Atrial fibrillation and flutter Practical Management Tips Internal

Atrial fibrillation and flutter: Practical Management Tips Internal Medicine Residency Program Noon Conference 2011

Learning Goals n. A brief discussion of supraventricular tachycardia (SVT) n Review of AF and AFl physiology and EKG differentiation n Management of atrial fibrillation (AF) n Management of atrial flutter (AFl)

Management of fib/flutter n Anticoagulation n Cardioversion n Rate control n Rhythm control n Ablation n Cardiothoracic surgery

But, first, a brief diversion n Definition of supraventricular tachycardia (SVT) n Differentiating among types of SVT n Differentiating AF from AFl

Supraventricular tachycardia n n n Abbreviated SVT “Supra” means “above” Supraventricular tachycardia comes from above the ventricles DO NOT CONFUSE with NSVT (non-sustained ventricular tachycardia) (Essentially) all narrow-complex tachycardia has a supraventricular origin

SVT possible sites of origin Sinus node n Atria n Atrioventricular node n His bundle n n Or some combination of the above

Supraventricular tachycardia n n n n Sinus tachycardia Multifocal atrial tachcyardia Paroxysmal atrial tachycardia AV nodal reentrant tachycardia (AVNRT) Atrioventricular reentrant tachycardia (AVRT) Atrial fibrillation Atrial flutter

Rare types of SVT Inappropriate sinus tachycardia (previously called SNRT or SANRT) n Junctional ectopic tachycardia (JET) and paroxysmal junctional reciprocating tachycardia (PJRT) -- mostly seen in infants and children n Nonparoxysmal junctional tachycardia (NPJT) -- seen in acute right coronary artery occlusion and digitalis toxicity n

Supraventricular tachycardia A nonspecific term that technically refers to seven separate diagnoses n When clinicians use the term “SVT, ” they mean that it is a narrow-complex tachycardia, and they cannot specify which one n Do not use the term “SVT” if you have an actual diagnosis n Do use “SVT” when the patient has “supraventricular tachycardia, not otherwise specified” n
Supraventricular tachycardia n n n n Sinus tachycardia Multifocal atrial tachcyardia Paroxysmal atrial tachycardia AV nodal reentrant tachycardia (AVNRT) AV reentrant tachycardia (AVRT) Atrial fibrillation Atrial flutter

When in doubt, use a vagal maneuver Adenosine 6 mg IV push -We don’t use enough adenosine! -But must be done with proper monitoring n Valsalva maneuver -Safe; usually ineffective n Carotid sinus massage -In properly selected populations, complications are rare n

Carotid Sinus Massage Contraindications n Carotid bruit n Prior stroke or transient ischemic attack, unless imaging has shown no significant carotid disease n Myocardial infarction in the previous six months n History of serious cardiac arrhythmias (VT, VF)

Vagal maneuvers Diagnostic -Usually you can learn which SVT it was by doing a vagal maneuver n Therapeutic -Vagal maneuvers can terminate AVRT and AVNRT n

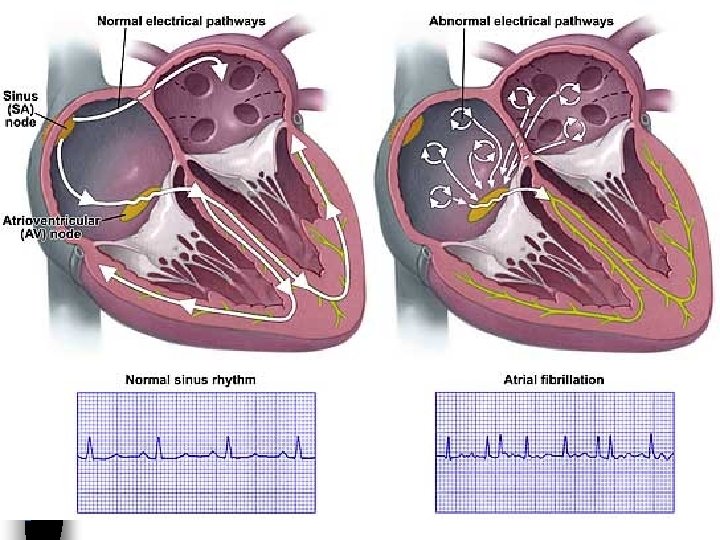
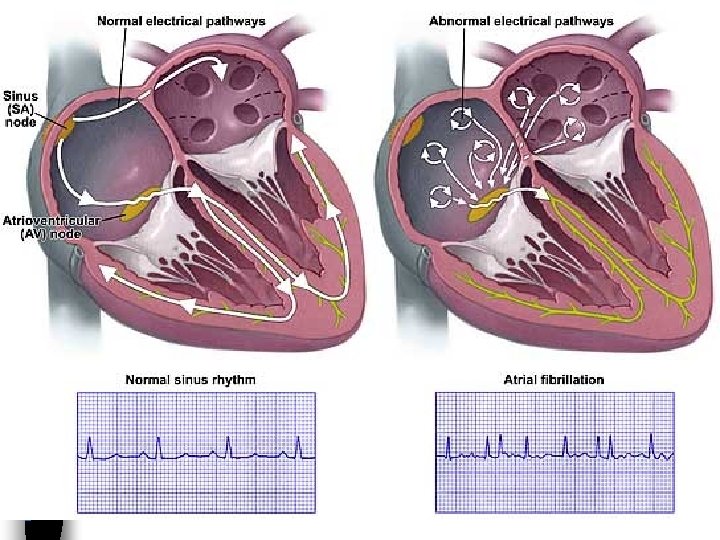
Differentiating AF from AFl n AFl is a macroreentrant atrial rhythm with a reentry circuit that involves a large area of atrial myocardium n AF is caused by multiple wandering wavelets, a hodgepodge of microreentrant circuits, often located in the pulmonary veins
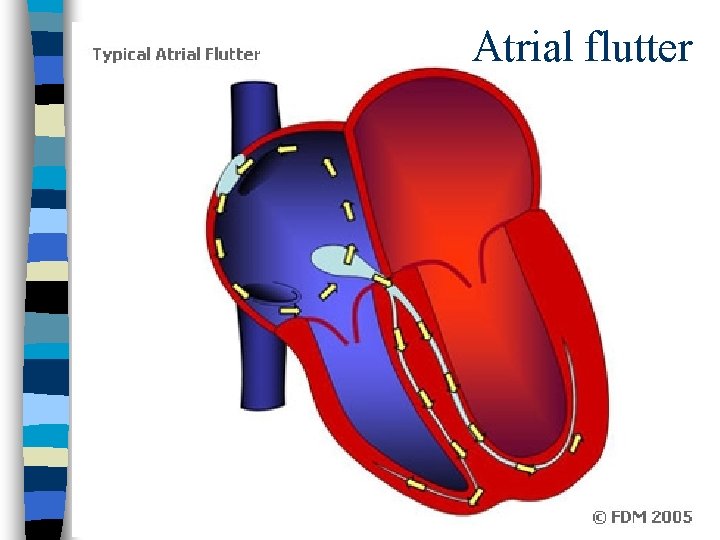
Atrial flutter

Atrial flutter n. P waves exhibit a “sawtooth” pattern referred to as flutter waves or “F” waves n Atrial rate is typically 250 -350 beats per minute (bpm)

Atrial flutter, continued n Classically, atrial rate is 300 bpm with 2: 1 AV conduction, leading to a heart rate of 150 bpm n But focus on the atrial pattern when diagnosing SVT--try to ignore the QRS complexes, just looking at the P (or F) waves at first

Atrial flutter (with 4: 1 response)
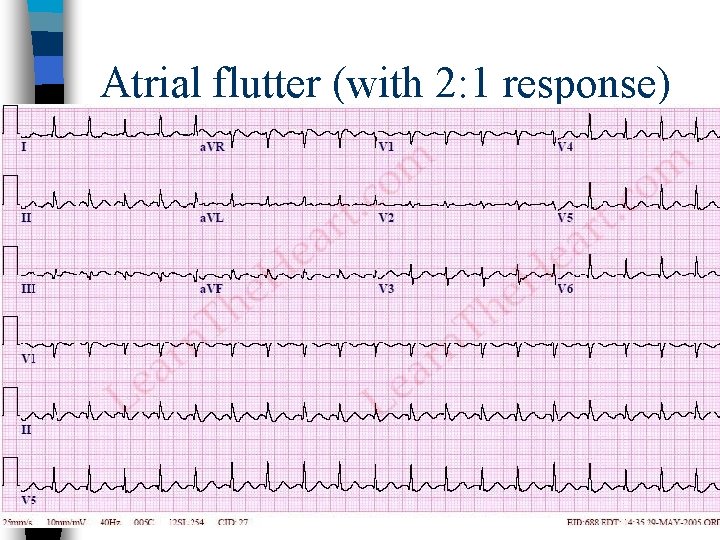
Atrial flutter (with 2: 1 response)

Atrial flutter (variable response)
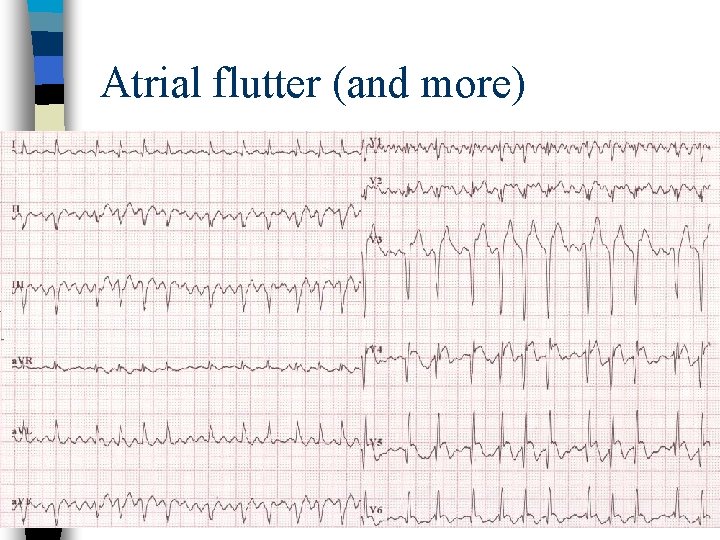
Atrial flutter (and more)


Atrial fibrillation n Rapid and irregular atrial activity at a rate of 350 -600 impulses per minute n Usually irregular ventricular response n There are no P waves n Sometimes the F waves are so fine, the surface EKG cannot detect them
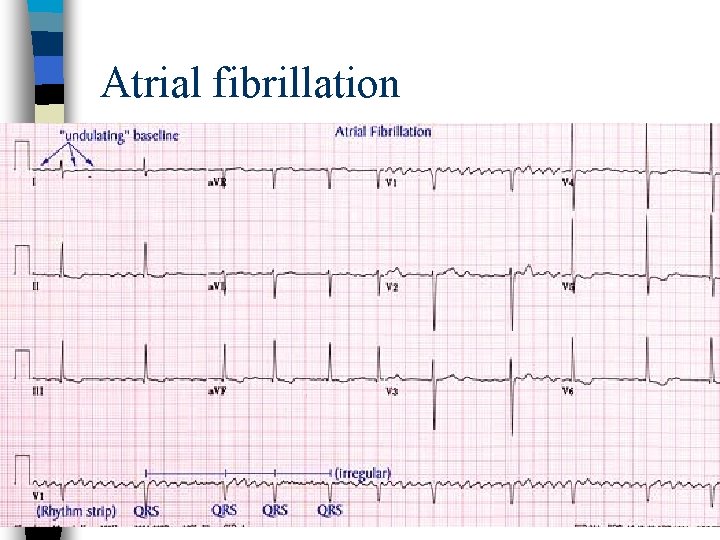
Atrial fibrillation

Atrial fibrillation

Atrial fibrillation terms n Paroxysmal n Persistent n Permanent n “Lone”

Atrial fibrillation terms, cont. n Paroxysmal -episodes terminate spontaneously in less than seven days n Persistent -fails to terminate within seven days

Atrial fibrillation terms, cont. n Permanent -AF lasts for more than one year, and -Cardioversion has not been attempted or has failed n “Lone” -patients less than 60 years of age without structural heart disease

Atrial fibrillation terms, cont. n This classification applies only when no clear reversible cause of AF. n If AF is clearly due to heart surgery, pericarditis, myocardial infarction, hyperthyroidism, pulmonary embolism, or other reversible causes, avoid this classification system

Management of fib/flutter n Anticoagulation n Cardioversion n Rate control n Rhythm control n Ablation n Cardiothoracic surgery

Anticoagulation (AC) n Recommendations are essentially the same for AF and AFl n First, assess if the patient is high risk for cardioembolic stroke n Most patients with high risk should be on AC if they ever were seen in AF or AFl

High risk for cardioembolic stroke n Rheumatic mitral stenosis -Mitral valve area less than 2. 0 cm 2 n Prosthetic heart valves n Hyperthyroid (? ) -2006 ACC/AHA/ESC guidelines recommend INR 2 -3 in all patients until euthyroid; ACCP does not comment on this

CHADS 2 score n For use in patients without the high risk factors on the previous slide n There are other risk models, including the CHADS 2 -VASc score

CHADS 2 score
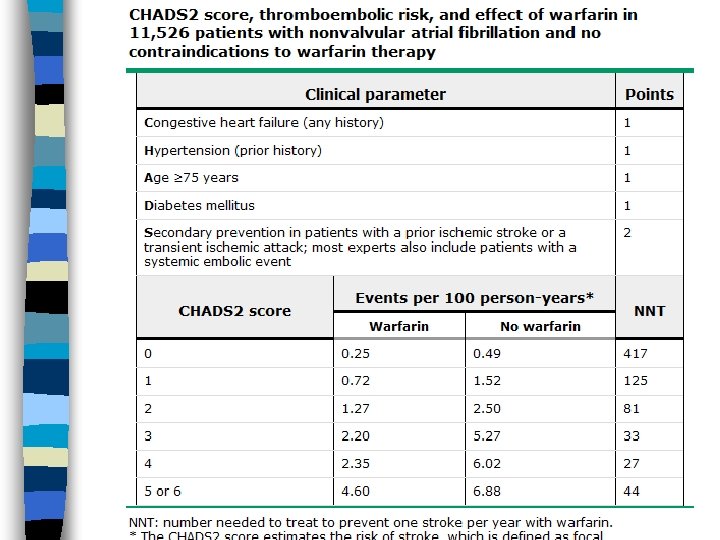
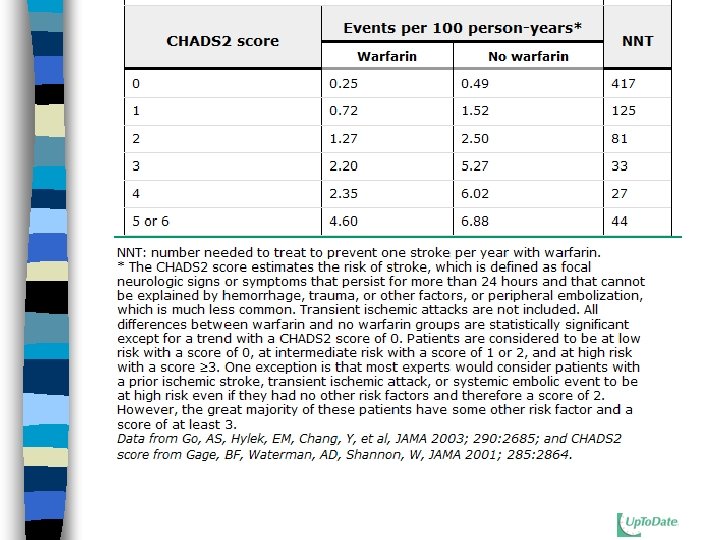

When can you stop AC? n If AF was due to a completely reversed reversible cause, maybe you can stop n For AFl, you can never stop n After ablation you still can’t stop n If you had HF, and your EF returns to normal, you still can’t stop n Paroxysmal has same risk as others

When to stop AC n Pretty much you have to develop a contraindication to anticoagulation before you stop it n Fall risk is a relative contraindication; it’s rare that someone is falling so frequently that it rises to the level of contraindication

When to stop AC n Really, paroxysmal AF has same stroke risk as other AF n Caution when diagnosing AF! If you misdiagnosed NSR with PAC’s or multifocal atrial tachycardia as AF, you can doom someone to lifelong AC

When to bridge with heparin n If patient has any evidence of hypercoagulable state n If patient has prosthetic heart valves n Otherwise, risk of intracranial bleeding and HIT outweighs benefit of reduced stroke risk and warfarin skin necrosis


Risk of stroke per day off AC n Less than 4 events per 100 personyears prevented n One day is 4/100/365=0. 0011% per day stroke risk reduction Efficacy and safety of anticoagulant treatment in acute cardioembolic stroke: a meta-analysis of randomized controlled trials. Paciaroni M, Agnelli G, Micheli S, Caso VS. Stroke. 2007; 38(2): 423.
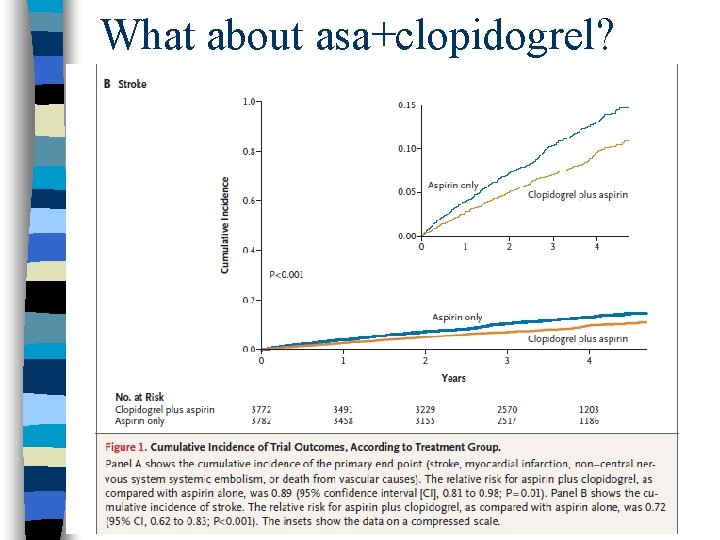
What about asa+clopidogrel?
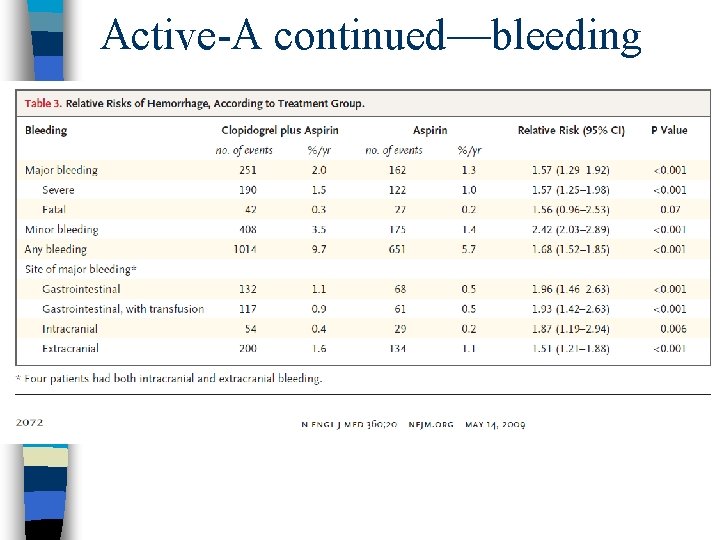
Active-A continued—bleeding

Take-home point n Warfarin>ASA+clopidogrel>ASA n This applies to stroke prevention n And to bleeding risk n Every AF patient who is off warfarin should be on aspirin unless there is a contraindication to ASA therapy

Clopidogrel + Warfarin = Bleed n ASA+warfarin and ASA+clopidogrel are relatively safe in most situations where both are indicated n Warfarin+clopidogrel has a relative risk of bleeding >3 times greater than warfarin alone n ASA+warfarin+clopidogrel has less rigorous data; evidence suggests >5 times greater than asa+clopidogrel alone

Dabigatran and Apixaban n Oral anticoagulant medications that do not require monitoring n Dabigatran approved for AC in AF/AFl in USA; NYS Medicaid and NBHN do not pay for it. Medicare part D does pay n Apixaban likely similar; not yet approved

You’re the night intern n 78 W with HTN, DM, COPD, and history of paroxysmal AF n Nurse pages you to say that HR is now 172 beats per minute after albuterol n You ask, “what’s the blood pressure? ” n The nurse says she will check. You go to the bedside.

You’re the night intern n HR=172 irregular, BP is 72/48 n Pt. is pale, diaphoretic, lethargic but responds to questions n You confirm with EKG that the rhythm is atrial fibrillation n Put patient in Trendelenberg position to optimize cerebral perfusion, then you…

Single best answer: Next step n A) DC cardioversion without sedation n B) Ativan 2 mg IV over 30 seconds, then direct current (DC) cardioversion n C) Amiodarone 150 mg IV over 15 min. n D) Diltiazem 10 mg IV over 2 minutes n E) Adenosine 6 mg IV push

Single best answer: Next step n A) DC cardioversion without sedation n B) Ativan 2 mg IV over 30 seconds, then direct current (DC) cardioversion n C) Amiodarone 150 mg IV over 15 min. n D) Diltiazem 10 mg IV over 2 minutes n E) Adenosine 6 mg IV push

Management of fib/flutter n Anticoagulation n Cardioversion n Rate control n Rhythm control n Ablation n Cardiothoracic surgery

Indications for cardioversion n Hemodynamically unstable patient with any (non-sinus) tachycardia with RVR n Cardiovert first; page cardiology second n When people are awake, sedate before cardioversion n (You learned this in ACLS)

Cardioversion when hemodynamically stable n Has never been shown to improve prognosis or reduce embolic risk, despite rigorous evaluation of this question in AFFIRM and RACE n Still, “every patient deserves a trial of sinus rhythm”
Cardioversion when hemodynamically stable n AFl is hard to rate control and easy to cardiovert n Heart failure (HF) may improve with restoration of atrial “kick” from cardioversion n Particularly important in severe diastolic HF, also beneficial in systolic HF

Cardioversion complication: Cardioembolism n Mostly in patients who are not anticogulated at time of cardioversion n Reduce risk by anticoagulating beforehand for 3 -4 weeks n If not on A/C for ~4 weeks prior, do TEE -If no thrombus on transesophageal echocardiogram, give heparin bolus, then cardiovert

Cardioversion complication: Cardioembolism n Continue anticoagulation for at least 4 weeks after cardioversion n If stroke risk is low enough, change from warfarin to ASA (+/- clopidogrel) n What if someone in paroxysmal AF selfcardioverts in front of you? Do they need 4 weeks of warfarin? If they selfcardiovert at home, will anyone know?

Cardioversion complications n ST-T changes, CK, troponin n Myocardial stunning n Transient hypotension n Pulmonary edema n Skin burns/Self-injury n Ventricular fibrillation (not if SYNC on) -Much more common in digitalis toxicity

DC Cardioversion, fine points n Usually should be done with one pad on front and one on patient’s back n Optimal current level to use in first shock is not known; lower in AFl n Biphasic is more successful than monophasic in terminating arrhythmias n Turn on the SYNC function

DC Cardioversion, fine points n If first attempt fails, try increasing the current to 200 joules n Then try changing the pad position n Then try pretreatment with antiarrhythmic drugs -might require long-term drug treatment n Still, about 1/3 of DC cardioversion efforts will fail

Chemical cardioversion n Usually with ibutilide n Restricted to Cardiology use n Lower cardioversion success rate than electrical, but more comfortable (no sedation needed) n Caution in long QT n Amiodarone IV is not cardioversion

Cardioversion take-home n When hemodynamically unstable, cardiovert immediately (with sedation if awake patient) n Consider doing with AC and TEE in other scenarios, especially newly diagnosed AF/AFl, AFl difficult to rate control, and HF—needs cardiology supervision

Management of fib/flutter n Anticoagulation n Cardioversion n Rate control n Rhythm control n Ablation n Cardiothoracic surgery

Rate control n Keep the patient in the arrhythmia n Simply slows down the rate n Beta blockers (β-B) n Calcium Channel Blockers (CCB) n Digoxin n Must continue anticoagulation

Rhythm control n Goal is to keep patient in sinus rhythm n First anticoagulate n Then load rhythm control medication n Then cardiovert (possibly with TEE) n Monitor for antiarrhythmic side effects n Can you stop AC in rhythm control?

Rhythm control: choice of agent n Amiodarone and dronedarone -Side effects and safety monitoring are an entire Up-to-Date article n Sotalol and dofetilide -Less side effect burden but less effective in maintaining sinus rhythm, requires hospitalization for QT monitoring during initiation, CKD is contraindication, needs cardiology approval at JMC

AFFIRM trial n Compared morbidity and mortality in patients randomly assigned to rate or rhythm control strategy n In the rhythm control strategy, patients were allowed to stop A/C if serial Holter studies showed no AF Wyse DG, Waldo AL, Di. Marco JP, Domanski MJ, Rosenberg Y, Schron EB, Kellen JC, Greene HL, Mickel MC, Dalquist JE, Corley SD. A comparison of rate control and rhythm control in patients with atrial fibrillation. N Engl J Med. 2002 Dec 5; 347(23): 1825 -33.

AFFIRM, continued n The question was: Which is better, rate control or rhythm control? n The answer was: Anticoagulation. n In both treatment arms, anyone with a subtherapeutic INR for any reason had higher stroke risk n Serial Holter did not predict stroke risk n Rhythm control had more side effects

Management of fib/flutter n Anticoagulation n Cardioversion n Rate control n Rhythm control n Ablation n Cardiothoracic surgery

Atrial flutter ablation n Takes about 30 minutes n Success rate >80% n Technically straightforward n Main complication is AF after n Should probably be offered to anyone who ever had AFl and has a good prognosis, unless they also had AF

Atrial flutter

Atrial fibrillation ablation n Also called pulmonary vein isolation n Can last more than six hours n Requires atrial septal puncture and heparinization

Atrial fibrillation ablation n Main post-procedural complication is a special type of atrial tachycardia n No evidence that it’s safe to stop anticoagulation afterward n Often requires repeat ablation procedure to maintain sinus rhythm

Ablate and pace n Insert a biventricular pacemaker n Ablate the AV node (on purpose) n Very high procedural success rate n But leaves the patient lifelong pacemaker dependent n Most useful in heart failure, particularly tachycardia-induced cardiomyopathy n Also in pacemaker-dependent patients

Management of fib/flutter n Anticoagulation n Cardioversion n Rate control n Rhythm control n Ablation n Cardiothoracic surgery

Surgical options n MAZE procedure -Routinely done during mitral valve surgeries; often done other times n LA appendage ligation n Percutaneous left atrial appendage occlusion (PLAATO) and others
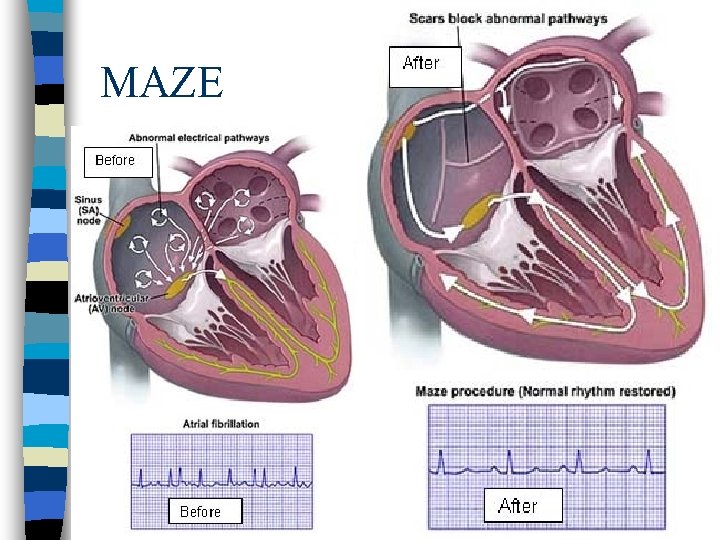
MAZE

PLAATO

PLAATO n Very cool; effectiveness studies of this and competing devices are underway

Learning Goals n. A brief discussion of supraventricular tachycardia (SVT) n Review of AF and AFl physiology and EKG differentiation n Management of atrial fibrillation (AF) n Management of atrial flutter (AFl)

Conclusion n n Anticoagulation, when indicated, is the most important treatment in most patients with AF/AFl; mostly warfarin/dabigatran Stronger AC has less stroke but more bleed Cardiovert your hemodynamically unstable patients right away Rate control for most patients Call cardiology for cardioversion, rhythm control, ablation, or surgery if appropriate
Thank you n Insert humorous cartoon or scenic image on this slide
- Slides: 84