anesthesiology, University of Regensburg, Germany. Transfusion. 1999 Jun; 39(6): 608 -15. l Intraoperative cell salvage during radical cystectomy does not affect long-term survival. Nieder AM, Manoharan M, Yang Y, Soloway MS. Department of Urology, University of Miami Miller School of Medicine, Miami, Florida 33140, USA. Urology. 2007 May; 69(5): 881 -4. l Intraoperative blood salvage in cancer surgery: safe and effective? Hansen E, Bechmann V, Altmeppen J. Department of Anesthesiologie, University of Regensburg, Germany. Transfus Apher Sci. 2002 Oct; 27(2): 153 -7. According to our experience with more than 700 procedures the combination of blood salvage with blood irradiation also is very effective in saving blood resources. With this autologous, fresh, washed RBC a blood product of excellent quality is available for optimal hemotherapy in cancer patients. l Blood salvage use in gynecologic oncology. Nagarsheth NP, Sharma T, Shander A, Awan A. Division of Gynecologic Oncology, Department of Obstetrics, Gynecology and Reproductive Science, Mount Sinai Medical Center, New York 10029 -6574, USA. Transfusion. 2009 Oct; 49(10): 2048 -53. Epub 2009 Jun 23. In this series of patients undergoing surgery for malignancies on the gynecologic oncology service, blood salvage with LRF was not definitively associated with hematogenous dissemination. l INTRAOPERATIVE BLOOD SALVAGE AUTOTRANSFUSION | 8

AUTOTRANSFUSION FOR A BETTER PATIENT OUTCOME … 5. 1. 2 Bacterial contamination: Intraoperative blood salvage and leukocyte depletion during liver transplantation with bacterial contamination. Liang TB, Li JJ, Li DL, Liang L, Bai XL, Zheng SS. Department of Hepatobiliary and Pancreatic Surgery, Key Laboratory of Multi-organ Transplantation of Ministry of Public Health, Key Laboratory of Organ Transplantation of Zhejiang Province, First Affiliated Hospital, School of Medicine, Zhejiang University, Hangzhou, China. Clin Transplant. 2010 Mar 1; 24(2): 265 -72. Epub 2009 Sep 24. l CONCLUSIONS: Autotransfusion devices with an additional LDF could significantly eliminate bacterial contaminants of shed blood during OLT Autologous transfusion of shed mediastinal blood after coronary artery bypass grafting and bacterial contamination. Andreasen AS, Schmidt H, Jarløv JO, Skov R. Department of Anesthesiology, Gentofte Hospital, Copenhagen, Denmark. Ann Thorac Surg. 2001 Oct; 72(4): 1327 -30. We found no significant difference in infection variables between patients with or without bacterial growth in the cultures. No patients suffered from early postoperative infectious complications. CONCLUSIONS: There is no further contamination of the shed blood during the period between initiating the autologous transfusion and the following morning. l INTRAOPERATIVE BLOOD SALVAGE AUTOTRANSFUSION | 9

AUTOTRANSFUSION FOR A BETTER PATIENT OUTCOME … 5. 2. 1: Recommandations: Despite the many studies undergoing to bypass those contraindications all major companies do not recommend the usage of there Autotransfusion device in case of contamination or malignancy. 5. 2. 2 Emergency: Although there are contraindications In life saving situations with the consent of the surgeon, Autotransfusion can be utilized in the presence of the previous stated contraindications i. e. sepsis, bowel contamination and malignancy. INTRAOPERATIVE BLOOD SALVAGE AUTOTRANSFUSION | 10

AUTOTRANSFUSION FOR A BETTER PATIENT OUTCOME … 6 -Disadvantages The disadvantage of autotransfusion is the depletion of plasma and platelets. The washed autotransfusion system removes the plasma and platelets, to eliminate activated clotting factors and activated platelets which would cause coagulopathy if they were reinfused to the patient. This disadvantage is only evident when very large blood losses occur. The autotransfusionist monitors blood loss and will recommend the transfusion of fresh frozen plasma (FFP) and platelets when the blood loss and return of autotransfusion blood increases. Typically the patient will require FFP and platelets as the estimated blood loss exceeds half of the patient's blood volume. When possible diagnostic tests should be performed to determine the need for any blood products (ie. PRBCs, FFP and Platelets). INTRAOPERATIVE BLOOD SALVAGE AUTOTRANSFUSION | 11

AUTOTRANSFUSION FOR A BETTER PATIENT OUTCOME … Advantages: • High levels of 2, 3 DPG • Normothermic • p. H relatively normal • Lower risk of Infectious Diseases • Functionally superior cells • Lower Potassium (compared to stored blood) • Quickly available • High RBC recovery over 90% • High Hct concentration > 50% Substances washed out: • Plasma • Platelets • White Cells • Anticoagulant Solution • Plasma free Hemoglobin • Cellular stroma • Activated clotting factors • Intracellular Enzymes • Potassium • Plasma bound Antibiotics INTRAOPERATIVE BLOOD SALVAGE AUTOTRANSFUSION | 12

AUTOTRANSFUSION FOR A BETTER PATIENT OUTCOME … WHY AUTOTRANSFUSION IS BETTER THEN STANDART HOMOLOGOUS BLOOD TRANSFUSION? INTRAOPERATIVE BLOOD SALVAGE AUTOTRANSFUSION | 13
AUTOTRANSFUSION FOR A BETTER PATIENT OUTCOME … l Effects of storage of blood: ↓PH ↑K+ ↓ 2, 3 DPG ↓Platelets, platelet function lost by 48 hours. ↓Coagulations factors (V & VIII INTRAOPERATIVE BLOOD SALVAGE AUTOTRANSFUSION | 14

AUTOTRANSFUSION FOR A BETTER PATIENT OUTCOME … PROBLEM RELATED TO THE TRANSFUSION OF HOMOLOGOUS BLOOD: l l l Transfusion reactions: Infections, viruses and most importantly Immunosupression / Immunomodulation Transfusion-related acute lung injury (TRALI) is a serious complication of blood transfusions that is thought to be most commonly caused by a reaction to White Blood Cell antibodies present primarily in the plasma component of blood products • When transfused, these antibodies can sometimes activate a type of White Blood Cell called a granulocyte, which causes plasma to leak into the lungs, creating fluid accumulation, a condition referred to as acute pulmonary edema There is currently no screening test for the prevention of TRALI, and there is no single intervention that can eliminate the risk of TRALI (1: 2000) INTRAOPERATIVE BLOOD SALVAGE AUTOTRANSFUSION | 15

AUTOTRANSFUSION FOR A BETTER PATIENT OUTCOME … Frequency and outcomes of blood products transfusion across procedures and clinical conditions warranting inpatient care: an analysis of the 2004 healthcare cost and utilization project nationwide inpatient sample database. Morton J, Anastassopoulos KP, Patel ST, Lerner JH, Ryan KJ, Goss TF, Dodd SL. Stanford University Medical Center, Stanford, CA, USA. l The objective of this retrospective cohort study was to assess frequency and outcomes associated with blood products transfusion. Data from the 2004 Nationwide Inpatient Sample database were used. Length of stay (LOS), postoperative infections, noninfectious transfusion-related complications, in-hospital mortality, and total charges were evaluated for transfused and nontransfused cohorts. Of the estimated 38. 66 million discharges in the United States in 2004, 5. 8% (2. 33 million) were associated with blood products transfusion. Average LOS was 2. 5 days longer, and charges were $17 194 higher for the transfused cohort (P <. 0001). Odds of death were 1. 7 times higher (P <. 0001) and odds of infection 1. 9 times higher (P <. 0001) for the transfused cohort. Increased provider awareness and recognition of the frequency and potential negative outcomes of blood products transfusion may encourage the adoption of novel approaches to minimize intraoperative and early postoperative bleeding, reduce transfusion requirements, and most important, improve patient-level postoperative outcomes and health-related quality of life. l INTRAOPERATIVE BLOOD SALVAGE AUTOTRANSFUSION | 16

AUTOTRANSFUSION FOR A BETTER PATIENT OUTCOME … Transfusions blamed for deaths after heart bypass NEW YORK (Reuters Life) - Getting a blood transfusion during or after heart bypass surgery may raise the risk of dying in the next few months after the operation, new research suggests. Moreover, this may explain in part why women are more likely than men to die after coronary artery bypass grafting (CABG), since women more commonly need transfusions than men do. "To the best of our knowledge, this is the first study to state that. . . transfusions may be the reason why women have a greater post-CABG mortality than men, " Dr. Mary A. M. Rogers, from the University of Michigan in Ann Arbor, said in a statement. In a study of Michigan Medicare beneficiaries, 88 percent of female CABG patients received a blood transfusion compared with 67 percent of male patients. Patients who received a blood transfusion were 5. 6 -times more likely to die within 100 days of undergoing heart bypass surgery than were non-transfused patients, the report indicates. © Reuters 2007. All Rights Reserved. l INTRAOPERATIVE BLOOD SALVAGE AUTOTRANSFUSION | 17

AUTOTRANSFUSION FOR A BETTER PATIENT OUTCOME … Older Blood carries Greater Morbidity and Mortality l Duration of red-cell storage and complications after cardiac surgery. N England J Med 2008 Mar 20; 358(12): 1229 -39. Koch CG, et al. l BACKGROUND: Stored cells undergo progressive structural and functional changes over time. We tested the hypothesis that serious complications and mortality after cardiac surgery are increased when transfused red cells are stored for more than 2 weeks. METHODS: We examined data from patients given red-cell transfusions during coronary-artery bypass grafting, heart-valve surgery, or both between June 30, 1998, and January 30, 2006. A total of 2872 patients received 8802 units of blood that had been stored for 14 days or less ("newer blood"), and 3130 patients received 10, 782 units of blood that had been stored for more than 14 days ("older blood"). Multivariable logistic regression with propensityscore methods was used to examine the effect of the duration of storage on outcomes. Survival was estimated by the Kaplan-Meier method and Blackstone's decomposition method. RESULTS: The median duration of storage was 11 days for newer blood and 20 days for older blood. Patients who were given older units had higher rates of in-hospital mortality (2. 8% vs. 1. 7%, P=0. 004), intubation beyond 72 hours (9. 7% vs. 5. 6%, P<0. 001), renal failure (2. 7% vs. 1. 6%, P=0. 003), and sepsis or septicemia (4. 0% vs. 2. 8%, P=0. 01). A composite of complications was more common in patients given older blood (25. 9% vs. 22. 4%, P=0. 001). Similarly, older blood was associated with an increase in the risk-adjusted rate of the composite outcome (P=0. 03). At 1 year, mortality was significantly less in patients given newer blood (7. 4% vs. 11. 0%, P<0. 001). INTRAOPERATIVE BLOOD SALVAGE AUTOTRANSFUSION | 18 CONCLUSIONS: In patients undergoing cardiac surgery, transfusion of red cells that

AUTOTRANSFUSION FOR A BETTER PATIENT OUTCOME … Increased mortality, postoperative morbidity, and cost after red blood cell transfusion in patients having cardiac surgery. Circulation 2007 Nov 12 Murphy GJ, Reeves BC, Rogers CA, l BACKGROUND: Red blood cell transfusion can both benefit and harm. To inform decisions about transfusion, we aimed to quantify associations of transfusion with clinical outcomes and cost in patients having cardiac surgery. Methods and RESULTS: Clinical, hematology, and blood transfusion databases were linked with the UK population register. Additional hematocrit information was obtained from intensive care unit charts. Composite infection (respiratory or wound infection or septicemia) and ischemic outcomes (myocardial infarction, stroke, renal impairment, or failure) were prespecified as co-primary end points. Secondary outcomes were resource use, cost, and survival. Associations were estimated by regression modeling with adjustment for potential confounding. All adult patients having cardiac surgery between April 1, 1996, and December 31, 2003, with key exposure and outcome data were included (98%). Adjusted odds ratios for composite infection (737 of 8516) and ischemic outcomes (832 of 8518) for transfused versus non-transfused patients were 3. 38 (95% confidence interval [CI], 2. 60 to 4. 40) and 3. 35 (95% CI, 2. 68 to 4. 35), respectively. Transfusion was associated with increased relative cost of admission (any transfusion, 1. 42 times [95% CI, 1. 37 to 1. 46], varying from 1. 11 for 1 U to 3. 35 for >9 U). At any time after their operations, transfused patients were less likely to have been discharged from hospital (hazard ratio [HR], 0. 63; 95% CI, 0. 60 to 0. 67) and were more likely to have died (0 to 30 days: HR, 6. 69; 95% CI, 3. 66 to 15. 1; 31 days to 1 year: HR, 2. 59; 95% CI, 1. 68 to 4. 17; >1 year: HR, 1. 32; 95% CI, 1. 08 to 1. 64). | 19 AUTOTRANSFUSION INTRAOPERATIVE BLOOD SALVAGE CONCLUSIONS. Red blood cell transfusion in patients having cardiac surgery is strongly associated with both infection and ischemic postoperative morbidity, hospital stay,

AUTOTRANSFUSION FOR A BETTER PATIENT OUTCOME … Two New Clinical Studies Show That Limited Exposure to Blood Transfusion Significantly Increases Morbidity and Mortality After Surgery: l 1) Bernard AC et al. Intraoperative transfusion of 1 U to 2 U of packed red blood cells is associated with increased 30 -day mortality, surgical site infection, pneumonia, and sepsis in general surgery patients. Journal of the American College of Surgeons. 2009; 208: 931 -937. l (2) Surgenor SD et al, for the Northern New England Cardiovascular Disease Study Group. The Association of Perioperative Red Blood Cell Transfusions and Decreased Long-Term Survival After Cardiac Surgery. Anesthesia & Analgesia 2009; 108: 1741 -1746. l In the general surgery study, researchers evaluated 125, 177 patients from 121 hospitals and showed that after adjusting for all risk variables, transfusion of a single unit of blood increased 30 -day mortality by 32% and morbidity (pneumonia, sepsis, or surgical site infection) by 23%. Transfusion of two units of blood increased the mortality risk by 38% and morbidity risk by 40%. In the cardiac surgery study, researchers evaluated long-term survival of 9, 079 patients at eight hospitals and showed that transfusion. AUTOTRANSFUSION of one or two units of | 20 INTRAOPERATIVE BLOOD SALVAGE blood increased six-month mortality 67% and five-year mortality 16%.

AUTOTRANSFUSION FOR A BETTER PATIENT OUTCOME … “More than 75 million units of blood are donated each year throughout the world. A significant proportion of these expose recipients of blood and blood products to unnecessary risk” WHO (World Health Organization) BLOOD TRANSFUSION SAFETY Information Sheet for National Health Authorities INTRAOPERATIVE BLOOD SALVAGE AUTOTRANSFUSION | 21

AUTOTRANSFUSION FOR A BETTER PATIENT OUTCOME … INTRAOPERATIVE BLOOD SALVAGE AUTOTRANSFUSION | 22
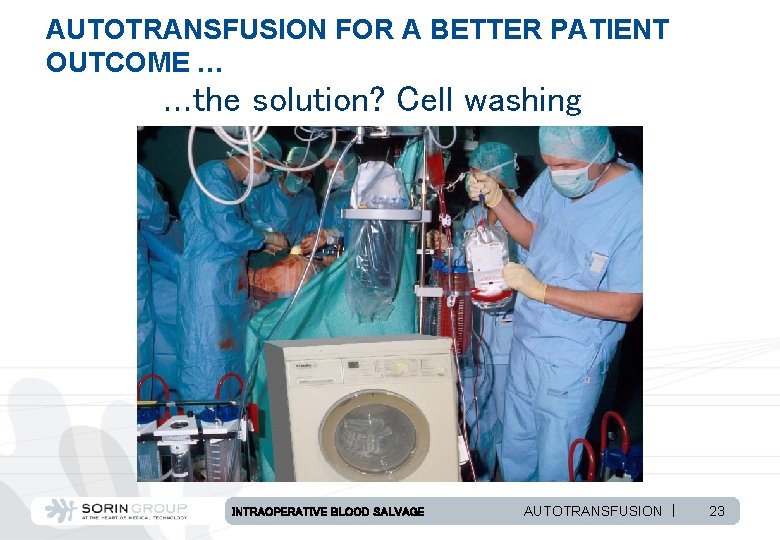
AUTOTRANSFUSION FOR A BETTER PATIENT OUTCOME … …the solution? Cell washing INTRAOPERATIVE BLOOD SALVAGE AUTOTRANSFUSION | 23

AUTOTRANSFUSION FOR A BETTER PATIENT OUTCOME … l Efficacy and cost-effectiveness of cell saving blood autotransfusion in adult lumbar fusion. C. Savvidou, S. N. Chatziioannou, A. Pilichou, S. G. Pneumaticos l summary. The objective of this study was to explore the use of cell saver blood autotransfusion in spinal surgery and to evaluate the efficacy and cost-effectiveness of cell saver blood autotransfusion during lumbar spine fusion in adults. Specific indications for the use of cell saver in adult lumbar fusion surgery have not yet been clearly determined. A total of 50 consecutive candidates for posterolateral fusion with internal fixation were prospectively randomized into either receiving perioperatively cell saving autotransfusion (Group A: 25 patients) or not (Group B: 25 patients). The use of cell saving technique did not exclude the use of allogenic blood transfusion. Surgical indications were spinal stenosis, spondylolisthesis, adolescent idiopathic scoliosis, degenerative scoliosis and fractures. Medical and financial data were recorded. A costanalysis was performed. Patients in Group A received 880 ± 216 m. L from cell saver and 175 ± 202 m. L allogenic blood. The patients in Group B received 908 ± 244 m. L allogenic blood. Blood volumes data collected were expressed in mean ± SD values. The cost of blood transfusion in Group A was 995 ±€ 447 per patient and 1220 ± 269 in Group B (P < 0. 05). In elective lumbar fusion blood requirements can be satisfied with 24 INTRAOPERATIVE BLOOD SALVAGE the use of autotransfusion. The use of cell saver appears to. AUTOTRANSFUSION be useful and cost-| effective during most elective lumbar fusions.

AUTOTRANSFUSION FOR A BETTER PATIENT OUTCOME … N. B. : For every 1 liter of Crystalloid given: Only 250 mls will stay Intravascular within 30 minutes, the rest of the 750 mls will cross extravascularly causing Organ Edema/Dysfx dropping the Viscosity and COP. It’s a lot easier to add volume than it is to take it off! INTRAOPERATIVE BLOOD SALVAGE AUTOTRANSFUSION | 25

AUTOTRANSFUSION FOR A BETTER PATIENT OUTCOME … l Platelet sequestration and autologous platelet gel Many of the newest autotransfusion machines are programmable to provide separation of blood into three groups; Red Cells, Platelet Poor Plasma, and Platelet Rich Plasma. Blood can be drawn from the patient just prior to surgery and then separated. The separated blood components which have been sequestered can be stored during the surgical procedure. The Red Cells and Platelet Poor Plasma can be given back to the patient through Intravenous transfusion during or after surgery. The Platelet Rich Plasma can be mixed with Calcium and Thrombin to create a product known as autologous platelet gel (APG). This is an Autologous product which can be used for a variety of techniques including use as a hemostatic aid, a dural sealant and an aid to fusion of bone. Its applications are being widely studied and reported in the literature on a regular basis recently. INTRAOPERATIVE BLOOD SALVAGE AUTOTRANSFUSION | 26

AUTOTRANSFUSION FOR A BETTER PATIENT OUTCOME … Most Importantly remember! “If its not yours its an Organ Transplant” with consequences, so try and do your best to avoid it! Your decisions effect the patient for the rest of their life! INTRAOPERATIVE BLOOD SALVAGE AUTOTRANSFUSION | 27
AUTOTRANSFUSION FOR A BETTER PATIENT OUTCOME … Thank you for your time! Questions? INTRAOPERATIVE BLOOD SALVAGE AUTOTRANSFUSION | 28
- Slides: 28