Atrial Fibrillation Dr Nidhi Bhargava 81013 Most Common

Atrial Fibrillation Dr Nidhi Bhargava 8/10/13

Most Common sustained clinical arrhythmia n Incidence rises with age- >5% over the age 65 -75 n

Risk factors for AF n n n n n Hypertension- accounts for 14% of AF in population Heart failure Male sex Diabetes Valvular MI LVH LVSD Left atrial dilatation Lone AF- with no structural or functional heart disease- 15%

Types of AF n Paroxysmal or recurrent (intermittent and self terminating) n n 35 -66% of all AF cases peak prevalence 50 -69 yrs At least a quarter may go progress to permanent AF Persistent (does not terminate spontaneously but may be effectively cardioverted) Permanent ( no longer reversible or reverses for brief interval only)
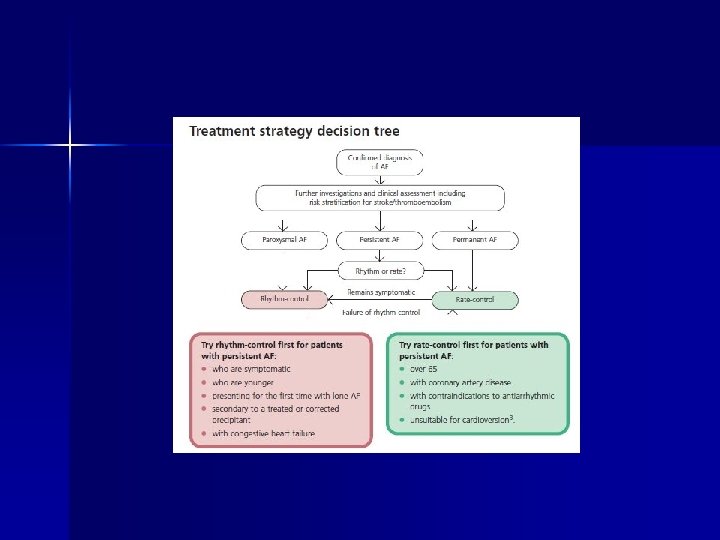

Effects of AF n Haemodynamic effects – Loss of atrial contraction and AV synchrony – Rapid ventricular rate – Irregular ventricular rate

Effects of AF n Symptoms – Palpitations – Breathlessness – Chest pain

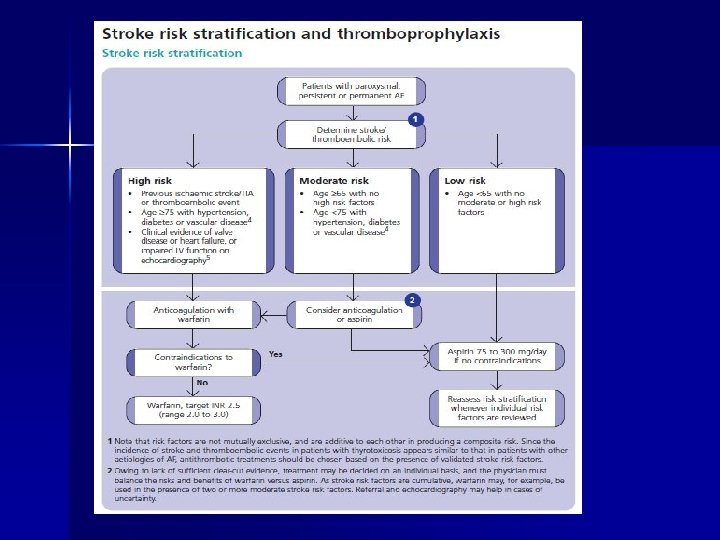
Effects of AF n Thromboembolism – Valvular AF -more so in pts. . with MS and AF (6% per year) – Non Valvular AF- 4 -5 times increased risk of stroke overall – Further increased risk if – Previous stroke or TIA (20 x increased risk) – Age >65, Hypertension and diabetes – CAD, LV dysfunction and Left atrial dilatation – <65 yrs. risk 1% per annum

Effects of AF Mortality- doubled in both sexes n Increased risk of stroke 4 -5 fold increase- further increase with age from 1. 5% in sixth decade to 23. 5% in the ninth decade n

Treatment n Restoration of sinus rhythm n Pharmacological cardioversion n Electrical cardioversion – External – Internal

Treatment n Maintenance of sinus rhythm n n Drugs DDD pacing Ablation of AF triggers Surgery for AF n Ventricular Rate Control n Anticoagulation

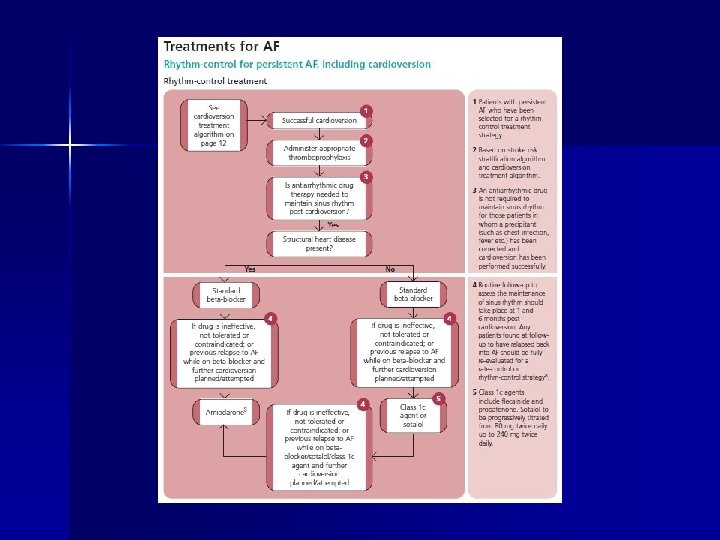
Treatment n Cardioversion (pharmacological and electrical) – Electrical cardioversion n External and Internal External- under GA, success rate 65 -90%, 200 -360 J Internal- under sedation- percutaneous electrode- success rate 90% – Pharmacological cardioversion – – n n Most effective if administered within 24 hrs. of onset Flecainide most effective- 72 -95% Others include amiodarone , sotalol, propafenone Less effective in chronic AF- Amiodarone most effective At least 4 weeks of full anticoagulation Anticoagulation to e maintained for 4 weeks after successful cardioversion

Treatment n Maintenance of Sinus rhythm – Drugs n n n Flecainde and Propafenone (Class 1 c) Sotalol better then propafenone Amiodarone – most effective but multiple side effects Beta blockers- no date available Digoxin- no effect – Pacing n n DDD pacing- reduce AF paroxysms Continuous atrial pacing-dual site or biatrial

Treatment n Focal Ablation n Targets AF initiating foci located in proximal pulmonary veins n Radiofrequency energy delivered n Used for pts. with paroxysmal AF n Pts. with chronic AF but can be successfully cardioverted at least for few seconds n Under LA n Success rate 70% in PAF and 50% in chronic AF

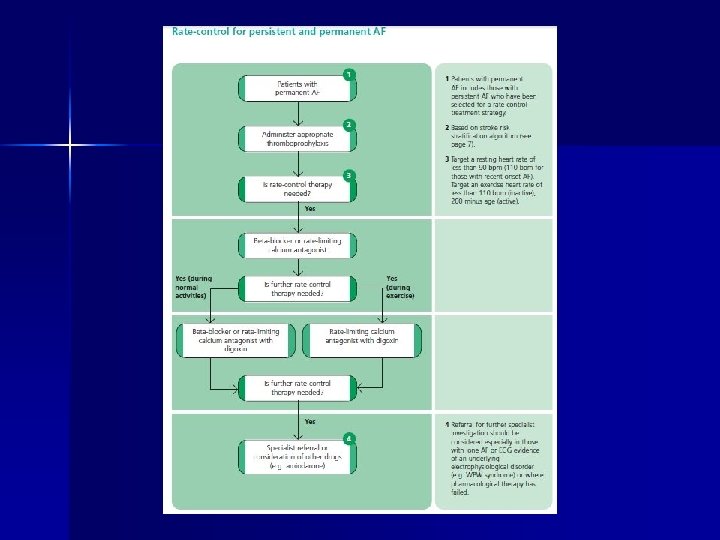
Treatment n Surgery for AF-Maze operation n Ventricular rate control n AV node ablation n Drugs n n Digoxin- not negative inotropic but less effective Diltiazem, verapamil and beta blockers- more effective but negatively inotropic
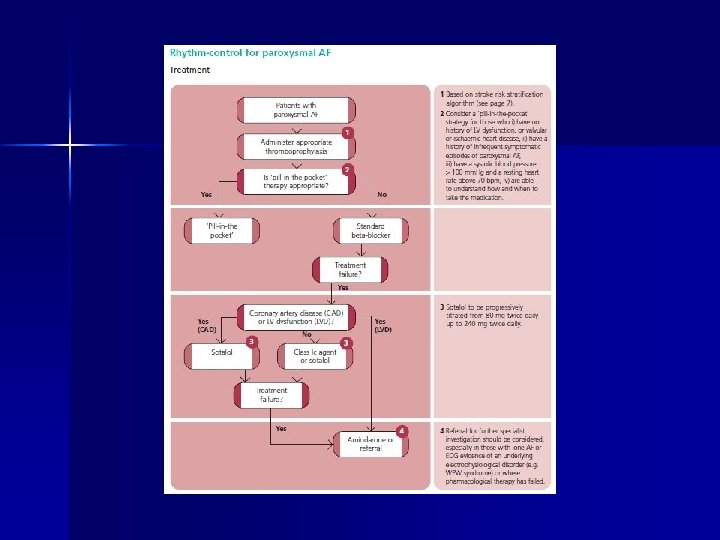
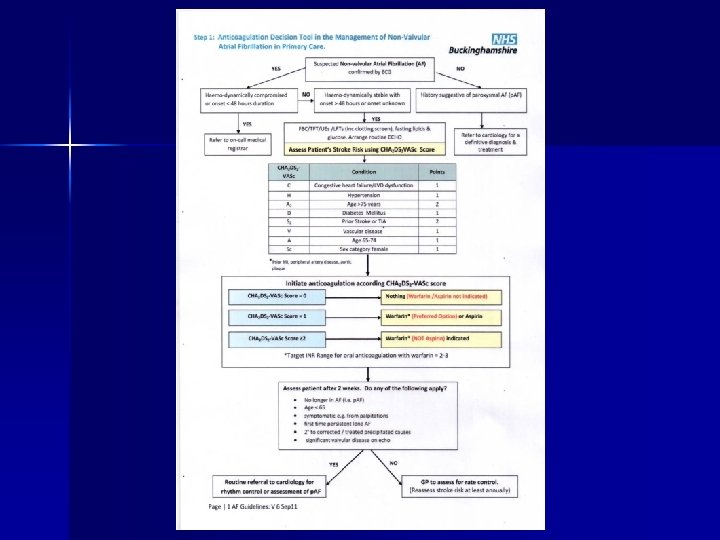
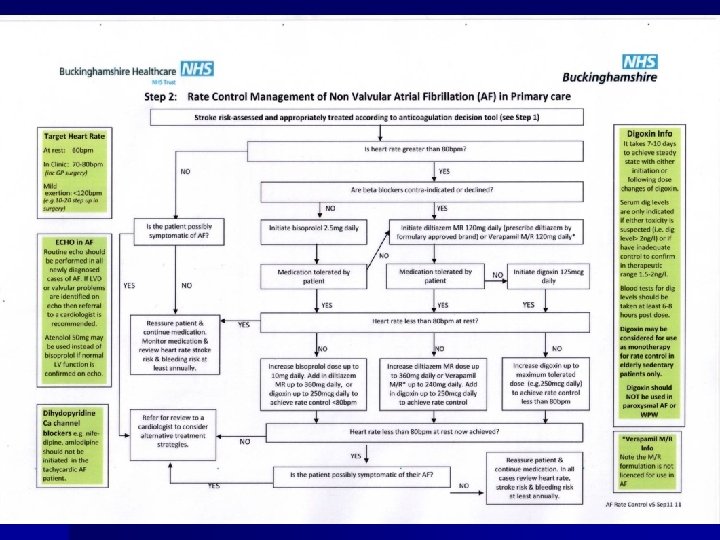

Case histories n A 67 years old female with no risk factors presents with palpitations n A 77 years old male with no risk factors is found to be in AF on routine examination n A 98 years old male with AF on warfarin presents with haematuria and subsequently diagnosed with Ca bladder n A 79 year old female with AF rate 120 -140/min, on warfarin and digoxin, asthmatic and has severe reaction to verapamil-treatment options n A 64 years old diabetic is in AF on routine examination
- Slides: 22