ATLANTOAXIAL INSTABILITY Atlantoaxial Joint AtlantoAxial Joint Atlantoaxial Instability

ATLANTOAXIAL INSTABILITY
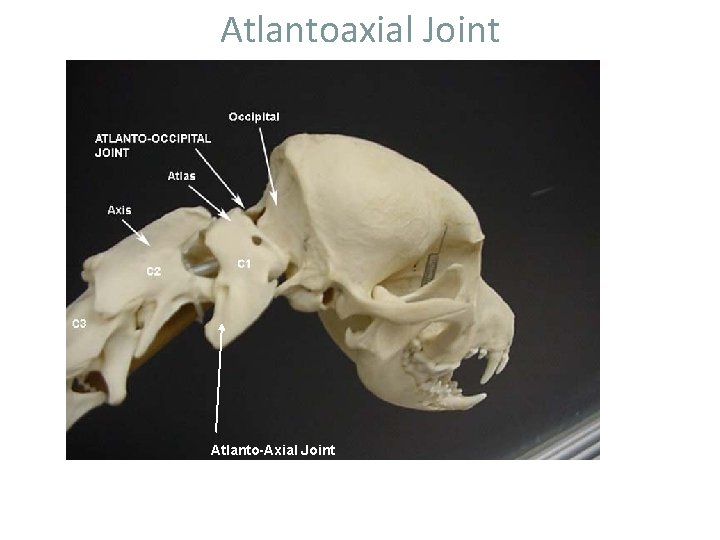
Atlantoaxial Joint Atlanto-Axial Joint

Atlantoaxial Instability (Subluxation) Signs • – – – Toy and miniature breeds Reluctance to be patted on head Neck pain May have tetraparesis (weakness in all 4 limbs) or tetraplegia (paralysis in all 4 legs) Sudden death due to respiratory paralysis Diagnosis— • – Radiographs: lateral x-ray of neck in slight ventroflexion • avoid further spinal cord damage with positioning
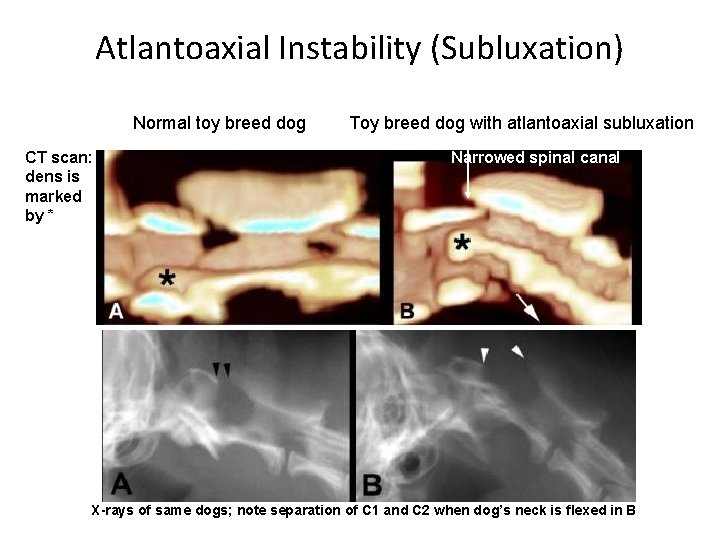
Atlantoaxial Instability (Subluxation) Normal toy breed dog CT scan: dens is marked by * Toy breed dog with atlantoaxial subluxation Narrowed spinal canal X-rays of same dogs; note separation of C 1 and C 2 when dog’s neck is flexed in B

Atlantoaxial Instability (Subluxation) • • Treatment— Medical • splint neck in extension with cage confinement x 6 w • treat like other spinal cord trauma – Surgical (if unresponsive to medical Rx) • stabilize/decompress • attach dorsal process of axis to arch of atlas • fuse atlas and axis joint with pins and bone graft • hemilaminectomy to relieve spinal cord compression – – – Client info— prognosis is fair to good for animals with mild signs animals should not be used for breeding; may be hereditary
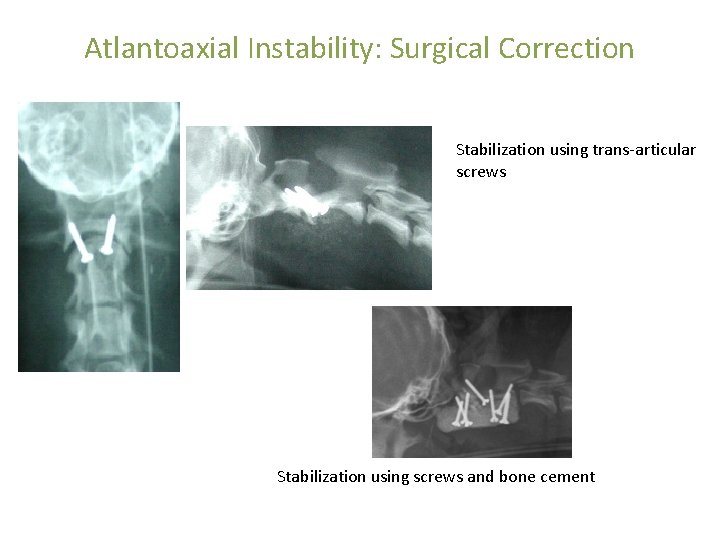
Atlantoaxial Instability: Surgical Correction Stabilization using trans-articular screws Stabilization using screws and bone cement

Cervical Spondylomyelopathy: Wobbler Cervical spinal cord compression as a result of caudal vertebral malformation or misarticulation. • – – – – – Large breed dogs (Great danes and Dobermans) Signs Progressive hind-limb ataxia (wobbly gait) Pelvic limbs cross each other when walking Abduct widely/tend to collapse May drag toes (wears dorsal surface of nails) Impaired proprioception Signs may also be present in front limb Crouching stance with downward flexed neck Rigid flexion of neck; may have neck pain

Cervical Spondylomyelopathy: Wobbler Dx • – – – Radiographs to show malalignment and narrowing of spinal canal Myelogram is essential to locate the region of compression CT and MRI if available

Cervical Spondylomyelopathy: Wobbler Rx—without treatment, prognosis is poor • Medical – • • • Anti-inflammatory doses of corticosteroids Neck brace Cage confinement Surgical – • • Decompression of spinal cord by laminectomy Stabilize vertebral column – – screws and wire dorsally spinal fusion ventrally

Cervical Spondylomyelopathy: Wobbler Client info • – – Prognosis is guarded Most likely a hereditary disease Multiple levels of compression less favorable prognosis than a single area of compression Surgery is risky and costly

Degenerative Myelopathy Etiology—unclear • – – May be autoimmune response to antigen in nerv sys Degeneration of white matter in ascending and descending tracts Signs • – – – Mainly in G Shep and Shep mixes (>5 yr) Progressive ataxia and paresis of hind limbs Loss of proprioception is first sign Dog “falls down” when trying to defecate Muscle wasting of back muscles along caudal thoracic and lumbosacral areas Symptoms progress until animal is unable to support weight on hind limbs

Degenerative Myelopathy Dx— • Neurologic Exam – ↓ proprioception ↑ patellar reflexes Lack of pain Normal sphincter tone; normal panniculus (pin prick) reflex • Radiographs usually normal Rx—none; symptoms will progress to paralysis Client info— • • • – – – Degenerative myelopathy is a progressive, incurable disease Although symptoms are similar at early stages, it is a different disease from hip dysplasia When dog cannot support weight, quality of life should be evaluated
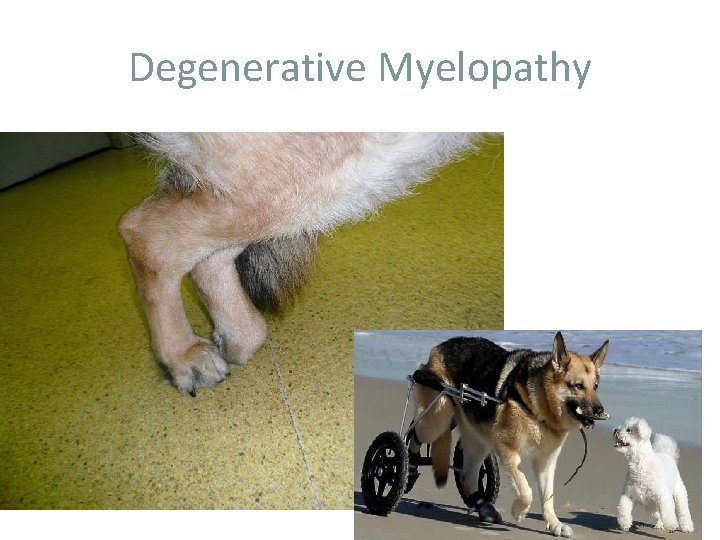
Degenerative Myelopathy

Deafness: Causes • – – – • • – – – – • damage to auditory pathway chronic otitis rupture of tympanic membrane damage to middle ear (ossicles) damage to auditory nerve hereditary or congenital bull terriers, Dobes, Rotts, Pointers, blue-eyed white cats, Dalmations, Aust Heelers, Aust shepherds, Eng setters, Catahoula related to drug therapy aminoglycosides (gentamicin, streptomycin, kanamycin topical polymyxin B Chloramphenicol Chlorhexidine w/ centrimide normal old age—usually due to atrophy of nerve ganglia or cochlear hair cells

Deafness Dx • – Inability to rouse sleeping animal with loud noise (e, g, . blast from air horn) is diagnostic Rx: No treatment is available in most cases • – Hearing aids are available for animals, but most will not tolerate something in ear canal Client info • – – – Hearing loss is permanent If hereditary, do not breed Animals can be taught to hand signals rather than words Animals should not be off leash when outside Hearing aids are available for dogs but are usually not tolerated; would only be appropriate for hearing impaired

Laryngeal Paralysis • 3 types (always be cautious of laryngeal paralysis because of the chance of rabies) Hereditary: seen in Bouvier des Flandres and Siberian Huskies • Seen at 4 -6 mo of age – Acquired: can occur from lead poisoning, rabies, trauma, inflammation of vagus nerve • 1. 5 to 13 yr of age – Idiopathic: seen in middle-age to old large- and giantbreed dogs; castrated dogs and cats have a higher incidence than female and non-neutered males –

Laryngeal Paralysis Signs: • – – – Dx: laryngoscopy will show laryngeal abductor m. dysfunction Rx: surgical intervention including: • • – – • Inspiratory stridor Resp distress Loss of endurance Voice change Dyspnea/cyanosis/complete resp collapse Arytenoidectomy Removal of vocal folds Client info: prognosis is guarded to good; do not breed if hereditary
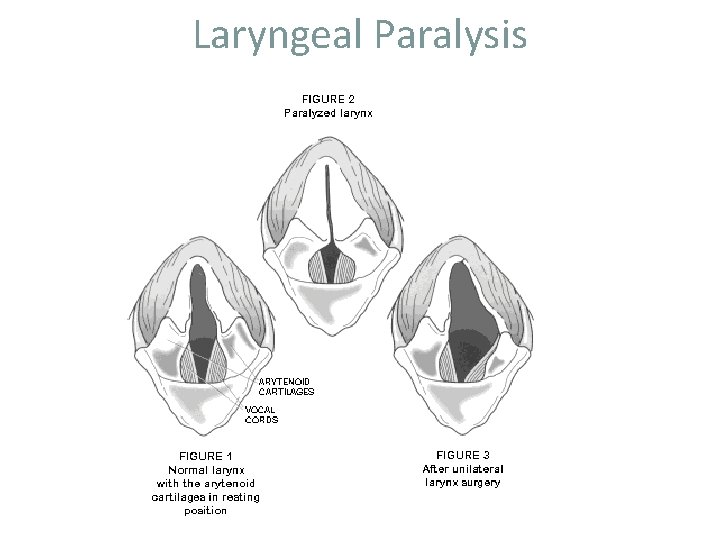
Laryngeal Paralysis

Megaesophagus • – Causes-lack of esophageal peristalsis (3 types): – • • – • – – – Hereditary—a gene for the disease is identified in wire-haired fox terriers and min schnauzers Congenital—Great Danes, German Shepherd, Irish Setters, Newfies, Sharpeis, Greyhounds (no gene ID’ed) evident about weaning time when solid food is introduced Due to incomplete nerve development in esophagus Acquired—may be seen at any age; Pb tox; may be associated with neuropathies (e. g. , myasthenia gravis, tick paralysis) Signs Regurgitation of undigested food Respiratory problems (aspiration pneumonia) Lack of growth
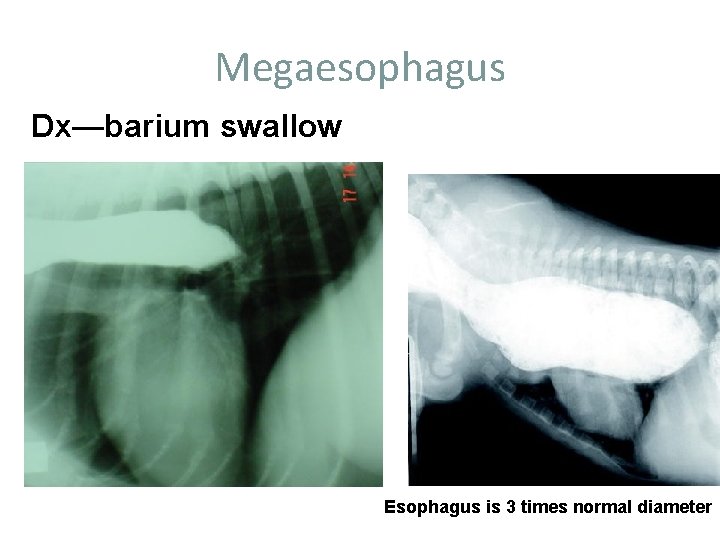
Megaesophagus Dx—barium swallow Esophagus is 3 times normal diameter

Megaesophagus • Rx – – • Elevated feeding (on platform, stairs) Liquid or soft diet high in calories Give several small feedings daily Gastrostomy tube (long term) is an option Client info – – – Prognosis—guarded to poor Treatment aim is to reduce clinical signs and prevent aspiration pneumonia There is no cure

Tick Paralysis • – – • – Cause—female tick (Dermacenter variablis, D. andersoni) → salivary neurotoxin Neurotoxin interfered with Ach at neuromuscular jct Not seen in cats; humans are affected Signs— – – • – Rx Gradual onset of voice changes and hind-limb ataxia (motor deficit) progressing to a flaccid, ascending paralysis (1 -3 d) Sensation is intact Ticks on the dog Remove ticks (manually or with dip) • – Usually resolves in 1 -3 d Supportive care until dog recovers • Ventilation required for resp paralysis
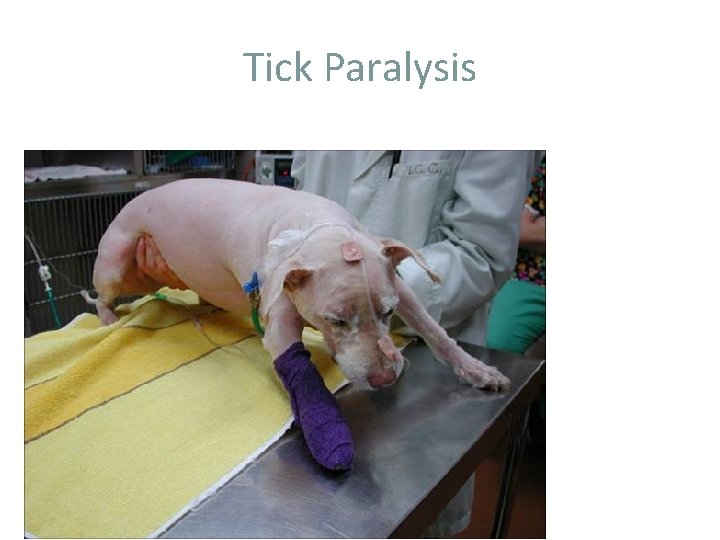
Tick Paralysis

Coonhound Paralysis (Polyradiculoneuritis ) -thought to be an immune response to an unknown etiologic factor in raccoon saliva -some dogs will get it 1 -2 wk after exposure, others exposed to same raccoon will not • – – – • • – – – Signs: similar to tick paralysis and rabies Weakness begins in hind limbs with paralysis progressing rapidly to a flaccid tetraplegia Alert, afebrile animal Loss of spinal reflexes (patella tap, etc) Loss of voice; labored breathing; inability to lift head May die of respiratory failure May last for 2 -3 mo (usually good Px) Rx: supportive nursing care Client info Dogs can be affected without exposure to raccoon May require long-term nursing care Some animals will regain total function, while more severely affected animals may not
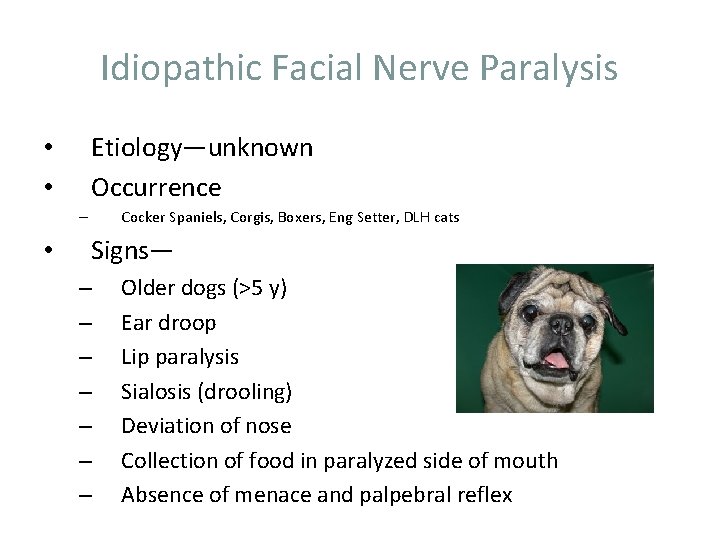
Idiopathic Facial Nerve Paralysis Etiology—unknown Occurrence • • Cocker Spaniels, Corgis, Boxers, Eng Setter, DLH cats – • Signs— – – – – Older dogs (>5 y) Ear droop Lip paralysis Sialosis (drooling) Deviation of nose Collection of food in paralyzed side of mouth Absence of menace and palpebral reflex

Idiopathic Facial Nerve Paralysis • Rx—efficacy of corticosteroids unknown – Artificial tears to prevent corneal ulcers – Keep oral cavity clear of food • Client info— – – Cause is unknown Complete recovery does not usually occur May develop keratoconjunctivitis sicca (dry eye) Animals may require life-long maintenance
- Slides: 26