Atherosclerosis and Stable Ischemic Heart Disease Martin Horvth

Atherosclerosis and Stable Ischemic Heart Disease Martin Horváth Department of Cardiology, Charles University in Prague, 2 nd Faculty of Medicine and Motol University Hospital

Overview Atherosclerosis – – Pathogenesis Epidemiology Clinical presentation Risk-factors Stable ischemic heart disease – Clinical presentation – Diagnostics – Treatment options
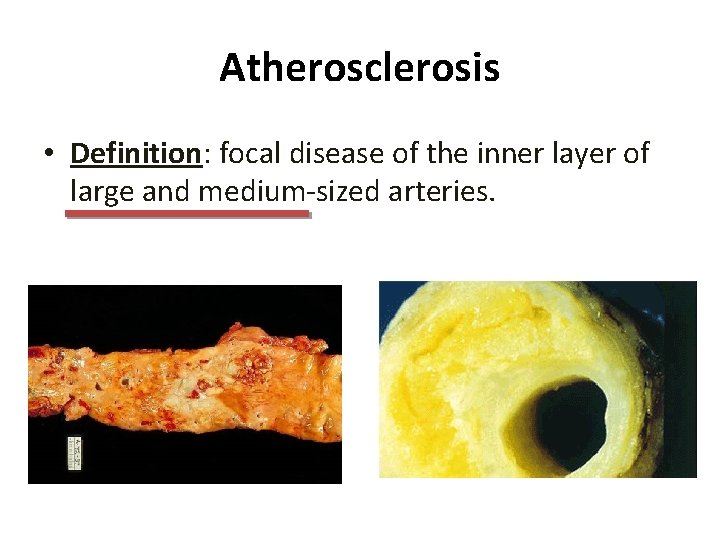
Atherosclerosis • Definition: focal disease of the inner layer of large and medium-sized arteries.

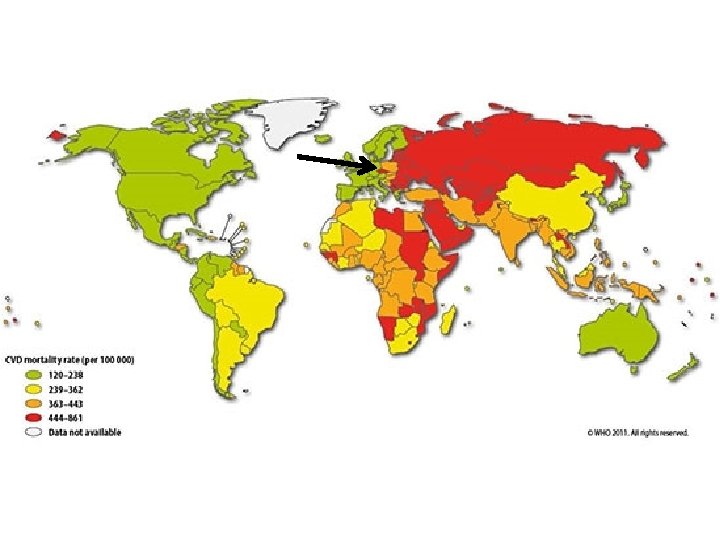
Why is it important? Epidemiology • Single most common “killer” – In 2008 17, 3 million deaths (7, 3 MI, 6, 2 stroke) • About ½ of deaths in developed countries • Involves many vascular beds and thus causes various diseases
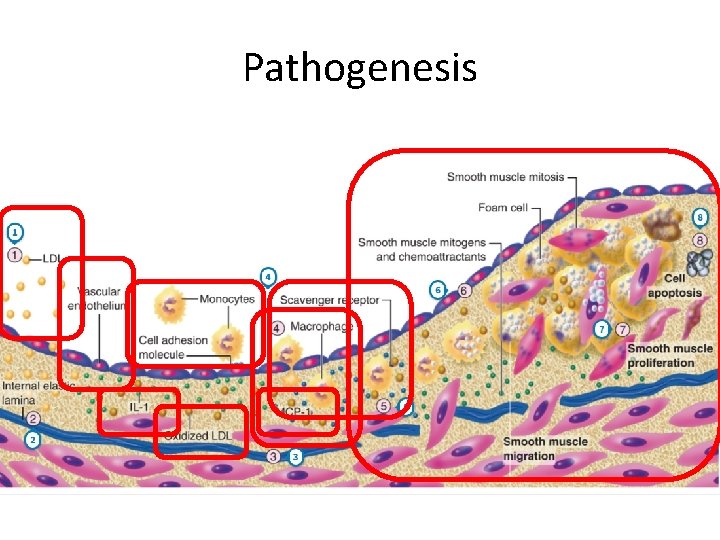
Pathogenesis
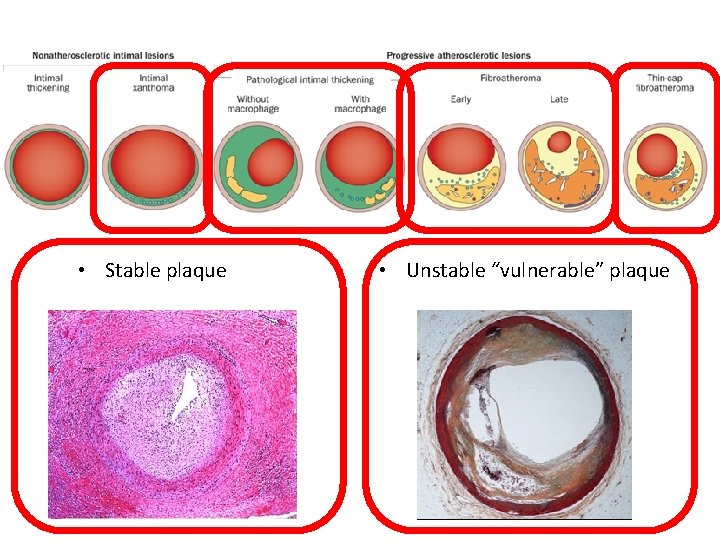
• Stable plaque • Unstable “vulnerable” plaque

Clinical presentation?
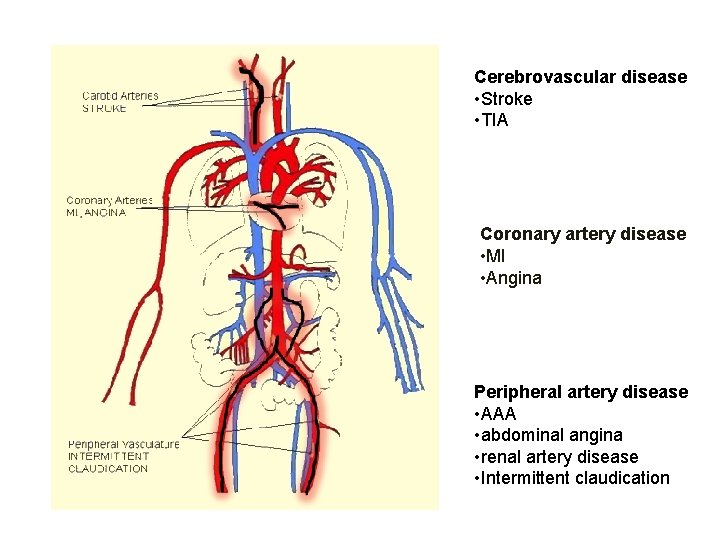
Cerebrovascular disease • Stroke • TIA Coronary artery disease • MI • Angina Peripheral artery disease • AAA • abdominal angina • renal artery disease • Intermittent claudication
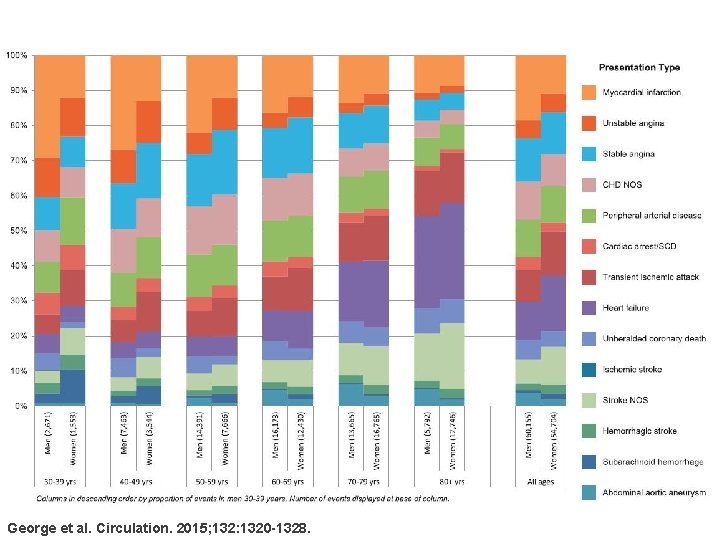
George et al. Circulation. 2015; 132: 1320 -1328.

Risk factors of atherosclerosis • Atherosclerosis is a systemic disease, but can be prevented. • Primary prevention is a key approach.

Risk factors of atherosclerosis development Non modifiable Modifiable • Age • Gender • Genetic • • • Hyperlipidemia Smoking Arterial hypertension Physical inactivity Diabetes mellitus Obesity
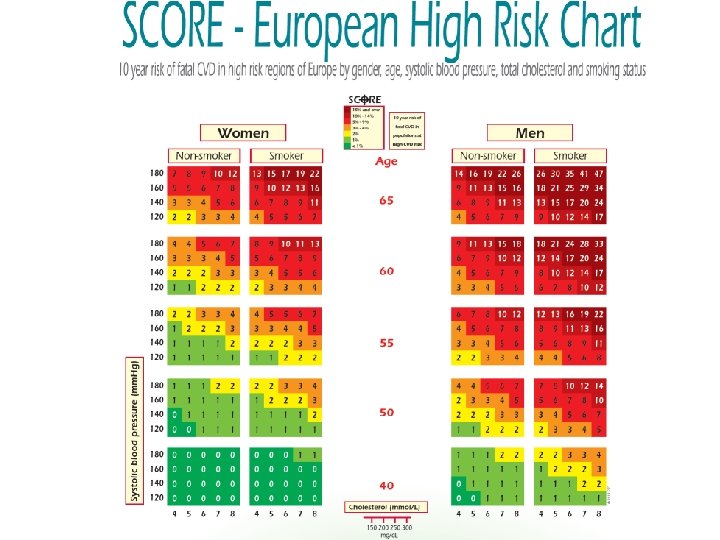

Dyslipidemia • Primary vs. secondary • Prevalence and mortality of CVD positively correlates with the level of total cholesterol and LDL • Total cholesterol • LDL • TAG • HDL
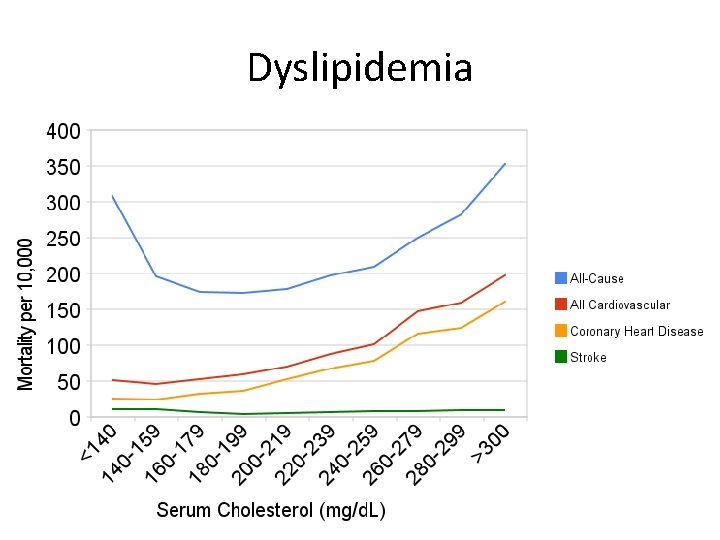
Dyslipidemia

Dyslipidemia Treatment options • Non-pharmacological § Diet § Exercise and avoidance of sedentary behaviors • Pharmacological § § Statins Ezetimibe Fibrates PCSK 9 inhibitors

Smoking • Active and passive smoking is a very important risk-factor • Nicotine promotes LCL-C oxydization, causes endothelial dysfunction, is prothrombogenic, promotes insulin resistance • Smoking cessation is the most effective mean of CV disease prevention and may leed to 36% reduction of MI mortality
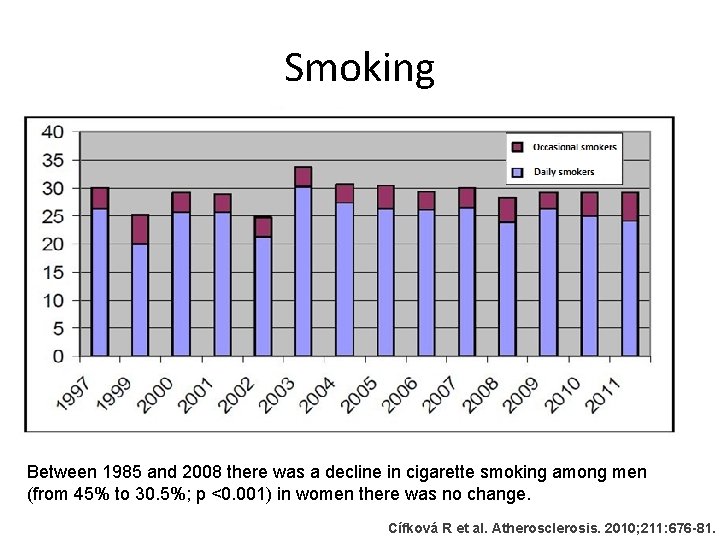
Smoking Between 1985 and 2008 there was a decline in cigarette smoking among men (from 45% to 30. 5%; p <0. 001) in women there was no change. Cífková R et al. Atherosclerosis. 2010; 211: 676 -81.
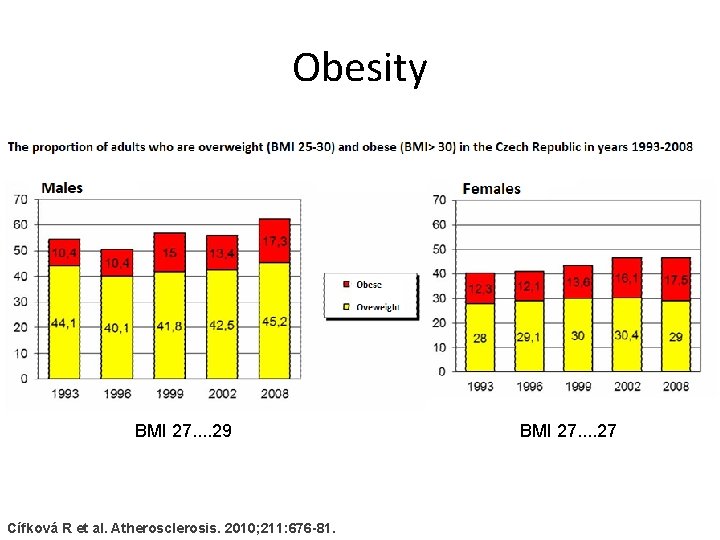
Obesity BMI 27. . 29 Cífková R et al. Atherosclerosis. 2010; 211: 676 -81. BMI 27. . 27
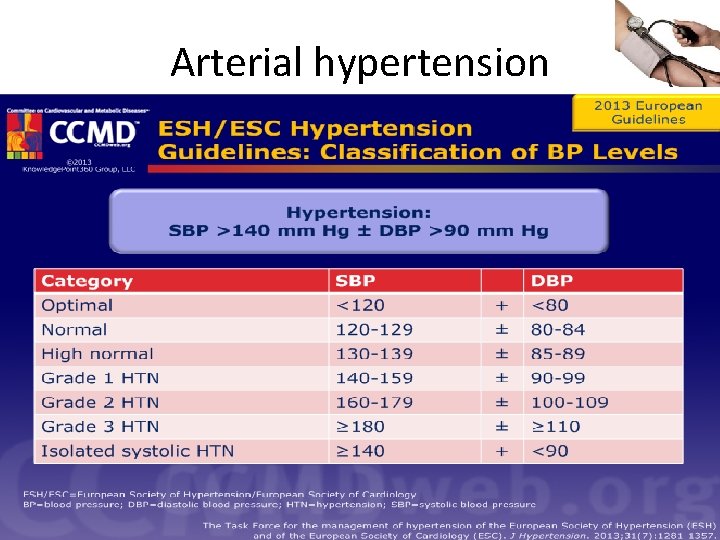
Arterial hypertension

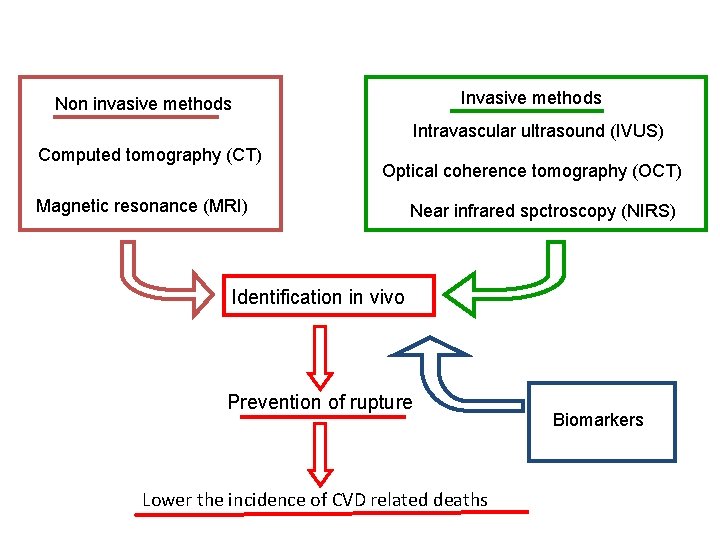
Invasive methods Non invasive methods Intravascular ultrasound (IVUS) Computed tomography (CT) Optical coherence tomography (OCT) Magnetic resonance (MRI) Near infrared spctroscopy (NIRS) Identification in vivo Prevention of rupture Lower the incidence of CVD related deaths Biomarkers
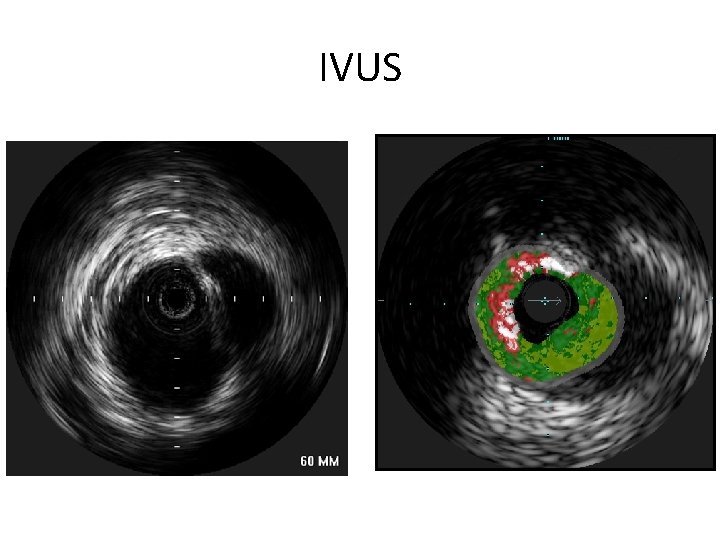
IVUS
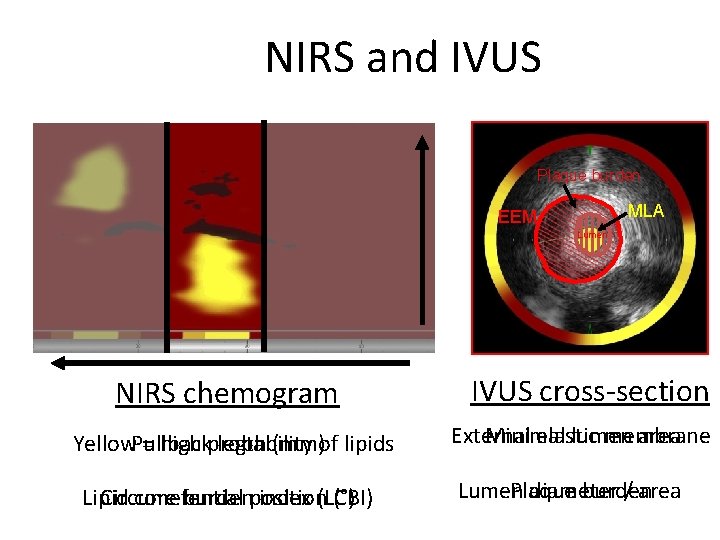
NIRS and IVUS Plaque burden MLA EEM Lumen NIRS chemogram Yellow = high probability of lipids Pullback legth (mm) Lipid core burden index (LCBI) Circumefential position (°) IVUS cross-section External elastic membrane Minimal lumen area Lumen diameter / area Plaque burden
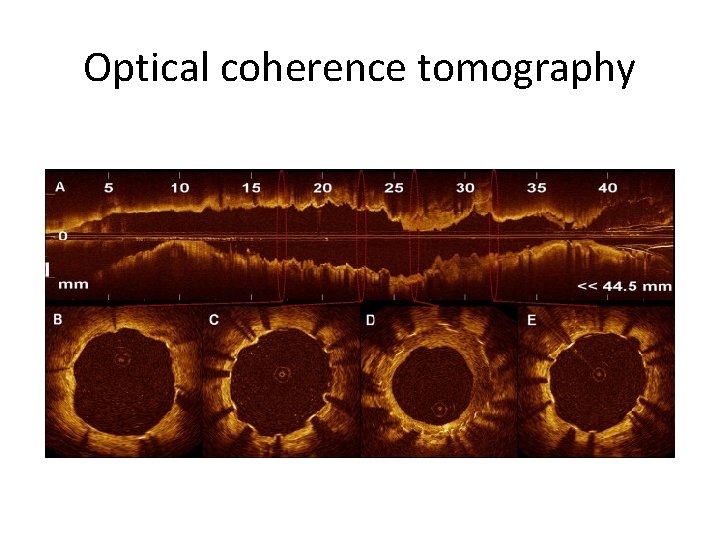
Optical coherence tomography

Stable ischemic heart disease
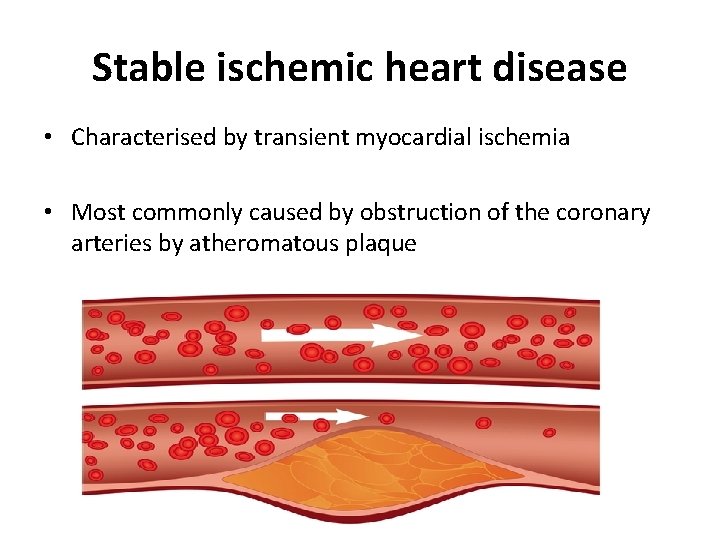
Stable ischemic heart disease • Characterised by transient myocardial ischemia • Most commonly caused by obstruction of the coronary arteries by atheromatous plaque
Physiology of coronary circulation • Coronary blood flow is phasic with maximal flow in diastole. • 75% of the oxygen delivered by coronary arteries is extracted by LV → limited oxygen extraction reserve in coronary circulation. • At 85% lumen diameter reduction at rest (85% at maximum exercise), vasodilator reserve is exhausted → inadequate pressure distal to the stenosis → rest or exertional myocardial ischemia

Classification • Chronic stable angina pectoris • Variant angina pectoris • Microvascular AP and syndrome X • Asymptomatic myocardial ischemia
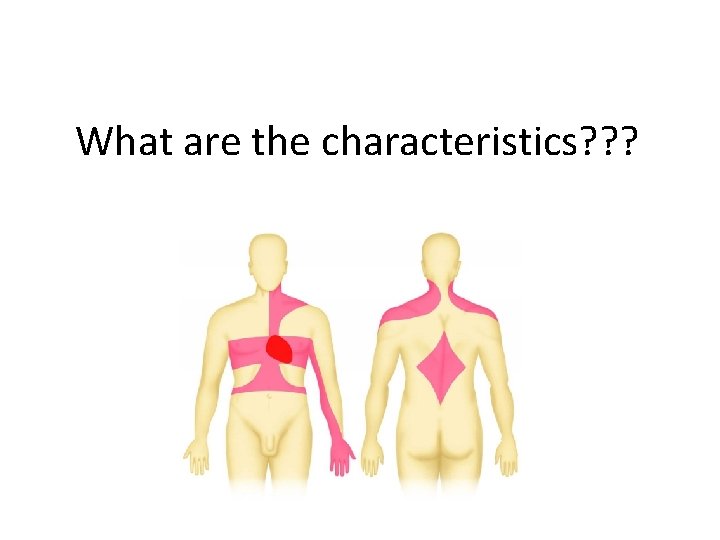
What are the characteristics? ? ?

Chronic stable angina pectoris • Typical angina pectoris and/or other symptoms Variant angina pectoris • Angina at rest associated with transient STsegment elevation, both resolving with the administration of nitrate.

Microvascular AP and syndrome X • AP caused by coronary microvascular dysfunction in patients who have nonstenotic arteries on coronary angiography. Asymptomatic myocardial ischemia • The objective evidence of myocardial ischemia (ECG) in the absence of chest pain.
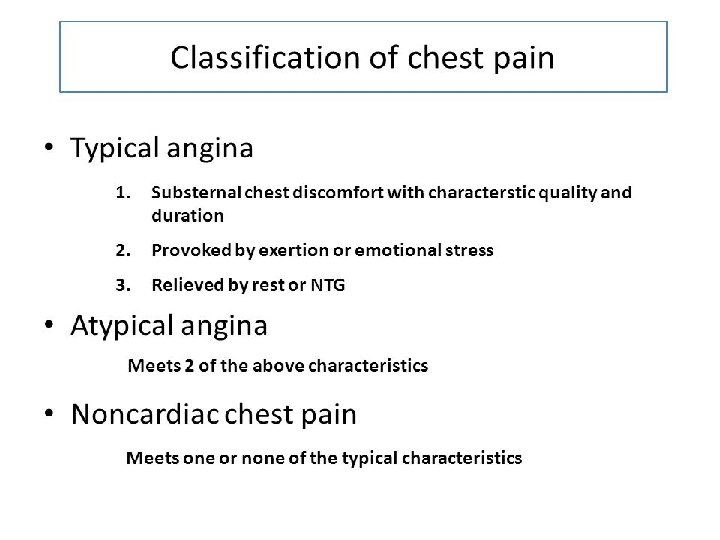


Grading of angina pectoris

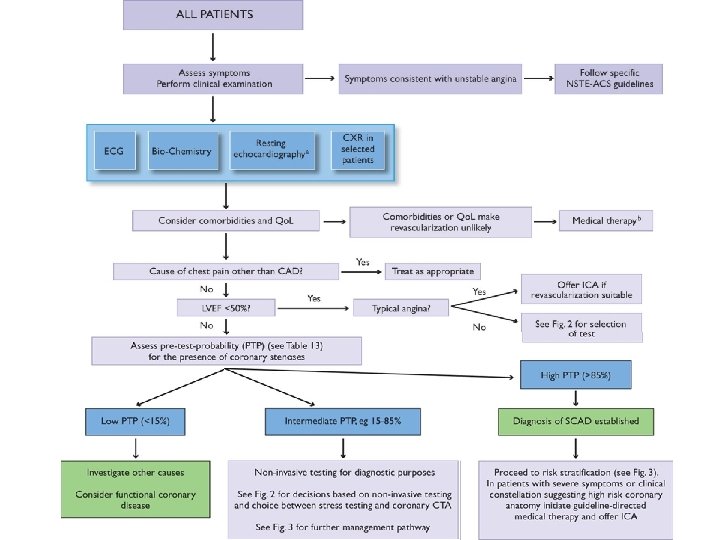
Evaluation • History- typical symptoms • Laboratory evaluation – dyslipidemia, hyperglycemia, renal disease etc. – biomarkers- hs-CRP, MMP-1, PAPP-A • • • Resting ecg ECHO Stress testing CT angio Coronarography
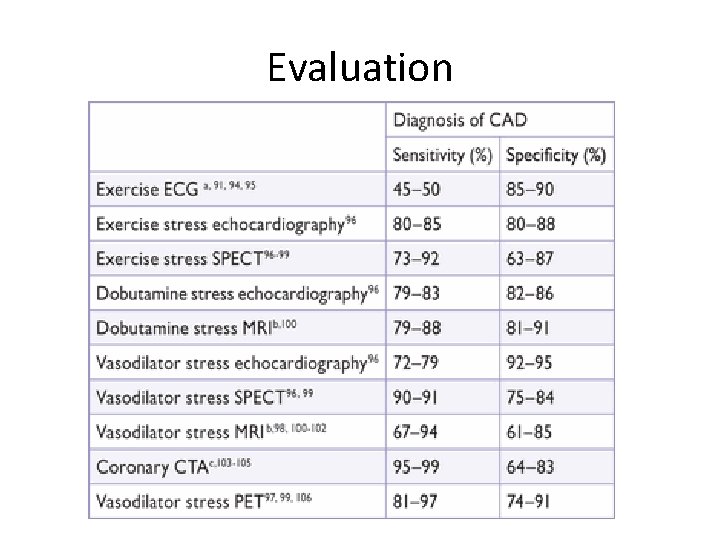
Evaluation
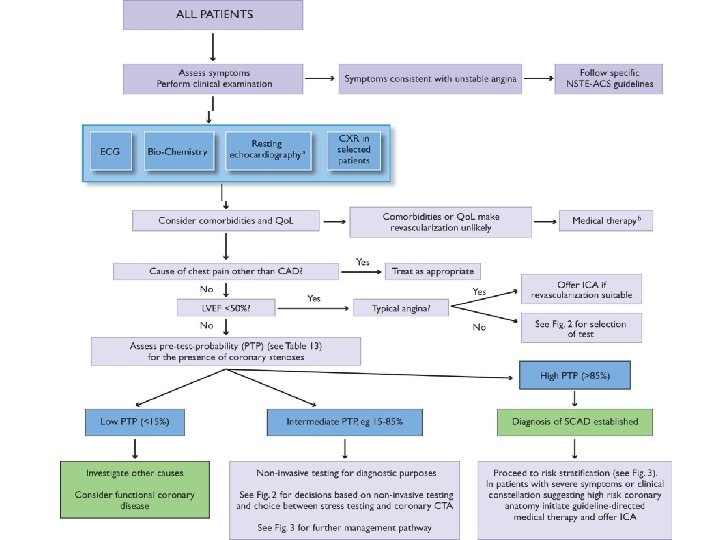
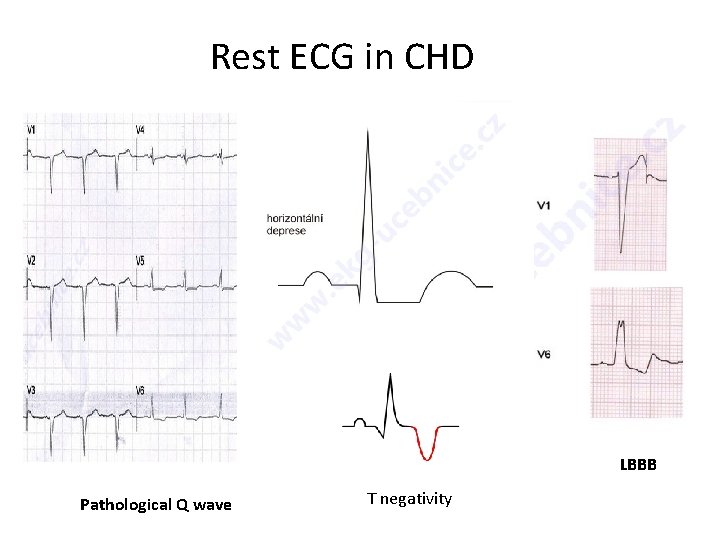
Rest ECG in CHD LBBB Pathological Q wave T negativity

Biochemistry • • Total cholesterol LDL HDL TAG hs-CRP hs-Tn. I fasting plasma glucose level HBA 1 C
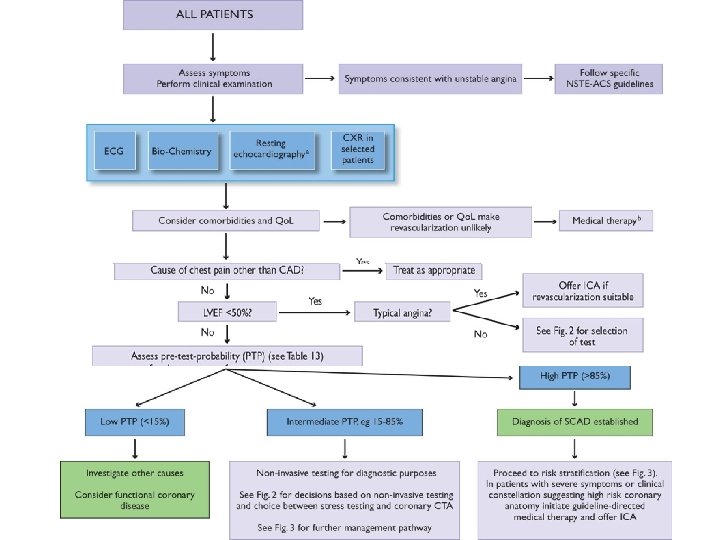
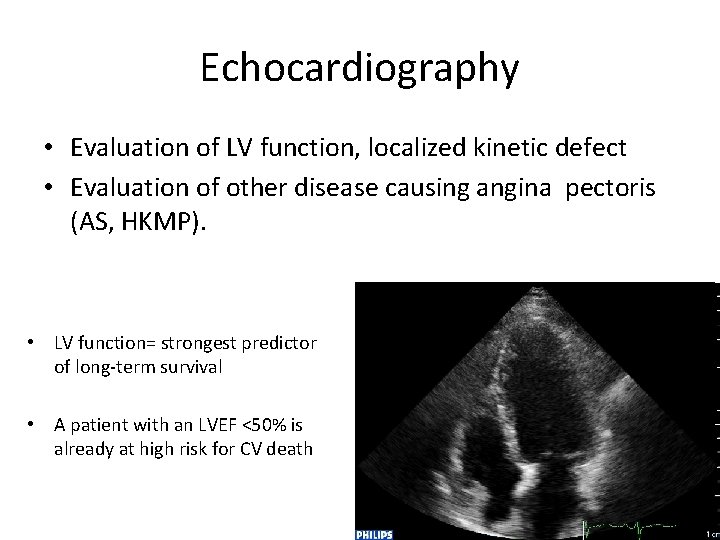
Echocardiography • Evaluation of LV function, localized kinetic defect • Evaluation of other disease causing angina pectoris (AS, HKMP). • LV function= strongest predictor of long-term survival • A patient with an LVEF <50% is already at high risk for CV death
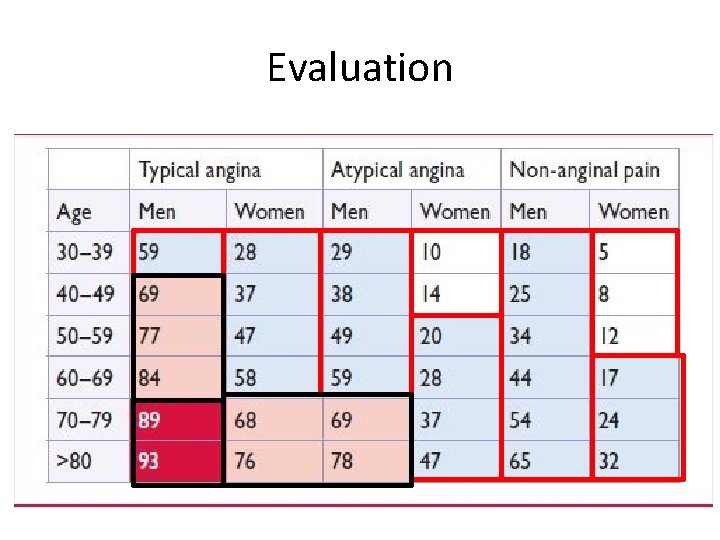
Evaluation
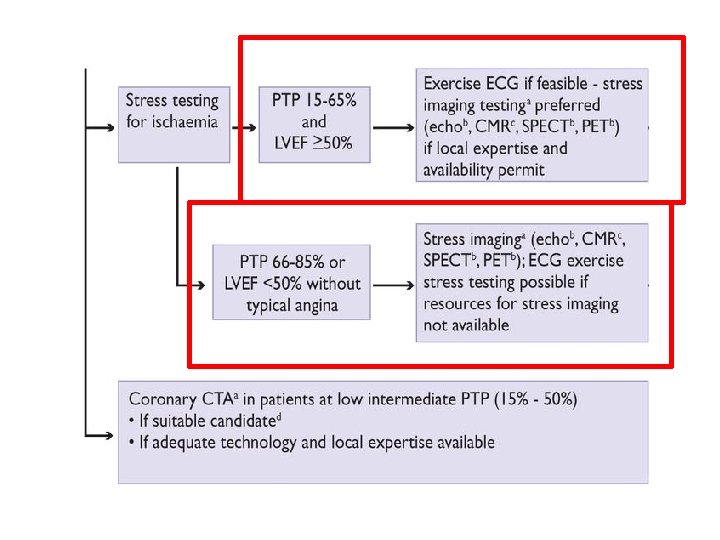

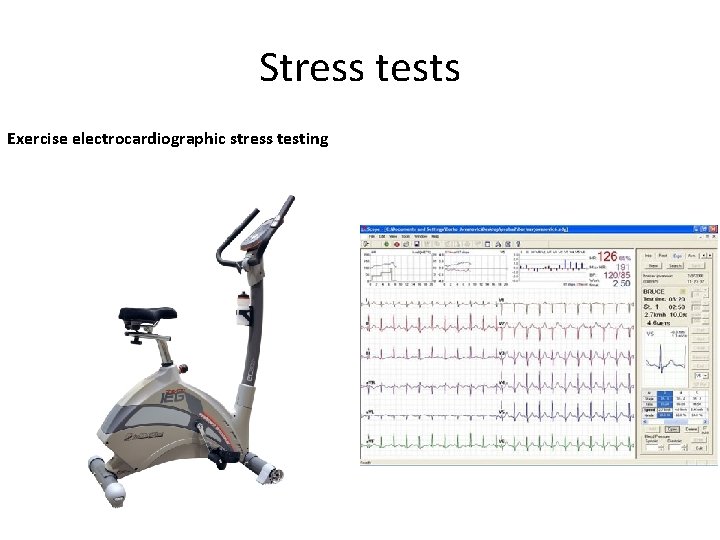
Stress tests Exercise electrocardiographic stress testing
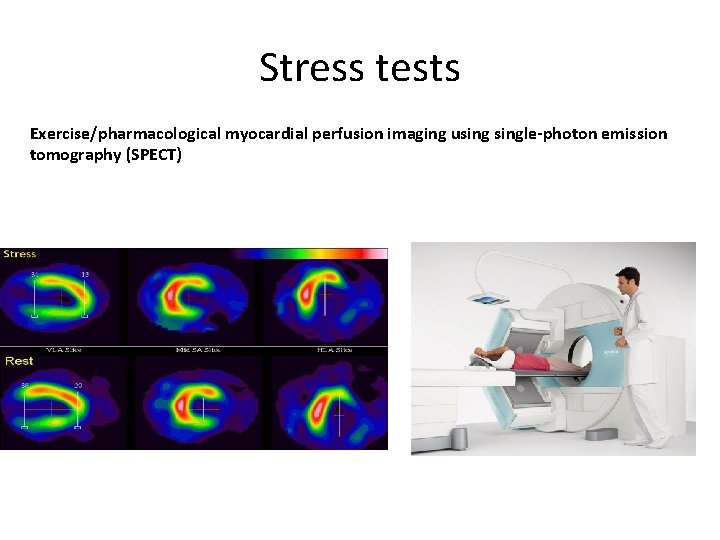
Stress tests Exercise/pharmacological myocardial perfusion imaging usingle-photon emission tomography (SPECT)
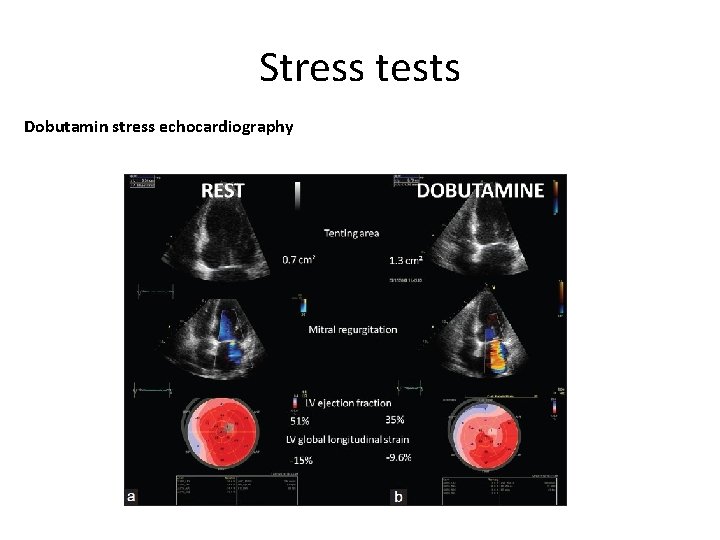
Stress tests Dobutamin stress echocardiography
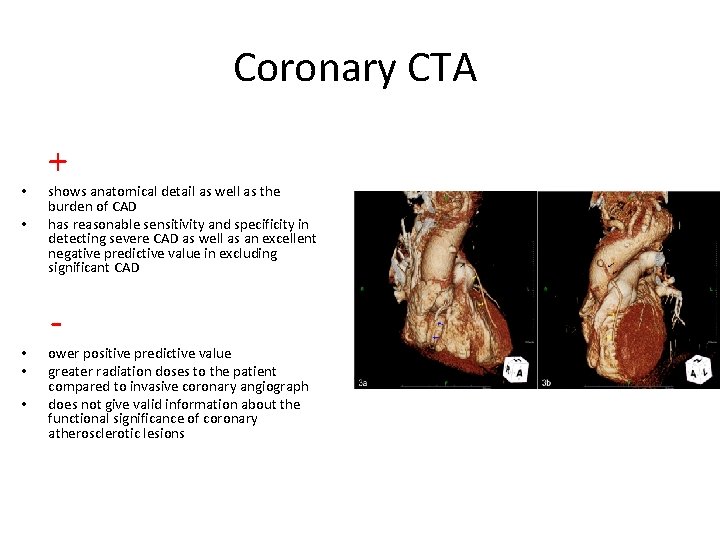
Coronary CTA + • • shows anatomical detail as well as the burden of CAD has reasonable sensitivity and specificity in detecting severe CAD as well as an excellent negative predictive value in excluding significant CAD • • • ower positive predictive value greater radiation doses to the patient compared to invasive coronary angiograph does not give valid information about the functional significance of coronary atherosclerotic lesions
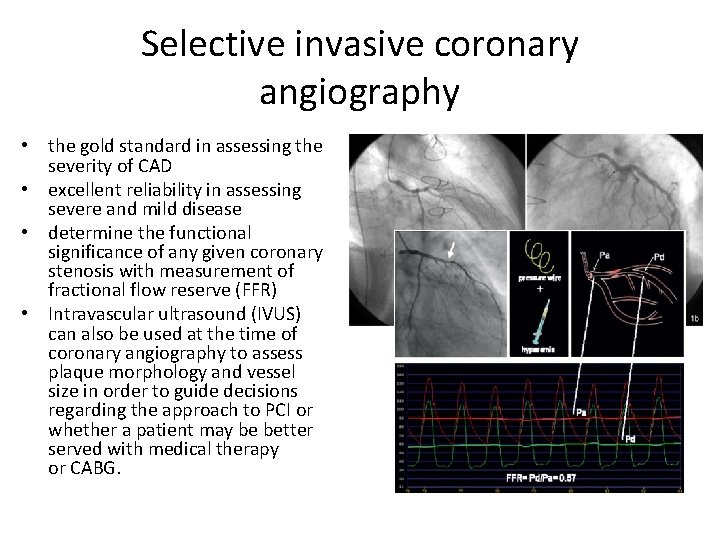
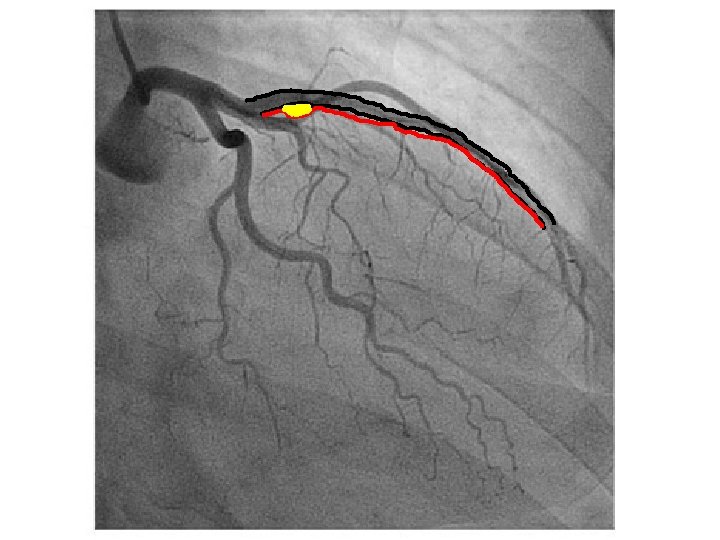
Selective invasive coronary angiography • the gold standard in assessing the severity of CAD • excellent reliability in assessing severe and mild disease • determine the functional significance of any given coronary stenosis with measurement of fractional flow reserve (FFR) • Intravascular ultrasound (IVUS) can also be used at the time of coronary angiography to assess plaque morphology and vessel size in order to guide decisions regarding the approach to PCI or whether a patient may be better served with medical therapy or CABG.

Management • Optimal medical therapy • Ravascularization – PCI – CABG

When to treat? How to treat? X Symptom relieve Prognosis

Optimal medical therapy • Symptom relieving drugs • Antiplatelet agents • Lipid-lowering agents • Prognostic medication

Relief of symptoms Anti-ischaemic drugs: • Nitrates: coronary arteriolar and venous vasodilatation - Short-acting nitrates for acute effort angina (sublingual nitroglycerin) - Long-acting nitrates for angina prophylaxis (Isosorbide dinitrate, Mononitrates)

Relief of symptoms II. Anti-ischaemic drugs: • Betablockers: reduce heart rate, contractility, AV conduction, increase perfusion o ischaemic areas by prolonging the diastole (metoprolol, bisoprolol, atenolol) • Calcium channel blockers: vasodilation and reduction of the peripheral vascular resistance - Non-dihydropyridines e. g. heart rate-lowering (Verapamil, Diltiazem) - Dihydropyridines (amlodipin)

Event prevention • Antiplatelet agents: - decrease platelet aggregation and may prevent formation of coronary thrombus (Low-dose aspirin, Clopidogrel) • Lipid-lowering agents: - (treatment target is LDL-C < 1. 8 mmol/L) • Renin-angiotensin-aldosterone system blockers: reduce total mortality, MI, stroke and heart failure among specific subgroups of patients (HF, PAD, DM)
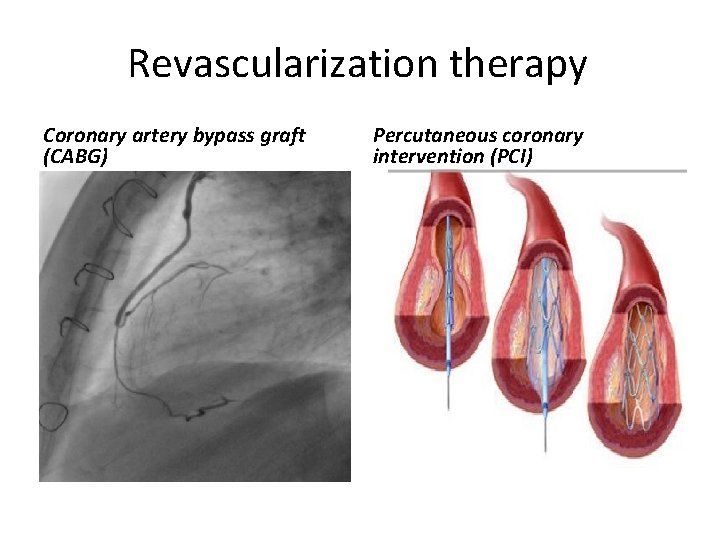
Revascularization therapy Coronary artery bypass graft (CABG) Percutaneous coronary intervention (PCI)

Revascularization? • Angina despite medical therapy? • Significant ischemia? – More than 10% on SPECT – More than 3 segments on stress ECHO – FFR <0. 80 • Systolic dysfuntion? • Coronary anatomy? – Multivessel disease, left main disease, proximal LAD
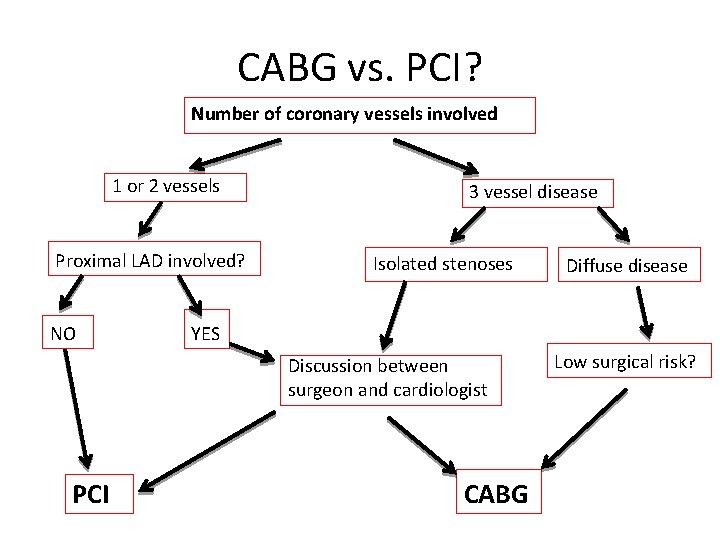
CABG vs. PCI? Number of coronary vessels involved 1 or 2 vessels Proximal LAD involved? NO 3 vessel disease Isolated stenoses YES Discussion between surgeon and cardiologist PCI Diffuse disease CABG Low surgical risk?

Thank you for your attention
- Slides: 60